Abstract
Substance use is a globally devastating social problem. Early maladaptive schemas (EMSs) are inefficient mechanisms leading directly or indirectly to psychological distress. The current study aimed to assess the role of EMSs in predicting opioid use disorder. The cross-sectional study was conducted in 2013 in Bojnurd at northeast of Iran on 60 male opioid users who received Methadone Maintenance Treatment (MMT) and 60 control males. The opioid users were selected randomly from MMT clinics and control subjects were selected and matched with opioid users using demographic variables. The subjects completed the Young Schema Questionnaire-Short Form (YSQ-SF). Except for SS (self-sacrifice), EG (entitlement/grandiosity), US (unrelenting standards), and FA (Failure to Achieve), the mean of other maladaptive schemas in the opioid user group were significantly higher than that of the control group, adjusted for multiple comparisons. Multivariate analysis of variance (MANOVA) indicated significant differences in maladaptive schemas between the two groups. Logistic regression identified that Emotional Deprivation, Mistrust/Abuse, and Unrelenting Standards can predict opioid use. As a result, the risk of opioid-related disorders in people with higher YSQ-SF scores in these schemas is higher. The findings conclude that the existence of underlying EMS may constitute a vulnerability factor for developing opioid use disorders later on in life. Provided the vast amount of scientific literature in evidence-based treatments focusing on EMSs, maladaptive schemas and related core beliefs can be detected and treated in adolescence to prevent the enactment of the schema and psychological distress likely to induce opioid use.
The World Health Organization has identified substance abuse as “the global burden,” its effects being so vast they can be identified as far as the third world causing devastation even in developed countries (http://www.who.int/substance_abuse/facts/global_burden/en/). A significant rise in substance use occurred from 2002 to 2009 (Health & Services, 2011). In Iran, substance users are estimated to be between 1.8 and 3.3 million people, most of them being opioid users (Mokri, 2002). In contrast, the newest and most effective therapeutic methods for substance use are still prone to high relapse rates. A pathogenic environment, in which substances are easily accessible, combined with an encouraging friend network undermines any progress in the therapy leading to relapse (Georgie, Sean, Deborah, Matthew & Rona, 2016). Effectively identifying and manipulating factors in commencing substance use has proven to be the best form to prevent substance use. Among the underlying causes of substance use, psychological factors are significantly important. The effect of biological and social factors is dependent on the psychological approaches of the individual toward substance use. As long as an individual lacks a positive attitude toward substance use as a solution to his or her problems or possess sufficient self-confidence in social environments, there is a lower probability that the individual will start substance use both on their own and as a result of peer pressure (Davison & Neale, 2000).
Among other influential psychological variables in an individual’s life, schemas are of a great importance. Based on the Diathesis-stress model in psychological pathology, many researches have investigated the role of family as a possible context for individual vulnerability (Harris & Curtin, 2002). Piaget (1954) and Bowlby (1969) [from (Gunty & Buri, 2008)] believed parents play a significant role in developing a model within one’s cognitive organization which works as a framework that affects individual’s interpretations, choices, and evaluations of his or her experiences. These frameworks are known as schemas. Young (1994) believes that each psychopathological symptom is related to one or more early schemas (Delattre et al., 2003). Studies suggested that early maladaptive schemas (EMSs) are inefficient mechanisms resulting in psychological distress, directly or indirectly (Cecero, Nelson, & Gillie, 2004). EMSs are long-standing emotional and cognitive patterns of self-defense that are developed in the early years of life and are the cause of many psychological disorders. These, combined with inefficient coping strategies adopted by the patient to deal with others, often lead to chronic symptoms of anxiety, depression, and substance use (Shaghaghy, Saffarinia, Iranpoor, & Soltanynejad, 2011). Young, Klosko, and Weishaar (2003) reported that EMSs and resulting malfunctioning coping strategies may underlie substance use. Furthermore, attempts to avoid emotional behavioral responses and negative cognitions of EMSs are associated with more severe substance use (Young et al., 2003).
