Abstract
There is now a significant amount of research that demonstrates the health benefits of vegetarian and plant-based diets, which have been associated with a reduced risk of obesity, diabetes, heart disease, and some types of cancer as well as increased longevity. Vegetarian diets are typically lower in fat, particularly saturated fat, and higher in dietary fiber. They are also likely to include more whole grains, legumes, nuts, and soy protein, and together with the absence of red meat, this type of eating plan may provide many benefits for the prevention and treatment of obesity and chronic health problems, including diabetes and cardiovascular disease. Although a well-planned vegetarian or vegan diet can meet all the nutritional needs of an individual, it may be necessary to pay particular attention to some nutrients to ensure an adequate intake, particularly if the person is on a vegan diet. This article will review the evidence for the health benefits of a vegetarian diet and also discuss strategies for meeting the nutritional needs of those following a vegetarian or plant-based eating pattern.
Keywords
Introduction
A vegetarian is someone who consumes a diet consisting mostly of plant-based foods, including fruits, vegetables, legumes, nuts, seeds, and grains. Some vegetarians also consume eggs and dairy products.
There are 4 main types of vegetarian diets: (1) a lacto-ovo-vegetarian consumes dairy products and eggs but no meat, poultry, or seafood; (2) a lacto-vegetarian eats dairy products but not eggs, meat, poultry, or seafood; (3) an ovo-vegetarian eats eggs but no dairy products, meat, poultry, or seafood; and (4) a vegan does not eat any animal products, including meat, fish, poultry, eggs, and dairy products; many vegans will also avoid honey.
‘Improved health is one of the many reasons people choose to adopt a vegetarian diet, and there is now a wealth of evidence to support the health benefits of a vegetarian diet.’
A 2009 nationwide poll conducted by the Vegetarian Resource Group estimated that approximately 3% of US adults are vegetarian (indicating that they never eat meat, poultry, fish, or seafood), and around 1% are vegan (they also never eat dairy, eggs, and honey). 1
Health Benefits of a Vegetarian Diet
Improved health is one of the many reasons people choose to adopt a vegetarian diet, and there is now a wealth of evidence to support the health benefits of a vegetarian diet. Research has found that vegetarians have lower rates of a number of health problems, including overweight and obesity, cardiovascular disease (CVD), hypertension, type 2 diabetes, some cancers, gallstones, kidney stones, constipation, and diverticular disease.2,3
Although vegetarians generally have a lower body mass index (BMI) and tend to be more health conscious than nonvegetarians, 4 health outcomes remain better even when these factors are taken into account. Furthermore, a number of studies have shown increased longevity among vegetarians.5,6 It is likely that these benefits result from both a reduced consumption of potentially harmful dietary components, including saturated fat, cholesterol, animal protein, red meat, and heme iron, and an increased consumption of beneficial dietary components, including fruit, vegetables, whole grains, legumes, and nuts, which are rich in dietary fiber, antioxidants, and phytochemicals. 7
