Abstract
The COVID-19 pandemic affected individual sleep quality, especially with high-stress levels. We assessed sleep quality in young adults during COVID-19, and mental health, stress, and screen time (ST) use. An international cross-sectional study was conducted from September 2020 to January 2021. The surveys assessed sleep quality (PSQI), ST use, and mental health. 183 participants were eligible for analysis. The average global PSQI score was 7.29 (sd = 3.58, n = 99). Associations were found between global PSQI scores and Fear of COVID-19 (r (98) = .223, P = .027), anxiety scores (r (99) = -.541, P < .001), increased total stress scores (r (88) = .486, P < .001), and depression (r (97) = .628, P < .001). Those currently quarantining had statistically higher PSQI scores than those who quarantined in the past (F (2,175) = 3.397, P = .036), but not for those who did not quarantine. Differences were found between genders for global PSQI (F (4,94) = 2.865, P < .027) and poor vs good sleep (X2 (1,98) = 3.982, P = .046). There was also a relationship between ethnicity and poor vs good sleep quality (X2 (2,94) = 6.538, P = .038). We did not find associations between ST and sleep quality but found poor sleep quality significantly related to mental health during COVID-19. We found no direct evidence that quarantining itself results in poor sleep quality. Interventions need to maximize sleep quality in certain groups, like females and ethnic minorities.
“Social isolation negatively affected mental health, resulting in increased substance use during COVID-19, particularly alcohol consumption.”
Introduction
The coronavirus-19 (COVID-19) pandemic caused various governments to enforce strict social distancing measures to restrict the spread of the virus. 1 The combined elements of an unpredictable pandemic with the implemented stay-at-home policies have characteristically contributed to the rise of psychological distress and mental health issues. 2 Impaired sleep quality and habits have been demonstrated in previous studies in association with elevated psychological distress (e.g., depression, anxiety, stress) and negative mood during the COVID-19 lockdown.3,4
Before the pandemic, sleep quality has been an area of interest since it plays a role in a person’s physical health, academic function, and mental health. 5 Increased screen time (ST) paired with low physical activity levels can be linked to increased mental health issues and low sleep quality in students, and increased study hours paired with academic pressures and lifestyle choices may also play a vital role in low sleep quality. 6 There is no doubt that unhealthy lifestyle behaviors have increased during the pandemic, including less physical activity, unhealthy dietary choices, sleep issues, increased ST, and less socialization.7,8 Studies have displayed the overwhelming impact the pandemic has had on young adults, mainly undergraduate and postgraduate students, who are more prone to low-quality sleep due to increased study hours brought on by academic pressures and lifestyle choices. 9
Despite increasing information regarding the young adult population and sleep during the pandemic, especially on its relationship with mental health, studies still need to include a broader overview of sleep quality, especially understanding the impact of quarantine on sleep. Little consensus exists on whether quarantining affects sleep quality, as research primarily focuses on sleep quality and mental health during quarantine with only some focus on broad populations (i.e., adults) or certain regions.10,11 Furthermore, there is little consensus on whether quarantining affects sleep quality, indicating multiple factors are involved and may depend on the population, region, age, gender, and other factors.11,12
Thus, this study aimed to bridge these gaps and assess sleep quality in young adults (ages 18-28) in multiple countries during the COVID-19 pandemic, focusing not only on various mental health aspects (anxiety, depression, fear of COVID-19, substance use, and stress) but also quarantine status and length of quarantine and other characteristics associated with sleep quality, like BMI and ST use.
Materials and Methods
Study Design and Setting
A cross-sectional study was conducted from September 2020 to January 2021. Participants were recruited by convenience sampling to participate in an online, international survey via the SurveyMonkey® survey platform. Participants were recruited by word of mouth, school-wide emails, major social media sites (i.e., LinkedIn, Twitter, Facebook), and online survey response platforms (i.e., SurveySwap and SurveyCircle) to reach internationally.
Sampling and Sample Size
As per the inclusion criteria, respondents were 18-28 years and required 100% completion of all validated questions within the survey to exclude respondents who randomly filled out answers. Respondents outside the targeted age range and those who failed to answer the validated questions accurately were excluded from the study.
294 participants completed the survey (182 from online response platforms, 93 from social media, and 19 from the local institution). After implementing inclusion and exclusion criteria (111 individuals aged less than 18 or above 28 years; or answered inaccurately to the validated questions were excluded), a sample of 183 respondents was used in data analysis.
Research Instruments and Assessments
Social Demographics
Data was collected on gender, ethnicity, race, age in 2020, current student status, employment, and country of residency within the past 6 months. Participants who were students and not employed were instructed to select “unemployed, not looking for work” for employment status. Body mass index (BMI, kg/m2) was calculated after respondents provided their body height (cm, feet/inches) and weight (kg/lbs.) with necessary conversion based on their choice of the U.S. measurement or the universal metric system.
COVID-19-Related Questions
Respondents were asked about their current COVID-19 status regarding whether they had been tested for the virus and if they had a COVID-19 infection. Quarantine status, past or present, was collected. If they were quarantined, respondents were instructed to provide the length of duration (days) they were in quarantine.
Sleep Quality
Sleep quality was measured using the Pittsburgh Sleep Quality Index (PSQI, 1989), a 19-item self-assessment questionnaire validated to assess sleep quality and difficulties in a 1-month interval during the pandemic. 13 A global PSQI score that ranges from 0-21 is calculated based on seven constructs: duration, disturbance, latency, daytime dysfunction, efficiency, quality, and medication use. 13 Respondents rated each item on a 4-point Likert scale (0 = Not during the pandemic, 1 = Less than once a week, 2 = Once or twice a week, 3 =Three or more times a week). The PSQI is calculated by the sum of every component. Participants were asked about their everyday sleeping habits on average during the COVID-19 pandemic (March 2020 - date survey completed), which included the times they usually had gone to bed at night (Time: hh/mm, a.m./p.m.), it had taken to fall asleep (in minutes), get up in the morning (Time: hh/mm, a.m./p.m.), and the average amount of sleep they got each night (in hours), indicating this might differ from the number of hours spent in bed. Respondents also indicated whether they felt their sleep quality changed during the pandemic.
