Abstract
Alcohol misuse is a significant health concern among gay, bisexual, same-gender-loving, and other men who have sex with men (MSM). Yet, little is known about the severity and predictors of alcohol misuse among self-reported young Black MSM. This study aimed to identify patterns of and factors associated with alcohol misuse in a sample of young Black MSM living in New York City. Baseline data from a randomized controlled trial aimed at improving the uptake of HIV testing among 250 MSM aged 18 to 29 were analyzed. Log-binominal regression analyses were conducted to assess the association of demographic and psychosocial factors with alcohol misuse in the past year and past 3 months among young Black MSM. Overall, 33.2% and 28.0% of young Black MSM in the study experienced alcohol misuse in the past year and past 3 months, respectively. In the adjusted model, factors positively associated with past-year alcohol misuse included marijuana use, a history of drug use, and having one-two or more than two male sex partners. Likewise, participants who used marijuana and those with one-two or more than two male partners were more likely to report past 3-month alcohol misuse. No significant association was found between positive screening for depressive symptoms, chemsex, internalized homophobia, and the likelihood of having alcohol misuse. The high prevalence of alcohol misuse underscores the importance of raising awareness of alcohol misuse and designing alcohol risk reduction programs that jointly address HIV risk among young Black MSM.
Keywords
Introduction
Alcohol misuse is defined as the consumption of alcohol that poses a heightened risk of adverse health and social consequences; however, not all instances of alcohol misuse necessarily require alcohol disorder treatment (National Institute on Alcohol Abuse and Alcoholism, 2020). Alcohol misuse, which encompasses hazardous drinking and binge drinking, is notably prevalent among gay, bisexual, same-gender-loving, and other men who have sex with men (MSM) in the United States, with approximately 1.5 times higher rate of past-month binge drinking compared with the general population (31.1% vs. 21.5%, respectively; Substance Abuse and Mental Health Services Administration, 2023). Despite being disproportionately impacted by HIV, research on alcohol misuse among Black MSM remains limited and inconclusive, especially in urban areas in the country (Washington et al., 2017). Prior studies also highlighted the gap in recruiting distinct samples of MSM who use alcohol but were not engaged in treatment settings (Irwin & Morgenstern, 2005; Santos et al., 2018). It is critical, therefore, to assess the pattern of alcohol misuse in the minoritized community to identify MSM at risk of hazardous drinking, especially in large cities with a high concentration of MSM, such as New York City (NYC).
High rates of binge drinking among MSM were associated with increased vulnerability to risky sex leading to HIV infection (Peacock et al., 2015; Woolf & Maisto, 2009), unfavorable outcomes among MSM living with HIV (e.g., antiretroviral therapy non-adherence; Sheinfil et al., 2022), mental health issues (Peacock et al., 2015), different types of intimate partner violence perpetration and victimization (Davis et al., 2016), and disruption in relationships, employment, and threat to financial stability (Wolitski et al., 2007). However, alcohol use disorder treatment remained underutilized among MSM in the United States (Hsiang et al., 2018). More than half of MSM with alcohol misuse received treatment for alcohol use, with 6.9% receiving pharmacotherapy (Santos et al., 2018). Recognizing the factors associated with alcohol misuse among MSM is crucial for improving access to alcohol misuse treatment.
MSM are the subpopulation most affected by HIV in the United States, and Black MSM accounted for 26.0% of new HIV diagnoses and 37.9% of diagnoses among all MSM in 2021 (Centers for Disease Control and Prevention, 2021). In NYC, the majority of new HIV diagnoses in 2018 were among MSM and Black individuals, comprising 52% and 46% of the cases, respectively. These figures highlight the disproportionate burden of HIV within the MSM community, particularly among Black MSM (New York City Department of Health and Mental Hygiene, 2019). Nearly half (47.0%) of MSM in NYC report binge drinking and excessive alcohol use (Centers for Disease Control and Prevention, 2019). Previous studies on Black MSM primarily examined the influence of substance use on HIV sexual risk behaviors in the United States in general (Allen et al., 2015, 2018). Particularly, the interplay between HIV infection and alcohol misuse has severe health consequences, notably contributing to antiretroviral therapy non-adherence (Sheinfil et al., 2022) and elevating the risk of incident HIV infection (Peacock et al., 2015; Woolf & Maisto, 2009) through factors like unprotected sex and engagement in multiple sexual partnerships (Allen et al., 2015, 2018).
