Abstract
To better understand the health status of men in the United States, this study aimed to assess the association of hardship on the presence of and pain severity among men 50 years of age and older. Cross-sectional multivariate logistic regression analyses were conducted using the 2010 wave of the Health and Retirement Study (N = 3,174) to assess the association between four hardship indicators and the presence of pain and pain severity among this sample of older men.
Results suggest that the association between the presence of pain and hardship was statistically significant across all four indicators: ongoing financial hardship (CI [1.05, 1.63], p < .05), difficulty paying bills (CI [1.42, 3.02], p < .001), food insecurity (CI [1.46, 3.15], p < .001), and not taking medication due to cost (CI [1.06, 1.66], p < .05), even after adjusting for all demographic factors.
The associations between pain severity and ongoing financial strain (CI [1.23, 2.83], p < .01) and difficulty paying bills (CI [1.02, 3.18], p < .05) were statistically significant. Results also indicate that education was a buffer at all levels. In addition, the interactive effect of hardship and Medicare insurance coverage on pain severity was significant only for ongoing financial strain (CI [1.74, 14.33], p > .001) and difficulty paying bills (CI [1.26, 7.05], p < .05). The evidence is clear that each hardship indicators is associated with the presence of pain and across some of the indicators in pain severity among men aged 50 and older. In addition, these findings stress the importance that Medicare insurance plays in acting as a buffer to alleviate some of the hardships experienced by older men. These findings also highlight the association between the presence of pain and pain severity for the overall quality of life, health outcomes, and financial position of men in later life.
The rise of economic insecurities leading to experiences of hardship, paired with the prevalence of the disease of chronic pain in the older adult population, is a growing public health concern (Siddall & Cousins, 2004). While positioned as a serious health outcome, pain has traditionally been defined as a physiological response to disease and tissue damage, and is often classified into different categories (e.g., neuropathic, nociceptive) based on its origin (Hadjistavropoulos & Craig, 2004). According to the Centers for Disease Control (CDC, 2015), more than half (54%) of all persons in the United States are diagnosed with at least one chronic disease, with three out of every four adults 65 and older reporting two or more medical illnesses. Yet, although accepted as a symptom of a disease diagnosis or injury, the recurrence of pain can also be considered a disease in itself. Existent data suggest that while many patients are diagnosed with a primary pathology (e.g., arthritis, diabetes), the changes to the peripheral nervous system may have demonstrable secondary pathology. Thus, the individual may then develop persistent pain as a disease, whereby it meets the criteria for a disease entity having its own pathology and symptoms (Cousins, 2007; Siddall & Cousins, 2004). This secondary pathology may have implications in understanding the association of pain and other chronic medical conditions.
Data suggest that the total health-care costs for both men and women for certain chronic pain-related medical conditions, ranged from $45.7 billion for moderate pain to $89.4 billion for severe pain, with incremental health-care costs for joint pain, being the most prevalent, ranging from $261 billion to $300 billion annually (Gaskin & Richard, 2012). While the direct outcomes of pain impact the functioning of a patient (i.e., mobility, productivity, disability), they also result in greater costs for the health-care system. Furthermore, there are also mounting indirect costs related to chronic pain, such as loss of employment and income.
Job loss and declining economic status are stressful life events regardless of circumstance. Lower economic status has been reported to be associated with increased pain frequency and severity (Johannes, Le, Zhou, Johnston, & Dworkin, 2010) and individuals with lower socioeconomic status (SES) tend to be most vulnerable to experiencing some form of hardship or financial strain (Blank & Burstrom, 2002). Although study findings have established a link between SES indicators such as education, income, occupation, and chronic pain (Portenoy, Ugarte, Fuller, & Haas, 2004; Saastamoinen, Leino-Arjas, Laaksonen, & Lahelma, 2005), SES only partially explains this relationship. Hardship, also conceptualized as financial stress or economic stress, is another recognized SES indicator (Drentea, 2000). The broader category may include indicators such as an individual’s ability to pay bills, ongoing financial stress, food (in)security, and medication needs (Tucker-Seeley, Marshall, & Yang, 2016). Although a relatively new area of inquiry, there is, a growing body of gerontological research examining the relationship between various forms of hardship and pain in general. Research by Rios and Zautra (2011) reported that financial hardship and daily financial worry were associated with increased vulnerability to pain.
