Abstract
Prevention and treatment of lifestyle-related diseases are realized through leading a healthy lifestyle. Activities supporting positive psychology can facilitate healthy behaviors and improve physiological health. Adding such activities to clinical care promotes attainment of the physical, social, and emotional elements of health, as defined by the World Health Organization—leading to (1) prolonged lifespan and quality of life, (2) lowered costs of care, and (3) reduced rates of provider burnout. A key challenge remains the translation of positive psychology–based practices into practical, implementable strategies by health care providers. An essential step is collaboration of positive psychology and health care researchers and practitioners to develop standards, terms, and measures and arrive at evidence-based clinical approaches addressing total well-being. The first Summit on Happiness Science in Healthcare enabled national experts and stakeholders in lifestyle medicine, medical education, health care administration, psychology, and community welfare to convene and identify best practices for practical implementation of positive psychology science into health care. This article draws on the summit discussions to address the gap between positive psychology theory and practical implementation in health care. We briefly summarize the positive psychology–health outcomes relationship and present key strategies needed to bridge this gap.
Keywords
“It is the dynamic, interactive, and multiplicative impact of physical and emotional healthy habits that promotes total well-being, including psychological well-being.”
Lifestyle-related diseases (LRDs) are a worldwide health concern, 1 affecting virtually all developed and modernizing countries and contributing 71% of the global burden of disease in 2016. 2 LRDs share predisposing risk factors related to unhealthy lifestyle, such as cigarette smoking, obesity, physical inactivity. and poor nutrition.3,4 Evidence also implicates mental health and social factors, such as stress, anxiety, and social isolation, as significant risk factors in LRDs.5,6 The latter risk factors are not well emphasized in clinical practice, despite significant data showing their influence on LRD severity and progression. 7 The complex interrelated factors in health and well-being may also explain, in part, other public health crises, including the opioid epidemic, increasing risky alcohol use among elderly individuals, and the rise in suicides in the United States.8-12
Prevention and reversal of LRDs can be achieved through adoption of healthier lifestyle habits.13-18 Promoting such habits requires addressing and ameliorating underlying causes of unhealthy behaviors, which can include negative emotional states that may not meet mental illness diagnostic criteria but can perpetuate unhealthy behavior patterns. 5 According to the World Health Organization definition, health includes physical, social, and emotional elements. Positive psychology, which studies the strengths that enable people and communities to thrive, 19 can have a significant role in addressing LRDs. Positive health, stemming from positive psychology practices, is an additional health asset that produces longer, healthy life and lowers disease risk and health care costs over and above disease risk factors addressed by traditional health care. Dissemination and implementation of positive psychology strategies by health care that assist health coaching and directly promote healthy physiological effects20,21 can have significant benefits, including improved emotional well-being, health outcomes, and quality of life22-28; decreased health care use29,30; lower health provider burn out 31 ; and increased longevity,32-35 with the potential for related benefits, such as enhanced social capital, volunteerism, and decreased violence and drug use. It is the dynamic, interactive, and multiplicative impact of physical and emotional healthy habits that promotes total well-being, including psychological well-being.36-60
The field of lifestyle medicine, which focuses on a healthy lifestyle for preventing and treating disease, has spearheaded the emphasis of positive psychology–based habits (such as gratitude practice) as a pillar of a healthy lifestyle. Positive psychology has been incorporated into training, standards, and certification exams, but the work of changing clinical practice to routinely include this pillar of health is in its infancy. Although community-based support can help patients implement and sustain healthy lifestyles outside the clinical setting, recommendations and attitudes of health care providers play a crucial role in engaging patients in treatment plans that promote emotional as well as physical well-being. Lack of consensus on practical translation is a problem that impedes adoption of these practices in the clinical setting.
