Abstract
There is a faction within the chiropractic profession passionately advocating against the routine use of X-rays in the diagnosis, treatment and management of patients with spinal disorders (aka subluxation). These activists reiterate common false statements such as “there is no evidence” for biomechanical spine assessment by X-ray, “there are no guidelines” supporting routine imaging, and also promulgate the reiterating narrative that “X-rays are dangerous.” These arguments come in the form of recycled allopathic “red flag only” medical guidelines for spine care, opinion pieces and consensus statements. Herein, we review these common arguments and present compelling data refuting such claims. It quickly becomes evident that these statements are false. They are based on cherry-picked medical references and, most importantly, expansive evidence against this narrative continues to be ignored. Factually, there is considerable evidential support for routine use of radiological imaging in chiropractic and manual therapies for 3 main purposes: 1. To assess spinopelvic biomechanical parameters; 2. To screen for relative and absolute contraindications; 3. To reassess a patient’s progress from some forms of spine altering treatments. Finally, and most importantly, we summarize why the long-held notion of carcinogenicity from X-rays is not a valid argument.
Introduction
Despite radiography being a well-established cornerstone of spine and pelvic biomechanical examination in the therapy of spine disorders, 1 -16 there are pressures to reduce the use of radiological imaging to assess spine structure and function within the chiropractic profession. 17 -20 This mounting pressure is by a select faction of mostly academics who claim that imaging is over-utilized within chiropractic. In 2017, this movement culminated in a major chiropractic association joining the Choosing Wisely program to denounce the use of X-rays for routine assessment of acute low back pain (within the first 6-weeks of onset) and not to use X-rays for repeated use to monitor patient progress. 17 These anti-imaging practice strategies have been shown to lack evidential support and to be antithetical to scientific reality. 18,19
Chiropractic anti-imaging activists reiterate common false statements such as “there is no evidence” for biomechanical assessment from X-rays, “there are no guidelines” supporting routine imaging, and that “X-rays are dangerous.” These arguments come in the form of recycled allopathic “red flag only” medical guidelines for spine care, 20 -22 opinion pieces 23,24 and consensus statements. 17 All of these claims are factually incorrect as has been extensively pointed out in several publications. 13 -16,18,19,25 -30 X-rays are, in fact, the only practical way to assess a patient’s essential biomechanical spinal parameters (e.g. cervical hyper/hypo-lordosis/kyphosis, thoracic hyper/hypo-kyphosis, lumbar hyper/hypo-lordosis, global/regional sagittal balance, pelvic tilt, sacral slope, thoracic inlet angle, pelvic morphology, etc.). 1 -12 As well, there are indeed chiropractic guidelines 31 -34 and rationale 13 -16,35 that support routine imaging and, as we will discuss later, low-dose radiation exposures from X-rays are now known to be harmless based on updated information. 36 -48
Problematically, the anti-imaging stance in chiropractic promulgates misinformation that confuses the public and contributes to divisiveness within the profession between those who practice specialty techniques that require routine spine imaging (to guide treatment) and those who practice generalized gross manipulation that, generally, do not use imaging. Further, the anti-imaging narrative gets amplified when reiterated in the literature, such as when mentioned in chiropractic clinical practice guidelines 49 -51 and when over-stated in low-quality studies. 52,53 It has also been thoroughly documented that the anti-imaging stance such as by the American Chiropractor’s Association’s participation in the Choosing Wisely campaign’s Points 1 and 2 anti-imaging stance is fraught with misappropriated medical references (i.e. practice of medicine references) and not supported by any legitimate chiropractic disciplined evidence. 18,19 Most problematically, this anti-imaging stance has led to insurance companies capitalizing on the opportunity to adopt policies that discriminate against chiropractors who take X-rays based on these practice strategies that are not representative of the profession, including Blue Cross Blue Shield (BCBS) and others. 18
While we acknowledge that traditional “red flags” (malignancy, fracture, inflammatory disorders, etc.) warrant radiographic screening for suspected serious disease processes (this is a concern for all primary care providers), our focus is on the routine use of radiographic imaging for the purposes of screening, assessment, patient management and monitoring of spine and pelvis (spinopelvic) biomechanical parameters from modern and contemporary chiropractic and manual therapy treatment methods. The purpose of this discussion is to assess the validity of common statements made against the use of routine X-ray use in chiropractic practice. Specifically, we show that routine X-ray use is an evidence-based tool to: 1. Assess spinopelvic biomechanical parameters; 2. Screen for relative and absolute contraindications to spine care; 3. Re-assess a patient’s progress to some types of spine rehabilitative treatments. Finally, we provide a synopsis of the most recent evidence showing the long-held assumption of carcinogenicity from X-rays is no longer a valid argument.
