Abstract
Black men comprise most new HIV infections in the Southern United States and have worse HIV outcomes than their non-Black counterparts. We developed an academic–community partnership in Nashville, Tennessee, to explore opportunities to improve HIV outcomes for Black men. We recruited barbers to an HIV training and focus group discussion about prevention and potential barber/barbershop-based strategies to address HIV-related needs for Black men. We assessed HIV knowledge and stigma with validated scales and conducted thematic analysis on discussion transcripts. HIV-related stigma was low (1.8 of 15 points [SD = 1.69]) among 13 participants of unknown HIV status (12 men and one woman). HIV knowledge increased among eight (67%) participants after receiving a brief HIV didactic. Participants described general health care barriers (e.g., the social norm that Black men do not go to the doctor until they are “damn near dead”), fears about unwanted HIV disclosure when seeking HIV testing or care, and community fears about negative stereotypes associated with HIV. Participants expressed enthusiasm about receiving more HIV-related training and utilizing communication skills and client/community relationships to serve as health educators and navigators. Barbers highlighted opportunities to disseminate HIV information in barbershops and combine HIV interventions with other health issues, such as COVID-19, and suggested that these interventions may help reduce HIV-related stigma. Our findings suggest that barbers and barbershops are an underutilized resource for disseminating HIV-related health information and engaging Black men in HIV and other important prevention and care activities such as COVID-19.
Background
There are 1.1 million people living with HIV (PLWH) in the United States (Centers for Disease Control and Prevention [CDC], 2020). After several years of marked decline, the number of new annual HIV infections in the United States has been stagnant since 2013 (CDC, 2018). An estimated 69% of new infections are transmitted by individuals who are aware of their HIV status but not virally suppressed (Frieden et al., 2015). In 2019, the U.S. Department of Health and Human Services launched an ambitious plan to “End the HIV Epidemic” in priority communities most affected by HIV. The goal of the End the HIV Epidemic plan is to integrate evidence-based interventions with innovative implementation strategies to address four pillars: (1) early HIV diagnoses; (2) rapid and effective HIV treatment; (3) protection of people at risk of HIV; and (4) rapid response to HIV clusters (Fauci et al., 2019). Priority communities were identified in 48 counties with the highest rates of incident HIV diagnosis and seven states with exceptional HIV burden in rural areas. 4 Tennessee (TN) is home to such priority communities. TN has the lowest linkage to HIV care rates in the country (with only 64% of newly infected patients establishing care in 2018) and remains below national targets for viral suppression (62% TN vs. 95% national target) (“Announcement: Monitoring Selected National HIV Prevention and Care Objectives,” 2017; CDC, 2018; Sutton et al., 2017). These data underscore a vital need for effective HIV care and treatment interventions in TN.
Black individuals are disproportionately burdened by chronic diseases, including HIV, and often face worse outcomes than racial/ethnic majority groups (Blackwell et al., 2014; Cunningham et al., 2017; Genberg et al., 2009; Hales et al., 2020). Research on linkage to HIV care in TN highlights disparities among important subgroups (Ahonkhai et al., 2018). Most notably, young males had only a 50% to 60% probability of linking to HIV care within 30 days of diagnosis and were the least likely risk group to establish care—a finding even more pronounced among non-Hispanic Black (Black) men (Ahonkhai et al., 2018; Pierce et al., 2022). Young Black men living with HIV in the South are a particularly vulnerable population contending with intersecting stigma related to race, class, and sexuality. These stigmas contribute to creating a challenging environment for health care–seeking behaviors (Bowleg et al., 2013; Bowleg et al., 2011; CDC, 2020; Gross et al., 2016; Lall et al., 2015). Young Black men comprise the majority of new HIV infections in TN, but have too often remained hidden from care (Tennessee Department of Health, 2021). Unfortunately, despite concerted efforts by the TN Department of Health (TDH) to minimize racial and ethnic disparities in linkage to care and other outcomes along the HIV continuum of care, these trends have persisted (Tennessee Department of Health, 2020). Finding and engaging young Black men in trusted settings to promote their health is critical to improving linkage to HIV care, improving their HIV outcomes, and ultimately ending the HIV epidemic in TN.
