Abstract
The Joint United Nations Program on HIV/AIDS estimates that between 0.3% and 0.7% of adults aged 15 to 49 years were living with HIV in Ecuador in 2013. However, very little is known about the HIV prevalence rate among men who have sex with men (MSM) in that country. A cross-sectional survey was conducted to investigate the knowledge, attitudes, and practices regarding HIV/AIDS as well as to estimate the prevalence of HIV among MSM in one of the cities with high HIV prevalence rates in Ecuador. In this study, questionnaires were administered to 307 adult MSM. An HIV prevalence of 10% was observed. Knowledge about HIV was high; 91% of participants could identify how HIV is transmitted. Although consistent condom use for anal sex was relatively high (89%) among participants who reported having pay-for-service clients, only 64% reported using a condom during oral sex with a client. Participants who had multiple male sexual partners (i.e., their stable male partners plus other partner[s]) had 3.7 times higher odds of testing positive for HIV compared with those who did not. They also had reduced odds of condom use. Participants who were forced to have anal receptive sex had 3 times higher odds of testing positive for HIV. Despite the finding that participants exhibited high knowledge about HIV/AIDS, a high prevalence rate of HIV was observed, which warrants targeted behavioral interventions. These data are consistent with MSM being one of the highest at-risk population groups for HIV in this region of Ecuador.
Keywords
Introduction
Although the prevalence rates of human immunodeficiency virus (HIV) in Latin America remain stable (between 0.2% and 0.7%; De Boni, Veloso, & Grinsztejn, 2014), the epidemic is globally expanding among men who have sex with men (MSM) independent of country or gross domestic product (Beyrer et al., 2012). In 2013, the United Nations estimated that between 0.3% and 0.7% of adults aged 15 to 49 years were living with HIV in Ecuador (The Joint United Nations Programme on HIV/AIDS, 2013). It is well documented that the rates of HIV/AIDS among MSM tend to be higher than in the general population, especially in developing countries (Baral, Sifakis, Cleghorn, & Beyrer, 2007; Montano et al., 2005). A recent study on HIV in the United States reported that more than half of new infections occurred within the MSM community (Goodreau et al., 2012). Little is known about the prevalence rate among MSM living in Ecuador. Previous research conducted in two major cities of Ecuador estimated the prevalence of HIV among MSM to be 14.5% in Quito (Montano et al., 2005) and 27.8% in Guayaquil (Montano et al., 2005). To the best of our knowledge, there are no studies that have explored the rates of HIV testing and/or HIV testing intentions in the country, particularly among MSM.
Ecuador has been noted for having one of the most progressive constitutions in the world giving protection for minorities, including sexual minorities like the lesbian, gay, bisexual, transgender (LGBT) communities (Martínez Dalmau, 2008). It is probable that such constitutional provisions may have helped to decrease stigma and discrimination, which could potentially benefit HIV prevention strategies. In fact, in a recent multicountry study, Henry et al. (2015) reported that approximately 80% of the Ecuadorians living with HIV stated that it was not a mistake to disclose their status to others. While Ecuador has achieved many milestones to ensure the inclusion for all its citizens to receive social services, there is still work to be done. In particular to assess where population needs are concentrated. A report from the Government of Ecuador (The Joint United Nations Programme on HIV/AIDS & Ministerio de Salud Pública del Ecuador, 2010) noted a significant increase in the number of HIV infections since the beginning of the 2000s and even more from 2008 onward. This study focuses on one of the regions with the highest HIV prevalence rates in Ecuador. This region also has a greater proportion of the population living below the poverty line and, therefore, lacks improved access to basic services like water and sanitation, let alone specialized HIV health care services. Data from the Ecuadorian Ministry of Health suggest that the HIV epidemic is still concentrated among most at-risk populations, including MSMs (The Joint United Nations Programme on HIV/AIDS, 2008) .
