Abstract
Introduction
Aging-in-place facilitate seniors to stay in their homes throughout the aging process. Place-based Occupational Therapy is a proposed service delivery model aimed at facilitating this. This study explores community occupational therapists’ perspectives on how place-based Occupational Therapy could facilitate aging-in-place and the perceived enablers and barriers to this model of care.
Method
The participants were occupational therapists working in the community setting. Data was collected through semi-structured interviews. An aging-in-place capability framework was employed to guide the interviews. A generic descriptive-interpretive qualitative research approach was used for the analysis.
Results
Data saturation was reached at the seventh interview (n = 7). Six major themes were generated to explore the perspectives of occupational therapists on a place-based strategy to deliver Occupational Therapy services: (i) maintaining health and function, (ii) partnering with caregivers, (iii) ideal location within neighborhoods, (iv) understanding clients’ environment strengthens intervention, (v) facilitating social connections and cognitive wellness, and (vi) enablers for service set-up. Besides financial support, key enablers include clinical expertise and program management experience.
Conclusion
Findings from this study can facilitate future planning of place-based Occupational Therapy services. The services should be fuss-free, short-term and affordable. The service should be sited where many older adults gather in their neighbourhoods, within walkable distance from their homes. Occupational therapists can contribute to program planning to maintain health and function and facilitate relationship building between older adults. There is potential for place-based occupational therapists to contribute to health promotion due to the profession’s unique focus on habits and environment.
Introduction
The World Health Organization (2024) had asserted that health and well-being are closely influenced by the social determinants of health, non-medical factors that influence health outcomes for example, education, housing, employment opportunities, social relationships and community networks. There is an ongoing interest globally to implement effective and cost-effective place-based interventions (McGowan et al., 2021). Differences in ‘place’ characteristics can contribute to health inequalities in different places for example, in England, healthy life expectancy differ by 21.5 years for females and 15.8 years for males between different local government areas (Office of National Statistics, 2018).
Place-based approaches are customized to meet the needs of local communities and involve various partners actively collaborating to solve complex issues (Queensland Government, 2023). Various countries have implemented place-based community health worker (CHW) programs as a way to improve health outcomes in their communities (Ahmed et al., 2022). In the United States, CHWs are trained to provide health education, advocacy, and support to individuals and families in their communities. Place-based CHWs are often “from the same community they serve, and possess a deep understanding of the community’s social, cultural, and economic context” (Ahmed et al., 2022). They provide health education and resources, signposting individuals to healthcare services, and advocating for their health and wellbeing (Ahmed et al., 2022). In Queensland, place-based approaches are driven by the community, and are part of the collective impact movement (Queensland Government, 2023).
In Singapore, with a rapidly ageing population, the health and social needs of the residents have increased (Chen et al., 2024). This demographic shift necessitates innovative strategies to support older adults’ functional independence and ability to age-in-place. In recent years, national initiatives such as Healthier SG and Age Well SG, prioritize enabling older adults to age-in-place, fostering independence and well-being in their familiar surroundings. Fortifying residents’ self-management capabilities through activation and empowerment and moving care from inpatient to the community settings thereby reducing reliance on hospital care, are game plans to keep the health system sustainable (Ge et al., 2023). Occupational Therapy (OT) plays a part in supporting this goal.
In Singapore, the three healthcare clusters have established their own regional health systems and function as population health managers, shifting focus from managing patients with acute illness episodically in facility-based settings to managing the health of populations through empowering people, and forming collaborative partnerships within the regions (Chen et al., 2024). The Communities of Care (CoCs) is a framework commissioned by the Agency for Integrated Care 1 to build local networks of collaboration among care providers, to deliver health and social care for a defined population of residents in neighbourhoods (Agency of Integrated Care, 2024). In CoCs, place-based approaches are customized to meet the needs of local communities and involve various partners actively collaborating to solve issues, with emphasis on place and residents (Queensland Government, 2023). Successful CoCs place residents in the center of the community care ecosystem and provide support to help them age-in-place and maintain interest and participation in managing their health. Place-based interventions offer promise to enhance the social determinants of health and reduce health inequities (Smedley & Amaro, 2016). An example can be care partners offering active ageing programs that leverage on unique assets in the neighbourhood and strengthen social relationships amongst residents.
Currently, community rehabilitation services in Singapore are either home-based or center-based. Home-based OT refers to OT provided in the client’s home. Centre-based OT services are provided at day rehabilitation centres (DRCs) sited in the community, where clients with rehabilitation goals attend therapy sessions. While both modes offer valuable support, limitations exist. A study by Chen et al. (2014) shed light on the barriers to DRC attendance such as functional (e.g. no direct transport from home to DRC), social (e.g. no caregiver to accompany client to DRC), financial (e.g. out-of-pocket expenses of DRC attendance add up over time) and perceptual (e.g. clients do not see the need for further rehabilitation). On the other hand, home-based therapy service providers may be unfamiliar with the client’s neighbourhood context as the providers typically cover a large geographical area or even island-wide. For example, home-based OT may be unaware of the barrier-free routes in local areas that are essential for training clients learning to drive mobility scooters.
