Abstract
Low testosterone levels in men contribute to altered sexual health, including low libido, erectile dysfunction, impaired sleep, and changes in mood and energy. Nearly half of all infertility cases are implicated by male factors, such as low testosterone levels and altered semen and sperm health. The purpose of this case series is to share the experience of two men taking a concentrated, highly bioavailable gelatinized form of specific phenotypes (sometimes referred to as colors) of Lepidium peruvianum (Maca-OG™) to improve reproductive health. One man experienced an increase in total testosterone levels and fertility parameters, including sperm concentration, sperm motility, and total sperm count. The second experienced an increase in total testosterone levels, energy, mood, and sleep. This case series highlights a natural alternative for male health to support the body’s production of testosterone, especially when hormone therapy is not medically indicated or desired by the patient, or there are concerns about hormone therapy reducing the body’s production of testosterone.
Introduction
Infertility and low testosterone production are two health concerns that can impact multiple aspects of a man’s life.
Infertility is defined as the inability to conceive after 1 year of unprotected, frequent intercourse. Factors contributing to infertility are numerous, impacting males and females. However, male factors are reported to contribute to 50% of all infertility cases (Leslie et al., 2024). Male infertility can be a result of primary testicular defects, such as low sperm production, abnormal sperm function or transport, endocrine dysfunction (including low testosterone levels and hypogonadism), and sexual dysfunction, though it is not limited to these parameters (Leslie et al., 2024; Martins da Silva & Anderson, 2022).
Testosterone levels in men decline gradually, at a rate of about 1% to 2% annually starting at the age of 30 (Martins da Silva & Anderson, 2022). Low and low-normal testosterone levels are known to contribute to decreased libido and erectile dysfunction, potentially impacting fertility and other aspects of sexual health. Furthermore, low testosterone has been implicated in mood disturbances and low energy (Zitzmann, 2020). Testosterone therapy is not suitable for all men, especially for those wishing to maintain their fertility (Martins da Silva & Anderson, 2022).
While conventional medicine is often utilized for fertility and low testosterone levels, it is reported that 9% to 70% of men worldwide utilize complementary and alternative medicine (CAM), which includes acupuncture, nutrition, and herbal medicine or supplements. Despite this, a scoping review found the evidence is limited for the effectiveness of these therapies (Fasanghari et al., 2024).
Lepidium peruvianum, commonly known as maca, is native to Peru. This cruciferous root vegetable was first described in the 1500s as a dietary staple and has gained attention in modern times as a popular dietary supplement (Gonzales, 2012). Although maca has been used historically in Peruvian culture, significant publications on its health benefits did not emerge until the early 2000s. Since then, numerous studies have reported the benefits of maca to men’s health, including increased energy levels, improvements in moods and cognition, increased sperm quality and reproductive outcomes, and improvements in sexual function and prostate health (Minich et al., 2024). Researchers have identified between 13 and 17 phenotypes (colors) of maca, though four colors are predominant: black, red, yellow, and purple. The colors of maca vary in their phytochemical and nutrient composition (Chen et al., 2018; Meissner et al., 2017; Zhou et al., 2017) and the physiological benefits it can provide (Minich et al., 2024). For example, black maca shows the most impact on sperm production, while yellow and red maca show moderate or no effect, respectively (Gonzales et al., 2009; Melnikovova et al., 2015, 2021).
This case series aims to contribute to the scientific literature by sharing the experience of two men using the concentrated specific phenotypes of Lepidium peruvianum (Maca-OG™), which resulted in increased testosterone levels and fertility parameters. These positive outcomes have not been previously reported in the scientific literature. After six non-consecutive, cumulative months of use, one patient experienced improvements in sperm concentration, sperm motility, total sperm count, and testosterone levels. The other patient experienced improvements in testosterone levels, energy, sleep, and mood after 3 months of use. The case report was written following the CARE guidelines (Riley et al., 2017).
CASE #1
Case Presentation: September 21, 2022
A 38-year-old Indian male presented for a fertility consultation after trying to conceive for one and a half years unsuccessfully. At the start of care, he weighed 185 pounds with a height of 5’10” and a BMI of 26.5.
