Abstract
Prostate-related conditions, including benign prostatic hyperplasia, prostatitis, and prostate cancer, represent significant health concerns, particularly among aging men. This study utilized a comprehensive review of existing literature and case studies to explore the effectiveness of integrative approaches, emphasizing nutrition, exercise, and lifestyle modifications, in managing prostate diseases. Data were collected from peer-reviewed journals, clinical trials, and meta-analyses focusing on dietary patterns, physical activity, and complementary therapies. The findings were synthesized to provide evidence-based recommendations. Results highlight that plant-based diets, rich in fruits, vegetables, whole grains, and healthy fats, demonstrate protective effects against prostate conditions, while diets high in saturated fats and processed foods increase risk. Specific bioactive compounds,such as lycopene, omega-3 fatty acids, and polyphenols, were linked to reduced disease progression. Physical activity emerged as a key component, enhancing hormonal balance, reducing inflammation, and improving survival rates in prostate cancer patients. Aerobic and resistance exercises were particularly effective in mitigating treatment side effects such as fatigue and muscle loss. Stress-reduction techniques, including mindfulness and yoga, alongside moderated alcohol consumption, further improved psychological well-being and overall prostate health. Integrative approaches, combining conventional treatments with holistic care, demonstrated enhanced outcomes by addressing the physical, emotional, and social dimensions of prostate disease. Emerging fields such as nutrigenomics and natural products offer opportunities for personalized interventions, paving the way for innovative management strategies. This study underscores the potential of integrative methods to improve disease outcomes, prevent progression, and enhance the quality of life for men affected by prostate conditions, advocating for their inclusion in prostate disease management protocols.
Introduction
Prostate-related conditions, including benign prostatic hyperplasia (BPH), prostatitis, and prostate cancer (PCa), represent a major health issue, especially for aging men. The prostate gland, situated just beneath the bladder, plays a vital role in male reproductive health by contributing to seminal fluid production (InformedHealth.org, 2006). Advancing age increases the likelihood of developing these conditions, which can have a profound effect on both health and quality of life (Singh & Bolla, 2023). Prostate cancer, a leading malignancy among men globally, exhibits varying prevalence across regions and often progresses gradually, though it can become aggressive and life-threatening in certain cases. BPH, a non-cancerous prostate enlargement, is common in older men and frequently causes urinary issues that disrupt daily activities (Aaron et al., 2016; Pendegast et al., 2021). Prostatitis, an inflammation of the prostate, can occur at any age and often results in chronic pelvic pain and urinary issues (Pendegast et al., 2021).
Prostate disease management has relied heavily on medical interventions, including pharmaceutical treatments, surgery, and radiation therapy. For prostate cancer, options such as radical prostatectomy, radiation therapy, and androgen deprivation therapy (ADT) are commonly employed (Gilbert et al., 2017; Siddiqui & Krauss, 2018). These depend on the stage and aggressiveness of the disease (Narayan et al., 2021). BPH is typically managed with medications such as alpha-blockers and 5-alpha-reductase inhibitors, and in some cases, surgical interventions such as transurethral resection of the prostate are necessary (Miernik & Gratzke, 2020). Prostatitis is often treated with antibiotics, anti-inflammatory drugs, and other supportive therapies (Vs et al., 2018). While these conventional approaches can be effective, they are not without limitations and potential side effects. ADT in prostate cancer can lead to osteoporosis, cardiovascular issues, and a decline in quality of life due to hormonal imbalances (Siddiqui & Krauss, 2018). Surgical treatments for BPH may result in complications such as incontinence and sexual dysfunction. As a result, there has been growing interest in integrative approaches that complement standard medical treatments with lifestyle modifications, nutrition, and exercise (Tabish, 2008).
Recent studies highlight how important nutrition is in preventing and managing prostate diseases. Diets abundant in fruits, vegetables, and whole grains, combined with a reduction in red and processed meats, are linked to a decreased risk of prostate cancer and other prostate-related conditions (Oczkowski et al., 2021). Key nutrients such as lycopene in tomatoes, polyphenols in green tea, and omega-3 fatty acids from fish have demonstrated promise in mitigating prostate cancer risk and progression (Maximova et al., 2020). The Mediterranean diet, characterized by a high intake of plant-based foods, healthy fats, and moderate consumption of dairy and wine, has been associated with a lower incidence of prostate cancer (Frattaroli et al., 2008). The diet’s anti-inflammatory and antioxidant properties are thought to underlie its protective effects on prostate health. Diets high in saturated fats, sugars, and processed foods have been correlated with an elevated risk of prostate disease, including aggressive prostate cancer (Bagheri et al., 2018). In addition, obesity, often stemming from poor dietary habits, is a recognized risk factor for both BPH and prostate cancer, highlighting the central role of proper nutrition in maintaining prostate health (Mousavi et al., 2024).
Physical activity plays a vital role in a comprehensive strategy for managing prostate diseases. Regular exercise has been found to lower the risk of prostate cancer, slow disease progression, and enhance survival rates (Spanoudaki et al., 2023). These benefits are attributed to mechanisms such as hormonal regulation, including insulin and testosterone balance, reduced chronic inflammation, and strengthened immune function (Pizot et al., 2016; Thomas et al., 2021). For men with BPH, exercise helps alleviate urinary symptoms by boosting cardiovascular health and reducing abdominal fat, a factor that can worsen lower urinary tract symptoms (LUTS; Pizot et al., 2016). In cases of chronic prostatitis, physical activity has been linked to decreased pain and improved overall quality of life (Moore et al., 2016).
Research highlights the importance of exercise in mitigating the side effects of prostate cancer treatments. Resistance training and aerobic exercises, for instance, are effective in reducing fatigue and muscle loss often caused by ADT while also enhancing mental health in patients undergoing cancer treatment (Dawson et al., 2018; Houben et al., 2023). In addition to exercise and diet, other lifestyle factors such as quitting smoking, managing stress, and moderating alcohol consumption significantly influence prostate disease management (Dawson et al., 2018). Smoking has been associated with increased prostate cancer mortality, and cessation is linked to improved outcomes in men with the disease (Houben et al., 2023).
Stress management is also critical, as chronic stress can worsen symptoms of BPH and prostatitis and may accelerate prostate cancer progression (Mousavi et al., 2024). Complementary therapies such as mindfulness meditation, yoga, and cognitive-behavioral therapy have been studied for their role in reducing the psychological impact of prostate diseases, improving mental health, and enhancing the overall quality of life (González-Valero et al., 2019; K. E. Riley et al., 2017).
Alcohol consumption is a controllable factor that influences health outcomes. While excessive alcohol intake has been associated with an increased risk of aggressive prostate cancer and exacerbated urinary symptoms in men with BPH (K. E. Riley et al., 2017), some studies indicate that moderate consumption, particularly of red wine, might have protective benefits. This potential benefit is attributed to resveratrol, a compound recognized for its anti-inflammatory and antioxidant effects (Snopek et al., 2018).