Given that 95% of substance users in Iran are men (Goodarzi et al., 2011; Mokri, 2002) and that worldwide substance use is predominantly more common among males (Sadock & Sadock, 2011), samples in the present study were chosen among male users. EMSs develop during childhood through relationships with significant caretakers. Once they developed, the EMSs selectively filter for confirming experience such that the schemas are extended and elaborated throughout the individual’s lifetime (Young, 1994). But substance use starts in adolescence or adulthood; therefore, the study aimed to determine the schema’s pattern in opioid users versus a control group and to assess the role of EMSs in predicting opioid use disorder, and also to determine which EMS suggests better predictions.
Materials and Methods
This cross-sectional study was carried out on male opioid users receiving Methadone Maintenance Treatment (MMT) in MMT clinics of Bojnurd (in northeast Iran). Sample size estimation was based on mean comparison of each schema between opioid users and the control group obtained from a pilot study with α = 0.05 and Power of Test = 80% . Sample size was estimated to be 56 individuals per group. As a precaution, the study was conducted on 60 opioid users and 60 control males so if some of the questionnaires weren’t completely answered and the authors had to remove them from the data, the sample size wouldn’t be affected.
First, the opioid users were selected randomly from MMT clinics and the control subjects were selected and matched with them in terms of age, education, marital status, and occupation. Opioid users were asked to introduce a nonuser man among their relatives, friends, or acquaintances similar to themselves in terms of demographic features; age (5 years younger or older); education (at a same educational grade); marital status (similar); and occupation (unemployed, self-employed, employee, laborer, and student). These demographic variables were chosen to be controlled by matching because relationships, jobs, and education are among the most important areas of life and the reenactment of EMSs in these areas is most significant, which in turn will result in confirming and consolidating the schemas. If the groups were in different states in these areas, the differences in EMS score could be due to the different opportunities for schema consolidation other than opioid use.
The nonuser subjects were then investigated deeply and meticulously in terms of substance use history. Subjects who had even one experience with use of drug, alcohol, or psychedelics were excluded. In other words, control group cases were homogenous with opioid users in all aspects but had no history of substance use.
The participants completed a demographic questionnaire and the Young Schema Questionnaire-Short Form (YSQ-SF) (Welburn, Coristine, Dagg, Pontefract, & Jordan, 2002). All subjects signed a written consent form to participate in the study. Names of the participants were not included in the questionnaire and their personal information was made to remain confidential with data analysis being carried out in groups. All participants were free to leave the study at any given time.
Materials
The Young Schema Questionnaire-Short Form: YSQ-SF is a 75-item scale. The items measure the presence of 15 maladaptive schemas selected by dataset of Schmidt, Joiner Jr, Young, and Telch (1995). These schemas include: Emotional Deprivation (ED), Abandonment/Instability (AB), Mistrust/Abuse (MA), Social isolation/Alienation (SI), Defectiveness/Shame (DS), Failure to Achieve (FA), Dependence/Incompetence (DI), Vulnerability to Harm (VH), Enmeshment/Undeveloped self (EN), Subjugation of Needs (SB), Self-Sacrifice (SS), Emotional Inhibition (EI), Unrelenting Standards (US), Entitlement/Grandiosity (ET), and Insufficient Self-Control (IS). Responses were indicated with a 6-point scale including:
1 = Completely untrue of me; 2 = Mostly untrue of me; 3 = Slightly more true than untrue; 4 = Moderately true of me; 5 = Mostly true of me; and 6 = Describes me perfectly. Good internal consistency, reliability, and validity of this version has been demonstrated (Waller, Meyer, & Ohanian, 2001; Welburn, Coristine, Dagg, Pontefract, & Jordan, 2002). Factor analysis by Welburn et al. (2002) indicated further support for the 15 identified EMSs of the YSQ-SF in a clinical sample. Reliability and validity of the Iranian version of this instrument was assessed and approved by Ahi, Mohammadifar, and Besharat (2007).
Statistical Analyses
The statistical methods used in the current study were the Independent t-test for comparing two means and the χ2-test to compare qualitative variables of two groups.