A single study in San Francisco explored the prevalence and correlates of alcohol consumption among MSM, regardless of their race/ethnicity (Santos et al., 2018). However, this study included sexual risk behaviors in its analysis of factors linked to alcohol consumption but omitted other factors prevalent among marginalized MSM. These factors encompass racial discrimination and homophobia (Kipke et al., 2020), child sexual abuse (Kipke et al., 2020; Levine et al., 2018), depressive symptoms, and internalized homonegativity (DiGuiseppi et al., 2021). Additional research is needed to comprehensively assess the effects of these risk factors on alcohol misuse among Black MSM. Such studies can improve our understanding of this interplay, informing more targeted interventions and support.
In NYC, existing studies conducted focused on examining MSM’s mental health and risk behaviors (Cerdá et al., 2017; Dawson et al., 2019; Downing et al., 2020), trends in methamphetamine use (Rivera et al., 2021), access to HIV prevention and treatment services (Babel et al., 2021), and motivation for alcohol use to intoxication among young adult MSM (Ristuccia et al., 2019). Our study contributes to the extant literature by examining factors that might uniquely influence alcohol misuse among young Black MSM in urban settings, including perceived racism discrimination, childhood sexual abuse, and internalized homophobia, in addition to previously identified risk factors such as mental health (DiGuiseppi et al., 2021), drug use, and number of sex partners (Santos et al., 2018). By exploring these factors, the research will deepen our understanding of the unique challenges and experiences faced by Black MSM about alcohol misuse. The primary objective of this study was to describe the alcohol use patterns and examine factors associated with alcohol misuse among young Black MSM in NYC. By focusing on this specific population, we aim to provide a comprehensive understanding of alcohol misuse within their unique social context. The findings from this study will contribute to the existing knowledge base and offer valuable insights for developing tailored interventions and support systems to address alcohol-related concerns among young Black MSM in NYC.
Method
Data Description
Data for this study were derived from the baseline survey of the TRUST intervention from July 2016 to December 2017, a time- and attention-matched randomized controlled trial aimed at increasing uptake of HIV testing among young Black MSM/Transwomen. The TRUST intervention is a brief, peer-based behavioral intervention providing information on standard HIV risk reduction, HIV testing, and a psycho-educational rapid HIV self-test training session. The participants in the control group attended a 30-minute didactic informational session about a range of self-screening approaches for common, adverse health conditions (Frye et al., 2021). In this study, a total of 250 young Black MSM who (1) were aged 18 to 29, (2) were males at birth, (3) self-identified as Black, and (4) resided in NYC areas were included in the analysis. The institutional review boards at the New York Blood Center (study approval number 648283-50) and State University of New York at Binghamton (study approval number 3579-15) approved the study.
Measurements
Alcohol Misuse
The Alcohol Use Disorders Identification Test-Concise (AUDIT-C; Bush et al., 1998) was used to evaluate alcohol misuse in the past year and past three months. The AUDIT-C scale included three items (i.e., frequency of alcohol use, number of standard drinks on a typical day, and frequency of drinking five or more drinks on one occasion), adding up to a summary score of 0 to 12. A score of four was considered alcohol misuse or hazardous drinking. Binge drinking was defined as consuming five or more drinks on one occasion and was then divided into infrequent (drank less than monthly or monthly) and frequent users (drank weekly, daily, or almost daily). The past-year and past 3-month AUDIT-C in this study presented good to excellent internal consistency (Cronbach’s α = .82 and α = .81, respectively).
Depressive Symptoms
Patient Health Questionnaire-2 (PHQ-2), a two-item scale, was used to screen for depression (Kroenke et al., 2003). Each item was scored from zero (not at all) to three (nearly every day). Summary scores of PHQ-2 ranged from zero to six, with a score of three or higher being considered positive screening for depression. The PHQ-2 scale in our sample reported good internal consistency (Cronbach’s α = .77).