HIV is a disease of major public health concern in this region of Ecuador but, most importantly, there is a substantial lack of data to facilitate informed, evidence-based decision making and planning to prevent new HIV infections and to provide care for those in current need. Major progress in stemming the tide of this disease will not be achieved until HIV intervention programs are readily available to key populations at higher risk for HIV and for people already suffering from the disease (World Bank, 2012). It has been demonstrated that increased access to health care and medication has improved the life expectancy of persons living with HIV (World Bank, 2012). There are still areas that need significant improvement. Knowledge about the spread of the disease has increased and persons do have greater access to condoms, however, there are still many who are not well informed about HIV and other sexually transmitted infections (STIs) in Ecuador (Cabezas, Fornasini, Dardenne, Borja, & Albert, 2013).
Efforts to obtain baseline data for the MSM population in this region of Ecuador will potentially provide the information needed for policy decision making and planning to formulate strategies for effective HIV/AIDS control within the study area. The aim of this study is to determine the prevalence of HIV among MSM in this region of Ecuador, and to assess HIV/STI knowledge and risk behaviors among them.
Methods
Study Design
A cross-sectional study among selected at-risk populations for HIV/STI was conducted in Ecuador between January and June of 2010. A questionnaire was used to collect relevant sociodemographic data and information regarding knowledge, attitudes, and practices about high-risk sexual behaviors. Questionnaire development as well as the definition of behavioral practices and selection of theoretical frameworks were based on methodological procedures used in other similar studies (Clark et al., 2008; Tabet et al., 2002). The results of this article discuss MSM, one of the selected at-risk populations for HIV/STI.
Study Population
Ecuador is a country located in the northwest region of South America with a per capita income of US$6,290.80 (World Bank, 2015). Its surface area is approximately 245,000 km2 and its population is more than 14 million (Instituto Nacional de Estadísticas y Censos, 2013). This study was conducted in the northwest region of Ecuador, which holds a disproportionate burden of the HIV/AIDS epidemic in the country.
Enrollment Procedure
The local MSM association, which advocates for the protection of its members against employment discrimination as well as provides continuing education in various fields, was pivotal in the enrollment process. After several discussions with representatives from the local MSM association, study personnel were provided with a complete enumerated list of MSM, including 501 registered members. The study coordinator generated a series of random numbers. Members of the MSM association contacted individuals with numbers corresponding to one of the random numbers generated and invited them to the study site, the counseling room of the local Ministry of Health (MOH) health center. The study site had a room separated from the public area to provide privacy to study participants. Confidentiality was better ensured by restricting access to the list to only study staff on a need-to-know basis. Subjects were listed by their nickname or alias. Real identities were not written down and the list was destroyed immediately after all data was collected.
The sample size for the study was estimated based on the following assumptions: (a) an HIV prevalence rate of 19%; (b) an MSM population of 501; (c) an expected response rate of 80%; and, (d) a type 2 error rate of 20%. This yielded an estimated required sample size of 233. The final number of MSM recruited into the study was 307.
Persons were eligible to take part in the study if they were male, 18 years or older, acknowledged having had sex with at least one man during the previous 6 months, and were able to understand the concept of and provided informed consent. Persons were not eligible for participating in the study if they were younger than 18 years (minor), not working or staying in the area, intoxicated at the time of the survey, or for any other reason unable to understand or provide informed consent.
Consenting men were initially met at the study site by a representative from the local MSM association along with a health care professional. After providing informed consent, the health care professional read the questions from the questionnaire to the study participant in private. Health care professionals were native Spanish speakers, the language on which the questionnaires were administered. The men were also asked to provide blood specimens that were tested for HIV. Blood specimens were tested at the Instituto Nacional de Higiene, which is the Ecuadorian MOH’s reference laboratory. Once the specimens were handed over to the Instituto Nacional de Higiene, the MOH followed up with participants about their test results as per standard MOH protocol.