The patient presented with a medical history of metabolic dysfunction-associated steatotic liver disease (MASLD), commonly called fatty liver, as medically diagnosed by his primary physician. In 2020, he tested positive for Helicobacter pylori. He was not taking any supplements or medication to address these health issues; rather, he was attempting to manage these concerns through diet and exercise. His primary reason for seeking care was to address male fertility, sperm health, and low libido. Secondary reasons included abdominal discomfort and symptoms of high stress, including overthinking, worry, and anxiousness.
At the time of the initial consultation, the patient reported following a vegetarian Indian diet, engaging in walking, yoga, and high-intensity interval training (HIIT) for 30 minutes daily, and sleeping 8 hours nightly. He works 40 hours a week, remaining mostly sedentary during that time. The patient expressed his desire to have a child as the driving force to seek care.
The patient was assessed using health questionnaires, physical exam, pulse and tongue evaluation, and previous bloodwork and semen analysis. Laboratory results completed in March 2022 (by a previous provider) confirmed low testosterone and low sperm motility. A repeat semen analysis was ordered by the treating clinician in August 2022 in preparation for the initial consultation. During that consultation, it was revealed that the abdominal discomfort felt by the patient was described as gastroesophageal reflux, bloating, and abdominal pain. Gastroesophageal reflux occurred after his largest meal of the day, followed by bloating. He experienced abdominal pain one to two times per week and was not aware of a particular cause of this pain.
The initial comprehensive consultation and subsequent consultations, which took place across 6 months, adhered to an acupuncture model of care that consists of assessment, interpretation, intervention, and monitoring. All consultations were completed in person.
Additional labs, imaging, and exams were requested. The patient was referred to a local urologist for an ultrasound of the testes. The clinician provided a clinical assessment that included gastrointestinal dysbiosis and adrenal dysfunction.
Recommendations were provided, as detailed in the Case Timeline and Recommendations (Table 1). This included weekly acupuncture visits to address stress and digestive concerns, a vegetarian, paleo-style food plan, continuing with regular activity and supplements, and applying ice to the testes once per day for 15 minutes. New supplement recommendations included Maca-OG™ (1500 mg twice daily) for sperm health and low testosterone levels, two supplements for digestive support, vitamin D (based on lab values), and a multivitamin focused on men’s health. Upon receiving these recommendations, the patient expressed excitement and high confidence in his ability to implement them.
Case #1 Timeline and Recommendations

Follow-Up Consultation #1: October 18, 2022
The patient returned to assess progress and review his labs and ultrasound results. The ultrasound of the testes was normal, with no blockages or abnormalities, and testosterone levels remained low-normal (435 ng/dL; Table 2). The patient received five acupuncture treatments by this time, resulting in a greater sense of calm throughout the day and some improvement in GI-related symptoms. However, the clinician discussed performing a stool test (GI Map) to investigate the patient’s digestive concerns, which the patient agreed to complete, and the clinician reiterated the original recommendations without any modifications (Table 1).
Case #1-Diagnostic Testing and Biomarkers

Note. FSH = follicle-stimulating hormone; LH = luteinizing hormone; mIU/mL = milli-international units per milliliter; ng/mL = nanograms per milliliter; pg/mL = picograms per milliliter; uIU/mL = micro-international units per milliliter.
Ordered by a previous provider. b Time of draw: 9:00 am.
Follow-Up Consultation #2: November 16, 2022
The patient returned approximately 1 month later to review the results from the stool test, which not only showed the presence of H. pylori and two non-commensal bacteria but also clinically low secretory IgA (Table 2).
Modifications were made to the patient’s recommendations to address these findings. This included a temporary pause to the initial supplements recommended in September 2022 and the beginning of an anti-microbial dietary supplement protocol, which the patient would follow for 2 months (Table 1 and Supplemental Material). After this time, the clinician would complete a reassessment to determine the next steps of care.
Follow-Up Consultation #3: February 8, 2023
A follow-up consultation was conducted at the conclusion of the 2-month anti-microbial protocol. The patient subjectively reported that he no longer experienced gastroesophageal reflux, bloating, or abdominal pain. He also reported a 10-pound weight reduction. At this time, the patient had received 15 acupuncture treatments to aid in stress management and digestive concerns.
After completing the anti-microbial protocol, the patient could start treatment for the primary reason that he sought care: to optimize fertility. Therefore, at this consultation, the patient was advised to resume the initial supplement protocol that included Maca-OG™ for men’s reproductive health (Table 1). The provider also ordered labs to be completed after a minimum of 12 weeks of use of Maca-OG™ (Table 2).
