Abstract
Despite improvements in oral health status in the United States, pronounced racial/ethnic disparities exist. Black men are less likely to visit the dentist, are twice as likely to experience tooth decay, and have a significantly lower 5-year oral cancer survival rate when compared to White men. The Minority Men’s Oral Health Dental Access Program employed a community-based participatory research approach to examine the oral health barriers and opportunities for intervention among Black men in a low-income, urban neighborhood. A cross-sectional study design was implemented through a self-administered survey completed among 154 Black males. The majority reported not having dental insurance (68.8%). Most frequently cited oral health care barriers were lack of dental insurance and not being able to afford dental care. Attitudes related to the significance of dental care centered on cancer prevention and feeling comfortable with one’s smile. The impact of oral health on daily life centered on social interaction, with men citing insecurities associated with eating, talking, and smiling due to embarrassment with how their teeth/mouth looked to others. Multivariate logistic regression revealed that those who had difficulty finding dental care were 4.81 times (odds ratio = 4.65, 95% confidence interval [1.80, 12.85]) more likely to report no dental insurance, and 2.73 times (odds ratio = 3.72; 95% confidence interval [1.12, 6.70]) more likely to report poor oral health. Community-based participatory approaches include assessment of neighborhood residents affected by the health issue to frame interventions that resonate and are more effective. Social, physical, and infrastructural factors may emerge, requiring a multilevel approach.
Introduction
Racial/ethnic minorities, men, individuals of lower socioeconomic status, and those with chronic illnesses and disabilities are among the most disadvantaged populations with respect to oral health care and access (Sabbah, Tsakos, Sheiham, & Watt, 2009; Zabos et al., 2008). Severe oral health conditions are higher among men when compared to women, and the prevalence of periodontitis was recently reported to be significantly higher among men than women overall, with findings that persisted across racial/ethnic groups (Centers for Disease Control and Prevention, 2011). Black men aged 35 to 44 years experience untreated tooth decay nearly twice as much as White men (Dye, Li, & Thornton-Evans, 2012; Satcher, 2003). Even more alarming is that while oral cancer incidence rates are steadily declining for all races, mortality rates for oral cancer are increasing among Black men (Bunnell et al., 2010; Howlader, Noone, & Krapcho, 2011). The unique social experiences of Black men, one of the most disadvantaged racial/ethnic and gender groups, warrants targeted attention due to increased unemployment, incarceration, discrimination, and homicide, all of which disproportionately increase rates of unhealthy behaviors and premature mortality (Jackson & Williams, 2006; Xanthos, Treadwell, & Holden, 2010; Young, Meryn, & Treadwell, 2008).
The causes of racial disparities in oral health are multifaceted and include inadequate access to dental care and unmet dental care needs (Jones et al., 2013). Affordability of dental care and low SES have been considered independent risk factors for poorer oral health (Buchwald et al., 2013; Finlayson, Williams, Siefert, Jackson, & Nowjack-Raymer, 2010). A recent longitudinal study confirmed the impact of SES on an individual’s ability to maintain good oral health and reported statistically significant associations between low SES, educational attainment, and oral health outcomes of periodontitis and tooth loss (Buchwald et al., 2013). Lack of dental insurance and dental insurance limitations are barriers to receiving dental care (Vujicic & Nasseh, 2014).
The Florida Dental Care study identified that attitudes around the importance of dental health are a determinant of dental care usage, and it reported a predominance of negative attitudes among the low-income Black population (Gilbert, Shelton, Chavers, & Bradford, 2003). Despite the negative attitudes toward dental care, the majority believed that dental visits are extremely important or that they are necessary to prevent dental problems (Gilbert et al., 2003). Studies have reported that awareness of dental service availability and dental attitudes related to care had a significant impact on an individual’s utilization of oral health care (Locker, 2009; Ramraj & Quiñonez, 2013).
To address oral health disparities, researchers have examined the effect of community characteristics on intragroup variations in oral health among Blacks. Researchers reported significant variations in the level of self-reported oral health among low-income Black neighborhood clusters indicating that, among them, there are characteristics that determine their relative ability to maintain good oral health (Finlayson et al., 2010). Others have identified the independent contributions of neighborhood disadvantage and individual SES to poor oral health. After adjusting for individual characteristics, residents of socioeconomically disadvantaged neighborhoods were significantly more likely than those in more advantaged neighborhoods to indicate that their oral health as poor (Turrell, Sanders, Slade, Spencer, & Marcenes, 2007).