Previous findings examining gender differences suggest that women were more likely to report higher health-care expenditures than men (Gaskin & Richard, 2012). Yet despite the growing literature documenting the economic impact of pain among women (Rios & Zautra, 2011), there remains a lack of data underscoring influence of economic hardship among older men. In assessing this relationship, it must be recognized that there is considerable heterogeneity among the adult gendered population, suggesting variability in the pain experience. In describing these differences, it has been argued that sex hormones may have a significant impact as factors that influence pain sensitivity and perceptions. Similarly, there are reported sex differences in clinical acute and chronic pain. Bartley and Fillingim (2013) further cited that identified biopsychosocial mechanisms may start to define these differences in response to pain (and treatment). Despite these findings, exploration is needed to determine if these hormones do indeed have an impact, and if so, how (Bartley & Fillingim, 2013; Fillingim, King, Ribeiro-Dasilve, Rahim-Williams, & Riley, 2009). What has been, and is often concluded, is that there are significant inconsistencies in reporting these differences. Therefore, in recognizing the difficulty in pain assessment, it may be necessary to initially understand the differences that occur within a given group before making inferences between groups.
While pain, gender (and sex), and hardship have received overwhelming attention, evidence defining the association between pain and specific hardships among men is less evident. To contribute to the understanding of this relationship, this study aimed to first examine the association of four indicators of hardship and pain presence and severity, and second, to assess whether having Medicare insurance coverage buffers the effect between hardship and the presence and severity of pain among a nationally representative sample of older Hispanic, non-Hispanic White, and non-Hispanic Black men 50 and older.
Three hypotheses guide this investigation: (a) hardship among men is associated with the presence of pain and/or increased pain severity, (b) in men, a positive association between hardship and presence of pain and/or increased pain severity is retained after controlling for relevant demographic factors including age, income, education, and marital status, and (c) with men, the impact of hardship on pain presence and/or severity is reduced with Medicare coverage compared to those reporting no coverage; perhaps having insurance coverage may reduce the stress associated with hardship. To our knowledge, this is one of a very few studies assessing these relationships among older men, which is a strength of this study.
Methods
Data Source and Procedures
Data used for this study were taken from the Health and Retirement Study (HRS), a nationally representative sample with a focus on the health, economics, demographics, and retirement processes of noninstitutionalized U.S. adults aged 50 years and older. Data for the HRS are collected bi-annually and has been collected since 1992. In 2006, a self-administered questionnaire that was left with respondents upon the completion of an in-person core interview was added to HRS. These are referred to as Leave-Behind Questionnaires. The purpose of these questionnaires was to collect additional information about the respondent’s psychosocial experiences without adding to the interview length (Smith et al., 2013). The HRS is a multistage area probability sample of U.S. households, with oversampling for African Americans, Latinos, and Florida residents.
Sample
Analyses included a subsample of men 50 years and older (from the 2010 wave of the HRS) who completed the leave-behind questionnaire. The questionnaire asked participants some of the financial hardship questions included in this study. Psychosocial information was obtained at each biennial wave of the HRS and information was included from a random 50% of the core panel of participants who completed the face-to-face interview (Smith et al., 2013). Fifty respondents were excluded from the analyses due to missing data. The final unweighted sample for subsequent analyses included 3,203 respondents (men). Additional information describing HRS in greater detail can be found elsewhere (Sonnega et al., 2014; Levy, 2015, p. 58; Heeringa & Connor, 1995; Juster & Suzman, 1995).
