Abstract
The current research describes the indicators of good nutrition among staff working in a hospital setting and determines if dietary indicators are associated with work-related burnout. In total, 501 staff of a large healthcare organization in SouthEast Queensland, Australia completed a health and wellbeing survey. Multiple regression models were constructed to describe the associations between dietary indicators and burnout, while controlling for age, gender, work role and level of employment. Among the total sample of healthcare workers, indicators of healthy eating were poor. Fewer than 40% reported their overall diet as very good and fewer than 15% of healthcare workers reported eating the recommended 5 or more servings of vegetables per day. There was an inverse relationship between good nutrition and burnout, across a range of indicators (including rating of overall diet, fruit and vegetable consumption and sharing meals with family), such that healthier eating indicators were associate with less burnout. Given that rates of both poor nutrition and burnout among healthcare professionals are high, findings from the current study suggest that efforts to promote better nutrition among healthcare workers are warranted. Future research may evaluate if improving the nutrition of healthcare workers has a positive impact on work-related burnout.
‘We found a statistically significant relationship between eating behaviour and burnout, such that indicators of poor diet were associated with greater burnout’.
Introduction
It is generally well-accepted that healthcare workers experience high rates of burnout. According to the World Health Organization’s International Classification of Diseases (ICD-11), burnout is a syndrome resulting from chronic and unmanaged workplace stress. It is characterized by feelings of exhaustion, mental distancing from one’s job and a sense of ineffectiveness. Measurement of burnout is imprecise as estimates of burnout vary widely. In studies of doctors, the prevalence of burnout ranges between 0% and 80%. 1 A systematic review of burnout in nurses estimated the global prevalence to be 11%, with significant differences by geographical region and specialization. 2 The COVID-19 pandemic put additional stress on healthcare workers and a national survey of American healthcare workers estimated that approximately half were experiencing burnout. 3
Burnout affects the health and wellbeing of workers, including healthcare workers. 4 Specifically, burnout has physical consequences included weight gain, chronic diseases (Type 2 diabetes, cardiovascular disease), pain disorders and early mortality. 4 Psychological consequences include sleep disturbances, depressive symptoms and symptoms of psychological distress. 4 In addition, burnout has consequences for the organization such as job dissatisfaction, absenteeism and resignation.4,5 In a national sample of nurses working in the US, among nurses who resigned from their job in the past year, more than 30% reported burnout as reason for their resignation. 5 For healthcare workers, burnout has additional consequences for the patient. These include lower levels of patient satisfaction and quality of care provided. 6
Evidence demonstrating the preventive role good nutrition plays in emotional wellbeing is well established. Systematic reviews have reported that diet quality and healthy dietary patterns play a protective role in preventing depression,7,8 anxiety 7 and cognitive decline. 9 The role nutrition plays in burnout is less understood, though a growing body of research suggests that poor diets may contribute to burnout among healthcare workers. A survey of doctors, nurses and residents working in hospitals in seven European countries found a positive relationship between burnout and fast food consumption. 10 Similar observations between greater burnout and indicators of poor diet have been made in studies of Dutch dentists 11 and employees working in other occupations (not healthcare).12,13 Moreover, new initiatives to prevent burnout among healthcare workers include promoting good nutrition as significant components of the intervention.7,14 This is important as the limited evidence available suggests that, in general, healthcare workers do not eat healthfully.15-17
The aim of the current study is to build on the body of research exploring the relationship between burnout and nutrition. Specifically, the aims of the current research are to describe the indicators of good nutrition among staff working in a hospital setting and to determine if dietary indicators are associated with work-related burnout.
Methods
A health and wellbeing survey amidst the COVID-19 pandemic was conducted with staff employed at Mater Health South Brisbane, a large healthcare organization in SouthEast Queensland, Australia. The primary aim of the survey was to explore how the COVID-19 pandemic affected the health and wellbeing of hospital-based staff. All staff (n = 6100) were invited to participate and, in total, 501 staff (88% female) completed the survey.
Invitations to participate in the survey were made through individual emails and reminders were sent via staff COVID email updates and staff online newsletters. Information about the research was provided with the invitation email and participants gave implicit consent given by starting the survey. The survey was administered online, via REDCAP, and was voluntary and anonymous. Participants could quit the survey at any time. The survey was open to staff for two weeks, between 17–31 August 2020. The Human Research Ethics Committee at Mater Research granted ethical approval for the survey.
