Abstract
Mental ill-health has increased among Iranian men in the recent years. Mental health is complexly determined by sociocultural, psychological, demographic characteristics, and some health-risk behaviors such as smoking. This study aimed to explore the association(s) between demographic factors, smoking status, social capital, and poor mental health status in a sample of Iranian men. The data were derived from a survey titled “Urban Health Equity Assessment and Response Tool–2” in Tehran, Iran (n = 11,064). A multistage sampling method was applied in the study. The General Health Questionnaire–28 was used to assess poor mental health status (range = 0-84, scores higher than 23 indicated poor mental health status). The data were analyzed using t test, chi-square test, and multivariate logistic regression. The means of age and family size were 47.14 ± 17.26 years (range = 20-91) and 3.54 ± 1.32 individuals (range = 1-15), respectively. The majority of the participants were employed (57%, n = 6,361). The prevalence of poor mental health was 36.36%, 95% confidence interval (CI) [35.46, 37.26]. The components of social capital were positively associated with poor mental health status. Family size (adjusted odds ratio [AOR] = 0.93; 95% CI [0.90, 0.96]), job status (unemployed vs. employed, AOR = 1.34; 95% CI [1.16, 1.55]), marital status (widowed and divorced vs. single, AOR = 1.09; 95% CI [1.02, 1.17]), education level (illiterate vs. academic, AOR = 1.18; 95% CI [1.09, 1.29]), and smoking status (smokers vs. nonsmokers, AOR = 1.46; 95% CI [1.31, 1.62]) were directly associated with poor mental health status in the logistic regression model. These results suggest that social capital could be an important approach for men to attain suitable mental health and reduce mental disorders. The high prevalence of poor mental health in men merits more attention in mental health policy and program planning.
Introduction
Mental health is defined as “a state of well-being in which every individual realizes his or her own potential, can cope with the normal pressures of life, is able to work effectively, and can make a contribution to community” by the World Health Organization (2014; Seyfhashemi, Yarian, Bahadoran, Jandaghi, & Mirmohammadkhani, 2015). Recently, the importance of mental health has received growing attention due to the increase in economic and mental stress around the world (Chen, Chen, & Landry, 2015). One of the important instruments for assessing metal health is the 28-item General Health Questionnaire (GHQ-28). In the GHQ-28, scores higher than 23 are considered as poor mental health status (range = 0-84). The dimensions of mental health based on GHQ-28 are somatic symptoms, anxiety and sleep problems, social dysfunction, and depression (Malakouti, Fatollahi, Mirabzadeh, & Zandi, 2007).
Poor mental health status is regarded as a global concern and accounts for a large proportion of the burden of disease in men and women in all communities (Lopez, Mathers, Ezzati, Jamison, & Murray, 2006). The Global Burden of Disease Study (2010) reported that mental disorders accounted for 183.9 million Disability-Adjusted Life Years or 7.4% of total Disability-Adjusted Life Years in the world (Whiteford et al., 2013). In addition, the burden of diseases due to poor mental health significantly increased in men (Lopez et al., 2006). A study in Ghana reported the prevalence of poor mental health was about 15.5% in men (Sipsma et al., 2013). In a nationwide study in Denmark, around 6.4% of men suffered from poor mental health (Christensen, Davidsen, Kjøller, & Juel, 2014).
According to previous studies on Iranian men, poor self-reported mental health was prevalent (Jafari et al., 2010; Noorbala & Akhondzadeh, 2015). The prevalence of poor self-reported mental health has also increased among men over the past decades, reflected by an increase in the incidence of depression and anxiety as dimensions of mental health (Jafari et al., 2010). A study in Iran (1998) reported that the prevalence of poor mental health was 14.90% in men, 95% confidence interval (CI) [12.20, 16.94] (Noorbala & Hafezi, 2012). Another study (2007) indicated that the prevalence of poor mental health increased to about 28.60% (95% CI [22.12, 35.20]) in Iranian men (Noorbala & Hafezi, 2012). Sharifi et al. (2015) in a 12-month diagnoses of psychiatric disorders in the Iranian population, reported that the prevalence of poor mental health in men was 20.89% (95% CI [19.12, 22.26]); accordingly, anxiety and depression were more prevalent compared with somatization and social dysfunction. In another study, the highest prevalence of poor mental health in Iranian men was reported to be 32.65% and 34.74% in Chaharmahal and Golestan provinces, respectively (Noorbala & Akhondzadeh, 2015). The increasing prevalence of poor mental health status in Iranian men might have been related to low socioeconomic status (SES) level, environmental and work-related stresses (economic and occupational stresses), and restricted social participation in the community (Noorbala & Hafezi, 2012).
Poor mental health status is intricately determined by an interaction of sociocultural, psychological, environmental, and biological factors and individual characteristics (Knight, Silverstein, McCallum, & Fox, 2000). Poor mental health status in men is associated with age, marital status, education level, job status, health-related factors, and Health-Related Quality of Life (Alonso et al., 2004; Gili, Roca, Basu, McKee, & Stuckler, 2013).
Social capital has been defined as norms, networks, and social links that facilitate collective actions. Social capital is related to a number of main subjective and public health factors. Social capital can act as a protective variable and promote mental health status and reduce socioeconomic inequalities (Hamano et al., 2010). It can also play a vital role in the prevalence of mental disorders. A previous study indicated that connectedness among people and social supports were associated with better mental health among communities (Nielsen et al., 2015). In addition, several studies have identified a positive relationships between high social capital and better mental health in individual levels (Irwin, LaGory, Ritchey, & Fitzpatrick, 2008; Verduin, Smid, Wind, & Scholte, 2014). However, these relationships have not been reported across researches consistently (Almedom, 2005).