Data Analysis
Questions included demographic information, knowledge of HIV transmission, and sexual practices. Data from the questionnaires and laboratory results were entered in duplicate into an EPI-INFO database and subsequent analysis conducted using STATA version 12. Bivariate analyses using chi-square and Student’s t tests were performed for categorical and quantitative variables respectively, to assess differences between groups. Characteristics and practices that were observed to be significantly associated with HIV test results were adjusted for age and marital status and then odds ratios calculated. All hypothesis tests were two-tailed with a type 1 error rate set at 5%.
Measures
Outcomes were operationalized before analysis. The following outcomes were measured in this study:
HIV (Positive/Negative): Positive if a participant’s blood sample tested positive for HIV and negative otherwise.
Reported Condom Use (Always/Not Always): Participants were asked on the questionnaire “Do you generally use condoms?” with each type of partner that they had. Response choices were “always,” “often (more than half of the time),” “sometimes (less than half of the time)” and “rarely/never.” Participants responding “always,” with each partner that they reported on, were classified as “always” for reported condom use. Otherwise they were classified as “not always.”
Consistent Condom Use (Always/Not Always): Participants were also asked “Did you use a condom the last time you had oral sex?” and “Did you use a condom the last time you had anal sex?” for each type of partner that they had. Response choices were “yes” and “no.” If participants’ reported condom use was “always” and they indicated “yes” for using a condom the last time they had oral and anal sex for each partner that they reported on, then consistent condom use was classified as “always.” Otherwise they were classified as “not always.”
Knowledge
Participants were asked questions on HIV transmission. There were 10 questions in total. Five questions included correctly identifying ways in which HIV can be transmitted such as “Do you think that HIV can be transmitted receiving a blood transfusion?” for which the correct response is “yes.” The other five questions included correctly identifying ways in which HIV cannot be transmitted such as “Do you think HIV can be transmitted by using the same bathroom as someone who is infected with HIV?” for which the correct response is “no.” Correct responses were totaled.
Correctly identified ways HIV can be transmitted: Number of correct responses for the 5 questions on ways that HIV can be transmitted
Correctly identified ways HIV cannot be transmitted: Number of correct responses for the 5 questions on ways that HIV cannot be transmitted
Comprehensive knowledge on HIV transmission: Total number of correct responses for all 10 questions.
Demographics
Participants were asked to provide demographic information. This included questions such as “What is your marital status?” Response choices were “single,” “married,” “cohabitating,” and “divorced/separated.”
Ethical Considerations
The rights of participants were protected throughout the study by adherence to Good Clinical Practices and other requirements as directed by institutional review boards. This cross-sectional survey and the subsequent data analysis were approved by registered institutional review boards in Ecuador (Comité de Bioética, Centro de Biomedicina, Universidad Central del Ecuador) and in the United States (Institutional Review Board, University of South Florida).
Results
Baseline Demographics
The distribution of demographic characteristics of the sample is reported in Table 1. A total of 257 (84%) participants lived in the city, 30 (10%) of them lived in rural areas of the same district where the city is located, and 20 (6%) lived in other districts of the region. Three hundred (98%) participants reported that they lived where they were for more than a year. Participants’ ages ranged from 18 to 56 years with a mean age of 23 years. Most participants (231 or 75%) were single (not legally married and not cohabitating) and only 15 (5%) were married. In all, 215 (70%) participants indicated that they had a stable partner. Although only about half (163 or 53%) of the participants indicated that they had not completed secondary education, the overwhelming majority (277 or 90%) could read and write easily. Slightly more than one third (111 or 36%) of the participants reported that they had a steady job while 231 (69%) reported that they had an income during the previous month. Approximately 142 participants, two thirds of those who indicated that they had an income during the previous month, also indicated that this income was less than or equal to US$240.
Summary of Sample Demographics.