The survey was conducted during a period where community transmission of COVID-19 was being actively managed. On 17 August 2020 (the first day of the survey), Queensland had 1091 confirmed cases of COVID-19 to-date and no community transmission for 28 days. On 20 August, a new community outbreak emerged bringing the total number of cases to 1122 by the completion of the survey. While the overall number of cases was low, concerns about community transmission and ultimate impact on the healthcare system were high. During this time, businesses were operating with COVID-safe plans and the state borders were closed. On 22 August 2020, Queensland Health announced restrictions limiting visitors to hospital.
Measures
All analyses were conducted using STATA/IC 16.1 software (College Station, TX). Proportions of each dietary indicator by work role were generated. Multiple regression models were constructed to describe the associations between dietary indicators and burnout, while controlling for age, gender work role and level of employment. All differences were considered to be statistically significant at
Results
In total, 501 staff (88% female; 10% male; 2% not specified) completed the survey. Of the participants, approximately 20% were under the age of 30, 24% were 30 to 39 years, 24% 40 and 49 years, 23% 50 to 59 years and 10% over the age of 60. Most participants were nurses (39%), 24% were hospital support staff, 17% were allied health workers, 15% were professional support staff and 10% were doctors (data not shown).
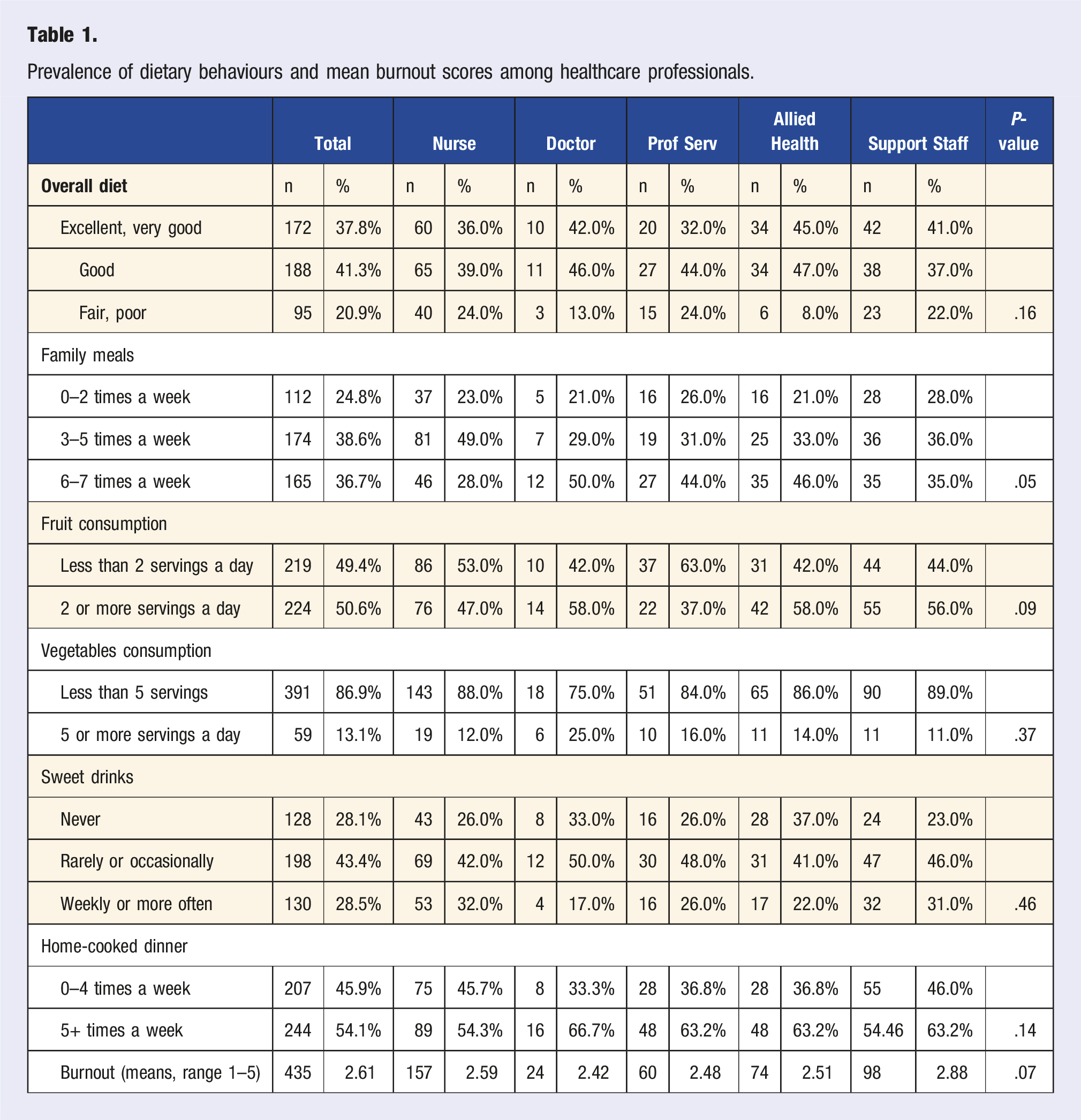
Prevalence of dietary behaviours and mean burnout scores among healthcare professionals.
