Abstract
Squamous cell carcinoma (SCC) of the bulbar urethra accompanied by lichen sclerosus (LS) is rarely reported. This study reports the case of a 56-year-old man with urethral squamous cell carcinoma (USCC) accompanied by a long history of genital LS. The man presented with a painful perineal mass and had a long-term history of urethral strictures and urethral dilatation. The patient developed a periurethral abscess that expanded to the perineum and formed an urethrocutaneousperineal fistula. An organ-sparing perineal resection and fistulectomy was performed according to the patient’s wishes. During the operation, residue-like pus mixed with necrotic tissues drained out. A section of the prepuce and the necrotic tissues were sent for histological analysis. Hematoxylin and eosin (HE) staining of the excised prepuce revealed classical LS. HE and immunohistochemical (IHC) staining of the necrotic tissues showed well-differentiated USCC. IHC staining showed the USCC to be positive for P53 and Ki-67 and negative for P16, suggesting the USCC was probably associated with LS. The patient received high-dose chemotherapy and radiation therapy and died 10 months after surgery.
Male genital lichen sclerosus (MGLSc), also known as balanitis xerotica obliterans, is a chronic progressive inflammatory skin disease that may affect the foreskin, glans, meatus, and urethra at any age. The exact causes are unknown, but autoimmune, genetic, infectious factors, local trauma, and hormonal factors have been implicated (Pugliese, Morey, & Peterson, 2007). The diagnosis is mostly clinical, with secondary phimosis, white xerotic appearance of the glans and foreskin, dysuria and even urinary retention (Fistarol & Itin, 2013), and confirmed by biopsy. Classical histopathological features include epidermal atrophy, dermal sclerosis with the loss of elastic fibers and collagen and an underlying band-like lymphocytic infiltrate. For affected patients, it is essential that urologists, dermatologists, histopathologists, surgeons, general practitioners, and pediatricians, respectively, have a solid knowledge of the disease (Fistarol & Itin, 2013). When not recognized and treated early, the progression of this disease may result in meatal stenosis and urethral strictures.
MGLSc is a disease that can progress to malignancy. The European Association of Urology (EAU) guidelines identify MGLSc as a strong risk factor for penile squamous cell carcinoma (pSCC) (Algaba et al., 2002). Recently, Pietrzak reported that 22% of patients presenting with pSCC had a histological diagnosis of MGLSc (Pietrzak, Hadway, Corbishley, & Watkin, 2006). Squamous cell carcinoma (SCC) of the male urethra is distinctly rare and urethral SCC accompanied by MGLSc has not been reported. Herein, a case of USCC associated with LS encountered by the authors is reported.
Case Report
A 56-year-old man complaining of perineal pain and dysuria had a long history of lichen sclerosus (LS), urethral strictures, and urethral dilatation. He was diagnosed with a periurethral abscess. Drainage and suprapubic cystostomy (SPC) placement was performed at a local clinic. The abscess did not improve, and over the next 3 years, expanded to the perineum, forming a non-healing urethrocutaneousperineal fistula with continuous purulent discharge. The patient had no history of trauma, drug abuse, venereal disease, calculus, or blood transfusion.
Physical examination revealed urethral meatus atresia and the glans with white atrophic xerotic plaques (Figure 1). There was an urethrocutaneousperineal fistula and purulent discharges with necrotic tissues flowing from the fistula (Figure 1). A biopsy was taken from the necrotic tissues and a histological analysis confirmed USCC. Urethroscopy revealed a lesion in the bulbar urethra without prostate and bladder invasion. On palpation, the prostate and bilateral inguinal lymph nodes were not enlarged. Hematological laboratory investigation, including testing for prostate-specific antigen (PSA), was normal. Chest and abdominal computed tomography (CT) and pelvic magnetic resonance imaging (MRI), as well as colonoscopy, were unremarkable (cT3N0M0).

The appearance of lichen sclerosus, with white xerotic plaques on the glans and urethral meatus atresia. Urethral sounds revealed an urethrocutaneousperineal fistula.
The patient refused cystoprostatectomy and wished to preserve his penis and testis. Considering the patient’s age, health status, expectations, and USCC stages, a bladder, prostate and penile-sparing perineal resection and fistulectomy was performed by two reconstructive urologists. During the operation, large amounts of residue-like pus mixed with necrotic tissues drained from the wounds (Figure 2). A section of the penile urethra and the necrotic tissues were sent for histological analysis.

