Abstract
Introduction: Healthcare providers play a crucial role in promoting sexual health among older adults, an important yet often neglected aspect of aging well. Although sexuality evolves beyond the reproductive years, it remains a meaningful part of life for many. Despite the natural decline in sexual activity with age, numerous older adults continue to value and engage in fulfilling sexual relationships. Unfortunately, targeted interventions to support later-life sexuality are lacking, creating gaps in care. Intervention: Sexuality in older adults is influenced by biological, psychological, and social factors. Clinicians should include comprehensive sexual health assessments, including STI screenings, as part of routine care. Providing age-appropriate sexual education and resources helps promote lifelong sexual wellness. Open communication between healthcare providers and patients is vital for addressing sexual concerns, often left unspoken due to stigma or discomfort. Additionally, adopting lifestyle medicine principles—such as balanced nutrition, regular exercise, stress management, and social connection—can enhance sexual health and overall well-being. Conclusion: Specialized training for healthcare professionals on the unique aspects of older adult sexuality is essential to bridge knowledge gaps. A holistic, evidence-based approach will empower providers to better support the evolving sexual health needs of older adults, improving their quality of life.
“Advancing research, education, and clinical training in this area will ensure that sexuality is recognized as a vital component of holistic, age-inclusive healthcare.”
Introduction
The combination of increased life expectancy and the aging Baby Boomer generation has led to an unprecedented global surge in the older adult population. In 2021, the U.S. Census Bureau reported that 55.7 million Americans were aged 65 or older, accounting for 17% of the total population. By 2050, this number is expected to rise to 83.7 million. 1 Globally, the population of individuals aged 65 and older is projected to reach 1.6 billion by 2050.2,3 This demographic shift highlights the critical need for a deeper understanding of the factors that promote adaptation and well-being in older adults. Such insights are essential for shaping healthcare practices and policies to meet the evolving needs of this growing population.
Aging is characterized by “progressive physiological changes in an organism that lead to senescence, resulting in a decline in biological functions and the organism’s ability to adapt to metabolic stress.” 4 As people age, the prevalence of age-related illnesses rises, leading to increased socio-economic costs. This has prompted scientists, healthcare organizations, and clinicians to focus on strategies to reduce late-onset diseases and enhance the quality of life in older adults. One key yet often overlooked factor contributing to well-being in this population is sexuality.5,6
Despite its importance, there is a significant lack of empirical research on sexuality and its influence on quality of life among older adults, especially women. Evidence supporting effective interventions and strategies remains limited. 7 This research gap may be attributed to cultural norms that emphasize youth in discussions of sexuality, alongside a common misconception that aging is inherently linked to asexuality. 8 However, there is a growing need to better understand the sexual needs of older adults, particularly as rates of sexually transmitted infections (STIs) and HIV are increasing in this demographic due to inadequate awareness and prevention measures. 9
The sexuality of older adults is shaped by a complex interplay of biological, psychological, social, and cultural factors. This review offers a comprehensive examination of the determinants of sexuality in later life and identifies effective interventions for improving patient care. By delving into the multifaceted influences of sexuality in older adults, healthcare providers can gain a deeper understanding of these dynamics and adopt strategies that support and enhance the well-being of their older patients. Addressing the sexual needs of this population can yield significant benefits, influencing not only individual patient outcomes but also advancing education, research, policy development, and clinical practices.
Dimensions of Sexuality
Sexual health cannot be fully defined, understood, or effectively addressed without considering the broader concept of sexuality, which serves as the foundation for key behaviors, attitudes, and outcomes related to sexual well-being. The working definition of sexuality is: “… a central aspect of being human throughout life encompasses sex, gender identities and roles, sexual orientation, eroticism, pleasure, intimacy, and reproduction. Sexuality is experienced and expressed in thoughts, fantasies, desires, beliefs, attitudes, values, behaviors, practices, roles, and relationships. While sexuality can include all of these dimensions, not all of them are always experienced or expressed. Sexuality is influenced by the interaction of biological, psychological, social, economic, political, cultural, legal, historical, religious, and spiritual factors.”
