Abstract
The availability of several treatment options for prostate cancer creates a situation where patients may need to come to a shared decision with their health-care team regarding their care. Shared decision-making (SDM) is the concept of a patient and a health-care professional collaborating to make decisions about the patient’s treatment course. Nurse navigators (NNs) are health-care professionals often involved in the SDM process. The current project sought to evaluate the way in which patients with prostate cancer make decisions regarding their care and to determine patients’ perspectives of the role of the NN in the SDM process. Eleven participants were recruited from the Prostate Assessment Centre by a NN. They were interviewed via telephone and their responses were analyzed using thematic analysis. Five interacting factors were determined to influence the way participants made decisions including level of anxiety, desire to maintain normalcy, support system quality, exposure to cancer narratives, and extent of practical concerns. NNs were found to increase knowledge, decrease indecision, and provide reassurance for participants. Based on the beneficial aspects of NN interaction reported in this study, the use of NNs in SDM programs should be encouraged. The results of the study demonstrate the complexity of the decision-making process when it comes to prostate cancer treatment. The factors elucidated in the study should be considered during the development and implementation of prostate cancer SDM programs.
Keywords
As the second most common cancer worldwide (Ferlay et al., 2014), prostate cancer, and the subsequent necessity to make treatment decisions, is an issue many men encounter. There are four options available for the management of localized prostate cancer, including radical prostatectomy, brachytherapy, external beam radiotherapy, and active surveillance. All management options are considered to be equally efficacious, for most men, for prevention of mortality, however, each option has its own set of unique consequences (Hamdy et al., 2016; Resnick et al., 2013; Zelefsky et al., 2016; Serrano et al., 2016). Other therapies such as cryotherapy and androgen deprivation therapy are not used for localized disease within Saskatchewan (Saskatchewan Cancer Agency, 2003). Androgen deprivation therapy is used as adjunct therapy in advanced prostate cancer and palliative measures in metastatic and refractory disease (Saskatchewan Cancer Agency, 2003; Karl & Konety, 2009). There is a large volume of information that patients must process and evaluate. Important medical decisions, such as those about prostate cancer treatment, can cause patients to experience anxiety and fear (Loewenstein, 2005). Therefore, prostate cancer patients may feel overwhelmed (Loewenstein, 2005) and might find a program to help them with their decision-making to be beneficial. Research investigating the way patients make decisions about their prostate cancer care would provide insight into the improvement of such a program. The current study sought to clarify the factors that dictate the way patients with prostate cancer reach a decision about their treatment. The study investigated the way nurse navigators (NNs), health-care professionals utilized in the decision-making program through the Saskatoon Prostate Assessment Pathway (SPAP), impact patient experience.
The concept of a patient and health-care professional collaborating and coming to a decision about the patient’s treatment course is referred to as shared decision-making (SDM) (Charles, Gafni, & Whelan, 1997). SDM is meant to enable patients to use their autonomy in a way that helps them come to the decision most consistent with their values and concerns. Patients are given information by a health-care professional, usually a nurse or physician, to help them understand their treatment options along with the benefits and potential complications of each choice. Most patients wish to be educated about their condition and involved in decisions about their care (Channa & Siddiqi, 2008; Levinson, Kao, Kuby, & Thirsted, 2005). However, other patients prefer to have physicians make the final decision about treatment course (Channa & Siddiqi, 2008; Levinson et al., 2005). SDM is particularly relevant to prostate cancer treatment for two reasons. It is a complex treatment decision for patients and patients sometimes express regret about their treatment, often due to impairment in sexual and urinary function that occurs after certain treatments (Christie, Sharpley, & Bitsika, 2015). Using SDM may help to avoid patient regret over treatment decisions by enabling the patient to be an active participant in determining his treatment course. SDM has been reported to increase patient level of knowledge and decrease decision-making conflict (Myers et al., 2016). Additionally, SDM promotes a positive view of most treatment methods and reduces the rate of individuals who choose to undergo radical prostatectomy (Myers et al., 2016). It has been reported that radical prostatectomy is the option patients most regret (Christie et al., 2015). Therefore, SDM may be an important tool for reducing patient treatment regret. Previously, SDM was posited to rely solely on the patient’s individual preferences and on the scientific knowledge that the physician/health-care professional imparts upon the patient (Charles et al., 1997). This study evaluates this claim and potentially elucidates other complex factors involved in the decision-making process.
The setting for the present research was the Irene and Leslie Dube Urology Centre of Health. All participants involved in the current study were recruited by the NNs from PAP. The prostate cancer treatment decision-making program at PAP uses a NN to implement the principles of SDM. The role of the NN is to spend time explaining patients’ treatment options and responding to their concerns (Government of Saskatchewan Ministry of Health, 2013). In previous studies, NNs have been reported to reduce distress and increase cancer patient compliance (Swanson & Koch, 2010). Patients report their experiences with a NN to be beneficial in their care (Thygesen, Pedersen, Kragstrup, Wagner, & Mogensen, 2010). NNs provide continuity of care and improve communication between patients and their health-care team; both of which are important examples of high quality patient centered care (McMullen, 2013; Wagner et al., 2010). There has yet to be a study evaluating the mechanisms by which NNs are able to assist patients in their care.