Assessing Spinopelvic Parameters
Recent statements made in the chiropractic literature include Jenkins et al. (2018) who stated: “there is currently insufficient evidence to recommend the use of routine spinal X-rays to analyse spinal biomechanics,” 20 and Corso et al. (2020) who stated: “We found no evidence that the use of routine or repeat radiographs to assess the function or structure of the spine, in the absence of red flags, improves clinical outcomes and benefits patients.” 52 The former article has been critiqued ad nauseam, 26 and the latter article was a “rapid review” that did not include any literature published in the last 15 years! It must be mentioned that specifically within the last 15 years (2005-2020) the literature has become replete with high-quality evidence correlating various spinopelvic parameters as measured from X-rays to various health outcomes in the spine care literature. 1 -16
A simple PubMed search of systematic reviews (SR) of particular spine parameters shows unanimous conclusions favoring significant relationships between altered spine parameters and physiological dysfunction. Forward head posture (i.e. anterior head translation), for example, is associated with headache, altered muscle activity, altered proprioception, altered breathing, pain and disability. 54 -56 Loss of lumbar lordosis, particularly loss of distal lordosis is associated with and causative for low back pain (LBP). 57,58 Osteoarthritis and spondylolisthesis are linked to LBP. 58,59 All of these spinal parameters are diagnosed by radiography and, again, these relationships are current scientific consensus based on SRs. 54 -59
As mentioned, despite factions within chiropractic claiming the opposite, the routine assessment of a patient’s spinopelvic biomechanical parameters is the standard for evaluating adult spinal deformity (ASD) and subluxation/misalignment patterns. 1 -16,60 -62 The International Spine Study Group (ISSG) in fact states: “accurate assessment of ASD requires a thorough radiographic evaluation of both the spine and pelvis, including concomitant assessment of the cervical, thoracic, and lumbar spine, as well as the femoral heads and pelvis.” 5 One chiropractic guideline 31 cites Hildebrandt 63 who outlines what radiographic images encompass a full spine radiographic evaluation, and these include full spine antero-posterior and lateral views, images of the femur heads, sacral base, and upper cervical specific views.
It is important to delineate why assessing spinopelvic parameters is so important to patient treatment. A monumental study was published in 2015 by the European Spine Study Group (ESSG) and a similar study in 2016 by the ISSG. 64,65 Pellise et al. showed that the quality of life burden on a sample of 766 ASD patients was significantly more detrimental compared to a database of about 25,000 patients suffering from the common ailments of self-reported arthritis, chronic lung disease, diabetes and congestive heart failure. 64 Similarly, Bess et al. demonstrated that the physical component summary scores from the SF-36 quality of life questionnaire in a sample of 497 ASD patients showed similar scores to patients suffering from diabetes, heart disease and rheumatoid arthritis, and that patients with more severe forms of symptomatic ASD “reported physical limitations and health impact as patients with limited use of arms and legs.” 65 These studies taken together provide compelling evidence that ASD can have devastating impacts on health that often exceeds the disease burden from well recognized chronic ailments.
It is important to delineate what the ISSG and ESSG considered as ASD; the criteria in these 2 reported studies 64,65 were identical and included forward sagittal balance >5 cm, thoracic kyphosis (T4-T12) >60°, pelvic tilt >25° (indicating a decreased distal lumbar lordosis), and scoliosis >20° as measured from full-spine patient radiographs (Figure 1). One may argue that an ASD patient presenting to a spine surgeon may represent a different population than one presenting to a chiropractor or manual therapist and therefore, a surgeon has more of a rationale to utilize X-ray. However, patients having spine deformities exceeding these specific parameter thresholds have been documented to be treated by chiropractors (e.g. anterior sagittal balance >5 cm, 66,67 thoracic hyperkyphosis >60°, 68 -70 pelvic tilt >25° indicating loss of lumbar lordosis, 71 -75 scoliosis >20° 76 -80 ). Indeed, the treatment of ASD patients who have significant disease burden often overlaps between spine surgeons and chiropractors/manual therapists.

Adult spine deformity specifically refers to the following spine deformity (subluxation) types as assessed with radiographic methods and present in any person 18 years and older: A, Thoracic hyper-kyphosis with a magnitude greater than 60°, green is ideal curve and red is patient kyphosis. B, Anterior (positive) sagittal balance of the C7-S1 plumb-line greater than 5 cm (pink line from centroid C7 to horizontal offset of centroid S1). C, Any frontal view scoliosis of greater than 20°. D, Sagittal pelvic tilt angle (PA) greater than 25°. Note, due to the inverse relationship between this PA measurement and sagittal sacral base angle (SBA), PA is descriptive of a SBA being decreased where normal SBA = 40°, and normal PA is approximately 17-18°. Thus, this measurement represents lumbar hypo-lordosis in the distal lumbar region.
