Abstract
Introduction
Sensory Modulation Interventions (SMI) assist people with mental illnesses to regulate emotional and physiological arousal. We aimed to conduct a scoping review to identify the study designs, geographical distribution, modality/regimen, barriers and facilitators in using SMI for individuals with mental illnesses.
Methods
A systematic search was conducted using Arksey and O'Malley’s framework with studies published on SMI from January 2010 to November 2020.
Results
17 articles were found to be relevant. One was a case-control study, qualitative (N = 3), mixed-method (N = 3), and case studies (N = 3), and the rest were pilot interventional studies (N = 8). The duration of sessions ranged from 2 to 30 minutes for 2 days to 3 years. The facilitators in using SMI were of being cost-effective and easily adaptable. Barriers were in terms of maintenance of sensory items. Sensory modulation based items related to proprioception, vestibular and tactile were the frequently used in the SMI based interventions used in the included studies.
Conclusions
SMI as an occupational therapy intervention for individuals with mental illnesses is evolving and more robust studies in the future are recommended.
Keywords
Introduction
Maladjustments in the psychological, biological, or developmental processes of an individual’s mental functioning that is characterized by disturbances in their emotions, thoughts, or behavior, is termed as mental illness which consists of a wide range of symptoms and problems, that may lead to issues with self-care, education, work, social, and family activities (American Psychiatric Association, 2019). Mental disorders have graduation in gravity, from absence to critical psychopathology; but are not inflexible phenomena. Some examples of mental illnesses are depression, schizophrenia, intellectual disabilities, and disorders related to substance abuse (World Health Organization, 2019).
Mental illnesses affect education and income levels, and it is seen in all cultures. The global economic and societal burden of mental health disorders is rising at a startling rate (Gmitroski et al., 2018). Moreover, the burden of mental illness and addictions is said to be larger than the burden of illness for other medical conditions, such as cancer and infectious diseases (Ratnasingham et al., 2013). Improving the occupational participation of individuals with mental illnesses may aid in reducing this burden of mental illness as a contribution to the society (Lannigan & Susan Noyes, 2019; Lipskaya-Velikovsky et al., 2015).
Sensory Modulation is the neurological ability of the central nervous system to regulate the sensory stimulus received from the environment that provides an opportunity for a behavioral response to that stimulus (Brown et al., 2019). According to Dunn’s model of sensory processing (Dunn, 2001), people with low registration do not notice sensory events in daily life that are immediately noticed by most people because they have high thresholds and passive response strategies. In contrast, people with sensory sensitivity notice much more sensory stimuli than most people and get easily distracted because they have low thresholds and passive response strategies. Sensory seekers actively use strategies to look for sensory input, while the sensory avoiders actively limit sensory-input (Sharfi & Rosenblum, 2015).
Studies have shown that persons with bipolar face low registration, sensory sensitivity, and sensory avoidance problems (Engel-Yeger et al., 2016). Additionally, people with mental disorders such as schizophrenia experience sensory modulation disorders with an under responsiveness, which in turn may influence the participation dimensions, thus affecting mental health (Lipskaya-Velikovsky et al., 2015). There are two concepts when referring to the term sensory modulation. One refers to physiological sensory modulation, which is the neurophysiological reaction that alters cellular mechanisms for habituation and sensitization. The second refers to the behavioral sensory modulation, which is the ability to appropriately regulate and organize sensory responses (Brown et al., 2019).
Individuals with significant mental illness have distinct sensory processing patterns in contrast to the general population and the evaluation of these sensory processing patterns in adults with significant mental illness can inform sensory-based treatment (Pfeiffer et al., 2014). The sensory based interventions aim at all seven senses: visual, tactile, gustatory, auditory, olfactory, vestibular systems, and proprioceptive (Machingura et al., 2018). Interventions that are based on sensory modulation could assist individuals to regulate emotional and physiological arousal. Sensory Modulation Intervention (SMI) has been highlighted as a non-invasive, self-directed, and empowering intervention that may support recovery and inform mental health practice (Scanlan & Novak, 2015). When people with mental illnesses are provided with SMIs that are nurturing such as gliding in a glider rocker while wrapped in a weighted blanket, it provides them the required sensorimotor opportunities to function adequately in their daily lives. The application of sensory modulation strategies has been proven to be helpful and supportive of functional performance, thus occupational therapists use SMI to help individuals to self-regulate through the process of self-organization and positive change (Champagne, 2011).
