Abstract
This scoping review explores factors that contribute to medical students’ burnout and identifies the barriers hindering efforts to address burnout and interventions implemented to improve well-being. This scoping review was conducted using the Arksey and O’Malley York methodology. The Joanna Briggs Institute (JBI) guidelines guided the processes of data extraction, evaluation, and reporting of findings. The most common interventions included peer-mentorship programs (n = 6), well-being curriculum interventions (n = 5), virtual wellness programs (n = 1), exercise-based events (n = 1), fireside chats (n = 1), reflective writing courses (n = 1), and faculty-led life coaching (n = 1). Commonly identified risk factors consisted of failure to nurture personal relationships that support emotional resilience (n = 4), the academic rigors of medical education (n = 4), poor time management (n = 3), and poor financial planning or a high debt burden (n = 3). In summary, these studies demonstrate a diverse range of approaches to improving student wellness as influenced through peer and faculty mentoring, highlighting the importance of intervention frequency, continuity across all stages of medical training, and the value of intimate, informal settings in enhancing faculty and student engagement. Our findings will inform future efforts in improving medical student burnout through the design and implementation of various types of wellness programming and systemic changes in medical education.
“Peer-directed approaches not only foster a sense of community but also are easy and cost-effective for institutions to implement.”
Introduction
Burnout is a psychological phenomenon which typically occurs in response to sustained stress.1,2 Symptoms associated with burnout include depersonalization, loss of a sense of personal accomplishment and a high degree of emotional exhaustion as defined by the National Academy of Medicine, all of which have the potential to carry forward throughout training. 3 In the 1990s, burnout was formally recognized in the medical field following research studies showing significant associations between physician burnout and medical errors. 4 Subsequent research revealed that burnout actually started earlier in medical training, with reported accidents and medical errors starting in medical school and lasting throughout residency. 5 In medical school, burnout has been noted to occur in stages as the student progresses in training, starting with inattention, lapses in memory, irritability which can progress to maladaptive habits including issues with professionalism along the lines of absenteeism, and finally landing at exhaustion which may result in depression. 6 It is important to note that burnout has further reaching effects such as the potential to create a sense of detachment and lack of engagement which can negatively impact empathy.1,6 Multi-institutional studies reveal that half, if not more, of medical students experience burnout. 7 A study by Rotenstein et al found that the prevalence of U.S. medical students experiencing symptoms of depression is three times higher than the prevalence of this mental health issue in their age-matched peers.8,9 As for residency, long resident training hours and higher incidence of mental health issues were some of the reported adverse consequences of reported burnout rates in the medical field.5,10 A meta-analysis of over 22, 000 residents showed an alarming burnout rate of 51%, which varied individually across specialties and led to worsening manifestations of mental health illnesses such as anxiety, depression, and PTSD. 11 Since burnout evolves on a continuum starting as early as medical school, continuing through residency, and worsens in clinical practice, it is important to start treating this potential epidemic as early as possible to not only equip students with the skills and strategies needed for building a career centered around wellness and well-being which can be maintained longitudinally into their practice years but also to reduce its severity both of which will be beneficial in future clinical settings. 12
Challenges in addressing burnout stem from its multilevel and complex etiology, with influential factors ranging from the individual to the interpersonal, organizational, community, and social levels.13,14 To address such barriers, the American Association of Medical Colleges (AAMC), the governing agency of medical schools in the United States, highly emphasizes the need of wellness integration into medical school curriculums. 15 Some US medical schools have begun implementing wellness programs to not only assess the stressors affecting medical student performance but also evaluate the extent of stress experienced in medical students. 15
Wellness interventions that have shown improvements in medical student well-being have been achieved at the college level including curricular revamping, changes in grading systems, and faculty training in mindfulness.1,16,17 Another main theme in reported program outcomes is that students should be involved in the implementation of wellness programs as these are not a one-size-fits-all approach but rather individualized interventions tailored to the needs of medical students and the type of burnout they are experiencing. 18 A recent systematic review exploring wellness interventions and their efficacy revealed that some components such as less competitive grading, mental health access, and mindfulness may improve student well-being. 19 However, the evidence on the impact of such programs, peer and mentor involvement, and sustainability of such crucial efforts is still limited in scope. 19 Additional studies are needed to further delineate the long-term sequalae of such interventions as well as to determine the most effective implementation strategies for sustainability of positive student wellness outcomes.
In this scoping review, our goal is to explore factors that contribute to burnout in medical students as well as to identify the barriers that hinder efforts to address medical student burnout and improve well-being. Our findings will inform future efforts in improving medical student burnout through the design and implementation of various types of wellness programming and systemic changes in medical education.
Methods
The review team comprised medical students, one public health expert, and one academic physician with expertise and firsthand experience in medical student wellness programs and student well-being. This scoping review was conducted using the Arksey and O’Malley York methodology, which provides guidance to the authors through a five-step process: (1) defining the research questions; (2) completing a comprehensive literature search for relevant studies; (3) excluding studies that do not align with the predetermined criteria; (4) categorizing and mapping the data; and (5) synthesizing findings, summarizing key data, and reporting the key insights. 20 The Joanna Briggs Institute (JBI) guidelines guided the processes of data extraction, evaluation, and reporting of findings. 21 This approach ensured transparency, reproducibility, and enhanced the credibility of the review’s conclusions. 21 The study sections were developed with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) checklist as a reference framework. 22
Step 1: Defining the Research Questions
Four research questions were formulated for this scoping review: (1) What are the risk factors associated and/or increasing the risk of medical burnout during medical school? (2) What are the barriers encountered by U.S. medical school programs in addressing medical student burnouts? (3) What is the role of faculty mentorship and peer social support in improving burnout and well-being in medical students? (4) What are future recommendations for the development and implementation of effective wellness programs in U.S. medical schools for improved medical student overall performance and mental well-being?