In fact, many spine patients seek non-operative care prior to surgery in attempts to avoid the invasive procedure 81 -83 (surgical procedures are often viewed as “last resort”) and even after surgical procedures, as there are high rates of surgical failures (i.e. the surgery does not eliminate the pains). 84 -87 It is also logical that more severe forms of spine deformities preclude lesser forms of spine deformities that ultimately progresses over time. 88,89 Thus, chiropractors and manual therapists who specialize in spine-altering treatment methods serve patients who have a myriad of subluxated spine displacement patterns (Figure 2 90,91 ). If spine patients and their instigating deformities can be treated successfully, this would prevent the later need for surgical procedures from evolving spine deformities (i.e. symptomatic ASD) which has been documented in the literature. 81 -83 Thus, manual therapists including chiropractors definitively treat ASD patients, and of course, also treat patients having less severe spine deformities.

There are many spine and pelvic parameters that can be measured from standing X-rays (Figures 1 and 3). 1 -16 Cervical lordosis, thoracic kyphosis and lumbar lordosis quantify the sagittal regional curves (Figure 3). Sagittal anterior-posterior displacement (translations) for forward head posture and of the total spine are also typically measured (Figure 1B). Pelvic position including the sacral inclination, pelvic tilt and pelvic incidence are also common measurements (Figure 1D). The scoliosis “Cobb angle” is also measured on the frontal view (Figure 1C). All the mentioned spinopelvic parameters can be easily quantified from radiographs using modern x-ray analysis software, and are amenable to structural change (except pelvic incidence and thoracic inlet angle which are stable morphologic measures in adults). Modern non-surgical spine rehabilitation procedures are becoming popular (e.g. Chiropractic BioPhysics® (CBP®), physiotherapy scoliosis specific exercise (PSSE), etc.) and for providers who practice such methods, full spine radiographic assessment is a necessity to quantify the presenting spinopelvic alignment that in turn, guides patient-specific treatment procedures.

Harrison posterior tangent method used to quantify cervical, thoracic and lumbar lordosis as well as any other sagittal subluxation patterns including individual intersegmental rotation angles (Courtesy CBP seminars).
Screening for Anomalies, Pathologies and Contraindications to Manual Therapies
Since manual therapies are unavoidably “hands-on” that also makes them patient-centric. In other words, manual treatments are ideally applied in a fashion that is custom-tailored to meet the unique needs of the patient and to also match their preferences. Case-in-point is that similar forces of thrusts during spinal manipulation would not be used for infants, children and frail seniors than would be used for healthy adults. More specifically, it is known that congenital anomalies, common pathologies, and relative and absolute contraindications to manual treatments are common 92 -96 and should be known prior to imparting forces into a patient’s spine and body.
Surprisingly there has been little study of the occurrence of anomalies, contraindications, and certain pathologies that would alter treatment approaches by manual therapists and chiropractors. 92 -96 Although it has been argued that spinal manipulation treatment is benign 20 (i.e. safe to apply to a wide population without comprehensive X-ray screening), mild adverse events are common. 97,98 Mild adverse events, although not catastrophic, present real challenges in daily practice and the avoidance of these occurring is important. 26 In contrast, there are many popular chiropractic adjusting techniques that are segment-specific (e.g. Atlas Orthogonal, Blair, Diversified, Gonstead, Grostic, Kale, Logan Basic, NUCCA, Palmer upper cervical specific, Toggle-recoil, etc.) and the thrust delivery is based on the initial examination of patient X-rays to ascertain 3-dimensional “thrust vectors.” Further, as mentioned, more recent patient-specific customized structural rehabilitation programs (CBP, PSSE, etc.) also require screening for precision assessment by X-ray and bony anomalies and pathologies including osteoarthritis that may alter treatment approaches unrelated to the necessary spinopelvic parameter relationships.
Of the studies done within the chiropractic literature determining the incidence of bone anomalies, specific pathologies, and contraindications to spinal manipulation, the overall evidential consensus is that these findings are very common (Table 1). 92 -96 After assessing 847 full spine patient X-rays, for example, Beck et al. determined that 68% of the sample had congenital anomalies, 6% had absolute contraindications (should not receive thrust manipulation), and 0.6-6.6% had “serious” pathology warranting referral for urgent medical assessment/intervention. 95 Young et al. diagnosed serious pathology in 44% of 262 patient lumbar radiographs. 93 Jenkins et al. found congenital anomalies in 28.5% of 2814 patient cervical X-rays and 18.3% of 1052 patient lumbar X-rays. 92 Other studies have found the combination of anomalies and pathologies to range from 66-91% of patient samples. 94,96
In one study reviewing the incidence of radiographic variations in 10,922 “healthy” German air force recruits, it was determined that, amazingly, “In only 2.6% were there no pathological findings.” 99 In a study of X-rays among 232 young, healthy Norwegian air force candidates it was determined that “many significant conditions are demonstrated among young healthy individuals” and among the 66% having anomalies, degenerative changes and deviations of posture, there was an average of 3.5 diagnoses per spine X-rayed. 100 They also stated “Since the population is highly selected, the figures we present may be minimum numbers in a western industrialized society.” 100 As seen, radiological studies of even so-called healthy people show that bone and joint skeletal anomalies and pathologies that translate into relative and absolute contraindications to spine manipulation, show these findings are extremely common and, again, can only be determined by routine X-ray screening.
