Abstract
Although yoga may help manage conditions comorbid with overweight and obesity, such as low back pain, whether yoga helps with weight loss or maintenance beyond that which can be achieved with diet and exercise remains unclear. A search of multiple databases through September 2012 was undertaken identifying peer-reviewed studies on yoga, meditation, mindfulness, obesity, and overweight. Studies on yoga and weight loss are challenged by small sample sizes, short durations, and lack of control groups. In addition, there is little consistency in terms of duration of formal group yoga practice sessions, duration of informal practices at home, and frequency of both. Studies do however suggest that yoga may be associated with weight loss or maintenance. Mechanisms by which yoga may assist with weight loss or maintenance include the following: (a) energy expenditure during yoga sessions; (b) allowing for additional exercise outside yoga sessions by reducing back and joint pain; (c) heightening mindfulness, improving mood, and reducing stress, which may help reduce food intake; and (d) allowing individuals to feel more connected to their bodies, leading to enhanced awareness of satiety and the discomfort of overeating. Thus, yoga appears promising as a way to assist with behavioral change, weight loss, and maintenance.
‘Although the practice of yoga may help overweight or obese individuals manage comorbid conditions . . . whether it helps with weight loss . . . remains unclear.’
Yoga is one of the most popular types of complementary and alternative medicine (CAM) practiced in the United States and is used far more often than any other type of CAM for weight loss or maintenance. 1 In 2007, 6% of adults reported practicing yoga, an increase of nearly 20% from 5 years earlier. 2 This rise in popularity might be expected given that more than 50 conditions are reported to benefit from regular practice. 3 Overweight or obese individuals are less likely to practice yoga than those who are normal-weight, 4 yet 40% of yoga practitioners are overweight or obese. 5
Yoga is a mind–body, or meditative movement, practice originating in ancient India that combines physical postures (asanas), breathing exercises (pranayamas), and meditation or relaxation. 6 The most common form practiced in the United States is Hatha yoga, which includes the yoga styles Ananda, Anusara, Ashtanga, Bikram, Iyengar, Kripalu, Kundalini, and Viniyoga. 6 These styles chiefly differ in the intensity of physical activity and strength training and in the emphasis placed on postures, breathing, and meditation. 7 A typical yoga session is a group class lasting 60 to 90 minutes led by an experienced teacher. 8 The session begins with a short period of meditation or relaxation (5-20 minutes), followed by a series of postures designed to build flexibility and strength (30-60 minutes), and concluding with a period of rest used to create deep physical and mental relaxation (5-30 minutes). 8 Individuals can practice each step of the session at home. Throughout the session, there is a focus on breathing with an aim to stimulate mental focus and body awareness.
Although the practice of yoga may help overweight or obese individuals manage comorbid conditions, such as low back pain,9,10 whether it helps with weight loss or maintenance beyond that which can be achieved with a calorie-reduced diet and increased exercise remains unclear. The purpose of this review was to summarize the evidence on yoga’s relation to weight loss and maintenance, paying particular attention to its impact on behavior, neuropsychology, metabolism, and inflammation. The review then provides the basis for recommendations on yoga practice in the management of weight loss and maintenance.
Methods
We searched for English language, peer-reviewed articles in PubMed and the Cochrane Collaboration database through September 2012 using key words in titles and abstracts such as yoga, meditation, mindfulness, obesity, and overweight. We reviewed references of identified articles to identify additional relevant articles and searched for articles written by authors known to have written extensively in the field of interest. Systematic reviews, meta-analyses, randomized controlled trials, clinical trials, and prospective cohort studies were included.