SMIs comprise of activities and modalities which are designed to facilitate specific types as well as amounts of sensation, at a given time, for therapeutic purposes (Machingura et al., 2018). When implementing a sensory modulation approach in mental healthcare facilities, there is a significant effect on the reduction of seclusion and restraints (Andersen et al., 2017). SMIs can help individuals to develop appropriate behavioral responses by enabling the processing of sensory information and facilitating effective occupational participation (Machingura et al., 2018).
When individuals encounter mental health crises, there could be increased levels of stress, cognitive, perceptual changes, and emotional distress, which might result in hyper or hyposensitivity to various sensory inputs (Bar-Shalita, et al., 2012). By altering the environment and using soothing stimulus, we can attain moderate or suitable arousal. It enhances the ability to adapt and regulate emotions (Machingura et al., 2018). Perceived unpleasantness due to various experiences and coping mechanisms tends to impact the lives of individuals in terms of time, thought, effort, and choices concerning social activities (Pfeiffer & Kinnealey, 2003). There is a relationship between sensory defensiveness and anxiety, and by following an intervention that is designed for individuals with sensory modulation disorder, both sensory defensiveness and anxiety could drastically decrease (Machingura et al., 2018). So, SMIs could impact sensory defensiveness and anxiety and assist individuals to improve their productivity and the quality of life (Pfeiffer & Kinnealey, 2003). By appropriately using sensory modulation strategies, we could provide experiential and alternative opportunities for de-escalation, empowerment, choice, increasing awareness, and skill development (Reed, 2017). An example of a SMI is a sensory room. A sensory room could help calm and alert the senses. A sensory room program aims to facilitate an environment for client-centered practice to provide opportunities for exploring self-regulation of emotions and acquisition of new coping skills to prevent or de-escalate aggressive behaviors. A sensory room is designed for goals that focus on de-escalation or prevention (Reed, 2017).
Since SMIs for adults with mental illness is evolving, a scoping review is the research method of choice at this point in time to map the existing literature in this field to inform further advance. Earlier review by Machingura et al., (2018) has mapped the literature on use of sensory modulations on adults with only schizophrenia. Since recently there has been an increased interest in the area of sensory modulation for persons with mental illness there are possibilities of having further studies after the last review done by Scanlan and Novak (2015). Hence, the current review will serve to recognize the recent advancement in the domain of SMIs for adults with mental illnesses. This will assist in identifying the application of related strategies in the occupational therapy clinical practice, and to further advance the research in this area.
We generated the following exploratory research question that will allow us to broaden our search. What is the available literature on the occupational therapy based sensory modulation interventions for adults with mental illness? On this basis, we formulated the objectives that include studying the existing literature on the sensory modulation interventions for adults with mental illnesses by identifying the range of study designs used, the geographical distribution, the modality/regimen used in studies related to the sensory modulation interventions for adults with mental illness and also to recognize the barriers and facilitators of utilizing the sensory modulation interventions for mental illness.
Methods
Search strategy
A scoping review is a method of mapping the core theories and concepts of a research area and synthesizing all possible evidence from both published and grey literature, through a broad search (Arksey & O’Malley, 2005; Levac et al., 2010; Munn et al., 2018). A scoping review helps in identifying and organizing the fundamental concepts, sources, and types of evidence available, which informs practice in the research area. It also helps in recognizing and analyzing knowledge gaps, identify the value, potential, and cost of executing a full systematic review, and in compiling and disseminating research findings (Arksey & O’Malley, 2005; Levac et al., 2010; Munn et al., 2018).