As a great detriment to the chiropractic profession, most “X-ray guidelines” for chiropractors have dedicated little to no emphasis on the unique aspects of manipulation of the spine and have neglected to provide guidelines reflective of the requirement to screen for important anomalies and relevant pathologies, and only discuss “absolute” contraindications (i.e. red flags). 20 -22 Such “red flag” guidelines for chiropractic are misleading those who strictly abide by them into having faith in red flag screening. It was pointed out recently that many red flags (i.e. signs of serious pathology) are based on little evidence, 101 -107 and are not as reliable as has been the enthusiasm for their endorsement. 19 Routine X-ray screening would identify important aspects idiosyncratic to the individual patient and allow for better care. We concur with Giles who stated: “because spinal manipulation involves forces to the spine and, in rare circumstances, may result in an adverse reaction it seems justified to image a patient’s painful spinal area when clinical trials involving spinal manipulation are conducted.” 108 (p130)
A comprehensive list of potentially relevant X-ray findings that could alter treatment approaches has been given by the Practicing Chiropractors’ Committee for Radiology Protocols (PCCRP) 31 (Table 2). It should be noted that patients presenting to a manual therapist typically have multiple indications.
Indications for Spine Radiography in Adults and Children Not Associated With “Red Flags.” 31

Re-assessing Structural Alignment Changes
As discussed, the goal of structural-based treatment (as opposed to symptom-based treatment) is to realign the global and segmental morphological shape of the spine and how a person stands relative to their center of balance. Repeating radiological procedures to re-assess spinopelvic response to treatment procedures is an essential practice that often leads to a change in treatment.
Treatment course changes from repeated X-rays may either take on 1 of 4 scenarios (Table 3). Possibilities include positive changes, no change or a worsening of parameters; as can be seen, each scenario has warranted treatment considerations. Logically, continued treatment options for chiropractors utilizing spine altering methods depend on measurement of the spinopelvic parameters as assessed from the follow-up (repeat) X-rays. This is an evidence-based and patient-centered healthcare practice despite the reiteration of anti-imaging narratives from small factions within the profession to not perform repeat imaging (e.g. ACA, 17 Corso et al. 52 ).
Differing Treatment Scenarios Based on Findings From Repeat X-rays Following Treatment Trials.

As has been outlined recently, there are abundant high-quality, randomized clinical trials (RCTs) that have definitively shown that non-surgical spine rehabilitation procedures can make significant improvements to the spine and posture in those suffering from many different spinal subluxation patterns. 72 -75,109 -125 The spinopelvic parameters having the most accumulated evidence of non-surgical improvements (i.e. RCTs) include the treatment of forward head posture, 109 -115 cervical hypolordosis/kyphosis, 110 -117 thoracic hyperkyphosis (hunchback), 118 -121 lumbar hypolordosis, 72 -75 and scoliosis. 122 -125 As can be seen, clinically significant magnitudes of corrections/improvements can be achieved in relatively short durations (e.g. weeks/months).
It must be mentioned that research for musculoskeletal treatments are less developed than other facets of health care research. 126 Therefore, the science is not complete, and in this respect, lesser forms of evidence (i.e. case reports/series) should be viewed as important and considered in guidelines created for the manual therapies, particularly chiropractic. 127,128 When considering the chiropractic and manual therapy literature showing improvements in other spine and pelvis deformities/subluxation types, there is evidence showing reduction of anterior whole-spine sagittal balance, 129,130 reduction of cervical pseudo-scoliosis, 131 -133 reduction of lumbar pseudo-scoliosis, 134,135 increase in thoracic hypokyphosis (straight back syndrome), 136 -138 reduction of thoracolumbar kyphosis, 139 increase in lumbar kyphosis (flat back syndrome), 82 reduction of lumbar hyperlordosis and pelvic tilt, 140 reduction of cervical spondylolisthesis, 141,142 and reduction of lumbar spondylolisthesis. 143,144