Results
Weight Loss and Management of Comorbid Conditions
There is a large body of evidence relating yoga to management of chronic conditions associated with overweight and obesity. Much of this research has been conducted by Indian investigators and published in Indian journals. 11 Yoga improves back9,10,12-15 and joint 16 pain; depression17-22 and stress/anxiety21,23; and insulin resistance, hypertension, and dyslipidemia.24-28 It also improves musculoskeletal flexibility.29,30 Limited data suggest that yoga may improve coronary artery disease and its risk factors by lowering blood pressure, increasing absolute and relative oxygen uptake, improving heart rate variability, decreasing sympathetic tone and baroreflex sensitivity, and slowing atherosclerosis.28,31 Yoga does not appear to help with asthma 32 or diabetes, 33 both of which may develop or worsen in the setting of excess body weight. Limited data prevent any conclusions to be drawn regarding effectiveness of yoga in pediatric populations.34,35
In contrast to data on comorbid conditions, data are more limited with regard to weight reduction and maintenance. One cross-sectional analysis reported that a greater number of hours of yoga practice over one’s lifetime were associated with a small but significantly lower body mass index (BMI) among middle-aged women (mean BMI of 24 for 1-2500 lifetime hours vs BMI of 20 for more than 15 000 hours), after adjusting for consumption of processed food and weekly exercise. 36 One prospective study observed that yoga practice (at least 30 minutes once per week) for 4 or more years was associated with a 3 lb lower weight gain among normal weight (BMI < 25) participants (9.5 lb vs 12.6 lb) and an 18 lb lower weight gain among overweight participants (−5.0 lb vs 13.5 lb; P for trend < .001 for both) even after accounting for diet and physical activity; among overweight individuals, 4 or more years of yoga practice was associated with a relative odds of 1.85 (95% confidence interval [CI] = 0.63-5.42) for weight maintenance (within 5%) and 3.88 (95% CI = 1.30-9.88) for weight loss (>5%) compared to weight gain (P for trend .03 and <.01, respectively). 8 In a randomized controlled trial of postmenopausal women, 16 weeks of yoga, compared to no exercise, led to decreases in body weight (3.9 kg), percent body fat (3.1 %), BMI (1.7 units), and waist circumference (1.7 cm). 37 Sixty patients with type 2 diabetes had a 2 kg decrease in weight after practicing yoga for 45 minutes each day for 45 days when compared to those who did not practice at all. 38
Several randomized controlled trials of patients with coronary heart disease have shown that participation in a lifestyle modification program (including, for instance, a low-fat vegetarian diet, stress management, exercise, and smoking cessation) with yoga leads to reduction in body weight, as well as of regression in atherosclerosis at 1 and 5 years.31,39-41 BMI decreased from a baseline of 32 to a BMI of 30, 30, and 31 at 4, 12, and 24 months, respectively in 28 women randomized to a comprehensive lifestyle modification program with yoga. 42 Two single-arm intervention studies, one of which included a vegetarian diet, both approximately 1 week in duration with 3 to 5 hours per day of yoga, reported small but significant decreases in BMI (0.4-0.5 units) or weight (0.6 lb).43,44 After 3 months of yoga and meditation in a single-arm study, there was a significant decrease in waist circumference (5 cm) among obese adults, 45 and while overweight and obese breast cancer survivors randomized to 6 months of yoga, versus waitlist control, experienced no weight change, they too had a decrease in waist circumference (3.1 cm [95% CI = −5.7 and −0.4]). 46 This change may indicate a gain in lean muscle mass and loss of abdominal fat. Four months of supervised stretching and yoga for 16 elderly men and women yielded no change in abdominal fat. 47 BMI decreased by only 0.2 units on average in 54 middle-aged adults after practicing yoga for 60 minutes 3 times per week for 8 weeks. 48
In teenagers, 8 weeks of yoga, compared to no exercise at all, led to a decrease in body fat percentage (4.3%) but no change in body weight or BMI. 49 A 5-month multicomponent behavioral intervention with yoga was associated with significant decreases in BMI z scores (−0.15 in z score in intervention participants compared with −0.08 in usual care participants; P = .01) among obese adolescent girls. 50 After 12 weeks of yoga among 20 teenagers, weight decreased by 2 kg, 51 and after 16 weeks there were similar decreases in weight among 53 obese adolescent girls. 52
Thus, there have been few studies on the relation between yoga and weight loss, and no randomized controlled trial has yet isolated the effect of yoga on weight loss beyond that obtained from diet and exercise. Studies to date on yoga and weight loss are challenged by small sample sizes, short follow-up, and lack of control groups. In addition, there appears little consistency in terms of duration of formal group sessions, duration of informal practices at home, and frequency of both. Nevertheless, studies suggest that yoga may be associated with weight loss or maintenance. It has been noted as well that people with an interest or belief in the benefit of yoga are more likely to participate in studies than those who are indifferent; for this reason, and since participants cannot be blinded to treatment, study results are likely to be biased toward yoga. 53 This bias can be mitigated by recruiting participants who are neutral in their attitude toward all treatment arms or to stratify for such attitudes during randomization. 53
Neuropsychology and Behavior
Multiple mechanisms may explain associations observed between yoga and weight loss and maintenance. Although nonstrenuous yoga practice may not substantially influence energy balance, 54 a vigorous session may result in a 250 kcal expenditure.8,55 Moreover, muscle and joint stretching during yoga may alleviate back pain, which in turn may allow for increased exercise. Yet the ability for yoga to facilitate weight loss or maintenance may chiefly be through its effects on neuropsychology and behavior (Figure 1).