Screen Time (ST) Behavior
Participants were asked about their time spent (hours per week) on ST use over the past week, based on a previously validated questionnaire, but modified to separate three categories (Entertainment (e.g., streaming services, television (TV), movies, music, and video games), social media (SM) (e.g., Facebook, Instagram, Twitter, Snapchat, TikTok), and educational/professional uses (online lectures, webinars, business meetings, and video tutorials). 14 Related activities about SM (e.g., chatting and sharing information/pictures) were included in the SM category. Examples were provided to distinguish each of the three categories measured to prevent confusion or wrong categorization. ST use was collected during the COVID-19 pandemic (March 2020-Present day) and before the pandemic (October 2019-December 2019). If no time was spent on ST, participants were instructed to answer “0” as their response.
Mental Health (Depression, Anxiety, Fear, and Psychological Impact of COVID-19, Overall Well-Being)
Depression was assessed using the patient health questionnaire (PHQ-9), a self-report scale for depressive symptoms. 15 It scores each of the 9 DSM-IV criteria on a 4-point Likert scale ranging from 0 (not at all), 1 (several days), 2 (more than half the days), and 3 (nearly every day). With a score ranging from 0-27, total PHQ-9 scores indicate minimal (0-4), moderate (5-14), and severe depression (15-27); scores ≥10 indicate possible depression. 16
Anxiety was assessed using the Generalized Anxiety Disorder 7-item validated questionnaire (GAD-7). 17 It is scored on a 4-point Likert scale ranging from 0 (not at all) to 3 (nearly every day), where a score ranges from 0 to 21 indicates minimum (0-4), moderate (5-14), and severe (15-21) anxiety levels.17,18
The psychological impact of the COVID-19 pandemic was assessed using the Impact of Events Scale-Revised (IES-R). 19 The 22-item measure calculated the overall IES-R score for COVID-19 distress and intrusion, hyperarousal, and avoidance. The level of difficulty for each item is scaled as 0 (not at all), 1 (a little bit), 2 (moderately), 3 (quite a bit), and 4 (extremely). Potential diagnosis for PTSD was indicated based on overall scores for partial (24-32), probable (33-38), and severe (≥39). 20 Subset averages for intrusion, hyperarousal, and avoidance were calculated in the data analysis.
Fear caused by the COVID-19 pandemic was assessed using the Fear of COVID-19 Scale (FCV-19S). 21 It is scored on a Likert scale ranging from 1 (strongly disagree) to 5 (strongly agree), where a score ranging from 7 to 35 assessed individual stress, anxiety, and fear during the pandemic, with 7 being the least amount of fear of COVID-19 and 35 being the highest amount of fear of COVID-19. 21
Subjective well-being was assessed using the WHO’s Five Well-Being Index (WHO-5). 22 The five-item self-reported scale calculates the lowest quality of well-being (0) from the highest (100) based on the raw score range from 0 to 25 from all five items multiplied by four. 22 Total scores were calculated for both pre-and during COVID-19 periods.
Substance Use
Substance use was assessed by the World Health Organization’s (WHO’s) Alcohol, Smoking, and Substance Involvement Screening Test (ASSIST V3.0, 2010). 23 Revised to study illicit uses of alcohol, tobacco, and cannabis, the ASSIST test is scored on a 5-point Likert scale ranging from 0 (never), 2 (once or twice), 3 (monthly), 4 (weekly), and 6 (daily or almost daily). 23 The need for treatment was indicated by total substance scores where it was not needed (<3), briefly needed (4-26), or intensively required (27+). 23 Additional questions were asked to calculate pack/years for tobacco use, average weekly alcohol consumption, and whether drug substance use was altered due to the pandemic.
Data Collection
Access to the medical institution’s SurveyMonkey® platform was limited to the research group, ensuring all collected information remains anonymous and confidential. No information would be shared with any individual outside the group. Data was also de-identified to limit response attribution to a respondent’s name.
Participants who met the inclusion criteria (18-28 years) were invited to complete the survey. It was solely their choice to participate in this study to learn more about how sleep, mental health, overall wellness, and ST usage are affected during the pandemic. Respondents were allowed to withdraw at any time and skip or refuse to answer any question.
A consent form was presented and obtained before each participant was administered the survey. There were no associated physical risks to completing the questionnaires. A disclaimer was provided to both the number of the National Suicide Prevention Lifeline and a link to mentalhealth.gov for additional services due to possible causes of anxiety, stress, or discomfort caused by any survey questions. The participants would receive no benefits, risks, or reimbursement for the survey. The survey would take approximately 30 minutes to complete. The data was collected and processed confidentially by the leading researchers within the group.
Ethical Consideration
The research protocol was approved by each member of the Institutional Research Committee (IRC) at the Saint Vincent and the Grenadines campus of the medical institution Saint James School of Medicine (research project #119).
Data Analysis
Data analysis was conducted using SPSS version 25.0 (IBM Corp, Armonk, NY). All statistics were assessed at the 95% confidence level with a significance level set at alpha = .05. Data analysis included the Levene test for equality of variances, independent t-tests, Pearson correlation, chi-square tests, Fisher’s exact tests, ANOVA tests, and Tukey post hoc tests. Missing data and those who answered “don’t know” and “refuse to answer” were removed from data analysis. Small sample size numbers (n < 10) were excluded. Sleep quality measurements were assessed against the following dependent variables: age in 2020, gender, ethnicity, race, student status, employment status, the continent of residence, weekly alcohol servings, pack-years, Fear of COVID-19 scores, past and current WHO-5 scores, past and current BMI, change in BMI, sleep duration, PHQ-9 scores, GAD-7 scores, IES-R total, IES-R intrusion, IES-R avoidance, IES-R hyperarousal scores, ST before and during the COVID-19 pandemic (total, educational, SM, and educational/professional), and ASSIST scores for tobacco, alcohol, and cannabis.
Results
Demographics
Summary of Demographic Information (n = 183).