The Current Study
To address the aforementioned oral health disparities experienced among Black men, The Minority Men’s Oral Health Dental Access Project (MOHDAP) was established as a pilot community-based participatory research (CBPR) program led by a community-based organization (CBO) in partnership with an academic institution, thus reversing the typical role of academia to serve as the lead in a CBPR project. The CBO and grant recipient was the Pittsburgh Community Improvement Association (PCIA). PCIA is a neighborhood-based, resident-led community development corporation formed to address housing and neighborhood revitalization issues in Atlanta’s blighted, historically Black Pittsburgh neighborhood. Established in 1883, Pittsburgh is one of Atlanta’s oldest remaining in-town neighborhoods. The working-class Black community was named Pittsburgh because the land south of the rail shops was so smoky and polluted that it resembled the steel mills of Pittsburgh, Pennsylvania. The Morehouse School of Medicine Prevention Research Center (MSM PRC) leads and supports community-engaged research and was the primary partner supporting program planning, implementation, data entry, and analysis. Both organizations espouse a CBPR approach in the development of health initiatives and have worked conjointly toward this goal for the past 10 years.
CBPR is a research approach that emphasizes community–academic partnership and shared leadership in the planning, implementation, evaluation, and dissemination of program processes and outcomes. Among the advantages of CBPR are strengthened neighborhood–campus relationships, improved research question relevance, enhanced research recruitment, implementation, collective dissemination, and shared benefit for a diverse group of stakeholders (Cargo & Mercer, 2008; Jagosh et al., 2012; Seifer, 2006). Conceptually, it is anticipated that through using CBPR, outcomes will include not only answering a research question but also addressing community-identified social, economic, or policy concerns (Israel, Parker et al., 2005; Wallerstein & Duran, 2010).
Prioritized communities were composed of four Metropolitan Atlanta Neighborhood Planning Units (NPUs). The City of Atlanta is divided into 25 NPUs within which citizen advisory councils are organized, representing a preexisting community leadership structure through which to partner in developing and implementing the intervention. The preexisting leadership structure of the NPUs, established in the 1970s, represented existing neighborhood strength among concerned citizens who have been at the helm, as senior partners, in leading CBPR with the MSM PRC since 1998. In its efforts to develop interventions to address health disparities and inequalities, the MSM PRC partnered with NPUs experiencing the greatest morbidity and mortality rates for chronic diseases and infections in the City of Atlanta (Lee, Leous, Botchwey, Guhathakurta, & Kennedy, 2012).
Prioritized NPUs (V, X, Y, and Z) represent increased poverty, a lack of neighborhood resources, and a plague of chronic diseases. At the aggregate level, 88% of these NPU residents are Black, young (median age, 30 years), and poorly educated (26% of adults did not complete high school). Of Black households within the four aforementioned NPUs, 40.9% live below the poverty level (Federal Poverty Guidelines, 2013).
To ensure a CBPR approach for MOHDAP, an advisory board was created with partner NPU residents at its core, along with agency and academic members. Based on the MSM PRC’s Community Coalition Board (CCB) model, the board governance structure stipulated that neighborhood representatives were always in the majority and that the chair, vice-chair, and secretary seats were filled by neighborhood representatives (Akintobi, Goodin, Trammel, Collins, & Blumenthal, 2011; Blumenthal, 2011a, 2011b). In any vote that pitted neighborhoods against academics and agency members the neighborhood members always maintained the majority of votes. The MOHDAP board’s purpose was to (1) set policy and oversee operations, (2) identify priorities and approve approaches, (3) create intervention awareness through dissemination to the partner organizations and agencies represented by the project, and (4) develop a strategic plan by which the intervention would achieve its objectives.
The MOHDAP board was involved in each step of the assessment process. First, they convened to identify and agree on oral health priorities and themes to be included in the assessment. The MSM PRC concurrently reviewed existing literature and reports in order to identify potential items to be included in the survey. Second, MSM PRC staff presented all potential surveys, related content, and each survey’s origin, including intended audience and purpose to the board. During this forum, each question was vetted, by category, to determine face validity, relevance, and meaning toward inclusion in the final survey. Next, the final survey was pilot-tested among members through a focus group to identify issues related to respondent burden, consistency with survey goals, and culturally relevant language. Community-led survey administration training, recruitment, and data collection were also central methodological elements that are detailed in the section that follows. The main objectives of this study were to conduct an assessment (1) to evaluate baseline oral health needs, attitudes, and barriers to care and (2) to identify access barriers in finding dental care among urban, Black men in low-SES communities toward development of a community-driven intervention.