Residue-like pus mixed with necrotic tissues draining from the surgical wounds.
Hematoxylin and eosin (HE) staining of the excised prepuce revealed classical LS, with epidermal atrophy, dermal sclerosis, and underlying band-like lymphocytic infiltration (Figure 3). HE and immunohistochemical (IHC) staining with CK5/6 of the necrotic tissues showed well-differentiated USCC, with apparent keratin pearl (Figure 4A, C) and intercellular bridges (Figure 4B, D) in the carcinoma nest. IHC evaluation with P53, Ki-67, and P16 staining showed that the USCC was strongly positive for P53 and Ki-67 and negative for P16 (Figure 5).
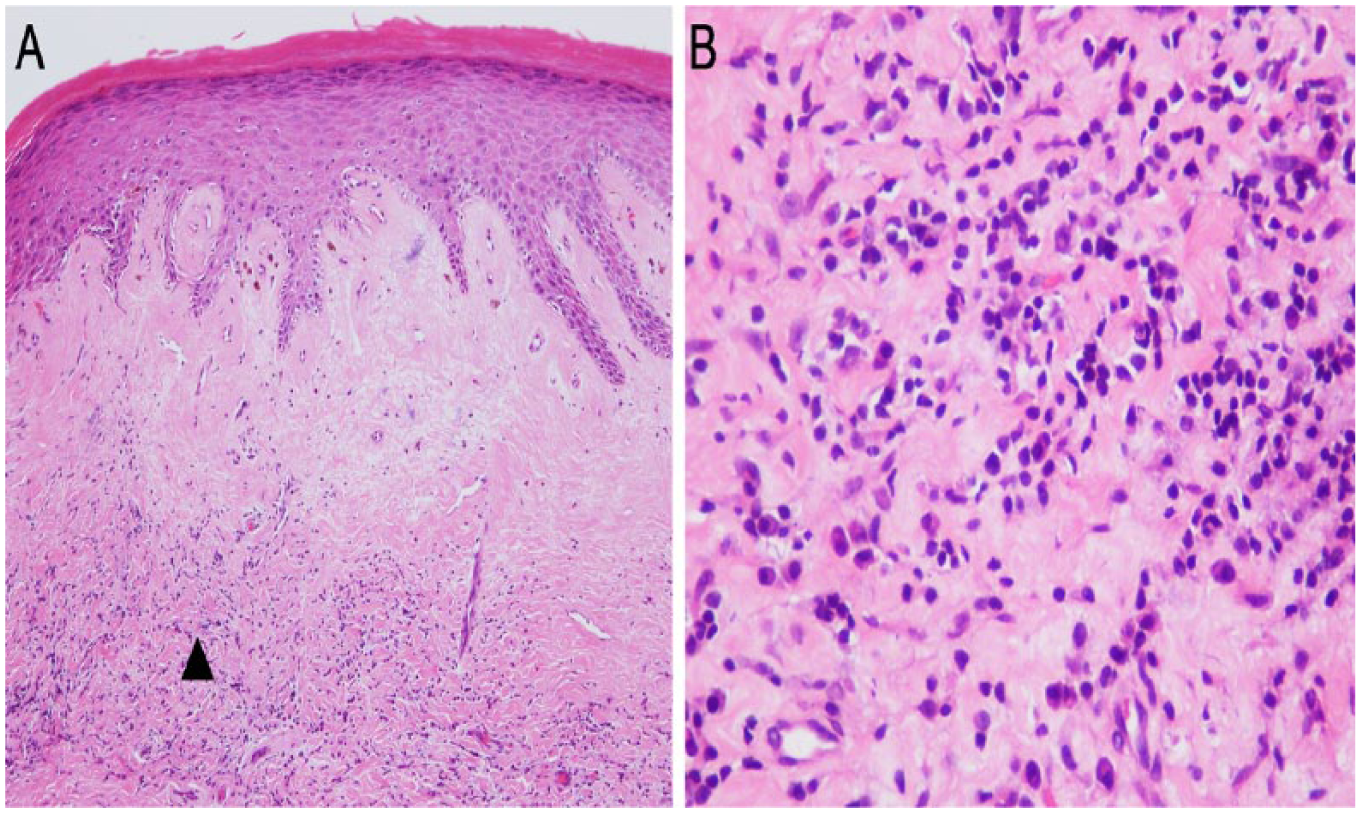
(A) Hematoxylin and eosin staining of the penile urethra specimen demonstrating lichen sclerosus: band-like infiltrate of lymphocytes in the dermis, hyalinization of collagen in the upper dermis, and orthokeratotic hyperkeratosis of the epithelium. (B) The magnifying area of “▲” indicates infiltration of lymphocytes. Original magnifications: 100× (panel A) and 400× (panel B).