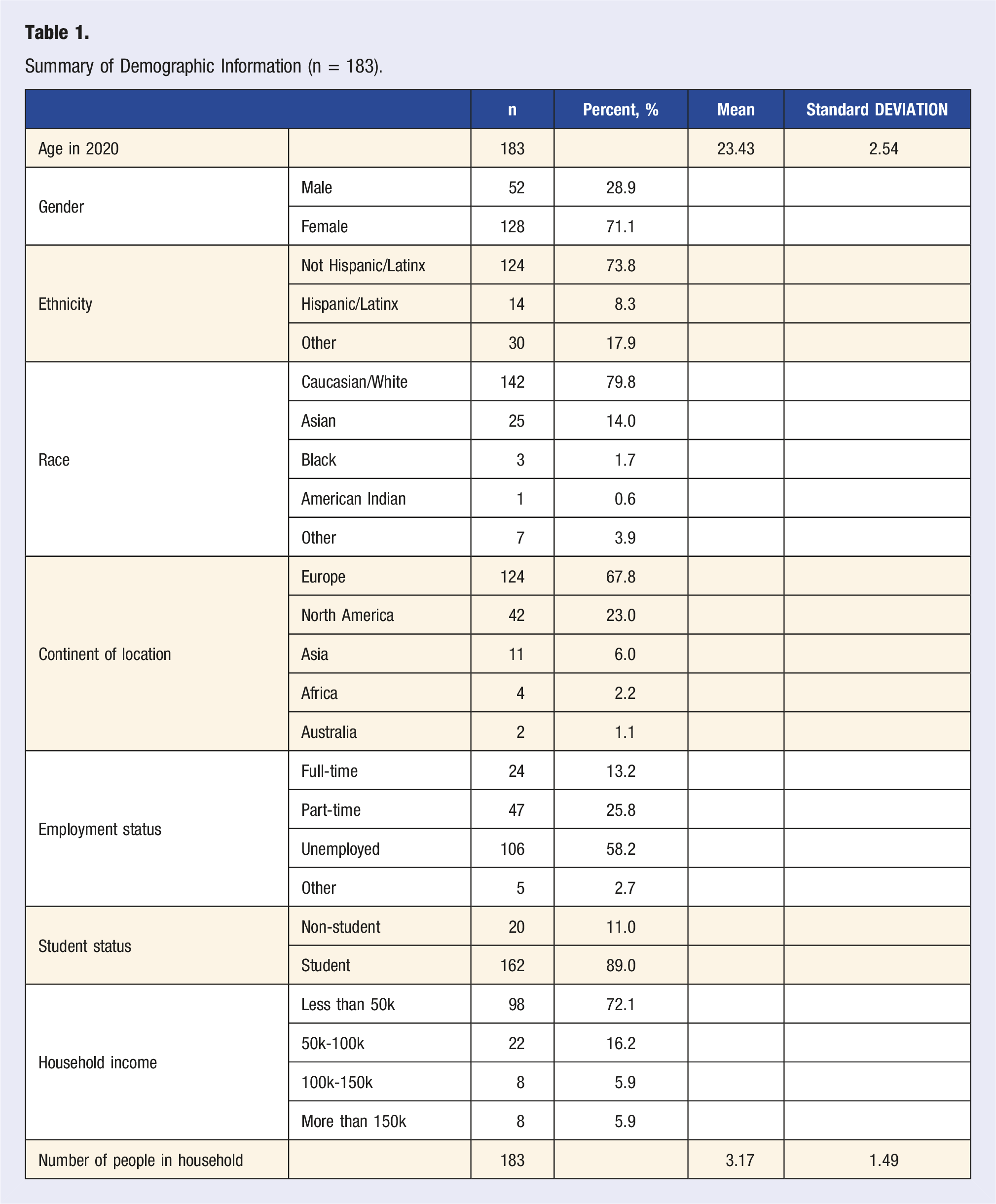
Out of 183 participants who were eligible for data analysis, the average age in 2020 was 23.43 years (sd = 2.54). 71.1% (n = 128) of participants were female, and 28.9% (n = 52) were male. 71.1% (n = 128) were not Hispanic/Latinx, and 17.9% (n = 30) identified as another ethnicity. 79.8% (n = 142) of participants were Caucasian/white, and 14.0% (n = 25) were Asian. 67.8% of participants were from Europe (n = 124), and 23% were from North America (n = 42). 13.2% (n = 24) were employed full-time, 25.8% (n = 47) were part-time, and 58.2% (n = 106) were unemployed (including students). 72.1% of participants (n = 98) had a household income of less than 50k; on average, the number of people in their household was 3.00 (sd = 1.00).
COVID-19 Statistics
COVID-19 Statistic Breakdown (n = 183).
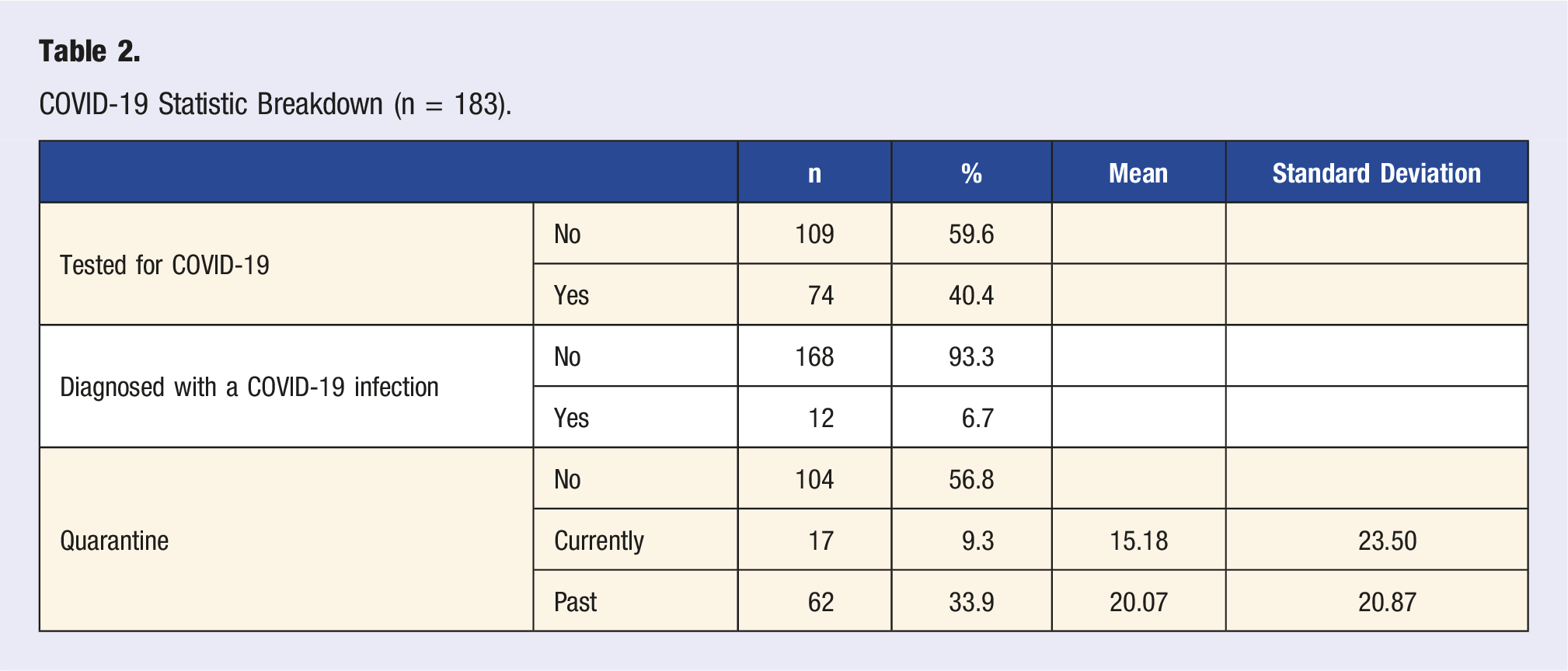
40.4% of participants (n = 74) were tested for a COVID-19 infection. 9.3% (n = 17) were currently quarantining, with an average of 15.18 days (sd = 23.50) spent in quarantine, and 33.9% (n = 63) were quarantined in the past with an average of 20.07 days (sd = 20.87).