Pressures to restrict the use of “repeat” (i.e. follow-up) X-rays for assessing patient response to treatment shows a complete disregard for the evidence discussed that definitively illustrates how modern spine rehabilitation techniques and practices successfully re-align the spine and pelvis for a wide variety of presenting subluxation/deformity patterns. The continued anti-X-ray sentiment from “consensus” and opinion within chiropractic needs to stop; it is antithetical to scientific reality and to the practice of contemporary chiropractic practice. We reiterate a quote from the late Michael A. Persinger: “what is happening in recent years is that facts are being defined by consensus. If a group of people think that something is correct, therefore it’s true, and that’s contradictory to science.” 145
Synopsis of Why Low-dose Radiation Is Safe
The ubiquitous underpinnings of X-ray restriction campaigns and other practice altering agendas discouraging X-ray use is the prevailing belief in the linear no-threshold (LNT) radiation carcinogenicity ideology. 145 Regarding radiation exposures from X-rays and the presumed fears of future untoward health effects, the classic carcinogenicity narrative has been reiterated loud and clear from a small faction within the chiropractic literature. 17,20,23,24,52
In a recent “rapid” review concluding no evidence for X-ray use in chiropractic, Corso et al. state: “A known risk for ionizing exposure is the increased frequency of cancer beyond that occurring spontaneously…” and this statement is used to reinforce their conclusions to not X-ray, “…and given the inherent risks of ionizing radiation…” 52 In a recent “narrative” review of X-ray use for chiropractic, Jenkins et al. state: “Without definitive thresholds of safe levels of radiation exposure, it should be assumed that some level of risk is associated with the use of X-rays,” 20 they go on to endorse the “As Low As Reasonably Achievable” (ALARA) radiation protection principle underpinned by LNT to keep exposures minimized. 20 The recent ACA declaration of their participation in Choosing Wisely, their Points 1 and 2 both mention “exposing the patient to radiation” as an additional point for making the case to not X-ray patients. 17
We and many others have recently provided details of why low-dose radiation exposures (<200 mGy), including those from X-rays and CT scans are not harmful. 13 -16,26 -31,36 -48 The issue of ionizing radiation carcinogenicity is the main underpinning for all anti-imaging rhetoric. Here we sum up many of the arguments against LNT and related concepts that refute the presumptive notion that X-rays cause cancer.
The LNT Model Is Not Valid for Low-Dose Radiation Exposures
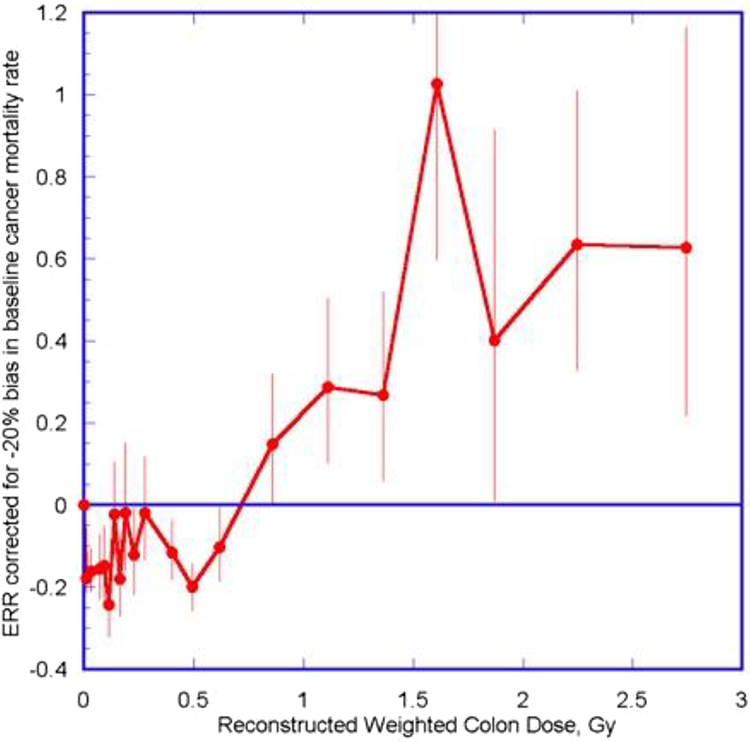
The Lifespan study (LSS) of the Hiroshima and Nagasaki survivor data is espoused to be the main evidential support for the LNT model, 146 however, the BEIR VII has been heavily criticized for being based on faulty assumptions and analyses. 147 -149 A recent analysis of the LSS data by Ozasa et al. was published in 2012, 150 and, when corrected for a “likely negative bias” in baseline cancer mortality, the data shows a non-linear (quadratic) curve that represents a hormetic pattern rather than the traditional assumed linear (LNT) pattern (Figure 4). 151,152 Thus, the persons exposed to the fallout outlived controls. 153 Further, others have questioned the validity of the LSS data to support the LNT, 154,155 for example, Socol et al. demonstrated that after performing a Monte-Carlo simulation of possible LSS outcomes, they determined that the LSS had insufficient statistical power to support the LNT. 155
On a more fundamental level, recent information has emerged that shows that the LNT model that was first adopted back in the 1950s was spawned based on scientific fraud and misconduct. 156 -159 The LNT model was adopted based on Hermann J. Muller’s original fruit fly experiments, 160 where very high X-ray radiation doses were shown to produce transgenerational phenotypic changes; these changes were claimed by Muller to be gene mutations. 158 -160 Significantly, the claimed gene mutations were only gene deletions and other chromosomal rearrangements; this misinformation misdirected the radiation genetics research field for decades. 158 As it turns out, there is good evidence suggesting that Muller’s nobel prize winning research published in Science in 1927 evaded peer review, and by doing so, he was able to claim primacy for discovering gene mutation. 158