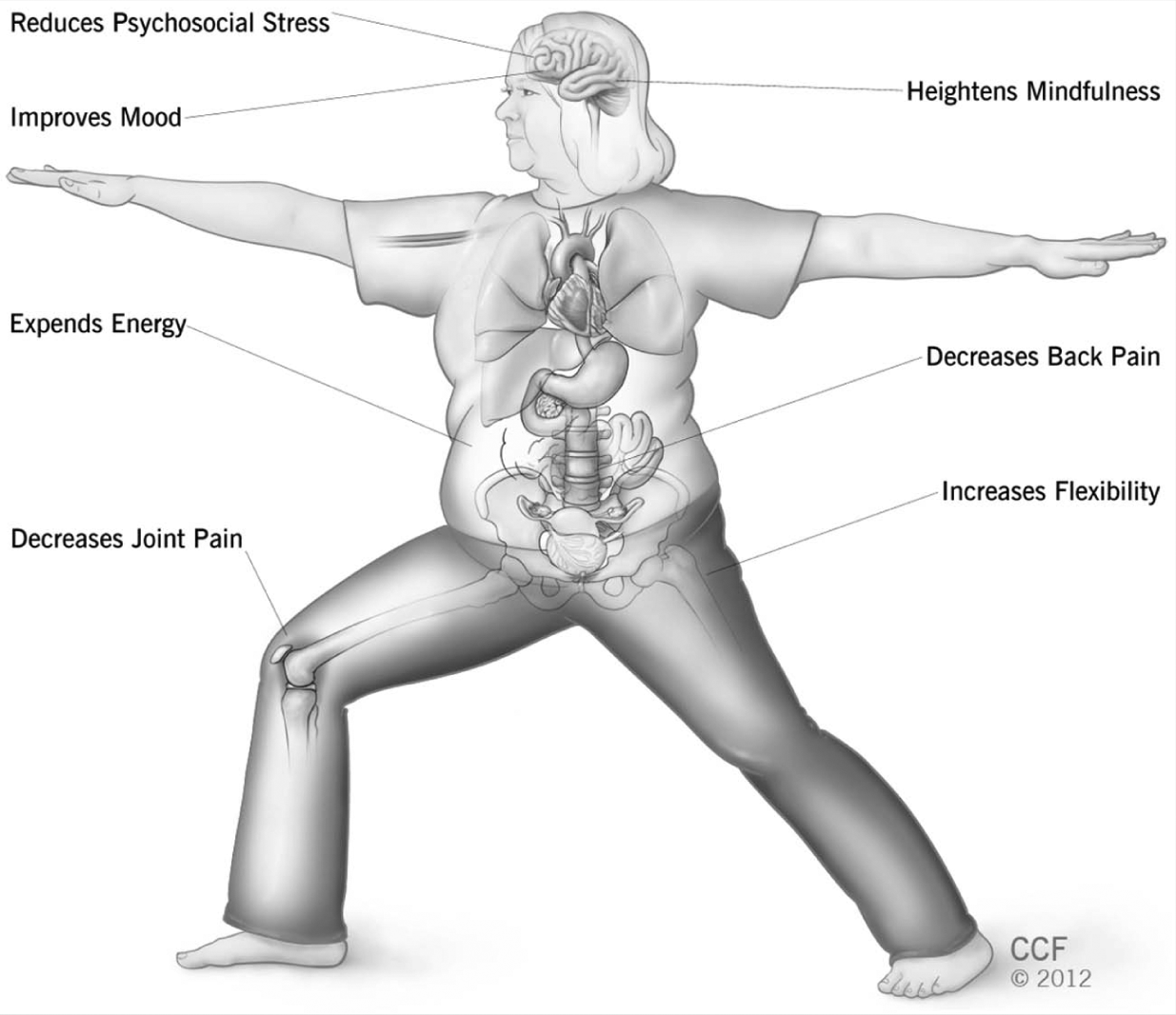
Benefits of Yoga in the Management of Overweight and Obesity.