PSQI Scores
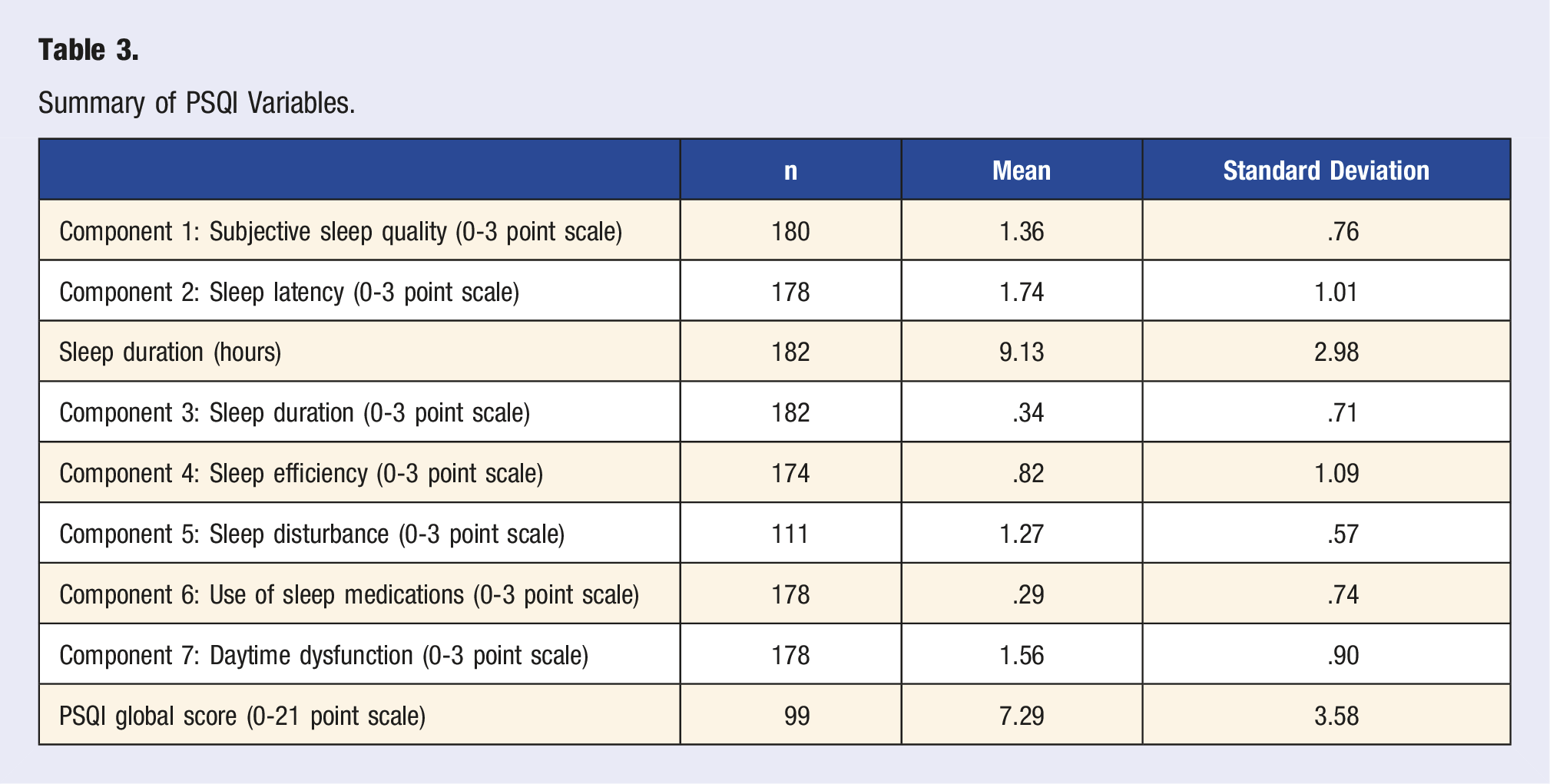
Summary of PSQI Variables.
Subjective Sleep Behavior Change Since the Start of COVID-19 (n = 183) and PSQI Global Scores.