The concept of integrative approaches to prostate disease management combines conventional medical treatments with evidence-based complementary therapies. These approaches are holistic, considering the patient’s physical, emotional, and social well-being. For instance, a comprehensive management plan for a patient with prostate cancer might include surgery or radiation, alongside dietary interventions, exercise programs, stress management techniques, and nutritional supplementation (González-Valero et al., 2019). Emerging fields such as nutrigenomics, which studies the interaction between genes and nutrients, are paving the way for personalized nutrition strategies in prostate disease management (Ferguson & Karunasinghe, 2011; Kiani et al., 2022). The use of phytochemicals, probiotics, and other natural products is being explored for their potential role in supporting prostate health and enhancing the efficacy of conventional treatments (Ferguson & Karunasinghe, 2011; Hao et al., 2022; Salehi et al., 2019).
Explicitly, prostate disease management is evolving toward more integrative and patient-centered approaches that emphasize the role of nutrition, exercise, and lifestyle modifications. These strategies not only complement traditional medical treatments but also empower patients to take an active role in managing their health. As research continues to uncover the complex interplay between diet, lifestyle, and prostate health, integrative approaches are likely to become an increasingly important component of prostate disease management. Predictably, integrative approaches hold the prospect of offering a more holistic and effective means of improving outcomes and quality of life for men affected by prostate conditions.
Case Studies on Successful Implementation of Integrative Approaches Toward Prostate Disease Management





Role of Nutrition in Prostate Health
Introduction
The prostate gland, an integral part of the male reproductive system, is responsible for producing seminal fluid, a vital component of sperm. Various factors can cause abnormal changes in prostate cells, potentially leading to malignancy or cancer. Prostate cancer accounts for approximately one-fifth of all new cancer diagnoses in men, making it one of the most common cancers after skin cancer (Public Health Agency of Canada [PHAC], 2015). Early warning signs often include urinary difficulties such as increased frequency and urgency, an inability to fully empty the bladder, blood in urine or semen, painful ejaculations, and abdominal or pelvic pain (PHAC, 2017). As the disease advances, additional symptoms like weight loss, fatigue, anemia, loss of bladder control, and bone pain may emerge.
The prevalence of prostate cancer varies significantly across countries and regions, influenced by factors such as exercise levels, obesity rates, genetic predisposition, and dietary habits (Ornish et al., 2013). Among these, diet and nutrition play a particularly pivotal role. Experts have highlighted that the stark differences in prostate cancer rates globally are largely attributable to dietary patterns. Plant-based diets, which include minimally processed foods such as vegetables, fruits, legumes, nuts, seeds, whole grains, and lean proteins such as fatty fish (e.g., salmon and sardines), are associated with a reduced risk of prostate cancer.
Unhealthy dietary habits, including the regular intake of saturated and trans fats or processed meats, significantly elevate the risk of developing prostate cancer (Kaiser et al., 2019). Such diets can interfere with hormonal balance, trigger oxidative stress and inflammation, and disrupt growth factor signaling and lipid metabolism, thereby fostering carcinogenesis in prostate cells. As diet is a modifiable risk factor, recognizing the protective and harmful roles of specific nutrients and eating patterns is essential for effectively preventing and managing prostate cancer.
Prostate Health: The Role of Nutrition
Diets rich in plant nutrients are becoming emerging options with potential benefits in mitigating prostate-related health conditions. Though the mechanism linking plant-based nutrients to a decrease in prostate cancer risk or management outcome is not clear, plant nutrients in fruits and vegetables have a long history that associates their intake with improved prostate health. Research evidence supporting improved prostate health risk or management outcome and plant-based foods or their constituents are ultimately scarce (Shah & Iyengar, 2022). Findings from various in vivo and in vitro trials, as well as clinical and epidemiological studies, have consistently demonstrated that both nutrients and food products play crucial roles in either promoting or preventing prostate oncogenesis. Certain nutrients, such as saturated and trans fats, along with processed meats, have been shown to disrupt normal prostate hormonal regulation, induce inflammation, enhance oxidative stress, and interfere with growth factor and lipid metabolism, collectively fostering prostate cancer development.
Research investigating the link between fat consumption and prostate cancer risk highlights that both the amount and type of fat consumed play a crucial role in disease progression. A study tracking 288,268 men, including 23,281 cases of prostate cancer over 9 years, found that those with high saturated fatty acid (SFA) intake—comprising up to 13.3% of their total energy—had a significantly elevated risk of developing advanced prostate cancer compared to individuals with lower SFA consumption (below 5.8%; Liss et al., 2019). Similar findings in animal studies by Sonn et al. (2005) showed accelerated cancer cell growth with increased dietary fat intake. Diets low in fat were associated with inhibited cancer development, reduced androgen sensitivity in cancer cells, and decreased malignancy. These effects are thought to result from fat intake’s influence on hormonal balance and androgen concentration, coupled with elevated oxidative stress.
Diets rich in fat have been associated with elevated levels of proinflammatory cytokines and the activation of critical signaling pathways regulated by transcription factors such as STAT-3 and NF-κB (Hayashi et al., 2018; Vykhovanets et al., 2011).
Diets rich in vegetables, fruits, and whole grains exhibit protective and therapeutic effects due to the bioactive compounds they contain, such as flavonoids, stilbenes, and lycopene (Ambrosini et al., 2008; Jalilpiran et al., 2018; Niclis et al., 2015; Walker et al., 2005). These compounds help mitigate oxidative stress and inflammation, countering processes linked to prostate cancer progression. Researchers emphasize that dietary patterns and nutrient intake are modifiable risk factors critical to the prevention and management of prostate-related health issues. Observational and epidemiological evidence-based studies have linked unhealthy diets, such as alcohol consumption, tobacco smoking, and increased proneness to noncommunicable diseases, including cancer(Bagnardi et al., 2015; Grosso et al., 2017; Kopp, 2019; Lope et al., 2019). Excessive caloric intake alongside high intake of SFAs and sugar has been associated with a high risk of prostate cancer. Uncontrolled caloric intake predisposes one to a condition called obesity (overweight), which is positively correlated with high cancer risks, hence, it is, however, rational to advocate that calorie restriction accompanied by weight reduction strategies can aggressively improve prostate health as reported by Bonorden et al. (2009). This claim was supported by the evidence-based finding that 30% reduction in caloric intake in Hi-Myc transgenic mice delays prostate cancer development and progression and similar caloric restriction in transgenic adenocarcinoma of the mouse prostate (TRAMP) mice with prostate cancer prolongs its survival (Rodriguez et al., 2007). It has been observed in preclinical studies that weight loss can suppress the proliferation of prostate cancer by significantly decreasing the plasma concentration of insulin-like growth factor 1 (IGF-1) with a concomitant reduction in inflammation that accompanies obesity (Blando et al., 2011).
