Abstract
Background
Postprandial sleepiness refers to the state of excessive drowsiness that occurs after consuming a meal. This transient phenomenon is experienced by many individuals, often leading to decreased productivity and impaired cognitive performance. This study examined the effect of a whole-food plant-based (WFPB) diet on postprandial sleepiness.
Methods
Ten participants who had postprandial sleepiness who were on a typical American diet transitioned to a WFPB dietary pattern for 21 days. Postprandial sleepiness was assessed using the Epworth Sleepiness Scale (ESS) questionnaire, focusing on Q7 “sitting quietly after lunch without alcohol” as well as Q5 “lying down to rest in the afternoon when circumstances permit.”
Results
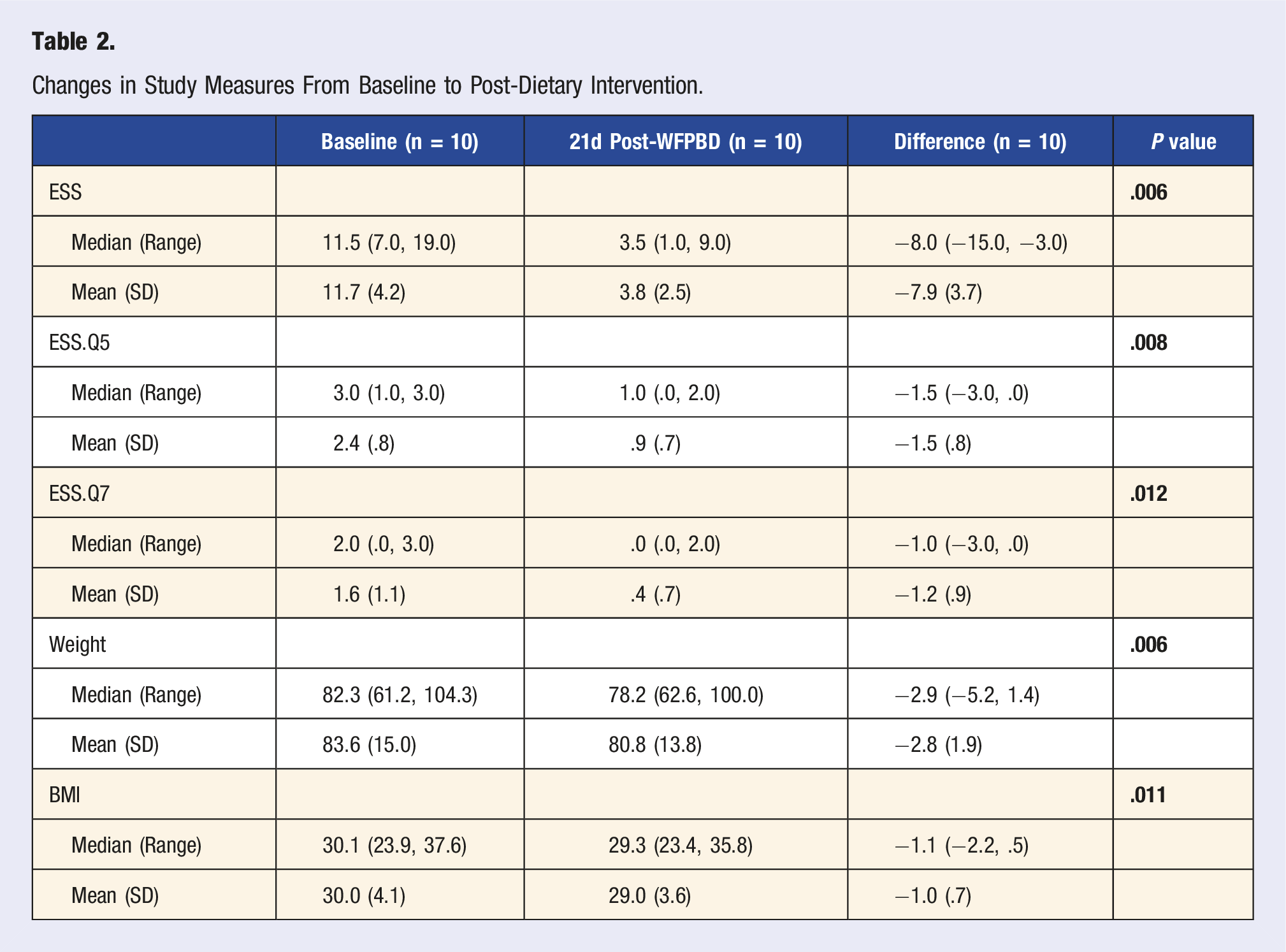
The participants had a mean age of 44 +/− 15 years, with 30% being male. There was a statistically significant reduction in sleepiness measured by ESS Q7 (median change = −1, P = .012) and ESS Q5 (median change = −1.5, P = .008). Moreover, there was a statistically significant decrease in overall ESS scores (median change = −8.0, P = .006), and weight (median change = −2.9 kg, P = .006).