Step 2: Conducting a Search for Relevant Studies
In collaboration with an expert research librarian (TF) with extensive experience in scoping review methodologies, a comprehensive set of keywords and Medical Subject Headings (MeSH) terms were developed to guide the search process. The search terms included:
Inclusion Criteria
Included in this review were peer-reviewed studies published in English between 2014 and 2024, conducted in the United States, that addressed factors associated with or increasing the risk of medical burnout during medical school. These studies explored the impact of wellness programs in medical schools, the role of faculty mentorship, and peer support in enhancing student well-being. The focus was specifically on medical students during their four years enrolled in a medical school program.
Exclusion Criteria
Excluded from this review were studies that did not focus on the role of faculty mentorship, peer social support, or wellness programs in improving medical student burnout rates. Studies conducted outside the United States, those not based on a pre-existing psychological diagnosis for burnout (e.g., anxiety, depression), or those published in a language other than English were also excluded. Additionally, review studies, editorials, case series, case reports, and published abstracts were not included. Conflicts were resolved through collaborative discussions between co-authors.
Step 3: Selecting Studies that Align with the Research Questions
Study Characteristics.
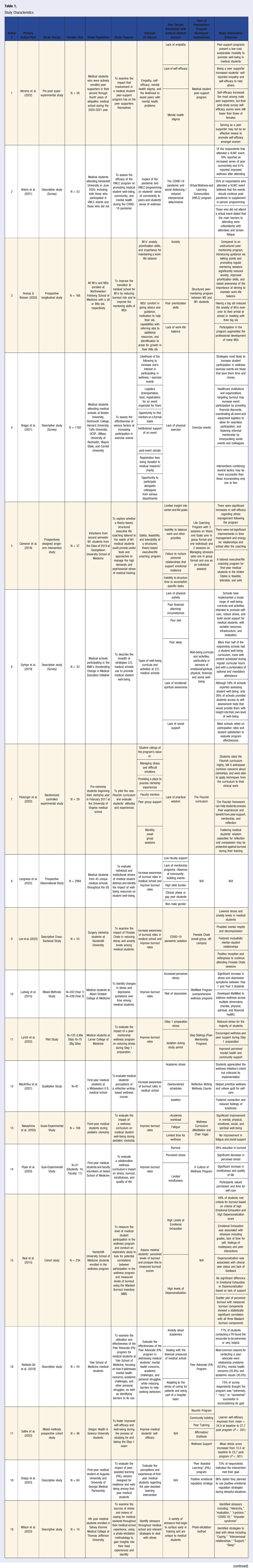
Barriers encountered by Medical Schools in Addressing Medical Student Burnout.
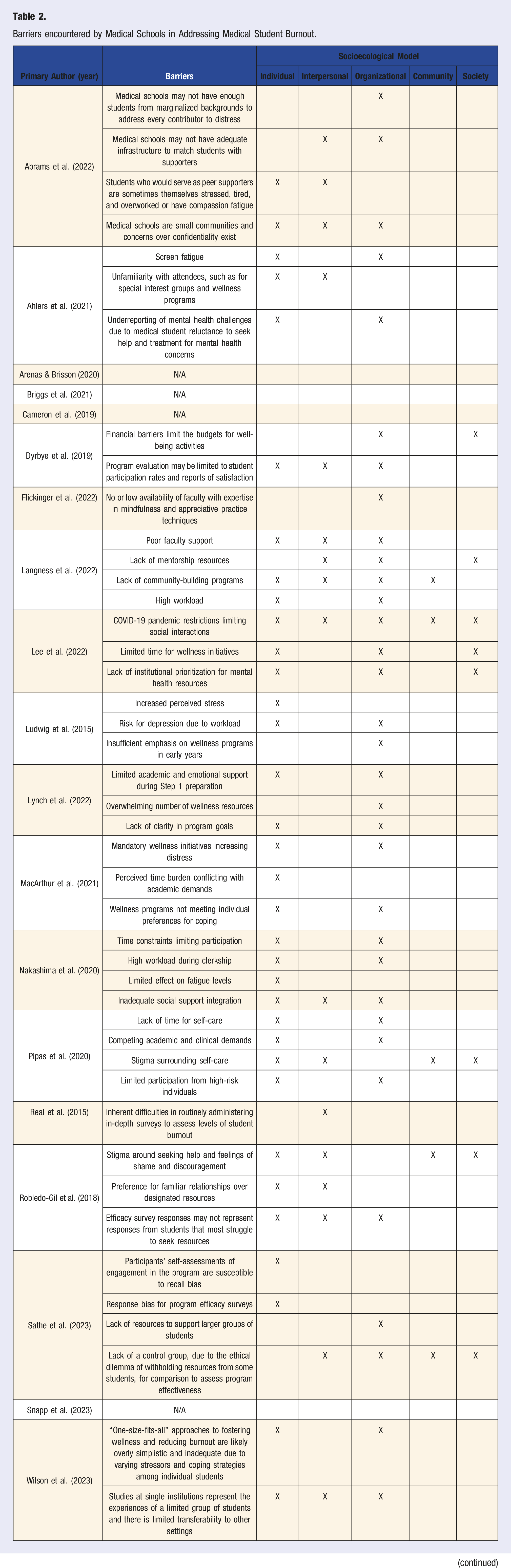
Role of Peer Support and Faculty Mentorship in Addressing Medical Student Burnout.