Despite substantial evidence supporting dietary influences on prostate health, some studies highlight the complexities involved in correlating specific diets with prostate cancer progression. For instance, a 180-day low-carbohydrate regimen in patients with biochemical recurrence showed no significant improvement in PSA doubling time compared to controls, underscoring the need for further research into the effects of calorie reduction and weight loss on prostate cancer progression (Freedland et al., 2020).
Processed and smoked meats are known to contain carcinogenic compounds such as polycyclic aromatic hydrocarbons, N-nitroso compounds, and heterocyclic aromatic amines, all of which contribute to the onset and progression of prostate cancer (Turesky, 2018). A case-control study by Niclis et al. (2015), involving 147 prostate cancer patients and 300 controls, identified four unique dietary patterns that influence prostate health.
The Traditional Pattern emphasizes high consumption of fatty red meats, processed meats, and starchy vegetables, while the Prudent Pattern prioritizes non-starchy vegetables and whole grains. The Carbohydrate-Heavy Pattern consists mainly of sodas, juices, and baked goods, and the Cheese-Focused Pattern revolves around cheese consumption. The study revealed that adherence to the traditional and carbohydrate-heavy dietary patterns was strongly correlated with an increased risk of prostate cancer progression. These findings are consistent with other controlled studies, which have similarly linked such dietary habits to heightened cancer risk (Shin et al., 2018; Walker et al., 2005). This growing body of evidence highlights the vital role that dietary choices play in influencing the risk and progression of prostate cancer. In addition, energy intake is a key factor; reduced caloric consumption has been associated with increased rates of apoptosis relative to angiogenesis and cell proliferation in cancer tissues, effectively suppressing cancer progression (Chen et al., 2011; Kopeina et al., 2017; Safdie et al., 2009). These findings suggest that energy modulation in diets could be a valuable strategy for mitigating cancer growth.
Plant-based nutrients, or phytonutrients, such as isoflavones found in soybeans, have demonstrated protective effects against prostate cancer. Soy-based foods such as tofu, soymilk, soy nuts, tempeh, and edamame are rich in flavonoids with antioxidant and anticancer properties (Zhang et al., 2017). Isoflavones, catechins, resveratrol, and related compounds have been shown to inhibit cancer cell growth through mechanisms such as androgen receptor modulation, suppression of testosterone conversion, and enhancement of tumor suppressor gene expression (Kumar et al., 2004; Sivoňová et al., 2019). These compounds are particularly abundant in Asian diets, which may explain the lower prostate cancer incidence observed in these populations (Kurahashi et al., 2007; Sonoda et al., 2004).
Green tea, abundant in polyphenols such as epigallocatechin-3-gallate (EGCG), has been widely researched for its cancer-protective effects. It suppresses prostate cancer cell proliferation and angiogenesis while inducing apoptosis. Experiments involving PC-3 prostate cancer cell lines demonstrated decreased expression of proliferation markers such as Bcl-2 and Ki-67, alongside increased activation of pro-apoptotic caspases, thereby lowering the potential for metastasis (Xu et al., 2019; Wang et al., 2016).
Lycopene, a powerful carotenoid antioxidant present in tomatoes and various fruits, has also demonstrated significant protective effects against prostate cancer. Thermal processing of tomatoes increases lycopene bioavailability, making products such as tomato sauce and ketchup valuable sources. Lycopene’s antioxidant properties help neutralize reactive oxygen species, repair DNA damage, and modulate cell cycle enzymes and IGF-1 activity, which are linked to cancer risk (Mirahmadi et al., 2020; Trejo-Solís et al., 2013). Studies have shown that higher lycopene intake correlates with a reduced risk of lethal prostate cancer, particularly in the pre-PSA era (Zu et al., 2014).
These findings reinforce the importance of dietary modifications, emphasizing the protective potential of plant-based diets and the risks associated with high-fat and processed food consumption. Further research is essential to fully elucidate the mechanisms through which these dietary factors influence prostate cancer progression and prevention.
Impacts of Exercise on Prostate Health: Evidence and Recommendations
Introduction
Prostate cancer has been referred to as the second most common form of cancer in men. Due to the substantial rise in the population of developed countries, it is expected that the incidence of the disease will rise further as a result of increased life expectancy and population of aged people (Torre et al., 2016). Improvement in the serological screening techniques applied in the detection of PSA has revolutionized early diagnosis, treatment, and management of prostate health with notable improvement in survival outcome (Miller et al., 2016). Physical exercise has been viewed as a provocative medicine with proven preventive, complementary and rehabilitative role in prostate, and other cancers management. Exercise has therefore been noted as an emerging synergistic and medicinal option that can improve symptoms, modulate prostate biochemistry, and delay progression of the disease, thereby leading to increased survival (Hart et al., 2017).
Exercise is a subset of physical activity that is planned, structured, and repetitive, which has as the final or intermediate objective improving or maintaining physical fitness (Dasso, 2018). The association between exercise and reduced prostate cancer progression and mortality has witnessed little proof, particularly in the underlying biochemical mechanism leading to the health benefits. There are, however, postulations that guided physical activity may acutely reduce tumor-associated hypoxia by increasing tumor cell perfusion. The postulation predicted possible structural adaptation of the tumor vasculature in response to exercise (B. D. Hayes et al., 2016). Identification of exercise as a safe, feasible, and effective treatment approach for advanced prostate cancer patients has been viewed as a major breakthrough, with epidemiological evidence showing an association between physical activity and increased survival rate. One of the major features of advanced prostate cancer is the potential for recurrence or invasion of the primary carcinoma to secondary locations. As a result, men with advanced prostate cancer face challenges of high disease burden, which as a result make it necessary to recommend treatment options such as exercise, which is known to be cheap, safe, noninvasive, and effective in reducing the disease burden. Exercise is therefore an emerging therapy in oncology (prostate cancer inclusive) with an excellent promise to meet patients’ requirements (MacAuley et al.,2015; Newton et al., 2016; Sallis, 2009). Physical activity is presently and increasingly being recognized as an essential component of treatment therapy that helps to improve or maintain a balanced physical function and quality of life in prostate cancer patients (S. C. Hayes et al., 2019). Research has shown that a planned regimen of physical exercise, not only during but also after completion of therapy, can reduce patients’ experience of fatigue (Buffart et al., 2015; Galvão et al., 2010, 2014; Segal et al., 2009). Researchers have indicated some level of proof that exercise may help ameliorate treatment-related toxicities (Cormie et al., 2015; Kapur et al., 2010).