Conclusion
Participants demonstrated significant improvement in postprandial sleepiness-related situations. Our findings showed that the WFPB diet may have potential benefits for reducing postprandial and overall daytime sleepiness.
“We found that a short-term (21-day) WFPB dietary intervention reduced postprandial sleepiness.”
Introduction
Postprandial sleepiness is a common phenomenon experienced by many people after a meal. 1 It is characterized by a feeling of drowsiness or fatigue that can lead to decreased alertness, impaired cognitive function, and decreased productivity. 2 Moreover, most individuals’ postprandial period after lunch coincides with a predictable “circadian dip” 3 resulting in a higher propensity of drowsiness in the early afternoon. Postprandial sleepiness can be particularly problematic for workers, especially those who operate heavy machinery or drive vehicles monotonously, 4 as it can increase the risk of work-related performance failures such as accidents and injuries. In addition, the direct and indirect economic burden associated with postprandial sleepiness is of concern. 5 Studies have assessed the influence of meal composition or portion size on postprandial somnolence, but the findings are inconclusive. Few studies have shown that a diet high in saturated fats is associated with drowsiness. 6 At this time, the exact mechanisms underlying postprandial sleepiness are not yet fully understood, but it is believed to involve a complex interplay of physiological, circadian rhythm, neurochemical, and behavioral factors.
While previous studies have investigated the impact of various dietary factors on postprandial sleepiness, limited research has focused on the potential benefits of a whole-food plant-based (WFPB) diet. This dietary approach emphasizes the consumption of minimally processed plant foods, including fruits, vegetables, legumes, whole grains, nuts, and seeds, while minimizing or excluding animal products and highly processed foods. Given the health benefits associated with a WFPB diet, such as improved insulin sensitivity and enhanced sleep quality,7,8 it is plausible that this dietary pattern may also modulate postprandial sleepiness. In addition, a recent study has shown that a WFPB diet intervention can significantly reduce daytime sleepiness in patients with obstructive sleep apnea. 9
Despite limited supporting data, there are potential mechanisms by which a WFPB diet may have a positive impact on sleep, such as by reducing inflammation, regulating hormones, and providing important nutrients.10-12 Additionally, some plant-based foods are rich in nutrients that have been linked to improved sleep. One such nutrient is tryptophan, an amino acid that is a precursor to the neurotransmitter serotonin, which is involved in regulating sleep. 13 Furthermore, some studies have suggested that the gut microbiome may play a role in sleep regulation and that a plant-based diet may help to promote a healthy and diverse microbiome.14,15 However, more research is needed to fully understand the relationship between a WFPB diet and postprandial sleepiness. Factors such as meal timing, macronutrient composition, and individual differences in metabolism may also play a role in how food affects sleepiness after a meal. Thus, to explore these research gaps, we implemented a pilot intervention examining the effects of a WFPB diet on postprandial sleepiness.
Materials and Methods
Participants were recruited from the community through flyers. Inclusion criteria were: 18-70 years of age, consuming a typical Western diet and experiencing sleepiness after eating lunch, and an Epworth Sleepiness Scale (ESS) score ≥3, as well as scoring >0 on the questions about these two situations: Q7 “sitting quietly after lunch without alcohol” and Q5 “lying down to rest in the afternoon when circumstances permit.” Exclusion criteria were: a diagnosis of diabetes, currently pregnant or lactating, consuming a vegan/plant-based diet, BMI ≤22, iron deficiency, and Vitamin B12 deficiency. This study was approved by the Mayo Clinic Jacksonville IRB: protocol 22-011794. The study was also registered on ClinicalTrials.gov NCT05706649.