Psychosocial Risk Factors
Perceived racism discrimination was defined as having ever been made fun of, harassed, or called names because of race or ethnicity; perceived homophobia discrimination was defined by ever being harassed, verbally and physically threatened because of sexual orientation (Choi et al., 2013); and childhood sexual abuse indicated having had a sexual experience (e.g., being felt up or fondled or having oral, vaginal, or anal sex, with someone who was at least 5 years older than you) and/or being pressured, forced, or intimidated into doing something that made participants feel uncomfortable (e.g., masturbation, sexual touching, oral, or anal sex; Williams et al., 2015).
Internalized Homophobia
Six statements scored on a 4-point Likert-type scale of zero (Strongly disagree) to four (Strongly agree) were used to measure internalized homophobia, such as “If someone offered me the chance to be completely heterosexual, I would accept the chance” (Koblin et al., 2013). Summary scores ranged from 6 to 24 with higher scores indicating higher internalized homophobia. The internalized homophobia revealed excellent internal consistency (Cronbach’s α=.90).
Drug Use
Participants were asked questions about their use of drugs (e.g., marijuana, powder and/or crack cocaine, and methamphetamine) in the past year and past three months (Koblin et al., 2017). Hard drugs comprised cocaine and methamphetamine. Chemsex included participants who used any drugs (e.g., marijuana, powder/crack cocaine, methamphetamine, and club drugs) within 2 hr before or during anal sex as a top or bottom.
Sexual Risk Behaviors
Participants were asked about the number of casual male sex partner(s) they had anal sex with as a top or bottom during the last three months (e.g., participants put their penis in other partners’ anus or butt, or they put other partners’ penis in their anus or butt, with or without ejaculation) (Wilton et al., 2009). For this study, we categorized the number of causal male sex partners into three different groups: 0, 1 to 2, and >2.
Data Analysis
All analyses were performed using STATA version 17 (StataCorp, 2021). Mean and standard deviation (SD) were presented for numeric variables while frequencies and percentages were reported for categorical variables. This study will examine both past 3-month and past-year alcohol misuse to provide a more comprehensive understanding of alcohol use patterns and trends among MSM. This temporal perspective will allow us to explore how alcohol misuse may change over time and whether specific factors are associated with short-term or long-term changes in behavior. Given the prevalence of alcohol misuse in the past year and past three months, prevalence ratio (PR) was reported in bivariate analyses. Significant factors in the bivariate analyses or from previous studies were from previous studies included in the multivariable model. Multivariable log-binominal regression analyses were conducted to assess the association between demographic factors, psychosocial factors, and drug use with alcohol misuse, and adjusted PR was reported.
Results
Demographic Characteristics
The mean age of 250 young Black MSM in the study was 22.8 (SD=3.0) with 44.8% (112/250) aged 22 to 25 (Table 2). Approximately 70.0% (174/250) were gay, and 24.4% (61/250) were bisexual. The majority of MSM in our sample identified as African/African Americans (76.4%, 191/250). Most participants were born in the United States (88.8%; 222/250) and about half were religious (119/250). Seventy-eight percent of respondents (195/250) graduated from high school or higher, and 62.8% (157/250) had a personal income of less than $10,000 in the past year. More than 75.0% (189/250) experienced financial insecurity in the household for rent, food, or utilities (e.g., gas, electric, phone) in the past three months. More than 42.0% of participants (106/250) were living with parents and/or family members’ houses or apartments, and approximately half (120/250) were ever incarcerated.