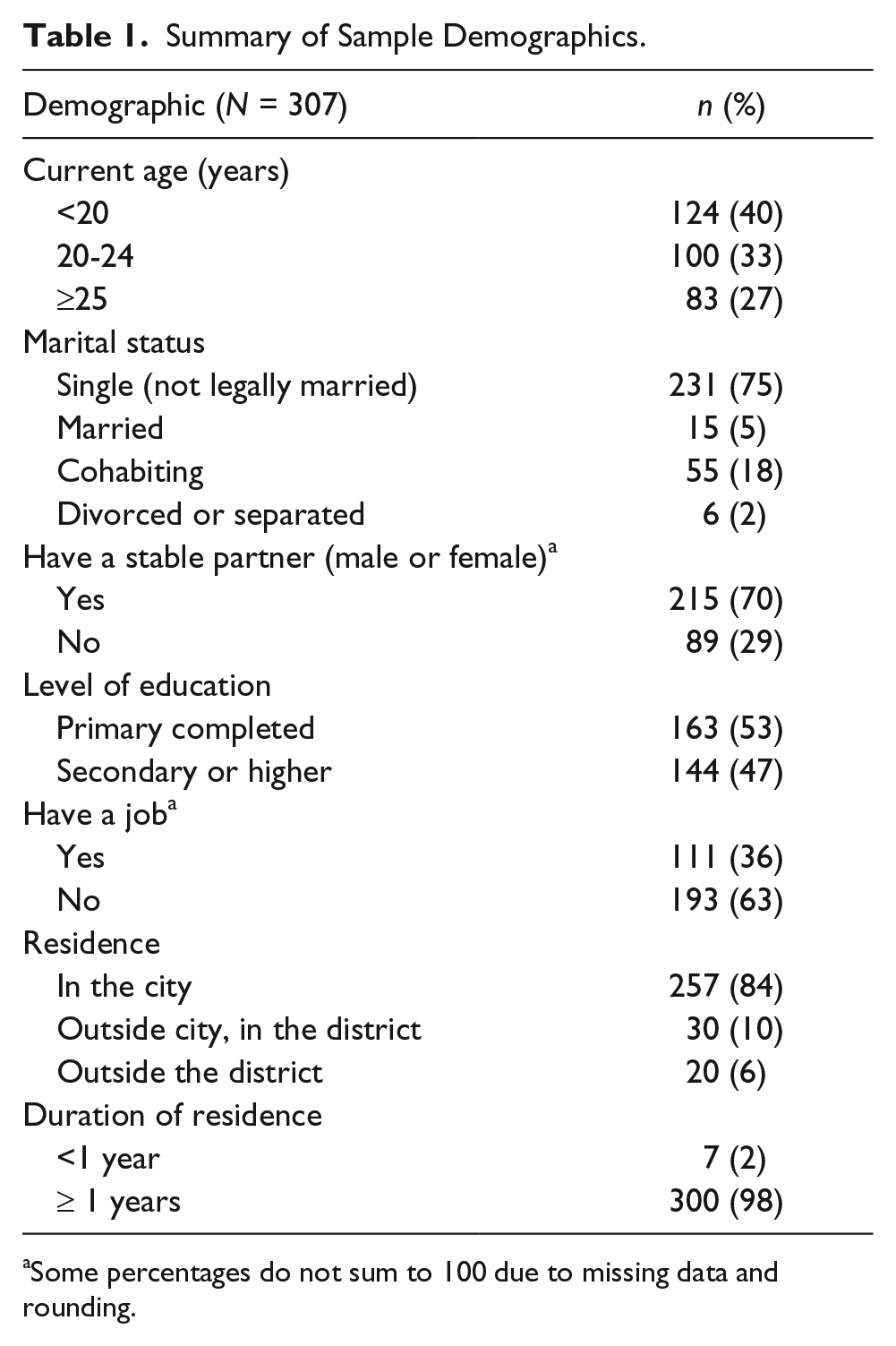
Some percentages do not sum to 100 due to missing data and rounding.