(A and C) Hematoxylin and eosin and immunohistochemical staining showed well-differentiated urethral squamous cell carcinoma, with keratin pearl in the carcinoma nest. (B and D) The magnifying area of “▲” indicates intercellular bridges. Original magnifications: 200× (panels A and C) and 400× (panels B and D).

Urethral squamous cell carcinoma was positive for P53 and Ki-67 and negative for P16: immunohistochemical staining (original magnification, 200×).
The patient subsequently received perineal radiotherapy and six cycles of cisplatin-based systemic chemotherapy and was examined every 3 months. Positron emission tomography (PET) showed a lumbar metastasis 5 months after surgery. The patient died of distant metastasis (breast and brain) 5 months later.
Discussion
USCC is considered a rare cancer, accounting for<1% of all malignancies. Chronic urethral inflammation/urethritis and urethral strictures are reported as predisposing factors for USCC (Gakis et al., 2013). MGLSc is a chronic inflammatory disease that may cause urethral strictures. MGLSc has been regarded as a strong risk factor for pSCC (Algaba et al., 2002), and may have some association with USCC. Because of the low incidence and the poor prognosis of USCC, a case of USCC accompanied by MGLSc is reported to share some experiences on the diagnosis and treatment of USCC and to alert clinicians to USCC’s aggressive malignancy and the potential negative effects of MGLSc on USCC.
USCC generally occurs in the fifth decade of life. Due to both clinical and social factors, it is often diagnosed at an advanced stage. The most common symptoms of locally advanced USCC include an extraurethral mass (52%), bladder outlet obstruction (48%), pelvic pain (33%), urethrocutaneous fistula (10%), abscess formation (5%), or dyspareunia (Gheiler et al., 1998).
The management of USCC is particularly challenging due to its rarity and the lack of randomized evidence to inform practice. The results from treatment with surgery alone for bulbar USCC have been disappointing, with 5-year disease-free survival rates of 0% to 15% (Dalbagni, Zhang, Lacombe, & Herr, 1999). More recently, combined treatment with surgery and chemoradiotherapy was suggested to improve local control and survival (Cohen et al., 2008). Cystoprostatectomy should be reserved as a primary treatment option in patients with extensive ductal or stromal involvement (Gakis et al., 2013) and is the recommended approach in EAU guidelines (Gakis et al., 2013). However, in this case, the patient did not wish to undergo such a procedure. The medical team had to respect the patient’s choice of local excision followed by a high dose of systemic chemotherapy and radiation therapy. Despite treatment with the combined strategies, the patient died of distant metastasis. The results suggested that combined treatment with chemoradiotherapy and organ-preserving surgery could not deter the long-term effects of bulbar USCC. Further research is needed to explore better management strategies.
Histopathologically, USCC was positive for P53 and Ki-67 and negative for P16. Bayard reported increased p53 and Ki-67 expression in pSCC and vulva SCC was associated with LS, especially in cases of chronic, long-standing LS (Carlson et al., 2013). Similar results appeared in this case, suggesting that USCC may also have some association with LS. P16 acts as a tumor-suppressing protein and has been reported to be significantly associated with HPV-associated pSCC and vulvar SCC (Carlson et al., 2013). HPV infection and p16 expression were also reported in the context of LS. This patient was negative for HPV infection, and USCC was negative for P16, which was in accordance with earlier findings.
Conclusion
In summary, USCC may have some association with MGLSc. Clinicians should be aware of the possible link between these entities. An organ-sparing perineal resection and chemoradiotherapy could not deter the long-term effects of USCC. The treatment of USCC remains challenging and further research is needed to elucidate better management strategies.
Footnotes
Acknowledgements
We would like to acknowledge the contributions of the participants who made this work possible.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