MANOVA was used to evaluate the group differences across EMS’s items simultaneously. Odds ratios (OR) of opioid use associated with clinically significant EMSs (schema score > 3) in comparison with not clinically significant EMSs (schema score ≤3) have been reported. The scoring method (schema score > 3 vs. ≤3) is consistent with that recommended by Young and Brown (2003) and that used in previous research with EMS and substance abuse (Shorey, Anderson & Stuart, 2011; Shorey, Stuart, & Anderson, 2012; Shorey, Stuart & Anderson, 2014). In addition, multiple logistic regression models, backward method, were used to identify the best subset of EMSs for prediction of opioid use. The final model was selected based on the smallest value of the Bayesian information criterion )BIC( (Schwarz, 1978). For each OR, 95% confidence interval was presented. The p-value < .05 was considered as significant level. To adjust for multiple comparisons, the Bonferroni correction was applied. All statistical analyses were performed using STATA IC windows, version 14.
Results
Demographic findings: Mean of age in opioid users and control group was 31.82 ± 8.07 and 32.12 ± 8.54, respectively. There was no significant difference in mean of age between the two groups (p = .84). Moreover, there was no significant difference in terms of education, occupation, and marital status between opioid users and the control group.
Means of all 15 EMSs in the opioid user group were higher than those of the control group. Except for SS, EG, US, and FA maladaptive schemas, the difference of other maladaptive schemas between the two groups were significant, adjusted for multiple comparisons (Table 1). MANOVA analysis indicated significant differences between the two groups in terms of EMSs (λWilks = 0.688, F (15,104) = 3.139, p < .001).
The Mean of EMSs in Opioid User and Control Groups.

Note. *Significant, based on multiple comparison adjustment; Bonferroni correction.
Results suggest the schemas’ level of severity or strength increases the odds ratio of starting opioid use. Among 15 EMSs, the severity of ED increased the likelihood of starting opioid use the most (Table 2).
Unadjusted Odds Ratio of Opioid Use in Clinically Significant EMSs in Comparison with Not Clinically Significant EMSs.
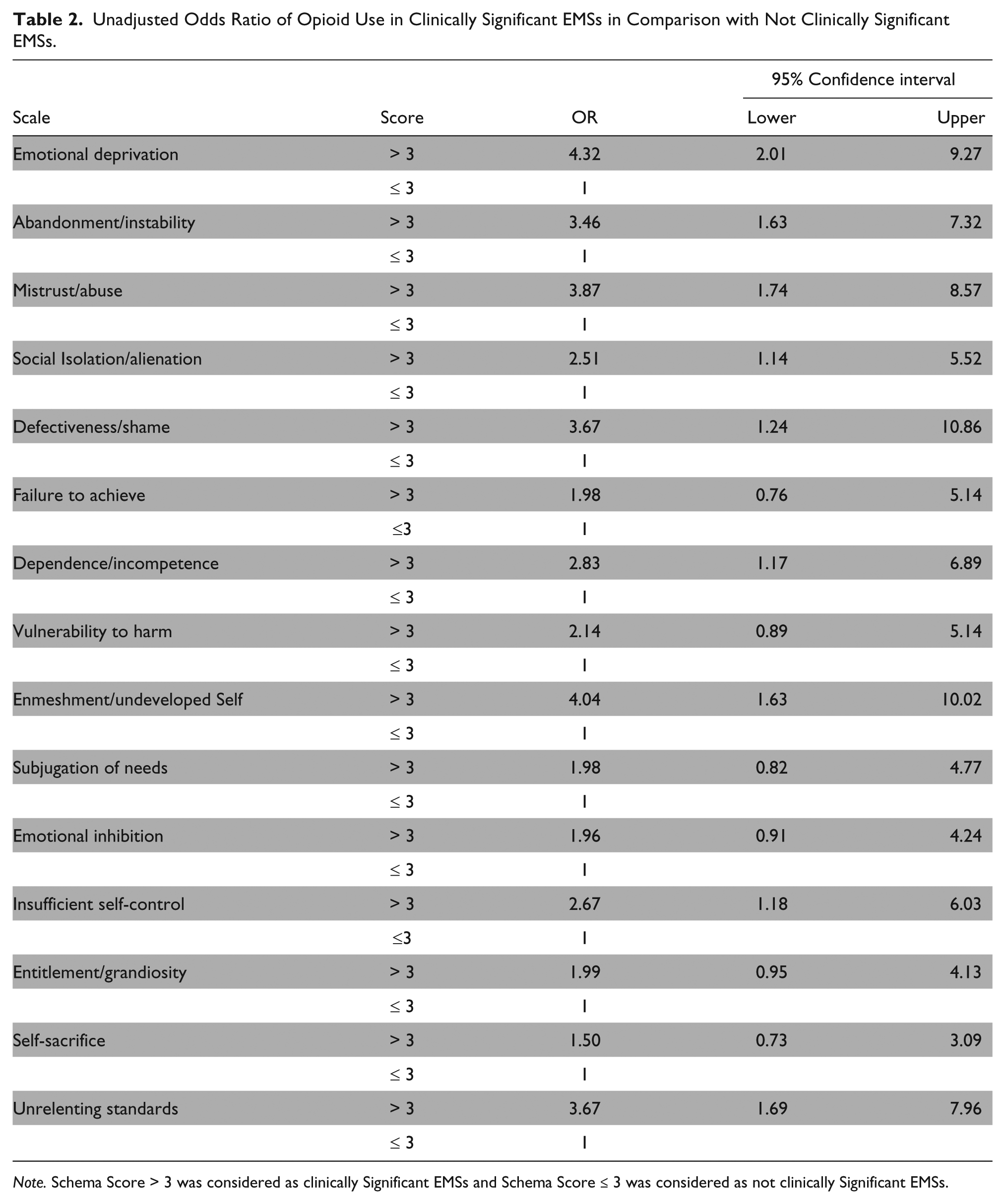
Note. Schema Score > 3 was considered as clinically Significant EMSs and Schema Score ≤ 3 was considered as not clinically Significant EMSs.
Multiple logistic regression modeling with backward method identified ED, MA, and US as the best subset of EMSs which can significantly predict opioid use as shown in Table 3. Therefore, males with maladaptive schemas (score > 3) in these three EMSs have a higher chance of opioid use.