Follow-Up Consultation #4: June 30, 2023
The patient returned to discuss the results of the latest labs and semen analysis. Positive outcomes in all parameters included improvements in total testosterone levels, sperm concentration, the number of total motile sperm, sperm motility, and sperm morphology (Table 2).
Results
A 38-year-old man experienced an improvement in multiple fertility parameters using Maca-OG™ as the primary treatment option. This included improvements in total testosterone levels, sperm concentration, the number of total motile sperm, sperm motility, sperm morphology (Table 2), and increased libido. The care plan targeted toward these parameters was initiated and followed for approximately 2 months before a 2-month cessation due to the finding and treatment of gastrointestinal dysbiosis. Treatment for fertility parameters was resumed and continued for approximately 4 months, as detailed in the writing of this case report.
The patient and his wife were waiting for these results before they decided to move forward with in-vitro fertilization (IVF). The couple chose IVF as a fertility treatment due to the wife’s reproductive history and the years the couple had spent attempting to conceive naturally. The patient continued to receive acupuncture twice per month, as well as maintained his supplement regimen throughout the IVF process.
In addition to the improvement in fertility parameters, the patient no longer experienced gastroesophageal reflux, bloating, or intestinal pain after completing a targeted anti-microbial protocol and regular acupuncture sessions. Further, his anxiety was well-managed with regular acupuncture sessions.
CASE #2
Case Presentation: December 22, 2023
A 44-year-old Caucasian male presented for a consultation to address concerns of persistent, medication-resistant depression with some irritability.
The patient has a medical history that includes a diagnosis in 2021 of major depressive disorder and chronic low back pain. Previous surgeries include a tonsillectomy in 1997 and a left ankle tendon repair in 2012. His family history is positive for major depressive disorder, generalized anxiety disorder, renal cancer, and rheumatoid arthritis. His parents are elderly but living and apparently healthy. No genetic or genomic information was available for this patient.
To address his diagnosis of depression, the patient was prescribed 10 mg daily of escitalopram by his primary care nurse practitioner but reported unwanted effects. The dose was reduced to 5 mg daily and was well tolerated. The man has no personal history of hospitalization or institutional enrollment for psychiatric care and denies active or passive suicidal or homicidal ideations.
Before taking escitalopram, the patient had experimented with dietary supplements, including oral lavender (Silexan 160 mg daily), 5-HTP, saffron (30 mg daily), magnesium (400–500 mg daily), and kava (750 mg in a beverage as needed) with no appreciable changes. The patient has previously worked with counselors on three occasions, but adherence was minimal due to difficulty in scheduling.
At the time of the initial consultation, the patient reported an inability to gain muscle mass despite consuming approximately 150 g of dietary protein daily and engaging in strength training 3 to 4 days per week for several years. He also practices yoga 4 to 5 days per week at home. He consumes approximately 1,800 calories, two cups of coffee daily, and two to three alcoholic beverages per week.
The patient reported taking several supplements, including creatine, a multivitamin, vitamins D and C, trimethylglycine, magnesium, and an adaptogenic combination formula (Table 3). He also reported receiving adequate sleep, including feeling well-rested upon waking, though he disclosed feeling moderate fatigue most afternoons and indicated that he “would nap if he could” most days. Sleep biometrics are monitored using an Oura Ring that he had purchased previously to monitor health metrics (Table 4).