Alcohol Use in the Past Year and the Past three Months
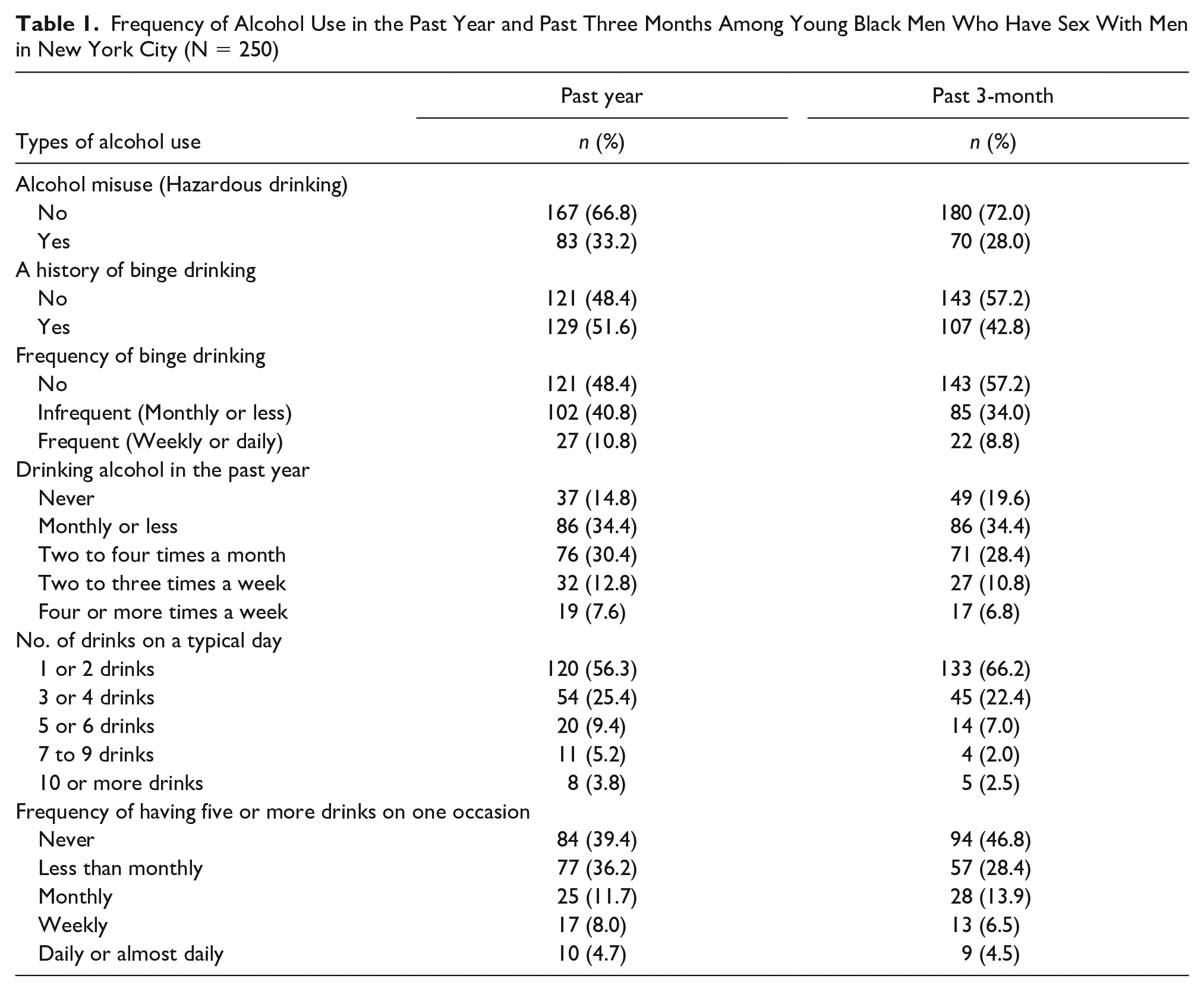
The prevalence rates of past-year and 3-month alcohol misuse were 33.2% (83/250) and 28.0% (70/250), respectively (Table 1). In the past year, 51.6% of participants (129/250) experienced binge drinking with 40.8% (102/250) and 10.8% (27/250) considered infrequent and frequent binge drinkers, respectively. More than a third of participants (86/250) reported drinking alcohol monthly or less. In the past three months, 42.8% (107/250) were binge drinkers with 34.0% (85/250) infrequent users and 8.8% (22/250) frequent users. The prevalence of past-year and 3-month drinking alcohol were 85.2% (213/250) and 80.4% (201/250), respectively. Among drinkers, 56.3% (120/213) and 66.2% (133/201) of participants reported having had one or two drinks on a typical day, respectively. Most participants did not have five or more drinks on one occasion in the past year (39.4%, 84/213) and the past three months (46.8%, 94/201).
