Abstract
Background and objective
Pulmonary rehabilitation programme (PRP) is an important component in the management of chronic obstructive pulmonary disease (COPD). However, to date so far there has been limited literature on the survival outcomes of patients with COPD after a PRP in Hong Kong. This study aimed to investigate the outcomes of a pulmonary rehabilitation programme on the survival rates of a retrospective cohort of patients with COPD.
Methods
This was a retrospective study that included subjects who participated in the PRP in a rehabilitation hospital from the year 2003 to 2015. A total of 431 patients with chronic obstructive pulmonary disease were identified from the electronic record system of the hospital. The dataset were split into two age groups for reporting and analysis using the mean age of 72 as the cut-off. Their median survival times were calculated using Kaplan–Meier analysis. Cox-proportional regression model was used to explore factors that predicted better survival. The most significant predictors were used as strata, and their respective effects on survival functions were analysed with Kaplan–Meier analysis again.
Results
The overall median survival of the cohort was 4.3 years. The median survival times of the younger patient group (aged <72) and the older patient group (aged ≥72) were 5.3 and 3.6 years, respectively. For the patients, aged <72 years old, Moser’s Activities of Daily Living class and the pulmonary rehabilitation programme completion rate were the most significant survival predictors. For the patients aged ≥72 years old, Monitored Functional Task Evaluation score was the most significant survival predictor.
Conclusion
Moser’s Activities of Daily Living class ≥2 and non-completion of PRP for younger group, low exercise capacity with Monitored Functional Task Evaluation score <17 for older group were identified as significant predictors of poor survival. The findings of this study helped identifying those patients with COPD who have the needs to be more intensively treated and closely monitored.
Keywords
Introduction
Pulmonary rehabilitation programme (PRP) is an important component in the management of chronic obstructive pulmonary disease (COPD). It is a comprehensive, patient-tailored intervention that includes exercise training, education, and self-management (Spruit, Singh, & Garvey, 2013). This non-pharmacologic intervention is known to have benefits including improvement in exercise performance, reduction in symptoms, and lessening healthcare utilisation (Global Strategy for the Diagnosis, Management and Prevention of COPD, 2017; Ko et al., 2011; Puhan, Gimeno-Santos, Cates, & Troosters, 2016; Spruit et al., 2013). However, the effect of PRP on the survival of patients with COPD was not fully investigated and reported.
The three-year survival rates of patients with COPD after PRP were reported to be 69–85% (Bowen et al., 2000; Daughton, James, Kass, & Patil, 1984). Some researchers reported that the following factors were associated with better survival: (a) completion of the whole course of PRP (Houchen-Wolloff et al., 2018), (b) greater improvement in exercise capacity and function on completion of the PRP (Bowen et al., 2000), and (c) those patients who were less dyspneic at baseline as well as on completion of the PRP (Nishimura, Izumi, Tsukino, & Oga, 2002). On the other hand, some researchers reported that the following factors were associated with mortality: lung cancer as co-morbidity, suffering from chronic respiratory failure and receiving noninvasive ventilation, and having more number of severe exacerbations with hospitalisation (Saraiva, Abreu, Neves, & Rodrigues, 2016). In views of the advancement in PRP in the past decades in the following aspects, such as putting more emphasis on collaborated self-management with pulmonary rehabilitation (e.g. integrating more psychological and behavioural strategies to reinforce smoking cessation, use of rescue pack for management of early exacerbations, etc.), recruitment of case manager to support self-management among individual patients, and extending the duration of PRP and/or incorporating a maintenance phase of PRP, there were good reasons to believe that PRP definitely plays a role in disease modification and mortality (Cosgrove, Macmahon, Bourbeau, Bradley, & O'Neill, 2013; Simpson & Jones, 2013; Zwerink et al., 2014). Therefore, there were two objectives for this study. First, it aimed to investigate the outcomes of PRP on the survival rates of patients with COPD based on a retrospective cohort of patients who had already completed the PRP in the local context. Second, it explored related survival predictors which might be useful to guide healthcare practitioners for better patient management.
Methodology
Participants and sampling
This was a 12-year retrospective longitudinal study for a group of patients with COPD who participated in the PRP in Kowloon Hospital during 2003–2015. In this setting, PRP was carried out in the form of a day-hospital on weekly basis with a total duration of 12–20 weeks. Respiratory Specialists, Nurses, Occupational Therapists, and Physiotherapists were members in the PRP team. The programme content included inhaler education, exercise, health qigong, activities of daily living (ADL) training, self-management, home oxygen prescription and monitoring, and medical consultation if indicated. Multidisciplinary case conferences were held monthly to monitor individual patient’s rehabilitation progress. After programme completion, patients were followed up at 3 months, 6 months, 1.5 years, 2.5 years, and 3.5 years. The electronic clinical record system – the Clinical Data Analysis and Reporting System (CDARS) of the hospital – was used to retrieve past records and has identified 500 patients who joined the PRP from the years 2003 to 2015. Sixty-nine patients without COPD diagnoses were excluded. Finally, 431 participants diagnosed as COPD were recruited for the study. Ethical approval was obtained from the Kowloon Central/Kowloon East Cluster Hospital Authority Ethical Committee (KC/KE-170047/ER-1).
Demographics and survival parameters
Mortality status, death dates, and the causes of death with reference to the 10th revision of the International Statistical Classification of Diseases and Related Health Problems (ICD-10) were retrieved from the CDARS on the 1st June 2018. Demographics and PRP parameters that might predict better survival were captured from the individual medical records of the CDARS. The factors available for analysis included gender, use of long-term oxygen therapy, predicted forced expiratory volume in 1 second (FEV1 predicted), forced vital capacity, PRP completion rate, and functional/quality of life scores as assessed using the following instruments: Chronic Respiratory Disease Questionnaire (Chan, Tam, Chan, Ng, & So, 2006), Morser’s activities of daily living (ADL) class, and Monitored Functional Task Evaluation (MFTE) score at baseline and on completion of PRP.
