Abstract
The prevalence of depression and anxiety in the Chinese male population with infertility is still uncertain. The prevalence of depression, anxiety, and a combination of both psychological symptoms was 20.8%, 7.8%, and 15.4%, respectively in 771 infertile Chinese men in the current study by the Mental Health Inventory–5 and the State–Trait Anxiety Inventory–Short Form questionnaires. Differences in demographics (age, education, and income) had no noticeable impact on the development of psychological symptoms. Clinical factors such as concomitant disorders (varicocele, epididymal cyst, and erectile dysfunction) were identified as risk factors associated with depressive symptoms (OR = 1.47; 95% CI [1.14, 1.90]; p < .001) and both depressive and anxiety symptoms (OR = 1.56; 95% CI [1.17, 2.08]; p < .001). An infertility duration over 2 years was associated with a high risk of anxiety symptoms (OR = 3.94; 95% CI [1.20, 12.93], p < .02). Other clinical conditions such as type of treatment and quality of sperm were not significant risk factors for psychological symptoms. This study provides evidence that Chinese men of reproductive age who suffer from infertility are vulnerable to psychological distress.
Introduction
Male infertility is a complex problem that affects approximately 7% of all men in modern society (Jungwirth et al., 2012). Infertility is defined as the inability to conceive after 1 year of unprotected intercourse for the couples who are of reproductive age (Boivin, Bunting, Collins, & Nygren, 2007; Rowe, Comhaire, Hargreave, & Mahmoud, 2000). Health problems, congenital abnormalities, reproductive disorders, and severe sexual dysfunction are considered to be causal factors for male infertility (Punab et al., 2017). Furthermore, infertility was reported as being associated with psychological conditions of men and their sexual partners (Donarelli et al., 2012; Fisher & Hammarberg, 2012; Peterson, Newton, & Feingold, 2007).
Depression and anxiety are frequently seen in infertile men (Gourounti, Anagnostopoulos, & Vaslamatzis, 2010). Inability to conceive for a long period after marriage, pressure from partners, peers, family and community, uncertainty of medical help, and physical or moral stress resulting from assisted reproductive techniques could all influence the susceptibility of adult males to anxiety and depression and/or aggravate existing psychological symptoms (Jongbloed-Pereboom et al., 2012). The negative impact of depression and anxiety on the couples’ sexuality, marital happiness, and quality of life may further the development of sexual dysfunction and the exacerbation of infertility. This interaction creates a vicious circle between depression/anxiety and infertile status and will undoubtedly worsen the situation, making male infertility a very difficult entity to be managed by andrologists, urologists, and medical psychologists in their daily clinical work (Monga, Alexandrescu, Katz, Stein, & Ganiats, 2004).
The reported prevalence of depression and anxiety in infertile men varies from 4.9% to 38% in different studies (Chiaffarino et al., 2011; Drosdzol & Skrzypulec, 2009; Gao et al., 2013; Volgsten, Skoog, Ekselius, Lundkvist, & Sundstrom, 2008). Drosdzol and Skrzypulec (2009) reported a relatively high prevalence of depression and anxiety (21%) among Polish infertile males in a survey of 188 subjects. A low prevalence of major depression (5.1%) was reported in infertile Swedish males (Volgsten et al., 2008). It seems that there might be a variance in prevalence of depression and anxiety in infertile men under different ethnic and demographic backgrounds. Understanding the influence of these differences on the prevalence of depression/anxiety symptoms in infertile men will give physicians, educators, and social workers an insight into associated risk factors, allowing them to more effectively help patients suffering from infertility (Beukers et al., 2012).
This study investigates the prevalence of depressive and anxiety symptoms and its associated risk factors in infertile Chinese men who have visited the andrology clinic of Peking Union Medical College Hospital which has more than 200 daily outpatient visits. In comparison with a Chinese study in which a high occurrence of anxiety symptoms (38.01%) was observed in a group of infertile men (Gao et al., 2013), this study focuses not only on the prevalence estimates of psychological symptoms in Chinese men with infertility but also on analysis of demographic and clinical risk factors associated with the prevalence of psychological symptoms. The authors hope that a combination of the two studies will allow us to attain an accurate estimate of the prevalence of depressive and anxiety symptoms and to understand potential risks associated with depression and anxiety in Chinese men with infertility.