Vegetarian diets differ from nonvegetarian diets in many respects, but the most significant difference is the absence of red meat intake in a vegetarian diet. Research has linked higher intakes of red meat and processed meat with an increased risk of obesity, 8 type 2 diabetes,9-13 gestational diabetes, 14 CVD,15-17 and some types of cancer.18-25 These findings are summarized in Table 1. A large study investigating the association of a wide range of meat intakes with chronic disease mortality found that both red and processed meat intakes were associated with modest increases in total mortality, cancer mortality, and CVD mortality. 26 Low meat intake, on the other hand, has been associated with greater longevity. 5
Studies Showing Association Between Red Meat Intake and Risk of Chronic Disease and Mortality
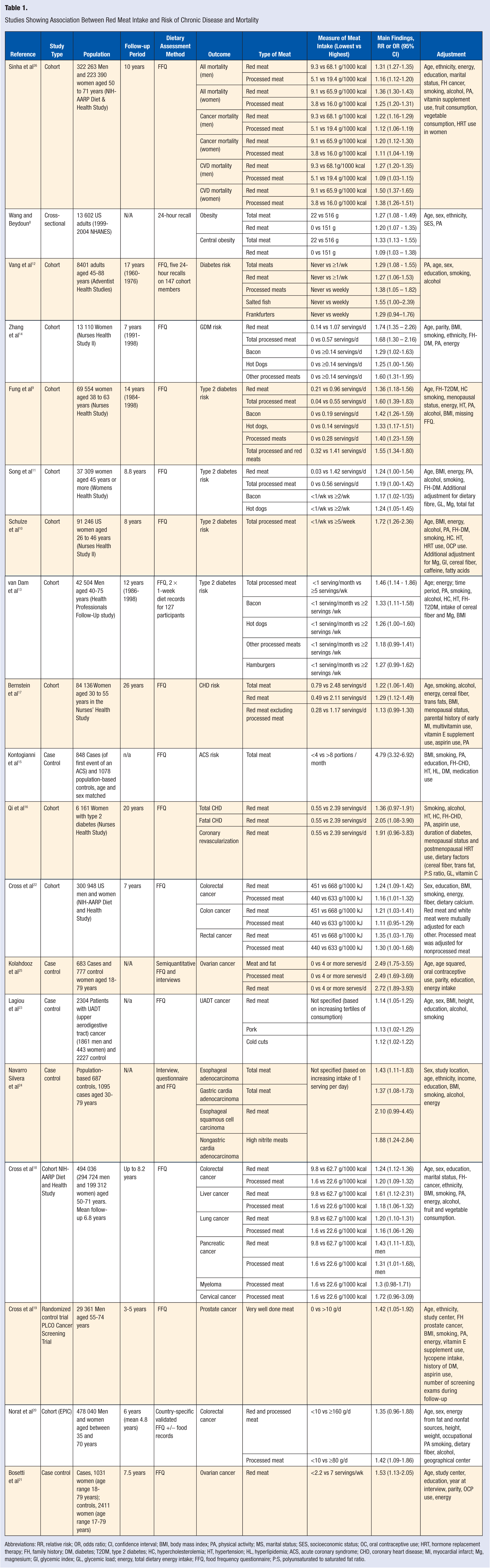
Abbreviations: RR, relative risk; OR, odds ratio; CI, confidence interval; BMI, body mass index; PA, physical activity; MS, marital status; SES, socioeconomic status; OC, oral contraceptive use; HRT, hormone replacement therapy; FH, family history; DM, diabetes; T2DM, type 2 diabetes; HC, hypercholesterolemia; HT, hypertension; HL, hyperlipidemia; ACS, acute coronary syndrome; CHD, coronary heart disease; MI, myocardial infarct; Mg, magnesium; GI, glycemic index; GL, glycemic load; energy, total dietary energy intake; FFQ, food frequency questionnaire; P:S, polyunsaturated to saturated fat ratio.
Overweight and Obesity
Research has consistently shown that vegetarians, and particularly vegans, are leaner than their omnivorous counterparts.27-30 The European Prospective Investigation in Cancer and Nutrition (EPIC) Oxford study compared weight gain over 5 years in almost 22 000 meat-eating, fish-eating, vegetarian, and vegan men and women. 28 Weight gain was lowest in the vegan group and those who, during follow-up, had changed to a diet containing fewer animal foods. The same study reported a significant difference in age-adjusted BMI between the 4 diet groups, with meat eaters having the highest BMI (24.41 kg/m2 in men, 23.52 kg/m2 in women), vegans the lowest BMI (22.49 kg/m2 in men, 21.98 kg/m2 in women), and fish eaters and vegetarians a similar, intermediate mean BMI. 29 Differences in macronutrient intakes accounted for about half the difference in mean BMI between vegans and meat eaters, with high protein and low fiber intakes most strongly associated with increasing BMI. 29 Similarly, the Adventist Health Study-2 found that mean BMI was lowest in vegans (23.6 kg/m2) and incrementally higher in lacto-ovo vegetarians (25.7 kg/m2), pesco-vegetarians (those who also ate fish; 26.3 kg/m2), semivegetarians (those who ate meat, poultry, or fish less than once per week; 27.3 kg/m2), and nonvegetarians (28.8 kg/m2). 30
There are a number of possible explanations for this association, including the lower fat intake, higher intake of dietary fiber, and lower energy density typical of a vegetarian diet. Foods such as whole grains and nuts are more regularly consumed by vegetarians and have been independently associated with a reduced risk of obesity and weight gain.31-33 A higher intake of red meat, on the other hand, has been associated with an increased risk of weight gain.34-36
Cardiovascular Disease
The most consistent evidence for the health benefits of a vegetarian diet relates to a reduced risk of coronary heart disease (CHD) and coronary disease mortality. Several studies have demonstrated a lower incidence of CHD,37-41 and a combined analysis of 5 prospective studies reported a 24% lower risk of mortality from ischemic heart disease (IHD) in vegetarians compared with meat eaters, with lacto-ovo vegetarians having a 34% reduced risk and vegans a 26% reduced risk.42,43 The benefit was apparent in those who had followed their diet for at least 5 years and was greater in younger age groups.