Measures
Dependent variable: pain
Pain is the dependent variable and it was measured using two items assessing a respondent’s presence of pain and pain severity. The presence of pain was measured with the question “Are you often troubled with pain?” Responses were dichotomized (no = 0; yes = 1). Pain severity was assessed by asking “How bad is the pain most of the time?” Responses to the pain severity question ranged from mild, moderate, or severe. The responses about pain severity were dichotomized: low levels of pain (mild/moderate = 0) and high levels of pain (severe = 1).
Independent variable: hardship
Hardship is the independent variable and was conceptualized using four indicators: (a) ongoing financial stress; (b) food insecurity; (c) taking less medications due to cost; and (d) difficulty paying bills. Ongoing financial strain was assessed with a one-item question asking, “If you ever had current or ongoing financial problems that have lasted 12 months or longer, how upsetting has it been to you?” Responses were dichotomous: absence of ongoing financial stress (no, didn’t happen = 0) and presence of ongoing financial stress (yes, but not upsetting/yes, somewhat upsetting/yes, very upsetting = 1). Food insecurity was operationalized with the question “In the last 12 months, did you ever eat less than you felt you should because there wasn’t enough money to buy food?” Responses were either (no = 0; yes = 1). Taking less medications due to cost was assessed by asking the question “At any time, have you ended up taking less medication than was prescribed for you because of the cost?” responses were either (no = 0; yes = 1). Difficulty paying bills was operationalized with a Likert-type question “How difficult is it for you to meet monthly payments on your bills?” Responses were dichotomized as absence of difficulty paying bills (not at all difficult = 0) and presence of difficulty paying bills (not very difficult/somewhat difficult/very difficult/completely difficult = 1).
Control variables: age, income, education, and marital status
All controls included for this analysis were demographic variables. These included age as a continuous variable ranging from 50 to 99 years, annual household income as a continuous variable ranging from $0.00 to 1,330,000. Education was assessed as a categorical variable (high school graduate = 0; less than high school graduate = 1; some college or more = 2), and marital status measured as a categorical variable (married = 0; separated/divorced/widowed = 1; single = 2).
Moderator variable: Medicare insurance coverage
Medicare Insurance Coverage Part A was measured with a single-item question, “Are you currently covered by Medicare health insurance?” Responses to this question were recoded (no = 0; yes = 1).
Statistical Analysis
Percentages, means, and standard deviations were calculated for pain (presence and severity), hardship, demographic characteristics, and Medicare insurance coverage. Since the outcome variables were dichotomous, multivariate logistic regression was used. All statistical analyses were conducted using STATA 14.0 (2015). A series of bivariate logistic regression models were conducted to test the association of hardship with the presence and severity of pain. Then a series of multivariate logistic models were performed to test the relationship between hardship and pain presence and severity, while controlling for demographic factors. The final model assessed the moderating role of Medicare insurance coverage in the association between hardship and pain (presence and severity).
Results
Differences in Levels of Pain Among Men
Table 1 provides demographic information about men who had no pain, mild/moderate pain, and severe pain levels in the sample. The average age of men with mild/moderate pain was 65.2 years (SD = 7.8) and men with severe pain was 64.5 (SD = 9.6). Participants with mild/moderate pain had a mean annual household income of $74,151 (SD = $62,610) and men with severe pain had a mean annual income of $39,792 (SD = $33,465). Compared to men who had a high school education or more, men with less than 12 years of education experienced almost 31% of mild/moderate pain and almost 33% of men experienced severe pain. Over 74% of the men experiencing mild/moderate pain were married/partnered, and 59% of men with severe pain were married/partnered. Among men with difficulty paying bills, almost 81% reported having severe pain. Twenty-one percent of men who had food insecurity reported having severe pain. Almost 69% of men with ongoing financial hardships reported having severe pain. Among men who took less medication due to cost, almost 25% reported severe pain. Additional demographic information is reported in Table 1.
Sample Characteristics of All Men (N = 3,174).

Note. Sample counts (N) are unweighted. Percentages and means are weighted by HRS individual-level sampling weights. HRS = Health and Retirement Study.