Exercise and Prostate Health: Evidence and Recommendations
Generally, regular and regimented exercise has been reported to be important primarily in the prevention of different forms of cancer. Exercise has been shown to have a link with decreased risk of endometrial, colon, bladder, renal, gastroesophageal, and breast cancer (Behrens & Leitzmann, 2013; Boyle et al., 2012; Keimling et al., 2014; Voskuil et al., 2007; Wu et al., 2013) in dose-related manner with convincing evidence that exercise reduces hematological cancer risks (Jochem et al., 2014). Researchers have adduced several evidence-based publications pointing to the role of exercise in ameliorating nonspecific symptoms related to cancer, reduction in cardiovascular risk indicators (Ligibel et al., 2008), and improves general reduction in body weight. Result of a meta-analysis published by Tomlinson et al. (2014) observed that exercise can moderately reduce cancer-related fatigue and improve symptoms of depression and sleep disturbance. An aerobic exercise has been identified in a Cochrane study by Cramp and Byron-Daniel (2012) to have a potential beneficial role for individuals with cancer-related fatigue during and after cancer therapy. As nonaggressive heterogeneous form of cancer, prostate cancer risk factors is different from the aggressive or lethal ones, thus a questionnaire-based study using 1,063 controls recorded that vigorous physical activity that spanned over the first 18 years of life decreased prostate cancer risk (Friedenreich et al., 2015; E. L. Giovannucci et al., 2006). Though some prospective studies have claimed no association between occupational activity or leisure time activity with prostate cancer incidence (Johnsen et al., 2009), a good number of published research outcomes have linked occupational activity with a lower risk of advanced stage prostate cancer. Similarly, some experts in various studies have identified a lower risk of advanced prostate cancer in men over 65 years who embark on various degrees of vigorous physical activity (E. Giovannucci et al., 2007). Other studies identified a higher risk of prostate cancer in a population of men undertaking exercise (Wiklund et al., 2008; Zeeger et al., 2005). It is therefore difficult to state with precision the quantity and type of exercise that would be associated with a higher or lower risk of prostate cancer.
Evidently, exercise has been shown to have identifiable benefits in ameliorating prostate cancer treatment side effects such as improved muscular strength, cardiorespiratory fitness, lean body mass, and fatigue (Gardner et al., 2014). It was observed in a study that 66 men undergoing radiotherapy notably had a significant reduction in rectal toxicity after 30 min of aerobic exercise thrice a week for 4 weeks, and others receiving androgen blockers improved fatigue, strength, triglycerides, and body fat with exercise (Kapur et al., 2010). Research data suggest that exercise can modify the biochemistry of prostate cancer and related parameters. In a study using 2,705 men without metastatic prostate cancer who survived at least 4 years after diagnosis, vigorous exercise types such as cycling, swimming, jogging for more than 3 hr weekly led to lower prostate cancer-related mortality (Kenfield et al., 2011). A related study observed a 57% reduction in prostate cancer progression rate in men, walking quickly was, therefore, associated with reduced progression irrespective of duration (Richman et al., 2011). Several other recent studies provide further evidence that physical exercise decreases prostate-related mortality (Friedenreich et al., 2016; Richman et al., 2011).
Exercise plays a role as an adjunct therapy to several conventional treatments such as radiotherapy, where it has been reported to modulate tumor vasculature and oxygenation (Siemann et al., 2015; J. M. Wiggins et al., 2018). It has been notably reported that exercise leads to vascular adaptations in humans (Green et al., 2017) since it improves oxygen delivery to peripheral tissues through vascular remodeling processes such as angiogenesis and arteriogenesis (Prior et al., 2003). This structural vasculature remodeling due to exercise may take place in the tumor, hence providing oxygen in a similar way as a working muscle during and after exercise. In a moderate exercise condition, mechanical energy is exerted on the walls of the vessel as exercise intensity increases, and this is thought to enhance development of functional vasculature (Prior et al., 2004; Suh et al., 2011). Exercise in a dysfunctional prostate vasculature may result in the development of more mature but reduced permeable blood vessels that function more normally. Consequently, increased heat rate and stroke volume during exercise can augment cardiac output and increase systemic blood flow, thereby potentially boosting the perfusion of prostate tumor cells. Exercise results in a mild hyperthermia with consequential increase in vasodilation that invariably results in increased mean arterial pressure, making it possible for increased oxygen diffusion over a distance within the tumor, alleviation of tumor hypoxia, which in turn enhances treatment response to radiotherapy. Some animal studies looked at lymphoma, breast, and prostate cancer. They also examined how exercise training affects tumor growth, blood vessel function, and oxygen levels in tumors. Jones et al. (2010, 2012) found that tumor growth differed between animals that exercised using a running wheel and those that did not exercise. In a follow-up study by Betof et al. (2015), it was reported that exercise significantly reduced tumor growth in breast cancer, an observation that was corroborated by Jones et al. (2012) and Buss and Dachs (2018) using mice with high cytochrome c oxidase subunit IV in which it was suggested that only mice with higher volumes of exercise recorded a decrease in tumor growth and metastases.
Research suggests multiple mechanisms through which physical exercise may influence prostate cancer development and progression, including the reduction of oxidative stress, upregulation of anti-inflammatory pathways, and activation of apoptotic processes (Capece et al., 2020). While no single dominant mechanism has been identified, studies highlight the complex interplay of these biological processes.
In a randomized controlled trial by Schenk et al. (2020), even a brief 20-min session of aerobic exercise was associated with increased expression of mechanisms linked to reduced prostate cancer development. This finding supports the broader understanding that both occupational and recreational physical activities contribute positively, although the specific pathways remain multifaceted.
Large-scale studies have also linked physical activity to extended healthy lifespans and reduced cancer-specific mortality in prostate cancer patients. For example, Bonn et al. (2015) and Langlais et al. (2021) reported a dose-dependent relationship between activity levels and years lived in good health. Participants aged 50 to 75 who reported 60 metabolic equivalent (MET) hours of weekly physical activity lived an average of 6.3 years longer in good health compared to those with lower activity levels. These findings emphasize the potential of exercise to enhance life expectancy and quality among prostate cancer patients.
Friedenreich et al. (2016) demonstrated similar benefits in a study involving 830 men with stages I to IV prostate cancer. Participants engaging in 119 MET hours of physical activity weekly for a year experienced a 42% reduction in disease-related mortality compared to those reporting 42 or fewer MET hours weekly.
Further evidence from Dai et al. (2019) highlights the effects of vigorous exercise on prostate cancer progression and mortality. Men who engaged in 20 min of vigorous exercise weekly before their diagnosis had a 43% lower risk of lethal metastatic progression compared to less active individuals. In addition, these men exhibited lower methylation levels in the CRACR2A gene, which encodes a calcium-binding protein implicated in prostate cancer progression. This gene-specific epigenetic modification underscores the biological impact of regular, rigorous exercise.
These findings collectively reinforce the importance of physical activity as a noninvasive intervention to improve outcomes and reduce mortality in prostate cancer patients, further supporting its role in comprehensive cancer management.