Potentially, place-based OT services operate within a defined geographical area, capitalizing on the strengths of both home-based and center-based services. Occupational therapists (OTs) can work directly with residents in their communities, tailoring interventions to address individual needs and utilizing neighbourhood resources. This approach aligns with successful place-based CHW programs implemented globally (Ahmed et al., 2022). On an individual level, the Person-Environment-Occupation-Performance (PEOP) model (Baum et al., 2024) postulated that interaction between an individual and his/her environment such as social support, public policies and the physical built-up environment, can positively or negatively affect the individual’s performance in occupations (activities, tasks or life roles). When there is good person-environment fit in supporting a valued occupation, successful performance eventually leads to improved participation and enhanced well-being of residents (Christiansen et al., 2024). Hence, when it comes to ageing-in-place, environmental factors such as the design, layout, and accessibility of the home and neighbourhoods as well as social networks, relationships and community support systems, greatly influence occupational performance of older adults. By incorporating these environmental factors within the PEOP model, clinicians can gain a better understanding and tailor more personalized solutions to better align older adults with their environment and occupations, ultimately improving their quality of life.
While place-based OT shows potential to be able to facilitate ageing-in-place, studies on this approach is lacking. To address the knowledge gap, this qualitative research study was conceptualized. The study design was guided by the conceptual framework on “ageing-in-place in the neighbourhood environment from a capability approach” (Bigonnesse & Chaudhury, 2021). This framework provides a multi-faceted understanding of ageing-in-place processes in the context of a neighbourhood environment.
In the framework, ageing-in-place is central and is influenced by key components of place integration, place attachment, independence, mobility and social participation (Bigonnesse & Chaudhury, 2021). These key components are essential for successful ageing-in-place and are in turn influenced by factors, that is, individual factors, accessible built environments (home & neighbourhood), proximity of services & amenities and meaningful social connections. These 4 factors are indirectly related to ageing-in-place through the place integration processes of familiarity, routines, habits & embodiment, safety and everyday life activities.
The conceptual framework was used to guide the development of the interview guide and thematic analysis. The study explored the perspectives of local community-based OTs on how place-based OT service facilitated older adults to age-in-place and what the perceived enablers and barriers to implementing this new model of care were.
Both the PEOP model and the “ageing-in-place in the neighbourhood environment from a “capability approach” conceptual framework emphasize the interaction between individuals and their environments in promoting well-being and participation. The PEOP model highlights the individual’s abilities, the environment, meaningful activities, and participation, while the capability approach focuses on enhancing individuals’ abilities to achieve desired outcomes within supportive neighbourhoods. Both models aim to empower individuals, adapt environments, and foster community engagement to support ageing-in-place, ultimately promoting independence and quality of life for older adults.
Methodology
Study design
This research employed a generic descriptive-interpretive qualitative research (GDI-QR) approach (Hill & Knox, 2021). This method involves in-depth exploration of participants’ experiences and perspectives through interviews. GDI-QR was chosen for its ability to gather rich descriptive data through open-ended questioning, allow for deeper interpretation of local community-based OTs’ perspectives of place-based OT model of care. Thematic analysis (Naeem et al., 2023) was used to identify recurring themes and sub-themes. Ethics approval was obtained from the Singapore University of Social Sciences (2023-GER 688-01 (001)), and written informed consent was obtained from all participants. The Consolidated Criteria for Reporting Qualitative Studies guideline (Tong et al., 2007) was used to guide the reporting of qualitative research.
Participants
Purposive (non-probability) sampling was used to recruit OTs working in community settings in Singapore. The researcher leveraged on her professional network to identify and invite potential participants who met the inclusion criteria through email. Three potential participants are the author’s ex-colleagues with no work association at the time of recruitment. Hence, there was no conflict of interest. The inclusion criteria are English-speaking, currently practicing OT with at least two years of experience working with older adults in community settings, comfortable with Zoom interviews and able to provide informed consent.