Attention to the breath and body position during yoga practice is a form of mindfulness training. This mindfulness is characterized by a heightening of the following activities: (a) observing (attending to, or noticing, internal and external stimuli, such as sensations, emotions, cognitions, sights, sounds, and smells); (b) describing (noting or mentally labeling these stimuli with words); (c) acting with awareness (attending to one’s current actions, as opposed to behaving automatically or absent-mindedly); (d) nonjudging of inner experience (greater objectivity, or refraining from evaluation of one’s sensations, cognitions, and emotions); and (e) nonreactivity to inner experience (allowing thoughts and feelings to come and go, without attention getting caught up in them).56,57 In the brain, mindfulness may be related to changes in activation of regions involved with attention (prefrontal cortex), conflict resolution (dorsal anterior cingulated cortex), and emotional processing (medial/orbitofrontal cortices). 58 Moderate-to-severe stress appears to increase growth of the amygdala and shrink the prefrontal cortex and hippocampus, whereas stress reduction leads to decrease in amygdala volume. 59 Although yoga is actually considered a type of meditation, 60 yoga is associated with improvements in more areas of mindfulness than is sitting meditation. 57
Increased mindfulness may be a key component to weight loss. 61 Heightened mindfulness of the body and its behaviors may spill over from the yoga practice to everyday life. This mindfulness in turn may help individuals address emotional eating (eating in response to negative emotions such as boredom, stress, or sadness) and external eating (eating in response to food-related stimuli such as the taste, sight, or smell of palatable foods), both of which have been associated with weight gain, and control of which have been associated with weight loss. 61 In addition, mindfulness may lead to greater positive outcomes expectancies (self-control, self-confidence), which correlate with weight loss in a bidirectional manner. 42
Mindfulness-training through yoga may also generate the relaxation response outside the yoga session, which can offset the physiological effects caused by perceived stress, 62 acutely and long-term. 63 The sense of relaxation that comes with the relaxation response occurs as a result of decreased oxygen consumption and carbon dioxide elimination; reduced blood pressure, heart rate, and respiratory rate; and low-frequency heart rate oscillations. 64 Alterations in neural oscillations (brain waves) may also occur. 65 Changes in sympathetic and parasympathetic neural activity result as certain yoga practices slow respiration to a rate that coincides with the frequency of Mayer waves (rhythmic fluctuations in blood pressure and heart rate under the control of the autonomic nervous system). 63 By overlapping respiratory rate and cardiovascular rhythms, sympathetic and vagal outflows synchronize, cerebral blood flow changes, and a sense of well-being develops. 63 The net effect is such that the relaxation response helps individuals cope with stressful situations that may lead to addictive behaviors, 65 such as comfort food overconsumption. 66
Inflammation and Metabolism
Obesity is characterized by systemic inflammation: levels of pro-inflammatory mononuclear cells, interleukin-6 (IL-6), tumor necrosis factor-α (TNF-α), C-reactive protein (CRP), and matrix metalloproteinase-9 are all higher in obese individuals compared to normal-weight controls. 67 Fat cells secrete many of these pro-inflammatory cytokines, which in turn are linked with obesity-related chronic conditions, such as cardiovascular disease 67 and fatty liver. 68 Physical fitness, beyond helping to minimize body fatness, is associated with lower systemic inflammation.69-71 In contrast, psychological stress72,73 and depression 74 are associated with higher levels of inflammation. When compared to yoga novices (those who practice yoga ≤12 times in their lives), experts (those who have practiced yoga 1 to 2 times per week for at least 2 years and at least twice per week for past year) have been found to have lower levels of inflammatory IL-6. 75 The cause remains uncertain; however, rather than resulting from the physical postures or breathing exercises, immune modulation likely derives from psychosocial stress reduction from the meditative or relaxing component of yoga since similar changes have been observed in studies of meditation.76-78