Barbershops may represent one such trusted setting for Black men. Black barbers and barbershops across the United States are widely regarded as confidants in trusted environments by their clients (Data USA, n.d.; Linnan, 2019; Luque et al., 2014). Barbershop-based strategies have been successfully used to disseminate health education and deliver treatment interventions for Black men (Data USA, n.d.; Linnan, 2019; Luque et al., 2014). Such interventions have targeted outcomes for people with cardiovascular disease, diabetes, and colorectal cancer (Linnan, 2019; Linnan et al., 2014; Victor et al., 2018). These models could be adapted to address other chronic health conditions such as HIV (Linnan, 2019). Prior research on barbershop-based interventions addressing HIV has focused on sexual health education and HIV prevention (Baker et al., 2012; Brawner et al., 2013; Jemmott et al., 2017; Wilson et al., 2014, 2019). Barbershop-based strategies to improve linkage to care and other outcomes along the HIV care continuum among young Black men living with HIV remain relatively unexplored (Baker et al., 2012; Wilson et al., 2014, 2019). This type of community-engaged strategy may help address pervasive disparities in HIV care in the South (Ahonkhai et al., 2018; Pierce et al., 2022).
Community engagement is defined as “the process of working collaboratively with and through groups of people affiliated by geographic proximity, special interest, or similar situations to address issues affecting their wellbeing.” Community engagement relies on building partnerships and coalitions that can serve as important catalysts to mobilize resource and influence change (Agency for Toxic Substances and Disease Registry [ATSDR], 2018; McCloskey et al., 2011). The community engagement continuum is often described on a spectrum that at one end describes outreach or consultation, and on the other end describes shared leadership. There is strong evidence that partnerships between academic and community that value and prioritize community input not only increase the relevance of research but also drive innovation, discovery, implementation, and dissemination of evidence-based research (Bodison et al., 2015; Selker & Wilkins, 2017). Community engagement has been vital to the progress in HIV prevention and treatment research (Karris et al., 2020; Rhodes et al., 2018). Despite its importance in guiding the development of equity-focused solutions for marginalized PLWH, community engagement remains inconsistently utilized (Karris et al., 2020; Rhodes et al., 2018; Shelton et al., 2021). Novel community-engaged research strategies will be vital to addressing pervasive racial/ethnic disparities in HIV outcomes and moving toward the goal of ending the HIV epidemic.
To address this need, this study first developed and strengthened a partnership between an academic institution (Vanderbilt University Medical Center [VUMC]) and a community-based organization (Street Works, a 501(c)(3) nonprofit) in Nashville, TN, to set up a community-engaged research project. Subsequently, mixed-methods were used to explore opportunities for engaging barbers and barbershops in local efforts to improve outcomes across the HIV care continuum for Black men in middle TN.
Method
Initiating the Partnership and Defining Partnership Goals
An infectious diseases physician-scientist at VUMC focused on interventions addressing poor outcomes along the HIV care continuum reached out to a community-based organization, Street Works, about forming an academic–community partnership. Street Works was founded in 1997 with a mission to prevent the spread of HIV and provide care and support services for individuals infected with and affected by HIV. Street Works has cultivated strong partnerships with a network of barbershops in the middle TN region by conducting a prevention initiative that features the weekly, free distribution of condoms and HIV educational materials, and partners with individual barbers in selected venues to exchange haircuts for free HIV testing. Preliminary data from academic team’s research on linkage to HIV care in TN were the impetus for the development of this partnership to explore how barbershop-based initiatives could address pervasive disparities in HIV care in the region (Ahonkhai et al., 2018; Pierce et al., 2022).
The academic and community team members met formally to discuss the role of each institution in the Partnership. The project team on the academic side included the physician scientist, a project manager, and a student intern. The community team from Street Works included an early intervention specialist (tasked with identifying and addressing barriers to medical care for individuals newly diagnosed with HIV) and members of their HIV prevention and education department. Consistent with principles of community-engaged research, the team created a Give-Get Grid to define what each partner was expected to contribute to and benefit from the Partnership (Table 1) (Southerland et al., 2013). These metrics, when defined early in a partnership, aid in maximizing stakeholder investment (Southerland et al., 2013).
Give-Get Grid for Academic–Community Partnership to Explore the Role of Barber/Barbershop-Based Strategies to Improve HIV Care for Black Men in Tennessee.

Note. EIS = early intervention specialists.