These findings are perhaps not surprising considering that vegetarians generally have a better cardiovascular risk profile than nonvegetarians, with lower total and low-density lipoprotein (LDL) cholesterol levels,38,44-48 a lower body weight,28-30 and a lower incidence of diabetes12,30,49 and hypertension,50-52 all of which contribute to CVD risk. Some research has also suggested that a vegetarian diet may reduce the susceptibility of LDL to oxidation. 53
Specific aspects of a vegetarian diet, including a lower intake of saturated fat, higher intake of soluble fiber, and increased consumption of whole grains, legumes, nuts, and soy protein, are likely to contribute to its cardiovascular benefits. 54 Several studies have demonstrated an association between whole grain intake and CVD risk, and a recent meta-analysis estimated that a greater intake of whole grains (2.5 servings per day vs 0.2 servings per day) was associated with a 21% lower risk of CVD events. 55 The National Health and Nutrition Examination Survey (NHANES) 1 Epidemiologic Follow-up Study found that consuming legumes at least 4 times per week, compared with less than once per week, was associated with a 22% reduced risk of CHD and an 11% reduced risk of CVD. 56 Similarly, the Japanese Collaborative Cohort Study (JACC) found an inverse association between bean intake (which included soy) and CVD risk. 57 The highest intake of legumes (4.5 servings per week) was associated with a 16% reduced risk of total CVD and a 10% reduced risk of total mortality. Regular nut consumption has been found to protect against CHD in both epidemiological and clinical trials. Nuts may protect against CHD through effects on lipids, lipid oxidation, inflammation, and vascular reactivity. 58 Soy protein has been shown to reduce total and LDL cholesterol levels, and a recent meta-analysis of 30 studies demonstrated a small but significant reduction in both total and LDL cholesterol with the consumption of 25 g of soy protein per day. 59 Since 1999, the US FDA has approved a health claim that foods high in soy protein may help lower heart disease risk. 60 Although individual components of a vegetarian diet may provide benefits for CVD risk, a combination of these foods is likely to provide the greatest effect. For example, a vegetarian diet incorporating soluble fiber, soy protein, almonds, and plant sterols has been shown to reduce LDL cholesterol by a similar amount as 20 g of lovastatin does, over 4 weeks. 61
Although some studies have linked red meat intake with CHD risk, 62 a recent meta-analysis found that processed meat intake, but not red meat intake, was associated with a higher risk of CHD. 63 Several studies have demonstrated the benefits of a Mediterranean diet—a mostly plant-based diet with low meat intake—for a reduced risk of CHD.64-66
Hypertension
Evidence suggests that a vegetarian diet may help in both the prevention and management of hypertension. 67 The EPIC-Oxford study found that non–meat eaters had a lower prevalence of hypertension and lower systolic and diastolic blood pressures than meat eaters, but this was largely a result of differences in BMI. 50 The age-adjusted prevalence of self-reported hypertension was significantly different between the 4 diet groups, ranging from 15.0% in male meat eaters to 5.8% in male vegans, and from 12.1% in female meat eaters to 7.7% in female vegans. 50 Fish eaters and vegetarians had a similar, intermediate prevalence of hypertension. In the Adventist Health Study-2, a significant, graded association with blood pressure was also observed. 51 Compared with nonvegetarians, vegans were 75% less likely to be treated for hypertension, lacto-ovo vegetarians 65% less likely, pesco-vegetarians 38% less likely, and semivegetarians 23% less likely.
A number of randomized clinical trials have shown that a vegetarian diet can lower blood pressure in both normotensive and hypertensive individuals.68,69 Although it is well accepted that both weight loss and reducing sodium intake can lower blood pressure, 70 the effect of a vegetarian diet on blood pressure appears to be independent of these, suggesting that other components of the diet are responsible,68,69,71 These findings are consistent with the results of the DASH (Dietary Approaches to Stopping Hypertension) trial, which found that a diet high in fruit, vegetables, whole grains, and low-fat dairy products significantly reduced blood pressure in those with normal blood pressure or mild hypertension. 72
Cancer
Overall, cancer rates in vegetarians appear to be moderately lower than others living in the same communities, and life expectancy appears to be greater.40,51,73 However, results for specific cancers are less convincing and require more study. 74 Most of the research conducted on vegetarian diets and cancer has involved lacto-ovo-vegetarians. Of the studies looking at vegan groups, most only cover a short period of time or a small group. Furthermore, many Western vegetarians choose a meat-free diet for its health benefits in addition to other health or lifestyle practices, such as abstaining from smoking and avoidance or moderate consumption of alcohol,5,39,75 which are also linked with cancer risk.