Exercise and Prostate Health: Recommendations
Prostate cancer management has been primarily focused on the use of chemotherapy, radiotherapy, and invasive surgery. Physical exercise is becoming an emerging option for its identified role as an adjunct treatment. Despite that the role of exercise on prostate health has not been clearly demonstrated, its biochemical and physiological contributions in diagnosed cases where it enhances patients’ survival and quality of life have been established. It can therefore be recommended that the prescribed exercise for prostate health should be well planned in terms of type, dose, frequency, intensity, and duration, taking into consideration the disease stage. Regular, planned, and appropriately dosed exercise can also be recommended for noninfected individuals as preventive therapy for prostate cancer.
Lifestyle Modifications for Prostate Disease Prevention and Management
Evaluating the Role of Smoking Cessation and Alcohol Moderation in Reducing Prostate Disease Risk
Smoking and Prostate Disease
Smoking is a well-established risk factor for numerous cancers, including lung, bladder, and pancreatic cancers. Smoking and its relationship with prostate disease, particularly prostate cancer, has been subject to extensive research with varying conclusions. Some studies have demonstrated a positive correlation between smoking and the progression of prostate cancer (Gottlieb et al., 2016; Zhao et al., 2021), while others suggest a more nuanced relationship (Al-Fayez & El-Metwally, 2023).
Observational studies indicate that cigarette smoking appears to be inversely related to prostate cancer incidence. However, smokers face a higher likelihood of dying from prostate cancer. It is important to consider that this lower incidence among smokers could be due to factors such as reduced participation in prostate cancer screening by smokers, potential misclassification errors, or selection bias in the original studies used (Al-Fayez & El-Metwally, 2023). The study also observed that the risk decreased with the duration of smoking cessation, emphasizing the importance of quitting smoking as a preventive measure. The mechanisms through which smoking contributes to prostate cancer progression may involve the accumulation of carcinogenic compounds such as polycyclic aromatic hydrocarbons and nitrosamines, which can induce genetic mutations and promote cancer cell growth (Sosnowski et al., 2016).
According to the study by Al-Fayez and El-Metwally (2023), which examined smoking habits (including status, intensity, duration, and cessation) as a risk factor for prostate cancer incidence and mortality, both independently and in combination with body mass index (BMI), smoking was associated with a reduced overall risk of PCa (HR 0.89), particularly for low-risk cases (HR 0.74). This effect was most pronounced in cases diagnosed during the PSA screening era. However, smoking was linked to a higher risk of death from PCa in the entire cohort (HR 1.10) and in analyses adjusted for clinical factors (HR 1.20). These findings were consistent across different case groups and further supported by data on smoking intensity, duration, and cessation. In addition, smokers who were obese (BMI ≥30 kg/m2) had an even lower risk of low-risk PCa (HR 0.40) but a notably higher risk of PCa mortality (HR 1.49).
Alcohol Consumption and Prostate Disease
The relationship between alcohol consumption and prostate health remains a subject of significant debate. While moderate alcohol intake, particularly of red wine, has been linked to potential health benefits due to its polyphenol content (e.g., resveratrol), its role in prostate cancer risk is less clear (Arranz et al., 2012; Vartolomei et al., 2018). Resveratrol, found in red wine, has antioxidant and anti-inflammatory properties that may help protect against prostate cancer.
Excessive alcohol consumption has been associated with an increased risk of prostate cancer. A meta-analysis by Middleton et al. (2009) found that heavy drinking—defined as more than three to four drinks daily—was linked to a 20% higher risk of prostate cancer compared to abstinence.
Biological Mechanisms: The link between alcohol and prostate cancer may involve several biological pathways. Hormonal Changes: Alcohol can influence testosterone levels, a hormone closely associated with prostate health and cancer development.
Carcinogenic Effects of Acetaldehyde (ACH): Ethanol is metabolized by alcohol dehydrogenase (ADH) into ACH, a carcinogenic compound.
ACH forms adducts with proteins and DNA, leading to mutations. It also inhibits enzymes like O6-methylguanine transferase, impairing DNA repair mechanisms.
ACH promotes the production of reactive oxygen and nitrogen species, increasing oxidative stress and cellular damage.
Folate Metabolism and Immune Response: Chronic alcohol consumption disrupts folate metabolism and weakens immune responses, potentially creating an environment conducive to cancer.
Enzymatic Activity and Prostate Health: Differences in ethanol metabolism may further influence cancer risk. Research indicates that patients with prostate cancer or BPH exhibit higher serum ADH activity and lower serum ALDH activity compared to healthy individuals (Macke & Petrosyan, 2022). Reduced ALDH activity results in prolonged exposure to ACH, increasing carcinogenic risks. However, these enzymatic differences do not appear to distinguish between cancer and BPH, suggesting a shared metabolic alteration in these prostate conditions (Figure 1).
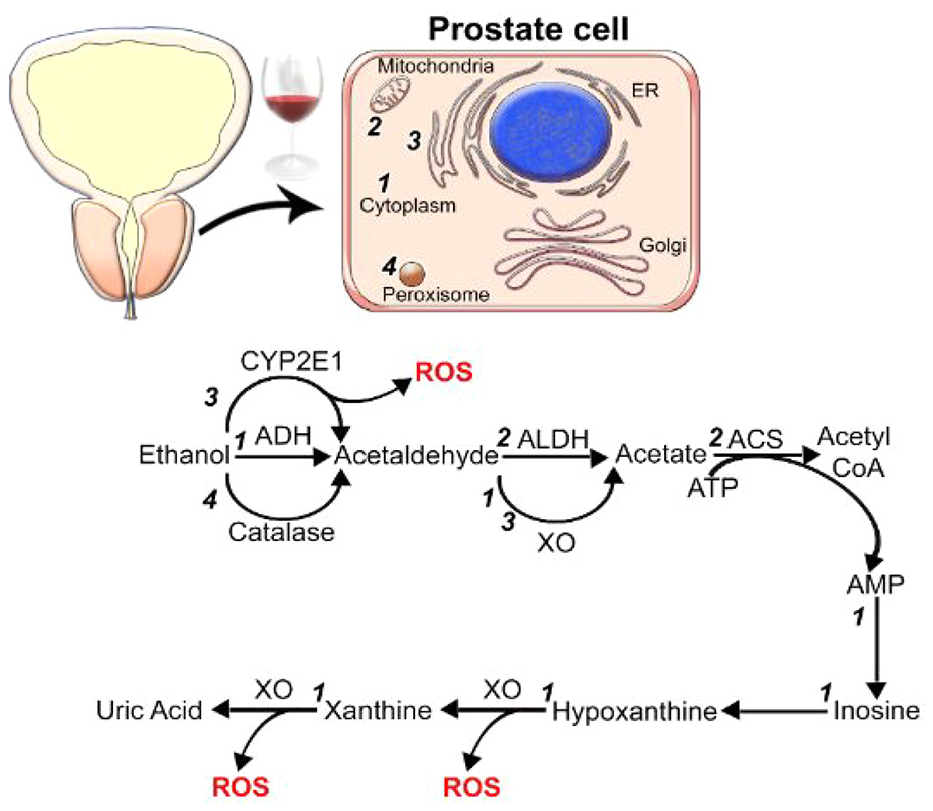
Alcohol Metabolism in Prostate Cells (Macke & Petrosyan, 2022).