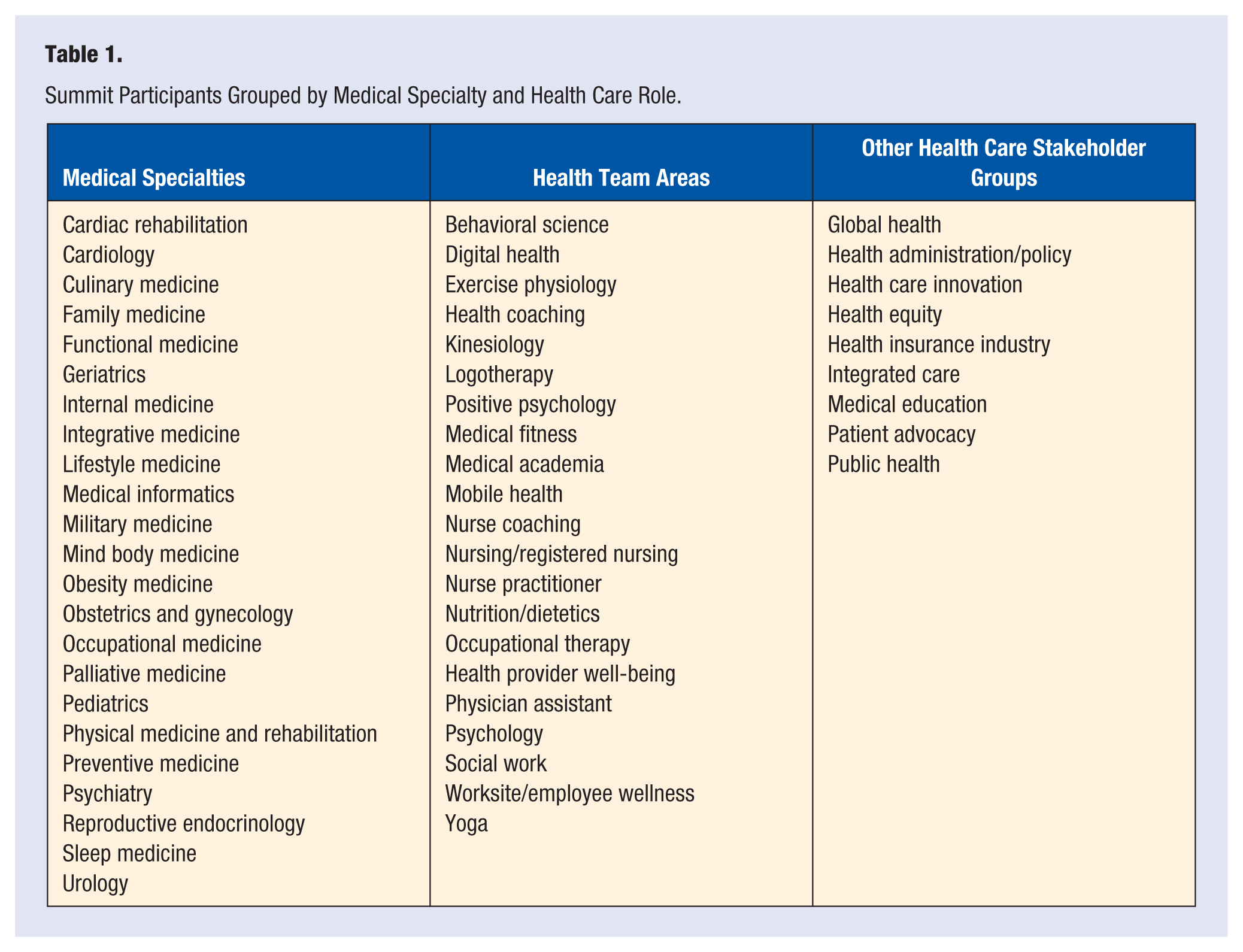
Progress can be made by involving key stakeholders and delineating their roles. The American College of Lifestyle Medicine (ACLM) and Dell Medical School convened the inaugural Summit on Happiness Science in Health Care in May 2018, inviting leaders in lifestyle medicine, positive psychology, and other areas of health care (Table 1). The goal was to recommend strategies for integrating positive psychology practices into health care communications, treatments, and patient and worker support programs (Table 2).
Summit Participants Grouped by Medical Specialty and Health Care Role.