Most (292 or 95%) participants were able to identify and name a disease transmitted by having sex. Participants displayed high knowledge about HIV transmission. A total of 280 (91%) participants knew how HIV/AIDS is transmitted. Answering on average 4.2 out of 5 questions correctly about ways HIV/AIDS can be transmitted, and 3.9 out of 5 questions correctly about ways HIV/AIDS cannot be transmitted.
Responses relating to participants’ male relationships are displayed in Table 2. Twenty-eight (9%) participants indicated that they lived with a male stable partner (MSP). Approximately 50 (16%) reported having sex during the past 30 days with a man who was not their MSP. Some (108 or 35%) reported a history of forced anal receptive sex and 12 (1 in 9) of those men indicated that they had been forced during the past 30 days. Male partners were reported to be MSP (22 or 7%), friends (28 or 9%) and pimps/clients (11 or 4%).
Summary of Participants’ Practices.

Some percentages do not sum to 100 due to missing data and rounding.
Responses relating to participants’ female relationships are also displayed in Table 2. Eighty-one (26%) participants were either married to or living with a woman, and 103 (one third) had sex during the past 30 days with a woman who was not their wife or female stable partner. A little less than half (144 or 47%) of the participants reported having sex with at least one woman during the past 30 days. They also reported that the number of women that they had slept with during the past 30 days ranged from none to 31 women. Fifty-two (17%) participants reported having sex with multiple female partners during the past 30 days.
The level of condom use was higher when the partner was indicated as being a friend compared with when the partner was indicated as being either an MSP or a pimp/client. Reasons given for not using a condom with each type of partner were varied and included: “partner didn’t want to,” “I didn’t want to,” “condoms not available,” or “other.” The most frequent answer given was “partner didn’t want to,” while the least frequent reason provided was “I didn’t want to.” Condom use was consistently lower for oral sex (35 or 42%) as compared with anal sex (55 or 65%) (p < .001).
Approximately 116 (38%) participants had previously taken an HIV test voluntarily. Forty-eight (16%) participants reported having an STI during the past 3 months. Most (223 or 76%) indicated that they would go to the MOH health center or a private clinic if they suspected that they had an STI.
HIV
The prevalence rate of HIV among the study sample was 10.5%. Most (181 or 59%) participants indicated that they had never voluntarily taken an HIV test. Among men who had never voluntarily taken an HIV test, 11 (6%) tested positive for HIV. While among men who indicated that they had voluntarily taken an HIV test, 16 (14%) tested positive for HIV. In bivariate analysis (Table 3), age and marital status were significantly associated with testing positive for HIV. Those who tested positive for HIV were slightly older than those who tested negative. Knowledge about HIV transmission did not display any significant association with testing positive for HIV. Having sex with a woman during the past 30 days, forced anal sex during the past 30 days, and having sex with a non-MSP during the past 30 days were all associated with testing positive for HIV. Tables 3 and 4 report the bivariate associations between characteristics and outcomes, while adjusted rates estimated by logistic regression models are displayed in Table 5. It was observed that those who had sex with a woman during the past 30 days had reduced odds of testing positive for HIV when compared with those who had not. Men who had sex with a non-MSP during the past 30 days had almost fourfold higher odds of testing positive for HIV when compared with those who did not have sex with a non-MSP. Men who had been forced to have anal receptive sex during the past 30 days had threefold higher odds of testing positive for HIV when compared with those who had not been forced to do so.
Bivariate Associations Between Demographic Characteristics and Study Outcomes (HIV and Condom Use).

Note. All values are given as number (percentage).
p < .05 for comparisons across HIV positive and self-reported condom use.; ** p <.05 for comparisions across HIV positive only; ***p < .10 for comparisons across self-reported condom use and consistent condom use.
Bivariate Associations Between Behavioral Practices and Study Outcomes (HIV and Condom Use).