Within Saskatchewan, there are four options for men with localized prostate cancer which include external beam radiotherapy, radical prostatectomy, brachytherapy, and active surveillance. Patients in the area who have an elevated PSA can be referred directly to a urologist or to the prostate cancer pathway for biopsy (Government of Saskatchewan, 2013). Patients are notified of their results by a NN and/or their general practitioner. If the patient is diagnosed with prostate cancer, regardless of whether they were referred through the pathway or directly to a urologist, an appointment is arranged with a NN to discuss their options (Government of Saskatchewan, 2013). After this appointment, the patient can be referred for treatment while others may desire further consultation with a specialist before moving on to treatment.
In this study, a qualitative approach was utilized and personal interviews were conducted to examine how prostate cancer patients engaged in the SDM process and the way in which NNs impacted this process. The intention of the current study was to understand how patients with prostate cancer experience SDM with the goal to improve the implementation of SDM programs.
Methods
Study Design
A qualitative research design was utilized to explore the experience of prostate cancer patients as they navigated the treatment decision-making process. The way in which patients perceived NNs was also investigated using this same qualitative approach.
Participant Characteristics
The eleven (n = 11) male participants in the study were recruited from PAP. Recruitment was halted at 11 participants because the researchers agreed data collection had reached saturation. All participants had been diagnosed with localized prostate cancer and had met with a NN at the Irene and Leslie Dube Urology Centre of Health. The mean age of the participants was 64.27 (R = 51–71). Out of the 11 participants involved in the study, five were from rural areas and six were from an urban center. The average length of time between diagnosis and interview was 22.64 days (R = 4–60). For more information on participant characteristics, see Table 1.
Participant Characteristics.

Participant Recruitment
The research team commenced with participant recruitment after receiving ethical and operational approval from Behavioral Research Ethics Board, University of Saskatchewan. All participants that met with NNs were given an information pamphlet about the study along with a consent form by the NN at the Irene and Leslie Dube Urology Centre of Health. Participants were consecutively recruited from June to August of 2017. All patients receiving information at the Irene and Leslie Dube Urology Centre of Health that met criteria for the study were asked to participate in the study. Those individuals that volunteered to partake in the study were later contacted via telephone by the interviewer to arrange an interview time. Participants consented verbally for the study after an oral consent form was read to inform them. This form was then filled out by the interviewer. All participants were offered a $50 honorarium for participation in the study.
Data Collection
Interviews were conducted via telephone by a lone researcher and the conversations were audiotaped. The interviews were semistructured and consisted of approximately 10 open-ended questions (see Appendix A for question list). Questions were aimed at identifying patient’s ideas about their decision-making process and about the NN. Average interview time was 22.98 min (R = 18.26–34.01).
Data Management and Analysis
During each interview, the interviewer recorded written notes. The interview recordings were later transcribed verbatim and then the data were analyzed using inductive latent thematic analysis (Braun & Clarke, 2007). Participant transcripts were read several times by the interviewer and then blocks of relevant participant responses were highlighted. These blocks of text were analyzed manually for initial codes. The initial codes were then grouped into larger potential themes. After this process was repeated for each transcript, all themes were recorded and consolidated into larger themes. Two researchers, in total, were involved in the coding process and when disagreement occurred, the final decision was deferred to the researcher who conducted the interviews.
Results
The results of the project are divided under the two research intentions. Part 1 focuses on the participants’ perspectives with regard to their treatment decision-making process, whereas Part 2 focuses on the participants’ experiences engaging with the NN.
Part 1: Participants Perspectives on Factors Involved in SDM
There were five overlapping themes; anxiety, practical concerns, maintaining normalcy, cancer narratives, and support system; found to contribute to the way men with prostate cancer made their treatment decisions. See Figure 1 for a visual representation of the themes and their interrelatedness.