Frequency of Alcohol Use in the Past Year and Past Three Months Among Young Black Men Who Have Sex With Men in New York City (N = 250)
Factors Associated With the Past-Year Alcohol Misuse
In bivariate analyses (Table 2), participants aged 26 to 29 (PR=2.09, 95% confidence interval [CI]: [1.31, 3.33]) and who were ever incarcerated (PR=1.64, 95% CI: [1.14, 2.36]) were more likely to report alcohol misuse in the past year compared with individuals aged 18 to 21 and those who had never been in prison, jail, or detention facilities. Participants with a history of marijuana use (PR=2.90, 95% CI: [1.59, 5.28]), hard drug use (PR=2.12, 95% CI: [1.59, 3.09]), and chemsex (PR=1.78, 95% CI: [1.24, 2.56]), and those who had multiple casual sex partners of 1 to 2 males (PR=2.07, 95% CI: [1.24, 3.43]) and more than 2 males (PR=2.28, 95% CI: [1.35, 3.82]) had higher odds of alcohol misuse in the past year (Table 3).
Demographic Characteristics and Their Associations With Alcohol Misuse Among Young Black Men Who Have Sex With Men in New York City (N = 250)

Note. PR = prevalence ratio; CI = confidence interval.
Psychosocial Risks and Their Associations With Alcohol Misuse Among Young Black Men Who Have Sex With Men in New York City (N = 250).
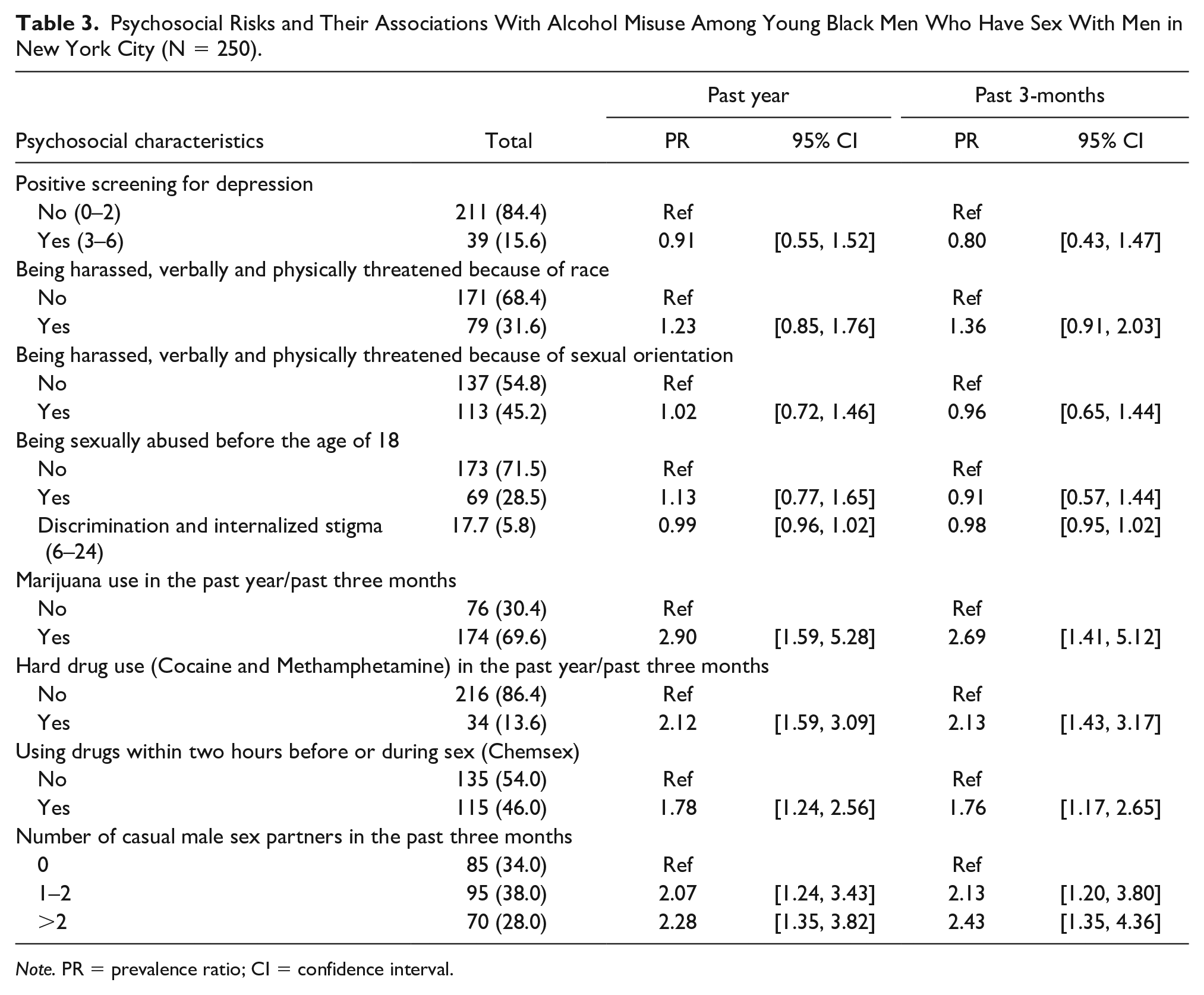
Note. PR = prevalence ratio; CI = confidence interval.
After adjusting for age in years and race in the multivariable analysis, factors positively associated with past-year alcohol misuse included a history of marijuana use (adjusted prevalence ratio [aPR] = 2.55, 95% CI: [1.33, 4.89]), a history of hard drug use (aPR=1.50, 95% CI: [1.02, 2.21]), and having one to two (aPR=1.87, 95% CI: [1.07, 3.26]) or more than two male partners (aPR=1.94, 95% CI: [1.08, 3.50]) (Table 4).