Relationship between eating behaviours and burnout.
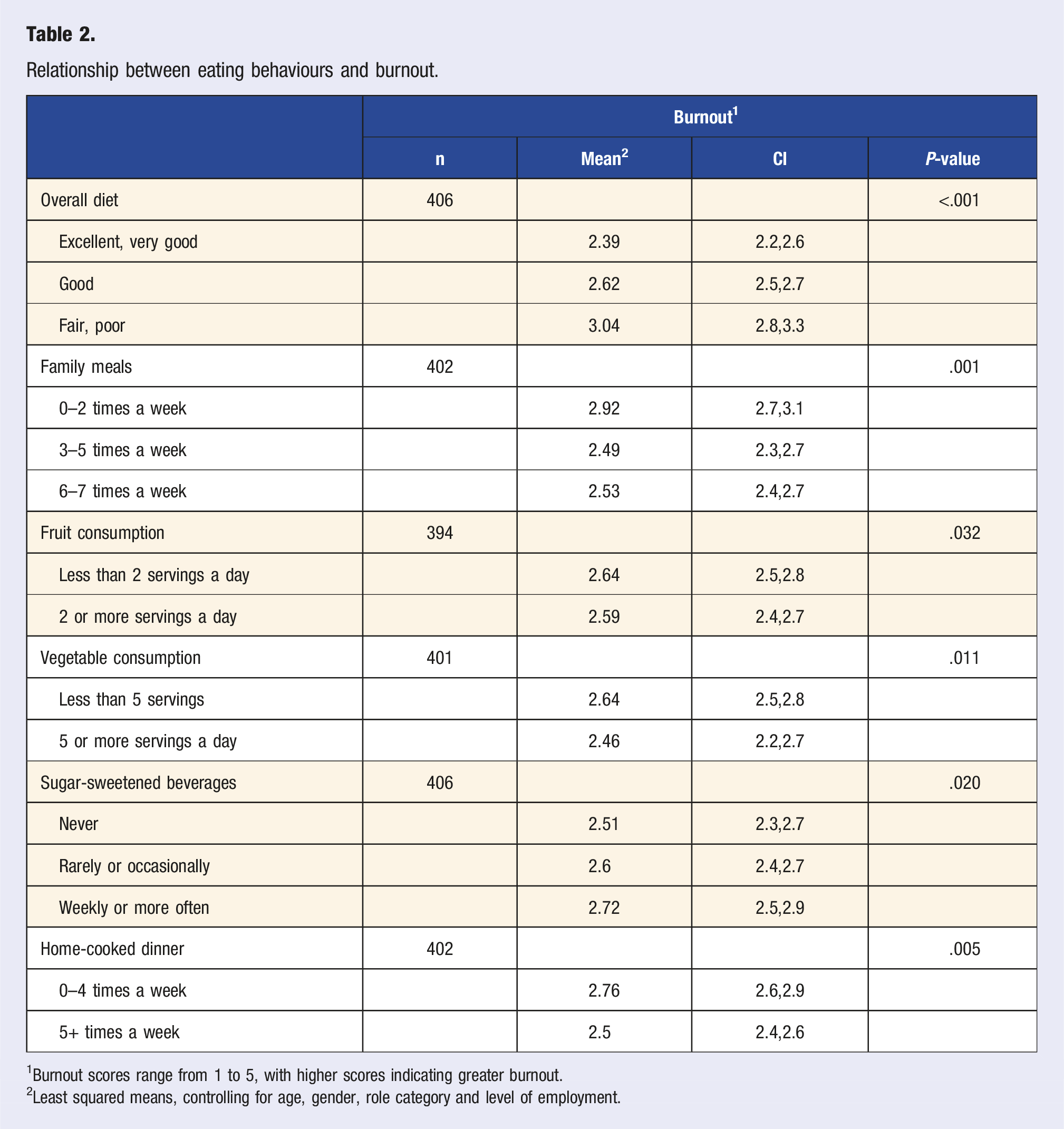
1Burnout scores range from 1 to 5, with higher scores indicating greater burnout.