The Partnership was expected to strengthen Street Works’s capacity to conduct community-based HIV research while continuing to provide lifesaving services to people infected with and affected by HIV. The Street Works team would learn about the key steps in conducting community-based research. The Partnership would additionally provide Street Works with greater access to information regarding funding opportunities for community-based HIV research. At the same time, the academic partner would learn from Street Works about accessing and building upon trusted community relationships in addition to learning from Street Works’s patient/client experience on how to optimally engage both community partners and patients—specifically young Black men living with HIV—in settings outside of the health center to promote individual health and well-being.
Study Population, Recruitment, and Consent
Street Works’s prevention outreach team recruited barbers from barbershops serving predominantly racial/ethnic minorities in the Nashville metropolitan area. Barbers who were a member of a racial/ethnic minority group and served primarily Black male clients in the barbershop were eligible to participate. The barbershops were part of Street Works’s weekly condom distribution program, and Street Works’s team members had long-standing relationships with both the barbershops and the barbers who operated them. Eligible barbers were invited to participate in a half-day, live, virtual workshop (via Zoom). Interested barbers were provided with a palm card that provided some information about the workshop and were encouraged to share the information with their colleagues for further recruitment. Barbers were recruited as stakeholder experts given their firsthand knowledge of and lived experience within the targeted community, and were accordingly compensated at a rate based on the local average value of volunteer time via VISA gift cards (Joosten et al., 2015).
Study Activities
The virtual workshop included basic HIV education, an assessment of HIV-related knowledge and stigma among barbers, and a facilitated discussion about the potential roles of barbers and barbershops to improve the HIV outcomes for Black men. Specifically, the academic team developed a 20-min didactic presentation on HIV prevention, transmission, and treatment for a general audience.
Data Collection
We assessed stigma utilizing a validated questionnaire with three sub-scales measuring negative attitudes toward PLWH, perceived discrimination in the community toward PLWH, and support for equitable treatment of PLWH (Genberg et al., 2009). Higher scores indicate higher levels of stigma (Genberg, 2009). The study team created this questionnaire using assessment items provided in the 2006 United States Agency for International Development (USAID, 2006) report on HIV/AIDS stigma to measure stigma in a general, non-medical population (and not specific to PLWH). The USAID Report documents indicators and accompanying questions to promote the quantitative measurement of HIV-related stigma for practitioners, policy makers, and donor agencies to document the impact of their programs on stigma. HIV-associated stigma was assessed one time before the didactic presentation.
HIV knowledge was assessed before and after the didactic presentation using a 22-item questionnaire with forced-choice statements (“true,” “false,” “don’t know”) that elicited HIV knowledge. This questionnaire contained all 18 items from the HIV-KQ-18, a scale designed to assess HIV knowledge in both clinical and nonclinical settings, and four items from the HIV-KQ-45 (a longer, 45-item scale from which the HIV-KQ-18 was adapted) (Carey & Schroder, 2002). The additional four items were: (1) a person can get HIV from a toilet seat, (2) it is possible to get HIV when a person gets a tattoo, (3) you can usually tell if someone has HIV by looking at them, and (4) cleaning a syringe multiple times with bleach and water before using it again kills HIV. Both the stigma and knowledge questionnaires were administered anonymously via the Zoom poll feature.
After the presentation and assessments, barbers participated in a focus group discussion. They were introduced to the Partnership objectives through a brief presentation, and then a study team member facilitated a discussion around four key issues: (1) health issues and concerns shared with the barbers by their clients, (2) barrier their clients faced to accessing health care, (3) role barbers could play in helping or motivating clients to get into or stay in HIV care to be healthy, and (4) potential barriers and facilitators to barber/barbershop-based initiatives focused on HIV care and treatment for Black men. Within Item 3, barbers were probed about comfort with sharing information about HIV, barbershop-based HIV testing, and access to HIV treatment within barbershops.
Data Analysis
We utilized descriptive statistics to summarize HIV knowledge (pre- and post-HIV education presentation) and HIV-related stigma among participants. The focus group discussions were recorded and transcribed by two team members. Thematic analysis was conducted to understand barriers and solutions to improving HIV care outcomes for Black men in the region.
Ethical Approval
Institutional ethical approval for this study was obtained (Institutional Review Board protocol no. 210065).