The Result of Backward Multiple Logistic Regression for Predicting Opioid Use Based on 15 EMSs.

Discussion
The current study demonstrated that EMSs can predict opioid use, that is, the more maladaptive the schema, the greater the likelihood of opioid use. Moreover, ED, MA, and US schemas were the best opioid use predictors among the 15 schemas.
The results identified that the mean of EMSs in the opioid user group is higher than that of the control group except for SS, ET, US, and FA. This is consistent with previous studies which report that substance users achieve higher scores in EMSs in comparison with nonusers (Roper, Dickson, Tinwell, Booth, & McGuire, 2010; Shaghaghy et al., 2011; Shorey et al., 2011).
Schemas are often related to high levels of negative affection and self-defeating outcomes, which may interfere in communication, autonomy, and self-expression (Young et al., 2003). In response to maladaptive schemas, individuals develop various coping skills in order to reduce negative consequences related to these schemas. These coping skills are generally malfunctioning and inconsistent and include avoiding behaviors such as substance use (Ball, 1998; Young, 1994). According to this assumption, Ball (1998) suggested that there is a relationship between EMS and substance use. Studies have reported that when therapy is deeply focused on the substance user’s maladaptive personal characteristics, more desirable results are achieved (Ball, 1998). EMSs may be related to substance use disorder, therefore simultaneous attention to substance use and the schemas may lead to effective therapeutic results (Ball, 1998).
ED, MA, and US schemas are the best predictors for opioid use per the current results. People justify any event or affair in their lives based on their schemas and their coping strategies are in accordance with that scheme.
EMSs are self-perpetuating and very resistant to change. Because EMSs lie at the core of one’s self-concept, it is familiar, comfortable, and unconditional (Swarm, 1983 cf Schmidt et al., 1995). The nature of an EMS prevents realistic processing of inconsistent information with the schema. At the cognitive level, the schema is maintained by highlighting information that confirms the schema, and negating or minimizing information that is inconsistent with it.
As a consequence of their schemas or in response to them, individuals with emotional deprivation may choose environments or people that are not capable of appropriate emotional support. This, in turn, leads to the maintenance of their schemas and works as a confirmation for their beliefs. According to the study of Shorey et al. (2011), aimed to investigate EMSs among 80 substance users and their spouses, there was a significant similarity between addicts and their spouses in some schemas (Young et al., 2003).