To this day, the major governmental and international radiation regulatory bodies continue to support the LNT model for risk assessment despite the exponential increase of evidence showing its invalidity. 161 -163 Recent reviews of available evidence, not surprisingly, do not support the use of the LNT for risk assessment from the low-dose exposure range. Vaiserman et al., for example, concluded that the “LNT has certainly not been proven to be true” and suggest that, due to the high economic and human costs, the present regulatory burden should be reduced. 162 Recently, the Society of Nuclear Medicine and Molecular Imaging convened a task group to examine the validity of the LNT and its applicability for use in risk assessment and radiation protection. The group concluded “the evidence does not support the use of LNT either for risk assessment or radiation protection in the low-dose and dose-rate region.” 163
Unfortunately, based on the dubious history surrounding the origins of the LNT and the continued loyalty to the LNT by the major governing bodies despite direct challenges to the continued endorsement of the LNT by these bodies (e.g. BEIR VII 147 -149 ), the LNT has evolved to be more political than scientific. 164,165 Many have presented possible alternatives to the LNT that may be plausible moving forward. 166 -171 Indeed, as Cardarelli and Ulsh argue, abandoning use of the traditional LNT model for low dose low-dose rate radiation risk assessment by incorporating updated science into the regulatory process could be successful to ensure science remains the underpinning of decision making, to educate the public on the lack of risks from low-dose radiation exposures, and to “harmonize government policies with the rest of the radiation scientific community.” 172 (p1)
ALARA Is an Obsolete Radiation Protection Concept
Since the LNT model is not valid for low dose radiation, any concept borne by it is also invalid and obsolete. 37,39,41 Many have pleaded for the termination of the ALARA concept and anti-imaging campaigns as used in medical imaging. 37,41 -44,170,171,173 -175 ALARA and the anti-imaging campaigns that endorse it including Image Gently (pediatrics), 176 Image Wisely (adults), 177 and Choosing Wisely, 178 leads to no benefits and ironically may cause more harm (Table 4). 37
Synopsis of How ALARA Causes More Harm Than Benefit. 37

Actual real harm (and presumed harm by increased radiation exposures) by adhering to the ALARA principle include propagating radiophobia, 179 which in turn, increases patient refusal for medically warranted X-rays, 180,181 which in turn, increases the burden to medical professionals attempting to deliver high-quality medical care. 37 Reduced image quality, by attempting to reduce radiation to the patient, 182,183 increases potential missed diagnoses. 41,174 Other harms include increased radiation exposures because of retakes (due to using too little exposure or gonadal shielding covering targeted anatomy), 37,182,184,185 increased use of alternate imaging methods that presents other unique risks (e.g. sedation during MRI), 182,186 and perhaps most importantly, increased liability to physicians. 37
In short, the ALARA concept would only be valuable if radiological medical imaging were proven to cause future cancers. However, this is not the case. In a recent study performing a quantitative evaluation of the methodological quality of an originally selected 4,382 studies in order to determine the evidentiary strength either supporting or refuting a causal relationship between low-dose radiation and cancer, it was determined that the majority of articles(84%) having high-quality methods found no increased risk of cancers from exposure less than 200 mSv. 187 The authors concluded “The evidence suggests that exposure to multiple CT scans and other sources of low-dose radiation with a cumulative dose up to 100 mSv (approximately 10 scans), and possibly as high as 200 mSv (approximately 20 scans), does not increase cancer risk.” 187
The Threshold of Carcinogenesis From Radiation Exposures Is High
As mentioned, when a 20% correction for baseline cancer incidence is accounted for in the Ozasa et al. 150 updated analysis of the LSS, the threshold for cancer incidence shows a value of 700 mSv (Figure 4). 151,152 Cuttler has reassessed the 1958 UNSCEAR data and found that the threshold for leukemia is at 1100 mGy (95% CI: 0.5-2.6 Gy), much higher than previously thought (Figure 5). 188,189 It was also noted than even in the persons who developed leukemia, they accounted for only 0.5% of the exposed cohort. 188 As Oakley and Harrison recently stated: “even considering the lower threshold dose of 700 mGy, this represents about 2 to 3 orders of magnitude greater than the amount of radiation given from medical X-rays.” 36(p.3) Thus, diagnostic X-rays cannot be expected to cause cancers.