Given the mixed evidence, current guidelines emphasize moderation in alcohol consumption as part of a healthy lifestyle to reduce the risk of prostate disease. The American Cancer Society recommends limiting alcohol intake to no more than two drinks per day for men, which may help mitigate the potential risks associated with alcohol while allowing individuals to enjoy the possible cardiovascular benefits of moderate consumption (Rock et al., 2020).
The Impact of Stress on Prostate Health and the Benefits of Stress-Reducing Practices
Stress and Prostate Disease
Chronic stress has emerged as a critical factor influencing the development and progression of various health conditions, including prostate disease. In prostate health, the effects of stress can be attributed to several mechanisms, such as hormonal imbalances, immune system suppression, and maladaptive behavioral responses.
Stress triggers elevated cortisol levels, and chronic cortisol elevation can suppress immune function and promote systemic inflammation, both of which are key contributors to cancer progression (Knezevic et al., 2023). Stress-induced neuroendocrine changes also play a significant role in prostate cancer. Studies by Zhang et al. (2020) and Kaarijärvi et al. (2021) demonstrated that stress activates signaling pathways, including those mediated by norepinephrine, which can enhance the expression of genes involved in tumor growth and metastasis. One such pathway includes the upregulation of vascular endothelial growth factor, a molecule that stimulates angiogenesis and supports tumor vascularization, facilitating cancer progression.
In addition to these physiological effects, chronic stress often leads to unhealthy coping behaviors, such as smoking, excessive alcohol consumption, poor dietary choices, and reduced physical activity. These behaviors further elevate the risk of prostate disease. For instance, Cao et al. (2021) found that individuals with high perceived stress levels were more likely to engage in habits that increase cancer risk, including smoking and sedentary lifestyles.
Managing chronic stress through targeted interventions, such as mindfulness practices, regular physical activity, and healthier lifestyle choices, is crucial not only for mitigating its physiological effects but also for reducing the behaviors that exacerbate prostate disease risk.
Benefits of Stress-Reducing Practices
Given the significant role stress plays in prostate health, incorporating stress management strategies is an essential aspect of comprehensive prevention and treatment plans for prostate diseases. Techniques such as mindfulness-based stress reduction (MBSR) and meditation have emerged as effective approaches for managing stress and enhancing overall well-being (Querstret et al., 2020).
MBSR, developed by Jon Kabat-Zinn, has demonstrated substantial benefits for cancer patients, including those with prostate cancer. According to Sheh (2021), MBSR programs notably reduced stress, anxiety, and depression in prostate cancer patients while improving sleep quality and immune system function. These outcomes indicate that MBSR not only eases the psychological challenges associated with prostate cancer but may also support improved clinical outcomes.
Integrating stress-reducing practices such as MBSR into daily routines offers a practical method for managing stress and promoting prostate health. When combined with other lifestyle interventions, such as maintaining a balanced diet and engaging in regular physical activity, these strategies contribute to a holistic approach to preventing and managing prostate diseases effectively.
The Role of Sleep Hygiene in Prostate Disease Prevention
Melatonin, a hormone primarily produced during sleep, is recognized for its anticancer properties, including its capacity to inhibit prostate cancer cell growth. Sleep disturbances, which reduce melatonin production, have been implicated in increasing cancer risk (Megerian et al., 2023). A study by Sartorelli et al. (2021) found that men with higher urinary melatonin levels had a reduced risk of advanced prostate cancer, emphasizing the protective role of maintaining healthy sleep patterns. Promoting good sleep hygiene—practices that foster regular and high-quality sleep—is a crucial strategy for mitigating prostate disease risk. Key sleep hygiene behaviors include maintaining a consistent sleep schedule, optimizing the sleep environment, and limiting stimulants such as caffeine and alcohol before bedtime.
Evidence from E. K. Wiggins et al. (2020) supports the connection between sleep quality and prostate cancer risk. While sleep quality did not influence overall or low-grade prostate cancer risk, poorer sleep was linked to an increased likelihood of developing high-grade prostate cancer. Men in the lowest sleep quality category had the highest odds, and those who struggled to fall asleep occasionally also exhibited higher risks. Interestingly, men who experienced daytime sleepiness showed lower odds of low-grade prostate cancer (OR: 0.65; 95% CI: 0.49–0.86). For managing sleep disturbances, cognitive-behavioral therapy for insomnia (CBT-I) has demonstrated effectiveness. CBT-I addresses behaviors and thought patterns that perpetuate insomnia, offering improved sleep quality and reduced cancer-related fatigue. Grassi et al. (2023) highlighted CBT-I as an effective intervention for cancer patients, while Savard et al. (2021) demonstrated its benefits in prostate cancer patients, reporting significant improvements in sleep quality alongside reduced anxiety and depression symptoms.
These findings collectively underline the importance of sleep hygiene and therapeutic interventions such as CBT-I in improving prostate health and mitigating cancer progression risks, particularly in the context of advanced disease.
Conclusion
Lifestyle modifications, including smoking cessation, alcohol moderation, stress management, and improved sleep hygiene, play critical roles in the prevention and management of prostate disease. Smoking cessation and reducing excessive alcohol intake can mitigate key risk factors for prostate cancer while stress-reducing practices such as mindfulness and meditation can help manage the psychological and physiological stressors associated with prostate disease. Furthermore, maintaining healthy sleep patterns through good sleep hygiene can support overall prostate health and reduce the risk of cancer progression. These lifestyle modifications, when integrated into a comprehensive approach to prostate disease management, offer significant potential for improving outcomes and enhancing the quality of life for individuals at risk of or living with prostate disease.
Alternative Therapies
Acupuncture
Acupuncture, a core component of Traditional Chinese Medicine, involves the insertion of thin needles into specific body points to harmonize energy flow (Qi) and manage symptoms. Within the realm of prostate diseases, acupuncture has been explored as a complementary therapy for alleviating symptoms such as urinary retention, pelvic pain, and quality-of-life impairments in conditions such as BPH and chronic prostatitis. A systematic review and meta-analysis by Lee et al. (2013) evaluated acupuncture’s efficacy in managing chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS). The analysis revealed that acupuncture significantly reduced pain and urinary symptoms in patients with moderate-to-severe CP/CPPS. Importantly, these benefits were sustained up to 24 weeks post-treatment, indicating acupuncture’s potential for long-term symptom relief.