Instruments
The Chronic Respiratory Disease Questionnaire (CRQ) was a valid and reliable instrument for measuring the health status of patients with chronic respiratory disease in the Hong Kong population. It evaluates the impact of dyspnoea, fatigue, emotion, and mastery of the disease on the ADL of patients with COPD.
Classification of functional pulmonary disability: The Moser’s Activities of Daily Living (ADL) class which was used to rate their actual performance of ADL over the last two weeks period (Moser, Bokinsky, Savage, Archibald, & Hansen, 1980) was used. The class ranged from 1 to 5 with higher ADL class indicating lower functioning. Moreover, an ADL class of higher than 2 was a cut-off score indicating that the patient is indoor bound.
MFTE score is a symptom-limited evaluation that measures patient’s monitored functional performance in a laboratory-based environment (Fong et al., 2001). It consisted of five functional tasks, namely indoor mobility, sitting to standing transfer, lifting, carrying, and stepping. The maximum total score is 20 with higher scores indicating better performance in ADL.
Statistical analysis
Patients were first split into two age groups using the mean age of 72 years as the cut-off for separate data analysis. Median survival time of the two groups of patients was calculated using Kaplan–Meier analysis. Cox-proportional regression model was then used to explore factors that predict a better survival rate. The most significant predictors were used as strata, and their respective effects on survival functions were analysed using Kaplan–Meier analysis again (Figure 1).
Results