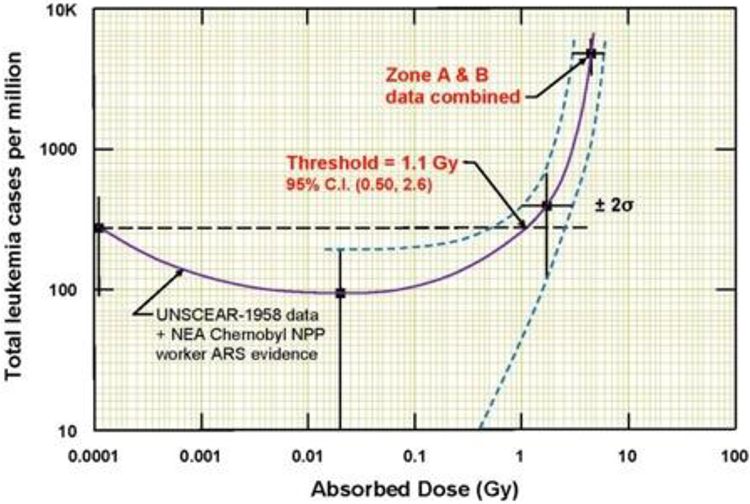
1958 UNSCEAR data indicates a threshold of about 1.1 Gy (1100 mGy; assuming RBE = 1) for radiogenic leukemia in 95,819 persons exposed to A-bomb radiation from Hiroshima. 189
Low-Dose Radiation Upregulates the Adaptive Protection Systems and Prevents Cancers
Although those that push to restrict routine and repeat X-rays for spine care quickly dismiss the concept of radiation hormesis (e.g. Kawchuk et al. 23 ), in our opinion, this reason alone invalidates X-ray fear-mongering from supposed future cancers. The fact is, and as Cuttler astutely reminds us, that experience over the last 120 years has shown that low doses of radiation stimulate the innate protection systems, including the immune system, and these processes involve more than 150 genes. 190
Exposures to low-dose radiation incites multiple and multi-hierarchical biopositive mechanisms that prevent, repair or remove damage caused mostly by endogenous reactive oxygen species (ROS) and H2O2 from aerobic metabolism. 191 -193 Indeed, non-radiogenic (i.e. naturally occurring) molecular damage occurs daily at rates many orders of magnitude greater than the rate of damage caused by low-dose radiation such as diagnostic X-rays. 194 -196 It is estimated that the endogenous genetic damage caused on a daily basis from simply breathing air is about one million times the damage initially resulting from an X-ray. 15 We concur that “it is factually preposterous to have radiophobic cancer concerns from medical X-rays after considering the daily burden of endogenous DNA damage.” 18(p7)
Many have presented overviews of the physiological mechanisms that lead to hormetic effects (Figure 6) 197 -202 and these redundant and efficient processes include DNA repair systems, programed cell death, cell cycle delay, cellular senescence, adaptive memory, bystander effects (exposed cells communicate to non-exposed cells), epigenetics, immune stimulation and tumor suppression (Table 5). The irony is that the stimulation and upregulation of innate protection mechanisms and immune status is what accounts for the curative effects from low-dose irradiation therapies for the treatment of many human ills including inflammatory and neurodegenerative conditions, infections and cancers (Table 6). 190, 203 -225

The adaptive response systems very efficiently prevent, repair or remove virtually all DNA alterations. 196
Body’s Multiple Adaptive Response Mechanisms That Prevent, Repair and Remove Damage Caused From Mostly Endogenous Reactive Oxygen Species and H2O2 From Aerobic Metabolism. 200

Historically, it is important to mention that many human diseases were treated by X-rays, so-called “radiotherapy.” Unfortunately, despite radiotherapy showing a 75%-90% efficacy rate, 203 the treatment fell out of favor due to the evolution of antibiotics and also from fears of radiation following the atomic bomb droppings during WWII. Radiotherapy was documented to successfully treat arthritis, 204 bronchial asthma, 205 carbuncles, 206 cervical adenitis, 207 deafness, 207 furuncles, 206 gas gangrene, 208 necrotizing fasciitis, 209 otitis media, 207 pertussis, 210 pneumonia, 211 sinus infection, 212 and tendonitis/bursitis. 213 These human ailments were treated using typical radiation doses ranging from 30 to 100 roentgen (∼0.3-1.0 mGy) which are fairly high doses, yet there are no reports of ill health effects from these treatments.
Many different cancers have also been successfully treated using radiotherapy. 214 -220 The typical patient dosing involves exposing the patient to 1.5 Gy over 5-weeks. 214 -217 It is also noteworthy that radiotherapy (whether given by X-rays or radon) has been making a resurgence in the literature; recent case reports have documented the successful treatment of cancers (e.g. prostate, colon, uterine, lung, and liver cell), ulcerative colitis, rheumatoid arthritis, pemphigus, diabetes types I and II, Alzheimer’s disease and Parkinson’s disease. 221 -225
The Total Collective Effective Dose (TCD) Concept Is Invalid for Low-Dose Radiation
LNT ideology assumes all radiation is cumulative, that an increase in one’s total collective effective dose (TCD) equates to a linear increase in harm. Thus, dose is used as a surrogate for risk.