10
Following is a breakdown of the four dimensions of sexuality (Figure 1). Dimensions of sexuality in public health.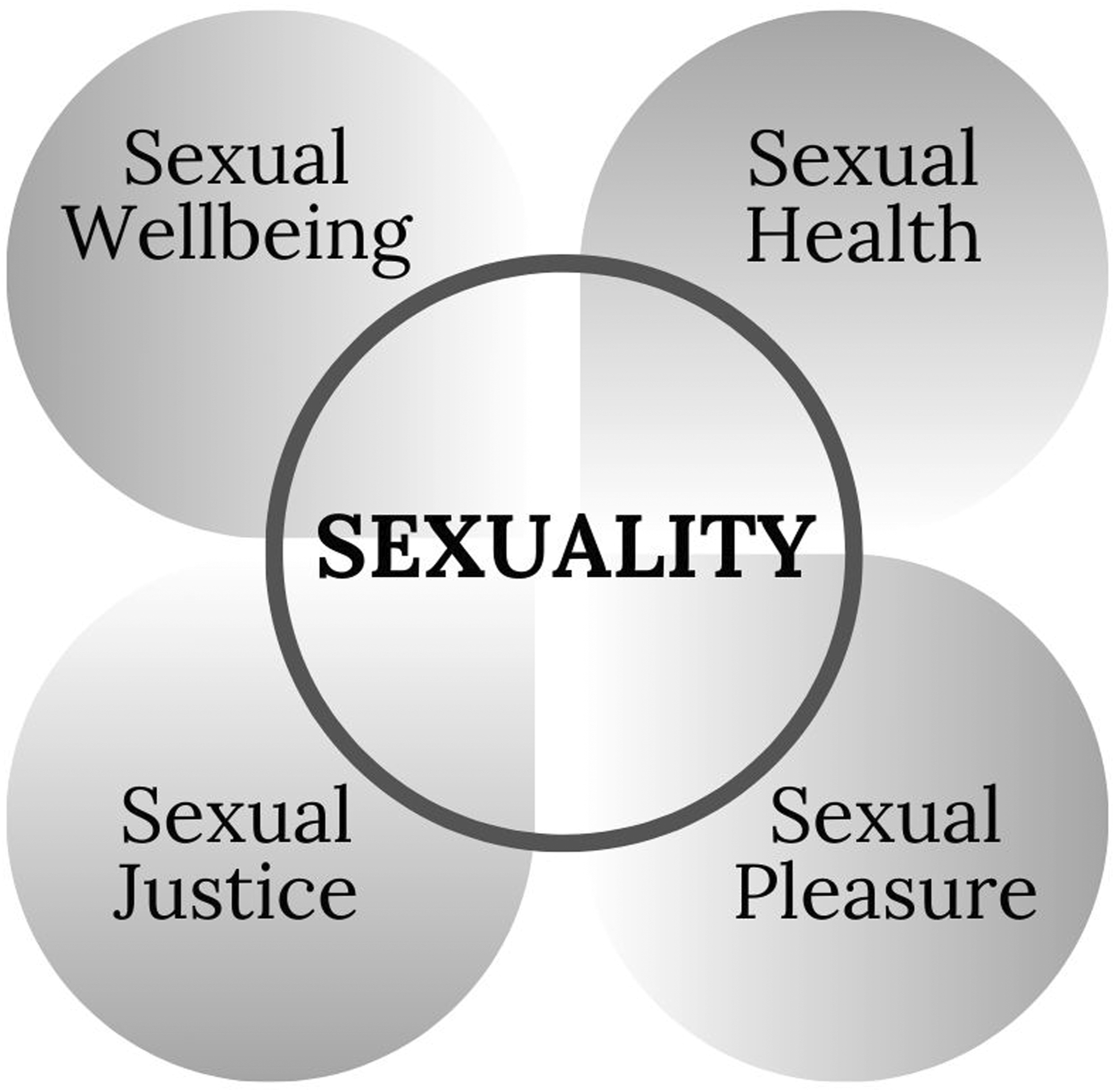
Sexual Health
Sexual health is a lifelong concern described by WHO 10 as “a state of physical, emotional, mental and social well-being about sexuality; (…) not merely the absence of disease, dysfunction or infirmity. Sexual health requires a positive and respectful approach to sexuality and sexual relationships, as well as the possibility of having pleasurable and safe sexual experiences.” Sexual health promotes safe and consensual sexual experiences. It includes access to sexual health services (such as STI testing), sexual education, and the ability to make informed decisions about one’s sexual life. This dimension of sexuality ensures that individuals have the knowledge and resources to engage in sexual activities safely and responsibly.