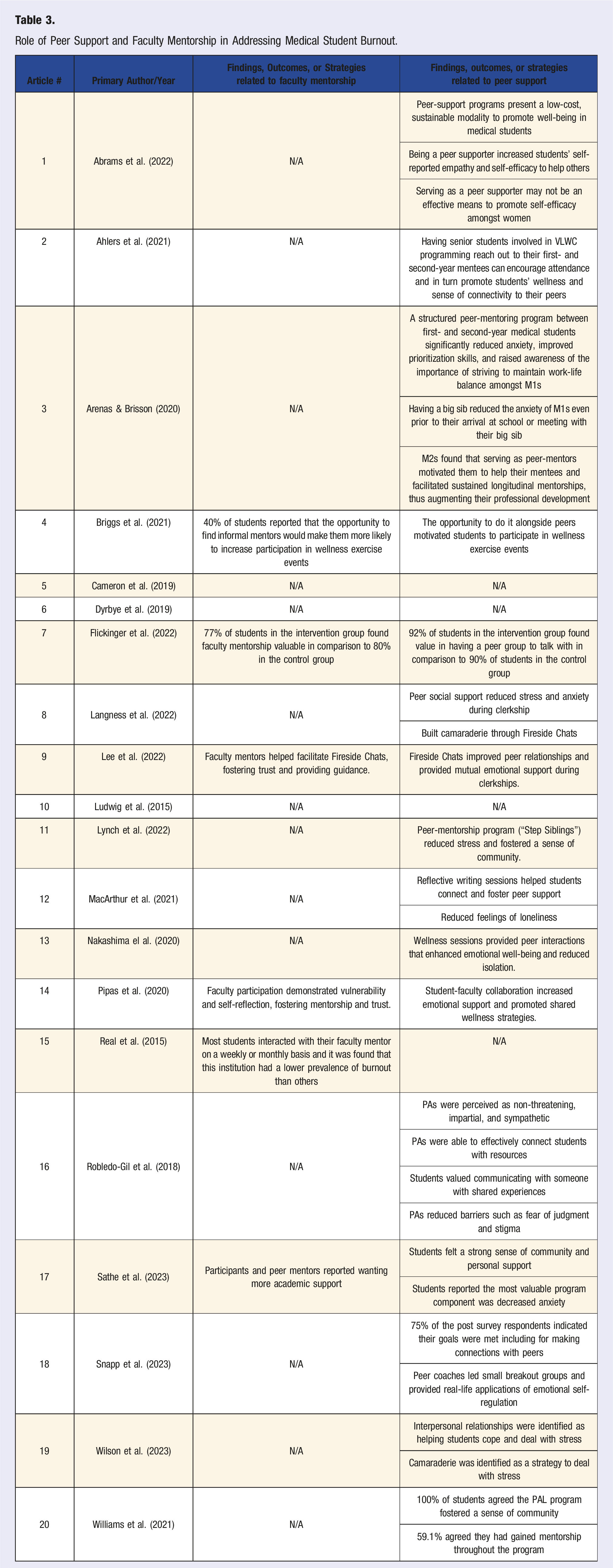
Recommendations for Future Design and Implementation of Effective Wellness Programs to