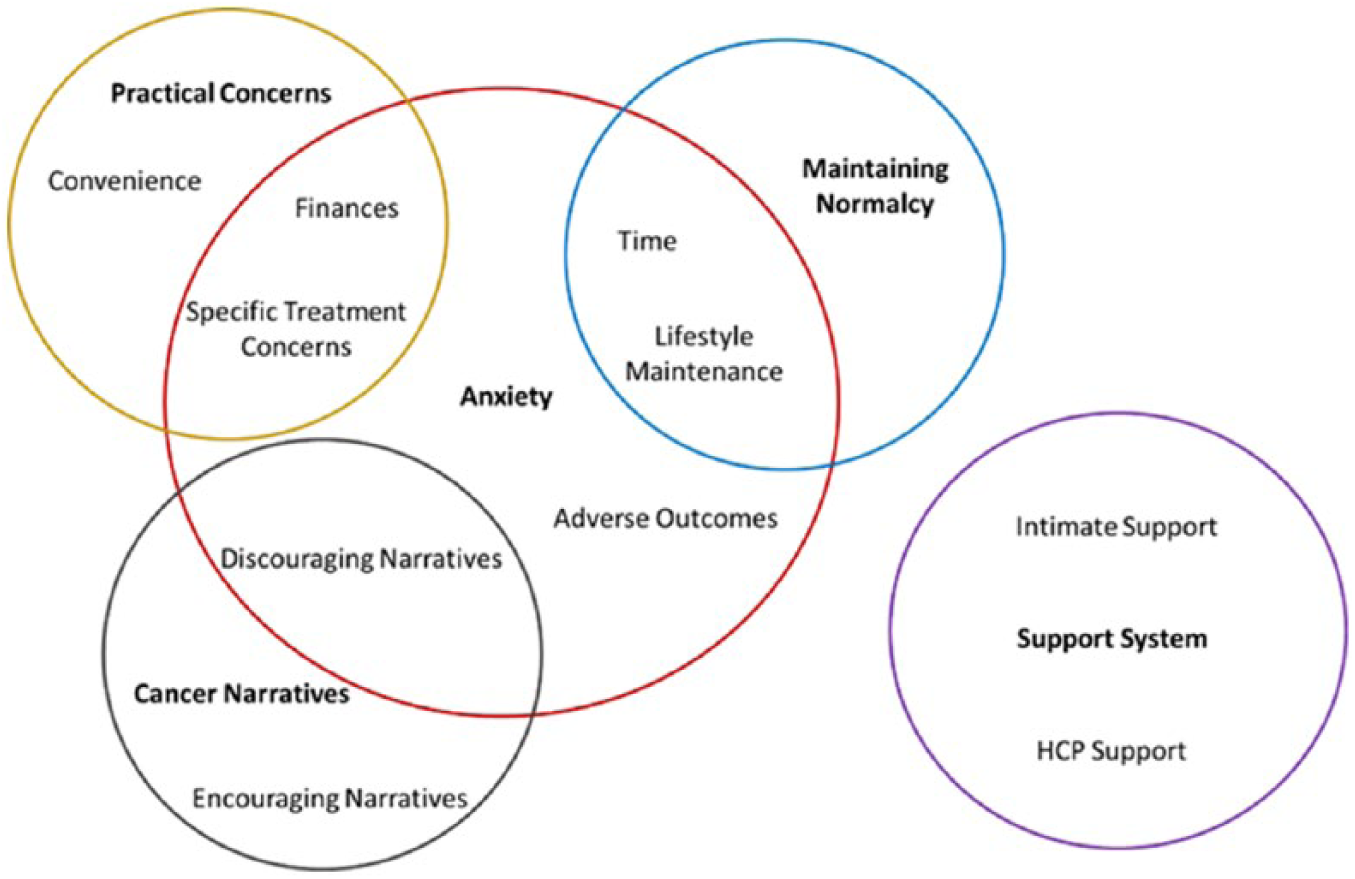
A visual representation of the themes and their relationships. Overlapping circles indicate convergence between themes and a specific subtheme.
Theme 1: Anxiety
The most salient theme participants expressed was anxiety about the treatment decision-making process. The theme of anxiety overlapped with several other themes in the study. However, it was also an independent theme in that participants expressed a fear of adverse outcomes associated with various treatment options. In general, participants attempted to choose treatment options that minimized their anxieties.
Subtheme 1: Fear of adverse outcomes
One common concern for participants was the negative potential outcomes of each treatment option. Four men were fearful of metastases and one of them specifically chose prostatectomy because they saw it as the option that most greatly minimized the risk of spread. As this participant expressed, the fear of metastasis was associated with the fear of death.
It’s been all right. Little bit concerned I guess […] I guess I’m just worried that it’s probably spread and I guess you worry about dying […]. Just thought that I have to do what I have to do and probably agreed that the best thing to do is surgery.
This participant expressed anxiety about choosing surgery, but this was outweighed by the anxiety from the prospect of death from metastases.
Surgery is a big step. I’m not looking forward to it, but I feel that’s what has to be done. I feel that if there is cancer there and it’s there I want it eliminated. And if it means, the consequences, I guess I’m willing to accept that, and that surgery, I guess.
Similarly, two participants were concerned about cancer recurrence and chose prostatectomy to minimize this risk.
My thinking at the time was that basically, if I had the surgery it’s out, it’s gone and I do not have to worry about it coming back at least in that area or that type of cancer.
One man was unable to come to a decision which seemed to result from the great amount of anxiety he felt about the side effects of any treatment option.
It doesn’t matter all the numbers that they shoot at you. In the end, you know, I’m pretty confident I know what the outcome’s going to be, and it’s a change in lifestyle. And that’s probably the biggest bridge for me to cross right now.
Another participant chose to undergo brachytherapy over radical prostatectomy because of his anxiety about the side effects of prostatectomy.
I want to do that pellet thing because I don’t want my prostate removed because I really don’t want to be wearing a diaper or anything like that.
Subtheme 2: Convergence from other themes
Finances were a source of anxiety. Two men worried about the money they would lose by being away from work for treatment options such as external beam radiotherapy. Participants also had unique anxieties about certain treatment options such as the accuracy of external beam radiotherapy or the safety of brachytherapy.
A common anxiety was the potential of prostate cancer recurrence and then being unable to remove it with prostatectomy if radiation therapy had previously been chosen.