Participants were provided with the Forks Over Knives handbook 16 as a resource, which contains an introduction to a WFPB diet as well as recipes for the participants to follow. Participants were instructed to consume a WFPB diet for 21 days. The research team was available to answer participants’ questions about following a WFPB diet throughout the study period. Study participants were not financially compensated.
Postprandial sleepiness was ascertained before and after 21 days of intervention via the ESS questionnaire. Following the end of the 21-day plant-based dietary intervention, the study team assessed participants’ self-reported height and weight, whether or not they experienced side effects, and level of dietary adherence from 1%–100% where 100% was absolute adherence to the dietary protocol without deviation.
Categorical variables were summarized as frequency (percentage) and continuous variables were reported as median (range) and mean (standard deviation). Wilcoxon signed-rank test was used to evaluate changes in ESS, weight, and BMI. All tests were two-sided with a P-value <.05 considered statistically significant. The analysis was done using R4.1.2.
Results
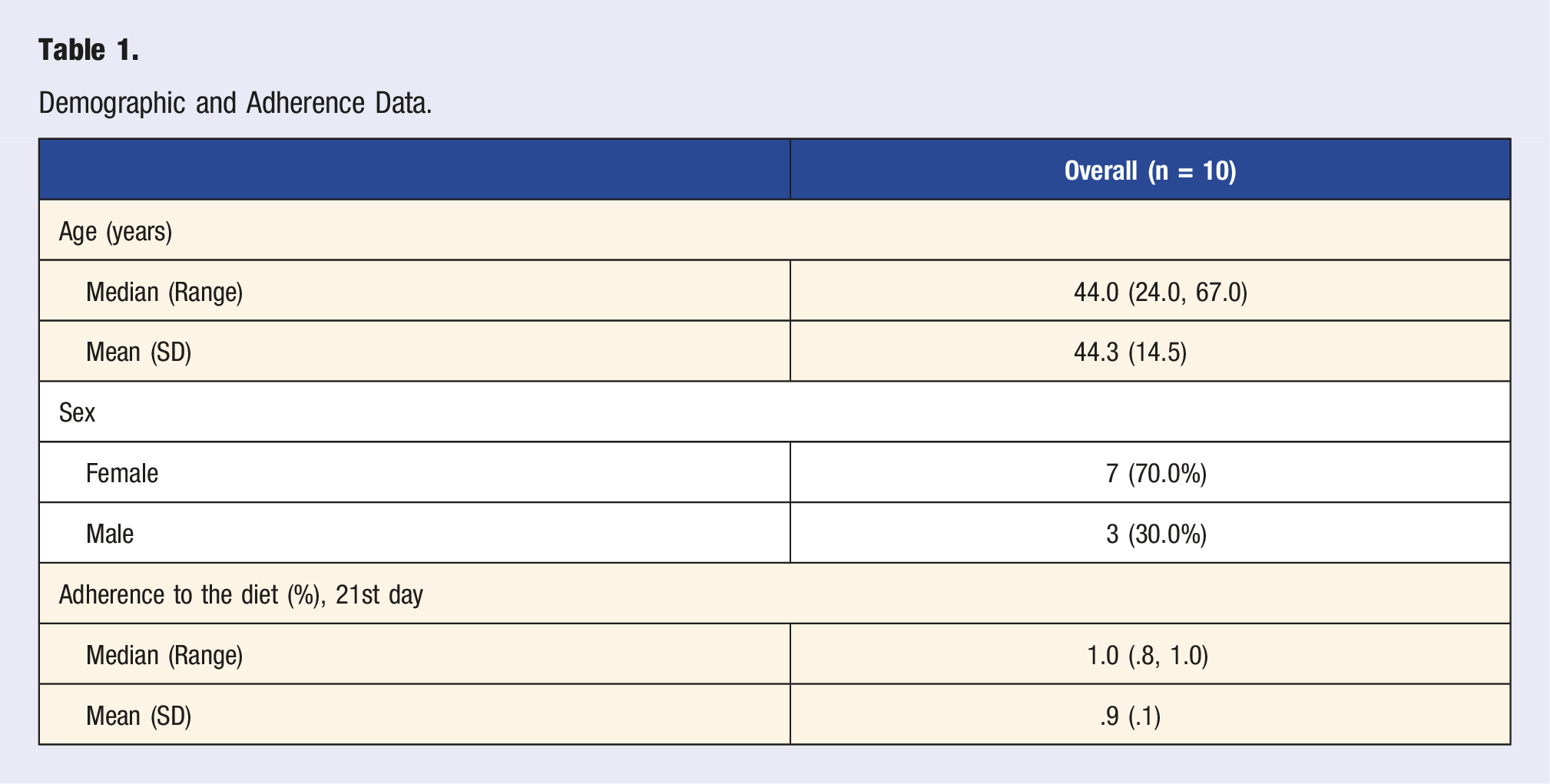
Demographic and Adherence Data.