Sexual Well-Being
Sexual well-being encompasses a comprehensive sense of satisfaction and fulfillment in one’s sexual life, extending beyond the mere absence of illness. It embraces a positive, respectful, and enjoyable approach to sexuality and sexual relationships. Critical aspects of sexual well-being include emotional and psychological satisfaction, self-esteem, sexual self-respect, comfort with one’s sexuality, and the cultivation of healthy relationships. It also involves self-determination and resilience in navigating sexual experiences. 11 Sexual well-being significantly contributes to overall life satisfaction and quality of life, recognizing the vital role of sexual expression and intimacy in human happiness and connection.
Sexual Pleasure
Sexual pleasure is the physical and emotional enjoyment derived from engaging in sexual activities, highlighting the positive and gratifying dimensions of sexual experiences. It encompasses various aspects such as arousal, orgasm, and overall sexual satisfaction, recognizing these elements as integral to a healthy and fulfilling sexual life.12,13 Sexual pleasure is a fundamental aspect of human sexuality, playing a crucial role in emotional well-being and the quality of personal relationships. Its importance extends beyond individual gratification, fostering deeper intimacy and connection within human interactions, ultimately contributing to a more enriched and balanced life.
Sexual Justice
Sexual justice entails the equitable treatment and recognition of all individuals’ sexual rights and freedoms. It highlights the importance of dismantling societal barriers and eradicating discrimination that hinders individuals from fully realizing these rights. This concept includes combating sexual violence, addressing discrimination based on sexual orientation or gender identity, and advocating for comprehensive sexual rights. 14 By fostering an inclusive and respectful society, sexual justice aims to create an environment where everyone can equally enjoy their sexual rights and freedoms.
Sexual Activity Among Older Adults
Research shows that the later years can still be full of passion. According to the National Social Life, Health, and Aging Project, many older adults continue to enjoy an active sex life. Approximately 73% of individuals aged 57–64, 53% of those aged 65–74, and 26% of adults aged 75–85 report being sexually active. 15 An investigation on sexual activity and sexual satisfaction among adults aged 60 and older found that among all participants, 46% were sexually active, with men (55%) reporting greater sexual activity than women (40%). Sexual activity and sexual satisfaction were found to be positively associated with self-reported health conditions and cohabitation. 16 A recent AARP survey of older adults in the United States found that 67% of respondents reported having a regular sexual partner. However, this figure diminishes with age. Among individuals aged 40–49, 79% reported having a consistent sexual partner, while the percentage drops to just 53% for those aged 70 and older. 17
Research on sexual activity and sexual satisfaction among unmarried and unpartnered older adults is relatively under-explored. One notable study revealed that women who were married or cohabitating had approximately eight times the likelihood of being sexually active compared to their unpartnered counterparts. Specifically, among women aged 60 and older, 67% of those in romantic partnerships reported being sexually active, whereas only 13% of unmarried or non-cohabitating women reported the same. The study also found that women who placed greater importance on sex were more likely to engage in sexual activity. Additional factors correlated with sexual activity included the absence of chronic health conditions, younger age, and a lower body mass index. Sexual satisfaction was significantly higher among sexually active women than among sexually inactive women. 18
Sexual Satisfaction Among Older Adults
A fulfilling sex life is a fundamental component of overall health and happiness, significantly influencing intimate relationships and contributing to quality of life.19-23 Research has even demonstrated that engaging in sexual activity can contribute more to happiness than an increase in income. 24 Data indicates that 82% of Americans aged 18–96 believe that sex is essential for happiness in a relationship. 25 Another study found that men and women over age 65 who reported any sexual activity in the past year had significantly higher mean enjoyment of life scores compared with those who were not sexually active. 26 Older individuals who engage in sex more frequently report higher levels of happiness and satisfaction.27,28 Interestingly, data suggests that satisfaction with one’s sex life peaks in the mid-to-late 30s and begins to decline after the age of 70. 5 These findings underscore the importance of addressing sexuality as a vital aspect of holistic well-being across the lifespan.
