Abstract
Cardiovascular disease presents a ten-fold higher risk of death than suicide in individuals with serious mental illness. Individuals experiencing first-episode psychosis already have high rates of modifiable risk factors contributing to cardiovascular disease. The initial 12 months are crucial for implementing behavioral interventions for effective risk factor modification and disease prevention. Coordinated Specialty Care (CSC) outpatient clinics provide multi-disciplinary team-based treatment for teens and young adults in the early stages of psychotic illness, significantly improving mental health outcomes and quality of life. However, these clinics lack support for addressing lifestyle behavior changes in their clients. The North Carolina Healthy Active Living (NC HeAL) program is an innovative clinical service offered to all CSC clients in this state. It offers personalized health and wellness coaching to help clients achieve meaningful health improvements. This paper provides a detailed description of the program’s development, the target population and setting, the roles and skills of the NC HeAL team, program components and evidence-based program measures. Results of program measures, feasibility, acceptability, implementation, and fidelity will be published separately.
“The overarching goal of NC HeAL is to enhance the health and quality of life for individuals with Severe Mental Illness (SMI).”
Highlights
• People with psychotic disorders die 20 to 30 years prematurely, largely due to chronic physical health conditions like respiratory disorders, cardiovascular disorders, and Type II Diabetes Mellitus. • Teens and young adults experiencing their first psychotic episode already have multiple risk factors for these chronic physical health conditions. • Improving nutrition, increasing physical activity, and stopping smoking are the established treatments for early intervention of these conditions. • Coordinated Specialty Care clinics are the logical location to address these lifestyle challenges, utilizing the specialized training of board-certified health coaches.
Introduction
Individuals with serious mental illness (SMI) have a life expectancy 20 to 30 years shorter than those without SMI. 1 Cardiovascular disease confers a ten-fold higher risk of death than suicide in people with SMI and they have a four-fold elevated risk of developing metabolic syndrome.2,3 Obesity and smoking are modifiable risk factors for these conditions, that can be reduced with the targeted interventions. Individuals with SMI are more sedentary compared to matched controls, consume diets of poorer quality, and have higher rates of smoking.4-6 By providing education, coaching, and resources that promote regular physical activity, healthy food choices, and smoking cessation, we can improve the health and quality of life for individuals with SMI.
First-Episode Psychosis
First-episode psychosis (FEP) describes individuals in the initial stages of a psychotic illness. 7 Unfortunately, these individuals already have high rates of all the modifiable risk factors that contribute to early and excess mortality. Nearly half of FEP individuals are overweight or obese, and body mass index (BMI) increases dramatically over the first months and years of treatment.8-10 This can be attributed to the adverse metabolic effects of antipsychotics and other psychiatric medications as well as suboptimal eating habits and sedentary behavior.8,11-13 Psychotic illnesses such as schizophrenia and schizoaffective disorder are typically life-long conditions, and the metabolic consequences of medications and suboptimal habits are expected to persist if not addressed.14,15
Coordinated Specialty Care Clinics
In 2008 the National Institutes of Mental Health (NIMH) launched the Recovery After Initial Schizophrenia Episode (RAISE) research project finding that a multimodal interdisciplinary approach to treating clients in the early years of psychosis was more effective than standard community care. This enhanced treatment program, known as NAVIGATE, is the model for over 50 early psychosis clinics in the United States. 16 These clinics, called Coordinated Specialty Care (CSC), offer a range of evidence-based interventions within a recovery-oriented and shared decision-making framework for teens and young adults in the first years of a psychotic illness.17,18 Individuals who receive CSC services experience significantly improved mental health outcomes and quality of life. 19
The NAVIGATE model acknowledges the need to address the client’s physical health in addition to their mental well-being, however few resources are directed towards physical health. Engaging in physical exercise, adopting a healthy diet, and quitting smoking have all proven beneficial to those with psychosis. 20 An emerging body of evidence suggests behavioral lifestyle interventions for teens and adults with SMI can help mitigate body weight gain, improve cardiometabolic risk factors, and increase physical activity (PA).21,22 These interventions must start early and be integrated into long-term treatment for the benefits to be sustained. 23 Importantly, increases in PA among FEP clients is associated with less weight gain and reductions in waist circumference 24 as well as improvements in cognition, positive and negative psychotic symptoms, and global functioning.25,26 Individual and group-based PA programs are acceptable, feasible, and effective for FEP populations.25-27
Coordinated Specialty Care clinics (CSCs) are the logical centers to support lifestyle behavior change among FEP clients to decrease early mortality risk factors before medical complications develop. Clinical guidelines increasingly recommend assessing nutrition, physical activity, and smoking status alongside weight and blood markers of metabolic status to assess current physical health and risk for future physical health problems. 27 Therefore, it is crucial that CSCs develop the expertise to offer lifestyle interventions to all FEP clients when they enter treatment. If interventions are applied only after significant weight gain or changes in metabolic markers, any intervention will be much more challenging. 28
This paper provides a description of the development of North Carolina Healthy Active Living (NC HeAL) situated in the CSC programs of this state. This paper describes the target population and setting, the roles and skills of NC HeAL team members, evidence-based program measures, and program components. Results of program measures, program feasibility and acceptability, program implementation and fidelity, and implementation lessons learned will be published separately. The University of North Carolina Institutional Review Board determined that this paper is a secondary analysis of de-identified data, was not human subject research, and thus did not require institutional review board review.