Address Burnout in Medical Schools.
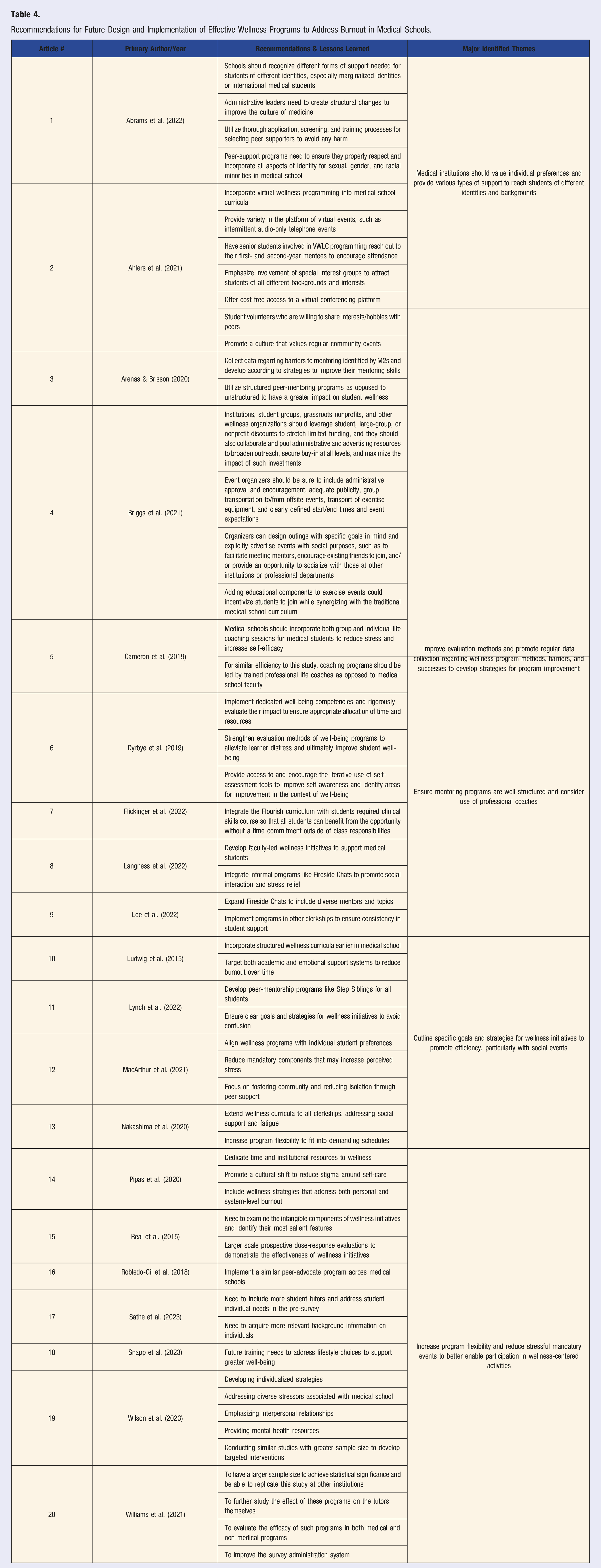
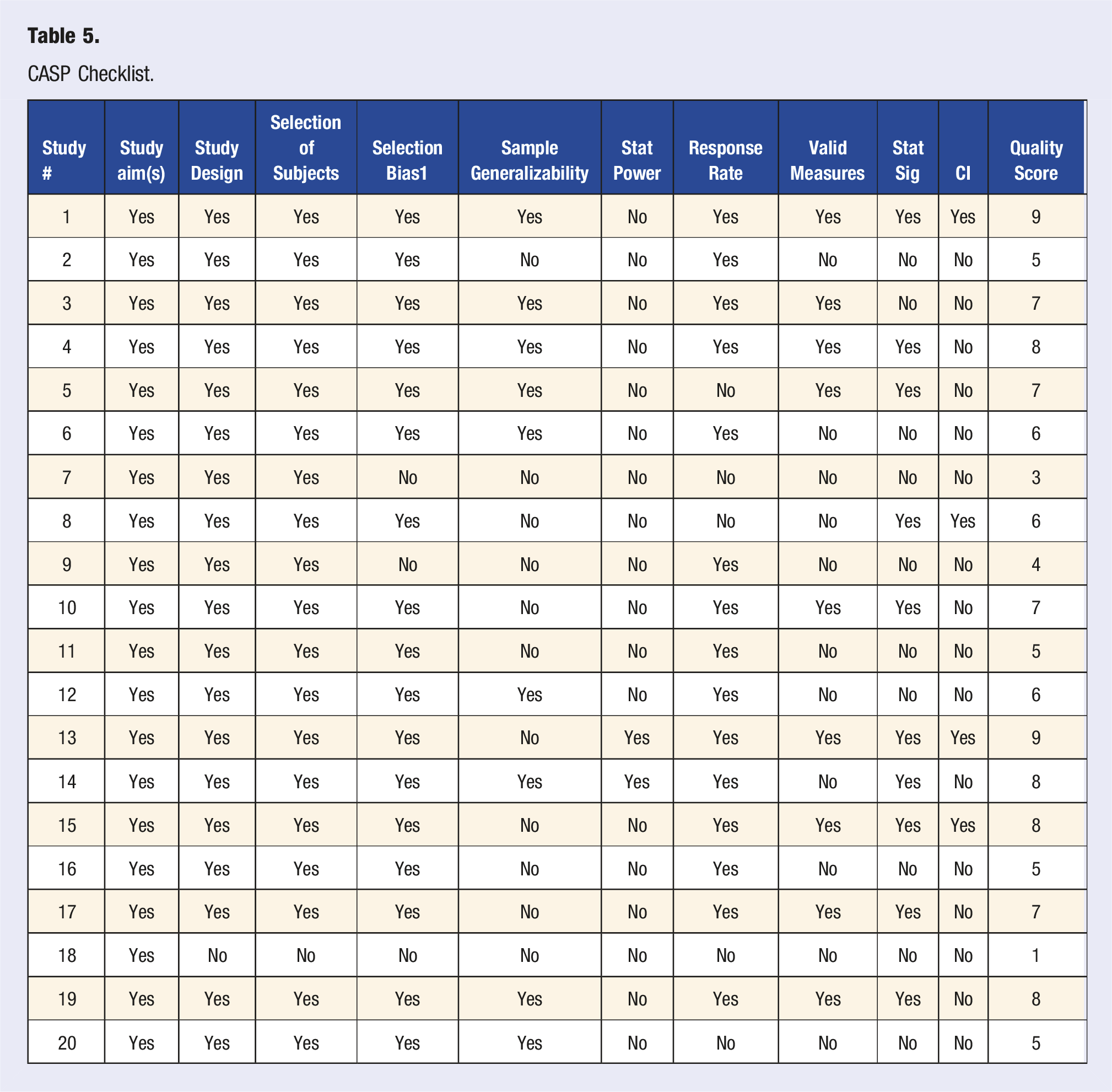
CASP Checklist.