2Least squared means, controlling for age, gender, role category and level of employment.
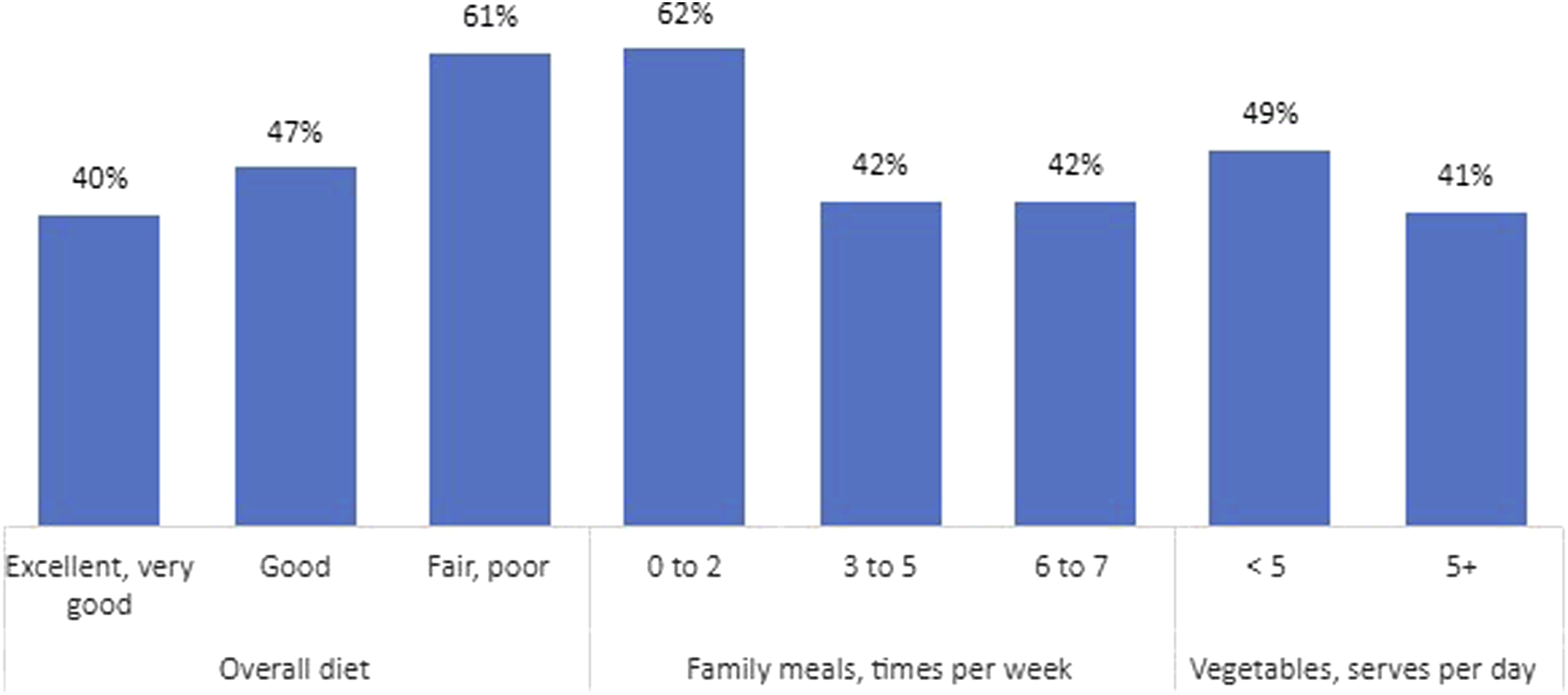
Prevalence of staff reporting any burnout, by selected dietary indicator. *Proportions reflect the percentage of staff who report any symptoms of burnout (equivalent to a score of 3 or higher). *Proportions are unadjusted. All relationships are statistically significant when accounting for age, gender, work role and level of employment.