NC HeAL Program
Prior to the implementation of the NC HeAL program, the CSC teams of North Carolina lacked necessary knowledge and manpower to address the range of unhealthy lifestyle habits of their clients. The NC HeAL project provides coaching expertise that identifies these unhealthy lifestyle factors in a client-centered manner and addresses them accordingly.
The NC Healthy Active Living program receives funding from NC SAMHSA through a block grant to promote physical health and support healthy lifestyles for FEP clients receiving services at North Carolina CSCs. The first years of treatment for a psychotic illness are crucial for symptomatic and functional recovery. NC HeAL believes that improving physical fitness and health is just as important.
NC HeAL offers personalized health and wellness coaching to help clients improve their health. Detailed nutrition assessments, education, and treatment planning are available. Furthermore, wellness education is provided to family members and clinic staff to emphasize the importance of physical health in recovering from a psychotic illness.
Target Population and Setting
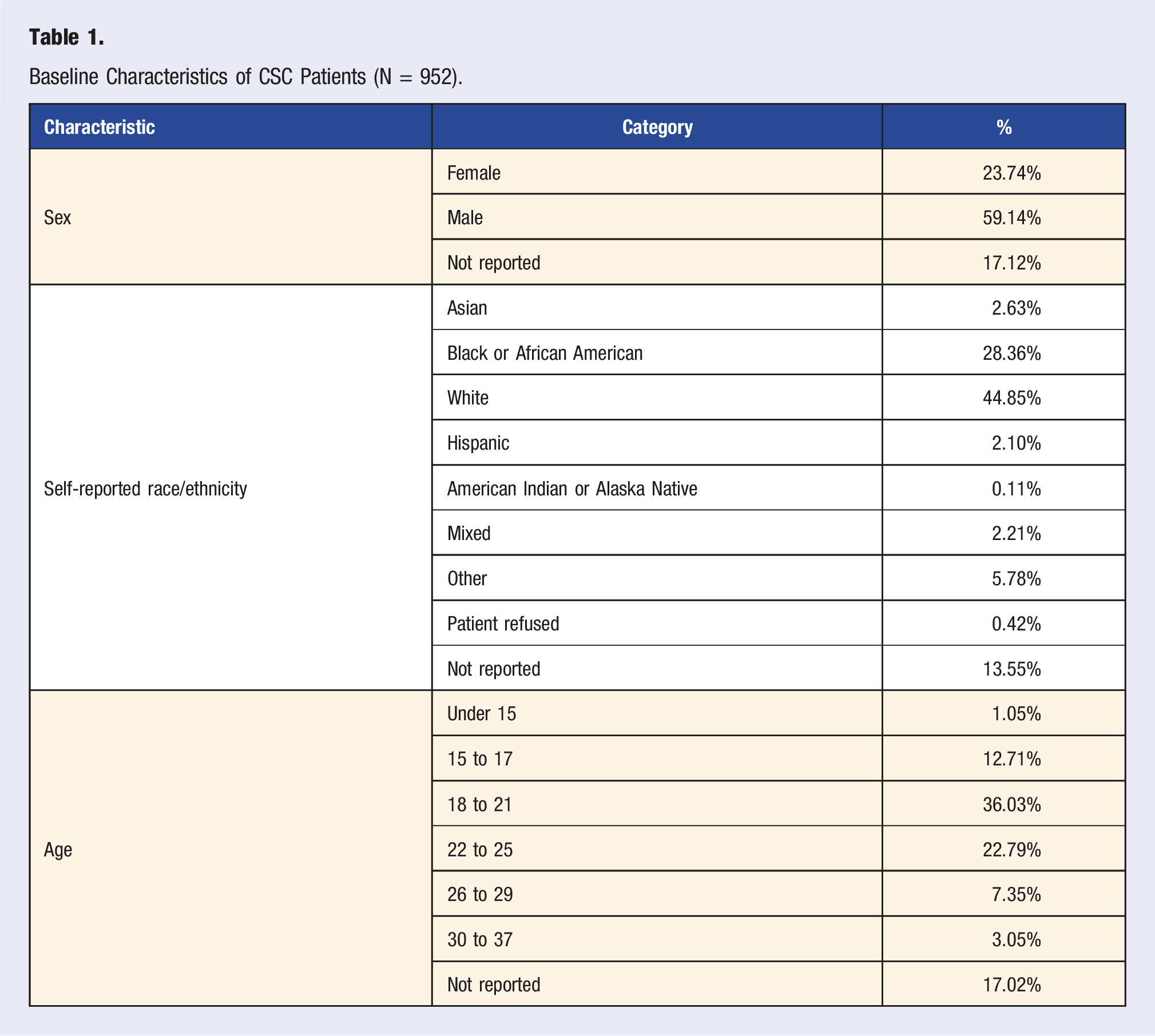
Individuals enrolled in the NC HeAL program receive psychiatric services from any of the six NC CSCs, are between the ages of 14 and 35, and are in the first 5 years of their psychotic illness. Among the NC CSC population, over half identify as male (59%) and the majority self-report as White (45%) or Black (28%).
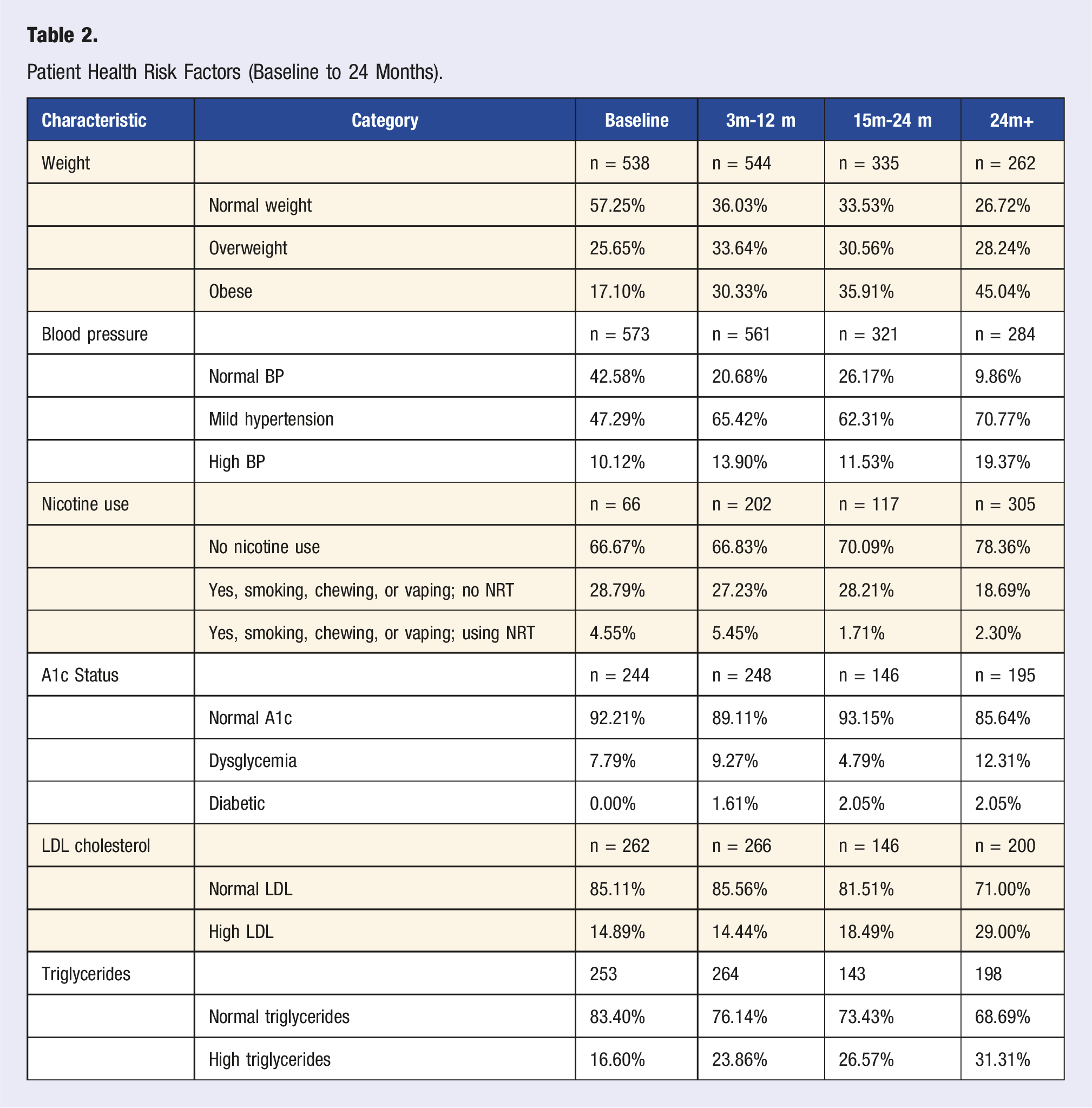
At entry into the NC CSC, nearly half the individuals are overweight (26%) or obese (17%). Published findings report that clients with FEP experience significant weight gain in the first 12 weeks of starting antipsychotic medication, with a mean increase of 8 kg. 29 Importantly, the first year is the critical period for developing metabolic abnormalities as up to 80% of the weight gained at three years occurred during this period. 30 Recent data from NC CSC clients (Table 2) supports this finding.