Steps 4 and 5: Data Charting and Collation, Summarization, and Reporting of Results
Study characteristics were compiled and organized by the primary author and year of publication, providing information on the study design, sample size, study population, age range, study purpose, outcome of interest, risk factors contributing to burnout, and the type and outcomes of any interventions implemented (Table 1). Table 2 identifies the barriers encountered by U.S. medical school programs in addressing medical student burnout and contextualizes these barriers within the five levels of the Social-Ecological Model (SEM) (individual, interpersonal, organizational, community, and societal levels). 24 The Social-Ecological Model (SEM) has been applied in public health research for its ability to address both individual behaviors and broader societal influences on health outcomes. 24 Its focus on layered interactions provides a comprehensive framework for evaluating the complex factors shaping health outcomes across social environments. 24 Table 3 describes the impact of faculty mentorship and peer social support on measures of medical student well-being and mental health outcomes. Table 4 presents a list of potential future recommendations for the development and implementation of evidence-based wellness programs aimed at mitigating burnout in medical schools. As described by Elo and Kyngas (2008), three phases of qualitative content analysis were employed for the results of the primary qualitative research: (i) preparation, (ii) organizing, and (iii) reporting. 25 During the preparation phase, we defined the overarching topic and identified key themes. The organizing phase involved inductive content analysis. Finally, in the reporting phase, we presented the synthesized findings in Table 5. Moreover, the research team utilized the CASP checklist, a well-established critical appraisal tool, to thoroughly assess the methodological rigor and overall quality of the included studies. 23 By applying this checklist, the authors ensured that each selected study upheld standards of credibility, while also allowing for the clear identification of strengths, weaknesses, and limitations of the reported findings. 23 This same critical appraisal technique has been utilized in prior scoping reviews, further supporting its methodological integrity.26,27
Results
The initial study extraction resulted in 1473 articles from PubMed (n = 437), Scopus (n = 996), and Cochrane (n = 40). After screening, 743 studies were excluded for focusing on the wrong outcome, including those that did not address factors associated with or increasing the risk of medical burnout during medical school (n = 454), did not explore the impact of wellness programs in medical school, or did not examine the role of faculty mentorship and peer social support in improving student burnout rates (n = 211). Additionally, studies were excluded for having the wrong study design (n = 56) or being conducted outside the U.S. Duplicate studies were removed (n = 700). Thirty studies met the inclusion criteria. Following a full-text review, 10 more studies were excluded, resulting in 20 studies retained for analysis (Figure 1). Study selection process using the PRISMA flow chart.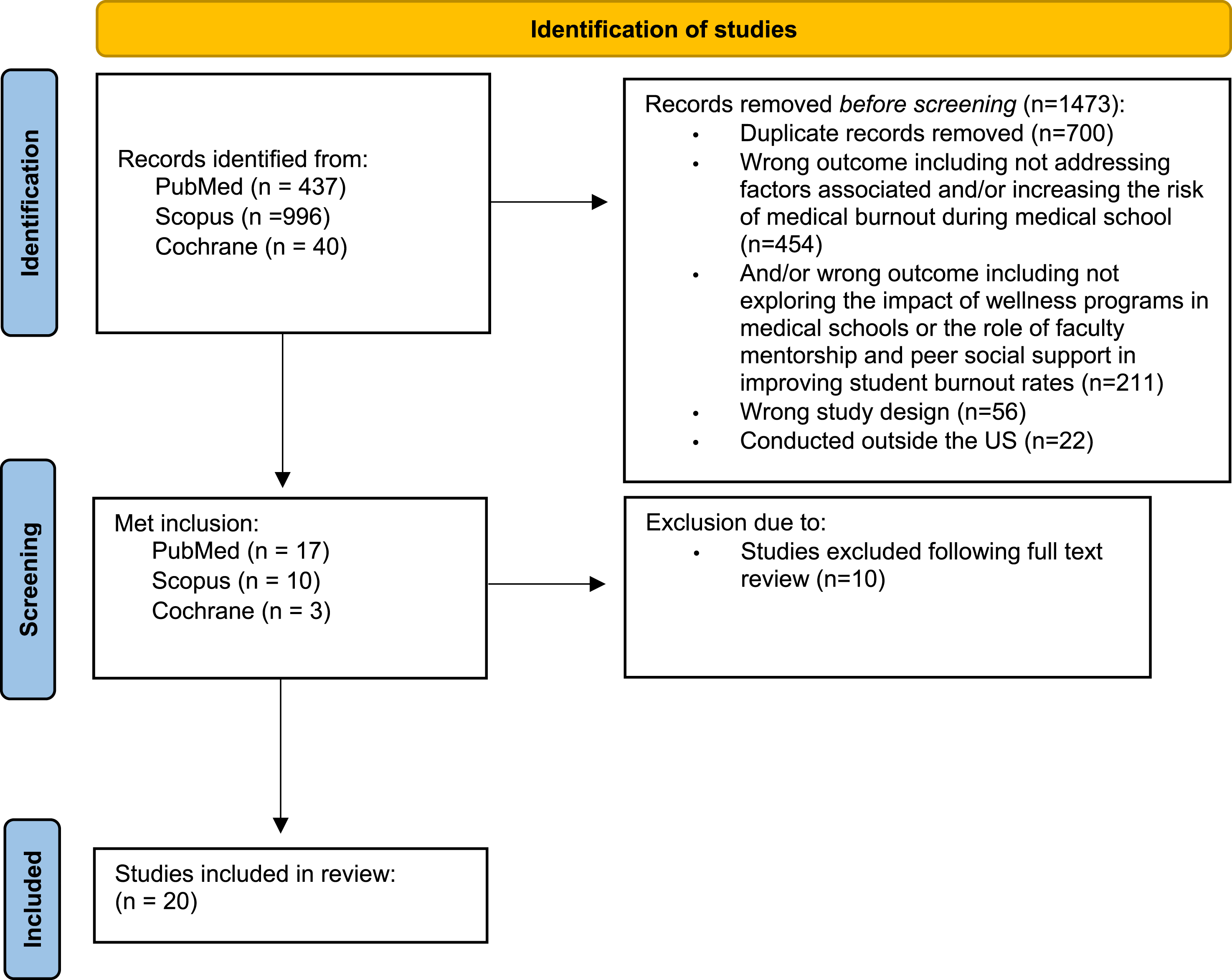
Of the 20 retained studies, published between 2015 and 2023, nearly three-quarters (15/20, 75%) were published in 2020 or in later years. Study designs included descriptive studies (n = 7), cohort studies (n = 3), quasi-experimental studies (n = 3), longitudinal studies (n = 1), observational studies (n = 1), a randomized controlled experimental study (n = 1), qualitative studies (n = 1), single-arm intervention studies (n = 1), a pilot study (n = 1), and a mixed-methods study (n = 1). Sample sizes varied, from as few as 10 fourth-year students in a descriptive study to 2984 students across 45 U.S. medical schools in a large observational study. However, most studies (65%) had fewer than 150 participants. The studies were conducted across diverse U.S. medical institutions, including both osteopathic and allopathic schools, spanning pre-clinical and clinical curricula. Access to database data involved medical schools across the U.S., such as Yale University, Augusta University, Oregon Health & Science University, Nova Southeastern University, Vanderbilt University, and Georgetown University School of Medicine. Interventions developed included medical student peer-support groups (n = 6), well-being curriculum interventions (n = 5), virtual wellness and learning community programs (n = 1), exercise events (n = 1), fireside chats (n = 1), and a reflective writing wellness course (n = 1), and faculty-directed life coaching (n = 1).