Four hundred and thirty-one patients with COPD participated in the PRP in the Respiratory Medical Department, Kowloon Hospital, between 2003 and 2015. The mean age of this cohort was 72.5 years, ranging from 45 and 90 years old. Most of them (46.7%) were at stage III as classified using GOLD classification (Global Strategy for the Diagnosis, Management and Prevention of COPD, 2017). The mean FEV1 predicted was 41.08%. The demographics of participants are shown in Table 1.
Demographics of participants.
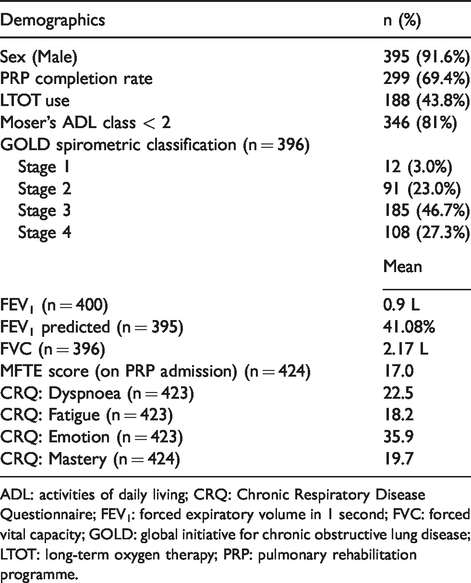
ADL: activities of daily living; CRQ: Chronic Respiratory Disease Questionnaire; FEV1: forced expiratory volume in 1 second; FVC: forced vital capacity; GOLD: global initiative for chronic obstructive lung disease; LTOT: long-term oxygen therapy; PRP: pulmonary rehabilitation programme.
As dated on 1 June 2018, a total of 322 participants (74.7%) passed away. A total of 274 death records contained identifiable death causes according to the ICD-10, and their causes of death are summarised in Figure 2. The top 3 causes of death were pneumonia, COPD, and bronchus/lung cancer. 73.4% of the participants died due to non-cancer respiratory related causes. The Kaplan–Meier analysis showed that the median survival of the cohort was 4.29 years (95% CI 3.9–4.7) (Figure 3). The median survival times of the two groups of patients – aged <72 years and aged ≥72 years – were 5.3 years (95% CI 4.4–6.2) and 3.6 years (95% CI 2.9–4.2), respectively (Figure 4).
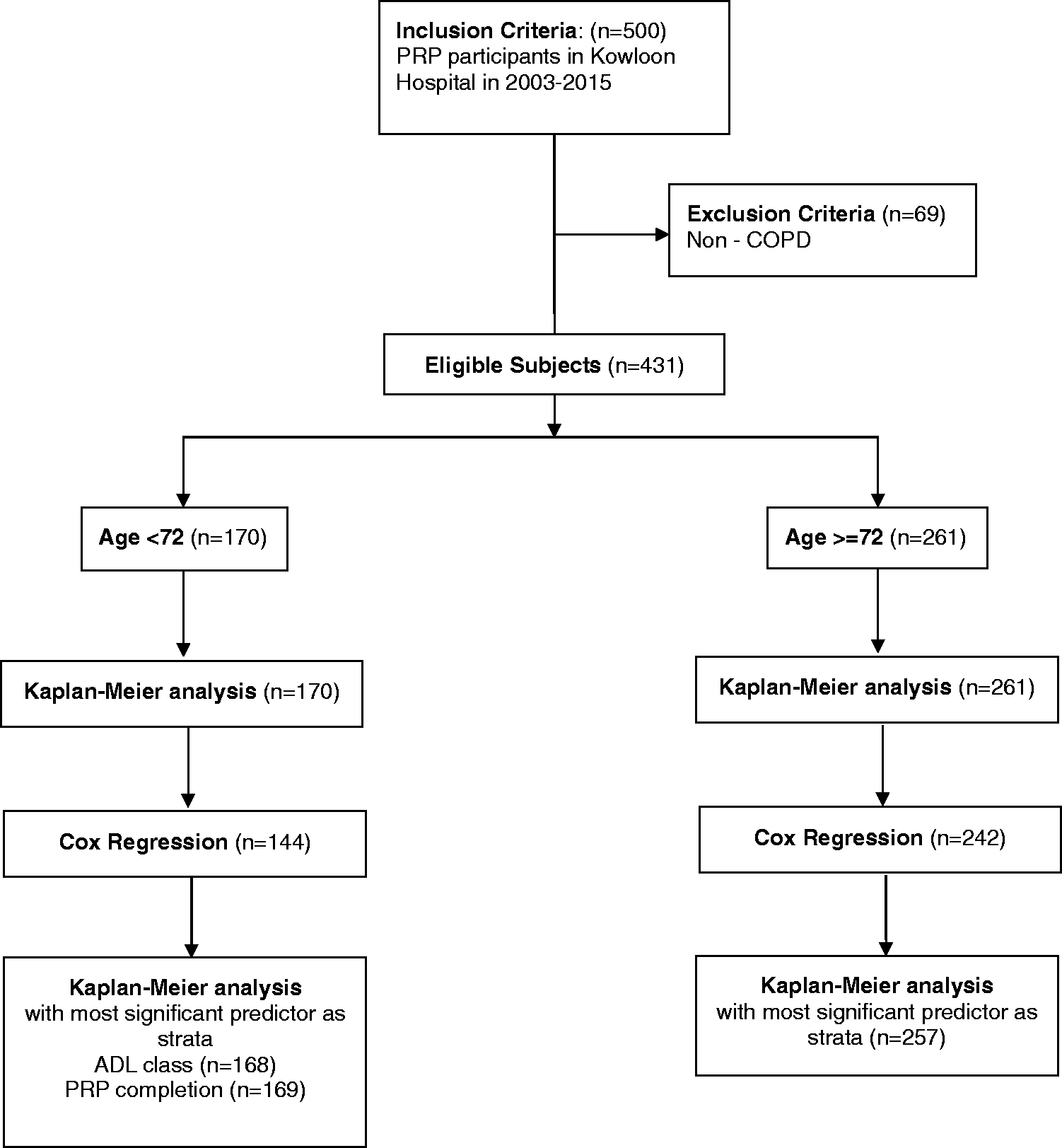
Consort diagram of the study. ADL: activities of daily living; COPD: chronic obstructive pulmonary disease; PRP: pulmonary rehabilitation programme.
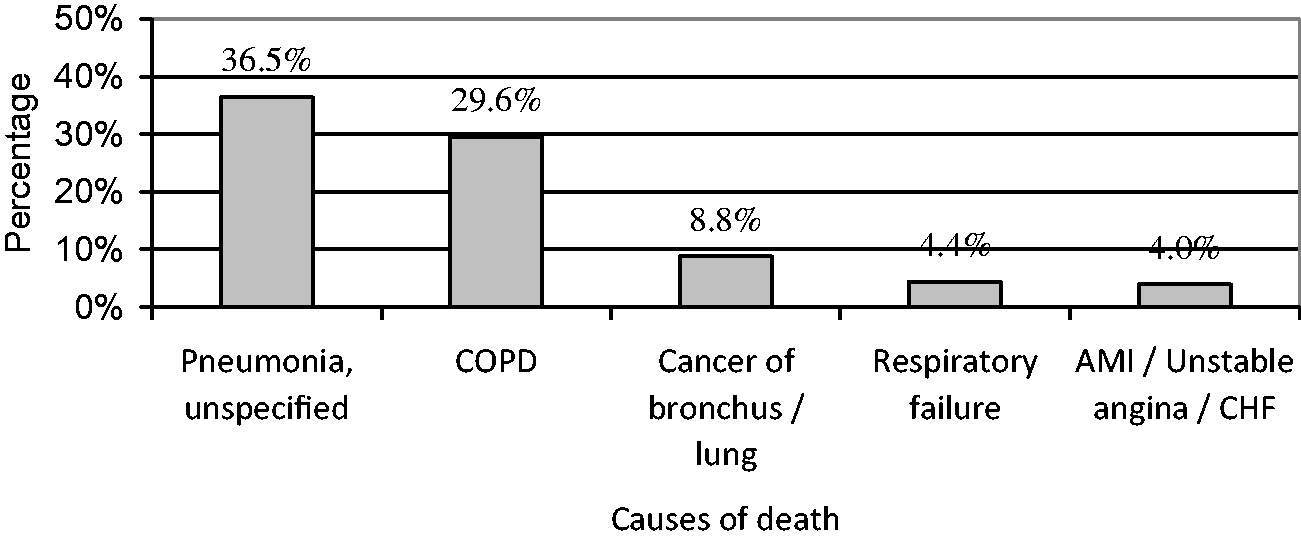
Causes of death according to ICD-10. AMI: acute myocardial infarction; CHF: chronic heart failure; COPD: chronic obstructive pulmonary disease.