An investigation by Penhollow and colleagues utilized a sample from The Villages, the largest active retirement community for individuals aged 55 and older in the United States. The results indicated that more frequent sexual behavior, less incidence of chronic health conditions, and more significant perceived locus of control were associated with increased overall sexual satisfaction among all participants. 29 A comprehensive study of U.S. adults found that 62% of men and 43% of women considered sexual health and satisfaction critical to their overall quality of life. Those in excellent health reported notably higher levels of sexual satisfaction compared to individuals in fair or poor health. 30 This underscores the strong link between physical well-being and sexual fulfillment, indicating that health plays a more pivotal role than age in determining sexual satisfaction. The findings suggest that prioritizing good health can significantly enhance sexual well-being, particularly as people age, reinforcing the connection between physical health and a satisfying sex life throughout the lifespan.
Male Sexual Dysfunction
Erectile dysfunction (ED) is a considerable health problem of global proportions, affecting up to 30 million men in the United States and 150 million men worldwide. It is reported that 40% of men between 40 and 70 years of age experience some form of ED. 31 Data from the U.S. National Health and Nutrition Examination Survey (NHANES) indicates that the prevalence of ED increases from about 5% in men aged 20–39 years to 15% in men aged 40–59 and to 70% in men aged 70 years and older. 32
Starting around age 30, men experience a gradual decline in testosterone levels, leading to decreased libido, reduced sperm production, and erectile dysfunction (ED). ED, characterized by the inability to attain and maintain sufficient penile rigidity for sexual intercourse, can lead to significant emotional and psychological consequences. Men affected by ED may experience withdrawal from sexual intimacy, poor self-esteem, depression, and anxiety. Additionally, ED can negatively impact work productivity, reduce sexual satisfaction, and lower overall quality of life for the affected individuals and their partners. 33
Pharmacological treatments for ED include Sildenafil (Viagra), Vardenafil (Levitra), and Tadalafil (Cialis). These medications provide symptomatic relief by enhancing erectile function but do not address the underlying causes of ED. 34 As the field of sexual medicine continues to advance with scientific and technological progress, further developments in ED management are anticipated, offering hope for more comprehensive treatment options in the future.
Female Sexual Dysfunction
For women, hormone production decreases dramatically with age, typically occurring in the late 40s to early 50s. Menopause leads to a significant reduction in estrogen levels, which can cause reduced libido, lower sexual desire, and hypoactive sexual desire disorder (HSDD). The prevalence of HSDD varies across age groups in the United States, with rates of 8.9% in women aged 18–44 years, 12.3% in women aged 45–65 years, and 7.4% in women aged 65 years and older. Research indicates that sexual dysfunction is more prevalent among women (43%) than men (31%). Factors such as age, education, and poor emotional health contribute to decreased sensation, lack of arousal, and overall sexual dysfunction. 35
Hypoactive sexual desire disorder (HSDD) is a complex and multifaceted condition that profoundly affects women’s sexual well-being. Also known as hyposexuality or inhibited sexual desire (ISD), HSDD is characterized by a persistent lack of interest in sexual activity. 36 For a clinical diagnosis, this lack of interest must cause significant personal or relational distress, distinguishing it from ordinary fluctuations in sexual desire. This critical qualitative aspect helps identify HSDD as a disorder that adversely impacts overall well-being and intimate relationships. 37 Addressing HSDD is essential for improving the quality of life and emotional health of those affected.