Scope of US Medical School Wellness Programs to Prevent and Address Medical Student Burnout
Included studies developed, implemented, and/or evaluated interventions to improve student wellness programs. Broadly, the interventions fell into three categories: peer-directed, faculty-directed, or alternative wellness approaches. Of the 20 studies, approximately 7 interventions (35%) were peer-directed, 5 interventions (25%) were faculty-directed, and the remaining took an alternative approach (n = 8). The most common interventions included peer-mentorship programs (n = 6), well-being curriculum interventions (n = 5), virtual wellness programs (n = 1), exercise-based events (n = 1), fireside chats (n = 1), reflective writing courses (n = 1), and faculty-led life coaching (n = 1). Key outcomes measured included stress reduction (n = 10), decreased anxiety (n = 2), improved student well-being (n = 5), and enhanced peer social support (n = 3) (Table 1).
Risk Factors Associated with Increased Risk of Medical Burnout During Medical School
Several key contributors to medical student burnout were highlighted in included studies (Table 2). Commonly identified factors consisted of failure to nurture personal relationships that support emotional resilience (n = 4), the academic rigors of medical education (n = 4), poor time management (n = 3), poor financial planning or a high debt burden (n = 3), lack of physical activity (n = 2), and the COVID-19 pandemic (n = 2). Other risk factors included lack of empathy (n = 1), lack of self-efficacy (n = 1), anxiety (n = 1), limited insight into career and life goals (n = 1) , poor diet (n = 1), poor sleep (n = 1), lack of emotional or spiritual awareness (n = 1), low faculty support (n = 1), absence of mentorship programs (n = 1), non-male gender (n = 1), clinical phase or gap year status (n = 1), high levels of emotional exhaustion and depersonalization (n = 1), and the challenges of adapting to the stress of patient care and working within a hospital team (n = 1). One study found nearly half of students met burnout criteria, characterized by high emotional exhaustion. Emotional exhaustion was strongly associated with stressors such as academic performance pressure, lack of time for self-care, feelings of inadequacy, and peer interactions. 28 Recognizing these growing trends, many schools have implemented programs to identify and assess student wellness. Although 59% of schools reported assessing student well-being, only 26% of schools provided medical students with access to self-assessment tools that would provide them with insight into their own level of well-being. 14 Furthermore, institutions that offered a greater number of well-being resources were associated with lower average levels of medical student distress (Table 2). 29
Role of Faculty Mentorship and Peer Social Support in Improving Burnout and Well-Being in Medical Students
Most peer-directed interventions focused on low-cost peer-mentorship or advocacy programs facilitated through mentorship between different class years (n = 6/7, or 86%) (Table 3). One intervention centered on recommendations to increase student participation in exercise events promoting wellness. 30 These peer-directed interventions varied in their focus, with some emphasizing emotional support and mentorship to promote overall well-being (n = 3), while others integrated peer-assisted learning (PAL) to enhance academic performance and resilience through structured educational sessions (n = 2).31-35 Additionally, one intervention specifically targeted the stress associated with USMLE Step 1 preparation, providing peer mentorship focused solely on emotional support rather than academic guidance during a challenging season of medical school (n = 1). 33 One study focused on peer-assisted education and tutoring sessions as a mechanism to enhance curriculum comprehension for students adjusting to medical school, highlighting its perceived benefits in improving knowledge and reducing test-taking anxiety. 34 Of these seven peer-centered intervention studies, all seven reported positive findings, indicating that peer mentorship often reduced self-reported anxiety and stress, improved coping mechanisms, and enhanced student focus work-life balance: many receiving positive feedback from students.30-36 Peer support is often cited for its ease of implementation, cost-effectiveness, and the sense of community it fosters (Table 3).