Note. All values are given as number (percentage).
p < .10. for comparisons across HIV positive; **p < .10 for comparisons across self-reported condonm use and p < .05 for comparisons across consistent condom use; *** p < .05 for comparisons across HIV positive, self-reported condom use and consistent condom use; **** p < .10 for comparisons across consistent condom use.
Adjusted Odds Ratios and 95% Confidence Intervals Across Study Outcomes (HIV and Condom Use).

Adjusted for age and marital status. bAdjusted for age.
p < .10. ** p < .05.
Condom Use
Reported condom use was higher than consistent condom use (167 or 54% vs. 134 or 44%; p < .001). In bivariate analysis, none of the demographic characteristics were associated with condom use. Nonetheless, characteristics and practices that were observed to be significantly associated with condom use were adjusted for age, and odds ratios calculated (Table 5). Participants’ knowledge of HIV transmission was associated with reported condom use. Participants’ mean knowledge score was higher among participants who reported always using a condom compared with those who reported not always using a condom. Consistent condom use was not associated with participants’ knowledge of HIV transmission. Men who lived with an MSP had reduced odds of reporting always using a condom as well as consistently always using a condom when compared to men who did not live with an MSP. Men who reported having sex with a man who was not their MSP during the past 30 days had reduced odds of reporting always using a condom and consistently always using a condom when compared with men who did not report having sex with men other than their MSP. While type of partner was not associated with reported condom use, it correlated with consistent condom use. Men who had sex with friends had increased odds of consistent condom use being always when compared with men who only had sex with an MSP during the past month.
Discussion
HIV
One aim of this study was to get some baseline information on the HIV status among the MSM population in the Northwestern region of Ecuador. Another aim of the study was to identify the risk factors associated with HIV among MSM. Younger MSM (<20 years) and older participants (≥25 years) had lower odds of testing positive for HIV when compared with MSM between the ages of 20 and 24 years. The lower odds among MSM younger than 20 years can be explained by their lack of sexual experience. It is therefore, imperative to have interventions for younger MSMs in order to reduce their likelihood of engaging in risky behavior and of acquiring new infections.
The findings in this study are consistent with a study conducted among MSM and transgender women in Ecuador which reported that persons who engaged in transactional sex were more likely to test positive for HIV when compared with those who had never engaged in transactional sex (Solomon et al., 2014). When asked to discuss reasons for not using condoms with each partner category (MSP, friend, pimp, or client), participants most frequently indicated that the reason for not using a condom was due to the partner’s desire to not use one. The participants’ desire to not use one was identified least frequently as the reason for not using a condom. This suggests a disparity of power in these types of relationships. Power disparity in relationships, as well as other types of disparities, have been noted to influence HIV transmission rates. Gant et al. (2012) noted that HIV diagnosis rates increased as income inequality rose among adults and adolescents between 2006 and 2008 in the United States. Many articles also discussed power disparities in heterosexual relationships and the difficulty experienced by women in negotiating safer sex practices with their partners (Clüver, Elkonin, & Young, 2013; Durevall & Lindskog, 2012; Volpe, Hardie, Cerulli, Sommers, & Morrison-Beedy, 2013). It is reasonable to expect similar issues to exist in the relationships among MSM. For instance, Mustanski et al. reported that disparities in relationships including those due to age and forced sex tend to be associated with increased HIV diagnosis (Mustanski, Newcomb, & Clerkin, 2011). This correlates with the findings of this study in which MSM having been forced to sustain anal sex were more likely to be HIV positive. Similarly, in a study among MSM, Balaji et al. (2013) reported that power disparities explained by race and educational status were more strongly associated with HIV infection than with individual risk behaviors. Altogether, this data would strongly support the inclusion of condom negotiation skills as well as access to condoms as part of basic health care services provided to the population, especially MSMs. In fact, Baral et al. noted in their 2007 meta-analysis that MSM appear to be an underserved population in many low- and middle-income countries.