Bremelanotide (Vyleesi) and Flibanserin (Addyi) are two FDA-approved medications developed to address HSDD in women. In clinical trials, Flibanserin (Addyi) resulted in an average of only one additional enjoyable sexual experience every 2 months. At the same time, Bremelanotide (Vyleesi) showed no significant increase in the frequency of satisfying sexual experiences. 38 However, other research demonstrated that Bremelanotide (Vyleesi) significantly improved sexual desire and reduced distress related to HSDD in women. 39 These medications provide symptomatic relief but do not cure the underlying condition. Addressing HSDD requires a comprehensive approach that includes psychological support and counseling to mitigate its broader impact on personal and relational well-being. Continued research and development in the field of sexual medicine are essential to improve the effectiveness of treatments and enhance the quality of life for affected women.
Risk Factors for Sexual Dysfunction
Sexual dysfunction is influenced by a variety of well-documented independent risk factors that span physical, psychological, and neurological conditions. Psychological factors, such as depression, anxiety, chronic stress, and low self-esteem, are significant contributors, often impairing sexual desire and performance. Neurological conditions also play a critical role. Stroke, diabetes, Alzheimer’s disease, Parkinson’s disease, multiple sclerosis, and spinal cord injuries can disrupt the brain–body connection essential for sexual function, leading to issues with arousal, sensation, or orgasm. 40
Hormonal imbalances, including low testosterone or estrogen levels, can cause reduced libido and sexual dysfunction in both men and women. Prostate conditions, such as benign prostatic hyperplasia (BPH), as well as the side effects of treatments for prostate cancer—such as surgery or radiotherapy—further complicate sexual health, particularly in men. Chronic pain conditions, such as arthritis, fibromyalgia, and other musculoskeletal disorders, can limit physical mobility and cause discomfort during sexual activity, reducing overall sexual satisfaction. Lastly, cardiovascular conditions—including hypertension, dyslipidemia, and atherosclerosis—affect blood flow and are strongly associated with erectile dysfunction and other sexual health issues. 41
Medications commonly prescribed for chronic conditions—such as antidepressants, antihistamines, antihypertensives, and certain diabetes drugs—can significantly contribute to sexual dysfunction. However, the impact extends beyond medications. Ignoring key principles of lifestyle medicine, such as maintaining a healthy diet, regular physical activity, effective stress management, avoiding substance abuse, getting adequate sleep, and staying socially connected, also plays a critical role in increasing the risk of sexual dysfunction. 41
Relationship dynamics play a critical role in sexual health. Issues related to relationship safety, emotional intimacy, and communication are essential determinants. Individuals who have experienced prior sexual, physical, or emotional trauma, as well as those currently in abusive or unhealthy relationships, are at an elevated risk for sexual dysfunction. These psychological and emotional factors can profoundly affect both desire and performance, complicating sexual well-being further. Addressing these underlying issues is essential for the effective management and treatment of sexual dysfunction. 42
Sexually Transmitted Infections (STIs)
Sexual risk-taking behaviors in older adults, particularly concerning sexually transmitted infections (STIs) such as human immunodeficiency virus (HIV), are an increasing public health concern. This population often lacks sufficient knowledge about STIs and is less likely to engage in safe sexual practices compared to younger generations, putting them at heightened risk. Data from the Centers for Disease Control and Prevention (CDC) reveal that STI rates among U.S. adults aged 65 and older more than doubled between 2012 and 2020. 43 Notably, infections such as syphilis, chlamydia, gonorrhea, and HIV/AIDS have seen significant increases and are expected to rise further as the aging population grows. 44
Healthcare providers need comprehensive training to recognize individuals at risk for STIs and conduct appropriate screenings to mitigate disease morbidity and mortality. Studies show that older adults often do not have sufficient opportunities to discuss their sexual health with medical professionals, which can result in undiagnosed and untreated infections. By incorporating proactive screenings that assess patients’ STI knowledge, providers can foster open and effective communication about sexual health with their older patients. This strategy not only encourages meaningful discussions but also ensures that older adults receive vital educational resources and interventions, promoting safer sexual practices and better overall health outcomes.