Faculty-directed approaches were often focused on institutional initiatives (n = 2), clerkship-specific interventions (n = 2), or mentorship/coaching sessions (n = 1). Of the faculty-directed interventions, institutional wellness initiatives and curricula sought to integrate multiple wellness strategies (n = 2).37,38 One small pilot study found that their initiative led to a 28% reduction in symptoms of burnout, along with a decrease in perceived stress. 38 Clerkship-specific interventions (n = 2) had varied results: one study demonstrated lowered stress and anxiety levels in medical students, while another found no improvement in fatigue and social support but noted improvements in mental, physical, and emotional well-being.39,40 Lastly, mentorship through the faculty coaching forum (n = 1) represented another avenue of intervention. 41 Surprisingly, one-on-one life coaching programs with faculty failed to produce significant improvements in time management; however, it did lead to significant increases in self-efficacy regarding stress management. 41 Other interventions present in the literature included a proposed reflective writing course, which medical students largely appreciated in theory. 42 However, they felt that adding the burden of writing assignments to their curriculum would likely increase stress rather than alleviate it. 42 One school developed a comprehensive approach to USMLE preparation that included weekly group exercises, daily affirmation emails, daily tutoring and gratitude-sharing activities, which enhanced self-efficacy among students. 43 Yet, this intervention was also associated with increased perceived stress and a decline in emotional health scores. 43 Another school developed a series of sessions incorporating storytelling, mindfulness, and reflective writing to provide options for coping, stress reduction, and emotional growth, but the study was limited by a small sample size due to voluntary participation. 44
Lessons Learned
In summary, these studies demonstrate a diverse range of approaches to improving student wellness as influenced through peer and faculty mentoring, highlighting the importance of intervention frequency, continuity across all stages of medical training, and the value of intimate, informal settings in enhancing faculty and student engagement (Table 4).
Critical Appraisal Skills Programme (CASP) Checklist
While all 100% (n = 20) of the studies in this review discussed study aims, only 95% (n = 19) of the studies described the study design and selection of subjects. Selection bias was mentioned in 85% (n = 17). Only 45% (n = 9) of studies discussed sample generalizability and valid measures. When explaining the statistical analysis of the studies, 75% (n = 15) noted response rate and only 10% (n = 2) of the studies stated statistical power. Further, when providing results, 50% (n = 10) of the studies discussed statistical significance and just 20% (n = 4) of the studies stated confidence intervals. Overall, the quality scores of all the studies ranged from 1 (n = 1, 5%) to 9 (n = 2, 10%) out of 10. 5% (n = 1) of studies had a score of 3, 5% of studies (n = 1) had a score of 4, 20% (n = 4) of studies had a score of 5, 15% (n = 3) of studies had a score of 6, 20% (n = 4) of studies had a score of 7, and 20% (n = 4) of studies had a score of 8. Studies with a quality score of 6 or 7, which comprises 35% of studies in this review, indicate a high-quality score of moderate rigor (Table 5).
Discussion
This scoping review aimed to define risks for medical student burnout in U.S. medical school and to assess the impact and role of schools’ wellness programs in addressing such burnout. It also evaluated the roles of faculty mentorship and peer social support in improving medical student burnout and well-being. Our findings provide future recommendations for the development and implementation of effective wellness programs in U.S. medical schools to improve medical student overall performance and mental well-being.
Results illustrate that medical school wellness programs reduce student stress and anxiety rates while helping to improve participants’ self-efficacy regarding coping strategies and self-care. Despite our study showing the importance of such programs, there remains a need for the establishment of more interventions to combat stress and mental health issues among medical students while enhancing their performance. Although different programs utilize often very different approaches, they collectively underline the overall value of institutional wellness programs in addressing student burnout. For example, medical students at the Kirk Kerkorian School of Medicine reported lower perceived stress when they spent more time engaged in wellness activities during the pre-clerkship and clerkship phases of medical school. 45 Similarly, looking outside solely the medical school context, college campuses have seen the beneficial impact of appropriately developed wellness programs. The Be REAL (Resilient Attitudes and Living) program, developed initially as a mindfulness-based coping-enhancement program at the University of Washington, showed an improvement in anxiety rates and a trend towards reducing depression. 46 These findings were illustrated not only when the program was run by facilitators in the research team, but also when the intervention was delivered by university staff, thus making it easier for institutions to implement. 46 At the University of California at San Diego (UCSD), researchers found that for-credit Learning Sustainable Well-being (LSW) courses led to an increased feeling of empowerment, increased compassion for self and others, and intention to continue practices learned in the class amongst students who took the courses. 47 Additionally, when comparing students in LSW courses with those not, students in LSW courses reported significantly greater mindfulness and psychological well-being. 47
Several currently implemented medical school wellness programs geared towards addressing medical student burnout are comprised of peer-directed interventions. Approaches vary and range from a focus on low-cost mentorship between peers for emotional support to promoting student participation in exercise events for physical well-being to peer-assisted learning to boost academic performance and reduce test-taking anxiety.30-36 Of the studies focused on peer-directed interventions that were examined in this scoping review, all reported positive student mental health outcomes.30-36 These included reduced student anxiety and stress, development of better coping mechanisms, and a stronger work-life balance. In addition, peer-directed approaches not only foster a sense of community but also are easy and cost-effective for institutions to implement. Examining peer-support programs across the nation, similar impacts of peer interaction on student well-being are seen. At one university in the Western United States, students who reported a greater frequency of speaking with their peers in their second year, particularly about challenges they experienced in school, reported higher self-perceived competence regarding academic performance even years later in their senior year. 48 Another study of undergraduate students located at a liberal arts college in the Midwest, found that students’ everyday interactions with peers contributed to more positive beliefs of academic self-efficacy. 49 In comparison to their peers, self-efficacious students have been shown to often adopt more challenging goals, illustrate more resilience, and experience lower levels of stress, anxiety, and depression in the face of academic difficulties, thus underscoring the value of peer interaction. 49