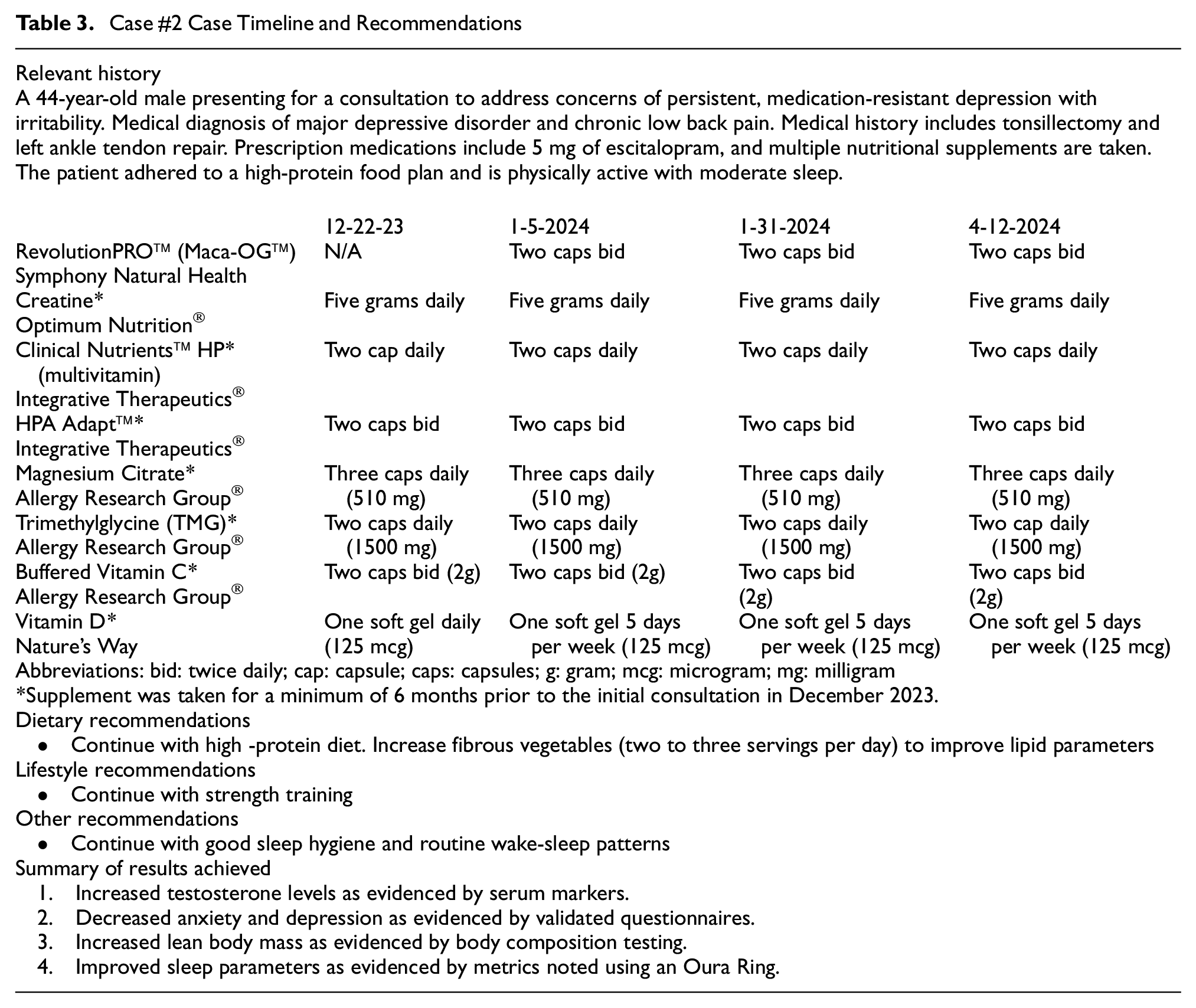
Case #2 Case Timeline and Recommendations
Case #2-Physical and Emotional Assessments

Note. BMI = Body mass index; GAD-7 = General anxiety disorder-7; PHQ-9 = Patient health questionnaire-9.
The patient reported he experienced weight fluctuations in the past 20 years up to 186 lbs. and as low as 154 lbs. b The patient utilized an Oura Ring. c Based on 90-day average. d Based on 30-day average.
The patient works in an administrative role and is married with one child. He reported high levels of occupational stress, but he stated that he feels well-supported by family and friends. He noted that he had trouble focusing and concentrating when under stress. No major life event stressors have occurred in the past 2 years.
A physical examination was conducted with no abnormal findings. The clinician noted bilateral loss of body hair in the lower extremities mid-tibial distally, and he had relatively fine arm hair yet coarse chest hair and no significant back hair. No scalp hair loss was observed, and there was some evidence of his ability to grow facial hair, although he was clean-shaven.
As part of the emotional assessment, validated questionnaires were completed, including Generalized Anxiety Disorder-7 (GAD-7) and Patient Health Questionnaire-9 (PHQ-9), with the results suggesting moderate anxiety and depression (Table 4).
Anthropometric measurements were conducted as detailed in Table 4.
The treating clinician ordered laboratory testing, which would be utilized with the assessments to provide recommendations for care.