Method
Data Collection
The study employed a cross-sectional design through administration of a 35-item survey to a convenience sample of Black men between January 2013 and May 2013. The study protocol, design, and intervention were developed, reviewed, and approved by the MOHDAP advisory board. The Morehouse School of Medicine’s institutional review board (IRB) reviewed and approved the project due to the MSM PRC’s role in data entry, analysis, and dissemination.
Recruitment and Survey Administration
Three MOHDAP board members and six partner community residents received MSM PRC training in participant recruitment and survey administration toward engaging residents in completion of the assessment at regularly occurring community events from the MSM PRC staff. MOHDAP board members and partner community residents were not paid for their participation in data collection. An average of 10 volunteer hours was estimated for data collection. Through established relationships with CBOs, participants were recruited at preexisting community meetings and events attended by members of the CCB or that serve predominantly urban, low-income, Black men. Participants were also recruited through flyers, referrals, and word of mouth. Interested community residents who met the inclusion criteria completed self-administered paper-and-pencil surveys. Trained MOHDAP board members and partner community residents were on-site and available to answer any questions that arose during completion of surveys. Participants received a $10 gift card for completion as an incentive for participation.
Sample and Study Population
Inclusion criteria for this study were Black men 18 years old or older. Black men were selected as priority population based on statistics that Black men experience the highest rate of dental disorders compared to White men and Black women (Centers for Disease Control and Prevention, 2011). Although 220 participants initially registered for the survey, 154 residents completed the survey questionnaires.
Measures
As previously detailed, the MOHDAP Oral Health Needs Assessment was finalized following a CBPR process that included oral health theme prioritization, review of several surveys by the board and MSM PRC, and subsequent pilot-testing of the survey tool. Sociodemographic information such as age (≤30 years old, >30 years old), annual income (≤$10,000, >$10,000), education (less than high school, completed high school or GED, some college/bachelor’s), employment status (full-time, part-time, unemployed, school), financial situation (unsatisfactory, satisfactory), dental insurance (yes, no), self-reported oral health status (poor, good/excellent), and last dental visit (≤1 year ago, >1 year ago) were assessed with a single item. Age of participants was dichotomized based on the average age of residents in the community. Marital status was grouped as single/never married, divorced/widowed, and married/cohabitating. Due to the impact of SES on an individual’s ability to maintain good oral health, participants’ financial situation was measured with one item asking, “Which of these statements best describes your present financial situation?” Participants were asked to choose one answer from the following responses: “I really can’t make ends meet,” “I manage to get by,” “I have enough to manage, plus some extra,” and “Money is not much of a problem; I can buy about whatever I want.” Financial situation was dichotomously coded as: “unsatisfactory” (“I really can’t make ends meet”) and “satisfactory” (“I manage to get by,” “I have enough to manage, plus some extra,” or “Money is not much of a problem”). All sociodemographic questions were adapted based on previously administered Center community health needs assessments, through which all questions were pilot-tested among community residents to ensure face validity and cultural relevance.
Attitudes Toward Dental Care
Attitudes toward dental care were assessed with items adapted from the Florida Dental Study Baseline Survey (1993). This instrument was used to collect information from North Florida residents regarding their dental health challenges. A reliability analysis was performed among the items to determine their internal consistency and resulted in an overall Cronbach’s alpha reliability coefficient of .8700. Interitem correlations were performed within the scales to determine the level of internal cohesion. The final factor analysis indicated that the first four factors accounted for just over 78% of the variance in the model. The loadings of the factors were consistent with the constructs being measured.
A series of questions and statements were posed to assess participants’ attitudes related to oral health and dental care with items also adapted from previously validated instruments including the Florida Dental Study Baseline Survey and the Chicago Dental Health Survey (Clancy & Wadhawan, 2009; Gilbert et al., 2003). To assess attitudes regarding the importance of dental care the following question was asked, “Why do you feel it is important to receive dental care?” Participants were asked to review a list of five statements related to reasons why they felt dental care was important, including “to relieve pain,” “to stop bad breath,” “to fix bad habits,” “to be comfortable with smile,” and “to prevent oral cancer.” The response options for each item included disagree, neutral, and agree. To examine attitudes related to preventive oral care, participants were asked to agree or disagree with each item in a list of statements related to dental care costs, keeping and caring from one’s natural teeth rather than pulling them, and being active in decisions about their dental care, among others. To explore participants’ experiences related to oral health care and its impact on daily life, participants were asked, “Have you ever in the past 6 months?”: “tried not to talk,” “smile,” “chew,” and so on, due to oral health problems, discomforts, or insecurities. Response options included never, sometimes, and often.