These findings highlight acupuncture as a promising adjunctive therapy for managing complex symptoms of prostate conditions, particularly when conventional treatments yield limited results. Further large-scale, high-quality trials are warranted to validate these outcomes and understand the underlying mechanisms of their therapeutic effects. Compared to sham acupuncture or standard care, on a total of 20 sessions and over a period of 8 weeks (Sun et al., 2021). Another study by Qin et al. (2016) demonstrated that acupuncture could improve LUTS in patients with BPH, with minimal adverse effects. These findings suggest that acupuncture may be a valuable adjunctive therapy in managing prostate-related symptoms. Despite these promising results, it is essential to acknowledge the limitations of the current evidence. Many studies have small sample sizes, varying methodologies, and a lack of long-term follow-up. Therefore, while acupuncture shows potential, more robust clinical trials are needed to establish its efficacy in prostate disease care conclusively.
Herbal Medicine
Herbal medicine has been extensively utilized in both traditional and contemporary healthcare systems for managing prostate diseases, among other conditions. Numerous herbs have been explored for their efficacy in promoting prostate health, yielding mixed results depending on the herb and study context.
Saw Palmetto (Serenoa repens): One of the most researched herbs for prostate health, saw palmetto, is thought to inhibit the enzyme 5-alpha-reductase, which converts testosterone into dihydrotestosterone (DHT), a hormone implicated in prostate enlargement (Paulis et al., 2021). While a systematic review by Nickel et al. (2022) found no significant improvement in LUTS associated with BPH compared to placebo, other research presents contrasting results. Kimura et al. (2024) reported that saw palmetto improved urinary symptoms and overall quality of life, highlighting the need for further studies to reconcile these discrepancies.
African Plum Tree (Pygeum africanum): P. africanum has been investigated for its anti-inflammatory and antioxidant properties. Extracts from the bark of this tree are believed to reduce LUTS and improve bladder function by modulating inflammatory pathways and relaxing smooth muscles in the urinary tract. Studies suggest modest efficacy, but variability in outcomes indicates the need for standardized preparations and dosage in clinical research.
Stinging Nettle (Urtica dioica): Stinging nettle has shown potential benefits in alleviating BPH symptoms, primarily through its anti-inflammatory effects and ability to inhibit sex hormone-binding globulin (SHBG). By reducing SHBG activity, nettle may indirectly decrease the availability of active DHT in prostate tissues. Preliminary studies suggest improvement in urinary symptoms; however, large-scale trials are still needed to confirm its therapeutic value.
Pumpkin Seed (Cucurbita pepo): Pumpkin seeds are rich in phytosterols, compounds that may inhibit DHT formation and have mild anti-inflammatory effects. Studies have reported that pumpkin seed extract can reduce the severity of LUTS and improve bladder function in men with BPH. Its affordability and safety profile make it a promising candidate for long-term use, though additional research is required to validate these findings (Antoniou et al., 2023; Leisegang et al., 2022; Stewart, 2022). A review by Chughtai et al. (2023) found that these herbs could provide modest symptom relief and improve urinary flow in patients with BPH. However, the quality of evidence remains low, with most studies being small, short-term, and not placebo-controlled.
Other Complementary Therapies
In addition to acupuncture and herbal medicine, other complementary therapies have been explored for their potential role in prostate disease care. These therapies include dietary supplements, mind-body practices, and energy-based therapies.
Dietary Supplements: The use of dietary supplements has become prevalent among prostate disease patients seeking to enhance their health and potentially reduce disease progression. Lycopene, a powerful antioxidant predominantly found in tomatoes, has been extensively studied for its potential in lowering prostate cancer risk. A meta-analysis by Rowles et al. (2020) concluded that higher dietary lycopene intake is associated with a reduced prostate cancer risk, though the observed effect size was modest. Lycopene’s ability to neutralize oxidative stress and influence mechanisms related to cancer progression supports its role as a potentially beneficial supplement.
In contrast, selenium and vitamin E, once widely believed to provide protective effects against prostate cancer, have not demonstrated efficacy in large-scale clinical trials. The Selenium and Vitamin E Cancer Prevention Trial (SELECT) revealed no significant benefit of these supplements in reducing prostate cancer risk, suggesting that their routine use for this purpose may be unwarranted (Yang et al., 2020).
Mind-Body Practices: Mind-body practices such as meditation, yoga, and tai chi are increasingly recognized for their holistic benefits in managing prostate diseases. These practices focus on reducing stress and improving emotional well-being, both of which are critical for patients dealing with chronic conditions such as prostate cancer and prostatitis.
MBSR programs, which incorporate meditation and gentle physical movements, have shown promise. Victorson et al. (2023) found that MBSR significantly improved quality of life and reduced psychological distress in prostate cancer survivors under active surveillance. Stress management is especially important in conditions such as chronic prostatitis, where exacerbations are often linked to heightened stress levels.
Yoga and tai chi, which combine physical activity with mindful awareness, may also benefit prostate disease patients by reducing anxiety, improving flexibility, and enhancing overall physical function. These practices, coupled with traditional medical therapies, offer a complementary approach to managing both the physical and psychological challenges associated with prostate diseases.
Holistic Approaches: Integration with Conventional Treatments
The integration of complementary and alternative therapies (CAM) with conventional treatments presents both opportunities and challenges. A holistic approach to prostate disease care involves combining evidence-based CAM therapies with standard medical treatments to address the physical, emotional, and psychological aspects of the disease (Demetriou et al., 2024). For instance, acupuncture may be used alongside pharmaceuticals to alleviate symptoms such as pelvic pain and urinary retention, reducing the need for higher doses of medication and minimizing side effects. Similarly, herbal supplements such as saw palmetto and stinging nettle may be recommended in conjunction with alpha-blockers or 5-alpha-reductase inhibitors to enhance symptom relief in BPH patients (Enitan et al., 2023).
Another strategy involves incorporating CAM therapies into survivorship care plans for prostate cancer patients. Survivorship care often focuses on managing the long-term effects of cancer treatment, such as fatigue, sexual dysfunction, and psychological distress. Mind-body practices such as yoga and meditation can play a significant role in improving quality of life and addressing these issues, as demonstrated by various studies (Emery et al., 2022).
Benefits of a Comprehensive Care Plan
A comprehensive care plan that integrates CAM therapies with conventional treatments offers several potential benefits for prostate disease patients, some of which include:
It allows for a more personalized approach to care, considering the patient’s preferences, values, and cultural beliefs. This patient-centered approach can lead to increased satisfaction and adherence to treatment plans.
The integration of CAM therapies may help reduce the side effects of conventional treatments. For example, acupuncture and herbal medicine may alleviate the adverse effects of hormone therapy in prostate cancer patients, such as hot flashes and fatigue. By addressing these side effects, patients may experience an improved quality of life and be more likely to continue with their prescribed treatments.
A holistic approach promotes overall wellness by addressing not only the physical symptoms of prostate disease but also the emotional and psychological aspects. This approach aligns with the principles of integrative medicine, which emphasizes the importance of treating the whole person rather than just the disease.