Multivariable Analysis of Factors Associated With Alcohol Misuse Among Young Black Men Who Have Sex With Men in New York City (N = 250).

Note. PR = prevalence ratio; aPR = adjusted prevalence ratio; CI = confidence interval. The model is adjusted for age in year and race (African/African American vs. no).
p < .05. **p < .01.
Factors Associated With The Past 3-Month Alcohol Misuse
Compared with participants aged 18 to 21 and those who were not religious, participants in the age groups of 22-25 (PR=2.03, 95% CI: [1.19, 3.45) and 26-29 (PR=2.40, 95% CI: [1.33, 4.31]) and those who were religious (PR=1.75, 95% CI: [1.16, 2.65]) were more likely to report alcohol misuse in the past 3 months. Incarcerated young Black MSM were more likely to have alcohol misuse compared to those without a history of incarceration (PR=1.63, 95% CI: [1.08, 2.45]). Furthermore, compared with men with income less than $10,000, the prevalence of alcohol misuse was higher among those with income of $10,000 to $19,000 (PR=1.84, 95% CI: [1.14, 2.96]) and $20,000-$29,999 (PR=1.74, 95% CI: [1.05, 2.88]). In addition, individuals with 3-month marijuana use (PR=2.69, 95% CI: [1.41, 5.12]), hard drug use (PR=2.13, 95% CI: [1.43, 3.17]), and chemsex (PR=1.76, 95% CI: [1.17, 2.65]) had a higher level of alcohol misuse (Table 3).
In the adjusted model, factors significantly associated with the past 3-month alcohol misuse included marijuana use in the past 3 months (aPR=2.30, 95% CI: [1.12, 4.71]), and having 1 and 2 (aPR=2.02, 95% CI: [1.07, 3.80]) or more than two male partners (aPR=2.18, 95% CI: [1.13, 4.19]). No statistical association was found between positive screening for depression, chemsex, and internalized stigma toward homosexuality with alcohol misuse in the past year and past 3 months (Table 4).