The difference there was, if you have radiation, the option of surgery was eliminated. That was the, kind of the nail in the coffin once I found that out. So I thought, rather than going through that, and then not being able to have the prostate taken out if it had to be or the cancer was spreading from that prostate, radiation I didn’t think was the cure-all so. My thought was eliminate the problem, get rid of it, then hopefully that’s the end of it.
Having exposure to discouraging cancer narratives was a source of anxiety for two participants. In one man’s case, he had to be reassured by his health-care team that he was not going to die from his prostate cancer as had happened to someone else he knew.
I know a gentleman that got diagnosed in the fall with prostate cancer and didn’t make it to the next fall. That was on my mind, but I think the interaction I had with [my healthcare team] and my daughter clarified that it’s, you know, in my case that that’s not going to happen.
Discouraging stories from cancer survivors had the potential to increase anxiety about treatment options and dissuade participants from choosing those options. This was illustrated by one participant who felt mistrustful of radical prostatectomy since this method of treatment proved to be ineffective in removing his brother’s prostate cancer.
[My brother] had his whole prostate removed fourteen years ago, and it’s come back because he thought, they thought, they got it all, but obviously they missed a cell […].
This participant was disengaged from making a decision and wanted to speak to more specialists before making a treatment decision. He was leaning toward watchful waiting rather than an active treatment option such as radical prostatectomy. This participant’s wife and daughter had also passed away from cancer. He seemed resigned to the idea of death as the endpoint of cancer which, in addition to the negative narrative he heard about radical prostatectomy, may explain his reluctance to choose an active treatment method.
Participants also felt anxiety about choosing options that deprived them of their sense of normalcy. One participant expressed how his indecision about treatment options was related to how he felt all treatment options will lead to a change in his lifestyle. This seemed to provoke both anxiety and anger for him.
I’m just a little angry about, you know, what’s—how it’s going to change my lifestyle. […] It’s—you know, there’s a bit of fear going here. Like I said, it’s a lifestyle change.
This also was related to a fear of the side effects that may accompany certain treatment options, such as sexual dysfunction.
The prospect of a lengthy treatment course, such as with external beam radiotherapy, was very anxiety provoking for some participants.
I want to get this over with and get back to working and go on with my life. This seems to me the quickest and best situation to do that. I’ve never been out of work in my life and I do not know what it is going to be like to lay around until I am healed. I have no idea what it’s going to be like, none. I think that bothers me worse than the cancer.
There were also anxieties related to specific aspects of the treatment options. This was demonstrated by one participant who was very worried about the accuracy of external beam radiotherapy.
I think there’s a lot of body parts that they manage to get besides what they’re aimed at. I don’t care how they say how good it is. That’s my feeling. Finances were also a significant anxiety for some participants. I don’t know my financial, how things are going to work, and that bothers me, a lot.
Concerns over finances had the potential to dissuade participants from choosing treatments that would have a greater financial impact. This will be discussed in more detail later in this report.
Theme 2: Practical Concerns
It was evident that some patients decided against treatment options not because of their dislike of that treatment method, but instead because the method was not feasible for their situation.
Subtheme 1: Finances
A major concern among participants was how the treatment methods would impact their financial situation. There was the potential for participants to be unable to work during recovery or lengthy treatment options. One participant expressed this while discussing his concerns about undergoing radiofrequency.
I don’t know my financial, how things are going to work, and that bothers me, a lot […] the only thing that concerns me is financial. Everything else is in the hands of God and the doctors so.
Another participant was concerned about being able to continue with the manual labor of farming and how taking time for treatment would impact his livelihood.
You know, harvest is coming. And what if I got to go for this whatever’s going to happen, and you know, so you worry about stuff like that. Because I farm by myself, hey?
Five participants lived in rural communities and therefore traveling to a major center for multiple treatments, such as with external beam radiotherapy, was too expensive. Therefore, as one patient expressed, these treatment options were eliminated as possibilities.
The radiation thing where we go for, what is it, two months or whatever? And every day of the week. We live two and a half hours away. It would be different maybe if I lived in Saskatoon, but I don’t. And so then it would be a matter of renting a place and living in there for—and two months, and I don’t want to do that.
Subtheme 2: Specific treatment concerns
Some treatment options were eliminated immediately by participants because of particular aspects of the treatment option. Participants most often expressed concerns about radiation therapy (brachytherapy and external beam). One concern was that if patients underwent radiation therapy they were no longer eligible for surgery if there was a cancer recurrence in the future.
If I had the radiation, being as I am still relatively young, you know, there is still potential for to comeback fifteen years down the line or something like that. At that point, the treatment options, because I already would’ve had the radiation once, treatment options would be limited. So I decided based on my age and my health the best option would be to get rid of the prostate now and not have to worry about it down the road.
There were also concerns about the precision of external beam radiotherapy.
I definitely will not have the beam. I’ve ruled that one out. The beam radiation. […] Well in my humble opinion, humble uneducated opinion, I think there’s a lot of body parts that they manage to get besides what they’re aimed at. I don’t care how they say how good it is. That’s my feeling.
Participants who expressed dissent about other treatment options were more varied in their reasoning. One participant was against brachytherapy because he was skeptical about the safety of this treatment method.