226
As just discussed, however, low-dose radiation exposures upregulate the innate adaptive response systems, which result in a net zero or less genetic damage (i.e. via over-repair) than was present prior to the initial exposure. This was proven to occur by Löbrich et al. who determined that DNA double-strand breaks (DSBs) occur in human lymphocytes after CT scans; however, these DSBs were repaired between 5 and 24 hours after the scan.
227
Most importantly, the endogenous repair mechanisms repaired more than the damage that had initially occurred from the initial scan. Indeed, the final DSB count was
This illustrates how the simple mathematical addition of low-dose exposures to increasing TCDs is theoretical risk and not reflective of reality. A case example is for an adolescent idiopathic scoliosis (AIS) patient, where repeat imaging is necessary during the treatment and monitoring of his/her condition. If we assume the dose threshold for leukemia is 1100 mGy as reported by Cuttler, 189 it has been stated: “Since the body’s adaptive response will repair damage done at each X-ray event, X-ray exposures of about 1 to 3 mGy will always remain at a level that is 367 to 1100 times below the carcinogenic dose threshold.” 39
It should be noted that even if the LNT were valid, “the calculation of the number of cancer deaths based on collective effective doses from trivial individual doses should be avoided.” 228
Risk remains a population-based metric; therefore, its assignment to the individual should never be interpreted deterministically. 229 This is because individual effective dose effects have uncertainty, up to plus or minus 40% due to age, gender, mass, etc. 230,231 Mitchel argues that the assumption of dose additivity is not supported by the literature and states: “at the low doses and dose rates typical of public and occupational exposures, the radiation protection principle of dose additivity, and the concept that risk can only increase as dose increases are not justified. In general, the use of dose as a surrogate for risk needs re-evaluation.” 226 (p287) The TCD concept is flawed and not valid as a model for assessing cancer risk from low-dose exposures. 226,232
Aged Cohort Studies Purveying Radiogenic Cancers From Prior Exposures Are Not Generalizable
LNT advocates quickly cite studies that show patient cohorts exposed to radiation during childhood (e.g. CT scans) have also been shown to have increased cancers in adulthood (e.g. Pearce et al., 233 Mathews et al., 234 Hong et al. 235 ). Although on the surface it may seem plausible, this correlation could be causal. The aphorism “correlation is not causation” applies. In fact, the critical flaw to these types of studies is that healthy children do not usually receive CT scans. Therefore, these studies suffer from “reverse causation,” or that the reason for the CT scan in the first place was due to underlying diseases that predisposes one to develop cancer, or actual suspicions of malignancy itself. 236,237
Indeed, Journey et al. proved reverse causation after first finding a statistical correlation of increased cancers in a cohort of adults who were CT imaged in youth. When controlling for the reasons for the scans, no statistical correlation prevailed. 238 Shibata et al. also determined that of 763 children receiving CT scans, 32% had congenital anomalies. 239 Since the normal incidence of congenital anomalies is only about 2.5%, they concluded “the population of children undergoing CT is completely different from that not undergoing CT. The 2 groups should not be compared.” 239 Thus, the oft cited and heavily amplified carcinogenic fears of future cancers from medical imaging is not supported.
Conclusions
Routine and repeat X-rays in the nonsurgical treatment of patients with spine disorders is an evidence-based clinical practice that is warranted by those that practice spine-altering methods. The evidence supporting such practices is based on definitive evidence supporting the rationale to assess a patient’s spinopelvic parameters for biomechanical diagnosis, to screen for relative and absolute contraindications for specific spine care methods, and to re-assess the spine and postural response to treatment.
The traditional and underlying presumption of the carcinogenicity from X-rays is not a valid notion because the LNT is not valid for low-dose exposures. The ALARA radiation protection principle is obsolete, the threshold for harm is high, low-dose exposures prevent cancers by stimulating and upregulating the body’s innate adaptive protection mechanisms, the TCD concept in invalid, and aged cohort studies assumed to show cancers resulting from previous X-rays are not generalizable to the wider population because they represent populations predisposed to cancers.
Red flags, or suspected serious underlying disease is a valid consideration warranting screening imaging by all spine care providers. We contend, however, that as long as the treating physician or rehabilitation therapist is practicing evidence-based methods, proven to improve spine and postural parameters in order to provide relief for the myriad of spinal disorders, spinal X-rays are unequivocally justified. Non-surgical spine care guidelines need to account for proven and evolving non-surgical methods that are radiographically guided, patient-centered, and competently practiced by those specialty trained in such methods. This is over and above so-called “red flag only” guidelines. The efforts to universally dissuade chiropractors from routine and repeat X-ray imaging is neither scientifically justified nor ethical.
Footnotes
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: P.A.O. is a paid research consultant for CBP NonProfit, Inc.; D.E.H. teaches spine rehabilitation methods and sells products to physicians for patient care that require radiography for biomechanical analysis.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by funds from CBP NonProfit, Inc.