Neighborhood Characteristics
To determine men’s access to dental care, data about the number of dental offices in each NPU were obtained from the online National Yellow Pages directory using each corresponding zip code. Forty-five dental offices were identified. Neighborhood dental care availability was stratified into two categories based on mean number of dental offices per NPU (≤10 dental offices per NPU vs. >10 dental offices per NPU).
Difficulty in Finding Dental Care
The main outcome measure was difficulty in finding dental care. This variable was based on dichotomous responses to the question “Is it difficult to find dental care?” (“Yes” or “No”).
Data Analysis
Frequencies were employed to examine sociodemographic characteristics and other independent predictor variables related to dental care or oral health. Chi-square analyses were used to evaluate differences between two subgroups of respondents (difficult to find dental care vs. not difficult to find dental care). Univariate and multivariate logistic regressions were employed to identify independent predictors of difficulty in dental care. Sociodemographic variables and other independent variables including dental insurance, self-reported oral health status, and last dental visit, which were significant in the univariate model, were then entered in the multivariate model. Factors significant at p < .05 were considered when examining the association between the outcome and the group. Statistical analyses were carried out using SAS Version 9.2 (SAS Institute Inc, Cary, NC).
Results
Demographics
Table 1 presents respondent demographic characteristics for the total sample (N = 154) and by subgroups based on the outcome variable (difficulty in finding dental care). One third of respondents reported their financial situation as unsatisfactory, and over half of respondents (57.3%) indicated an annual family income of less than $10,000. The majority of respondents reported not having dental insurance (68.8%). There were no significant demographic differences between those with difficulty compared to those without difficulty getting care.
MOHDAP Needs Assessment Participant Demographic Characteristics.

Note. MOHDAP = Minority Men’s Oral Health Dental Access Project; NPU = Neighborhood Planning Units.
p < .05.
Among residents who reported having dental insurance, the largest proportion had Medicaid coverage (42.6%), followed by dental coverage through employment (36.2%) and the Department of Veterans Affairs (12.8%). As well, nearly 71% had had adult teeth removed, with 9.8% reporting one tooth, 46.2% reporting between two to six teeth, and 14.4% having all adult teeth removed. There was no significant difference between alcohol and smoking rates between the two groups.
Barriers to Finding and Regularly Seeing a Dentist
The most frequently cited barriers to oral health care were not having dental insurance (26.5%) and not being able to afford dental care (19.4%). Other barriers reported were related to access, which included not knowing where to go for dental service (10.4%), lack of transportation (5.9%), proximity to the dentist (3.6 %), and the provider not taking their dental insurance (6.6%). When asked to identify where they sought routine care, the bulk of respondents indicated not having a dentist for routine care (46%) or seeking care through acute service or low-cost facilities (e.g., hospitals, social programs, public health clinics; 21.9%). The majority of participants (89.4%) also cited having negative experiences at previous dental visits. Reasons cited for not visiting the dentist included not liking injections or the dental drill. Some participants were not comfortable with what the dentist would say about the status of their teeth, while others said that generally bad experiences, primarily defined as having discomfort or pain at the dentist, made them reluctant to see a dentist regularly.
Factors Associated With the Importance of Dental Care
Most respondents (80%) felt that dental care was important for the prevention of oral cancer (Figure 1). The next highest proportion of respondents cited dental care being important to feel comfortable with their smile (71%). These factors were closely followed by the priorities of preventing bad breath, bad habits that cause harm, and then desire to remove pain.