As underlying factors in forming an ED schema, researchers identify that weak family control, weak affectability among family members, significant role of the mother figure in the family, father’s weak function, and parents’ substance use are associated with children’s substance use (Pinheiro et al., 2006). Substance users’ family members report various psychological problems such as depression, substance use, psychological trauma, and also medical problems (Ray, Mertens, & Weisner, 2009). Furthermore, patients may be emotionally less accessible due to substance use which results in defective communication. Consequently, in such malfunctioning family environments which most substance users have experienced, they are dealing with weak emotional relationships and emotional deprivation, family members are not emotionally accessible, and there is not enough support and communication so they experience rejection and distrust.
Young et al. (2003) assume that a considerable contributing factor in an MA schema is the experience of child abuse and neglect. Former studies suggest that there is evidence of child abuse in addicts’ life histories. Rostami, Zarei, and Larijani (2010) reported a significant positive relation between adulthood substance use and having suffered from abuse in childhood (Rostami et al., 2010). Therefore, these schemas may have developed in response to heavy trauma in childhood and it is possible that maladaptive schemas meditate the relation between child abuse experiences and substance use. This issue merits further studies.
In concerns to the “Unrelenting Standards” schema in which opioid users scored higher, individuals with this schema generally feel the need to achieve their ambitious standards and do so in order to avoid disapproval and shame. Other’s appraisal has a great importance for a perfectionist, causing worry over disapproval of others, consequently leading them to avoid actions that may result in resentment or disapproval (Egan, Wade & Shafran, 2011). Setting unrealistic and inflexible standards and bounding themselves to reach them, believing that it is a disaster if they fail, they will experience psychological distress and associated negative emotions. Consequently, they may start using maladaptive coping strategies like substance use in order to cope with these emotions.
Researchers report that EMSs are consistent over time (Riso et al., 2006), yet they are improvable via interventions (Young et al., 2003). Modifications in EMSs lead to symptom improvement after therapy (Nordahl, Holthe, & Haugum, 2005). Based on the evidence and results of the current study, it is suggested to perform interventions in order to improve and modify these schemas so as to prevent opioid use by eliminating this basic factor.
According to severity and strength of the predictive schemas, which are proposed as opioid use risk factors, the question can be raised as to what extent can education change clinically significant maladaptive schemas into less strong schemas? In order to prevent opioid use, interventions should be made before opioid use and during adolescence, that is, when schemas are developed and are distinguishable but are not solid and strong yet. At this stage, consistent behaviors with the schema have not consolidated it yet, so modification is easier. Even after this stage and during opioid use disorder, schemas can be modified, albeit in a more difficult way.
It should be noticed that although it can be suggested that EMSs represent vulnerability factors for developing opioid use disorders, it is also possible that the development of opioid use disorders lead to or exacerbate EMSs, and both of these situations might be true as well—a sort of feedback loop that maintains the opioid use disorder. This issue merits further investigation with proper methodologies.
Strengths and Limitations
According to international scientific databases such as Medline, Scopus, and Google Scholar, this is the first study carried out to investigate the likelihood of opioid use according to maladaptive schemas. A main problem of this study was that the number of individuals involved was limited to people who were being treated by a Methadone Maintenance Program. Also, because of the limited number of subjects in each group, the authors did not cross validate the predictor model.
Conclusion
This study concludes that risk of opioid use can be predicted according to EMSs, especially US, ED, and MA schemas. Since treatment is proposed for improving maladaptive schemas, these schemas can be detected and treated in adolescence to prevent people from developing opioid use disorder.
Footnotes
Acknowledgements
The authors wish to thank the Research Department of North Khorasan University of Medical Sciences, for their funding support, and all participants of the study.
Abbreviation List
1 MMT: Methadone Maintenance Treatment
2 ED: Emotional Deprivation
3 AB: Abandonment/Instability
4 MA: Mistrust/Abuse
5 SI: Social Isolation/Alienation
6 DS: Defectiveness/Shame
7 FA: Failure to Achieve
8 DI: Dependence/Incompetence
9 VH: Vulnerability to Harm
10 EN: Enmeshment/Undeveloped self
11 SB: Subjugation of Needs
12 SS: Self-Sacrifice
13 EI: Emotional Inhibition
14 US: Unrelenting Standards
15 ET: Entitlement/Grandiosity
16 IS: Insufficient Self-Control
17 MANOVA: Multivariate analysis of variance
18 OR: Odds Ratio
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