Participant Demographics (n = 7)
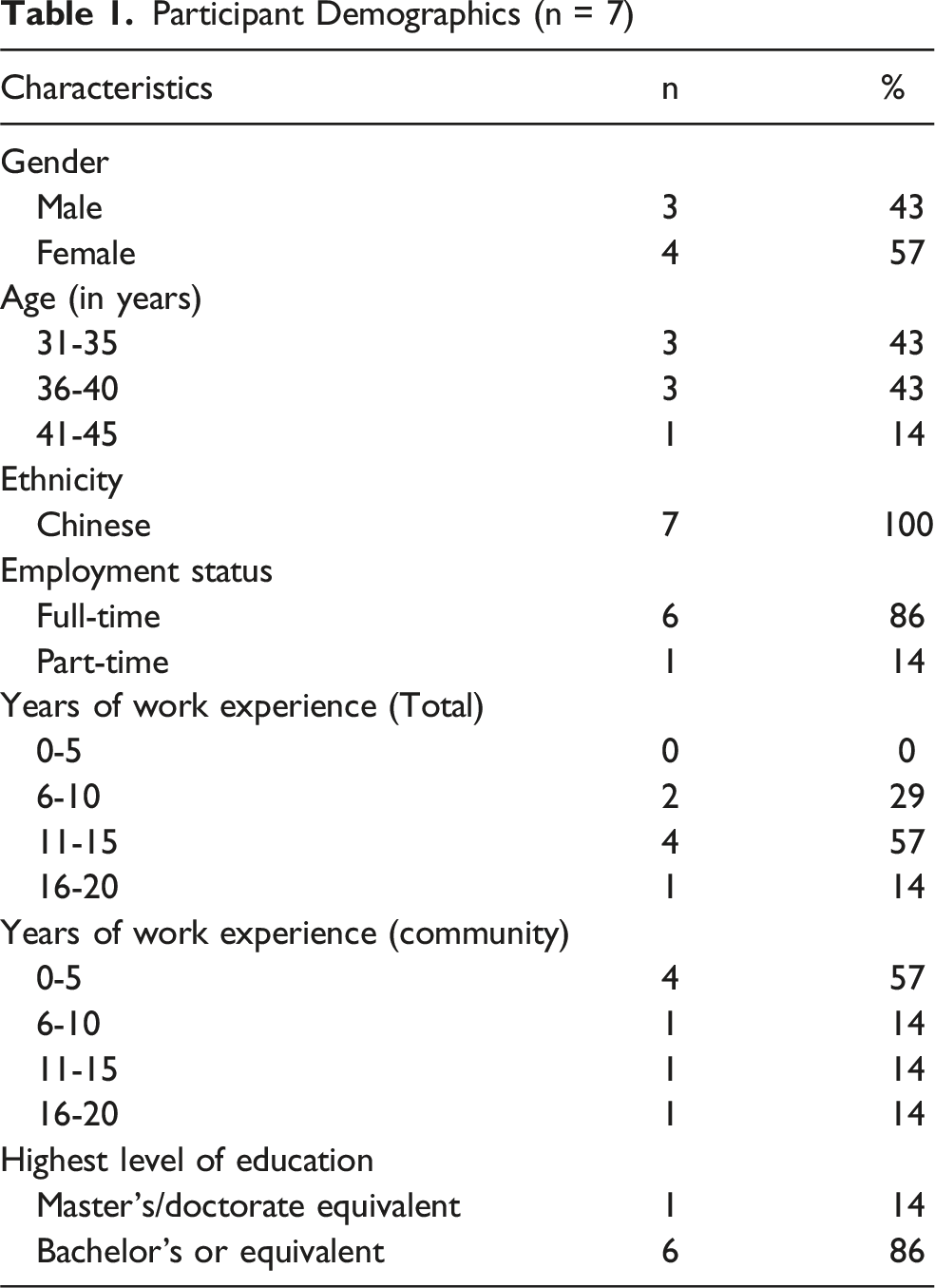
Study procedures
Before each interview commences, the researcher provided participants with information on the research and on place-based OT. All participants signed the informed consent form and emailed back to the researcher. All interviews were conducted by the researcher via the teleconference platform Zoom (Zoom Video Communications, 2023) following a pre-developed interview guide. The interviews took place between December 5th, 2023, and February 21st, 2024, in Singapore, lasting 60-80 minutes each (average 65 minutes). The interview guide included key questions and prompts, ensuring consistency across interviews. No repeat interviews were conducted. All participants were reimbursed approximately USD$22(S$30) to compensate for their time.
The researcher facilitated the interviews and took field notes. Interviews were audio-recorded and transcribed from audio to text using the Zoom platform. The researcher then anonymized the transcripts and manually checked and edited them for accuracy by listening to the audio recordings. Afterward, the audio recordings were deleted for confidentiality.
Data analysis
A qualitative analysis software QDA Miner Lite (version 3.0.2) was used to organize the data. The researcher familiarized herself with the transcripts to get a good understanding of the data. The researcher initially coded the first two transcripts to identify common themes. Codes were then refined for consistency. Subsequently, the remaining five transcripts were coded line-by-line using the refined coding framework. Similar codes were clustered to create themes. New themes were added as novel concepts emerged from the data. Themes and sub-themes were ultimately developed based on the seven participants’ narratives. Data analysis was performed simultaneously with data collection, until data saturation was reached. Data triangulation was performed by the researcher comparing the field notes taken during each interview with each transcript before coding. Following data collection, member checking was performed, where participants reviewed the findings for comments and corrections. The second author, a psychologist with expertise in research methodology, provided technical advice throughout the research process.
Some initial themes aligned with the interview guide that was based on the “ageing-in-place in the neighbourhood environment from a capability approach” framework (Bigonnesse & Chaudhury, 2021).
Results
Six major themes emerged (refer to Appendix) from data analysis:
Theme 1: Maintaining health and function of older adults
Four participants opined that place-based OT services can partner older adults to work on what matters to them to maintain their health and functional abilities. P002 illustrated with the example of “a client who wished to walk to the coffee shop a few blocks away to buy his own meals”. P002 then brainstormed with the client and accompanied the client to trial different modifications and succeeded.
P004 envisioned place-based OT to be a “fuss-free, timely service that meets residents’ needs and support ageing-in-place”. He mentioned that “if there’s a place-based OT there every Tuesday morning, residents can just make an appointment to go and consult. So then they will come, and the OT can advise them or signpost them to what they need, or do some quick consult to solve their problems.” P003 perceived place-based OT helps older adults to “really age-in-place” so they do not have to frequent the emergency departments, or be admitted to nursing homes if they cannot cope at home. P006 opined that place-based OT services are suitable for short-term interventions (likely 3 or less sessions) such as equipment prescription, caregiver training and prevention work.