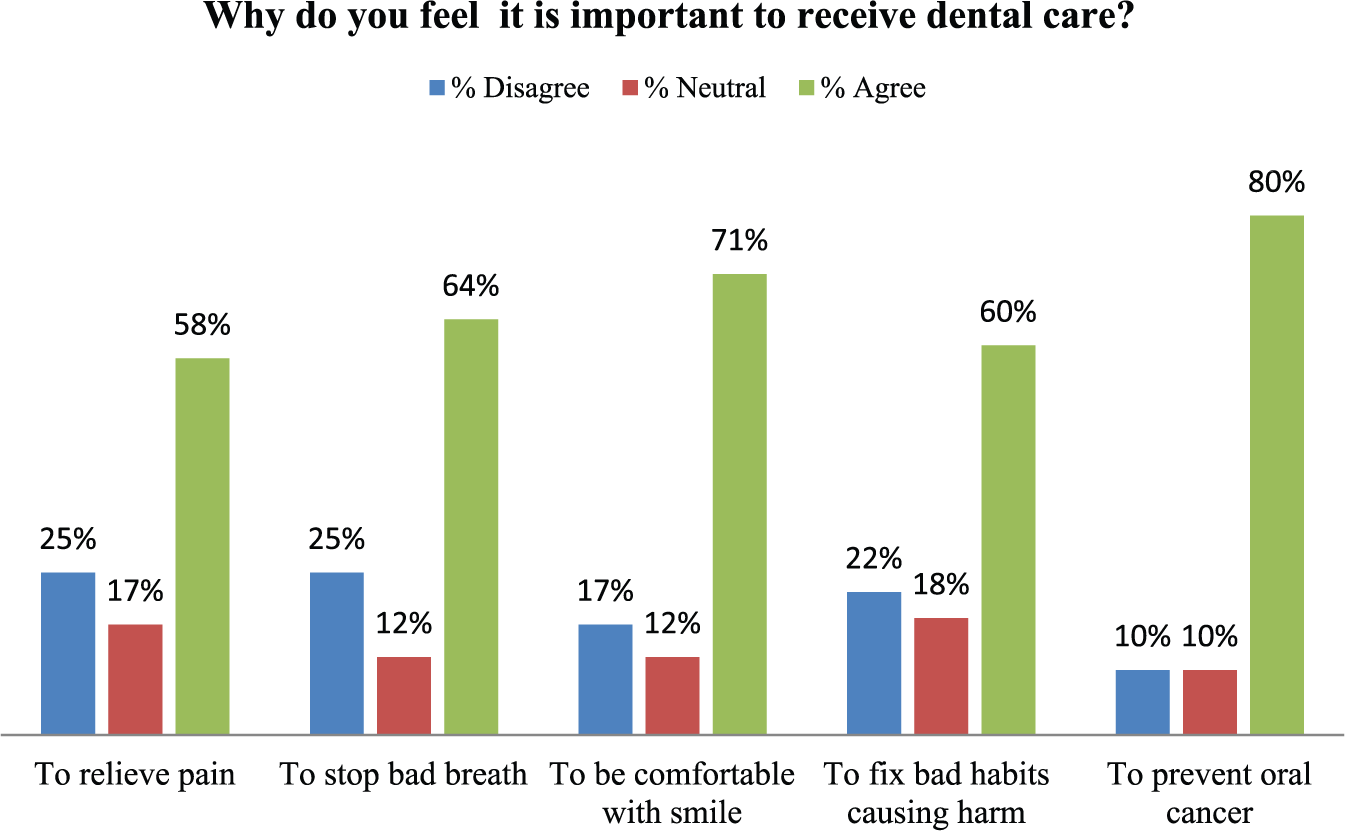
Attitudes regarding the importance of dental care.
Dental Care Attitudes
The majority of men (91%) wanted to be active participants in their dental care decisions (Figure 2). An equal proportion felt that it is important to keep natural teeth (88%) and that brushing and flossing were important for oral health (88%). Despite previously cited financial barriers to finding and regularly seeing a dentist, most (74%) felt that the care they received was worth the cost.

Attitudes related to preventive oral health care.
Perceptions of the Impact of Oral Health on Daily Life
While most respondents, across categories, responded never, it is noteworthy to rank the types of responses in the often category (very often and fairly often; Figure 3). The largest proportion of men often felt discomfort in trying to chew hard things (35%) or were unable to eat the foods they liked because of their teeth, dentures, or gums (24%). Other respondents often tried not to talk (26%) or smile (24%) because they felt that they had unattractive teeth and/or gums or were simply embarrassed by how they looked (22%). These responses are well aligned with aforementioned attitudes related to the social implications of dental care, with the second highest proportion of responses associated with being comfortable with one’s smile.