Changes in Study Measures From Baseline to Post-Dietary Intervention.
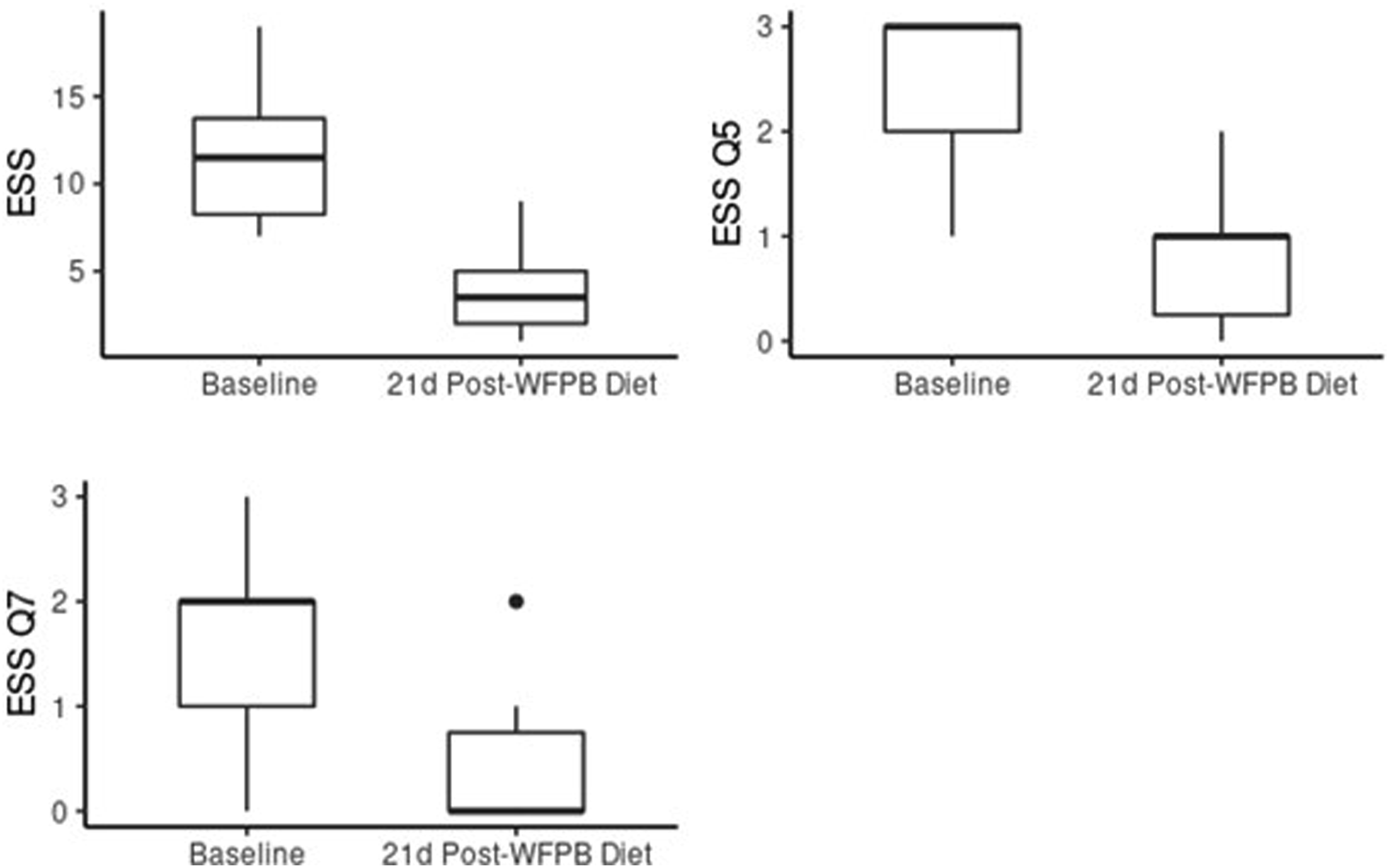
Box plots of change in ESS scores from baseline to 21-day Post-WFPBD.