Method
Participants
Eight hundred and forty-four Chinese males who suffered from infertility and visited the andrology clinic of Peking Union Medical College Hospital from November 2015 to March 2016 were recruited to the study. Seven hundred and eighty-one outpatients signed the consent and agreed to participate in the survey. Selection criteria included individuals whose partners had been unsuccessful in conceiving a baby with unprotected intercourse for more than 1 year and who had a sufficient level of Chinese reading and writing. Individuals diagnosed with mental illnesses such as dementia and delirium and men in their second or third marriage who had had a child with one of the ex-partners were excluded to rule out some compound factors on depression/anxiety and the infertility. The questionnaire was filled in by participant himself after a brief introduction by clinicians or nurses. Seven hundred and seventy-one questionnaires were received and considered to be valid and 10 were excluded because of an incomplete questionnaire. Demographic information was collected from participants including age, education levels, and monthly income. Medical histories were also obtained from their medical records, including infertility years; other disorders potentially affecting infertility such as varicocele, epididymal cyst, and erectile dysfunction (ED); the severity of illness (three degrees defined as mild: infertility caused by one single condition; moderate: infertility caused by two or more conditions; severe: infertility caused by known genetic abnormalities or other untreatable disorders), and treatments received. A sperm sample was also collected and examined in a clinical laboratory. Numbers and mobility of sperm were determined and categorized as mild oligospermia (≥10 and ≤15 million/ml), moderate oligospermia (≥5 and <10 million/ml) or severe oligospermia (<5 million/ml; WHO Laboratory Manual for the Examination and Processing of Human Semen–Fifth edition, 2010). The information collected was subjected to the assessment of risk factors associated with depression and anxiety in the cohort. The study was approved by the Research Ethics Committee in Peking Union Medical College Hospital.
Questionnaire
Two questionnaires, the Mental Health Inventory–5 (MHI-5) and the Six-Item State–Trait Anxiety Inventory–Short Form (STAI-6), were used in the survey. The MHI-5 is the abbreviated version of the MHI (38 items) that was developed to provide an assessment of several domains of mental health including depression, behavioral control, and general distress. The MHI-5 is a structured, self-report questionnaire (5 items) that the patient can generally complete within 10 to 15 minutes with little or no intervention from an interviewer, allowing us to assess the mood of the participants in the past 4 weeks (Berwick et al., 1991). When the total score was 52 or under, depression was primarily considered (Strand, Dalgard, Tambs, & Rognerud, 2003). The MHI-5 has been widely used to assess depression in a variety of populations and has a coefficient reliability of 0.82 (Cronbach’s alpha; Rugulies et al., 2013; Yamazaki, Fukuhara, & Green, 2005). The STAI-6 is a short form of the introspective psychological inventory consisting of six self-report items pertaining to anxiety affect, and has been widely used to assess participants’ anxiety (Wichman, Ehlers, Wichman, Weaver, & Coddington, 2011). The goal was to compile a set of six items at four levels (1 = not at all, 2 = somewhat, 3 = moderately, and 4 = very much) each that could measure anxiety of an individual at a given moment (Bekker, Legare, Stacey, O’Connor, & Lemyre, 2003). A “normal” score is approximately 34 to 36 and scores equal to 45 or above indicate the status of anxiety (Spielberger, Gorsuch, Lushene, Vagg, & Jacobs, 1983). Higher STAI scores suggest higher levels of anxiety. The STAI-6 has a coefficient reliability of 0.86 (Cronbach’s alpha) for men’s anxiety status (Wichman et al., 2011).
Statistical Analysis
Multiple logistic regression analysis was used to analyze the association of depression and anxiety with information on demographics and medical conditions collected from participants with infertility. The odds ratios (ORs) and 95% confidence intervals (CIs) were calculated and expressed as risk factors for the psychological symptoms. Statistical significance was defined as p < .05. Statistical analysis was performed using the Statistical Package for Social Sciences (SPSS) for Windows Version 18 (SPSS Inc., Chicago, IL, USA).
Results
The average age of participants was 32.3 ± 5.6 years, ranging from 19 to 65 years in this survey. A majority of participants were 40 years old or younger (92%) with a large proportion of individuals receiving education at high school level and above (82.8%). Most had an annual income between ¥24,000 and ¥120,000 (72%). Participants’ demographic information is presented in Table 1.
Prevalence of Psychological Symptoms in Infertile Chinese Men and Their Demographic Information (N = 771).

Among 771 participants who submitted valid questionnaires, 339 have varied degrees of psychological symptoms (44.0%) on assessment. According to the MHI-5 and STAI-6 data, the prevalence of depressive and anxiety symptoms was 20.8% (160/771) and 7.8% (60/771), respectively. One hundred and nineteen participants had both MHI-5 and STAI-6 scores above the thresholds, indicating that the prevalence of both depressive and anxiety symptoms was 15.4% (119/771), with 24.4% (29/119) considered to have severe symptoms.