Arksey and O`Malley`s (Arksey & O’Malley, 2005) framework for scoping reviews was used in the current review to identify the extent of research done in the domain of SMI for adults with mental illnesses (Figure 1). The following databases were chosen for the review -PubMed/MEDLINE, CINAHL Complete, Scopus, Web of Science, Sage Journals, ProQuest, Springer Link, and OT Seeker as these are the databases in which majority of the occupational therapy research is published. The keywords for population (mentally ill OR mental illness OR psychiatric illness) and intervention (sensory modulation OR sensory integration OR sensory based) were combined with Boolean operators for the literature search. The search was conducted in the month of September 2020. PRISMA Flow Chart.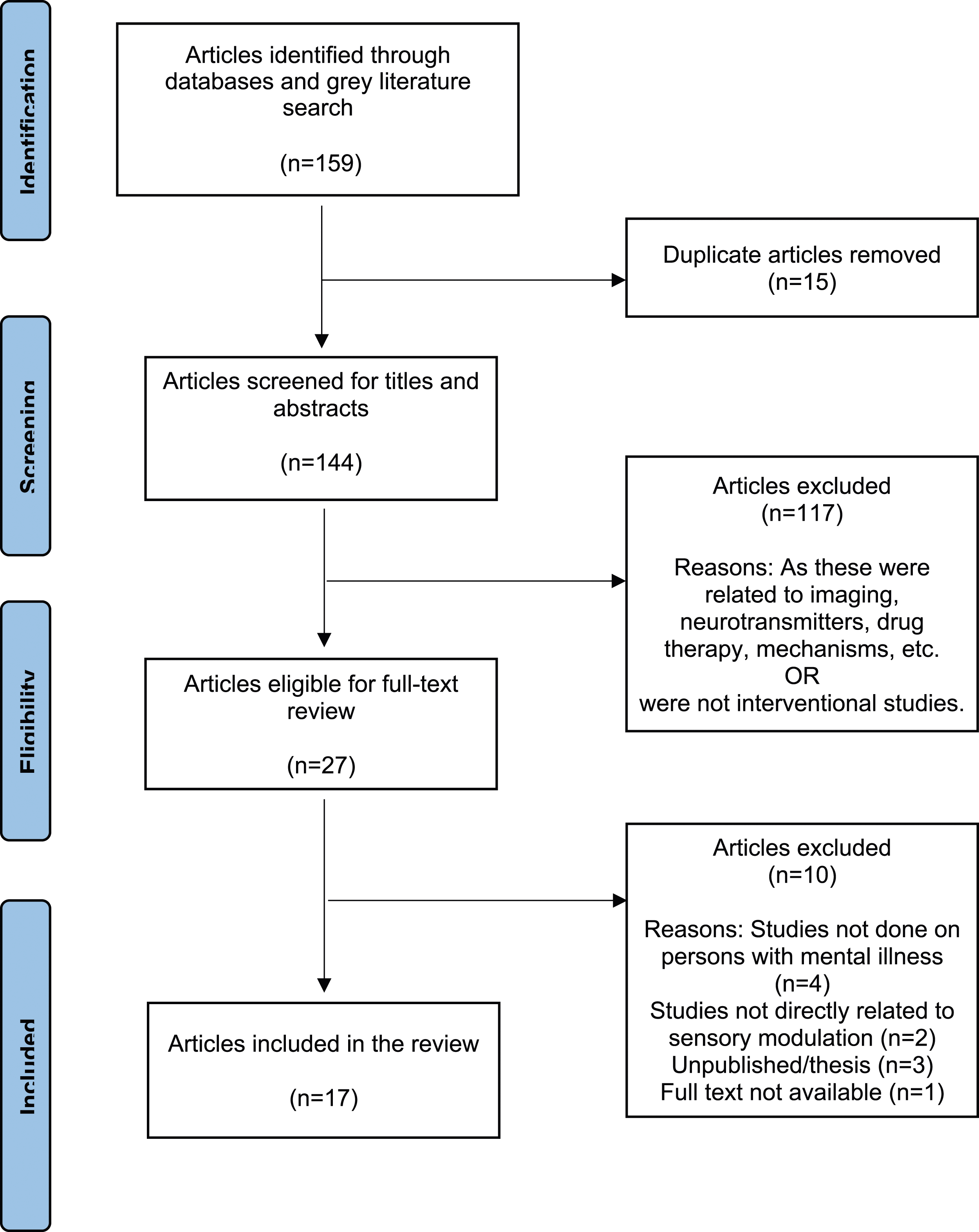
Study selection criteria
A total of 159 articles were obtained from the included databases by the first four authors. After removing the duplicate articles, a total of 144 articles remained. The titles and abstracts of the retrieved articles were screened by the first four authors (NK, SJ, AF, SR) independently, out of which 117 articles were excluded for reasons being that the studies were either related to imaging, neurotransmitters, drug therapy, neuro mechanisms, were observational studies or were not interventional studies. If any discrepancy existed between the reviewers, the fifth author (SQ) was consulted and final decision was taken (Figure 1). The obtained 27 articles were reviewed full text