Discussion
The current study aimed to describe the eating behaviours of healthcare workers and explore the relationship between indicators of good nutrition and burnout. Overall, we found that the healthcare workers participating in our study do not report eat healthfully, with few differences by work role. That is, doctors, nurses, allied health and non-clinical staff all eat too few fruits and vegetables and most do not report their diet very good or excellent. In addition, there was a significant relationship between dietary indicators and burnout, where poorer quality diet indicators were associated with greater burnout.
Findings of the current study, with regards to the poor eating behaviours of healthcare staff, are consistent with previous research of healthcare workers. A survey of more than 5000 nurses and midwives in Australia found that only 8% ate the recommended number of servings of fruits and vegetables daily. 16 A systematic review 17 of nurses in the US found that more than 50% were at risk of a poor diet and a separate study 20 found that a similar proportion (54%) had irregular meal patterns. While research exploring lifestyle behaviours of nurses is abundant, studies exploring health indicators of other healthcare staff is more difficult to find. That said, at least one study has examined the prevalence of overweight/obesity among various healthcare workers in England. 15 In the survey of more than 20,000 participants, the prevalence was high among all sectors of the workforce including nurses (60%), other healthcare professionals (49%), unregistered care staff (68%) and other staff (62%).
We found a statistically significant relationship between eating behaviour and burnout, such that indicators of poor diet were associated with greater burnout. These findings are consistent with previous studies of healthcare workers10,11 and those working in other occupations.12,13 The nature of this relationship cannot be determined with the current study. It is possible that poor diet may play a role in the experience of burnout among healthcare workers as poor nutrition is well-accepted as a modifiable risk factor for other mental health concerns.7-9 It is also possible that healthcare workers who are experiencing burnout at work may feel exhausted with other aspects of their lives, and this impacts their ability to eat well. Regardless, findings from the current study suggest that healthcare workers are in need of support to eat better. Interventions to support healthcare workers to eat healthier meals, share meals with their families and reduce their consumption of discretionary foods should result in a physically and emotionally well workforce, with potentially less burnout.
Strengths of the current study include the large sample size of healthcare workers broadly (not just nurses). Though there are a few limitations to consider when interpreting these findings. First, the response rate for the survey was low and the respondents may not represent all employees or any sub-category of employee. In addition, the survey was framed as a wellbeing survey during the COVID pandemic and that may have biased who responded. It is worth noting though that in Australian hospitals, approximately 40% of the staff are nurses and 10% doctors 21 and this breakdown is similar to who responded to the current survey. Second, the measures of dietary indicators in the current study were brief and not previously tested for validity and/or reliability. That said, these measures do not attempt to measure dietary intake comprehensively, rather they attempt to describe the key dietary behaviours associated with health. Third, the measures of dietary indicators were self-reported and subjective. It is possible that participants who were experiencing greater burnout may have reported their overall diet more poorly because of how they were feeling.
Rates of both poor nutrition and burnout among healthcare professionals are high. Findings from the current study suggest that efforts to promote better nutrition among healthcare workers may have a positive impact on work-related burnout. While more research testing the effectiveness of nutrition interventions on reducing work-related burnout is needed, it appears that some organizations are recognizing the significance of good nutrition for the wellbeing of their healthcare staff.7,14 Previous research found that healthcare staff support initiatives to improve the nutrition environment of hospitals, particularly those making healthy meals more accessible and affordable. 22 As hospital-based, healthcare workers are often required to work on weekends or through the night, interventions that improve the quality and availability of meals available onsite may be an effective first step towards improving the eating behaviours for staff. 23
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