This scoping review examined several faculty-directed approaches to improving burnout and well-being among medical students. The approaches ranged in focus from institutional initiatives to clerkship-specific interventions to mentorship/coaching sessions. Institutional initiatives were found to reduce burnout and perceived stress, while clerkship-specific interventions contributed to improvements in students’ mental well-being. Mentoring and coaching was found to depend largely on appropriate training for efficacy. Faculty mentoring has also been shown to have a strong impact among nursing students who, across several different studies in both the U.S. and abroad, reported reduced levels of stress, anxiety, and depression when participating in mentoring programs in didactic or clinical settings. 50 At the Saint Louis University School of Medicine, rates of depression, anxiety, and stress were significantly lower among medical students who participated in an expanded wellness program comprised of longitudinal, integrated curricular-changes including faculty mentorship. 51 For graduate students, those with positive, high-quality faculty mentoring have been shown to not only have greater levels of positive mental health and well-being at that time, but also in the years of study following high-quality mentoring. 52
Based on findings from the literature, we propose solutions to the aforementioned barriers identified in this scoping review. Medical institutions can address the lack of diverse approaches by valuing individual preferences and provide more varied types of support in order to reach students of different identities and backgrounds.31,39 For example, students at the Arizona campus of Mayo Clinic Alix School of Medicine noted that wellness curriculums can be more inclusive and well-received by broadening their horizons from more conventional activities associated with wellness, such as yoga and mindfulness, to include those less stereotypically linked, such as book clubs, interest groups, or integration of humanities within the core curriculum. 18 To combat a dearth of appropriately trained faculty and a lack of clarity in goals, mentoring programs should be well-structured and consider use of professional coaches.41,42,53,54 Additionally, wellness initiatives can outline specific goals and strategies to promote efficiency, particularly with social events.30,31
To better assess program efficacy and develop strategies for improvement, programs can better evaluation methods and promote regular data collection regarding wellness program methods, barriers, and successes.14,34 One program at the Frank H. Netter School of Medicine is considering using an objective structured clinical examination format to assess students’ counseling skills with standardized patients after Lifestyle Medicine and Student Wellness sessions, thus allowing facilitators to determine how well students can apply the skills they learn without relying solely on self-perceived knowledge. 55 Programs can also increase student participation in wellness-centered activities by increasing flexibility and reducing stressful mandatory events.40,42,44 To address students’ time constraints, the Frank H. Netter School of Medicine found that delivering their wellness content in a scheduling gap when students did not have competing clinical responsibilities resulted in greater program engagement. 55 Schools such as the University of Missouri have also worked to increase student buy-in via the implementation of a mandatory wellness orientation for first-year medical students to decrease stigma and increase recognition of the importance of early intervention for mental well-being. 56
Although there exist various examples of wellness approaches to improve medical student burnout, institutions continue to face barriers to implementing such interventions. From the student perspective, barriers include time constraints, fatigue, and stigma around seeking help, all of which limit student participation in wellness programs (Table 2). Major institutional barriers encountered towards implementation of such programs include one-size-fits-all approaches that fail to address individual concerns, lack of clarity in program goals, and limited availability of appropriately trained faculty (Table 2). Among those with implemented programs, there remain barriers such as response bias towards appropriate evaluation of program efficacy. An additional major institutional barrier to implementing wellness programs includes financial constraints. A study surveying 32 medical schools across the U.S. found that institutional budgets for wellness activities were typically small, and only 26% of institutions surveyed used funds towards evaluating the efficacy of their wellness programs. 14 In another survey of wellness programs across the U.S. and Canada, 45 of 86 institutions (52%) reported a lack of financial support as a barrier to further developing their wellness program, making it the most reported barrier in the study. 57 Of the 7 surveyed schools that did not have a wellness program already in place, nearly 30% reported that inadequate financial support as a barrier to creating one and 57% cited insufficient administrative support as an addition barrier for the same. 57 This extends beyond the individual institution to encompass a lack of not only sustained funding for wellness programs, but also for increased research in this area. Of the limited studies that exist on this topic, researchers frequently highlight the importance of an iterative process and emphasize the need for medical schools to routinely monitor student well-being and assess the impact of new wellness programs. 51 Recommended areas for further research include randomized control trials to assess efficacy of wellness interventions, more approaches focused on psychological domains of well-being, and longitudinal studies to assess long-term impacts of interventions—all of which will require according funding. 19
Limitations
Our scoping review was limited in that, while we conducted a comprehensive search of the literature through three databases, only 20 articles met our inclusion criteria. This is in part due to the fact that our review was limited to articles in only these three databases and did not encompass tracing of reference lists, gray literature, manual searches of journals, or published scientific reports. An additional limitation is that since a remaining 65% scored an average or low score in terms of rigor, generalizability of results might be limited by the quality of evidence in drawing conclusions for future studies. This highlights a need for larger amounts of research in this area, which can be further accomplished by additional training and staff in U.S. medical colleges to identify and address medical student burnout at early stages for effective intervention.
Conclusion
In a time of increasing anxiety and depression amongst medical students specifically, the need for institutional support and student wellness programs is greater than ever. The findings of this study will inform the future development, dissemination, and implementation of innovative wellness programs to improve rates of burnout among medical students. Our findings also highlight the role of peers and faculty in addressing medical student burnout, as well as strategies for their successful integration in such programs. Further research in this area is needed to assess the efficacy of existing wellness programs by means beyond student self-perceptions. As research continues in this track and institutions improve their evaluation of student wellness and wellness programs, a call for increased attention and funding to this matter is imperative to better the mental health and overall well-being of our medical students.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