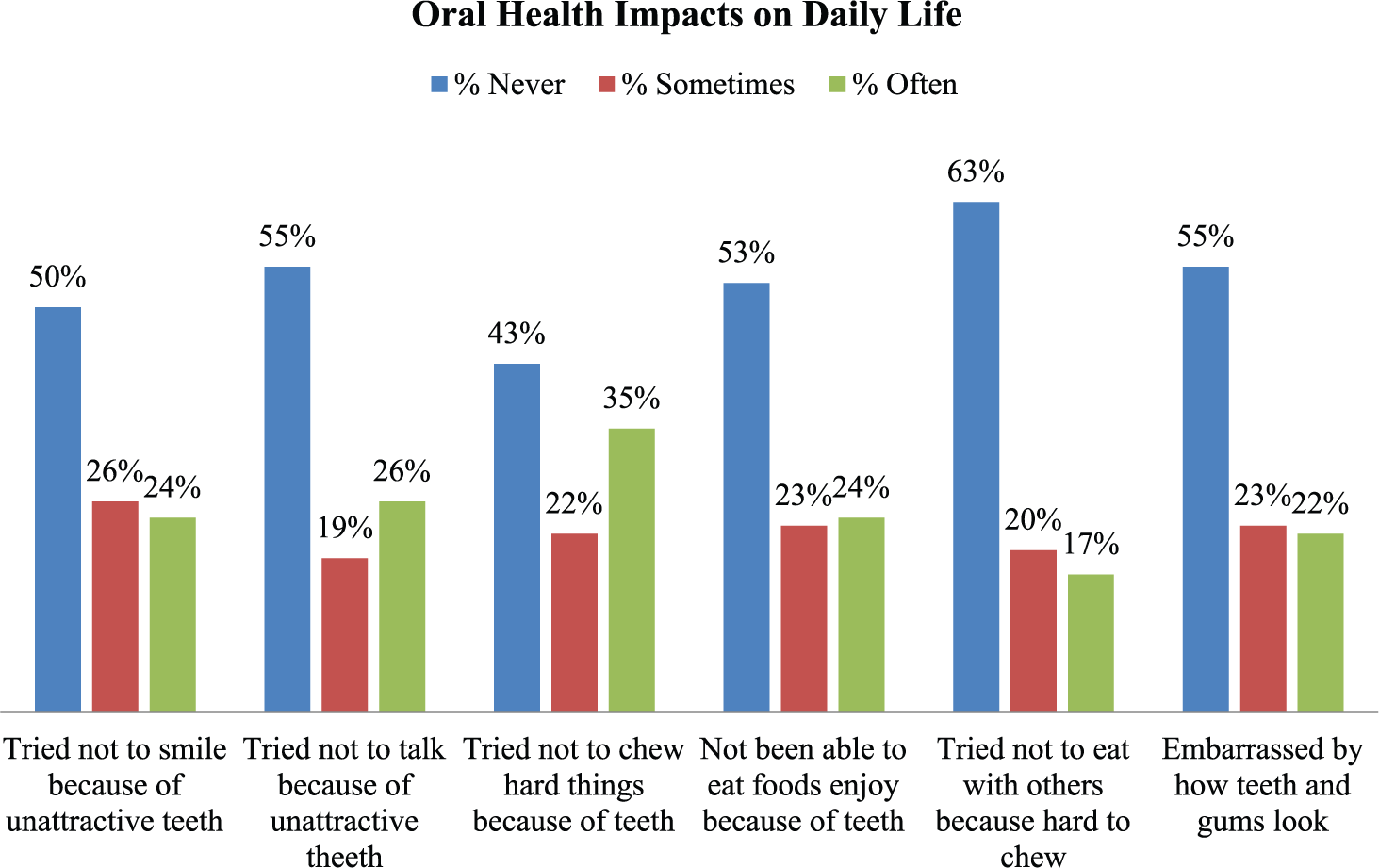
Experiences related to how oral health affects daily life.
Multivariate Results
Logistic regression was performed to assess factors that may be associated with participants’ overall difficulty in finding dental care (age, financial situation, annual family income, dental insurance, current oral health status, and number of dental offices in each NPU; Table 2). The number of dental offices was not statistically significant. Nonetheless, the authors did see a significant trend with suggesting that participants who had difficulty in finding dental care were 3.3 times more likely to live in NPUs with fewer than 10 dental offices. Stepwise selection was applied to reduce and finalize the model. In the final model, those respondents who had difficulty in finding dental care were 4.81 (odds ratio [OR] = 4.81, 95% confidence interval [CI; 1.80, 12.85]) times more likely to report the absence of dental insurance, and 2.73 (OR = 2.73, 95% CI [1.12, 6.70]) times more likely to report poor oral health status.
Logistic Regression Analyses Predicting Difficulty in Finding Dental Care.

Note. OR = odds ratio; CI = confidence interval; NPU = Neighborhood Planning Units.
Discussion
This study examined the oral health attitudes, perceptions, and barriers to oral health care seeking among Black men living in urban low-income communities. Despite the prioritized population experiencing economic challenges, the majority of respondents (68.2%) reported their financial situation as satisfactory. When describing their barriers to oral health care seeking and finding a dentist, these results were more specifically contextualized. Study findings revealed that the absence of dental insurance and poor self-reported current oral health status were independent and statistically significant determinants of perceived difficulty in dental care in the final model. These results are aligned with previous research, which indicated that no dental insurance and poor self-rated oral health were associated with having a cost-prohibitive dental care need (Muirhead, Quiñonez, Figueiredo, & Locker, 2009; Ramraj & Quiñonez, 2013).