Sub-theme 1.1 Supporting older adults recently discharged from hospitals to prevent deterioration
For clients recently discharged from inpatient care and awaiting acceptance to community rehabilitation in DRCs which typically takes from two or more weeks, three participants articulated that place-based OT can potentially reduce wait time for therapy, so they do not deteriorate functionally while awaiting DRC services. P001 conveyed that “place-based OT can provide more timely solutions to these clients because waiting time can be very long. The clients’ profiles or care needs would have changed during the wait”.
Sub-theme 1.2 Supporting older adults after community rehabilitation
Two participants envisioned that just-in-time place-based OT can be a post-discharge service that DRCs provide for their discharged clients. If the discharged clients require DRC service again, the place-based OT service can refer the clients back to the DRCs. One participant articulated that place-based OT service can also refer clients to community-based ageing-in-place services such as Active Ageing Centres (AACs) so they do not deteriorate functionally post discharge from DRCs. AACs are drop-in centres that are initiated in neighbourhoods to engage older adults with social and leisure activities in groups such as karaoke, arts & craft, cooking and exercise programs, befriending and referrals to care services (Ang, 2024). There are 208 AACs in Singapore as of April 2024 (Ang, 2024).
Another two participants felt that place-based OT services can help clients re-integrate back to the community by checking whether discharged clients are complying with the home exercises taught by the DRC therapists and whether equipment prescribed to clients like personal mobility aids are being used. Three participants concurred that sometimes clients need time to consider whether to join the AACs and place-based OT can follow up with them and introduce them to the AACs.
Theme 2: Partnering caregivers to provide seamless and coordinated care
Four participants acknowledged the important role that caregivers (usually family members or domestic helpers) play in supervising clients to perform home exercises. If caregivers are taught to modify the home exercises and come up with different repertoires to execute the homework to achieve therapy goals, then the clients will be meaningfully engaged.
Several participants opined that place-based OT services can be a valuable signposting service to caregivers to navigate the healthcare system such as sharing with caregivers about community resources which can benefit clients and/or caregivers. These can be situation-based support such as psychosocial support, financial support or even home-based support. This has been also brought up by Ge et al. (2023) who opined that seamless access to community resources is a critical enabler for self-management and that clients have limited knowledge concerning the range of options and services that can meet their needs. One participant shared that place-based OTs can also teach caregivers to distinguish credibility of online health information from misleading material.
Theme 3: Place-based OT services are ideally located within neighbourhoods proximal to residents’ homes
Currently, DRCs face a challenge to coordinate transport timing with therapy slots and client’s availability. Mismatch of these variables result in long wait time for clients to be admitted to DRC.
Clients will usually be accompanied by caregivers if they need to travel on transport to access services. Clients’ children may have to take leave to accompany them if the domestic helpers are unable to manage. P005 and P003 both opined that there will be more convenience and cost savings on transport if clients can access the place-based OT by walking or wheelchair or using motorized devices. Caregivers will not need to take leave to bring the clients there through taxi or car.
Most participants concurred that place-based OTs will value working near to the clients’ homes, as they can easily walk or take a feeder bus to see clients in their homes and neighbourhoods. This can translate to more work efficiency for OTs as they do not have to make arrangements and spend time travelling in transport both ways. Three participants felt that to be closer to older adults, the ideal site for place-based OT services will be within or near AACs. Two participants mentioned that place-based OTs can set up OT posts within AACs on a regular basis.
One participant opined that the service location and accompanying amenities are very important especially during wet weather for example having sheltered walkway, sheltered car park, proximity to public transport. For clients to access a centre within walking distance, a sheltered walkway is important. As they mostly walk or come in wheelchairs, their caregivers are pushing them. When it rains or is too sunny, it is challenging for the caregiver to hold the umbrella, and push the wheelchair simultaneously. When it becomes too difficult, clients and/or caregivers may choose to abandon the therapy session altogether.
Theme 4: Understanding clients’ routines, habits, everyday activities and environment strengthens the impact of therapy
Clients have placed attachment (emotional bonding) to their homes and neighbourhoods (Bigonnesse, 2017). Therapists’ familiarity with their clients’ routines, habits, everyday activities (which happen in their homes and neighbourhoods) strengthen the impact of therapy. Place-based OTs can contextualize the recommendations they provide to clients and incorporate familiar elements into therapy practice. P001 recounted that “when we bring this client out for community integration, then they walk past this particular hawker stall. The next time when I visit the hawker stall, I will ask the hawker if the client comes to eat daily. In community, you can’t be just attending to the client, you need to see what’s the bigger picture, understand the community this client operates in”.
It is important for place-based OT to get a lay of the land so that he/she can figure out what the needs of this particular community. The knowledge and the flexibility to work with residents living in an area is important. For example, one participant explained by comparing Chinatown with Shunfu (see Appendix). Clients’ familiarity with services in their neighbourhoods make it fuss-free for them to get appointments. Therapists can leverage on the peer support networks within the neighbourhood to persuade clients to change their behaviors.
Theme 5: Facilitate older adults to develop meaningful social connections and maintain cognitive wellness
AACs have a mandate to offer evidence-informed programs to meet five key domains of social, physical health, cognitive, learning and volunteerism (Age Well, 2024) to their clientele. Participants expressed that there is a role for place-based OT to value-add to AAC offerings such as training the AAC staff to plan group programs to meet different needs. AAC staff are typically non-healthcare nor social care professionals who may lack knowledge to plan and conduct group activities to meet therapeutic goals effectively.