Bivariate Regression Analysis of the Association Between Hardship and Pain
Table 2 reports bivariate regression results for the presence of pain by each hardship variable respectively. Findings suggest that men who had ongoing financial hardship had a 1.4 greater odds of having trouble with pain (CI [1.13, 1.70], p < .01). Men who experienced food insecurity had a 2.5 greater odds of having trouble with pain (CI [1.78, 3.30], p < .001). Findings also suggest that men who had taken less medication because of cost had a 2.5 higher odds of having trouble with pain (CI [1.69, 3.56], p < .001). Among men who had difficulty paying bills had a 1.5 greater odds of having trouble with pain (CI [1.19, 1.76], p < .001). Also in Table 2 are bivariate regression results for severity of pain by each hardship variable respectively. Among men who had ongoing financial hardship had a 2.7 greater odds of experiencing severe pain (CI [1.47, 3.46], p < .001). Men who experienced food insecurity had a 2.6 greater odds of experiencing severe pain (CI [1.46, 4.62], p < .01). Findings suggest that men who took less medication due to costs had a 2.3 great odds of experiencing severe pain (CI [1.31, 4.03], p < .01). Findings also suggest that men who experienced difficulty in paying bills had a 2.6 greater odds of experiencing severe pain (CI [1.443, 4.52], p < .01).
Bivariate Associations Between Hardship and Pain.

Note. (1) Sample counts (N) are unweighted. (2) Estimates are weighted. Models include a constant term. 95% confidential intervals are in brackets. (3) Odds ratio is the proportion between the odds of pain in those with and without each hardship variable.
p < .05. **p < .01. ***p < .001.
Multivariate Regressions Analysis of the Association in Pain and Hardship
Multivariate analyses adjusting for all demographic factors are found in Table 3. It suggests that men who experienced food insecurity had a 2.1 greater odds of experiencing pain (CI [1.42, 3.02], p < .001). Men who had taken less medication due to cost had a 2.1 greater odds of having trouble with pain (CI [1.46, 3.15], p < .001). Also in Table 3 are findings suggesting that men who experienced ongoing financial strain