and finally a total of 17 full text articles were included based on the following inclusion criteria: (i) Articles available in full-text and published in English, from January 2010 to September 2020 so as to identify the recent research done in the field of SMI (ii) studies done on adult mental illnesses as defined in the Diagnostic and Statistical Manual of Mental Disorders, fifth edition (DSM-5) and International Statistical Classification of Diseases and Related Health Problem, 10th version (ICD-10), (iii) studies on adults of ages 18+ years, (iv) SM interventional studies including qualitative studies. Exclusion criteria were as follows: (i) SMI studies conducted on the pediatric population, (ii) studies done on SMI for adults with attention deficit hyperactivity disorder (ADHD), autism spectrum disorder (ASD), and neuropsychiatric conditions like dementia, TBI, etc., (iii) studies on hearing, vision, or similar sensory impairments and, (iv) letters to the editor, correspondence, editorials, fact sheets, and viewpoints on SMI. Studies done on persons with ASD and ADHD were excluded in the current review as the focus of the current review was to identify literature on use of SMIs only in mental illnesses or psychiatric conditions. The obtained final 17 articles were reviewed by all the authors and the data was charted and collated.
Results
Description of the included studies
Data Chart of the Included Studies.
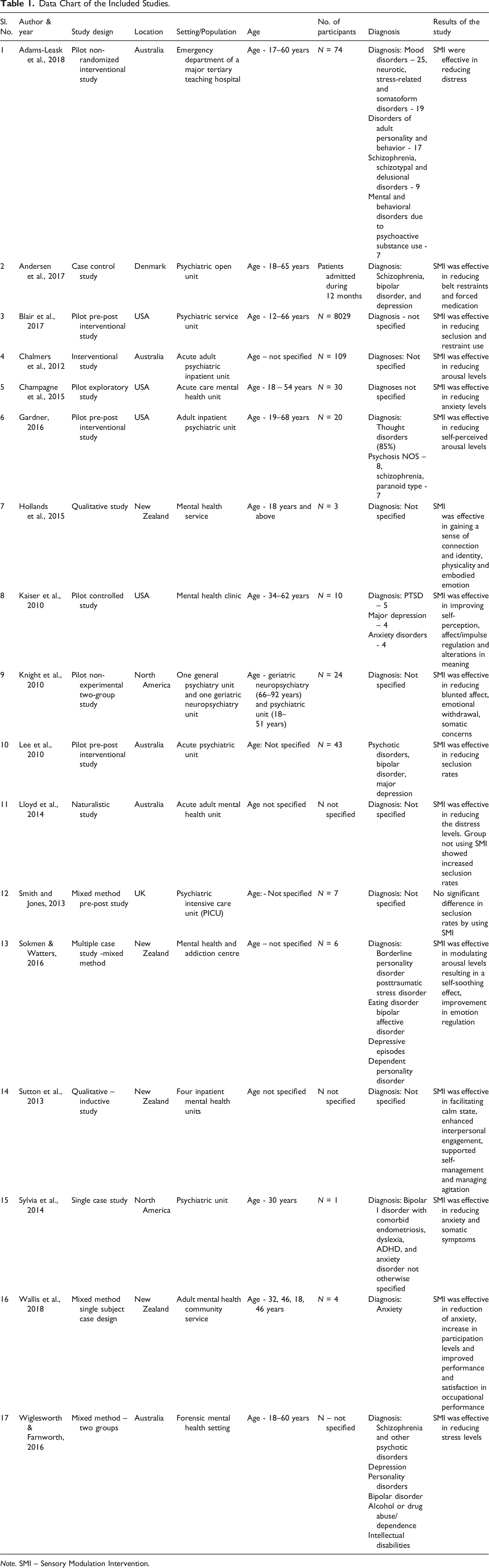
Note. SMI – Sensory Modulation Intervention.