Two participants mentioned that place-based OTs can also share with AACs’ staff what OTs do, and the AAC staff can be the eyes and ears to pick out and refer vulnerable residents for example those with high fall risk, to the OT Posts. Residents with needs can come to the OT posts themselves (self-referrals) if they understand how place-based OT can help them.
P003 commented that place-based OT can “help residents attending AACs to be healthier by participating in group exercises, developing more hobbies and making more friends”. Potentially, place-based OTs based in AACs can encourage residents to attend activities organized by the AACs and relate to residents how participation can help them improve their health. OTs can embed healthy habits into daily routines (Epley et al., 2021) into the design of AAC activities. P006 also commented that place-based OTs can visually check on frail residents in the AACs, especially those with physical disabilities and offer help. She shared that her team did a sensing check with one AAC and found that about 30% of the AAC’s clients are frail and likely will benefit suitable from place-based OT interventions. The place-based OTs will also be able to discuss with AACs’ staff how the AACs can help these frail residents.
Theme 6: Barriers and enablers in setting up place-based OT services
Participants mentioned three enablers to place-based OT, namely subvention, OT experience and endorsement from the hospitals. These are mostly system-level enablers.
Sub-theme 6.1: Reducing out-of-pocket payment increases access to place-based OT services
All participants shared that many day care clients prefer to use government-subsidized services, otherwise they are reluctant to attend. Non-subvented services is a potential barrier to implementing place-based OT services. P001 remarked that “many prefer to have their OT services in the hospital because they can confirm they can get the subsidized rate, rather than coming to the community”. Hence, availability of subvention will increase access to the place-based OT service and improve the sustainability of the service. As shown in previous studies (Jalali et al., 2021), maximizing the public sector’s share and reducing out-of-pocket payment in health services can help residents feel comfortable to seek health services when they need it. As place-based OT services are meant to be short-term and just-in-time to meet clients’ needs, clients may be more inclined to access the service when subvention is available fuss-free and out-of-pocket payment is minimized. Some participants brought up that the subvention for place-based OT services should ideally be simple and straightforward, and clients do not have to undergo means testing.
Sub-theme 6.2: Place-based OTs need clinical, contextual and program management capabilities
Participants all agreed that place-based OTs have to work for a few years before taking on the role. Most participants opined that having acute hospital work experience is important as this offers the therapist structured training opportunities to treat clients presenting with a wide range of medical conditions. Place-based OTs will likely be working independently in respective geographical areas and will need to know and perform a repertoire of OT interventions. It is unlikely that recent OT graduates will be able to take on place-based OT roles effectively, making inexperience a likely barrier to implementing place-based OT services. P005 remarked that it would take him at least 5 years of work experience before he is confident to assume this role. Two participants advocated that place-based OTs should be familiar with the concept of social determinants of health, which are contextual factors affecting clients’ health and quality of life. Another two participants advocated for place –based OTs to have an understanding of program management.
Sub-theme 6.3: Hospitals’ endorsement engender trust between clients and place-based OT services
The third barrier to implementing place-based OT services is clients’ and family members’ unfamiliarity with community rehabilitation services. Two participants brought up about endorsement from the healthcare professionals in the hospitals to clients to give confidence to clients that community place-based OT services are “legit” that is provide real, genuine care and are trustworthy.
Discussion
This study explored the perspectives of local OTs on the potential of place-based OT services to support older adults’ ageing-in-place initiatives in Singapore, aligning with national programs like Healthier SG and Age Well SG. The GDI-QR approach is pragmatic and gathered data that is detailed, in-depth and rich, capturing the complexity and nuances of participants’ experiences and perspectives, which are applicable to real practice settings. The findings revealed a strong consensus among participants that place-based OT can be a valuable addition to the healthcare system, contributing to successful ageing-in-place. The findings are consistent with the PEOP model (Baum et al., 2024). By integrating place-based strategies with the PEOP model, OTs can develop more effective and contextually relevant interventions that support individuals in achieving their goals and improving their quality of life whilst ageing-in-place.
Strengthening community rehabilitation through place-based OT
This study identified two key areas where place-based OT can bridge gaps in current rehabilitation services. Firstly, participants highlighted the potential for place-based OT to initiate early community rehabilitation for clients discharged from hospitals. Studies by Koh et al. (2012) demonstrated the importance of timely supervised therapy for maximizing functional recovery post-stroke. Place-based OT services can bridge the waiting period before clients are accepted into DRCs, potentially improving long-term outcomes.
Secondly, the study revealed concerns among participants regarding the lack of support for clients and caregivers following discharge from DRCs. This aligns with Picco et al. (2016)’s findings on caregiver dependence among older adults in Singapore. Participants emphasized the need for continued support to prevent functional decline and to empower clients and caregivers. Scorrano et al. (2018) highlighted the importance of caregiver knowledge and motivation in adherence to home exercise programs. Place-based OT services can address this gap by providing education and support to both clients and caregivers, promoting self-management and adherence to therapy plans.