The World Cancer Research Fund reported in 2007 that there is convincing evidence that consumption of red meat and processed meat increase the risk of colorectal cancer. One would therefore expect vegetarians to have a lower incidence of colorectal cancer than those who eat meat; however, the evidence to support this is not consistent. Whereas US Adventist studies found that vegetarians had a lower risk of colon cancer, a study of British vegetarians found that they had a similar rate of colon cancer to nonvegetarians.40,51,76-78 It may be that the classification of vegetarian and nonvegetarian is too simple, and vegetarian diets may differ widely in nutrient composition, even in the absence of red meat. This may particularly be the case when comparing vegetarians in different countries.51,78 The definition of vegetarian may also differ between studies, with some classifying themselves as vegetarian while still regularly consuming seafood or white meat. It has been suggested that more descriptive vegetarian subtypes need to be used for epidemiological research. 51
The higher fiber intakes of vegetarians may play a major role in reducing colon cancer risk. 79 The bulking effect of fiber may increase the transit rate of carcinogens through the bowel and reduce the surface contact exposure of carcinogenic compounds with the bowel wall.80,81 Those who eat vegetarian diets have colonic environments that are different from those who eat meat-rich diets. They tend to have lower colonic cell proliferation, different profiles of intestinal bacteria, lower levels of fecal enzymes, and lower levels of mutagens in feces—all of which may play a role in reducing bowel cancer risk.82-84 However, the protective effects of fiber on colorectal cancer remains controversial, with a large pooled analysis suggesting that dietary fiber intake did not affect colorectal cancer incidence. 85
Research also suggests that lifelong vegetarianism may be associated with a reduction in the risk of breast cancer through its association with a higher intake of vegetables, fruit, soy, and pulses and the avoidance of red meat.86-90 Potential reasons for a lower incidence of breast cancer include the fact that vegetarians have lower levels of blood estrogens, longer menstrual cycles, and a later onset of menstruation, resulting in a reduction in exposure to estrogen. 89 However, more recent studies have not supported these findings, and further research to clarify the benefits of a plant-based diet for breast cancer prevention is needed.
The health benefits of protective compounds in a plant-based diet have been linked to the prevention of cancer initiation and the retardation of cancer cell growth. Foods that are central to vegetarian diets such as whole grains, legumes, fruits, and vegetables are rich in fiber, folic acid, phytochemicals, and antioxidants. 91 Carotenoids, ascorbate, tocopherols, selenium, dithiolthiones, isothiocyanates, indoles, phenols, protease inhibitors, allium compounds, plant sterols, limonene, and other biologically active compounds are often collectively referred to as phytochemicals that, among many other properties, have anticancer activity.92-95
In addition to the cancer-protective effect of a plant-based diet, eating red meat may contribute to cancer formation. The consumption of red meat cooked at high temperatures, diets rich in animal fat and cholesterol, or diets high in animal protein may increase the risk of developing cancer.18,26,96-98 Red meat, particularly high-fat processed meats, may give rise to cancerous compounds when cooked at a high temperature, the metabolism of which are risk factors for the development of cancer. 99 Excessive iron is also thought to promote the formation of reactive species of free radicals that can damage cells. 99 However, although some researchers have found significant results showing a direct link between red meat, heme iron, and high temperature cooking and cancer formation (see Table 1), the issue remains contentious and requires further research.
Diabetes
Vegetarian and vegan diets offer significant benefits for the prevention and management of diabetes. Observational studies have demonstrated a significantly lower risk of type 2 diabetes in individuals following a vegetarian diet when compared with nonvegetarians.30,49 The original Adventist Health Study found that vegetarians had approximately half the risk of developing diabetes, with a significant association observed between red meat intake and diabetes risk, independent of body weight, other dietary factors, and physical activity. 49
In the more recent Adventist Health Study-2 involving more than 60 000 men and women, those following a vegan diet were found to have a diabetes prevalence that was approximately one third that of nonvegetarians (2.9% vs 7.6%), whereas the lacto-ovo vegetarians, pesco-vegetarians, and semivegetarians had an intermediate diabetes prevalence of 3.2%, 4.8%, and 6.1%, respectively. 30 After adjusting for confounding factors, those following a vegan diet had an almost 50% reduction in the risk of developing type 2 diabetes compared with nonvegetarians. The risk reduction became incrementally smaller as more animal products were consumed: lacto-ovo vegetarians had a 46% reduction in risk, pesco-vegetarians a 30% reduction in risk, and semivegetarians a 24% reduction in risk. 30
Whether the reduction in risk of diabetes in vegetarians can be attributed to the absence of meat or the higher intake of plant foods such as whole grains, legumes, and nuts is unclear. However, several studies have shown a positive association between dietary heme iron intake and heme iron intake from red meat and the risk of type 2 diabetes.11,100-103 A positive association between the intake of red meat, processed meats, and animal protein and the incidence of type 2 diabetes has also been demonstrated,9-12 and a high intake of red meat prior to becoming pregnant significantly increased the risk of developing gestational diabetes. 14
In the Adventist Mortality Study and Adventist Health Study, those who were weekly consumers of all meats (including red meat, poultry, and fish) were 29% more likely to develop diabetes compared with those who ate no meat, whereas those who consumed any processed meats (including salted fish and frankfurters) were 38% more likely to develop diabetes. 12 Furthermore, long-term adherence (over a 17-year interval) to a diet that included at least weekly meat intake was associated with a 74% increase in the risk of diabetes compared with long-term adherence to a vegetarian diet (no meat intake). Even after controlling for weight and weight change, weekly meat intake increased the risk of diabetes by 38%. A recent systematic review and meta-analysis of cohort studies of meat consumption and type 2 diabetes risk estimated the relative risk comparing high versus low intake, and this was 1.17 for total meat, 1.21 for red meat, and 1.41 for processed meat. 104 The authors predict that a 120 g/d increase in red meat consumption increases the risk of diabetes by 20% and a 50 g/d increase in processed meat consumption increases the risk by 57%.