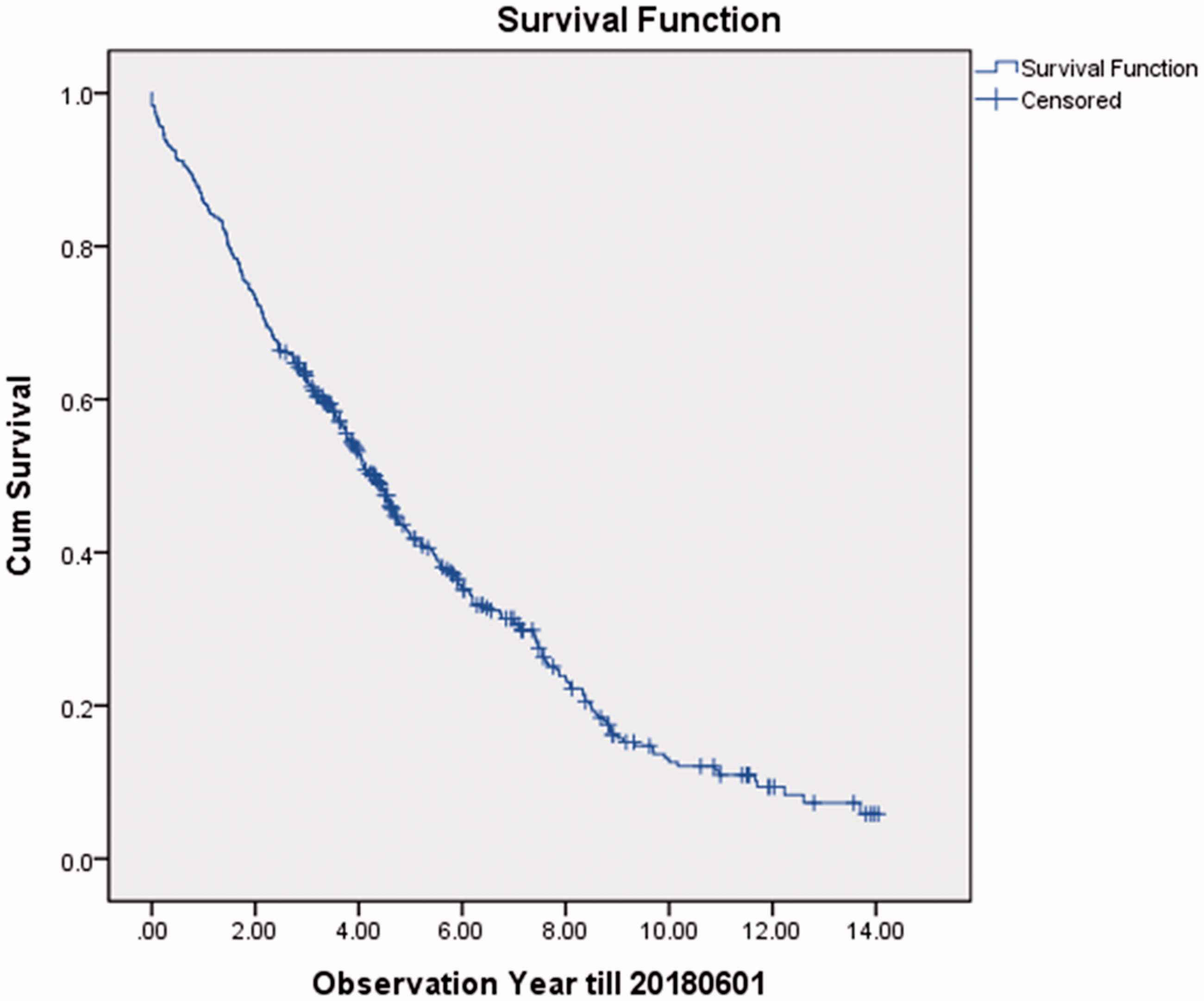
Kaplan–Meier analysis for all recruited subjects (n = 431).
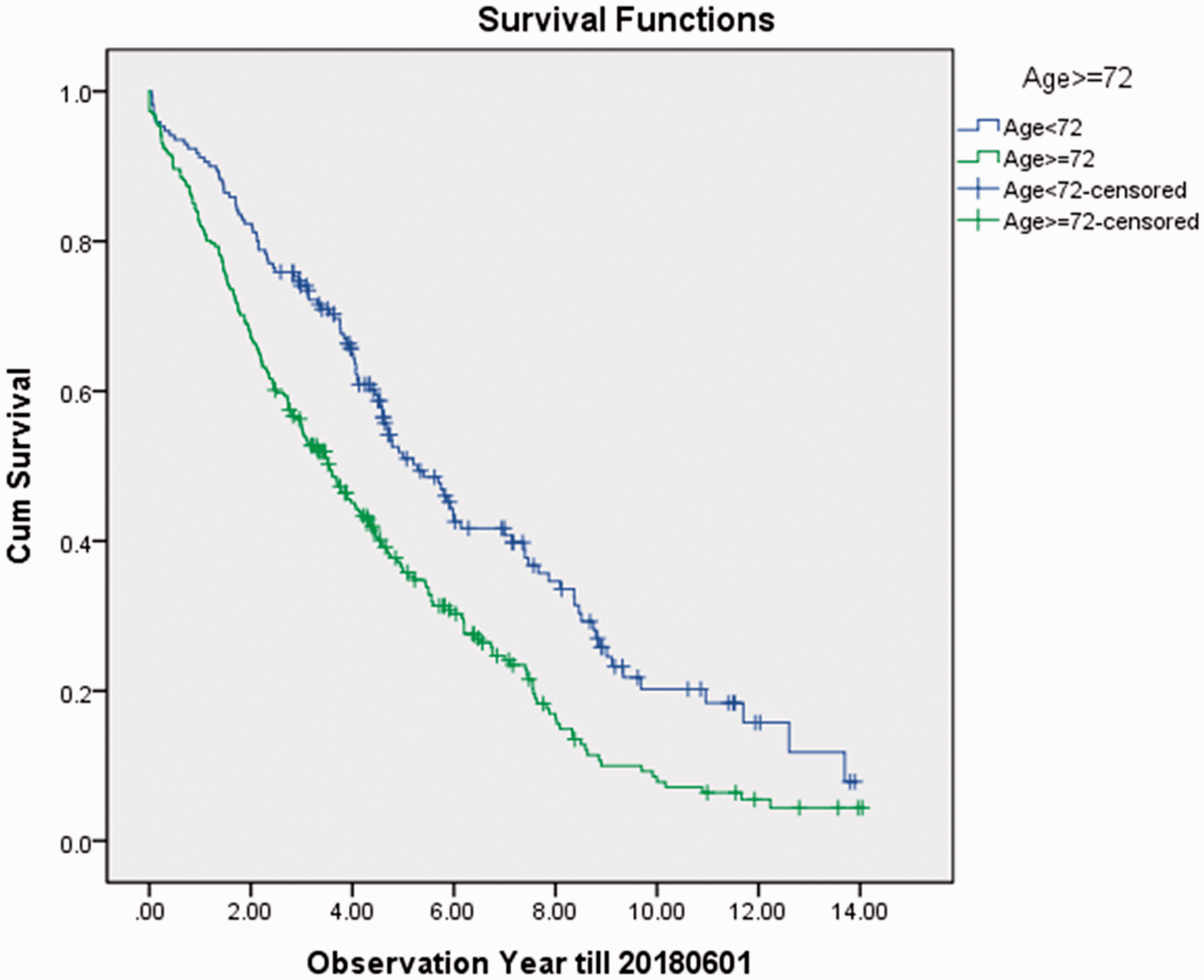
Kaplan–Meier analysis for all recruited subjects (n = 431), age group as strata.