The adipocytokines leptin and adiponectin, both secreted by fat cells, may augment or dampen inflammation: leptin stimulates monocyte and T-cell release of IL-6 and TNF-α, activates macrophages, and promotes CRP production; adiponectin enhances production of anti-inflammatory IL-10 and decreases CRP, IL-6, and TNF-α. 30 Leptin also acts to decrease appetite and increase energy expenditures, and exogenous leptin administration has been shown to stimulate sympathetic nervous system activity, which in turn has been associated with the development of insulin resistance and an increase in cardiovascular disease risk. 79 Greater frequency and years of yoga practice have been associated with lower leptin levels and a higher adiponectin-to-leptin ratio, independent of BMI, cardiorespiratory fitness, central adiposity, and mood. 30 In addition, several,80-84 but not all,85,86 recent studies also suggest that regular yoga practice decreases circulating cortisol, exposure to which has been associated with higher leptin 87 and visceral adiposity. 88
In obese individuals, leptin resistance may develop and its sympatho-excitatory role may be depressed, leading to weight gain and lower than expected blood pressures. 89 Low sympathetic nervous system activity may be a risk factor for weight gain, but sympathetic activity increases in response to weight gain, thereby attenuating the original impairment. 90 As increased sympathetic activity may be associated with increased energy expenditure, 90 yoga’s ability to attenuate such activity may be counterproductive to weight loss. 91
Discussion
Current recommendations for the lifestyle management of obesity include a low-calorie diet (eg, a deficit of 500-1000 kcal/day), physical activity (at least 30 minutes or more of moderate-intensity exercise most days of the week), and behavior therapy (strategies that provide tools for overcoming barriers to compliance with dietary and physical activity recommendations). 92 Yoga may be considered a form of behavioral therapy. However, yoga does not incorporate all the components of behavioral therapy (self-monitoring, stimulus control, problem solving, contingency management, cognitive restructuring, and social support) and is thus not a replacement. 92 However, yoga may act as a stepping stone to more intense behavioral therapy. Moreover, compared to other mindfulness practices, such as the body scan or sitting meditation, yoga may more easily allow for the transfer of mindfulness into everyday life since it requires attention to the body while it is moving. 57
The regular practice of yoga may assist the lifestyle management of overweight and obesity by (a) increasing energy expenditure during practice sessions; (b) facilitating exercise outside of the sessions by reducing back and joint pain; (c) heightening mindfulness, improving mood, and reducing stress, which may reduce food intake; and (d) allowing practitioners to feel more connected to their bodies, leading to enhanced awareness of satiety and the discomfort of overeating. 8 In addition, obese individuals have reported lower levels of pleasure during exercise than nonobese individuals, 93 and exercise intensity is perceived to be higher in obese than normal-weight individuals. 94 Yoga may be a stepping stone, or precursor, to more vigorous physical activities. 8 Moreover, the commitment and discipline of regular yoga practice, as well as the sense of community and support of group classes, may prepare an individual for diet and physical activity changes. 8
Conclusions
Yoga may be most beneficial in the treatment of overweight and obesity before an individual begins a diet and exercise program. Although no guidelines currently exist for such a prescription, based on our experience, we propose the following: 3 months of formal, instructor-led yoga classes of 45 to 60 minutes once or twice per week. This schedule allows for the individual to become comfortable with yoga and begin to develop mindfulness and relaxation and physical benefits. The practitioner can do the yoga standing or sitting, depending on comfort and comorbid conditions (Figure 2 and Supplementary Figures [the online supplement figures are available at http://ajl.sagepub.com/supplemental]). She should practice on her own for 20 minutes each day on which there are no group classes. During these informal sessions, the individual can do an abbreviated program, beginning with a short period of meditation or relaxation (5 minutes) followed by a series of postures (15 minutes), and ending with a period of rest (5 minutes). As the practitioner becomes more comfortable and proficient with yoga, she may include additional postures and more frequent or longer periods of practice. She may start a diet and exercise weight loss program after 3 months, unless motivated to do so earlier. Ideally, the individual will continue with as much of the formal and informal yoga sessions as possible once the diet and exercise changes begin.