had a 1.9 higher odds of experiencing severe pain most of the time (CI [1.23, 2.83], p < .01). Men who experienced difficulty paying bills had a 1.8 higher odds of experiencing severe pain most of the time (CI [1.02, 3.18], p < .05). Additionally, men who had some college or a college degree had lower odds of experiencing severe pain compared with those who had been to high school only. This was significant for all four models.
Multivariate Regression Analysis of the Association Between Hardship and Pain.

Note. (1) Sample counts (N) are unweighted. (2) Estimates are weighted. Models include a constant term. 95% confidential intervals are in brackets. (3) Odds ratio is the proportion between the odds of pain in those with and without each hardship variable. (4) This model is adjusted for all demographic factors.
p < .05. **p < .01. ***p < .001.
Multivariate Regressions and the Moderating Effect of Medicare Insurance
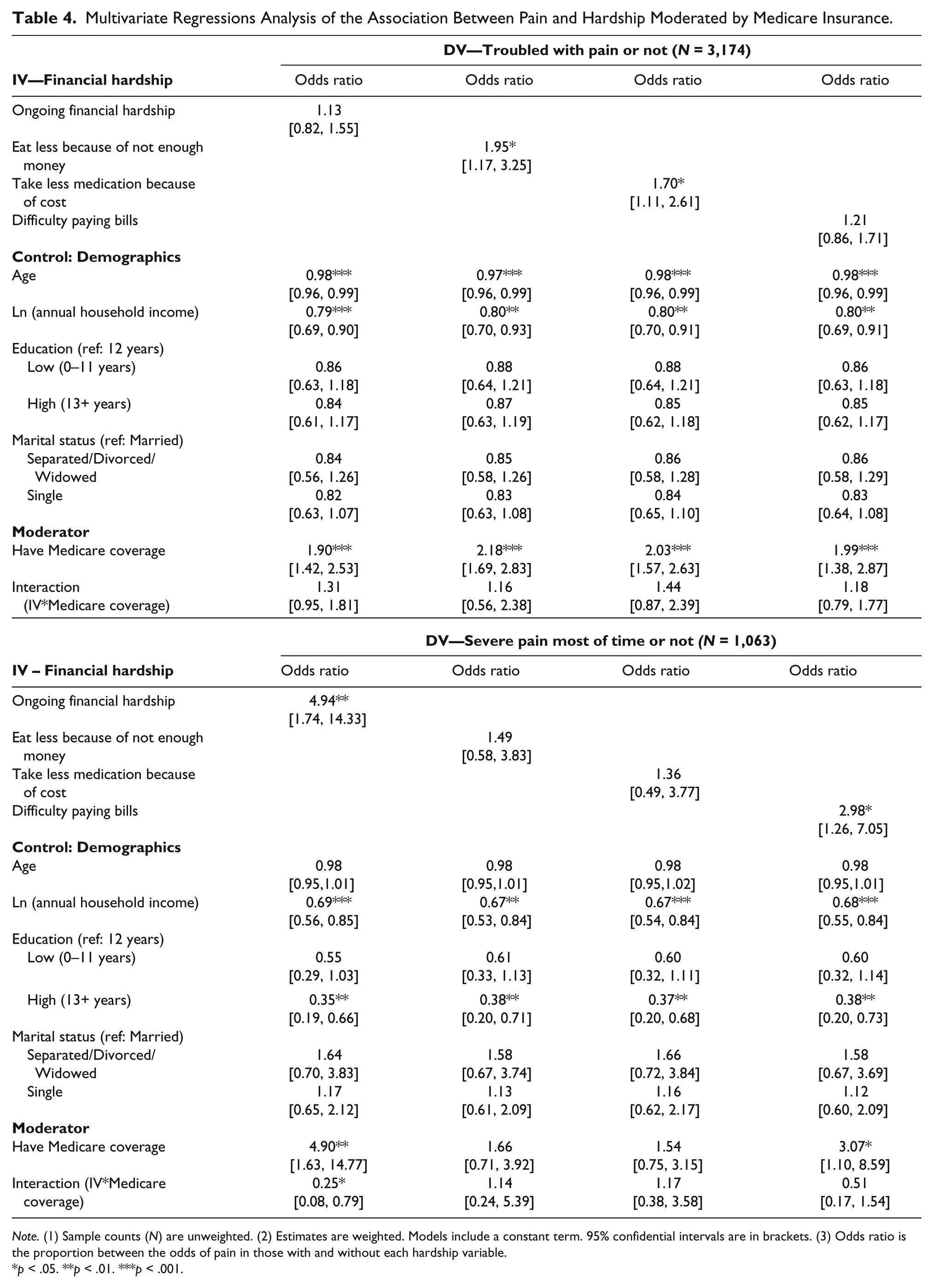
The first part of Table 4 provides results for men who are often troubled with pain and the effect of having Medicare insurance coverage. Results suggest that men who experienced ongoing financial hardship had a 1.1 odds higher of having trouble with pain compared to men who did not experience ongoing financial hardship controlling for all other covariates (CI [0.82, 1.55], not significant). Men who had Medicare coverage had a 1.9 higher odds of having trouble with pain compared to men who did not have Medicare coverage controlling for all other variables (1.42, 2.53, <.001). Men who experienced ongoing financial hardship and who had Medicare coverage had a 1.3 high odds of having trouble with pain compared to men who had ongoing financial hardship and did not have Medicare coverage (0.95, 1.81, not significant).
Multivariate Regressions Analysis of the Association Between Pain and Hardship Moderated by Medicare Insurance.
Note. (1) Sample counts (N) are unweighted. (2) Estimates are weighted. Models include a constant term. 95% confidential intervals are in brackets. (3) Odds ratio is the proportion between the odds of pain in those with and without each hardship variable.
p < .05. **p < .01. ***p < .001.