Intervention
Pillars of Lifestyle Medicine
Lifestyle medicine emphasizes the importance of healthy behaviors as the foundation of overall health, which is particularly relevant for the sexuality of older adults. The six pillars of lifestyle medicine—nutrition, physical activity, stress management, avoidance of risky substances, restorative sleep, and social connection—are vital for improving the prevention and management of disease, as well as enhancing sexuality.45,46 I. Nutrition: Clinicians should emphasize the importance of a high-fiber, plant-based diet abundant in fruits, vegetables, whole grains, and legumes when advising older patients. This diet is crucial in supporting cardiovascular health, directly influencing sexual function. Such nutrition choices can also help increase energy levels and improve sexual vitality and stamina.47-49 II. Physical Activity: Encouraging older patients to engage in regular physical exercise is essential for maintaining sexual function and overall health. Physical activity enhances blood circulation, improves flexibility, and strengthens muscle tone—all critical to sustaining sexual activity. Better blood flow supports erectile function and vaginal lubrication, while greater flexibility and muscle strength improves comfort and endurance during sexual activities. Beyond the physical benefits, exercise also stimulates the release of endorphins, which alleviates anxiety and depression. This mental uplift has a direct and positive effect on sexual desire and performance, making exercise a powerful tool for holistic health improvement.50,51 III. Stress Management: Clinicians should strongly encourage older patients to incorporate stress-reduction techniques such as mindfulness, meditation, and yoga into their daily routines. These practices have been shown to effectively reduce stress, a common factor that can diminish sexual desire. Fostering healthy social connections and promoting open communication about sexual needs and preferences can further help relieve stress. This holistic approach not only enhances sexual satisfaction but also strengthens emotional intimacy, creating more fulfilling and connected relationships.52-54 IV. Avoidance of Risky Substances: It is essential for healthcare providers to guide older patients toward avoiding harmful substances such as tobacco, excessive alcohol, and recreational drugs, all of which can have adverse effects on libido and sexual performance. Regular consultations are also essential for managing medications, ensuring they do not negatively impact sexual function.55,56 V. Restorative Sleep: Healthcare clinicians should prioritize the role of quality sleep in promoting overall health, particularly in relation to hormonal balance and energy levels. Adequate, restful sleep is essential for regulating hormones like testosterone and estrogen, which directly impact sexual desire and function. Encouraging patients to adopt good sleep hygiene—such as maintaining a consistent sleep schedule, creating a calm sleep environment, and limiting screen time before bed—can improve sleep quality.57-59 VI. Social Connection: Strong social connections are vital for emotional and physical health, including sexual well-being. For older adults, maintaining social engagement creates a sense of belonging and emotional security, positively influencing sexual function and satisfaction. Loneliness and social isolation, on the other hand, are associated with depression, anxiety, and decreased libido.60-63 Healthcare providers should encourage older adults to participate in community activities and social clubs and maintain close relationships with friends and family.
Comprehensive Sexual Assessments
Clinicians, including healthcare practitioners, providers, therapists, and counselors, are uniquely positioned to address sexual concerns and offer essential support to their older patients. By creating a safe and open environment, clinicians can encourage discussions about sexuality, enabling patients to receive the necessary guidance and interventions to improve their overall health. Many older adults are hesitant to seek help for sexual problems even if they significantly impact their quality of life. In one study of patients with ED, 78% had not discussed the issue with their primary care physician, and 82% of these patients said they would have liked the doctor to have initiated a conversation on the topic so they would have felt less embarrassed. 64 Among racially/ethnically diverse women, the majority did not seek professional help with sexual issues due to discomfort and perceptions that older adults were primarily asexual. 65
Data indicates that sexual assessments are frequently neglected in clinical practice, particularly among older adults. A study investigating the sexual history-taking practices of nurse practitioners for patients aged 50 and older involved a random sample of 500 members from the American Academy of Nurse Practitioners (AANP). The findings revealed a concerning trend: only 2% of respondents consistently conducted a sexual history with their patients, while 23% had never or rarely performed such assessments. 66 Moreover, a study of 135 primary care physicians (PCPs) found that discussions about sexuality were notably infrequent. Only 38% of male patients and 22% of female patients had discussed sexual concerns with their physicians. Additionally, 61% of patients reported rarely or never discussing STIs with their PCPs. 67 This highlights a significant gap in sexual assessment among older adults.