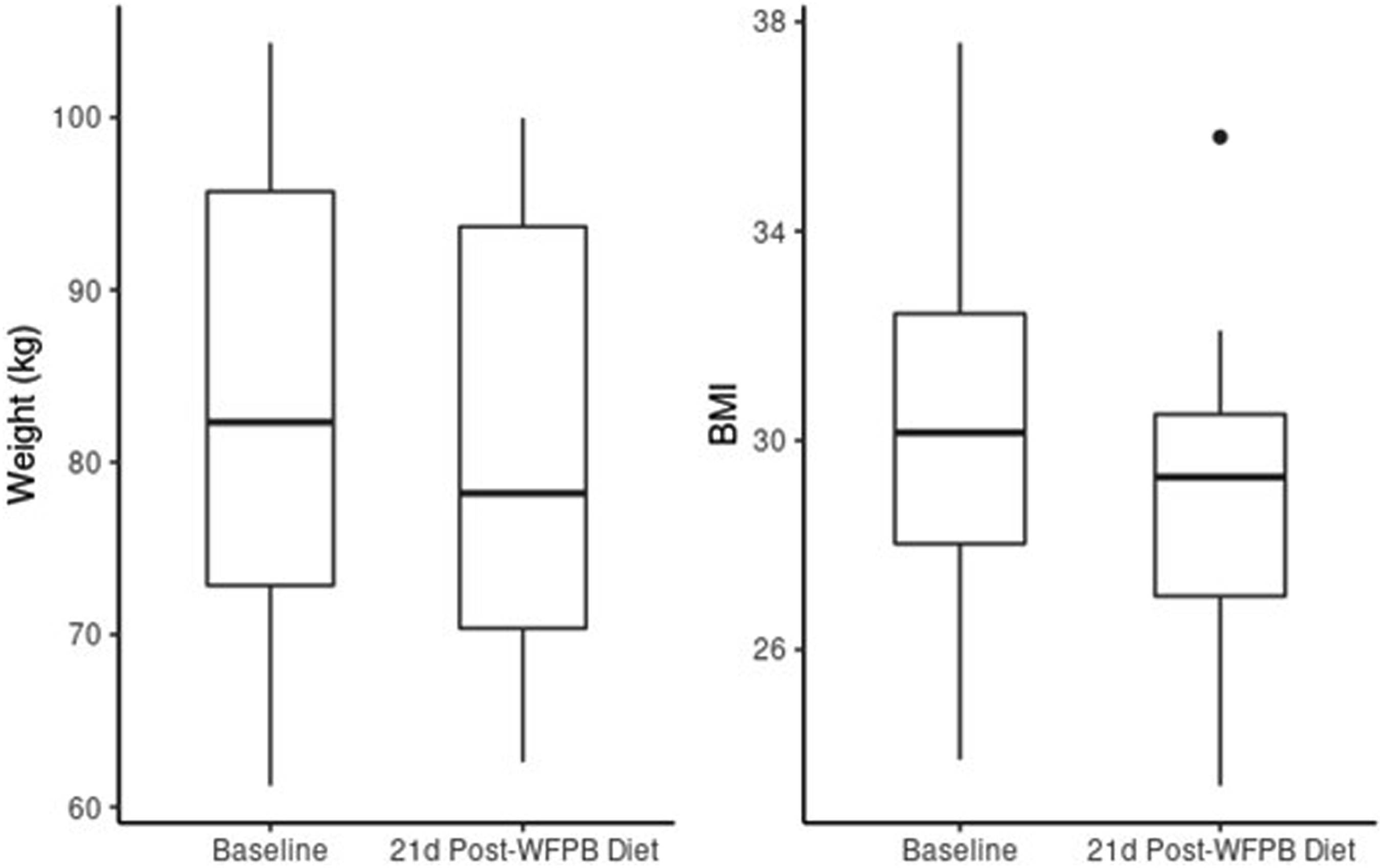
Box plots of change in weight and BMI from baseline to 21-day post-WFPB diet.