Only 116 (38%) study participants had previously taken an HIV test voluntarily. This proportion is much smaller than that reported in the 2011-2012 study conducted among MSM in Guayaquil, Ecuador (Sánchez-Gómez et al., 2015). In that study, investigators reported that 54% of their participants had previously been tested for HIV (Sánchez-Gómez et al., 2015). In this study, 11 (6%) men who had not previously taken an HIV test yielded positive results for HIV. Altogether this data suggest that it is important to encourage sexually active men, regardless of how they identify their sexual orientation, to know their HIV status. A report published by the Centers for Disease Control and Prevention (CDC) in 2013 identified that approximately 33% of MSM who were unaware of their status engaged in unprotected sex (CDC, 2013). Encouraging HIV testing is a key component of HIV/STI prevention strategies as the rate of unprotected sex among persons unaware of their status is more than twice as high as the rate among those who were aware of their status (CDC, 2013).
It is well documented that stigma and discrimination are barriers to persons accessing health care services. Ecuador is known as a country with legislation and constitutional provisions that have been updated to provide inclusion for all persons. The target sample size for this study was estimated to be 233; however, 307 persons were recruited. This suggests that MSM in Ecuador feel comfortable participating in research even answering questions of a personal nature. In fact, the recruited sample population was comfortable with answering the questionnaires, not least because there was intense and close work with the local MSM association to facilitate communication with its members. This provided strength to this research, which resulted in the joint development of best practices for conducting research within this community.
Men married to women and who also have sex with other men continue to provide a bridge through which HIV might spread between the MSM and the general population (Setia, Sivasubramanian, Anand, Row-Kavi, & Jerajani, 2010). Although participants were not asked to identify their sexual orientation it can be estimated that at least 138 (45%) of them were behaviorally bisexual, based on their responses. Other researchers have reported varying proportions of MSM identifying as bisexual. These rates range from about 35% (Gutiérrez, Molina-Yepez, Morrison, Samuels, & Bertozzi, 2006) to 60% (Kim et al., 2013). A high proportion of bisexual men report inconsistent condom use in their heterosexual relations (Lau et al., 2008). To be eligible, participants identified themselves as MSM who had sex with a man during the past 6 months. However, approximately 81 (26%) participants indicated being married or living with a woman, 103 (34%) indicated having had sex with a woman who was not their wife or stable partner, and 138 (45%) indicated that they had had sex with a woman during the past 30 days. This data suggest that at least a proportion of the local MSM population could be serving as a bridge between MSM and the general population. In their 2011 study conducted in El Salvador among bisexual men, Kim et al. noted that bisexual behavior was associated with other risky sex behaviors with both male and female partners (Kim et al., 2013). It was further noted that bisexual men demonstrated a distinct identity and were in need of tailored interventions (Kim et al., 2013).
In this study, the estimated HIV prevalence among MSM living in this region of Ecuador was 10.5% which compares with 14.5% reported in similar population in Quito, the capital city of Ecuador, and to 27.8% in Guayaquil, the main port of Ecuador (Montano et al, 2005). Similarly, the HIV prevalence rate observed among MSM in this study is lower than the estimates for other South American regions including the ones reported by Bautista et al. in 2004 for Ecuador (16.6%), Peru (11%), Colombia (19.7%), Bolivia (20.6%), Argentina (14.5%), Uruguay (16.9%), and Paraguay (13%). Noteworthy, the latter study in South America was conducted on data from 1999 to 2002, which are the earlier years of the epidemic and probably when prevention methods had not been scaled up. That might partially explain why the rates reported in this study are relatively lower. Additionally, the study by Bautista et al. (2004) had a different recruitment strategy whereby MSMs were recruited in specific venues like discos, bars, and streets (for commercial male sex workers) which may result in a selection bias leading to high-risk subpopulation groups.