In addition to the absence of red meat, there are a number of other aspects of a vegetarian diet that may protect against and assist in the management of type 2 diabetes, including a lower intake of saturated fat and a higher intake of dietary fiber, whole grains, legumes, and nuts. These dietary factors have also been shown to reduce CVD risk, one of the main complications of diabetes. Furthermore, substituting soy or vegetable protein for animal protein in the diet has been shown to reduce the risk and progression of renal disease in both type 1 and type 2 diabetes.105-110
There are only a few intervention studies assessing the effects of a vegetarian diet in people with diabetes, and weight loss has generally been greater on the vegetarian diets, making it difficult to determine the independent effect of the diets. 111 However, greater weight loss may be one of the advantages of a vegetarian diet because even small amounts of weight loss can help in both the prevention and management of type 2 diabetes. One study comparing a low-fat vegan diet with a diet based on the American Diabetes Association (ADA) guidelines found that the vegan diet reduced HbA1c levels significantly more than the ADA diet (by 1.23 vs 0.38 percentage points in those who did not change medication). 112 Furthermore, 43% of people were able to reduce their medication compared with only 26% in the ADA group. Earlier studies of low-fat vegan diets in patients with type 2 diabetes have also demonstrated significant improvements in blood glucose control and blood fats as well as considerable reductions in medication use,113,114 although the larger of these studies was not controlled.
Other Diseases
Limited research has suggested that a vegetarian diet may also reduce the risk of other health conditions, including diverticular disease, gallstones, rheumatoid arthritis, gout, and kidney disease. Although these findings are positive and add to the evidence of the health benefits of a vegetarian diet, the small number of studies mean that further research is required to confirm these benefits.
Diverticular disease
Vegetarians tend to have a lower incidence of diverticular disease than nonvegetarians. 115 This is believed to be a result of the higher dietary fiber intake of vegetarians from an increased consumption of whole grains, fruits, vegetables, nuts, and legumes. 3 More recent research suggests that diets high in fat and red meat, independent of fiber intake, may be linked to an increase in diverticulitis. 116
Gallstones
Vegetarians may be only half as likely to develop gallstones as nonvegetarians. 117 In a cross-sectional study, the prevalence of gallbladder disease was significantly lower in female vegetarians than female omnivores (12% vs 25%). 117 In addition, a 20-year prospective study of 80 898 women found that increased consumption of vegetable protein was associated with a reduced risk of having a cholecystectomy. 118 A separate evaluation of the same cohort of women found that increasing the consumption of fruits and vegetables was associated with a decreased incidence of gallstones. 119 In hamsters fed a lithogenic diet, the incidence of gallstones was decreased in a dose-dependent manner by progressively replacing casein with soy protein in the diet.120,121 It has been proposed that the lower BMI of vegetarians; higher fiber, legume, and lecithin intakes; and possibly greater soy protein intake may be contributing factors. 122 A recent study in women found that frequent nut consumption (often higher in vegetarian diets) reduced the risk of cholecystectomy. 123
Gout
Limited research suggests that gout may also be less common in vegetarians. A study of nearly 50 000 male individuals older than 12 years, comparing those who suffered from gout with those who did not, found that the consumption of meat, particularly red meat, and all types of seafood significantly increased the risk of gout. 124 Eating more than 2 servings of red meat per week increased the risk by 50%, whereas eating more than 1 serving of canned tuna per week increased the risk by 28%. In contrast, no increased risk was seen with the consumption of purine-rich vegetables, and there was no association with the overall vegetable protein intake. There was a protective effect from vegetable and dairy proteins, with the consumption of low-fat dairy products significantly reducing the risk of gout. A second study looking at the effect of a vegetarian diet and different omnivorous diets on the risk of uric acid crystallization found that the risk of uric acid crystallization was highest with high levels of meat intake and Western diets, declined significantly on a balanced omnivorous diet, and was lowest on a vegetarian diet. 125
Rheumatoid arthritis