The data analysis identified that depression seemed to have a higher occurrence in participants younger than 30 years with low income (≤¥2,000 per month), while anxiety was seen frequently in participants older than 40 years. Depressive symptoms were more frequently encountered than anxiety symptoms in infertile men at the clinic (Table 1). It was also observed that medical conditions had a direct impact on prevalence of psychological symptoms. The prevalence of depression and depression/anxiety increased with longer periods of infertility, more concomitant disorders, and increasing severity of those disorders (Table 2).
Prevalence of Psychological Symptoms in Infertile Chinese Men and Their Medical Histories (N = 771).

Note. ART = assisted reproductive techniques.
Multiple logistic regression analysis was conducted to identify the risk factors associated with depression, anxiety, and a combination of both psychological symptoms in Chinese men with infertility in the current study. Numbers of concomitant disorders were identified as a risk factor for depression (OR = 1.47; 95% CI [1.14, 1.90]; p < .01) and both depression and anxiety (OR = 1.56; 95% CI [1.17, 2.08]; p < .01); and infertility for 2 years and longer was identified as a risk factor for anxiety (OR = 3.94; 95% CI [1.20, 12.93]; p < .02), respectively (Table 3).
Prevalence of Psychological Symptoms and Associated Risk Factors in Infertile Chinese Men (N = 771).
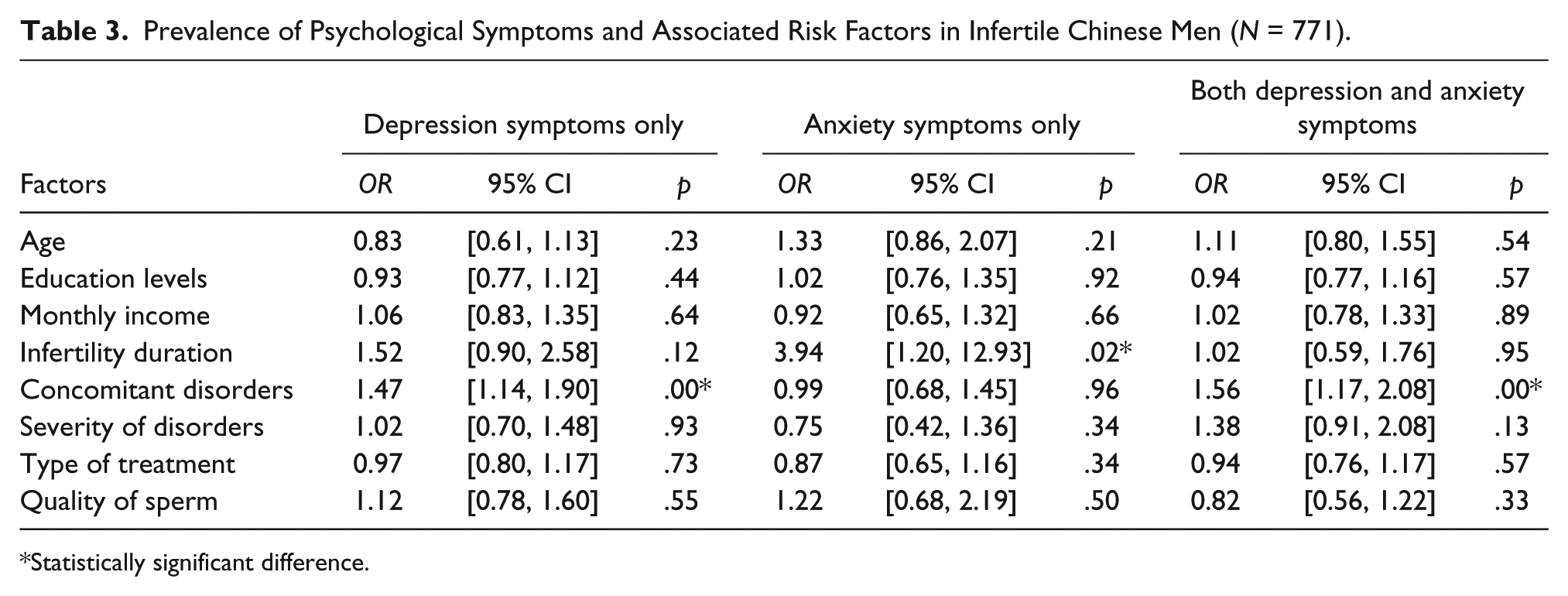
Statistically significant difference.