Among men who experienced food insecurity had a 2.0 higher odds of having trouble with pain compared to men who did not experience food insecurity controlling for other variables (CI [1.17, 3.25], p < .05). Men who had Medicare coverage had a 2.2 higher odds of having trouble with pain compared to men who did not have Medicare coverage controlling for other variables (CI [1.69, 2.83], p < .001). Men who experienced food insecurity and had Medicare coverage had a 1.2 higher odds of having trouble with pain compared to men who experienced food insecurity and did not have Medicare coverage (CI [0.56, 2.38], not significant).
Men who took less medication had a 1.7 higher odds of having trouble with pain compared to men who did not take less medication due to cost controlling for all other variables (1.11, 2.61, p < .05). Men who had Medicare coverage had a 2.0 higher odds of having trouble with pain compared to men who did not have Medicare coverage controlling for all other variables (CI [1.57, 2.63], p < .001). Men who took less medication due to cost and had Medicare coverage has a 1.4 higher odds of having trouble with pain compared to men who took less medication due to cost and did not have Medicare coverage.
Men who had difficulty paying bills had a 1.2 high odds of having trouble with pain compared to men who did not have difficulty paying bills controlling for all other variables (CI [0.86, 1.71], not significant). Men who had Medicare coverage had a 2.0 higher odds of having trouble with pain compared to men who did not have Medicare coverage controlling for all other variables (CI [1.38, 2.87], p < .001). Men who had difficulty and had Medicare coverage had a 1.2 higher odds of having trouble with pain compared to men who had difficulty paying bills and did not have Medicare coverage.
The second part of Table 4 provides results for men who experienced severe pain most of the time and the effect of having Medicare insurance coverage. Results suggest that men who experienced ongoing financial hardship had a 4.9 higher odds of experiencing severe pain compared to men who did not experience ongoing financial hardship controlling for all other covariates (CI [1.74, 14.33], p < .01). Men who had Medicare coverage had a 4.9 higher odds experiencing severe pain most of the time compared to men who did not have Medicare coverage controlling for all other variables (CI [1.63, 14.77], p < .01). Men who experienced ongoing financial hardship and who had Medicare coverage had a 0.3% or 70% lower odds of experiencing severe pain compared to men who had ongoing financial hardship and did not have Medicare coverage (CI [0.08, 0.79], p < .05).
Men who experienced food insecurity had a 1.5 higher odds of experiencing severe pain compared to men who did not experience food insecurity controlling for other variables (CI [0.58, 3.83], not significant). Men who had Medicare coverage had a 1.7 higher odds of experiencing severe pain compared to men who did not have Medicare coverage controlling for other variables (CI [0.71, 3.92], not significant). Men who experienced food insecurity and had Medicare coverage had a 1.1 higher odds of experiencing severe pain compared to men who experienced food insecurity and did not have Medicare coverage (CI [0.24, 5.39], not significant).
Men who took less medication had a 1.4 higher odds of experiencing severe pain compared to men who did not take less medication due to cost controlling for all other variables (0.49–3.77, not significant). Men who had Medicare coverage had a 1.5 higher odds of experiencing severe pain compared to men who did not have Medicare coverage controlling for all other variables (CI [0.75, 3.15], not significant). Men who took less medication due to cost and had Medicare coverage has a 1.2 had higher odds of experiencing severe pain compared to men who took less medication due to cost and did not have Medicare coverage (CI [0.38, 3.58], not significant).
Men who had difficulty paying bills had a 3.0 high odds of experiencing severe pain compared to men who did not have difficulty paying bills controlling for all other variables (CI [1.26, 7.05], p < .05). Men who had Medicare coverage had a 3.1 higher odds of experiencing severe pain compared to men who did not have Medicare coverage controlling for all other variables (CI [1.10, 8.59], p < .05). Men who had difficulty paying bills and had Medicare coverage had a 0.5 or 50% lower odds of experiencing severe pain compared to men who had difficulty paying bills and did not have Medicare coverage (CI [0.17, 1.54], not significant).