Results
Program Participants, HIV Knowledge, and HIV-Related Stigma Assessments
Thirteen barbers (12 men and one woman) participated in two workshops (seven attended the first workshop and six attended the second workshop). Among the 12 participants who completed the HIV knowledge questionnaire both before and after the didactic presentation, the average initial knowledge score was 15.5 out of a total 22 points (SD = 4.15), and the average follow-up knowledge score was 17.9 (SD = 2.71). Eight participants (67%) had an individual improvement in their score. The average total HIV-related stigma score was 1.8 out of a total 17 points (SD = 1.69) for 12 participants who completed the assessment.
Barriers and Solutions to Improving HIV Care for Black Men in TN
Thematic analysis of the facilitated focus group discussion revealed several important barriers and solutions for improving HIV care outcomes for Black men in the region (Figure 1). Participants first described several structural and interpersonal obstacles to accessing health care in general, such as cost and concern about poor treatment and/or negative interactions experienced within in the health care system. Barbers subsequently described challenges that centered around HIV-associated stigma that remained deeply rooted in the community. Participants also discussed other entrenched beliefs held by Black men about health and concerns about the capacity to cope mentally with unwanted illness (especially HIV), both of which caused many to delay seeking out health care until very late in a disease course when they feel very sick or symptomatic.
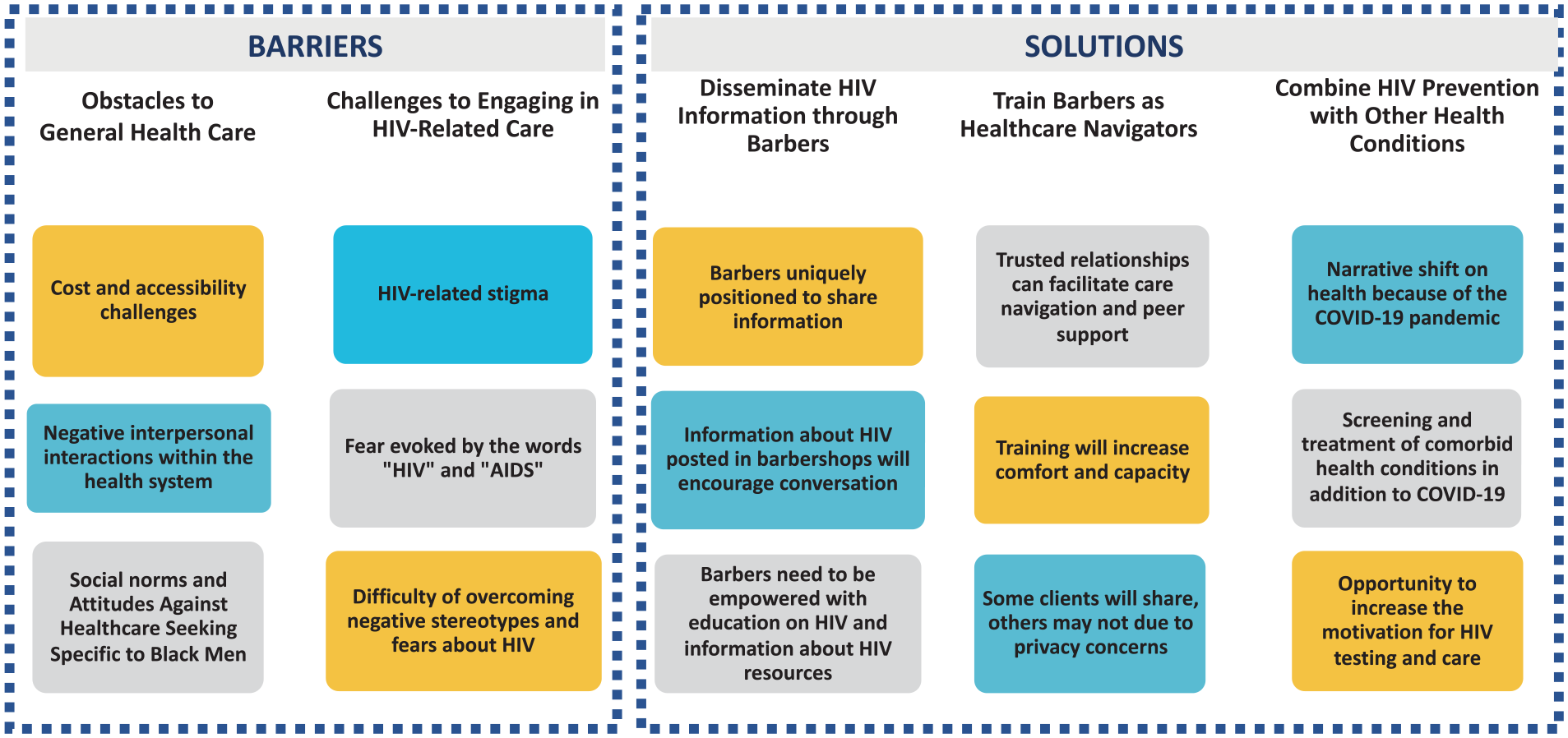
Perceived Barriers and Solutions to HIV Care for Black Men Among Barbers in a Southern U.S. City
Participants were eager to play a role in addressing racial disparities in HIV care outcomes for Black men and in reframing the narrative in the community about HIV. They identified some ways in which barbers and their shops could be leveraged to address stigma and other barriers to health care, including comprehensive training of barbers, provision of educational HIV-related materials that they could display in their shops to promote conversation, and ensuring that barbers understand how to navigate key steps in the care continuum (especially HIV testing) so that they can be better positioned to discuss it with clients. Participants also discussed the potential role they, as barbers, could serve as peer navigators. Participating barbers also described how COVID-19 has spurred a focus on health status in the community, which should be used as an opportunity to provide the required education about HIV by pairing it with information about COVID-19.
Obstacles to General Health Care
Barbers described that their clients, most of whom are Black men, face several challenges to accessing health care in general. These challenges include cost, general access, and concern about poor treatment and other negative interactions when in the health care system. One participant said, “We worry about it being costly . . .” Another shared, “Or then when you do go, they don’t diagnose you right. . .you will be concerned about what another person is gonna say, you go to . . . a general hospital or something, they’ll treat you like a piece of garbage.”