For patients aged <72 years, ADL performance (p = 0.025), and PRP completion rate (p = 0.01) were found to be significant survival predictors (Table 2). The median survival times for those with Moser’s ADL class <2 and those with Moser’s ADL class >2 were 5.7 years (95% CI 4.6–6.9) and 4.1 years (95% CI 2.1–6.1), respectively (Figure 5). Moreover, the median survival times for PRP completer and non-completer were 7 years (95% CI 5.2–8.8) and 4.1 years (95% CI 2.8–5.3), respectively (Figure 6).
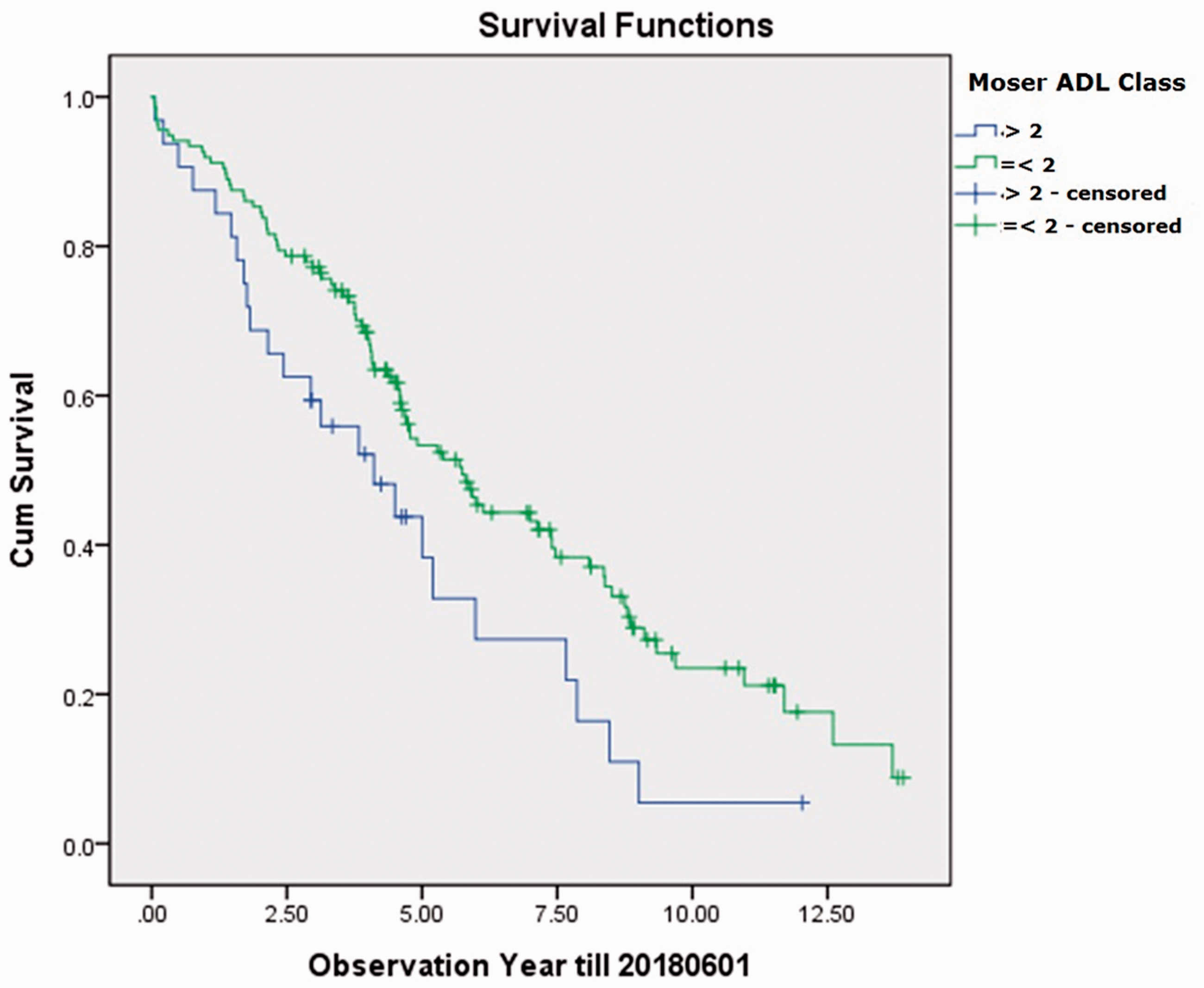
Kaplan–Meier analysis for age <72 subjects (n = 168), ADL class as strata. ADL: activities of daily living.