Baseline Characteristics of CSC Patients (N = 952).
Patient Health Risk Factors (Baseline to 24 Months).
NC HeAL Team
The psychiatrist on the team is medical director of one of the NC CSC clinics and has worked with the FEP population for 20 years, has a Fellowship in Integrative Medicine and is a Tobacco Treatment Specialist.
The program manager serves as a liaison between the NC HeAL team, EPI-NC, additional EPI-NC programs, and the CSC clinics. She is also responsible for budget management and purchases along with developing health communication materials and website maintenance.
The health coach is a National Board-Certified Health and Wellness Coach (NBCHWC) with over 10 years of professional coaching experience. Additionally, she is an ACE certified personal trainer, behavior change specialist, and diabetes prevention program (DPP) lifestyle coach.
The registered dietitian on the team holds a master’s degree in public health nutrition and is registered with the Academy of Nutrition and Dietetics. She has over 10 years of experience working with clients and families in psychiatric settings.
A public health doctoral candidate serving the team is a nationally certified personal trainer (ACE) and an experienced project manager on randomized controlled trials investigating energy expenditure, clinical exercise testing, and biometric assessments.
NC HeAL Program Framework
The design of the NC HeAL program is guided broadly by three frameworks; shared decision-making, human centered design, and social cognitive theory, as described below. The services provided at the individual client level are determined by their medical history, stage of behavior change, and life development stage.
Shared Decision-Making