I didn’t want the seeds implanted in my prostate, because I don’t think that’s a good thing to put uranium or whatever the hell it’s made of, into your body. So that was eliminated.
Yet another participant decided against any option requiring surgery because he was worried about how painful the treatments would be.
I didn’t want to be operated on, I wanted to try the radiation first. I hate pain.
Theme 3: Exposure to Cancer Narratives
All participants reported having experience with individuals who had cancer in the past. Eight participants reported having experience with individuals who had prostate cancer specifically. These narratives were either a source of encouragement or discouragement to the participants depending on the content expressed in the narrative.
Subtheme 1: Encouraging narratives
Exposure to individuals who were prostate cancer survivors and who had positive treatment experiences were encouraging for participants. All participants reported reaching out to family and friends who had gone through prostate cancer treatment. It was common for participants to report that they relied on prostate cancer survivors to inform their decisions regarding care.
I know a couple of people who have had that done, and I know a couple of people who have had surgery, and I also know people who have had radiation. So I’ve thought that what I would do is contact each of those fellows and discuss with them what they thought. If that was a good idea, or how they went about it, and so on.
One man heavily relied on the opinion of his friend when he decided to undergo radical prostatectomy. The friend expressed that the biopsy was worse than the surgery to remove his prostate which reassured the participant about his choice to undergo radical prostatectomy.
I had heard somebody else had had it, and they’re quite comfortable with it after they had did it. So, you know, that’s what I thought anyway was one of the better way to go.
A similar narrative was reported by a man who decided on brachytherapy.
The pellet thing [brachytherapy] just seemed like the best answer for me. […] there’s another guy I know in town here […] and he’s had that pellet thing, and he said it worked absolutely fine […] That’s why I’ve chose that way to go.
One participant preferred the information provided by survivors over the information given to them by the NN. This participant had made his treatment decision based on the cancer narratives of his brothers prior to his meeting with the NN.
It’s pretty well I already had it figured out before then. Just because, you know, if it was—if I was the first one I could understand that being an issue, but having all this information certainly from my brothers, […]. I have five brothers and four of them, including me, you know, have this.
Subtheme 2: Discouraging narratives
Three participants had members of their family or social circle who had died from cancer. This was related to participants having a negative view of their illness. This was especially apparent for one participant who had experienced multiple deaths from cancer within his family.
My wife has passed away. She’s been passed for twelve years. She died of breast cancer. […] I lost my daughter at twenty years old from stomach cancer. They—on my wife’s side they’ve got a bad gene. So it killed my daughter too. She died about five years ago.
When asked what life has been like since his diagnosis, the same participant gave a response which demonstrated his resignation toward his illness.
Oh it’s fine. You got to die some time.
Theme 4: Support Systems
All participants had some sort of support system that helped to make their treatment decisions. There were two types of support systems that participants cited throughout their decision-making process. This included intimate support; which came from friends, family, and spouses; and support from health-care workers.
Subtheme 1: Intimate supports
Participants reported that intimate supports encouraged them to continue actively seeking a decision.
My wife. The few friends that I’ve told. Some of my close relatives. They’re all helpful in, you know, sort of persuading me to move forward. Through encouragement. Talking to me.
In one case, the participant was persuaded away from watchful waiting by his wife’s desire for him to undergo an active treatment option.
Well my wife just thought I was going to do nothing about it. So she was quite happy when I chose [brachytherapy].
Some participants relied even more heavily on their spouses’ opinions. When one man was asked what he felt he needed in order to make his decision he replied: My wife and information from [the nurse navigator] […] My strength is in my wife that is just the way it is, maybe some people don’t but my support is all with my wife […] My wife loves me and we’re going to get through this together.
Family and spouses enabled patients to make a decision by being present with them as they journeyed through the prostate cancer pathway process. Family and friends were sources of affirmation for the patient.
Well, I had support with my wife […] everybody else is sympathetic and they agree with the decision I made.
Subtheme 2: Health-care support (family practitioner, nurse navigator; affirmation of treatment choice)
Nine participants expressed the desire to have their treatment choices affirmed by a health-care professional. In most cases, it was sufficient for the NN and/or their family physicians to have played a role in the decision. Four participants reported their conversations with the NN to be reassuring and calming.
I had a wonderful conversation with [the NN], and, you know, I must give her credit. She’s very knowledgeable and quite capable of keeping a calm lid on things, describing the situation.
Further ratification, from a urologist or oncologist, was desired for six participants before the participants felt comfortable making a definitive decision. However, only two of these participants considered themselves to be undecided about their treatment course.
I figure I’m alright until, like I say, until I see this urologist specialist and then I’ll know, you know, I’ll make a more informed decision then.
When one participant was asked if he had made a treatment decision, he expressed that he needed to hear from an oncologist before deciding between two options.
Getting closer. Not there. I’m—I see an oncologist on Monday to pursue questions about the radiology, and I’m on the fence equally I would say between surgery, or the brachytherapy.
One man seemed to hope that the specialist would explicitly tell him which option to choose.
It all comes back to this doctor, you know, and depending on what he has to say and I’m sure he’ll have his point of view on what I should do.
Four men just wanted affirmation that they made the correct treatment choice.