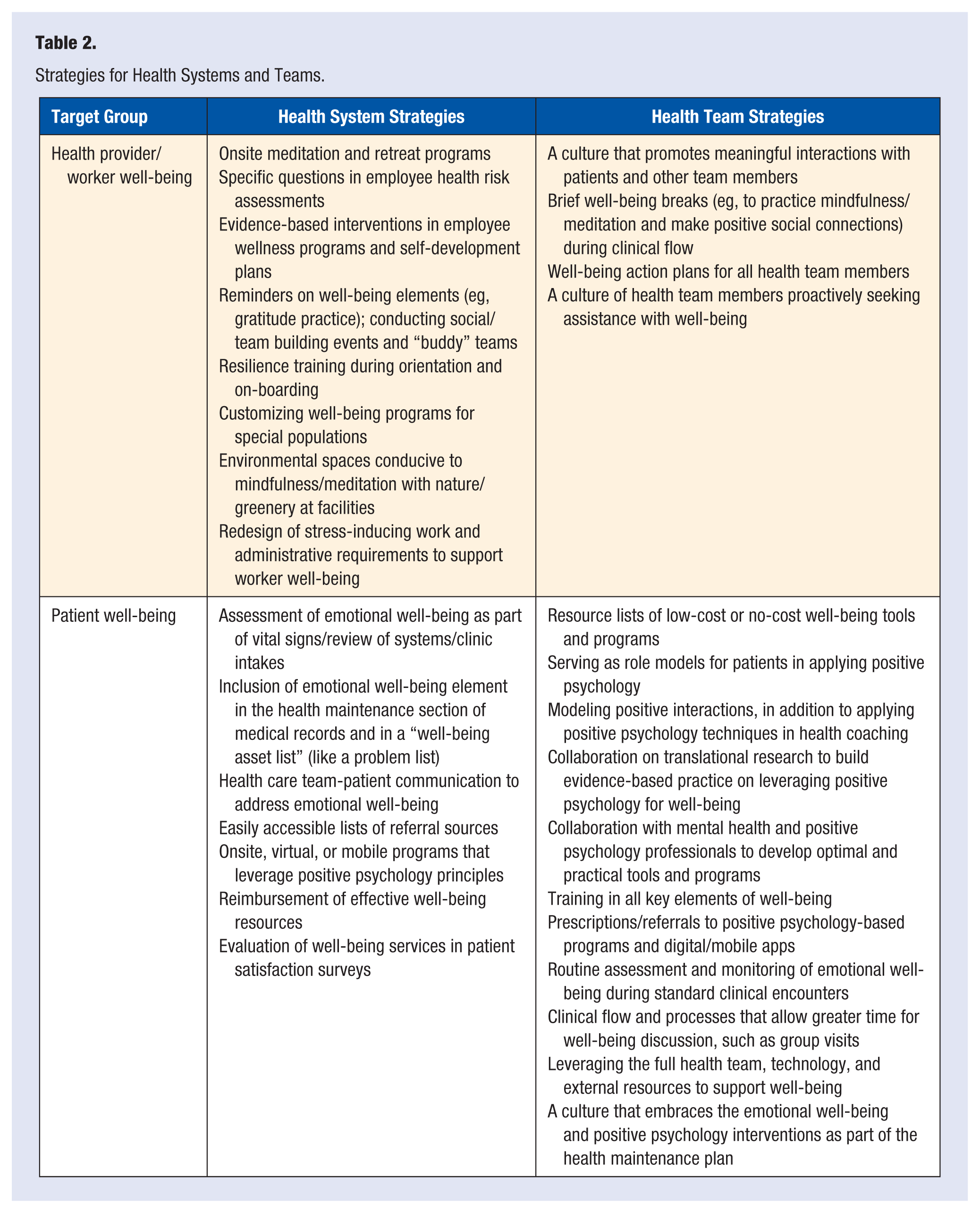
Strategies for Health Systems and Teams.