Discussion
This is one of few studies evaluating patterns and predictors of alcohol misuse in a sample of young Black MSM in NYC. Our findings showed a high prevalence of past-year and 3-month binge drinking among young Black MSM, which are in line with findings from the 2017 National HIV Behavioral Surveillance Report (Centers for Disease Control and Prevention, 2019) indicating that the prevalence of binge drinking during the 30 days before the interview were 45.0% and 31.9% among HIV-negative and HIV-positive MSM in general, and 47.0% among MSM in NYC. This suggests a need for targeted interventions and support programs to address alcohol misuse in this specific population. In addition, our findings are twice compared to 21.5% of Americans aged 12 and older who reported binge drinking in the past month in 2023 (Substance Abuse and Mental Health Services Administration, 2023) due to differences in age and study population. Previous studies indicated that older MSM are more likely to report alcohol use and alcohol misuse (Bhambhani et al., 2021; Liu et al., 2016). Another study conducted in San Francisco documented that nearly 25.0% and 19.3% were weekly and at least weekly binge drinkers (Santos et al., 2018) which were much higher than the respective rates in our study. This could be attributable to different sampling strategies: Santos et al. used respondent-driven sampling to recruit MSM, while our study relied primarily on online advertising, face-to-face outreach, and referrals by study participants (Frye et al., 2021), which could generate more diverse study populations. Future studies need to consider different sampling strategies to recruit a diversity of MSM to be representative for estimating alcohol use.
Notably, our findings highlighted the higher risk of alcohol misuse among young Black MSM in NYC compared with the adult population in New York State overall and other urban settings. The respective past-year and three-month prevalence rates of alcohol misuse in our study were 33.2% and 28.0%, much higher than 16.7% of adults in New York State who reported heavy drinking and excessive alcohol use in the past 30 days (New York State Department of Health, 2020). While our study measured alcohol misuse among MSM in the past year and past three months, the New York State report focused on alcohol misuse among adults in the past 30 days. Alcohol misuse is a key factor for HIV and STI infection among MSM because intoxication could in part interfere with the use of prevention methods (e.g., condoms; Liu et al., 2016; Wray et al., 2019). These findings emphasize the importance of raising awareness of alcohol misuse and implementing alcohol risk reduction programs in this vulnerable and hard-to-reach population.
In both bivariate and multivariable analyses, internalized homophobia was not statistically associated with alcohol misuse. Previous findings revealed that MSM might use alcohol as a strategy to cope with homosexual stigma or violence due to sexual orientation (Bruce et al., 2008; Wolitski et al., 2007). For example, the odds of binge drinking among those with high internalization of negative societal attitudes were 2.1 times higher compared to those with low self-stigma (Peacock et al., 2015). Furthermore, in our study, we assessed internalized homophobia using six questions with excellent internal consistency. It is necessary to further validate the scale we used to measure internalized stigma and evaluate the association between internalized homophobia and alcohol misuse with a large enough sample size. In addition, we found no statistical association between having positive screening for depression and alcohol misuse. In this study, PHQ-2 was used to screen for major depression, and internalized stigma was evaluated based on six single questions. Hence, further studies should use the full version of depression evaluation (e.g., PHQ-9) following a positive screening using PHQ-2 and stigma scales (e.g., Mayfield’s 23-item internalized homonegativity scale; Peacock et al., 2015) to assess the association with alcohol misuse.
Stevens et al. reported that alcohol was the most widely used substance among MSM with chemsex-related drug use (Íncera-Fernández et al., 2021). In our study, using drugs within two hours before or during sex increased the probability of alcohol misuse to 1.76 times; however, after controlling for demographic characteristics, chemsex was no longer a significant factor. This could be attributable to the broader definition of chemsex in our study which encompassed individuals using various substances such as marijuana, powder/crack cocaine, methamphetamine, and club drugs within two hours before or during anal sex, regardless of their role (top or bottom). In contrast, chemsex often refers to the use of methamphetamine in North America (Flores-Aranda et al., 2019). Although there is no agreement on the definition of chemsex which varies based on the cultural and geographical contexts (Flores-Aranda et al., 2019), it is well noted that chemsex among MSM is associated with significant physical, biomedical, and psychosocial harm (Stevens et al., 2020). Hence, more research is needed to examine the association between chemsex and alcohol misuse among MSM as well as develop psychosocial and behavioral interventions to support MSM with a history of chemsex that is positively associated with alcohol misuse.