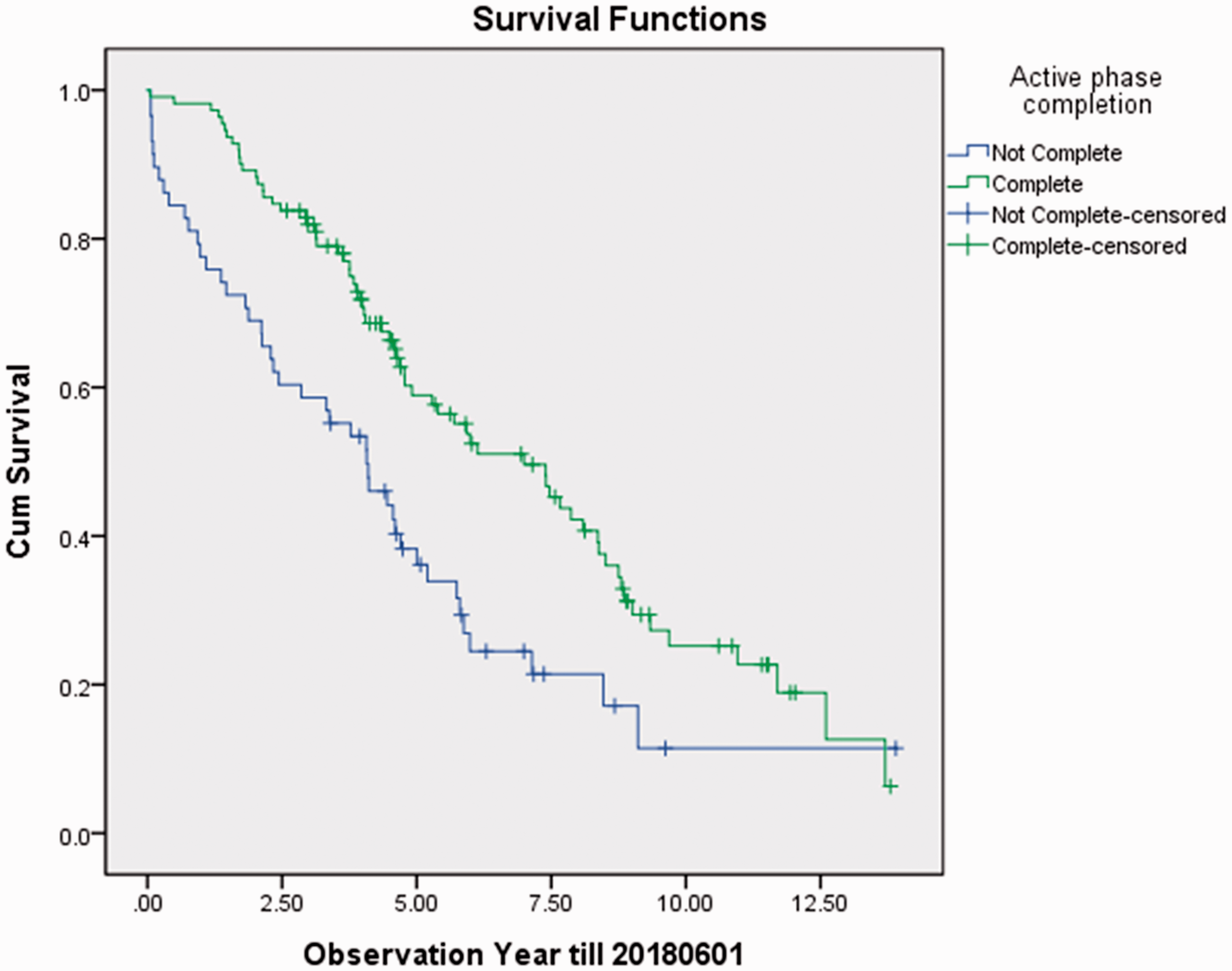
Kaplan–Meier analysis for age <72 subjects (n = 169), PRP completion as strata.
Results of cox regression analysis.
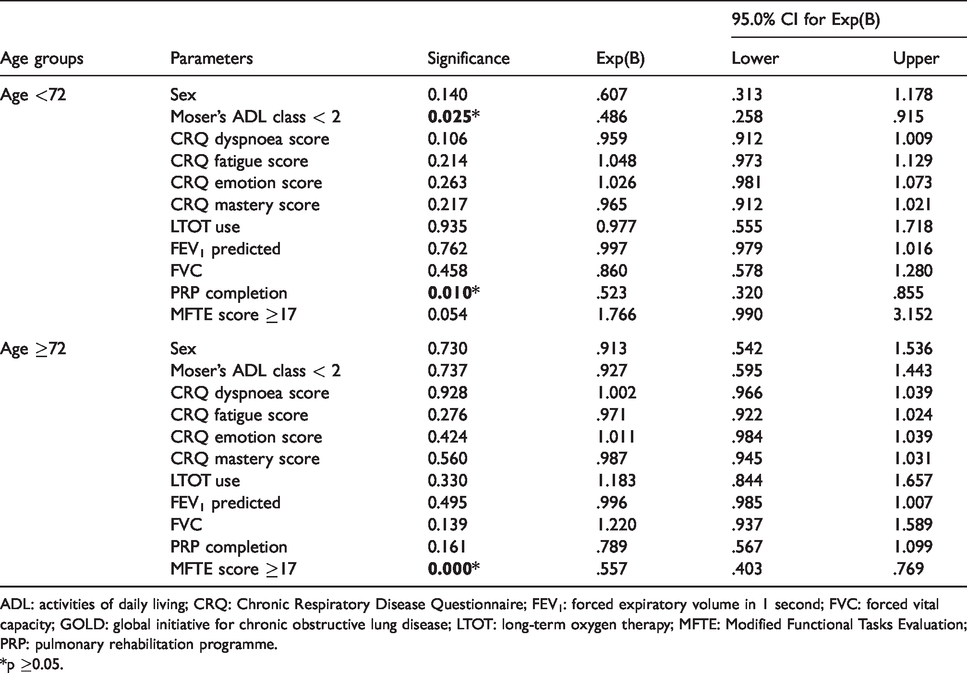
ADL: activities of daily living; CRQ: Chronic Respiratory Disease Questionnaire; FEV1: forced expiratory volume in 1 second; FVC: forced vital capacity; GOLD: global initiative for chronic obstructive lung disease; LTOT: long-term oxygen therapy; MFTE: Modified Functional Tasks Evaluation; PRP: pulmonary rehabilitation programme.
*p ≥0.05.