These findings underscore the critical need for clinicians to conduct comprehensive sexualassessments to provide holistic care. Such assessments include a detailed sexual medical history, STIs and HIV status, medication use, and evaluation of sexual functioning. Additionally, clinicians should assess sexual activity and related behaviors that may indicate risk, including relationship status, number of sexual partners, frequency of sexual intercourse, injection drug use, types of sexual activities, and history of sexual abuse.
A comprehensive sexual assessment must also include the collection of patients’ sexual orientation and gender identity (SOGI). Gathering SOGI information enables healthcare providers to identify and address specific health disparities faced by lesbian, gay, bisexual, transgender, queer, and similar minority (LGBTQ+) populations. This inclusive approach ensures that the unique needs of these communities are met, fostering a more equitable healthcare environment.68,69
Key elements of a comprehensive sexual assessment.

Practical sexual assessment relies on validated questionnaires and their integration into electronic health records (EHRs) to ensure comprehensive and inclusive care. Key questionnaires include the Sexual Health Inventory for Men (SHIM), which evaluates erectile dysfunction, providing reliable data for clinical assessment, and the Female Sexual Function Index (FSFI), which assesses critical dimensions of female sexual function, aiding in diagnosing and treating sexual disorders. The PROMIS Sexual Function and Satisfaction Measures, developed by the NIH, cover multiple aspects of sexual function for both men and women, offering a broad perspective on sexual health. The Brief Sexual Symptom Checklist for Men and Women (BSSC-M/BSSC-W) serves as a quick screening tool designed to identify sexual problems, facilitate early intervention, and improve patient outcomes. Additionally, the Sexual Orientation and Gender Identity (SOGI) Survey collects comprehensive data on sexual orientation, gender identity, and related health behaviors, ensuring inclusive and culturally competent care. 69
Integrating validated questionnaires into electronic health record (EHR) systems can significantly enhance the efficiency and thoroughness of sexual assessment for older patients. Many healthcare organizations have developed custom templates for these assessments, establishing a foundation for consistent and comprehensive patient evaluation. These adaptable and shareable templates promote best practices across various clinical settings. For example, Epic Systems and Cerner’s PowerChart EHR systems can create and customize templates specific to multiple medical specialties. Healthcare providers can design sexual health assessment templates that incorporate sections for medical history, risk factors, and current sexual concerns, ensuring a more thorough and tailored approach to patient care. These customized templates streamline the data collection and analysis process, facilitating more efficient, detailed, and practical evaluations, ultimately improving the quality of sexual healthcare delivery. 70
The integration of templates not only standardizes care but also enhances the ability of healthcare providers to deliver tailored and sensitive patient care. By embedding these questionnaires into the EHR, providers can ensure that all relevant information is systematically captured, facilitating better patient outcomes through improved clinical decision-making and personalized treatment plans. Furthermore, using these templates across different clinical settings promotes consistency in care delivery, ensuring that all patients receive thorough and evidence-based assessments regardless of where they are seen. This standardized approach helps to identify and address sexual issues more effectively, contributing to overall improved patient health and satisfaction. 71
Healthcare Practitioner Training
Despite recognizing their crucial role in addressing sexual matters with older patients, healthcare providers often feel undertrained and are not proactive in discussing these issues. Barriers to assessing a sexual history among PCPs include time constraints, lack of privacy, interruptions, lack of communication skills between providers and patients, personal factors such as age and gender, lack of support, and absence of a sexual assessment template within EHR systems.72,73 Research reveals that younger and less experienced healthcare providers reported more significant discomfort in addressing sexual issues among their older patients. 74 Data indicates sexual problems are often not discussed due to lack of training in sexual education, insufficient knowledge of sexuality, embarrassment on the subject, and a lack of confidence in being able to discuss sexual matters with their patients.75-80 Healthcare systems can overcome these barriers by implementing healthcare provider training, patient educational interventions for effective provider and patient communication, and policy changes to update EHR technology to include sexuality as part of a comprehensive health assessment.