Several studies have shown that individuals with rheumatoid arthritis may benefit from a period of fasting followed by a low-fat vegetarian or vegan diet.126-129 A systematic review of 4 controlled studies lasting at least 3 months found a clinically and statistically significant effect of such diets. 130 The exact mechanism for these improvements is unclear, but they may be a result of a reduction in inflammation. 126 Weight loss may also play a part; however, a pooled analysis of 3 studies found that weight reduction did not significantly contribute to the improvement in rheumatoid arthritis when individuals were on lacto-vegetarian, vegan, or Mediterranean diets. 131
Kidney disease
High intakes of animal protein may have adverse effects for those with underlying kidney problems. A study of individuals with type 2 diabetes and macroalbuminuria found that eliminating red meat from the diet, either by replacing it with chicken or by following a lacto-vegetarian, low-protein diet improved renal function and blood fat levels. 108 In patients with type 1 diabetes, improved kidney function has been demonstrated following dietary intervention in which animal protein was replaced with vegetable protein 109 and soy protein. 110 A recent study in patients with type 2 diabetes and nephropathy found that replacing 35% of animal protein intake with soy protein significantly reduced proteinuria and urinary creatinine. 106
The Multiethnic Study of Atherosclerosis found that in those without diabetes or CVD, a dietary pattern rich in whole grains, fruit, and low-fat dairy food was associated with a lower risk for microalbuminuria and high mean albumin-to-creatinine ratio (ACR), whereas intake of nondairy animal foods was positively associated with high ACR. 132
Meeting Nutritional Needs
The American Dietetic Association support the fact that, in addition to their health benefits, well-planned vegetarian diets, including vegan diets, are nutritionally adequate and are appropriate for individuals during all stages of life. 133 Some nutrients can be more difficult to obtain on a vegetarian diet, but careful planning and, in some cases, the use of fortified foods or supplements can ensure that an individual’s nutrition needs are met while maximizing the health benefits of a vegetarian or vegan diet.
Protein
Although the adequacy of protein in vegetarian diets is sometimes questioned, vegetarian diets usually exceed protein requirements, although they may provide less protein than a nonvegetarian diet. 133 Because most plant foods contain limited amounts of one or more essential amino acids, it was once thought that certain combinations of plant foods had to be eaten at the same meal to ensure sufficient essential amino acids. It is now known that strict protein combining is not necessary, provided energy intake is adequate and a variety of plant foods are eaten each day, including legumes, whole grains, nuts and seeds, soy products, and vegetables. 134 Furthermore, soy protein has a PDCAAS (protein digestibility–corrected amino acid score) that is almost identical to meat. 135 Plant sources of protein include legumes, nuts, and soy products, including soy milk, soy yoghurt, tofu, and tempeh. Grains and vegetables also contain protein but in small amounts.
Vitamin B12 (Cobalamin)
Vitamin B12 is found only in animal products, so a deficiency of this vitamin is a potential concern for anyone following a vegan or vegetarian diet or anyone who significantly restricts animal products. Serum levels of vitamin B12 are generally lower in vegetarians, especially vegans, decreasing with increasing duration of following the diet.136,137 Although it can take several years for deficiency symptoms to develop, anyone excluding animal products will eventually become deficient if their diet is not adequately supplemented. Recent findings from the EPIC-Oxford study showed that in a cohort of 689 men (226 omnivores, 231 vegetarians, and 232 vegans) 52% of vegans, 7% of vegetarians, and 1 omnivore were classified as vitamin B12 deficient. 136
Although plant foods, including mushrooms, tempeh, miso, and sea vegetables, are often reported to provide some vitamin B12, they are not a reliable source of this vitamin. These foods contain an inactive form of B12, which interferes with the normal absorption and metabolism of the active form in the body and will not prevent a deficiency. 138 Recent research has found some bioavailable vitamin B12 (in the same form present in animal products) on the surface and in the flesh of mushrooms. 139 These amounts, however, are small and inadequate to meet dietary needs. A reliable source of biologically active vitamin B12 is recommended on a regular basis, either from fortified foods or supplements. In particular, all vegans should supplement their diet with vitamin B12, and this is especially important for women who are pregnant or breastfeeding, to prevent deficiency in their baby. 140
Iron