The ACLM, which advances professional competencies in its field, 61 is at the forefront of this shift, by recommending positive psychology practices, along with physical activity and healthy nutrition in treatment plans. The American Board of Lifestyle Medicine, which tests certification examinees on lifestyle medicine, has increased attention to the topic by adding positive psychology to its examination.
Terms and Definitions for Research and Clinical Applications
Positive psychology is the scientific study of the strengths, such as character strengths, positive relationships, and life purpose, that enable individuals and communities to thrive and lead meaningful and fulfilling lives.62,63 Positive psychology practices aim to increase positive emotions, cognitions, and behaviors and enable one to better navigate the inevitable negative emotions that occur with life challenges. Examples of these activities that can be adopted as healthy habits include gratitude, savoring, mindfulness, acts of kindness, forgiveness, meaningful activities, and prioritizing positivity. 22 Such habits can lead to positive health, which “focuses on promoting people’s positive health assets—strengths that can contribute to a longer, healthy life.” 64 Although tools and measures are being developed for several related terms, including psychological well-being, subjective well-being, happiness, and resiliency, these terms are not consistently used, and the nuanced definitions can be confused. Hence, the refinement and standardization of terms, definitions, and measures for use in health care and fields outside of the psychology are crucial for cross-discipline research, clinical application, and best practice guidelines.
This article uses the terms healthy lifestyle to refer to physical habits that lead to health; positive psychology for habits that can lead to mental, emotional, and positive health; and total well-being for physical, emotional, social, and positive health.
The Healthy Lifestyles and Positive Psychology Link for Health
All major elements of a healthy lifestyle, including a whole-food, plant-based diet, consistent moderate- to high-intensity physical activity levels and adequate, quality sleep, improve emotional and total well-being.36-60 Loneliness, depression, and isolation can worsen perception and severity of chronic disease and affect mortality; hence, social health is another key health element.65-70
Positive psychology practices such as sustained gratitude and mindfulness practices and ongoing activities that promote life purpose have been associated with a wide range of health-related behavioral and physiological effects, including fewer strokes and myocardial infarctions 71 ; lower body mass index, lipids, hemoglobin A1C, and insulin resistance; better heart rate variability among other risk factors72,73; declining health care use 74 ; increased use of preventive services 29 ; engagement in healthy eating and physical activity 30 ; and longevity.70,75 Such practices are also associated with greater self-efficacy, self-control, adherence, inflammatory markers, immune function, cognitive capacity, and neuroplasticity as well as reduced pain, analgesic use, anxiety, depression, hostility, and stress.23,24,76,77
People who report a greater number of happy moments are more prone to exercise, not smoke, use seat belts, eat well, drink alcohol in moderation, stay married, and have prosocial behaviors and better work productivity.25,26 Positive emotions are not only associated with promoting behavior change, but also with physiological benefits. Wound healing, inflammation, telomere length, and endocrine regulation are among many physical processes that are associated with emotion27,28,32-34,78 and happiness. 36 Even fleeting positive “micro-moments” contribute to total well-being24,79-81 health and longevity.19,20 The summit leaders recommended that leader organizations aggregate the evidence-based positive psychology practices that can be referenced by health care settings. An example is the Greater Good in Action online resource with brief, practical guides to science-based practices for a positive and meaningful life.
Involvement by Stakeholder Groups to Advance Total Well-being
A multilevel, coordinated approach involving multiple stakeholders is associated with improved health outcomes and changes at a population health level. 82 Hence, the advancement of total well-being with positive psychology practices as a standard element of health care will require communication, coordination, and collaboration with multiple stakeholder groups, including health organizations, government, fitness industry, health insurance industry, and community organizations as well as providers and individuals. Each group has a role that can enhance the work of other stakeholders. Strategies presented here focus on health care systems and teams to promote health worker and patient total well-being (Table 2).
Health care leaders can champion this movement to disseminate the science in positive psychology relevant to health care settings, providers, and teams; translate the evidence into practical programs, applications, and skill building tools; develop training programs; and leverage outcomes data and compelling stories. Clinicians can seek to deepen the provider-patient relationship by opening up about how they face challenges, encouraging patients to open up, asking positive questions (such as what is going well?), and building treatment plans based on patients’ strengths and values. Clinicians can also leverage gratitude and hope and work with health systems to promote meaningful roles. Ultimately engagement by all stakeholders can propel this vision as standard care.