Discussion
The prevalence estimates of depression and anxiety in adult men with infertility were varied in different studies. Results from the current survey identified that 44% of participants diagnosed with infertility had psychological symptoms. The prevalence of depression, anxiety, and a combination of both psychological symptoms was 20.8%, 7.8%, and 15.4%, respectively. The prevalence of depressive symptoms in the current study was close to the Polish result and while the prevalence of anxiety symptoms was similar to most of the studies mentioned above except for the Chinese one with a very high prevalence. The discrepancy likely results from different survey methods used in the current study versus Gao et al.’s (2013) study rather than ethnic and demographic differences. The current survey focused on assessment of psychological symptoms and risk factors associated with development of psychological symptoms in infertile Chinese men using both MHI-5 and STAI-6 which are considered the most reliable methods for evaluation of mental health status globally. The Self-Rating Anxiety Scale and the Self-Rating Depression Scale survey methods were used in Gao et al.’s (2013) study to investigate sexual dysfunction and its psychological burden and to evaluate a possible correlation between sexual problems and psychological symptoms in infertile Chinese men. Self-Rating Anxiety Scale and Self-Rating Depression Scale used in Gao et al.’s (2013) study were a modified Chinese version (Zhang, 1993), while the MHI-5 and STAI-6 used in current study were the original version. The average age of subjects surveyed was also different in the two studies (28.47 ± 6.29 vs. 32.3 ± 5.6). All these differences could result in the discrepancy between the prevalence of anxiety symptoms observed in the two Chinese studies. A noticeable limit in these studies is that survey subjects were recruited regionally from a single andrology clinic. Thus, large scale and population-based epidemiological surveys are needed in the near future. Nevertheless, depression and anxiety are common problems in men with infertility in China as well as worldwide.
Depressive and anxiety symptoms observed in men with infertility may result from various causes, including unknown etiology, uncertainty of prognosis and treatment outcome, long-term waiting, financial stress related to treatment and counseling, and pressure from peers and sociocultural background (Ogawa, Takamatsu, & Horiguchi, 2011). Peronace, Boivin, and Schmidt (2007) reported that psychological factors also play an important role in male infertility etiology, which affects personality, social behavior, relationship intimacy, and sexual activities. Interaction between psychological stresses and infertility could aggravate both conditions making male infertility a complicated problem to be managed clinically. It is critical to identify some risk factors associated with psychological symptoms for individualized treatment. Beutel et al. (1999) reported that infertile men at relatively young ages had high scores of depression. However, other studies reported high prevalence of depression observed in men at 40 years or older (Kleinberg, Aluoja, & Vasar, 2010; Nicolosi et al., 2011). Results from the current study demonstrate that a high prevalence of depressive symptoms (23.3%) was observed in participants younger than 30 years, while anxiety symptoms was more frequently seen in participants older than 40 years (12.7%). Statistical analysis did not provide evidence that age is a definite risk factor associated with both depressive and anxiety symptoms in this group of Chinese men. A total of 92% of participants in the study were at or younger than 40 years. The authors speculate that the traditional Chinese concept of having babies might only create a moderate psychological burden on the young generation in comparison with the old generation who were rooted to the traditional Chinese ideology that the fatherhood was uppermost in a marital relation. Educational level was considered as a risk factor associated with depression in the general population (Ansseau et al., 2008; Barkow et al., 2003). A person with a high level of education could cope with life stresses in a more optimistic and less depressive manner (Bjelland et al., 2008; Noorbala et al., 2008). Most participants had received education at or above high school (83%). This might be another reason that education level was not a risk factor associated with depressive and anxiety symptoms in the current study.
The results also reveal that male medical disorders are risk factors for infertile men to develop psychological symptoms. The risks for depressive symptoms and both depressive and anxiety symptoms were increased significantly (1.47-fold and 1.56-fold, respectively) in men who suffered from varicocele, epididymal cyst, and ED. The prevalence of depression and depression/anxiety was as high as 27% and 20% in infertile men with three concomitant disorders. Varicocele and epididymal cyst are abnormalities of the male reproductive system during development. Such disorders could affect blood supply to the testes and impair the mechanism of temperature regulation locally, resulting in low quality and reduced amount of sperm (Baazeem et al., 2011). Discomfort and pain caused by the disorders further the psychological burden on patients with infertility. Existing infertility plus extra psychological burden is likely the cause for the increased OR of depression. Many studies reported a high incidence of ED in infertile men (Khademi, Alleyassin, Amini, & Ghaemi, 2008; Song, Kim, Yoon, Hong, & Shim, 2016). ED is a male sexual disorder in which psychological factors play an important role. Inability to erect for insertion and ejaculation has a direct impact on infertility. When the infertile man experiences ED, psychological distress is elevated for both himself and his sexual partner, leading to increased susceptibility to depression and anxiety.