Optimizing service delivery through neighbourhood-based care
This study underscored the importance of locating place-based OT services within clients’ neighbourhoods. This aligns with Bigonnesse and Chaudhury's (2021) concept of “place integration,” emphasizing the connection between individuals and their environment. Research by Koh et al. (2022) and van Dijk et al. (2015) suggested that proximity to services and accessible public transportation are crucial factors for successful ageing-in-place.
Being situated within neighbourhoods allows place-based OTs to gain a deeper understanding of clients’ routines, habits, and living environments (Bigonnesse & Chaudhury, 2021), facilitating tailored ageing-in-place interventions that can better meet clients’ needs. This can significantly enhance the effectiveness of therapy compared to generic approaches. OTs can work with clients to develop goals for themselves to better interact with their living environments. With healthy interaction between individuals and their environments, individuals will experience success and improved well-being in occupational performance.
Leveraging AACs for enhanced social connectivity
This study identified AACs as potential locations for place-based OT services. AACs are established within residential estates to directly support older adults. Social participation, a key element of successful ageing-in-place (Anaby et al., 2011), can be fostered through AACs. Place-based OTs can contribute to program planning within AACs, ensuring activities are meaningful and cater to diverse interests and abilities (Koh et al., 2022; Wong et al., 2019).
Furthermore, place-based OTs can design and oversee inclusive therapeutic group activities within AACs, facilitating social connections and combating social isolation, particularly for older adults living alone (Linton et al., 2018; Ministry of Health, 2023). This aligns with Levasseur et al. (2015)’s finding that social interaction with peers can motivate older adults to stay active and engaged.
Additionally, place-based OTs can play a vital role in identifying vulnerable older adults at risk, such as those living alone or with complex needs. Collaboration with existing community providers like AAC staff and community nurses can be established to identify and facilitate referrals of frail residents and provide basic interventions, promoting a cost-effective and efficient system.
Enablers for sustainable place-based OT services
The study identified three key enablers for setting up sustainable place-based OT services from the participants’ perspectives - subvention, OT experience, and hospital endorsement. These factors differ from those highlighted in existing literature on place-based approaches (Rong et al., 2023). This emphasizes the uniqueness of implementing a place-based OT model within the Singaporean context.
Subvented services were seen as crucial for increasing access and program sustainability. Additionally, participants emphasized the need for OTs with strong clinical experience, coupled with an understanding of the social determinants of health and program management skills to lead place-based OT services. Mentorships to support newer therapists to transition to become place-based OT was suggested. Finally, endorsement from healthcare professionals in hospitals was identified as a potential factor to build clients’ trust and confidence in the quality of place-based OT services.
Implications for practice
The study presented findings on what place-based OT can offer. Clinicians can utilize the findings to develop place-based OT services. Place-based OT services can work with clients transitioning from hospitals or DRCs to prevent functional decline and empower them in self-management. Additionally, they can support caregivers by signposting them to navigate the healthcare system and accessing community resources.
The study suggests locating place-based OT services within neighbourhoods, potentially in AACs, to improve physical accessibility for residents. Place-based OTs can train and collaborate with AAC staff to design programs that meet diverse needs of residents through embedding health-promoting habits and routines (Epley et al., 2021) into the AAC programs.
There is potential for place-based OTs to influence and value-add to health promotion on a population health level. This will involve deeper understanding of how OTs, with expertise in habit formation and environment, contribute to prevention and management of chronic diseases, which are vital aspects of health promotion. There is opportunity to work with the AACs, the healthcare clusters and other organizations in the community to achieve this.
Limitations and future research
The study’s qualitative design provided rich insights and transferability but limits generalizability. Another limitation is potential social desirability bias as some participants may have responded in an overly positive manner as this is a new model of care. They may have downplayed the negative aspects of the model. Another limitation is potential researcher bias as her interpretation and perspectives as a senior OT in the field can influence the data collection and analysis process.
More research is needed on the perspectives of healthcare and community care professionals including hospital-based OTs, community nurses and general practitioners, as well as older adults themselves on the place-based model of care. Future research could also investigate the feasibility of implementing the place-based OT model in some AACs and the scalability to all AACs in Singapore. Additionally, the right sitting of cost-effectiveness models for place-based OT need investigation.
Conclusion
This study provides valuable insights into the potential of place-based OT to support ageing-in-place. The findings suggest that place-based OT can address gaps in current community rehabilitation services, optimize service delivery through neighbourhood-based care, and leverage on AACs to enhance social connectivity for older adults. The perceived advantages, envisioned service model, and identification of enablers provide a foundation for further development and implementation. One lesson learnt is that place-based OT services will likely look slightly different in each country, as the service focus on the unique health and social needs of the residents in the neighbourhoods, and evolves around the current service offerings in the community. Due to OT’s unique focus on the interaction between person, environment and task, a place-based model of care offers a good and effective compliment to OT services.
Footnotes
Acknowledgements
The author would like to thank the participants for participating in the study.
Ethical Consideration
Institutional Review Board (IRB) approval was granted from the Singapore University of Social Sciences {2023-GER 688-01 (001)} for this research project.
Consent to participate
Informed consent to participate was written. All participants have consented and signed the informed consent form.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The research was supported by the Tan Tock Seng Hospital Occupational Therapy Enabling Fund; 2023-001.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The data generated during and/or analyzed during the current study are not publicly available due to confidentiality and privacy of the participants.