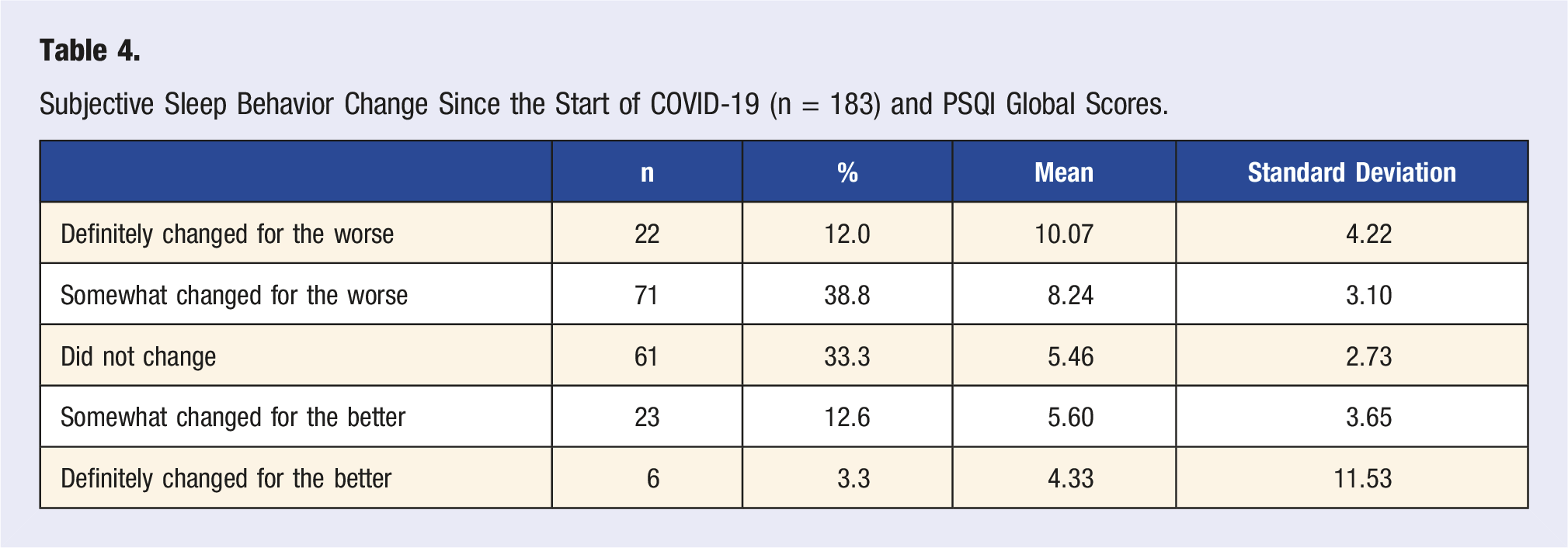
Those currently quarantining (x = 1.35, sd = .86, n = 17) had a statistically significant difference compared to those who were under quarantine in the past (x = 1.98, sd = .99, n = 61) for the sleep latency domain, F (2,175) = 3.397, P = .036. This was also seen for PSQI global scores, F (2,96) = 4.527, P = .013. Lastly, those who spent longer time currently quarantining were negatively correlated with sleep disturbance scores, r (10) = −.761, P = .011.
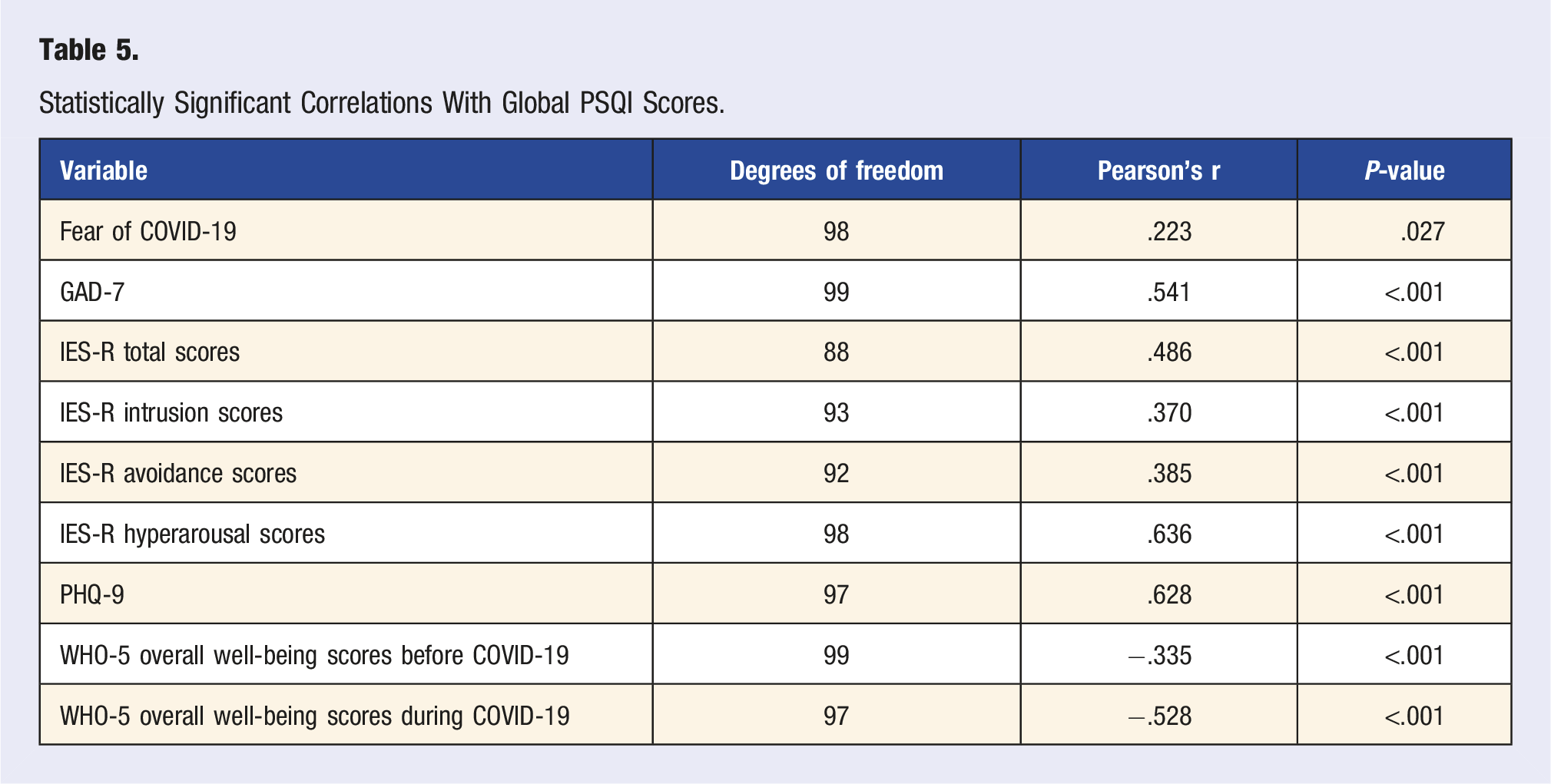
Statistically Significant Correlations With Global PSQI Scores.