Out of the 17 studies included, 6 each were from North America (Blair et al., 2017; Champagne et al., 2015; Gardner, 2016; Kaiser et al., 2010; Knight et al., 2010; Sylvia et al., 2014) and European continent (Andersen et al., 2017; Hollands et al., 2015; Smith & Jones, 2013; Sokmen & Watters, 2016; Sutton et al., 2013; Wallis et al., 2018) and 5 were from Australian continent (Adams-Leask et al., 2018; Chalmers et al., 2012; Lee, Cox, Whitecross, Williams, & Hollander, 2010; Lloyd et al., 2014; Wiglesworth & Farnworth, 2016).
Only one study was a case control study (Andersen et al., 2017) with the rest being either pilot pre-post interventional (Adams-Leask et al., 2018; Blair et al., 2017; Chalmers et al., 2012; Champagne et al., 2015; Gardner, 2016; Kaiser et al., 2010; Knight et al., 2010; Lee et al., 2010), qualitative (Hollands et al., 2015; Lloyd et al., 2014; Sutton et al., 2013), mixed method studies (Smith & Jones, 2013; Sokmen & Watters, 2016; Wallis et al., 2018; Wiglesworth & Farnworth, 2016) or single case study (Sylvia et al., 2014).
Out of the 17 studies reviewed, only one study reported of no specific effects of SMI (Smith & Jones, 2013). The other studies reviewed identified the effect of SMI on improved arousal levels (Chalmers et al., 2012; Gardner, 2016; Sokmen & Watters, 2016), reduced anxiety (Champagne et al., 2015; Sylvia et al., 2014; Wallis et al., 2018), stress (Wiglesworth & Farnworth, 2016), distress (Adams-Leask et al., 2018; Lloyd et al., 2014), agitation (Sutton et al., 2013) and somatic concerns (Knight et al., 2010; Sylvia et al., 2014). SMI was found to induce a self-soothing effect (Sokmen & Watters, 2016; Sutton et al., 2013), helped in better self-perception (Hollands et al., 2015; Kaiser et al., 2010), emotional regulation (Hollands et al., 2015; Kaiser et al., 2010; Knight et al., 2010; Sokmen & Watters, 2016), self-management and interpersonal engagement (Sutton et al., 2013). Also, SMI was found to be beneficial in reducing forced medication intake (Andersen et al., 2017) and improved occupational performance (Wallis et al., 2018).
Age and diagnosis of the participants
The age of the participants in the included studies ranged from 18–92 years. The diagnosis of the participants included in the studies were mood disorder (Adams-Leask et al., 2018; Andersen et al., 2017; Lee et al., 2010; Sokmen & Watters, 2016; Sylvia et al., 2014; Wiglesworth & Farnworth, 2016), neurotic and stress related disorder (Adams-Leask et al., 2018; Kaiser et al., 2010; Sokmen & Watters, 2016; Wallis et al., 2018), personality disorder (Adams-Leask et al., 2018; Sokmen & Watters, 2016; Wiglesworth & Farnworth, 2016), schizophrenia (Adams-Leask et al., 2018; Andersen et al., 2017; Gardner, 2016; Wiglesworth & Farnworth, 2016), substance use disorder (Adams-Leask et al., 2018; Wiglesworth & Farnworth, 2016), depression (Andersen et al., 2017; Kaiser et al., 2010; Lee et al., 2010; Sokmen & Watters, 2016; Wiglesworth & Farnworth, 2016), specifically thought disorder (Gardner, 2016), and psychosis (Gardner, 2016; Lee et al., 2010).
Facilitators and barriers in using sensory modulation interventions
Details of SMI Used.