Note
Appendix
Themes, Illustrative Quotes and Implications for Practice
Theme
Illustrative quotes
Implications for practice for place-based OT services
Maintaining health and function of older adults
‘I think place-based OT service is a stop gap thing, something to bridge between a more permanent service like AAC. Yeah. So, for example, like if the clients going to be discharged or somewhere else and the waiting time is too long. Then this service is there to really make sure that client don’t decline. They really continue to improve as much as they can while waiting to go to somewhere permanent.” (P002)
This is what we are doing with our community partner, Tan Tock Seng Community Health Team. So we discharge some of our better clients to them and say, “Yeah, anything if you need to refer the client back, just refer back, we are happy to take the client back.” Yeah, because we can’t follow up with them once they are discharged from our DRC. (P007)
Place-based OT services will work with clients who are in transition (discharged from acute or DRCs) to prevent deterioration of health and function through providing short-term, just-in-time interventions e.g. reviewing assistive equipment as functional status changes
Partnering caregivers to provide seamless and coordinated care
“Some of them don’t even know what services are out there even though they are educated. So besides looking at the clients, we also look at the caregivers, what are their needs. If they are very stressed out, we will tell them about services nearby, are you keen to try. We help them to navigate the healthcare system” (P002)
“Instead of having to be referred to the medical social worker (MSW) to enquire about community resources, a knowledgeable place-based OT can help caregivers navigate the landscape. The MSW’s time can be conserved to manage financially and socially complex cases.” (P004)
“So not only doing just OT work, but also help caregivers to know what is available in the community be it psychosocial support, financial support or even home-based support, whatever service they need.” (P006)
“Some caregivers don’t know what services are out there even though they are educated. So besides looking at the client, we also look at the caregivers, what are their needs. If they are very stressed out, we will tell them about services nearby, are you keen to try. We help them to navigate the healthcare system.” (P002)
“Once in a while, we need to educate caregivers on how to evaluate websites. To see whether is it really you can trust one? Or is the website trying to sell something to you. Why do you want to believe them?” (P003)
Place-based OT will work with caregivers including signposting and guiding them to navigate the healthcare and community care systems to obtain the care that their loved ones need
Place-based OT services are ideally located within neighborhoods, proximal to residents’ homes
“It makes sense from a patient perspective as well, because when they come to us, it’s not so logistically challenging. And if they are actually able to walk to us. Take a feeder bus. It reduces barriers to entry.” (P005)
“So sometimes we have 0830 slot. But the family will tell you. Oh, 0830 is too early. We cannot get ready but that is the only available slot for transport. So if let’s say, they cannot take that slot right, they might be put on the wait list. So if they prefer 2 pm therapy slots. Then we have to let them wait until another client coming at 2 pm discharges, then we can give them the slot. So there is a delay in rehabilitation, if they have to wait for certain things to be in place for them to come.” (P004)
“Most of the clients stay in HDB. So if they can just push downstairs across the road to get the service within 5 to 10 min it will be good. So the proximity does matter.” (P006)
Place-based OT services should be availed to residents staying in surrounding blocks within a geographical boundary, to enable easy access to residents’ homes and neighborhood environments
Understanding clients’ routines, habits, everyday activities, and environment strengthens the impact of therapy
“I think the level of complexities is reduced, the reach is more and because of the familiarity the person or the practitioner has with the environment, the recommendations are a bit more specific.” (P005)
“Then we will also see where are points the clients gather like void deck, those chairs. We will just go by and say hello to the people there and then sometimes from there, we get to know more information. Or, if we see the client, we will say, “Hey, Aunty, how come today you are not walking so well. Do you want to come in for rehab or not?” (P002)
“Then you can actually see where the clients stay, where they usually go. Where they get their kopi, how they buy their food. If they use the motorized scooter, where do they go. I mean, it’s easier and better also. Cos we can better understand the environment. Why here got a barricade? Where are you going to drive your scooter and all? Cos they don’t realize cos they have been walking all these while. But they walk stop, walk stop. Then suddenly they realize got all these barriers.” (P007)
“If you are there in Chinatown, and you know that everyone is like, stay alone that type. You know that what you need to do is very different. You can’t just go in and do your home visits, you may need to work with community partners to clear the hoarding, clean the place up etc.