Reported side effects of the diet included bloating (3 participants), increased bowel movement (1 participant), and constipation (1 participant). No other side effects were reported. Participants reported a median diet adherence of 100% in the 21-day period (range between 80%-100% adherence) and a mean adherence of 90% (with a SD of 10%). To put this in perspective, none of the participants reported having more than 3 meals in the course of the 21 days that deviated from a WFPB diet. In our post-study survey, 7 out of 10 participants reported that they would likely continue consuming a WFPB diet in the future. The rest of the participants decided to modify their regular diet by adding more vegetables and fruits and/or reducing daily meat consumption.
Discussion
In this study, we used the ESS subcomponent questions, specifically Q7 to ascertain the chance of dozing “sitting quietly after lunch without alcohol,” and partially relevant Q5 “lying down to rest in the afternoon when circumstances permit” as surrogate measures of postprandial sleepiness in the absence of an existing, validated instrument. We compared scores obtained before and after the 21-day WFPB dietary intervention. We found that a short-term (21-day) WFPB dietary intervention reduced postprandial sleepiness. In addition, we observed a marked improvement in overall daytime sleepiness in our cohort with an average reduction of 8.0 points in ESS, which outperforms the use of stimulant medication (e.g., modafinil). 17
The relationship between diet and sleep has been the subject of recent research, with a particular interest in how whole-food plant-based diets impact sleep quality. One possibility is that higher sleep variability is directly associated with daytime sleepiness and greater glucose variability. 18 Hence, the high-fiber foods included in the WFPB diet may enhance the ability to stabilize serum glucose, improve insulin sensitivity, 19 and subsequently decrease daytime sleepiness. 18 Studies have found that diets with high-fiber content, such as the DASH diet and Mediterranean diets, are associated with better sleep quality,20-22 which in turn may potentially improve excessive daytime sleepiness. In contrast, a diet high in saturated fats has been associated with drowsiness and decreased sleep quality. 23 Thus, it has been demonstrated that reduced N3 (deep) sleep was associated with higher fat and carbohydrate intake. 24 High-fat meals have been shown to stimulate the release of cholecystokinin, which activates specific receptors on the vagal nerve and reduces alertness.10,25 Inflammation may also impact sleep quality, with diets high in anti-inflammatory components being linked to improved sleep. 26 Additionally, a higher dietary intake of certain (poly)phenols, such as lignans and hydroxycinnamic acid, has been associated with better sleep quality among adult individuals.11,27 These (poly)phenols may act through several mechanisms, including positive modulation of GABA(A) receptors, stimulation of melatonin synthesis, and improvement of endothelial function. Furthermore, dietary sources of melatonin and its precursors, tryptophan and serotonin, have been shown to improve sleep quality, with fruits, nuts, and whole grains being important dietary sources of melatonin.12,28 These findings suggest that dietary interventions focused on increasing the intake of specific nutrients and plant compounds may provide a safe and effective means of improving sleep quality in the general population. 29
Finally, the existing literature suggests a strong association between diet patterns and the gut microbiome.30,31 Plant-based diets, particularly Mediterranean and vegetarian, have shown a favorable impact on the gut’s bacterial flora, potentially contributing to improved health outcomes.32-34 Dietary fiber, which is abundant in whole-food plant-based diets, has been shown to positively affect the composition of gut bacterial flora. 14 The relationship between the gut microbiome and sleep has been explored 15 and indicators of balanced gut flora have been associated with improved sleep quality. 35
There are limitations to this pilot study including the small sample size and lack of a control group; pre-study dietary recall was not performed; detailed dietary records were not captured during the study; the study duration was short; and all participants self-reported personal biometrics. Future investigations should consider utilizing continuous glucose monitors (CGM), assessing pre and post-dietary intakes, utilizing a control group, including clinic biometric measures as well as objective sleep assessments such as polysomnography and maintenance of wakefulness test.
Conclusions
Overall, our findings showed that the WFPBD may have potential benefits for reducing both postprandial sleepiness and overall daytime sleepiness. Further research is needed to fully understand the mechanisms underlying these associations and to determine optimal dietary patterns for improving sleep health.
Footnotes
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: JC is supported by the Mayo Clinic in Florida Research Accelerator for Clinicians Engaged in Research-plus Program. This work is also supported by philanthropic donations from Mr. and Mrs. Zearley.
Data Availability Statement
All data related to this study is available by contacting the corresponding author.