Healthcare practitioners must be thoroughly trained to address patients’ sexual needs and concerns, creating a supportive, nonjudgmental environment where patients feel comfortable discussing their sexuality openly. Practitioners should provide comprehensive guidance on preventing and treating sexual dysfunction while offering strategies for sustaining sexual satisfaction. This includes challenging cultural misconceptions about sexuality in later life, addressing barriers to sexual expression, and educating patients on reducing the risks of STIs and HIV transmission. Physician training should emphasize integrating comprehensive sexual assessments into routine care, with a focus on understanding and respecting diverse sexual orientations and gender identities (SOGI). By addressing these critical issues, healthcare providers can foster a more inclusive perspective on sexuality, empowering older adults to engage in safe, satisfying sexual experiences.
Sexuality Resources for Healthcare Clinicians
Healthcare clinicians can access a variety of reputable repositories to support their sexual education efforts for older adults. The National Coalition for Sexual Health (NCSH) is a collaborative initiative comprising diverse organizations, healthcare providers, and advocates dedicated to advancing sexuality and well-being. For clinicians, the NCSH offers valuable resources, including evidence-based guidelines, training materials, and tools designed to improve the delivery of sexual care services. The coalition emphasizes the importance of comprehensive sexual education across diverse populations, preventive care, and open, inclusive communication between healthcare providers and patients. 81
The American Sexual Health Association (ASHA) provides an extensive range of resources designed to assist clinicians in educating and training on the sexual health of older adults. These offerings include educational materials, professional development opportunities like online courses and workshops, and evidence-based clinical guidelines. ASHA also offers expert consultations and patient education materials, and supports advocacy efforts to promote sexual health awareness. In addition, their research initiatives supply valuable data that inform and refine clinical practice. Utilizing these resources allows clinicians to elevate their expertise, delivering high-quality, compassionate care tailored to the sexual health needs of older adults. 82
The Sexuality Information and Education Council of the United States (SIECUS) supports clinicians in educating and training about sexuality among older adults by providing comprehensive educational resources, professional training programs, and evidence-based research. SIECUS fosters collaboration and networking opportunities, allowing clinicians to share best practices and innovative approaches to deliver age-appropriate, culturally sensitive care. Utilizing SIECUS’s resources, clinicians can enhance their expertise and offer high-quality, informed, sensitive care to their older patients. 83
Conclusion
Despite the notable gaps in practical strategies to support sexuality among older adults, healthcare clinicians are in a unique position to address this vital issue. A key challenge remains: the widespread lack of formal training on sexual problems specific to this population. Implementing comprehensive, evidence-based training programs is crucial to provide clinicians with the knowledge and skills needed to address sexual concerns effectively and with confidence. Such programs should offer a holistic understanding of the physiological, psychological, and social dimensions of sexuality in aging, ensuring that clinicians are well-prepared to provide nuanced, empathetic care.
Applying the pillars of lifestyle medicine—nutrition, physical activity, stress management, avoidance of risky substances, and fostering social connections—can have a profound impact on sexuality in older adults. Integrating sexual assessments into electronic health record (EHR) systems offers a practical and efficient way to streamline the documentation and evaluation process. Normalizing sexual assessments as a routine part of patient care allows clinicians to address this frequently neglected aspect of well-being, ensuring it receives the attention it deserves in comprehensive clinical practice.
Future research must prioritize a deeper understanding of the unique needs of older adults to develop innovative, evidence-based interventions to enhance the quality of care. Personalized care that takes into account differences in age, cultural background, gender identity, sexual orientation, relationship dynamics, and health disparities can significantly improve the relevance and effectiveness of sexual healthcare for older adults. Future research must examine the long-term impact of personalized interventions, explore the potential of technology in supporting sexuality, and develop strategies to overcome the stigma and barriers that often hinder open discussions about sexuality in later life. Advancing research, education, and clinical training in this area will ensure that sexuality is recognized as a vital component of holistic, age-inclusive healthcare.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