In addition, several participants described their thoughts about the social norm that Black men typically do not seek health care until absolutely necessary. For example, one participant said, “You know, [Black men] don’t like to go to the doctor a lot.” Others indicated that it takes physical pain, advanced illness, or severe illness of a loved one to motivate health care–seeking: “That’s what black men do. We don’t go until we’re damn near dead.”
And also, I just had a birthday. So just in the last couple of years [I started] on a petition, or every 90-day basis, to check up or stuff like that. But until then, I didn’t. . . . I had to lose people. . . My mom died at 52 and then my aunt died at 55. So then became real to me that I might need to make sure that I got my ducks in order.
Challenges to Engaging in HIV-Related Care
Participants described how fear of stigma was a barrier to HIV prevention, care, and treatment. Specifically, they described fear that might arise from simply accessing services at facilities associated with HIV and fear that might arise about the capacity to cope mentally with an unwanted illness. They explained that these fears can lead to delays in seeking health care. One participant shared, So even though you’re getting the help, there is a stereotype. So, it’s one of those things where all the help is concentrated in the same places. . . . But just the fact that you get off the van here or you go there, you automatically are outing yourself. You know what I’m saying, by having HIV, or have a disease and stuff like that, and so that caused a lot of people not to seek the help because it’s only in certain spaces.
Another participant agreed, . . .it would be a whole lot helpful in getting folks to get tested, if those tests were available at other places that didn’t scream “I got HIV,” or “I think I got HIV.” You know like a drug test. Like a drug test now can be tested anywhere.
Another participant described mental health as an important unaddressed obstacle for seeking HIV care: . . .depression is at an all time high. And I speak to about with my clients right now. . . . And I’m pretty sure that’s a down feeling to, to feel as though you slipped up like that, you know, cuz, it’s nobody’s fault but ours, so for you to slip up and trust somebody and then you know, your whole life turns around, that’s a big change in your life. So depression will be my answer to that, you know, I would say depression plays a lot into why we don’t do a lot of things.
Participants also described palpable fear elicited by the words “HIV” and “AIDS” even in the face of knowledge about the availability of effective treatment. One participant exclaimed, “I’d rather get shot than say I got AIDS.” Another participant offered, “When you hear AIDS, you can say some nice stuff about it but it’s AIDS. . .I know I can live and all that, but I’ve got AIDS.”