So I kind of felt that, depending on what this specialist says, I’ll probably leave it and just, you know, do my bloodwork and stuff like that, and just go with the recommendations of the doctors.
Two men preferred privacy and did not want to discuss their options with their family or friends. These individuals relied solely on the NN and specialists to make their treatment decisions.
I didn’t really have any [support]. I just, you know, it’s something I didn’t really want to spread around and tell people, so I’ve kind of kept it to myself. So I haven’t really asked anyone for support […] I realize what’s going on, and you know, I don’t need anyone else’s advice. So I’m pretty clear on what I’m going to do. Like I say, it just depends on what this specialist says which will tell me totally.
Four participants relied on their general practitioners for advice regarding their treatment.
My old doctor said the success rate is good with this [brachytherapy] if you get it early and do it early. So this is early. So that’s why and how I made my decision.
Three participants consulted with family members who were also health-care professionals. The opinions of these supports, which had the dual role of being an intimate support and a health-care support, were held in high regard.
My family, I have an RN who’s my sister’s RN, so she, well, was one of the first people that I talked to.
Theme 5: Maintaining Normalcy
A preoccupation for participants was that active treatment posed a disruption in their lives. This usually meant that treatment would take up a significant amount of time and caused a disruption in their daily routine. The other main concern was that the side effects of treatment would cause a permanent change in their lifestyle.
Subtheme 1: Time
A highly salient theme expressed by participants was concern about the amount of time that certain treatments would take. Participants felt that certain treatment options, especially external beam radiation therapy, which requires treatments over the course of approximately 8 weeks, would cause too much of a disruption in their lives. Those that expressed this wanted a treatment that would allow them to continue with their lives as quickly as possible. There was a sense of urgency among these participants as they wanted to expediently deal with their cancer. One participant expressed these thoughts when discussing why he chose brachytherapy over other treatment options: It’s in days instead of weeks. I’m not going to be tied up for five days a week for eight weeks. Or, going under the knife, I will be restricted going to a procedure that will be two days, maybe three in observation. [Brachytherapy] is more feasible and yeah, lets me live my life on my schedule instead of being tied down for eight weeks or going under the knife.
Another participant distinctly expressed a sense of urgency when discussing why he chose radical prostatectomy: My thought was eliminate the problem, get rid of it, then hopefully that’s the end of it.
Subtheme 2: Lifestyle maintenance
One man was concerned that their life was not going to be the same after treatment. He seemed to accept that a lifestyle change was unavoidable.
I’m just a little angry about, you know, what’s—how it’s going to change my lifestyle. […] It’s—you know, there’s a bit of fear going here. Like I said, it’s a lifestyle change. That’s the biggest hiccup for me is that, you know, coming to acceptance of the lifestyle change.
This participant appeared to be concerned with the prospect of sexual dysfunction that is associated with many of the treatment options.
I mean, at my age we’re certainly not sexually active. I mean, we still have intimacy, not very often. And I would say that that’s the part that’s affecting me right now.
Seven men were concerned with trying to minimize possible lifestyle changes by choosing the least invasive option. However, the men who expressed this idea did not choose active surveillance. These men may have been attempting to find a balance between active treatment to reassure themselves about the course of their illness and the maintenance of their lifestyle. For two men, the least invasive treatment choice was brachytherapy.
It’s really surgery, but it’s really not so much. So I prefer that idea. Especially when the nurses at the urology department there at [hospital] said that there’s no indication which particular type of treatment is better than the other. So I prefer the one that’s not as aggressively—I don’t want really surgery so much. I’m—I’ve decided probably the least invasive. I don’t know. Is it? Well it’s invasive, but I mean, rather than radiation. I really don’t want to be in getting radiated for two months. If you can just have some pellets put in there.
Part 2: Patient Perception of the Nurse Navigator’s Role
When participants were asked about their interactions with the NN they consistently reported two major ideas. Participants reported that NNs helped them to move away from indecision and gain knowledge about their illness. NNs were reported to be a source of reassurance and support for participants which helped them to make their decisions.
Theme 1: Previous Indecision and Increased Understanding
When asked about their decision-making ability prior to the NN meeting nine participants reported that they were completely undecided. For example, this participant stated: Yeah. I was really at no decision. I was in turmoil, and confused, and certainly nowhere near a decision at that point.
Another participant cited a lack of information as the source of his indecisiveness.
I was really kind of no-where up till when I met with [the NN]. Because I knew that I had it, I did not know how bad it was, or what the score, the score was, whether it was advanced or low-grade minor, or whatever you want to call it. So, up until I started getting all the information from the nurse practitioner and that, I hadn’t really formed any decision or potential best course action at that point.
Ten participants reported that their meeting with the NN increased their understanding of their illness and treatment options.
[The NN] explained all the different options to me, and how just different steps and how different things were I was no it was—I’m not going to say it made it easy but it made it more informed and good on why I lean that way, and yeah.
For the two individuals who were not able to make a decision after the NN meeting, it still served to move them closer to a decision point.
Quite frankly, not near a decision bef—yeah. I mean, I was doing the reading and the research, and just, I was on—I wasn’t even on the fence. I just didn’t know what to do. I’m getting closer to a decision.