Although the top barriers to dental care and finding a dentist were absence of dental insurance and the cost of dental care, other causes were lack of information (i.e., I don’t know where to go) or other barriers related to access (i.e., distance not suitable, no transportation). Zabos et al. (2008) identified similar barriers in their investigation, including lack of coverage, insufficient coverage, inability to find a dentist who accepts their dental insurance, the wait time for coverage to become active, and perceived poor quality of care for uninsured or underinsured people.
Dental care attitudes demonstrated that most men valued oral health. Most felt that dental health was important, that pulling teeth is not better than maintaining their own, and that oral health is connected to their health at large. The largest proportion of respondents indicated that their past dental care was worth the investment. These results are consistent with those of others, indicating that individuals want to pay something for services rendered, deeming it of higher quality. Even a minimal fee required for service may improve perceptions of care, rather than if services are no-cost (Sommers, Goold, McGlynn, Pearson, & Danis, 2013). This may be an important strategy to consider for populations similar to MOHDAP respondents to encourage increased oral health care seeking. These individuals represent those that have low annual incomes but include a fair proportion who feel they have enough to manage financially and may be willing to pay for services, even if uninsured.
Study findings shed some light on the psychological and social costs associated with poor oral health for participants. Not being able to chew or enjoy certain foods with others because of oral discomfort made an impact on the daily life. Some men expressed that because they felt their teeth or gums were unattractive, they were reluctant to talk or smile and embarrassed in social situations. These findings are supported by earlier investigations that have reported that poor oral health can affect one’s speech, which also restricts social interactions, lowers one’s self-esteem, and detracts from physical appearance (Eli, Bar-Tal, & Kostovetzki, 2001; Zhang, McGrath, & Hägg, 2006). Black men, particularly those who are of low SES already face discrimination and have negative stereotypes that may be exacerbated based on their appearance including their smile and teeth.
Findings from this study indicate the critical need for more dental offices in communities, particularly those who are underserved. Findings suggest that the presence of neighborhood resources, such as dental offices, facilitates dental care. Participants who had difficulty in finding dental care were 2.4 times more likely to live in NPUs with fewer than 10 dental offices. This finding is aligned with previous investigations reporting that neighborhood health and social resources are protective (Finlayson et al., 2010; Turrell et al., 2007). Recently, researchers applied a multilevel approach to assess the relationship between neighborhood characteristics and dental caries severity among low-income Black. The study reported that the severity of caries decreased with a higher number of churches, while it increased with a higher number of grocery stores (Tellez, Sohn, Burt, & Ismail, 2006). While not statistically significant, these results indicate the influence of factors, beyond the individual, that may be central to oral health intervention approaches.
With the well-recognized unique influences of social determinants of health, subsequent studies investigating a broader array of local factors would inform a more comprehensive approach to not only intervention development but also policy changes to improve access and proximity to oral health services in particular and preventive health services in general (Centers for Disease Control and Prevention, 2011; World Health Organization, 2013). Public health practitioners, clinicians, and researchers generally agree that social, physical, and environmental factors are central to understanding and addressing increased mortality and morbidity risk across the life span. These factors represent neighborhood contexts or conditions in which people are born, grow, live, work, and age and serve as barriers or facilitators to optimal health (World Health Organization, 2013).
Potential Intervention Strategies and Approaches
CBPR should ideally be directed toward individual, social, and infrastructural factors that work together to mitigate or bridge the oral health disparities gap. At the individual level, Black men engaged in MOHDAP could serve as ambassadors in shaping the intervention. Additionally, these men could increase awareness regarding the benefits of oral health and preventive dental screenings through local media outlets and audiences including NPU meetings and community events frequented by local elected officials. The social implications of the ambassadors’ roles not only may serve to empower a cadre of men who have historically been disengaged in efforts to promote health but also will create positive changes toward enlisting other men to take a proactive approach toward healthier lifestyles. Infrastructural supports toward increased access to and availability of dental services, with institutional incentives for local dentists who become program partners, could be strategic systems approaches to this model.