Females (x = 7.94, sd = 3.61, n = 69) had statistically higher PSQI global scores compared to males (x = 5.66, sd = 3.02, n = 29), t (96) = -3.001, P < .003. We also found a statistical significance between groups for continents, F (4,94) = 2.865, P < .027. Australia and Africa were excluded due to the low sample size numbers in the analysis (n < 5). People in North America had a mean PSQI score of 8.90 (n = 20, sd = 4.79), Europe had a mean score of 7.16 (n = 69, sd = 3.13), and Asia had a mean score of 4.14 (n = 7, sd = 1.35) (Figure 1). Comparison of global PSQI scores by continent.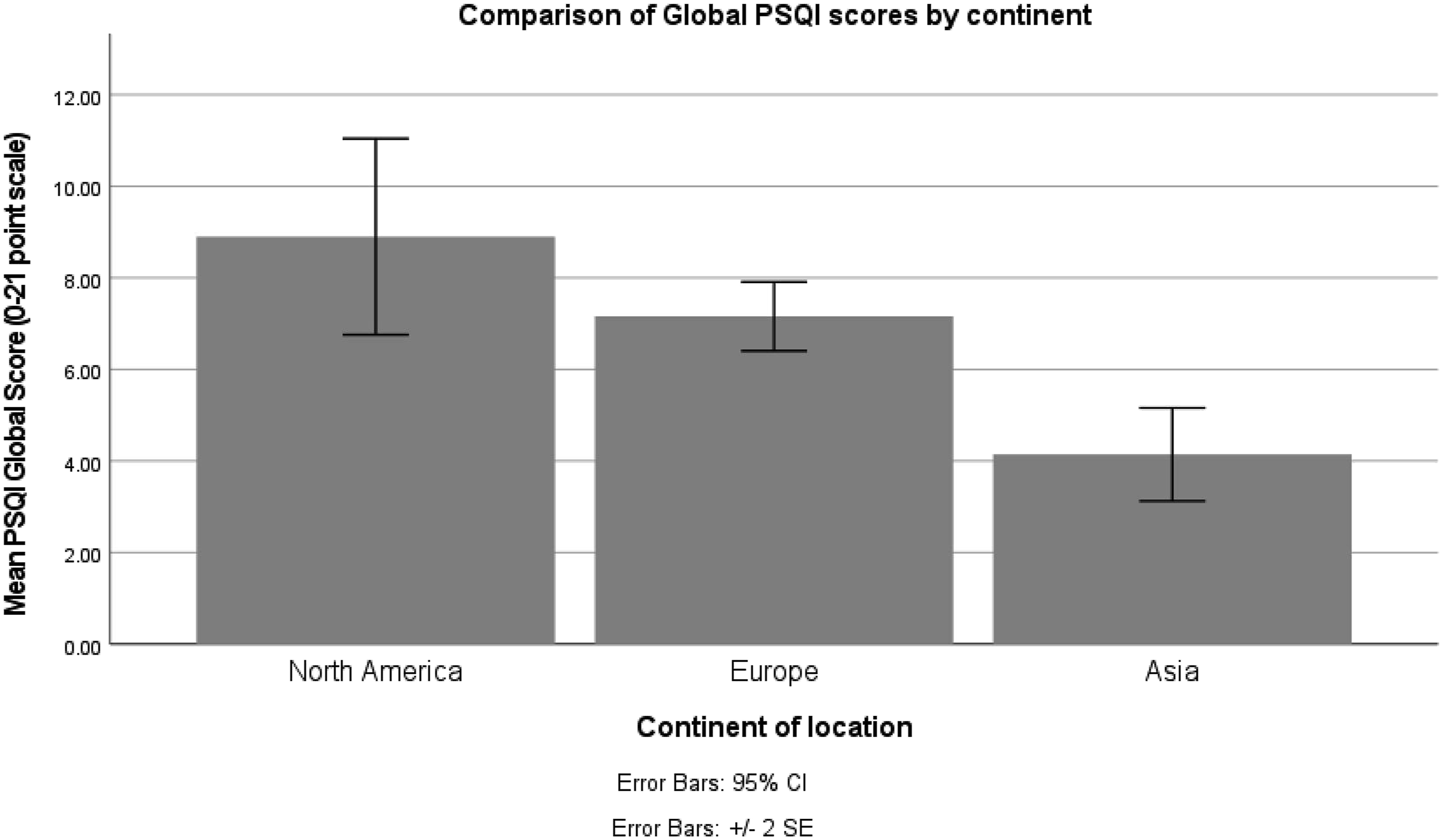
We found no associations between PSQI global scores and age in 2020, race, ethnicity, student status, employment status, household income, and the number of people in the household.
Good Versus Poor Sleep Quality
After individual PSQI scores were categorized into poor or good sleep quality based on cut-off scores, 63.6% had poor sleep quality (n = 63), and 36.4% of respondents had good sleep quality (n = 36).
Comparison of Poor Sleep Quality and Good Sleep Quality Groups and Dependent Variables.