Ideas about why the meeting was informative included that the NN gave them knowledge in small easy to understand portions, the knowledge was given in an organized way, and since participants were given materials to go home with, information about all of their options was easily accessible.
[…] when [the NN] explained all the different options to me, and how just different steps and how different things were […] I’m not going to say it made it easy but it made it more informed and good on why I lean that way, and yeah […] Well they narrowed the choices down to what my options were so it made the decision absolutely a lot simpler because the information that they’d given me was all right in front of me and with discussions and everybody around it was very simple, and very good.
Two participants reported that they appreciated it when the NN gave them information that was specific to their situation.
They laid out exactly at what level my cancer was kind of rated, or graded at. And based on the grading what the potential treatments were, what treatments were available or optional, and what treatment were kind of not on the table. Actually, for mine because of the grade of it, all options were pretty well on the table. If it were to be a higher grade, these options would have not been.
Participants consistently reported that being informed of the benefits and ramifications of each treatment option was helpful in clarifying their options.
[…]she did thorough job in describing what the options were, with the ramifications and the logistics and all that kind of stuff. So it’s pretty straightforward decision as far as I’m concerned.
Theme 2: Reassurance (Empathy, Trust)
NNs played an important role in decreasing participant anxiety by being empathetic toward the participants and offering them reassurance about their illness course. For example, one participant was concerned that they were not going to survive their cancer and the NN was able to assuage this concern.
Well, the first day was pretty rough, but after we talked to the nurse, and she said it could be cured or pretty big chance it was because it isn’t progressive […] She told us things like what could go wrong and what the options are and gave us half the thought that, hey, this could be beat. Because they caught it early there’s a good chance it could be beat.
Participants expressed that the NN thoroughly explained their situations on a personalized level and that having this information specific to their situation eased their anxiety.
[The NN] was delightful to talk to. I just, you know, put me at ease a little bit, but you know, it’s nothing to laugh at, but I’m, you know, I’ve got to deal with it.
The NN interaction was also reassuring for patients because they viewed the information given to them by the NN to be reliable.
[The NN], the information from her was just, you know, clear and it wasn’t biased in any way because she hasn’t had to do it herself, so yeah […] So I think that what she told me, I believe what she told me is true, so I think that all of the avenues are available.
Discussion
The intention for this study was twofold: to examine the factors that contribute to the decision-making process of men with prostate cancer; and to investigate patient perception of the NNs’ impact on their decision-making process. Five themes were identified that influenced decisions regarding prostate cancer treatment: level of anxiety, practical concerns, exposure to cancer narratives, support system quality, and desire to maintain normalcy. While other factors influenced which choice was made about their treatment, practical concerns seemed to dictate the options that were eliminated.
The most salient theme expressed by participants in the study was anxiety. Many of the other themes converged with this central theme. Participants were anxious about loss of income, the methodology of certain treatments, the recurrence of their prostate cancer, and the inability to maintain their current lifestyle after treatment. The participants feared adverse outcomes associated with specific treatment options. Exposure to negative cancer narratives increased the patients’ anxieties about certain treatment options. This led them to choose options aside from the ones in the negative cancer narratives.
The idea of anxiety influencing treatment decisions is supported by past studies demonstrating that higher levels of anxiety can cause men to seek out active and more invasive treatment options sooner than is medically necessary (Latini et al., 2007). Following treatment, men who undergo radical prostatectomy have lower levels of anxiety compared to those who opted for active surveillance (Dale, Bilir, Han, & Meltzar, 2005). Nelson et al. (2005) surmised that decreased anxiety levels after surgery were due to patients’ desires to be completely rid of their cancer and that they felt radical prostatectomy gave them the best chance of this. SDM programs lower the number of men who choose radical prostatectomy, arguably the most invasive treatment option, as their treatment path (Myers et al., 2016). Additionally, this is the treatment option most regretted in later years after treatment. Therefore, SDM programs may mitigate this anxiety and help patients to make a choice that is more congruent with their future lifestyle goals (Stacey et al., 2017). If so, this means that SDM programs will spare patients invasive surgeries and the adverse outcomes associated with this option. It may also reduce health-care costs by avoiding unnecessarily invasive procedures (Lee & Emanuel, 2013).
Participants who desired to maintain normalcy wanted a treatment that would let them return to their daily lives as quickly as possible. Another component of maintaining normalcy was the desire to maintain the lifestyle participants had prior to their diagnosis. Although most men did not elaborate on what they meant by a change in lifestyle, one participant expressed that he was primarily upset by the likelihood of sexual dysfunction with the active treatment options. Men wanted to choose the least invasive option, but these men also seemed to balance this with the desire to ease their anxiety about recurrence by choosing an active treatment option. Many of the participants seemed to ignore that active surveillance was the least invasive treatment option and instead opted for the least invasive active treatment option. In a study on decision-making in breast cancer patients, Charles, Redko, Whelan, Gafni, and Reyno (1998) surmised that participants’ desires to choose active treatment stemmed from a desire to be in control of their cancer, reduce uncertainty about disease progression, and to reduce guilt if there were a recurrence. This is consistent with the results of the current study whereby participants’ decisions also seemed to be driven by a desire to reduce anxiety about cancer spread/recurrence.