Strengths
Several characteristics of the CBPR approach represented MOHDAP’s strengths that aligned with or extended findings of previous studies. One of the basic principles of CBPR is that academic researchers who want to conduct effective public health initiatives must invest the time and resources in partnerships with community residents, who are gatekeepers to establishing and maintaining community buy-in, ownership, and sustainability (Anderson et al., 2012; Andrews, Newman, Meadows, Cox, & Bunting, 2012). The nearly decade-long CBPR relationship between MSM PRC and PCIA enabled an ease in identification of existing and new local community residents to lead in assessment activities. Furthermore, the CCB governance infrastructure provided a framework that maintained a community leadership majority and prioritized lay knowledge critical to understanding and developing a culturally relevant MOHDAP measurement tool (Minkler, 2005). Additionally, MOHDAP community research capacity building, through training residents to critically review, develop, and lead in survey administration, has been previously linked to increases in research confidence and the generation of community-owned health interventions that are more effective in improving health (Viswanathan et al., 2004; Wallerstein & Duran, 2010). Related MOHDAP outcomes were increased community engagement as well as transferrable skills toward the conduct of subsequent assessments of health priorities. Finally, while CBPR ideally positions community residents as equal or senior partners (Blumenthal, 2006), this power sharing often does include a balanced share of grant funds. At its foundation, MOHDAP reversed the traditional model of an academic institution being the fiscal lead. PCIA, held the preponderance of fiscal power, with support from the MSM PRC, an academic subcontractor.
Limitations
Findings must be interpreted in light of acknowledged limitations. A small, convenience sample of program participants were recruited at local sites in Atlanta; therefore, the results are not generalizable. Participants in the study may have been more likely to be unemployed and have free time versus people who could not participate because they were at work. Another limitation was that the participants did not have an objective clinical dental exam; their current dental health status was self-reported. Specific dental services that were difficult to find, such as dental sealing, cleaning, fillings, root canal, extraction, and dentures, were not examined, which also serves as a limitation. Last, the authors were not able to investigate the independent contribution of neighborhood disadvantage and individual characteristics in details.
While the previously established CBPR relationship between MSM PRC and PCIA facilitated a strong community engagement process, there were differing organizational cultures that were limitations. First, while PCIA, partnering CBOs and community residents were poised for immediate action on notification of grant award, MSM PRC had inherent delays related to IRB reviews and revisions that had to be addressed prior to their engagement. This would have been overcome through anticipating and planning for the additional time necessary for academic institutional clearances associated with community-led and academic partner–supported research. The importance of ethics education and IRB understanding, beyond communities knowing what they “sign up” for when participating in clinical trials, has been heightened as federally funded research programs prioritize community-engaged research, where communities not only advise or participate but also may lead or colead research (Anderson et al., 2012). Second, academic administrative delays associated with MSM PRC subcontract processing prior to the hire of mission-critical staff created delays and challenging relationships due to communities that were eager to initiate work and collaboration. Finally, despite a written protocol for survey data collection, there were surveys with missing responses that have been detailed earlier. This may have been due to differing cultures associated with relative weight placed on community engagement, in general, versus survey completion, in particular, to increase sample size and statistical strength of variables central to the community assessment. These issues are important to address in subsequent partnerships through detailed protocols for data collection, planning, and implementation, which are limitations cited elsewhere (Mohammed, Walters, LaMarr, Evans-Campbell, & Fryberg, 2012).
Conclusions
Results of the current study demonstrate the significance of insurance coverage, dental care costs, access, and awareness among determinants of dental care for Black men. The authors observed that poor self-reported oral health status was an independent and statistically significant determinant of perceived difficulty in finding dental care. Neighborhood characteristics, including the proportion of dental providers, had a significant impact on oral health care seeking and finding a dentist, demonstrating the significance of a multilevel intervention. The results of the study could be helpful for policy makers and citizen advisory councils in creating the political will toward the development of multilevel interventions that address the individual, contextual and social determinants of oral health that meet the needs of their communities among Black men. PCIA and MSM PRC have worked conjointly to complete the MOHDAP pilot phase and will continue to partner using a CBPR approach that builds on the strengths and challenges identified toward effectively engaging Black males. The unique social experiences of Black men as among the most disadvantaged racial/ethnic/gender groups warrant targeted attention, with implications for advancing health equity.
Footnotes
Acknowledgements
The authors would like to thank Donoria Evans, MPH, Brittany Newton, MPH, Monique Eppinger, MPH, and Daniel Blumenthal, MD, MPH, for their critical review of this article or support in project planning and implementation.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project was supported through funding from the DentaQuest Foundation, the Centers for Disease Control and Prevention (CDC) Health Promotion and Disease Prevention Research Center (Grant No. 1U58DP005945-01), and the National Institute on Minority Health and Health Disparities (NIMHD; Grant No. S21MD000101). The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIMHD or the CDC.