An essential, initial step is forging partnerships between the lifestyle medicine/health care community and positive psychology community to integrate evidence-based practices into medical and health professional education. Summit leaders unanimously agreed that a foremost priority is to address the well-being of health care providers, which not only enhances quality and safety for all, but also has the potential to springboard their shift in clinical practice through a personal experience of the benefits of a healthy lifestyle with positive psychology habits.
In the era of an explosion of digital health services and products, those focused on behavioral health and positive psychology can serve as tools to support providers who prescribe healthy habits and refer for interventions. Providers of low-income patients can recommend simple, low, or no cost, empirically based activities that boost total well-being such as mindfulness or time in nature.83-85
As the key role of positive psychology in health is showcased and the contributions of stakeholders to increase these services and supports are harnessed, our society will reap significant benefits. In fact, a broad array of benefits noted in this article can result, including improved health outcomes and quality of life, increased longevity, and decreased health care use and provider burn out.
Acknowledging Challenges
In the evolving health care system, integration of healthy lifestyle interventions, especially with positive psychology elements, faces barriers. As interest in the critical role of these interventions in the prevention and treatment of chronic diseases increases, we will need to address implementation challenges. Inadequate reimbursement for the counseling and support remains a primary hurdle. The need for further research on the role of positive psychology in health, lack of awareness by patients and providers about the impact of positive psychology on health, and inadequate professional training and practice guidelines are a few additional challenges. Initial steps to incorporate evidence-based positive psychology approaches into total well-being plans are encouraged while we identify solutions to address barriers. An example is engaging providers to add positive psychology activities to healthy lifestyles prescriptions, such as gratitude practice, along with eating a whole-food, plant-based diet and being physically active.
Conclusion
Health is more than the absence of disease; health is physical, social, and emotional well-being. It also includes positive health—resulting from positive psychology-based habits that produce longer, healthy life and lower disease risk and health care costs—over and above the risk factors addressed by traditional health care. A shift toward integration of positive psychology practices has the potential to empower the health care and public health communities to more effectively address current and emerging crises, such as skyrocketing obesity and diabetes rates, the opioid crisis, the new epidemic of loneliness, and rapidly rising provider burn out. Hence, we urge health care and other stakeholders to take action and support this movement by communicating on this issue, disseminating and adopting feasible strategies, and collaborating in research and practical resource development.
Footnotes
Acknowledgements
We would like to acknowledge the members of the American College of Lifestyle Medicine’s Happiness Science and Positive Health Committee who provided guidance to this article: Carrie Barron, Susan Benigas, Ingrid Edshteyn, Kristen Collins, Janani Krishnaswami, Jenny Lee, Noémie Le Pertel, Liana Lianov (chair), Rachel Millstein, Quinn Pauly, Joe Raphael, Sondra Redmont, David Ring, Deepa Sannidhi, and Anne Wallace. We also would like to acknowledge the Summit on Happiness Science in Health Care presenters whose contributions led to this article: Marc Braman, Rhonda Cornum, Edward Diener, Angie Kalousek Ebrahimi, Steve Flowers, Barbara L. Fredrickson, Peter Giza, Sean Hashmi, Leif Hass, Gail Ironson, Andrea Klemes, Jessica Matthews, Rachel A. Millstein, Michael P. O’Donnell, Dean Ornish, Michael D. Parkinson, Edward M. Phillips, Patty Purpur de Vries, David Ring, Mark Rowe, Michael Steger, and Blaine Wilson.
Authors’ Note
This article is based on a workshop given at the Annual Meeting of the American College of Lifestyle Medicine 2018 in Indiana, IN.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
Not applicable, because this article does not contain any studies with human or animal subjects.
Informed Consent
Not applicable, because this article does not contain any studies with human or animal subjects.
Trial Registration
Not applicable, because this article does not contain any clinical trials.