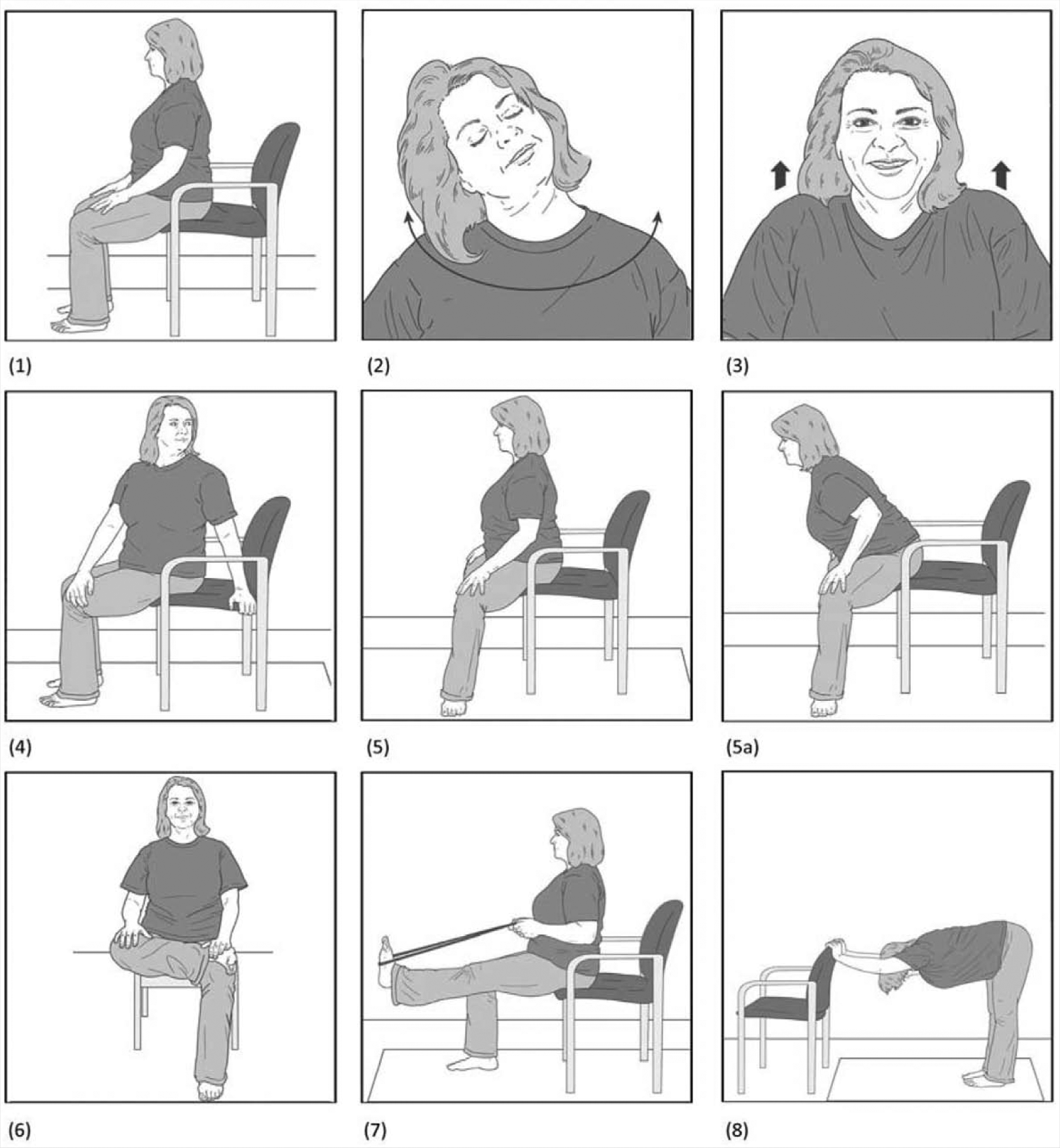
Yoga Poses in the Management of Overweight and Obesity.