For patients aged ≥72 years, their MFTE scores as rated during admission to the PRP could significantly predict their survival outcomes (p < 0.000) (Table 2). The median survival times for those having MFTE score ≥ 17 and <17 were 4.9 years (95% CI 3.7–6.0) and 2.2 years (95% CI 1.5–2.9), respectively (Figure 7).
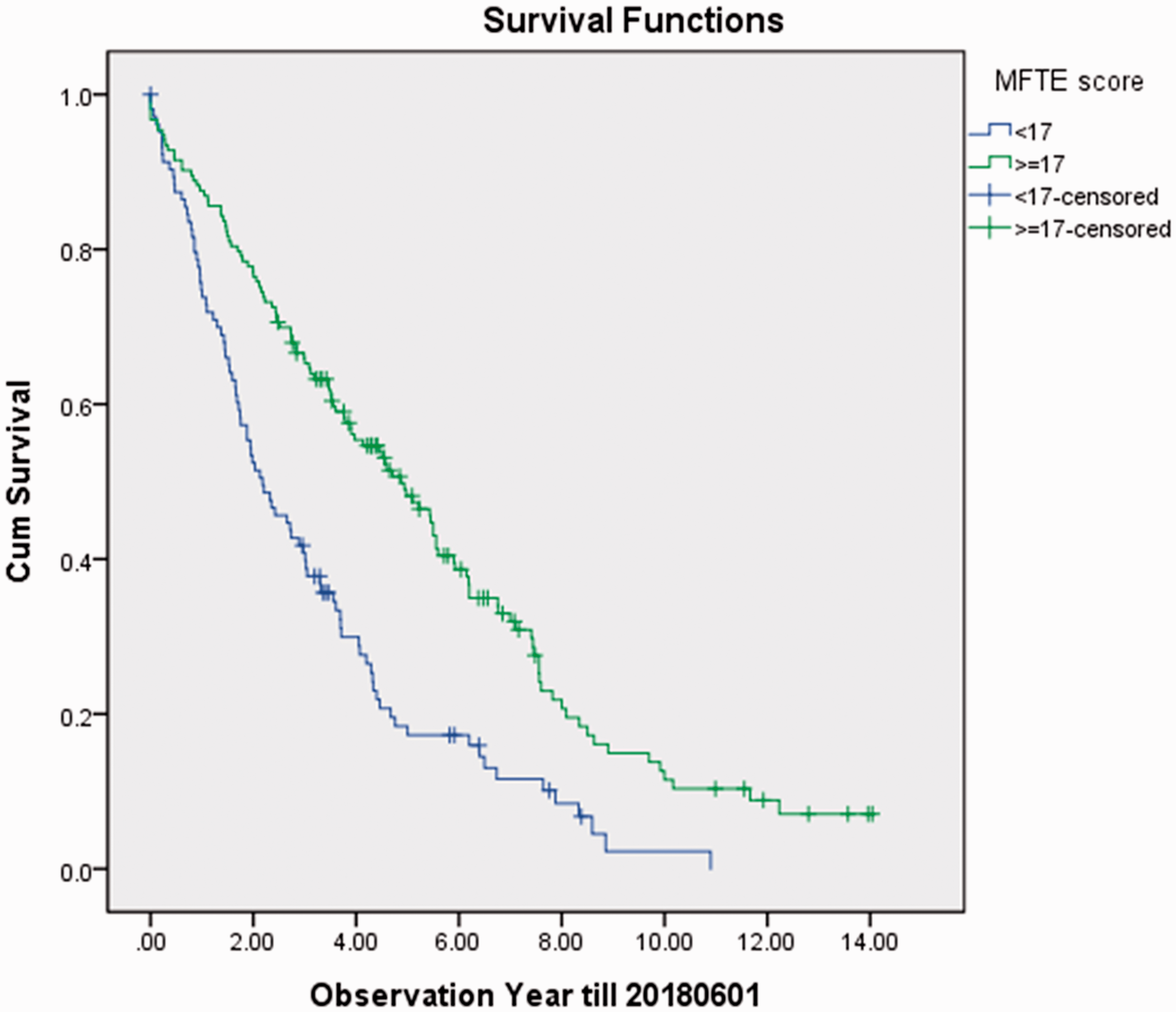
Kaplan–Meier analysis for age ≥ 72 subjects, MFTE score as strata. MFTE: Modified Functional Tasks Evaluation.
Discussion
Our findings provided evidence for the survival outcomes of patients with COPD after a local PRP. In this study, participants were followed up for 3.5 years after completing the active phase of our PRP. Comparing with the findings of other overseas studies that investigated the survival functions of participants after PRP (Dajczman et al., 2015; Hjalmarsen et al., 2014; Saraiva et al., 2016; Varela, Anido, & Larrosa, 2006; Voogd et al., 2009), the participants recruited in the current study were older in average (Table 3). This might account for the findings that our participants have comparatively a shorter survival rate as compared to those studies by Hjalmarsen et al. (2014) and Voogd et al. (2009). The present study identified that the MFTE score which reflected functional capacity of subjects could be a significant survival predictor for older participants. In addition, our findings suggested that better ADL performance as indicated by lower Moser’s ADL class and successful completion of PRP may significantly predict better survival rate in younger participants after PRP (Table 2). The overall findings would help our local healthcare providers working in settings with PRP to identify suitable patients for timely intervention and support.
Comparison of survival outcomes among patients after PRP in different studies.