After discussing negative stereotypes in the community about HIV and powerful, fear-evoking narratives about HIV, participants emphasized reframing this narrative. One participant asserted, So, it’s one of those things that honestly, I feel as though it would need to be recategorized, like repainted . . . to come up with a different name for something instead of AIDS . . . The name it’s something where we built it to be in our head is what I’m saying. So, this is we built it up, we built it to issue [where] we scare ourselves. . . You have to rename it. I don’t know. I don’t want to hear AIDS.
Another participant shared, I think once, once the media changed the narrative about HIV, I think it’d probably be a little more easier amongst young Black men. . . .You know, like It’s just hard to really talk to somebody about if you had AIDS. You couldn’t go to your homies, and be like, ‘Hey, bro, you know what I’m saying, I’m dealing with this. I’m dealing with that.’ You can’t do that. Not in these times or any other times if I could really imagine. I just feel like once the media changed the narrative, I think it’ll be a little more sensitive, as far as the conversation [about HIV] is concerned.
Leveraging the Role of Barbers as Trusted Confidants to Promote HIV Education and Stigma Reduction
Participants emphasized their role as trusted leaders in the community. They described how barbers could disseminate information in their shops and through their networks that reach more widely across the Black community.
Several participants described how they were uniquely positioned as barbers in the community to share information: You know, barbers, we’re like the bartenders, you know, and like, the doctor before the doctor, you know, I mean, and like psychiatrists because, people come to us, and they feel like we’re trusted and sharing things with us. So what I think needs to be done, what, what us as barbers can do is, like, get information that you all can provide to us, and then like, expose it to our clients . . .
Others shared how the environment in the barbershop is ripe for discussion and how conversations that start in the barbershop easily spread beyond the shop and into the community. One participant said, “I mean, we go hard, we talk about whatever. . . . You know, because it ain’t nothing under the sun that we don’t talk about over here.” Another described, “All you have to do in a barbershop is start something say one word, and somebody else will carry it on. . . But if we have the information that you all have if you all provide us with that.” Still another said, “Most likely one conversation in a barber shop will end up outside of the barbershop with another person and then that is like a web of like information that will get out.”
Participants felt that they could play an important part in reshaping this narrative about HIV because of their unique position within their communities. One offered, “It’s up to you to change that energy, and, and stuff within your place, you know, and to make it what it is. . . . it’s up to us to change the narrative of it, and we can most definitely do it.”
Equipping Barbers to Disseminate Information as Trusted Leaders in Trusted Environments
All participants expressed interest in increased HIV education for barbers. They described that it is not common to see educational material about health topics in the shops and felt this lack of available material was a critical missed opportunity to share health and HIV-related information with their clients. One participant shared, “You don’t see a lot of literature and postage about HIV especially in barbershops. If you could have more posters and flyers along with the condoms that Street Works has. . .”
Many barbers felt that it would be helpful to have these HIV educational materials provided to them so that they could combine their acquired knowledge with these materials to educate clients. Participants described themselves as conduits of information for their clients and felt that if they were equipped with education and materials this would be an easy way for them to disseminate HIV-focused information. One said, “We need more information and education about [HIV], this will give us reason and education to execute that conversation.” Another agreed, “Get [HIV] information that you all can provide to us and expose it to our clients. . . we can have the literature there. If they ask about it, we can share about it.”
Participants emphasized the importance of having information not just about HIV prevention, transmission, and treatment, but also about how to navigate the process of getting an HIV test and establishing HIV care. They advised that clients need to know locations of HIV clinics and names of people they could contact with any questions. Offering this kind of access-related information would show clients that they have options and the ability to choose resources for care. One individual suggested, “I think the target should be giving them education about it [HIV], letting them know the location [of HIV clinics], the people to contact and the symptoms. Letting them know they have the option/choice.”
Participants also advised that they could encourage HIV testing by showing their clients how easy it is to get tested for HIV: “I would want to show how easy it is to go get tested for HIV. . .and really encourage them by informing them.”