In both crude and adjusted models, marijuana was significantly associated with the past 3-month and past-year alcohol misuse. A prospective study among American adults showed that marijuana smokers were five times more likely to develop an alcohol use problem, compared with those who had not used marijuana (23% vs. 5%, respectively; Weinberger et al., 2016). More importantly, Alcohol use and marijuana use during sex contribute to an increased risk of unprotected sex among MSM (Mackesy-Amiti & Ouellet, 2010). Specifically, the likelihood of participating in unprotected anal intercourse was approximately three times greater during sexual encounters involving both cannabis and alcohol compared with those without any substance consumption. (Firkey et al., 2021). These findings underscore the urgency for additional research aimed at unraveling the underlying mechanisms and designing effective interventions to support individuals grappling with concurrent substance use issues.
Our study revealed that young Black MSM with multiple casual male sex partners had a higher likelihood of misusing alcohol, which is similar to the findings of a study conducted among MSM in San Francisco (Santos et al., 2018). Again, these findings highlight the need to develop MSM-specific interventions that jointly address alcohol misuse and HIV risks. More importantly, we found that young Black MSM with a history of marijuana use and hard drug use were more likely to report alcohol misuse. These findings were consistent with prior studies indicating that using illicit drugs was positively associated with alcohol misuse (Liu et al., 2016). Santos et al. indicated that methamphetamine and cocaine were positively associated with hazardous drinking in bivariate analysis, although the authors used a different version of the alcohol use disorders identification test (i.e., full AUDIT; Santos et al., 2018). It is noted that existing studies, even with the general population, recommended differently gendered cutoffs for alcohol misuse with both the short and the full version of AUDIT based on the achievement of sensitivity and specificity (Moehring et al., 2019; Villarosa-Hurlocker et al., 2020). Alcohol use screening tools are necessary, therefore, that distinguish between sex- and gender-related characteristics which, in turn, could propose optimal screening cut-offs for alcohol misuse in this hard-to-reach population.
This study has several limitations. The original study focused on evaluating the efficacy of an intervention to increase HIV self-testing among young Black MSM and transwomen (Frye et al., 2021). This study with a small sample size targeting young Black MSM was not representative of the MSM community in NYC, although we implemented divergent sampling strategies (e.g., online advertising, in-person outreach, etc.) to recruit the best diverse pool of young Black MSM. In addition, the main outcomes of interest are self-reported which could suffer from the social desirability bias. Therefore, we presented the prevalence and correlates of both past-year and past 3-month alcohol misuse and concluded that there remain generally similar results regarding determinants of alcohol misuse. Finally, as discussed earlier, we used short versions of depression symptom severity as well as internalized stigma toward homosexuality which, in turn, might be unable to capture the covariates of interest. Future studies should implement the full versions of these scales to assess the association with alcohol misuse.
Conclusion
The high prevalence of binge drinking and alcohol misuse among young Black MSM emphasizes the need to raise awareness of alcohol misuse as well as alcohol risk reduction programs should be designed to jointly address HIV risk in this vulnerable population in NYC. Moreover, it is crucial to integrate linkage to care or treatment services for alcohol misuse and HIV prevention efforts within these programs. By addressing both the alcohol-related concerns and the associated risk of HIV transmission, we can better support the overall well-being and health outcomes of young Black MSM in NYC. Future studies should incorporate comprehensive assessments of mental health risks and internalized homophobia scales to enhance our understanding of their association with alcohol misuse, thus informing the development of more effective interventions and support systems.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the National Institute on Drug Abuse under Grant #R01DA (mPIs: Frye & Wilton). The sponsor does not have a role in study design, data collection, analysis or interpretation of results, writing of the manuscript, or decision to submit for publication.
Ethics and Consent Statement
Ethical approval for the study was obtained, and consent forms from all participants were obtained prior to the study.