The duration of infertility is another risk factor associated with development of psychological symptoms in infertile men. There was 3.94-fold increased risk of anxiety symptoms (p < .02) and 1.52-fold increased risk of depressive symptoms (p = .12) in participants diagnosed with infertility. The corresponding prevalence of depression and anxiety was observed as 22% and 9%, respectively, in participants who reported not conceiving for 2 years or more. It was reported that anxiety symptoms in infertile women reached its highest level in the second and third year of infertility (Domar, Broome, Zuttermeister, Seibel, & Friedman, 1992). Patients and their partners who had suffered from infertility and received different treatments had their concern over the difficulty of having a baby increased considerably. Anxiety increased as they tried different approaches to solve the problem as they aged. Under the traditional Chinese culture, men bear power and responsibility to add a generation to the family tree. As infertility goes on, failures of various assisted reproductive procedures exacerbates psychological distress substantially. This undoubtedly makes couples with infertility more susceptible to the development of anxiety and depressive symptoms than those without the problem. It seems that the longer the infertility and the more concomitant disorders the patients have, the higher the risk associated with depression and anxiety will be. The reason that long-term infertility increased anxiety symptoms more than depressive symptoms in this study is still unknown. A further study with larger sample size is justified to extend the results.
Type of treatment for infertility was not a risk factor associated with development of psychological symptoms in infertile Chinese men. The prevalence of depressive and anxiety symptoms were more or less similar whether drugs, injections, or assisted reproductive techniques were used for treatment of infertility (Table 2). A previous study reported that women who received in vitro fertilization had a relatively high occurrence of depression or anxiety (Oddens, den Tonkelaar, & Nieuwenhuyse, 1999). However, the current results were different from this report. The authors speculate that men with infertility may not have the strong reactions emotionally and/or underreport their distress to treatment methods for their infertility that women would experience (Peterson et al., 2007). Diagnosis and initiation of assisted treatment were associated with elevated infertility-specific anxiety, and unsuccessful treatment could lead to a state of lasting sadness. However, rates of clinical psychological symptoms in most of these patients were not significantly higher than in the general population (Fisher & Hammarberg, 2012).
Some limitations of the current study are present. Numbers of subjects involved in the survey were relatively small. The study was conducted in one andrology clinic only, though the participants came from different regions across the country seeking medical help for their specific problems because the clinic is the national center for diagnosis and treatment of complex and rare diseases. The MHI-5 and STAI-6 questionnaires were first used in the study without modification for assessment of anxiety and depressive symptoms in infertile Chinese men. Even with the limitations mentioned, the current study discloses the prevalence estimate of depressive and anxiety symptoms as one of two surveys that studied psychological problems of infertile Chinese men. The risk factors associated with depression and anxiety were also analyzed in this special group of Chinese males. Concomitant disorders and infertility duration are identified as significant risk factors associated with psychological symptoms. Thus, andrologists, urologists, psychologists, counselors, and social workers should acknowledge the susceptibility of infertile Chinese men to depression and anxiety when they make a diagnosis and treatment plan for infertility (Li, 2014). The authors hope this study helps to guide a future nationwide survey on the prevalence of psychological symptoms in Chinese men of reproductive age who are dealing with infertility.
Footnotes
Acknowledgements
We are grateful to Mr. Cong Cheng (the Department of Epidemiology, Taishan Medical College, Shandong, China) for his expertise and guidance in statistical analysis. We acknowledge Dr. Tiejun Gao (the University of Alberta, Edmonton, Canada) for his scientific discussion and English editing on the article. We are thankful to Ms. Gayle Simonson (BSc, MA) for her professional editing on English and context checking scientifically in resubmitted version of the article.
Author Contribution
Hong-jun Li and Rong-huan Jiang initiated and completed the study design; Bin Yang, Pu Wang, and Yu-xia Qi collected the data and performed analysis. Bin Yang and Jian-chao Zhang have completed the first draft for review and revise by all other authors.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was supported by Beijing Natural Science Foundation (Grant No. 7162152) and National Natural Science Foundation of China (Grant No. 81370698) and the Open Project of National Health and Family Planning Key Laboratory of Male Reproductive Health (Grant No. 2016GJK01).