Patient Perspectives: Personalized Medicine and Alternative Therapies
Understanding Patient Preferences
Patient perspectives play a crucial role in the successful integration of CAM therapies into prostate disease care. Understanding patient preferences involves exploring their beliefs, values, and expectations regarding CAM therapies and conventional treatments. A survey by Clarke et al. (2015) found that a significant proportion of prostate cancer patients expressed interest in using CAM therapies, with many perceiving them as natural and safer alternatives to conventional treatments. However, patients also reported a lack of reliable information and guidance from healthcare providers regarding CAM use. This highlights the need for better communication between patients and providers to ensure that CAM therapies are used safely and effectively (Jurisevic, 2020).
Another aspect of understanding patient preferences is recognizing cultural differences in CAM use. For example, traditional herbal medicine may be more prevalent among patients from Asian or African backgrounds, while mind-body practices such as yoga and meditation may be preferred by Western patients. Healthcare providers should be aware of these cultural differences and respect patients’ choices while providing evidence-based guidance (Khosla et al., 2024).
Challenges and Future Directions in Integrative Prostate Disease Management
Challenges
Evidence-Based Integration
Lack of High-Quality Research: One of the primary challenges in integrative prostate disease management is the paucity of rigorous clinical trials and longitudinal studies (Heidenreich et al., 2014). While there is anecdotal evidence and preliminary studies suggesting the benefits of nutrition, exercise, and lifestyle modifications, there is a critical need for more robust, large-scale studies to establish their efficacy unequivocally (Nuhn et al., 2019).
Standardization Issues: The heterogeneity of integrative approaches presents a significant hurdle. Dietary recommendations, exercise programs, and lifestyle modifications can vary widely, leading to inconsistent outcomes (Abrams, 2018). Developing standardized guidelines that are universally accepted remains a daunting task.
Patient Compliance and Lifestyle Changes
Adherence to Regimens: Encouraging patients to adhere to comprehensive lifestyle changes can be challenging. Many patients find it difficult to maintain strict dietary habits, regular exercise routines, and other lifestyle modifications over the long term. This noncompliance can significantly affect the success of integrative management strategies (Calvo-Schimmel et al., 2021; Focht et al., 2018).
Behavioral and Psychological Barriers: Psychological factors such as motivation, mental health issues, and lack of support can impede patients’ ability to make and sustain necessary lifestyle changes. Addressing these barriers requires a multifaceted approach that includes behavioral therapy and patient education (Bourke et al., 2014; Spring et al., 2019).
Healthcare Provider Knowledge and Training
Limited Training in Integrative Approaches: Many healthcare providers lack formal training in integrative medicine. This gap in knowledge can lead to reluctance or inability to recommend and support integrative strategies effectively. Continuous education and training programs for healthcare professionals are essential to bridge this gap (Bauer et al., 2020; Steinhorn et al., 2017).
Interdisciplinary Collaboration: Effective integrative management often requires collaboration among various healthcare professionals, including nutritionists, physical therapists, psychologists, and primary care physicians. Ensuring seamless communication and coordination among these professionals can be challenging but is crucial for comprehensive care (Jani et al., 2015; D. S. Riley et al., 2016).
Healthcare System Barriers
Insurance and Cost Issues: Integrative approaches often involve interventions that are not fully covered by insurance plans, leading to high out-of-pocket costs for patients. This financial barrier can limit access to comprehensive integrative care for many patients (Khalil et al., 2018; Leach & Veziari, 2022).
Systemic Inertia: The traditional healthcare system is often slow to adopt new approaches, especially those outside conventional medical practices. Integrating nutrition, exercise, and lifestyle modifications into standard prostate disease management protocols requires systemic changes that can be met with resistance (Templeman & Robinson, 2011; Veziari et al., 2017).
Future Directions
Advancing Research and Evidence
Large-Scale Clinical Trials: There is a pressing need for more large-scale, randomized controlled trials to evaluate the effectiveness of integrative approaches in prostate disease management. Future research should focus on identifying the most beneficial dietary patterns, exercise regimens, and lifestyle modifications (Tree & Dearnaley, 2018).
Longitudinal Studies: Long-term studies are crucial to understanding the sustained effects of integrative strategies on prostate health and disease progression. These studies can provide insights into the long-term benefits and potential risks associated with various integrative approaches (Calvo-Schimmel et al., 2021).
Personalized Medicine
Tailored Interventions: Future integrative prostate disease management should move toward personalized medicine, where interventions are tailored to the individual’s genetic, environmental, and lifestyle factors. Advances in genomics and biomarker research can facilitate this personalized approach (Ramnarine et al., 2019).
Technological Integration: The use of technology, such as wearable devices and mobile health applications, can help monitor patients’ adherence to lifestyle modifications and provide real-time feedback. These tools can enhance patient engagement and adherence to integrative management plans (Sorrentino & Di Carlo, 2023).
Enhanced Patient Education and Support
Educational Programs: Developing comprehensive educational programs to inform patients about the benefits of integrative approaches and how to implement them effectively is crucial. These programs should be accessible and designed to empower patients to take an active role in their health management (Lessa & Alves, 2024).
Support Systems: Establishing robust support systems, including peer support groups and counseling services, can help patients overcome psychological and behavioral barriers to lifestyle changes. Integrating these support systems into standard care can improve adherence and outcomes (Crawford-Williams et al., 2018).
Healthcare Provider Training and Collaboration
Interdisciplinary Training: Implementing training programs that emphasize interdisciplinary collaboration and integrative medicine principles can equip healthcare providers with the necessary skills to support and implement integrative strategies effectively (Bauer et al., 2020).
Collaborative Care Models: Promoting collaborative care models that bring together various healthcare professionals can ensure a holistic approach to prostate disease management. These models can facilitate better coordination and communication among providers, leading to improved patient outcomes (Jani et al., 2015).
Policy and Systemic Changes
Insurance Reforms: Advocating for policy changes that increase insurance coverage for integrative approaches can reduce financial barriers and increase access to comprehensive care (Leach & Veziari, 2022).
Systemic Integration: Encouraging the integration of integrative medicine into standard healthcare protocols can help overcome systemic inertia. This can be achieved through policy advocacy, professional guidelines, and the promotion of best practices (Veziari et al., 2017).
Footnotes
Consent for Publication
All the listed authors have agreed for this article to be published in this journal.
Author Contributions
All the listed authors have contriuted in writing this review as follows: Patrick Maduabuchi Aja: Conception, analysis, methodology, supervision. Peter Chinedu Agu: Conception, writing original draft, analysis, software. Angela Mumbua Musyoka: Conception, methodology, resources, writing original draft. Wisdom Ngwueche: conception, writing origina draft, resources, review and editing. Joseph Uche Odo: conception, methodology, investigation, writing original draft. Esther Ugo Alum: conception, writing original draft, resources, investigation. Ilemobayo Victor Fasogbon: conception methodology, review and editing, software. Mbyemeire Herbert: methodology, writing original draft, resources. Ejike Daniel Eze: Conception, writing original draft, supervision, resources.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
Data will be provided upon request from the authors.