Utilizing Barbers as Health Care Navigators
When participants were asked about their willingness to be health care navigators, some described how their trusted relationships with clients could facilitate both peer support and care navigation: I feel like barbers and hairstylists play a major role in the world. Just as doctors and nurses do, you know. We interact with different people, different races, different nationalities. So I feel like we have a big voice in the community. . . . If I did have a client, and I could be wrong, if I did have a client, like that was struggling with HIV or something to that nature, I feel like I make my clients comfortable and that I would be able to be supportive of them, and I’ll be able to help them.
Another shared, I feel that the conversation is open to be discussed. . . . it’s really not a discussion that you would probably want to discuss with someone, you know, if you got three or four people sitting around, waiting to get a cut. So more so [it’s] like, on an individual scale with you and that client, it gives you the time and the space to have that conversation. So definitely the conversation needs to be initiated. And once you have that client to open up, then you know, you throw in, you know, about health care, by the HIV. And you know, is kind of just getting to the client where you can get that relationship where you have that comfortability to have the conversation.
Some participants cautioned that not all barbers or clients would feel this degree of comfort due to concerns about privacy and stigma about HIV within their community: As far as Black men, we’re not going to have that conversation—especially in the barber shop. I can say it’s totally different in the barbershop, and for somebody to break that out in front of everybody. I’m pretty sure everybody kind of feel uncomfortable, with the state we in, as Black people.
Despite this acknowledgment about hesitancy, the participants demonstrated a willingness to be part of HIV-related outreach. One participant enthusiastically shared, “I’m all in on whatever we can do to really pass and get this message through to young black men. I like, totally down for that.”
Overall, participants believed that they would be empowered to have conversations about HIV with clients if they had sufficient HIV education: “I definitely think maybe [the intervention] should be HIV barber training courses, where barbers can put up that information [about HIV]. . . But I do think [there] should be more training.”
Combining Efforts to Address HIV With Other Health Conditions
Some participants described that hearing about COVID-19 and associated comorbidities has made people more aware of their health status in general and the need for screening and treatment of comorbid health conditions in addition to COVID-19. One participant explained how the COVID-19 pandemic has shifted the narrative on health entirely. Others agree that this shift in the prioritization of health may provide an opportunity to increase the motivation for HIV testing and care, and provide health-related information to a receptive audience: What the Coronavirus has opened my eyes to that, you know, it can happen to you, it can happen to me, you know. Just as people think that they can’t get HIV or they invincible or it can’t happen to them, and they talk all around it. . .We need to take advantage of the [COVID-19] pandemic. Everyone is going to get tested for COVID-19. It [HIV testing] can be incorporated with that.
Discussion
Our study utilized community-engaged research methods to guide the process of identifying potential barbershop-based solutions to address important racial disparities in HIV care outcomes. Specifically, we formed an academic–community partnership with a community-based organization in middle TN that collaborates with a network of barbers and their barbershops to deliver HIV prevention services. The Partnership convened 13 barbers to assess their HIV knowledge and attitudes; discuss challenges for accessing health care, in general, and HIV care, in particular, among Black men; and provide potential solutions to those challenges. Several themes arose during focus group discussions that revolved around perceived norms, fear, and stigma as barriers to health care–seeking, the need to reframe HIV messaging with a more positive tone to counteract those beliefs, and the potential for barbers and barbershops to be a conduit for HIV education and care navigation given their extensive community reach and trust.
Our findings suggest that, in this region, barbershops are an underutilized resource for disseminating HIV-related health information as the shops are important canvases for information-sharing within the community. Barbers are trusted messengers who can be trained to relay this information. Feedback from barbers highlighted their enthusiasm for playing a role in reframing the narrative around HIV, which they believed could help in reducing HIV-related stigma in the community. Importantly, our cohort of barbers showed increased HIV knowledge scores after a brief, focused HIV education session. Furthermore, our findings suggested that barbers themselves, and the valued relationships they have with their clients, could likely be leveraged to help improve outcomes along the entire HIV care continuum for their community by adapting approaches (like health care navigation and health education) to be delivered by barbers.
The barbers in our cohort suggested pairing information about HIV with other important health conditions as a way to connect with people in the community. They emphasized that the COVID-19 pandemic created an opportunity for health promotion as it has caused communities, including Black men, to pay closer attention to their health. Community-based health promotion became a central component of COVID-response activities, especially in communities disproportionately affected by the disease (Palmer et al., 2020). Public health leaders have called on trusted community messengers to share accurate and reliable information about COVID vaccines and treatment—a role that, with training, barbers could play (Palmer et al., 2021).