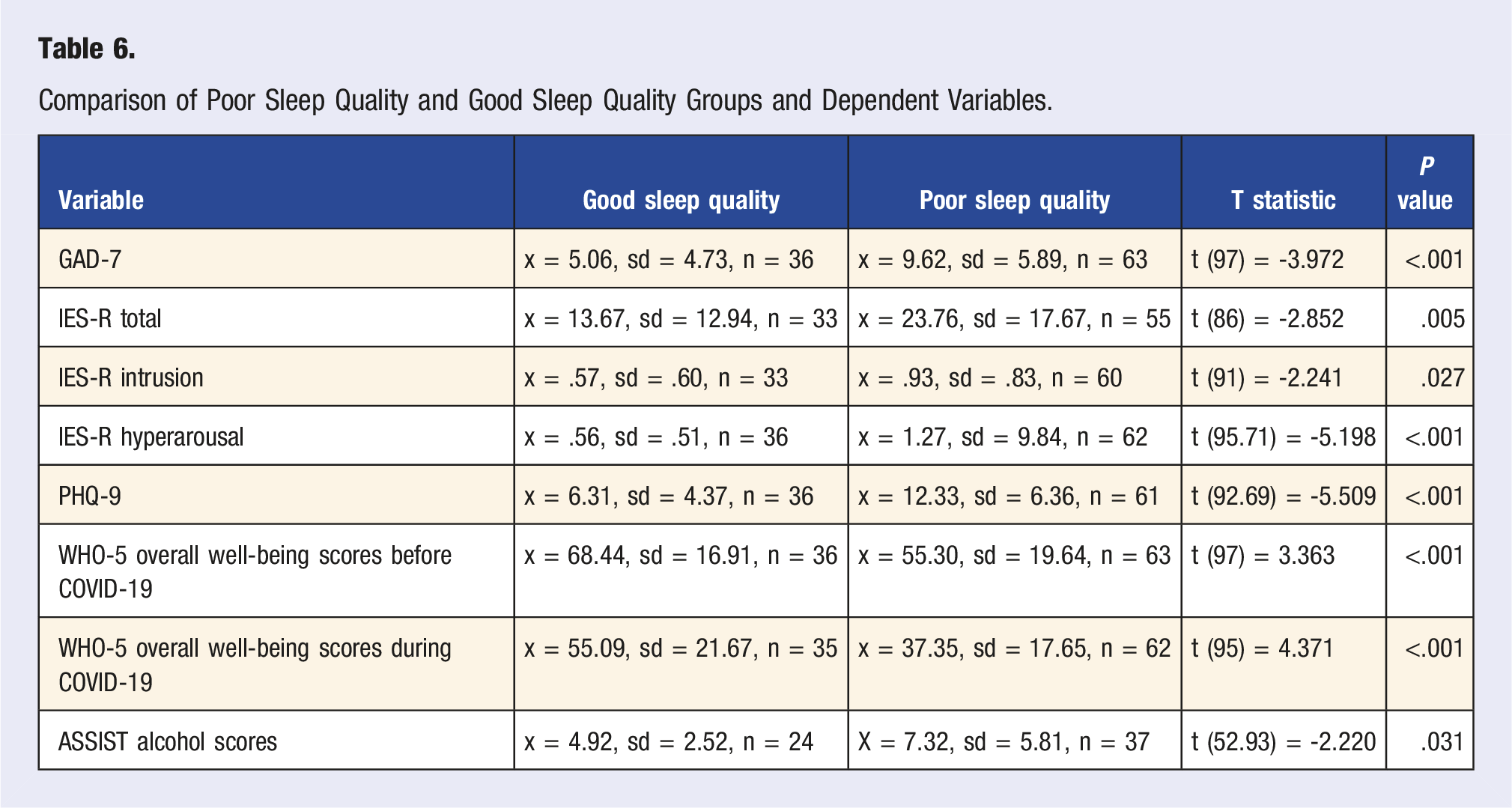
We also found a relationship between gender and sleep quality. Females were likelier to fall into the poor quality sleep category than males, X2 (1,98) = 3.982, P = .046. There was also a relationship between ethnicity and sleep quality. Those who identified as Hispanic/Latinx were likelier to fall into the poor quality sleep category than those who were not Hispanic/Latinx, X2 (2,94) = 6.538, P = .038. We found no differences between good vs poor quality sleep categories and age in 2020, race, student status, continent, employment status, household income, and the number of people in the household.
Discussion
Overall, we found that our population’s average global PSQI score was 7.29 (sd = 3.58), indicating that, on average, participants had poor sleep quality (Table 3). Slightly over half (50.8%) of our participants indicated that their sleep quality had gotten worse since the start of the COVID-19 pandemic (Table 4), and the cut-off for the PSQI scores showed that 63.6% of participants (n = 63) had poor sleep quality. We also found a significant difference between groups in subjective sleep behavior change since the start of the COVID-19 pandemic and PSQI global scores (F (4,94) = 7.644, P < .001), indicating that most of our participants were seemingly aware of their sleep quality. Poor sleep quality is associated with poorer daily functioning, even in healthy young adults, warranting the need to optimize sleep hygiene and sleep quality for better health outcomes and quality of life.24,25 The average sleep duration was 9.13 hours (sd = 2.98), which was longer than expected. However, Zheng and colleagues also found longer sleep duration in young adults during the COVID-19 pandemic, which should be investigated further as longer sleep duration (9+ hours) can increase the risk for cardiovascular issues.26,27 Out of all the sub-components of the global PSQI scoring, our sample size’s lowest score was in the use of sleep medications (x = .29, sd = .74, n = 178) and the highest in sleep latency (x = 1.74, sd = .1.01. n = 178) (Table 3). Other researchers found sleep latency changes in young adults during the COVID-19 pandemic, potentially linked to increased stress levels during the pandemic.28,29 However, Benham 29 also saw increased use of sleep medications in undergraduate students in the United States, something not found in this study. This could be due to the availability of sleep medications in other countries, cultural differences, or our population not having access to healthcare and medications.
Those who were currently quarantining had better global sleep quality scores than those who were quarantined in the past (F (2,96) = 4.527, P = .013), but both groups still had poor sleep quality scores, on average. We also found that those who did not quarantine at all had an average poor sleep quality global PQSI score of 6.92 (sd = 3.51, n = 59), but there was no significant difference between those who did not quarantine and those who quarantined in the past or present. This finding is common in similar studies, suggesting a complicated relationship between sleep quality and quarantining, dispelling the myth that the two are synonymous with each other.30,31 Although some quarantined individuals may have poor sleep quality, it may not be due to quarantine itself and could be due to other factors, like stress and symptoms associated with COVID-19. 32 Recent literature indicates different people have varying mental health effects due to quarantine, and a similar argument could be made for sleep quality, especially since sleep and mental health go hand-in-hand. 33
With general sleeping disorders related to depression and decreased interest in daily activities, studies have shown an increased shift to unhealthy lifestyles reported in more significant portions of young adults due to strict quarantine orders during the COVID-19 pandemic.7,34 We also found significant mental health findings, further corroborating with studies linking poor sleep quality to stress, anxiety, and depression during the COVID-19 pandemic.35-37 Depression (r (97) = .628, P < .001), anxiety (r (99) = −.541, P < .001), and stress (r (88) = .486, P < .001) were all clearly associated with poorer global PSQI scores, which was also seen while comparing good sleep quality vs poor sleep quality (Table 6). In addition, higher PSQI scores were associated with greater fear of COVID-19, an emerging trend.38-40 Yet, we did not find a difference between Fear of COVID-19 scores when comparing the good and poor sleep quality groups, suggesting that the link in our sample size is weak and warrants additional insight. We also found associations between wellness and poor sleep quality and, in particular, those who had lower well-being scores before the pandemic were more likely to have higher PSQI scores (r (99) = -.335, P < .001). This suggests that distinct populations, especially those suffering from existing mental health conditions or other factors that might influence well-being, may suffer from poorer sleep quality during the pandemic.