Condom Use
Interventions for safer sex practices to reduce HIV and STI transmission have typically been aimed at increasing condom use. To that effect, researchers have tried to identify factors that correlate with condom use. Fifty-six (18%) participants reported always using a condom with their MSP, although only 39 (13%) reported consistent condom. These findings are lower than previous reports (Sánchez-Gómez et al., 2015).
In the same study by Sánchez-Gómez et al. (2015) among MSM, 6% reported consistent condom use with female partners, which differs from the findings of this study on condom use with female partners. In this study 130 (42%) participants indicated “always” for self-reported condom use with occasional female partners, whereas 118 (38%) indicated “always” for consistent condom use with occasional female partners. Condom use was lowest with female stable partners. Only 80 (26%) MSM indicated “always” for self-reported condom use with their female stable partner. These statistics suggest that practices among the MSM population of Ecuador are varied across geographical locations and are likely confounded by incorrect perceptions of what constitutes risky behaviors based solely on the type of sexual partner.
Inconsistent condom use remains a large barrier to overcome in the fight to curb the spread of this disease. Although participants appear to have intentions for safer sex practices, they would seem to lack self-efficacy since they do not use condoms as frequently as they report to. This is demonstrated in the disparity between the rates indicated for self-reported condom use being “always” (167 or 54%) and consistent condom use being “always” (134 or 44%). These results correlate with previous studies among Ecuadorian MSM which have reported that 55% of subjects had unprotected sex with their last 3 partners (Gutiérrez et al., 2006; Jacobson et al., 2014). Moreover, a positive association between condom use and education attainment was observed in the same studies (Gutiérrez et al., 2006; Jacobson et al., 2014).
The quality of knowledge among MSM is concerning and how this knowledge translates into practice appears to be substantially lacking. In this study, an association between knowledge about HIV/AIDS transmission and condom use was observed. In fact, participants appeared to perceive risk differently depending on the sex act. Twenty (42%) of the participants who indicated that they did not use a condom during their last oral sex act reported that they always use a condom. Seven (24%) of the participants who indicated that they did not use a condom during their last anal sex act reported that they always use a condom. In addition, 11 (15%) of the participants who indicated that they did not use a condom during their last sex act with an occasional female partner reported that they always use a condom. This suggests that while MSM may have knowledge about safer sex practices and condom use, they may not recognize the need to employ condoms for various sex acts due to their perception of the risk associated with that act. These results bring into focus the need for HIV/AIDS/STI prevention programs in Ecuador and other regions to help curb their spread. (Jacobson et al., 2014; Kim et al., 2013).
Limitations
This study has some limitations. It is possible that some of the results may have been affected by social desirability bias. This can be defined as the over reporting of responses deemed as being the accepted norm and underreporting of those deemed not to be acceptable. Social desirability is also more prevalent among studies involving personal topics such as sexual practices (Krumpal, 2013). Furthermore, studies in which persons are not anonymous are more likely to include this type of bias (Grimm, 2010; Krumpal, 2013). In this study, condom use with female partners was much higher than rates reported in previous literature such as the one conducted by Sánchez-Gómez who utilized computer-assisted self-interviews for data collection (Sánchez-Gómez et al., 2015). Future studies utilizing other data collection methods are needed to further explore the issues related to MSM in Ecuador. Data reported in this study represents information about the local MSM community. In order to further explore issues related to HIV among MSM in Ecuador, additional studies expanded to other geographical areas are needed to compare needs according to areas, which may vary greatly in culture and practices.
Footnotes
Acknowledgements
The authors would like to acknowledge the support offered by the different institutions that made this work possible, including Universidad San Francisco de Quito, University of South Florida, Baylor College of Medicine, Fundación Raíces, the local MSM Association, the Secretaría de Educación Superior, Ciencia, Tecnología e Innovación del Ecuador (SENESCYT), and the local branch of the Instituto Nacional de Higiene Leopoldo Izquieta Perez, Ecuador.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