Barbershops have become an increasingly popular venue for health interventions (Victor et al., 2019). One systematic review found that most of the published interventions in Black beauty salons and barbershops addressed cancer (50%) or hypertension (36%). Although the data are fewer, Black barbershops have been used to promote reproductive health. For example, the Barbershop Talk with Brothers randomized controlled trial in New York reported that, after the intervention, barbershops had a 61% increased risk of not having condomless sex (Wilson et al., 2014). One widely cited, barbershop-based intervention integrated a pharmacist into the shop to deliver pharmaceutical care for hypertension. This intervention resulted in significant, sustained blood pressure control at 1 year for individuals in the intervention arm (68%) compared with those in the control arm (11%) (Bassett et al., 2018). Although the specific components of this intervention that drove treatment success remain unknown, it is clear that delivering such services outside of traditional health care settings may be optimal for some Black men (CDC, 2021).
Despite the success of these approaches, all chronic diseases are not alike, and a pharmacist-based medication intervention for PLWH may carry the enormous weight of a highly stigmatized illness. While our barbers scored low overall on an HIV stigma assessment, they still described very potent images of HIV and the stigma it carries in the community. They cautioned that any interventions targeting continuum of care outcomes in the barbershop setting would have to be delivered with stigma in mind as a potential barrier, but also highlighted how barbershop communities could themselves help to reduce HIV-related stigma by promoting a different, “re-branded” narrative about HIV. They emphasized the need to destigmatize HIV care continuum services by removing them from stigmatized health-related environments (such as health centers and AIDS service organizations)—an approach that could be supported by promoting self-testing for HIV and other medical conditions at home and in safe community spaces (Baker et al., 2012). It is possible that stigma has precluded barbershop-based treatment (rather than prevention) interventions for PLWH. But at least one study outside the United States, based in beauty salons (not barbershops), suggests that this approach may hold promise. This study integrated a contraception and pre-exposure prophylaxis (PrEP) intervention for South African women, and found that three quarters or more of women were comfortable receiving injectable contraception, PrEP, and HIV testing in the beauty salon (Hill et al., 2021).
There are no published studies utilizing barbers as health care navigators for PLWH. However, health care navigation has been recommended as an intervention to improve linkage to care, treatment, and retention for PLWH (CDC, 2021). Health care navigation is a process by which an individual guides a patient through and around the barriers of a complex care system to help ensure timely diagnosis and treatment (CDC, n.d.; International Advisory Panel on HIV CCO, 2015; Koester et al., 2014). Successful models of health care navigation for colorectal cancer screening have leveraged Black barbershops in New York (Cole et al., 2017). For PLWH, health care navigators are typically employed by health departments or AIDS service organizations to work with newly diagnosed patients to promote linkage to and engagement in care. Like traditional health care structures, these models are not working for many Black men, and bringing the health care navigator role to a trusted messenger, in a trusted environment, may provide the type of contextually and culturally appropriate care needed by some individuals. Our cohort of barbers were still enthusiastic about the idea as long as they had appropriate training and support to play this role.
This study has both strengths and weaknesses. Facilitated by an academic–community partnership, the greatest strength was our use of a community-engaged approach to assess the potential form and acceptability of barber and barbershop-based solutions to address the HIV care needs of Black men in the Southern United States. One weakness of this analysis was that our use of an urban environment convenience sample of barber may not be generalizable to other communities. Another weakness is that barbershop patrons were not included in the study. While the perspective of such patrons will be critical to obtain in follow-up research, in our analysis, the barbers themselves represented both a key focus for intervention and the target community for intervention—Black men at risk of or living with HIV.
Conclusion
Barbers in middle TN described untapped opportunities to design HIV prevention and treatment services that build on barbers’ standing in the community and trusted relationships with their patrons to provide health education and care navigation; use the barbershop context to spread information beyond the walls of the shop to larger networks in the Black community; and build on their expertise as key stakeholders in the community to reframe a fear-based narrative about HIV. Furthermore, our analysis underscores the importance of engaging barbers as key stakeholders and experts in the community to develop equity-focused solutions to addressing important health disparities for HIV and other pressing health needs.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was supported from NIH 5R25MH080665, 5P30AI110527, CTSA UL1TR000445.