Follow-Up Consultation #1: January 5, 2024
A follow-up consultation was conducted to review laboratory results and clinical recommendations for care.
Based on the patient’s symptoms, laboratory results (Table 5), and clinical assessment, the clinician provided recommendations as detailed in the Case Timeline and Recommendations (Table 3). The recommendations focused on improving testosterone levels from low-normal to more optimal levels. The patient was not a candidate for testosterone replacement therapy based on current prescribing guidelines. Therefore, the patient was instructed to begin using Maca-OG™ (1500 mg twice daily), and to continue taking his current supplements, but to reduce his vitamin D intake to 5 days per week rather than seven due to his high-normal levels. A minor modification in his diet included increasing fibrous vegetables and consuming two to three servings of vegetables per day to help improve lipid parameters.
Case #2 Diagnostic Testing and Biomarkers

Note. CMP and CBC were within normal limits unless otherwise noted. Abbreviations: eGFR = estimated glomerular filtration rate; H-high = HDL, high-density lipoprotein; HS CRP = high sensitivity C-reactive protein; LDL = low-density lipoprotein; LH = luteinizing hormone; mcmol/L = micromoles per liter; mg/dL = milligrams per deciliter; mg/L = milligrams per liter; mIU/mL = milli-international units per milliliter; mL/min = milliliters per minute; N/A = not applicable; ng/mL = nanograms per milliliter; nmol/L = nanomoles per liter; pg/mL = picograms per milliliter; SHBG = sex hormone binding globulin; TSH = thyroid stimulating hormone; uIU/mL = micro-international units per milliliter.
Time of draw: 8:08 am. b Time of draw: 7:27 am.
Follow-Up Consultation #2: January 31, 2024
A follow-up consultation was completed to ensure adherence to the recommendations and monitor progress. This visit was conducted via video conferencing.
The patient reported excellent compliance with the supplements, “never missing a dose” since the last visit. He subjectively reported better daytime energy, feeling leaner and stronger, and that his mood mildly improved, with reduced episodes and severity or irritability. He admits to not regularly consuming the recommended vegetable intake but that he “is trying.”
The clinician reiterated the original recommendations without any modifications (Table 3).
Follow-Up Consultation #3: April 12, 2024
The patient presented for a follow-up to discuss the results of recent laboratory markers and assess his progress on mood, energy, and focus. He reports adhering to the recommendations (Table 3) and has not knowingly changed his diet or exercise routine.
The patient subjectively reported his energy as “solid with very little interest or need for napping in the afternoon.” He also reports completing a strength-training workout without feeling exhausted.
At this time, improvements included enhanced sleep parameters, increased lean body mass (+8.6 lbs.), decreased anxiety and depression (Table 4), and a significant improvement in total testosterone from 469 to 616.6 mg/dL and free testosterone from 45.7 to 164 pg/mL (Table 5). In addition, a reduction in inflammation was observed as measured by hs-CRP (Table 5).
In consultation with the patient, continuation of Maca-OGTM was agreed to at 750 mg twice daily with potential re-evaluation in 12 months.
Results
After 12 weeks of using Maca-OG™, the patient experienced a substantial increase in total and free testosterone (31.5% and 259.9%, respectively), increased lean body mass, improved sleep, decreased generalized inflammation, improved energy, and decreased anxiety and depression.
Discussion
Preclinical and clinical studies report on the benefits of maca, including increased energy levels, improvements in moods and cognition, increased sperm quality and reproductive outcomes, and improvements in sexual function and prostate health (Minich et al., 2024). However, most studies are animal-based, with only 14 of 30 clinical trials exclusively having studied parameters of men’s health, despite maca’s popularity as a dietary supplement.
Maca-OG™, commercially known as Revolution Macalibrium® and RevolutionPRO, is a proprietary concentrated formulation of Lepidium peruvianum that was the primary treatment for both men in this case series. At the writing of this case series, published data specific to Maca-OG™ is unavailable. However, the clinicians have utilized this supplement in clinical practice alongside therapeutic lifestyle change programs for over 10 years, with noted success in addressing male fertility and testosterone-related health concerns. The exact mechanism of action of Lepidium peruvianum is not fully understood, but it is believed to work through the hypothalamus-pituitary-adrenal-gonad (HPAG) axis, with the plant sterols, glucosinolates, and alkaloids contributing to its effects (Meissner et al., 2017; Minich et al., 2024; Ross, 2021).