Shared decision-making (SDM), described as health care providers and a client working together to make health care decisions, is an effective framework for empowering FEP clients.31,32 SDM uses evidence-based information about available options, the provider’s knowledge and experience, and the client’s values and preferences. 33
Human Centered Design
Human centered design (HCD) is a humanizing, iterative, and creative approach to addressing challenges. 34 It is a framework that involves the human perspective at every stage of the design process. 35 In health care, HCD positions clients as active participants in designing a program that responds to their needs by listening and learning from their lived experiences.36,37
Social Cognitive Theory
The NC HeAL program is guided by the evidence-based Social Cognitive Theory (SCT) 38 that promotes self-management behavior (e.g., adopting a healthy lifestyle) through self-regulating cognitive processes. 39 Extensive evidence supports the use of SCT in behavioral lifestyle interventions demonstrating moderate effect sizes for nutrition and PA improvements.40-43 Accordingly, SCT domains, social support, self-efficacy, self-regulation, and outcome expectations, have been selected as the targeted mechanisms of action (MOA) to improve risk factors among clients44-46; all four of which are significant MOA for positive lifestyle behaviors broadly in young adults and among FEP populations.40,47-50
Clinic Sites
The NC HeAL program is offered at the six CSC sites across North Carolina. As of September 2024, these sites collectively have an active census of 203 FEP clients. Each site has its own distinct population needs and demographic diversity. As a result, providing customized services and resources to each clinic based on the clinic leadership’s perception of the needs hierarchy and client and family requests is essential for effective program success.