The second part of the study, which investigated patients’ perception of the role of the NNs during the SDM process, found that NNs reduced indecision and increased participants’ understanding of their illness and their treatment options. Participants appreciated hearing the benefits and potential side effects of each treatment option. It is important that patients feel well-informed about their treatment decisions as lower levels of knowledge are associated with greater cognitive dissonance when making decisions (Kaplan et al., 2014). This in turn lowers effective decision-making (Kaplan et al., 2014), which may increase regret and dissatisfaction after treatment (Christie et al., 2015). NNs were also a source of reassurance for participants. They decreased participants’ anxiety by expressing empathy and reassuring them about the course of their illness. Participants felt comfortable that the information they received from the NN was informed, true, and unbiased. Therefore, receiving the information from the NN was reassuring for the participants and they felt secure in making decisions based on this information. In turn, by reassuring the participants, the NNs were decreasing the patient’s anxiety levels. Since lower anxiety levels are associated with better decisions, interaction with the NNs was helping the participants to make better, or at least more informed, decisions. Past research has reported that NNs provide better quality of care for patients by providing continuity of care and improving communication (McMullen, 2013; Swanson & Koch, 2010; Thygesen et al., 2010; Wagner et al., 2010). The results of the current study are coherent with this research and therefore add to the growing body of literature showing that NNs are beneficial in the care of patients making complex care decisions.
The results of this study illustrate that patients often have specific and individualized concerns that guide their treatment choices. This calls attention to the need for personalized medicine, especially in situations where patients may need to make complex decisions regarding their care. However, it also illustrates the commonalities by which patients make their decisions in this context and presents the opportunity for health-care professionals to anticipate these needs and address them. Therefore, the results of the current study could be used to guide the revision and implementation of SDM programs, especially for those regarding prostate cancer. Based on this study, SDM programs could focus on easing patient anxiety about decision-making by providing patients with clear information that is broken down into easily manageable steps. Information provided to patients should likely be clearly presented with the harms and benefits of each treatment option explained thoroughly. Narratives of patient experiences with each treatment method could also be incorporated into the information that patients receive. This may act to neutralize the narratives that participants have heard previously. These ideas are also supported by the International Patient Decision Aid Standards (IPDAS) checklist (Holmes-Rovner, 2007) which includes recommendations on the design and implementation of decision aids. The IPDAS guidelines state that this must include a description of the health condition, options, procedures, harms/side effects of options, and chances of positive negative outcomes. It is also recommended that if narratives are going to be used in the aid that a range of positive and negative narratives must be presented.
One important aspect the current study revealed was the patients’ desires to feel as though the information they received was coming from a trusted and unbiased source. Past research has identified that when prostate cancer patients are uncertain of a decision when consulting a urologist, the decision is subject mostly to the will of the physician (Scherr et al., 2017). This means that the decision is usually made based on medical factors or personal preferences of the physician rather than on the values and goals of the patient (Scherr et al., 2017). This illustrates the need for an intermediate health-care professional, such as a NN, to aid in the decision-making process.
Limitations
Face-to-face interviews were not possible for this study because many of the participants were from rural areas. Therefore, to accommodate participants that did not live near the treatment center, interviews were conducted via telephone. This may pose a limitation as participants may have been more forthcoming with their responses when interviewed in person (Aquilino,1994; Greenfield, Midanik, & Rogers, 2000). However, men in particular may feel anxious in face-to-face interviews, especially when there is emotional content elicited by the interview questions (Affleck, Glass, & Macdonald, 2012). Therefore, since there is a barrier between the interviewer and interviewee during telephone interviews, men may feel less anxious and more willing to speak about their experiences.
At the time of the interviews, the participants were not all at the same stage of the decision-making process. Some of the participants had firmly decided, others were near a decision but needed further health-care professional affirmation, and some were completely undecided. Therefore, some responses may have changed once they were further along in their decision-making process.
Future Directions
Since the major limitation of the current study was that participants were not at the same stage with their decision-making, future studies should attempt to contact patients after treatment decisions have been made. It would also be illuminating to speak to patients after treatment to investigate the role of anxiety in prostate cancer treatment by asking patients about their anxiety pre and post treatment. This would quantify the different levels of anxiety that patients feel when undergoing the various treatment options and would further clarify the effect of anxiety on the decision-making process.
Conclusions
The results of the current study add to the existing literature surrounding SDM in complex medical situations and to the growing body of literature supporting the use of NNs in this context. It provides further insight into the way men with prostate cancer make decisions regarding their care. Based on the results of the current study, patients’ level of anxiety, degree of practical concerns, desire to maintain normalcy, exposure to cancer narratives, and quality of their support system should be taken into consideration during the formulation of SDM programs. The necessity of including NNs in the SDM process was also illuminated in this study and demonstrates that their use in SDM programs should be encouraged.
Footnotes
Appendix A. Interview Guide
Acknowledgements
We thank the Leslie and Irene Dube Urology Centre of Health and the nurse navigators of the Saskatoon Prostate Assessment Pathway for volunteering their time and assisting in our study.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Funding for this project was provided by the College of Medicine, University of Saskatchewan.