Females in our sample had statistically poorer sleep quality than males (t (96) = -3.001, P < .003), and they were also more likely to fall into the poor sleep quality category (X2 (1,98) = 3.982, P = .046). Females having poorer sleep quality during the COVID-19 pandemic are well-researched.41,42 In addition to lower sleep quality, women were found to have suffered more significant distress and anxiety during the pandemic amid lifestyle changes induced by the quarantine measures that led to emotional disturbance, insomnia, depression, low mood, and irritability. 43 The sum of negatively-impacted lifestyle behaviors driven by such negative isolating environmental factors, such as relationships with others in the household, have become a risk factor related to the prognosis of cardiovascular disease in women, which is the leading cause of mortality for women in a 2019 study.43,44 Furthermore, there is growing evidence suggesting that loneliness may play a role during the pandemic and various mental health outcomes, something that both females and younger adults faced during the height of the pandemic.45,46 These underrecognized risks along with the prevalence of risk factors (i.e., high LDL cholesterol, obesity, diabetes) have contributed to worsened health factors disproportionally younger women compared to men. 44 Thus, reaffirming the need for optimizing lifestyle behaviors to reduce these comorbidities leading to worse off life expectancy and early death. Another crucial demographic finding is that those who identified as Hispanic or Latinx were more likely to fall into the poor sleep quality category (X2 (2,94) = 6.538, P = .038), adding to the scarce literature regarding specific ethnicities and sleep quality during the COVID-19 pandemic.
Although we did not find an association between alcohol and global PSQI scores, we found a significant difference between good and poor sleep quality groups and ASSIST alcohol scores, t (52.93) = −2.220, P = .031. We found that the average ASSIST alcohol score was 4.92 (sd = 2.52, n = 24) in the good sleep quality group but 7.32 (sd = 5.81, n = 37) in the poor sleep quality group. However, servings of alcohol for each group did not have a statistically significant difference, indicating a more complex relationship between sleep quality and alcohol use. Du and colleagues 47 also found in their study focusing on US adults that there was an association between sleep quality and alcohol consumption, relating it to stress levels. Since we found that increased stress from the pandemic is also associated with sleep quality, this is a high possibility that the two are interconnected. However, we did not find an association with consumption, but rather potential substance abuse despite both groups falling into the lower risk category. 48 Correlations between alcohol consumption and decreased sleep quality are well studied. Alcohol interrupts sleep by inhibiting the central nervous system (CNS), ultimately decreasing sleep onset latency, decreasing rapid eye movement (REM) sleep, and increase number of times a person wakes during sleep. 49 Higher alcohol consumption is associated with worse sleep quality with higher odds of having shorter deep duration and snoring/obstructive sleep apnea (OSA). 49 Social isolation negatively affected mental health, resulting in increased substance use during COVID-19, particularly alcohol consumption. 50 Alcohol consumption fluctuated over the course of the pandemic, especially during the early times of COVID-19, and other countries, like Canada and Poland, also saw an increase in alcohol sales.51-53 International cross-sectional studies have reported increased consumption percentage associated with poor overall mental health symptoms among young adults (aged 18-34 years) with reasons including the lack of daily routines, stress, and boredom.4,50 In Mediterranean areas, more subjects reported increased frequency of their alcohol intake that included individually or drinking with their life partners at home to cope with anxiety and depression during isolation. 54 These findings are critical and warrant immediate interventions, considering the long-term detrimental effects of chronic alcohol use, like hypertension, heart failure, stroke, and hepatic steatosis leading to cirrhosis. 55
Despite previous research suggesting the link, we did not find an association between sleep quality and ST before or during the COVID-19 pandemic. 56 Cellini and colleagues 36 also found that although people increased their use of digital media before bedtime, it did not affect sleep quality, corroborating our findings. However, a recent suggests that the amount of ST may not be the only factor, and it is more important to focus on percent change. 8 We also did not find any associations between BMI and sleep quality, indicating that there might be a complex relationship between the two, and this sample population may have a protective factor that has yet to be explored. 57 We also found no associations between employment status and sleep quality, as well as with student status.31,42 The discrepancy between findings could suggest that it is less about the role and more about stress levels, but a detailed study would need to investigate this theory more.
There are many limitations to this study. For one, our sample demographics are skewed to white/Caucasian and non-Hispanic/Latinx individuals, and from North America and Europe. Furthermore, a large portion of the sample size compromised students and females. No data was collected on a participant’s mental health or sleep disorder history. Lastly, we used subjective self-reported measures and less effective sleep quality measures.
Conclusion
Overall, young adults during the COVID-19 pandemic have exhibited poor sleep quality. Because sleep quality impacts psychological state, the immune system, and physical health, there needs to be targeted interventions and greater access to assessing and optimizing sleep quality in young adults. Our study found that it is highly tied to mental health factors, especially stress, and focusing on mental health and sleep quality may be the most beneficial step forward. However, it is also essential to tailor interventions for those with increased risk factors, like females, minority ethnicities, and Western countries. Lastly, there may be no direct evidence that quarantining results in poor sleep quality; rather, sleep quality should be more associated with mental health and stress.
Data Availability Statement
The data given this article are the raw data presented in this study are not publicly available, but senior author Michelle Wiciak can provide additional statistical analysis in response to a reasonable request. Participants received assurance that all responses would remain confidential within the research team with limited access to databases except the listed co-authors.
Footnotes
Acknowledgments
The authors would like to acknowledge the valuable contributions of Sreenivas Sappati-Biyyani and Alexis Sotomayor, all young adult participants who participated in the international survey, and support of the faculty of Saint James School of Medicine in the conduct of the study.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
All procedures performed in studies involving human participants were per the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
All participants included in the study participated in the informed consent process with an additional informed consent for all individual participants for whom identifying information is included in this article.