Meeting and Communication Format
Weekly NC HeAL development team meetings began in the Fall 2021 and are held via an online meeting platform.
Development Phase
All development phase activities were conducted with the following goals; (1.) establish continuous mutual learning and communication between NC HeAL program team, subject matter consultants, and FEP clients, (2.) develop, prototype, and test program measures, and (3.) obtain guidance on program feasibility and meaningful results. Program refinement came directly from this phase which allowed for tailoring of program material based on feedback from key informant interviews (n = 6). Key informants included clinical researchers, implementation scientists, and an exercise physiologist. Final decisions on program materials, measures, and meaningful results were decided collectively among the team from an extensive literature review and acceptability testing among a small sample (n = 28) of FEP clients.
Implementation Phase
A phased roll out began across sites in the fall of 2023. NC HeAL project personnel attended CSC clinical meetings to introduce the initiative and encourage referrals. During both the 2023 and 2024 NC FEP symposia NC HeAL team members presented, tabled, and strengthened informal site relationships. As of October 2024, 75 clients have been referred across all sites.
Program Components
Tailored Lifestyle Health and Wellness Coaching sessions are guided by the framework, guidelines, and session structure as outlined by the National Board of Health and Wellness Coaching (NBHWC). 51 During initial sessions, the coach and client explore the client’s visions, values, and priorities. These initial sessions aim to strengthen client motivation and establish baseline health and wellness. Clients are encouraged to create wellness goals in behaviors they consider ready and able to change. Subsequent sessions build on goal progress with the coach recalibrating the plan as needed. A strong emphasis is placed on helping the client reflect on their experiences, while also providing accountability, resources, and support. 52 The coaching support is ongoing and frequency of sessions ebb and flow depending on client’s preferences.
Coaching sessions are documented in the electronic health record (EHR), as an account of coach and client discussion topics, client goals, and assessment results, for the client’s information and to aid communication with the client’s clinical team. Appointments are held over HIPPA compliant Zoom platform. On average, sessions last 30-minutes with varying lengths and frequency depending on client preferences.
Family Education and Support are provided through NC HeAL team presentations at multi-family group meetings. Additionally, a family member is welcome to join any coaching session with the client’s permission.
Evidence-Based Measures and Outcomes
The purpose of the NC HeAL program is to promote and increase healthy lifestyle behaviors by a clinically meaningful difference (CMD). Mitigation of the expected increase in body weight and the accompanying metabolic consequences associated with the initiation of FEP treatment will also be considered meaningful. 53 The following lifestyle behavior measures are collected at baseline, and 3-months intervals except as noted differently, by a NC HeAL health coach or psychiatrist.
Lifestyle Behavior Measures
Physical activity readiness will be determined by the 7-item Physical Activity Readiness Questionnaire (PAR-Q+). Collected only at baseline, the PAR-Q+ aims to uncover health conditions that would require physician clearance prior to the client starting an exercise program. 54 Given the nature of the present program, the PAR-Q+ is recommended instead of requiring a physical exam for all participants. 55
Mediterranean Dietary Adherence will be assessed by a previously validated 11-item adapted Mediterranean Diet Screener which assesses southern U.S. Mediterranean diet quality and adherence. 56 This instrument has been widely accepted and validated across multiple randomized clinical trials in North Carolina, ensuring its applicability and cultural relevance for the local population. 57 It assesses the frequency of servings and dietary behaviors. Scores will be reported as total score and as low (0-4), moderate (scores 5-7) and high (scores 8-11). A higher score is considered higher diet adherence. Notably, others have demonstrated that individuals with high Mediterranean diet adherence have a lower prevalence of estimated 10-year cardiovascular risk compared to those with low adherence. 58
Physical activity levels will be estimated by the validated short form version of the International Physical Activity Questionnaire (IPAQ-SF) and via minutes of PA data collected in the Fitbit app for clients who choose to engage with the device.59-61 Improvements in PA, such as transitions from low to moderate or high activity levels, will be regarded as the CMD for the IPAQ-SF, as will an increase of 2000 daily steps for those using the Fitbit.62-64 Nicotine dependence will be assessed by the 6-item Fagerstrom Test for Nicotine Dependence. A higher score is considered higher dependence. Notably, an increase of one unit at baseline decreases the odds of abstinence at 6-months by 11%. 65 6-months of continuous abstinence at the individual level and achieving this outcome in 7% of total program clients will be considered the CMD for the program.66,67
The previously discussed MOA (social support, self-efficacy, outcome expectations) and program satisfaction will be measured from an adapted 6-item ecological momentary assessment (EMA-6) that was created for the program from previously validated and reliable scales.68-71
Clinical Measures
The following measures will typically be collected in clinic by certified medical assistants, with a small percentage obtained as self-report in situations where in-person collection is not feasible. Vital signs will be collected every 3-months and labs collected every 12 months.