If I go to Shunfu, all very well off one, got helper one, don’t need transport one. They all get driven to our center that type. Then the whole approach would be very different. So might be going to all the landed houses and all. Place-based OT needs to know how to navigate all these.” (P002)
“Compared to you know, I have to go to a hospital. I have to make an appointment which is very tech based. I have to reply a SMS. If I have to change my appointment, I have to send the SMS. Press 1 or 2. Most seniors don’t know how to do that. But in a smaller place-based setting, its literally when they just come in. Okay, Uncle, you want another appointment. I have another slot at 1030. Let me just write it out for you. Give to your helper.” (P005)
“Peer support is very crucial, because sometimes as an outsider or professional, when I say “you must not wear slippers, you can fall down”. Then we say already, they also, like one ear in, one ear out. But then, if it’s a friend or neighbor who tells them, “Please lah, don’t wear this, not good, I fall down before”. Then I don’t even need to say anything. Automatically, it just convinced. Yeah. So I think, having that is quite useful.” (P002)
Place-based OT services should be availed to residents staying in surrounding blocks within a geographical boundary, to enable easy access to residents’ homes and neighborhood environments
Facilitate older adults to develop meaningful social connections and maintain cognitive wellness
“The place-based OT can advise and even train the staff in AAC to create some activities to meet the needs of residents like social, cognitive, even physical needs.” (P001)
“Currently, activities offered in the AAC might not interest the clients. However, there’s not much choices given to them. Let’s say, the group activity is a coloring class. So most of them sit there and color, but some of them, who have never done coloring before, and suddenly, you just want to engage them But the activity may not be enough to stimulate them cognitively so they get dis-engaged. So I feel that AAC staff will benefit from OT training them on choosing of and grading suitable group activities.” (P004)
“I also tried to do groundwork. I went to do door knocking. You were able to see from outside whether like this this case, need or not. Yeah. But then the thing is like, I think the good thing about me being a OT versus layman is. I know what to look out for compared to my AAC colleagues. So many things that I can pick up but they couldn’t. and if I never go home visiting, then this thing will not be picked up. Unless they come and discuss case with me.” (P006)Place-based OTs can give inputs to AAC’s menu of programs to meet residents’ social, cognitive and physical needs and train AAC staff to plan the activities
Reducing out-of-pocket payment increases access to place-based OT services
“Another thing is the funding and also whether it is subsidized. of course our residents will all go for the subsidized services.” (P001)
“From the end user perspective, like, are they willing to pay for it? Yeah, because somehow, or rather, someone has to pay for, and I think I don’t think it’ll be infinite, like MOH will just keep funding it fully.” (P003)
“Also, the subvention part shouldn’t be too complicated. Will be helpful if clients can just show CHAS card or PG/MG cards etc. Otherwise you have to hire an Exec to do all the back end work which also increases the cost of the service.” (P004)
Conduct proof-of-concept trials at low cost or no cost for place-based OT to gauge acceptance of concept by older adults and collect data. For sustainability, it is essential to convince funders such as MOH, AIC or healthcare clusters (through capitation funding) of the value that place-based OT brings, using the data collected from the trials
Place-based OTs need clinical, contextual and program management capabilities
“Because of the nature of place-based OT, it might be hard for someone who is fresh from uni to get the supervision and training that they need.” (P003)
“For OTs who have at least passed their conditional registration and they wish to venture into place-based OT, as long as they are being closely supervised by a very senior person who is able to do it, it is still possible. We can explore a triaging kind of model. If I’m placing OT in a particular area of Singapore, then probably I have like 10 of them. The 10 of them will do their own screening. But if they have any issues, they will raise it up to a senior who provide ad-hoc coverage, but most of the time really just managing to ensure the right-siting of care of the clients seen by the place-based OTs in their various stations. So this person will do case discussions with the younger therapists and probably helping to manage the more complex cases. I think it is not cost effective to wait for OTs to gain the enough level of experience, looking at the needs of the older adults in Singapore.” (P003)
“OT training has focused more on function and medical aspects. It’s good for the community OT to know about the importance of social aspect. When we train, we are looking more at the client’s function more medically. Yeah. So after I work in the community then, I understand. Actually, the social aspect has a big influence on the health of residents.” (P001)
“Even when I hit the first within the first decade of my profession, I may not get very much involved in costing per se. But as I go beyond that sheer number of years, I always have to bear in mind about the cost effectiveness of the plans or the program that I’m implementing.” (P003)
“Probably some program management knowledge so that at least we can evaluate our program for funder that we are seeking support from.” (P001)
To keep place- based OT service cost-effective, an OT headcount will likely be shared across a few place-based OT service locations, with support staff being upskilled to help. As such, the place-based OT should be able to practice independently, having experience in treating clients with a wide range of health conditions and being familiar with community resources. Thus, place-based OT should be fully registered OTs with experience in both acute and community care
Hospitals’ endorsement engender trust between clients and place-based OT services
“The trust that patients have in the upstream and downstream quality of care needs to be more seamless and improve.” (P005)
“The healthcare professionals in the hospital must be able to say, We’re gonna transit you to this to these guys. They are legit. Then that’s the sort of trust. I think what’s happening now is people still are a bit hesitant, or there’s this difference in expectation of the quality of care in the hospital and in the community. So sometimes they may say, Hey, you know, I just want to go back to the hospital. I don’t want to come down to community. Unless I really have to. Because the quality of care is better, I would rather, you know, stick with these guys. Yeah. So the perceived quality of care to me is really important. So the handshake between the community partners and the hospital has to be really tight. And I guess the trust that the clients would have in place-based practitioners starts upstream, because currently. It is still in the minds of our client base. Still, very hospital centric.” (P005)
Another participant shared that families prefer their loved ones to be seen in hospital outpatient services as they do not have to pass messages between healthcare teams
“Families sometimes prefer to send the clients to the outpatient in the hospital, because they prefer to have the entire team in the hospital to manage the client, rather than like oh, in in nursing home. Then they need to like, communicate with the specialists in the hospital.” (P001)
To build trust with partners including hospitals, place-based OT services need to establish effective systems of working together with the collaborating organizations. There can be regular case conferences to discuss challenging cases, and established ways to communicate with one another on client care