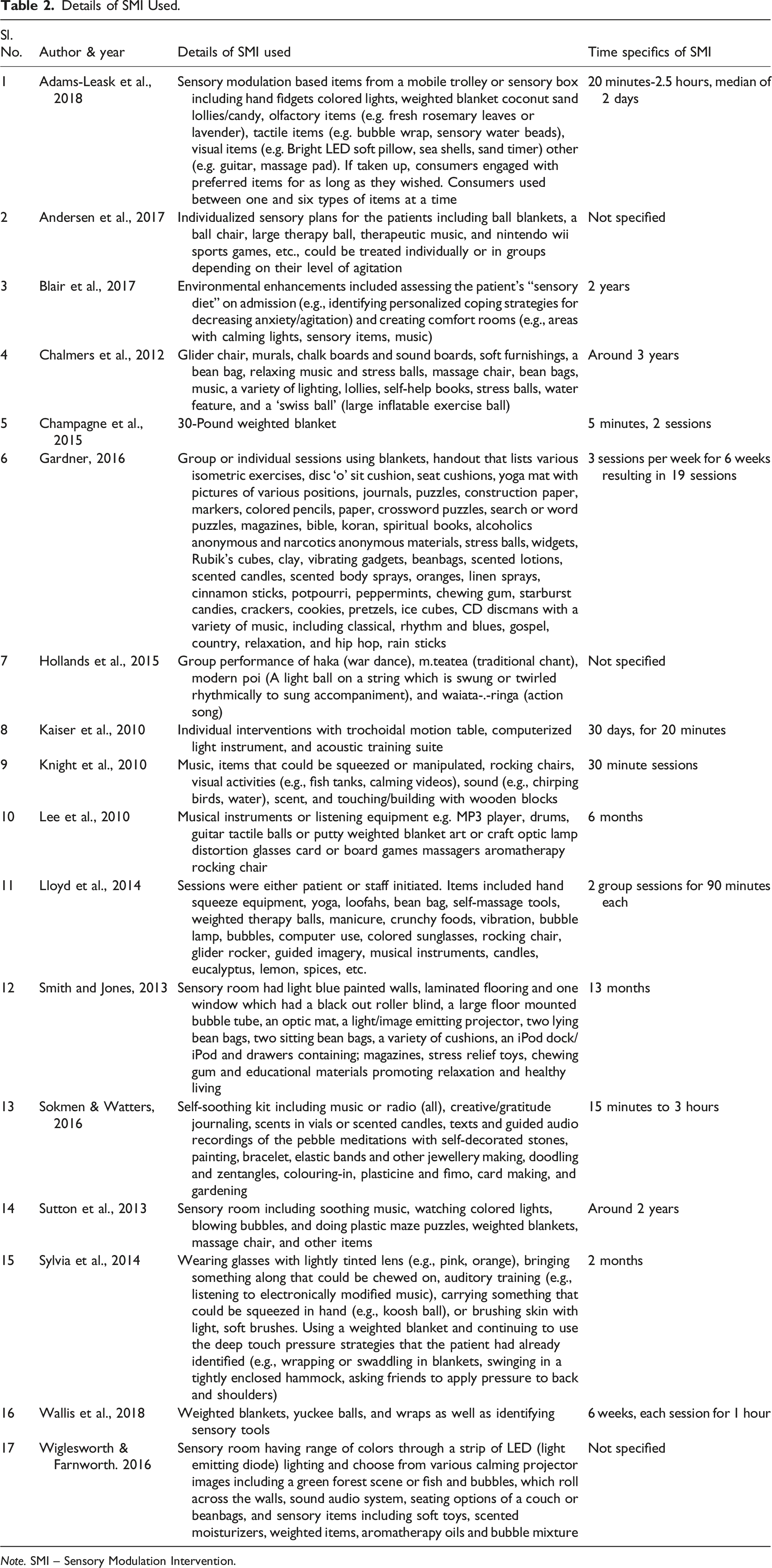
Note. SMI – Sensory Modulation Intervention.
Discussion
The purpose of this scoping review was to map the extent of research done in the field of SMI for individuals with mental illnesses.
The current scoping review identified 17 studies that have used SMI on individuals with mental illness with around 13 articles published during 2013 through 2018. The literature on SMIs is at an early stage (Machingura et al., 2018). This increasing trend of studies identified in the current scoping review signifies the increasing interest in the area of sensory modulation in mental illnesses.