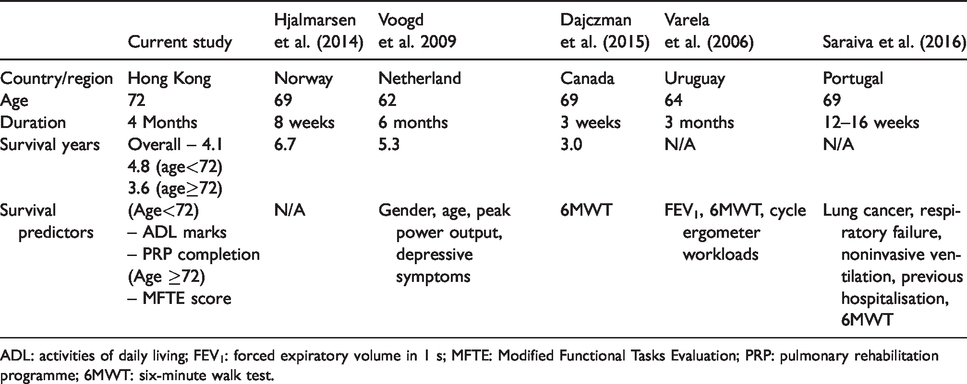
ADL: activities of daily living; FEV1: forced expiratory volume in 1 s; MFTE: Modified Functional Tasks Evaluation; PRP: pulmonary rehabilitation programme; 6MWT: six-minute walk test.
Survival is an important outcome in healthcare research but it appears that not many occupational therapists are interested to investigate. There was a ground breaking research in the late 1990s which reported that social and productive activities that involved little or no enhancement of fitness could lower the risk of all-cause mortality as much as fitness activities do (Glass, de Leon, Marottoli, & Beckman, 1999). Their findings suggested that in addition to increased cardiopulmonary fitness, activity might confer survival benefits through psychosocial pathways (Glass et al., 1999). There were other studies that reported interesting findings particularly on the effect of occupational therapy on survival. Gitlin, Hauck, Winter, Dennis, and Schulz (2006) found that in-home occupational therapy intervention might reduce mortality in functionally vulnerable older people. Maekura et al. (2015) found that a personalised pulmonary rehabilitation and occupational therapy might also reduce mortality for patients with advanced COPD. Therefore, if the assumption that there is a relationship existing between occupation and health, we believe that occupation can have inherited potential to modify disease conditions and survival (Iwarsson, Isacsson, Persson, & Schersten, 1998).
Occupational therapists started to provide rehabilitation services to patients with COPD in selected local settings in Hong Kong way back in 1989 (Chen, 1989). In line with the advancement in PRP in the recent decades, more emphasis is put on facilitating behaviour and/or lifestyle change for disease management in the rehabilitation of patients with COPD. Thus, with our strong training background in both physical and psychosocial aspects, local occupational therapists had grasped further opportunities to contribute and influence in related aspects (So, 2015). Occupational therapists have become core members of the PRP, and even case managers in the providing post-discharge community support services for this group of patients (Ng, 2014). In the review of the global challenge of respiratory medicine in the 21st century, Alam (2016) also advocated that occupational therapy could have a profound effect on respiratory health by increasing awareness through education, training, advice on lifestyle, and daily occupations of patients with COPD which could then reduce related economic costs and enhance patients’ health and wellbeing.
As shown from the results among the younger participants with COPD aged ≥72 years, a higher Moser’s ADL class and non-completion rate of PRP were identified as the ‘at risk’ group with poor survival. We suggested that by identifying the underlying reasons for those patients defaulting PRP (due to, for example, medical reasons, psychological and social barrier, and motivation problems, difficulties for out-door transportation, etc.), the rehabilitation team could develop a better care plan for them. The care plan might include prescription of portable oxygen and assistive devices, utilising community resources, home-based pulmonary rehabilitation, counselling, and motivational interviewing, which would help to facilitate their completion of the PRP (Konkle-Parker, 2001).
For the older participants with COPD (aged ≥ 72 years), low exercise capacity with MFTE score < 17 was the most significant risk factor to survival. A previous study also indicated that exercise capacity could be the best predictor of mortality in patients with COPD (Oga, Nishimura, Tsukino, Sato, & Hajiro, 2003). Findings from another systematic review also identified that patients with COPD were generally very inactive, and this physical inactivity was detrimental to both quality and quantity of life (Spruit, Pitta, McAuley, Zuwallack, & Nici, 2015). Therefore, increased efforts for better understanding the determinants of physical activity, as well as effective strategies to improve this variable, must be a prominent goal in pulmonary rehabilitation. Application of various behavioural strategies, such as health coaching, occupational lifestyle redesign, etc. to promote patients’ participation in different varieties of physical and/or sport activities, including higher physically demanding home activities, might help to improve their physical capacity levels and then their survival outcomes.
Regarding causes of death, 73.4% of our participants in PRP passed away due to non-cancer related respiratory diseases. Apart from exercise training, disease management might be a way to help this group of patients for improving their survival outcomes. Further enhancement and integration of the ‘Living Well with COPD’ model with an emphasis on managing exacerbations, using inhalers properly, etc. was also a potential area for service improvement in future (Bourbeau, Lavoie, & Sedeno, 2015). Further studies on the benefits of disease management might also be helpful in guiding our PRP towards a more evidence-based practice.
Limitations
Although the sample size of this study was large enough for regression analysis, this study still had limitations. Firstly, this was a longitudinal study, a comparison group for participants without participating in PRP is suggested to be used for comparison in future. As there were limited data available in the CDARS, other useful data, such as BODE index and smoking status, etc., were unavailable from the system. It was also suggested that the clinical system should capture these parameters for the purpose of survival analysis in future.
Conclusion
To the best of our knowledge, this study was the first local study investigating the survival outcomes of patients with COPD after a PRP. It also explored related survival predictors which might be used to guide healthcare practitioners and occupational therapists to identify those individuals who should be more intensively treated as well as closely monitored, and to help in identifying those treatment areas which should focus on improving patients’ survival.
Footnotes
Acknowledgements
We would like to dedicate this piece of work to the late Dr CHEN Nai Kwi William (1947–2019), the first Chief of Service of the Respiratory Medical Department of Kowloon Hospital who introduced the first ambulatory multi-disciplinary pulmonary rehabilitation programme to Hong Kong and who assisted to develop the first occupational therapy treatment room near the wards of Respiratory Medical Department.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