Discussion
There is growing concern regarding the impact hardships may have on the quality of life and general well-being of adult men. To understand the consequences of these social, behavioral, and economic indicators, this study aimed to examine the effects of hardship on the presence of pain and pain severity among men across socioeconomic groups. Our data provided interesting results of the association between pain and the four hardship indicators. These findings support those of previous empirical research in which economic insecurity was hypothesized and was associated with physical pain (Chou, Parmar, & Galinsky, 2016).
Although the empirical literature for over half a century reflects a robust relationship between socioeconomic status and health status (Adler & Ostrove, 1999; Burgard & Kalousova, 2015; Haas, 2006), the debate continues as to which pathway is most influential: poor health leading to lower social mobility and the connection with labor market or lower socioeconomic status and its influences on health outcomes. It has been suggested that health selection may have a significant role in an individual’s connection with the labor market (Stolove, Galatzer-Ley, & Bonanno, 2017). It is logical that those in poor health would have a precarious and tenuous connection with the labor force at best. For those in poor health who are working, in the event they become unemployed, the likelihood of being rehired is limited. The concept of health selection or drift may play a yet undetermined role in these men’s experiences and perception of pain. Due to their already poor health, lower SES men’s participation in the labor market is precarious. With limited participation, in the event of an economic shock such as unemployment, these men limited options in accessing medical care when needed further decreases. Research evidence exists showing a strong association between unemployment and health outcomes (Brand, 2015). As articulated by Haas, an individual’s socioeconomic position is predicated on their health status. Future research of experiences of pain among men would benefit from the inclusion of earlier health status variables to determine if the pathway into downward economic and social mobility is indeed related to poor health. Nearly 20 years ago, Adler and Ostrove (1999) recommended research take into considering the influence of SES across demographic variables such as race and gender on health status and outcomes. In the current economic environment, we suggest that experiences of pain be included as well.
Using data from the Health and Retirement Study, the first hypothesis that hardship would be associated with the presence of pain and/or pain severity was supported. Findings indicate a strong association between each of the four hardship indicators (difficulty paying bills, food insecurity, ongoing financial strain, and taking less medication due to cost) and the presence of pain and pain severity. Specifically, eating less due to cost (food insecurity) gives reason to consider some potentially troubling aspects for these men. For example, it has been established that hunger is associated with pain, psychologically and physically. While it cannot be confirmed with these findings, it is plausible that the pain experienced by these men was associated with the sensation of missed meals and or reduced caloric intake also referred to as “hunger pangs” (Schilbach, Schofield, & Mullainathan, 2016).
Another interesting finding was the relationship between taking less medication and the presence of pain and pain severity. Previous findings suggest that by not taking prescribed medication(s), one could potentially exacerbate a chronic health condition, thereby causing physical pain (Chou et al., 2016; Nandi, Charters, Strumpf, Heymann, & Harper, 2013; O’Neill, Sorhaindo, Xiao, & Garman, 2005). This behavior may be attributed to reduced financial ability or capability. These behaviors may also contribute to chronic conditions becoming more pronounced or out-of-control which in turn, may potentially enhance the perception of pain. Both eating less and taking less medication serve as both endogenous and exogenous variables to the pain experience, whereby both the direct and indirect implications are manifestations of each other. For example, not having the financial means to purchase food can have implications on taking less medications. Some prescribed medications, must be taken with food, or drink, and so on. Not doing so can lead to long-term effects, with deleterious physical outcomes (e.g., pain). Similarly, due to increasing health-care costs, additional or increased deductibles, and medications dropped from coverage through insurance plans, an individual may forfeit purchasing the necessary medications that may counter illness symptoms. This, in turn, may exacerbate a number of reported (pain-related) chronic illnesses. Future research may provide additional answers in understanding the manifestations of pain (i.e., physical, somatic and psychological) when an individual report’s limited food intake. This may also apply when pain is reported from individuals taking medications for chronic health conditions.
The second hypothesis, that there is a positive association between greater hardship and the presence of pain and/or increased pain severity, even after controlling for demographic factors (i.e., age, income, education, marital status), was partially supported.