Research from the 1960s suggests that a unique and identifying feature of Lepidium peruvianum (compared to Lepidium meyenii) is its ability to extend beyond the HPA axis into the HPAG axis based on its impact on the testes and ovaries (Minich et al., 2024)
Of importance, research has shown that there are up to 17 different phenotypes (or colors) of maca. The colors (predominately red, black, yellow, purple, gray, and white) vary in their DNA and active ingredient profiles and elicit different physiological responses in the body (Geng et al., 2020; Meissner et al., 2015, 2017; Minich et al., 2024). Red maca has been shown to reduce prostate hyperplasia in men (Minich et al., 2024). Black and yellow maca are known for their energy and fertility-enhancing properties, including their impact on sperm health and libido (Abdulzahra et al., 2024; Alcalde & Rabasa, 2020; Melnikovova et al., 2021; Minich et al., 2024), whereas a concentrated proprietary combination of maca phenotypes for women (Maca-GO®) demonstrated a positive impact on hormone balancing in peri- and postmenopausal women (Minich et al., 2024).
Aside from the favorable patient outcomes, additional strengths were revealed by the cases. First, the clinicians did not introduce significant dietary or lifestyle recommendations that may have accounted for the positive outcomes. Second, the timing of the blood draw for testosterone was appropriate; morning timing of testosterone assessment is important because testosterone levels exhibit a diurnal variation, peaking in the early morning and providing the most accurate measurement of baseline levels. Third, the 38-year-old male (Case #1) was treated separately for his stress and dysbiosis, utilizing therapies that are not known to impact sperm parameters or hormone levels. Fourth, the treatment of the 44-year-old male (Case #2) introduced only one new therapeutic intervention, allowing for a stronger association to be made regarding the impact of Maca-OG™ on testosterone levels. In addition, validated questionnaires were used to assess this patient’s mood.
Limitations
The clinicians acknowledge the limitations of this case series. First, a multi-modal approach to clinical care does not allow for a definitive conclusion regarding the effectiveness of any one therapy. This is especially reflective of the patient presented in Case #1. Second, the authors recognize that the outcomes of two individuals (N = 2) cannot be translated into a larger population and the outcomes should be interpreted accordingly. Therefore, the authors believe that further research of Maca-OG™ as a solitary treatment option for male fertility and its impact on testosterone levels should be explored by researchers. At the time of submission, the authors are unaware of studies demonstrating the successful use of this specific maca formulation on testosterone levels and sperm parameters.
Conclusion
Case reports are an excellent way for healthcare providers to share successes and provide opportunities for learning based on clinical experience rather than clinical trials (Kligler, 2021). This case series (N = 2) demonstrated the safe and effective use of Maca-OG™ to support sperm health, healthy testosterone levels, and male fertility in as little as 3 months.
Though a cause-and-effect relationship cannot be concluded, this case series demonstrates how Maca-OG™ enhanced male reproductive health and testosterone levels for two men. This finding may provide a foundation for other clinicians to consider this therapy in their practice or for researchers to explore the hormone and fertility-enhancing benefits of Maca-OG™.
Supplemental Material
sj-docx-1-jmh-10.1177_15579883241304570 – Supplemental material for Optimizing Testosterone Levels and Fertility Outcomes
Supplemental material, sj-docx-1-jmh-10.1177_15579883241304570 for Optimizing Testosterone Levels and Fertility Outcomes by Kim Ross, Corey Schuler and Marc Sklar in American Journal of Men's Health
Footnotes
Acknowledgements
The author would like to acknowledge the patients who graciously consented to share their information.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: CBS had a previous consultant relationship with and holds shares in Symphony Natural Health Inc., and MS and KR are independent contractors of Symphony Natural Health Inc., manufacturer of the maca supplement referred to as Maca-OG™ and commercially known as Revolution Macalibrium® and RevolutionPRO™.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was made available for open access due to the financial support of Symphony Natural Health Inc., manufacturer of the maca supplement referred to as Maca-OG™ and commercially known as Revolution Macalibrium® and RevolutionPRO™.
Ethical Approval
The institution does not require ethical approval for reporting individual cases or case series.
Informed Consent
The patients presented in this case series provided written informed consent to publish patient information in the present manuscript. The patients also received a copy of the manuscript to read and review.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