Most studies being pilot studies showed that there is an interest in studying and applying the sensory modulation approach in mental health settings. Having only one case control study shows that there is lack of higher-level research with respect to the SMIs for individuals with mental illnesses (Andersen et al., 2017). However, the results also indicate a potential for conducting higher-level research with sensory modulation approach. There is an evolution seen in outcomes measured from earlier studies to the current studies. Earlier studies have focused more on effects of sensory modulation interventions on distress levels (Novak, Scanlan, McCaul, MacDonald, & Clarke, 2015), the recent study showed improvement in occupation such as public transportation on use of sensory strategies (Wallis et al., 2018). This highlights the role of occupational therapy in improving the functional outcomes using SMI.
SMIs involved items related to visual, auditory, gustatory, olfactory, proprioception and vestibular sensations. The duration of sessions provided ranged from 2 to 30 min for 2 days to 3 years. The ambiguity in the protocol followed could be due to the client centered nature of the SMIs. Developing a protocol for implementation of SMI for persons with various mental illnesses could be beneficial in implementation of SMI in various mental health settings. This would also aid in gauging the effectiveness of the SMI in better possible ways such as through studies with higher rigor.
The facilitators for the use of SMI seem to outweigh the limitations and these interventions fit the client centered practice of occupational therapy (Sumsion & Law, 2006). The therapist will have to assess the sensory profile of the patient to provide the optimal range of sensory items for the person with mental illness to choose from. The aspect of choice in acute settings where seclusion and/or restraint might be used seems very powerful in maintaining the individual`s self-esteem, individual identity and autonomy. The SMIs also support the recovery model (Jacobson & Greenley, 2015) that highlights the shift of treatment to increased participation of individuals with mental illness in day to day occupations rather than only symptoms. Moreover, the choice of equipment used during interventions is made by the person with the mental illness by which the individual may feel empowered because of active participation and involvement in the interventions given. Nevertheless, the SMIs are easily adaptable because of which these interventions could be practiced even in the community. Use of SMIs could be a better alternative worthy trying out for persons with mental illnesses before moving on to physical restraints (Moghadam et al., 2014).
Limitations
Only published literature in English was searched in the current review, which may have resulted in missing relevant studies. The reviewers have tried all possible ways to look for relevant articles but individual biases of the authors may not be negated. The current review may help future researchers to conduct relevant research related to gaps identified in the current review. Most of the studies identified in the current scoping review have found that there is a positive effect of SMIs in treatment of mental illnesses. But, there is the risk of bias that invites us to be cautious when interpreting these results. Future studies may focus on evaluating the effectiveness of sensory modulation interventions specifically on various occupations such as activities of daily living, instrumental activities of daily living, social participation, sleep and rest, education and leisure participation for various conditions in mental illness. Also, studies could be done in developing guidelines in terms of duration and the type of modalities that could be used for persons with different mental illnesses based on their sensory profile.
Conclusion
The current review aimed at mapping the existing literature on sensory modulation interventions for adults with mental illnesses. Based on the identified studies it can be concluded that sensory modulation interventions have the potential in reducing distress levels, and modulating the arousal levels thereby improving the occupational participation of adults with mental illnesses. Moreover, this review would help clinicians in implementing evidence-based decisions in using sensory modulation interventions to treat adults with mental illnesses. Future research should focus on evaluating the effectiveness of sensory modulation interventions in various types of mental illnesses using more randomized controlled trials and longitudinal studies to identify if sensory modulation interventions can bring about a change in sensory modulation in adults with mental illnesses.
Footnotes
Acknowledgements
The authors like to acknowledge Ms. Deena Dimple Dsouza and Mr. Shashank Mehrotra for their assistance in drafting the manuscript.
Author’s contributions
Ms. Nayantara R. Kandlur, Ms. Ashmica Claire Fernandes, Ms. Suzanna Rupal Gerard, Ms. Shruthi Rajiv and Ms. Shalini Quadros contributed at the initial proposal stage. Ms. Nayantara R. Kandlur, Ms. Ashmica Claire Fernandes, Ms. Suzanna Rupal Gerard, Ms. Shruthi Rajiv conducted the initial search under the guidance from Ms. Shalini Quadros. All the authors contributed towards drafting of the manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