Body weight will be measured to the nearest 0.1 kg on electronic scales calibrated yearly. 72
Height will be measured using a wall mounted stadiometer to the nearest 0.1 cm.
Body mass index (BMI) will be calculated as: body weight in kilograms divided by height in meters squared. 73
Blood Pressure (BP) will be measured in the client’s preferred arm with a sphygmomanometer after a 5-minute rest with the client seated comfortably with feet on floor and arm supported. Blood pressure will be categorized as per ACA/AHA 2017 guidelines. 74 Data from both observational and randomized studies have demonstrated that decreases in Systolic BP of 5 and 10 mm Hg are associated with 10% and 20% reductions respectively in cardiovascular disease events, independent of comorbidities. 75 As such, a mean difference in BP of at least 5 to 10 mmHg for Systolic BP compared with baseline, or 3 to 5 mmHg for DBP, may be considered a CMD. 76 Importantly, CMD for BP is not anticipated without a reduction in body weight. 77 Two kg of weight loss at 6-months has been reported to induce a reduction of 3.7 mmHg for systolic and 2.7 mmHg for diastolic BP. 78
Lipids and hemoglobin A1c will be measured in the non-fasting state via blood draw, collected and analyzed per clinic standard of care. For hemoglobin A1c, a 0.5% decrease will be considered a CMD.79,80 For lipids, any reduction from an elevated level to below the upper limit is a CMD. Short-term change in lipids are unlikely without weight loss; for cholesterol, a reduction of 1.3% per kg lost is expected, and for triglycerides a 1.6% reduction per kg lost is anticipated. 81 Notably, recent literature suggests that intensive nutritional interventions can lead to improvements in blood pressure, fasting blood sugar, and triglycerides in as little as 24-48 hours, even without significant weight loss.82,83 While this study does not involve an intensive treatment protocol, it is important to acknowledge that nutrition-focused approaches can contribute to short-term metabolic improvements.
Conclusions
Individuals recently diagnosed with a psychotic disorder frequently have unhealthy lifestyles, contributing to metabolic problems, chronic physical conditions, and premature death. Despite this, there are few programs promoting healthy lifestyles in this population.80-82 NC HeAL is a novel service of the North Carolina Coordinated Specialty Care clinics which delivers evidence-based education, coaching, and resources to clients experiencing first-episode psychosis (FEP) to empower them to make healthier food choices, increase physical activity, and quit smoking. Through personalized coaching the program will tackle the specific challenges clients face when pursuing these lifestyle goals during the early stages of a psychotic illness.
The overarching goal of NC HeAL is to enhance the health and quality of life for individuals with Severe Mental Illness (SMI). If this goal is attained with program measures demonstrating beneficial lifestyle changes and improvements in risk markers of chronic disease, then the NC HeAL program will be addressing an important gap in care. Additionally, all program components have been developed with future dissemination in mind. We anticipate that the program materials will be both feasible and well-received for implementation in future FEP programs.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Early Psychosis Interventions of North Carolina (EPI-NC) is funded by the NC Division of MHDDSA and supports NC First-Episode Psychosis Coordinated Specialty Care (NC-CSC) Programs. Federal Community Mental Health Services Block Grant (CFDA #93.958).
Ethics Approval
The University of North Carolina Institutional Review Board determined that this is a secondary analysis of de-identified data, was not human subject research, and thus did not require institutional review board review.