There are 2 types of iron in food: heme iron found only in animal foods, such as meat, poultry, and fish, and nonheme iron found in animal foods, including eggs and plant foods such as legumes, whole grains, nuts, seeds, dark green leafy vegetables, and dried fruit. Nonheme iron is not as well absorbed by the body but its absorption is increased significantly in the presence of vitamin C. 141 Polyphenols such as tannins, found in tea and coffee, 142 and phytates in whole grains and legumes can inhibit the absorption of iron, with vitamin C aiding absorption most effectively in meals containing high levels of phytates and polyphenols.143-145 The net effect of various enhancers or inhibitors may be less important in a highly varied diet, where no one factor is present in sufficient amounts to be of significance.146,147
Vegetarian diets can contain as much or more iron (nonheme) than mixed diets, primarily from whole grain breads and cereals, including fortified cereals.148,149 Surprisingly, iron deficiency is not more common in vegetarians, although iron stores (as shown by ferritin levels) are often lower.150-153 It is thought that lower iron stores may reduce the risk of chronic diseases as previously discussed. Iron requirements are set 80% higher for vegetarians than for nonvegetarians because of bioavailability issues with nonheme iron 144 ; yet it has been suggested that these bioavailability concerns may have been exaggerated by studying absorption from single meals under lab conditions because the influence of enhancers and inhibitors was much less pronounced over several weeks in comparison with single-meal studies.147,154
Despite concerns regarding dietary bioavailability and iron absorption, iron status is thought to be the determining factor regulating nonheme iron absorption. 155 Humans can adapt successfully to a wide range of iron requirements and intakes. 156 Absorption is regulated by physiological requirements and iron status more than the type of food eaten or its bioavailability—lower body stores result in intestinal adaptation, with increased absorption and reduced excretion.133,152,154,157 During pregnancy, women will absorb 60% more iron when requirements are highest.157-159
Zinc
Although zinc is found widely in plant foods, like iron, its absorption is dependent on body stores and requirements—the body appears to adapt to lower intakes by reducing losses and increasing absorption.152,160 As with iron, zinc deficiency is no greater in vegetarians than in nonvegetarians, 152 and zinc intakes of vegetarians are close to recommended levels. 148 Absorption of zinc is reduced by phytates found in wheat bran, whole grains, and legumes. However, processing a food by leavening (yeast in breads), soaking, fermenting, or sprouting can reduce the phytate level and make zinc more readily available. 161 Again, like iron, commonly eaten plant foods, such as nuts, seeds, and whole grains, are high in zinc and may be the reason for the apparent satisfactory status in vegetarians.
Calcium
Research has found that calcium intakes are generally similar between lacto-ovo vegetarians and nonvegetarians, 163 although vegans typically have lower intakes.148,164 A recent review of the literature concluded that there are no significant differences in bone health indices between lacto-ovo vegetarians and those who eat meat, and although vegans do have lower bone mineral densities (BMDs), the differences are not clinically significant.165,166 The EPIC Oxford study found that the fracture risk was similar in vegetarians and in meat and fish eaters, but there was an increased risk for vegans. 164 However, no increased risk was observed in those consuming at least 525 mg/d of calcium, suggesting that the lower calcium intake of some vegans was responsible for the increased fracture risk. In contrast, a recent study in postmenopausal Buddhist nuns following a lifelong vegan diet found that despite a much lower intake of calcium (330 vs 680 mg/d in omnivorous women), bone mineral densities were similar to nonvegetarians. 167 There was no significant correlation between calcium intake and BMD.
For lacto-ovo vegetarians, dairy products provide plenty of calcium. Vegans can obtain their calcium from fortified soy milk and yoghurt, tofu (set with calcium salts), or other plant foods rich in calcium. Plant foods that have high calcium bioavailability include low oxalate greens, which have a bioavailability of 50% to 60% compared with cow’s milk at around 32%, whereas the bioavailability from fortified soy milk, sesame seeds, and almonds is estimated to be around 21% to 24%. 163 Thus, many plant foods can provide a significant amount of bioavailable calcium despite generally being lower in calcium content than dairy foods. Absorption of calcium is improved in the presence of vitamin D, whereas excretion of calcium is increased by sodium, caffeine, and, according to some studies, by excess animal protein.163,168-171 Low protein intakes, however, may also reduce calcium absorption. 170 The 1999-2002 National Health and Nutrition Examination Survey (NHANES) found an increased risk of fractures in postmenopausal women with low protein intakes (<46 g/d) despite calcium intakes of at least 1200 mg/d. 170 These findings may be particularly relevant to those following a vegan diet who may have a lower intake of both calcium and protein.