Findings suggest that both higher and lower levels of education appear to act as protective factors against the effects of hardship and pain. Previous empirical research has found a link to the buffering effects of higher education levels against the experience of pain in the presence of financial difficulties. This may be the result of the increased potential for securing employment, a sense of self-control over one’s economic situation, a larger support network with the capability of providing financial assistance or financial instruments to draw upon during downturns (Chou et al., 2016; Ross & Wu, 1995; Winkleby, Jatulis, Frank, & Fortman, 1992). The finding, in this study, that lower levels of education offers a degree of protection in the presence of hardship related to finances and pain is interesting. We speculated that men with lower education levels have grown acclimated and accustomed to difficult circumstances and conditions across their lives of which the presence of hardship and pain is just a continuation of their life course. This finding may be supported through Dannefer’s theory of cumulative advantaged/disadvantage (2003). The “status maintenance” and “social class” (p. S329) of the men with lower educational levels may contribute to their perception of hardship and pain as ordinary features of their existence. This finding clearly indicates and suggests that future research should investigate the influence of education on experiences and responses to pain associated with a variety of circumstances including but not limited to hardship.
This finding is consistent with other works which also suggest that educational level acts as a buffer against the experience of pain, especially in the presence of financial difficulties (Chou et al., 2016; Ross & Wu, 1995; Winkleby et al., 1992). The protective effect of education against the perception of pain emanating from different hardships warrants further empirical investigation. Additionally, those reporting lower levels of income may be employed in physically demanding jobs (e.g., construction, foundry) which in turn contribute to their perceptions of and experiences with pain. Future research will need to assess the type of employment men hold and the physical demands associated with it in order to assess pain levels appropriately.
The third hypothesis that men who had Medicare insurance coverage reported experiencing less pain was partially supported. That Medicare acts as a buffer for those troubled with pain suggests the importance of this social protection mechanism in potentially alleviating some of the concerns men may have when faced with choices regarding the use of financial resources to purchase medication. In addition, men may be more likely to experience less stress associated with whether to purchase or not purchase needed medications. Therefore, the health-care plan an individual currently has or selects in the future may have implications for his or her health outcomes.
The limitations of this study are that the data were cross sectional thus presenting only one point in time of hardships on subjective pain presence and severity. Future research would benefit from the utilization of a longitudinal study of men and their experiences of pain through several business and economic cycles. Additionally, the inclusion of men younger than 50 years of age would provide a longer perspective from which to assess the effects of economic cycles on men’s presence and severity of pain. The use of single-items for the presence of pain and its severity may have failed to capture the full dimensions of pain. Future research must expand its measures of pain and examine a broader perspective of the nature of pain and its severity. The research of Nahin (2015) poses several questions which appear more comprehensive in the assessment of pain and its effect on the individual as well as the duration and limitations presented by an episode(s) of pain.
Another limitation of this study was the use of Medicare insurance coverage “in general.” For example, not all Medicare insurance plans provide “all-inclusive” coverage, this of course depends on the plan an individual decides to purchase. These findings suggest that those receiving Medicare are able to access health-care services when pain episodes occur whereas those without health insurance coverage are left to address their pain experiences through self-medication or other methods of relief. The fact that coverage allows men to seek out and utilize medical guidance when experiencing pain reflects the importance of providing adequate medical care for eligible populations.
Future research regarding the association between hardship and pain would be enhanced by including unhealthy health behaviors (e.g., drinking, smoking, substance abuse). The association between unhealthy health behaviors as coping strategies and their relation to pain and hardship is under explored. Although these limitations indicate and suggest caution in terms of generalizing the findings to the population, this study does delve into a topic which has received less than adequate attention in the empirical research literature. Moving forward it is important that future research not only examine the gender differences in the perception and severity of pain associated with the intricate connection with hardship; but it may also examine the intersectionality of gender and race whereby these experiences may vary considerably.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The research conducted for this manuscript was supported by the National Institutes of Health. Dr. Marshall is funded by a K01 career development award (Grant# 5K01AG048416-03) from the National Institutes of Aging.