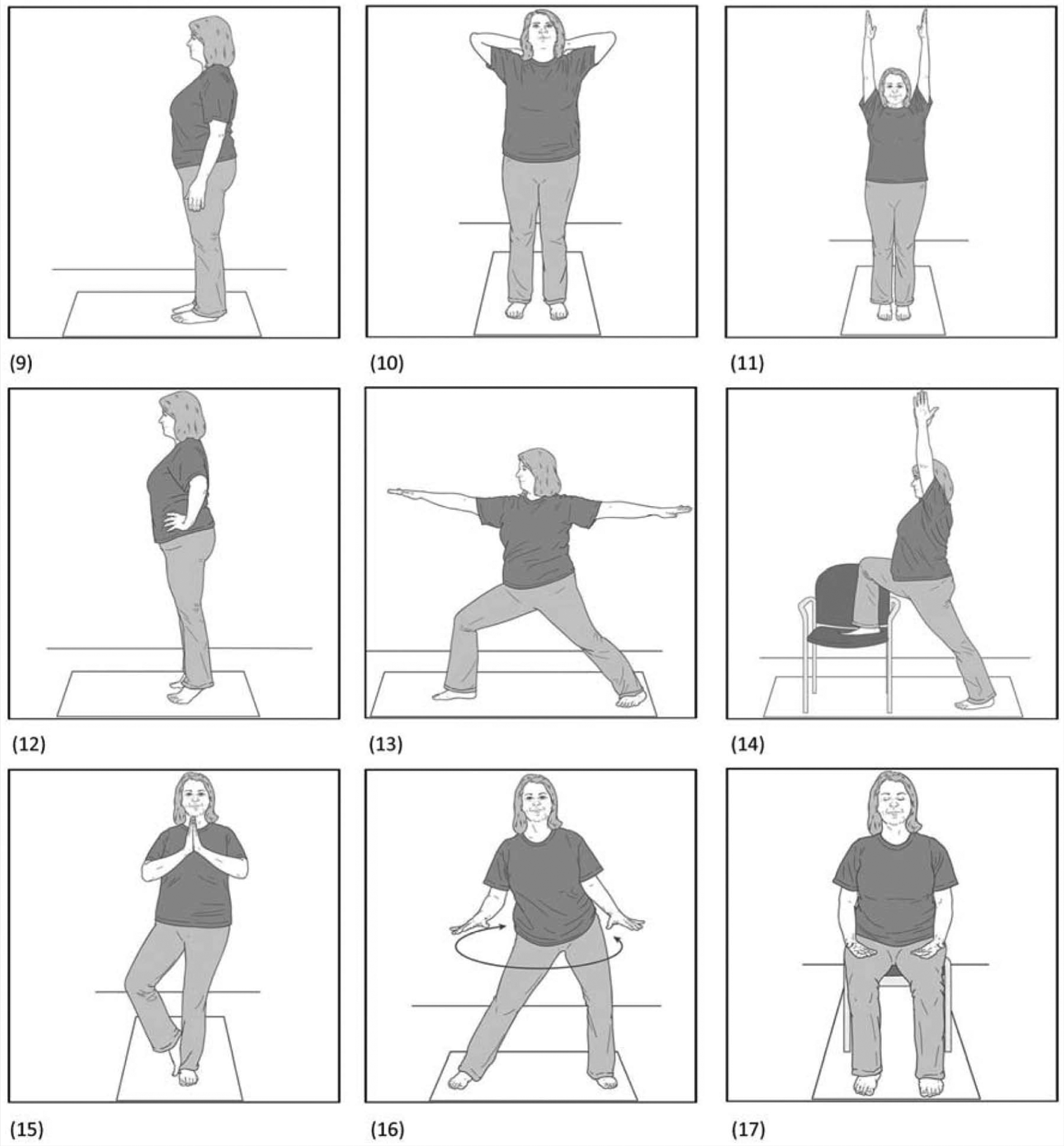
Yoga Poses in the Management of Overweight and Obesity.
There are few risks, side effects, or adverse events associated with yoga practice. Muscle strain may be the most likely. However, one should confer with a physician before starting the recommended yoga program. Any pain during yoga practice is reason to stop and discuss the pain with a yoga instructor or physician. As with any physical activity, caution is recommended for individuals with cardiac or pulmonary disease and consultation with a physician is recommended. Although individuals with chronic obstructive pulmonary disease and hypertension appear disinclined to do yoga, 5 whether this reflects a fear that yoga may compromise breathing or elevate blood pressure is uncertain, but no evidence to date suggests this happens with any regularity.
Footnotes
Acknowledgements
We would like to thank Ken Kula, Ross Papalardo, Amanda Mendelsohn, and Precious Lopez for help with preparation of the figures. The research was supported by institutional funds of the Cleveland Clinic Wellness Institute.