Essential Fatty Acids
Omega-3 fatty acids play an important role in health and disease, particularly with respect to cardiovascular health but also in inflammatory diseases and neurological and eye development. 173 Because fish and seafood are the main sources of long-chain omega-3 fatty acids, obtaining an adequate intake on a vegetarian diet is difficult. Vegetarians obtain omega-3 fats predominantly from the omega-3 fatty acid α-linolenic acid (ALA), but there is debate over the efficiency of conversion of ALA to the longer-chain docosahexaenoic acid (DHA) and eicosapentaenoic acid (EPA). 174 For vegetarians, it has been suggested that a ratio range of 2:1 to 4:1 of omega-6 to omega-3 would maximize conversion 174 and reduce any thrombotic tendency that might increase their generally low risk for CVD. 175
There is some evidence to suggest that the requirement for omega-3 fatty acids in vegetarians is higher because of the inefficient conversion of ALA to EPA and DHA and the lack of direct sources of these fatty acids. 174 However, a recent study showed smaller differences in plasma n-3 polyunsaturated fatty acid status between fish eaters and non–fish eaters than would be expected from dietary intakes, which could be explained by a greater conversion of ALA to EPA and DHA in the non–fish eaters. 176 Some believe that a vegetarian’s need for omega-3 fatty acids can be met by dietary ALA. 177 DHA is absent from unsupplemented vegan diets and present in limited amounts in vegetarian diets. Hence, the proportions of DHA in plasma, blood cells, breast milk, and tissues are substantially lower in vegans and vegetarians compared with omnivores; however, the significance of this difference on health outcomes remains unclear.174,177,178 Omega-3 requirements appear to increase as omega-6 intake increases, and reducing omega-6 intake to <2% of energy greatly reduces omega-3 requirements. 179 To optimize omega-3 fatty acid status in vegetarians, it is best to avoid saturated and trans fats, and favor monounsaturated fats rather than omega-6 fats. The richest sources of ALA include chia seeds and linseeds (or flaxseed oil). Walnuts and soy products also provide a good source of ALA, with smaller amounts present in green leafy vegetables.
Both ALA and marine-derived omega-3 fatty acids are associated with a reduced risk of CVD. 174 Adding DHA-fortified foods to an already healthy vegetarian diet may have little additional health benefits in terms of CVD. 180 However, those with higher requirements, such as pregnant and breastfeeding women, and those at greater risk for poor conversion, such as people with diabetes, older people, and premature infants, may benefit from microalgae-rich DHA supplements.174,181,182 Omega-3-rich eggs or foods fortified with algal DHA are direct sources of DHA.
Vitamin D
Vitamin D is best known for its role in bone health—we absorb very little calcium when vitamin D levels are low. A relatively new area of research is its role in diseases such as cancer, heart disease, strokes, arthritis, multiple sclerosis, and even depression. 183 Recent evidence suggests that vitamin D deficiency is a public health problem not just for vegetarians and is more widespread than once thought. 184 Vitamin D is unusual in that it is more like a hormone than a vitamin, and given the right amount of careful sun exposure (the main source of vitamin D), our skin can produce what we need. However, the amount we produce depends on many factors, including the time of day, season, latitude, skin pigmentation, use of sunscreen, amount of skin exposed, length of time of exposure, and age. 133
Vitamin D is found naturally in only a few foods such as oily fish (cod liver oil), wild mushrooms, and eggs. Because only a few products contain vitamin D, it is also added to some dairy products and other fortified foods. Although lacto-ovo vegetarians obtain some vitamin D from eggs and dairy products, most of their intake comes from fortified foods, Vegans rely only on fortified foods to obtain adequate dietary intake. Recent research found that button mushrooms exposed to ultraviolet irradiation produced vitamin D, which could potentially provide a food source for vegans. 185 There are 2 main forms of vitamin D used for supplements and fortification: D2 (ergocalciferol), which is sourced from plants (yeast), and D3 (cholecalciferol), which is sourced from animals (sheep’s wool). It has been suggested that D2 has only about 60% of the bioavailability of animal-derived D3, 186 but other studies suggest that they are equally absorbed.133,183
Whereas some studies have shown that vegetarians, and particularly vegans, have lower intakes of vitamin D compared with nonvegetarians,187-189 the recent Adventist Health Study-2 found no relationship between serum vitamin D concentrations and vegetarian status, suggesting that factors other than diet have a greater influence on vitamin D levels. 190 If sun exposure and intake of foods fortified with vitamin D is inadequate to meet the requirements, vitamin D supplements are recommended. 133
Conclusion
Well-planned vegetarian diets are not only nutritionally adequate but also provide many health benefits, particularly in the prevention and treatment of many chronic diseases. In fact, in Western countries, a vegetarian diet may present a significant advantage over meat-based diets, and a number of studies have shown increased longevity in vegetarians.
Although potentially lower in some nutrients, careful planning can help ensure that both vegetarian and vegan diets meet all the current recommended intakes for essential nutrients as well as maximize the intake of protective components present widely in plant foods. In fact, a vegetarian diet may well be one of the best ways to meet population dietary guidelines. AJLM