Commonly, individuals with higher SES have better mental health. Education level, income, job status, and other demographic variables were also among the social and economic factors or “social determinants” that were associated with mental health (Williams, Cunich, & Byles, 2013). Little is known about the mechanism of effect of socioeconomic and demographic factors on poor mental health status in men (Baum, Garofalo, & Yali, 1999).
Men are more likely to smoke cigarette than women in all communities, possibly because of their working conditions or emotional status, and are thus more susceptible to smoke-related illnesses (Taylor, Taylor, Munafò, McNeill, & Aveyard, 2015). The prevalence of cigarette smoking also differs in Iranian men and ranges from 6.3% to 38.5% in recent years. A recent meta-analysis study of the Iranian population reports that the cigarette-smoking prevalence was about 19.8% in men (Moosazadeh, Ziaaddini, Mirzazadeh, Ashrafi-Asgarabad, & Haghdoost, 2013).
A large body of evidence has demonstrated that smoking status is related to mental health (Taylor et al., 2014; Taylor et al., 2015). However, it is not clear whether reducing daily cigarette smoking is associated with change in mental health status. Smokers may experience longer times of and more intense symptoms, such as depressed mood, anxiety, and irritability, that can lead to mental disorders (Taylor et al., 2015). Taylor et al. (2014) reported that quitting smoking was related to reduction of anxiety, depression, and stress and improvement of mood, mental health, and quality of life.
Therefore, based on the results of the literature review, the present population-based study aims to explore the association between demographic factors, smoking status, social capital, and poor mental health status in the male population of Tehran, Iran.
Research Design and Method
The study data were extracted from a population-based survey titled “Urban Health Equity Assessment and Response Tool–2” (Urban HEART-2), which was conducted among 22 districts of Tehran, the capital of Iran, in 2011. Using a multistage sampling method, the authors first applied stratified sampling and considered each of the 22 districts as a strata, after which 200 blocks were selected randomly from each district through the cluster sampling method. The subsequent sampling strategy included random selection of eight households from each block. After that, a man within four age groups (20-24, 25-45, 46-65, and older than 65 years) was selected from each household. Finally, 11,064 men in 22 districts participated in the study.
The inclusion criteria for selecting samples were men aged 20 years and older, residing in the selected living districts, and consent to answer questionnaires. The study was conducted by more than 200 trained surveyors within a rigorous monitoring and quality assurance system encompassing field observations.
Data Collection Tools
The study data were collected using a social capital questionnaire and a mental health questionnaire (GHQ-28). Validity and reliability of GHQ-28 (Malakouti et al., 2007) and the social capital questionnaire (Kassani, Gohari, & Asadilari, 2012) have been confirmed in previous studies in Iranian populations. GHQ-28 is an instrument used for screening of mental health disorders and has four dimensions, including somatic symptoms, anxiety and sleep problems, social dysfunction, and depression. The scores of each dimension could range from 0 to 21, with the scores above 6 indicating higher degrees of the related disorders. The scores of mental health (GHQ-28) ranged from 0 to 84, scores higher than 23 were regarded as poor mental health status in this study (Malakouti et al., 2007).
The social capital questionnaire administered in this survey consisted of nine questions in various levels of close family, relatives, friends, neighbors, colleagues, same ethnicity and religion, and general public. The first four items of the questionnaire were designed to measure voluntary participation, collective activity, trust, and social cohesion using a 5-point Likert-type scale. Another item involved the subitems of truthfulness and avoidance of lying, trusteeship, amnesty, fairness and justice, honesty and reliability, and courage to tell the truth. Four other items were also about social support, participation in association activities (parents–teachers collaboration, religious groups, athletic groups, charities, professional groups, political parties, ethnic groups, and scientific groups), social status (in terms of cultural, social, economic, and other factors), and social networks (the relation with groups of family members, relatives, friends, neighbors, and colleagues). According to factor analysis of this questionnaire in the Iranian population, three components of social capital were individual trust, cohesion/social support, and social trust/associative relations. These three components explained 66.14% of total variance of the social capital tool. Cornbrash’s alpha coefficients were .91, .70, and .77 for individual trust, cohesion/social support and social trust/associative relations, respectively (Kassani et al., 2012).
Cigarette-smoking status was determined via the following question: “How often do you smoke cigarettes at present?” (1: every day; 2: at least 5 times a week, but not every day; 3: never). The men who smoked at least 5 times a week one cigarette or more were considered to be cigarette smokers, and the remainder of the men was considered to be nonsmokers.
The scores of mental health as the dependent variable were categorized into two groups; GHQ scores <23 and >23 were considered to be without (0) and with (1) poor mental health, respectively. It should be mentioned that the participants’ age, family size, nationality, house ownership, job status, education level, marital status, smoking status, and social capital were regarded as independent variables.
Ethics Statement
The study protocol was approved by the ethics committee of Shiraz University of Medical Sciences. Written informed consents were obtained from all the participants and they were reassured about the confidentiality of their information.
Data Analyses
Using Stata SE-11 software, data analysis was conducted through descriptive statistics, t test, and chi-square test. The variables with a p < .20 in univariate analyses among potential confounder variables listed in Tables 1 and 2 were entered to the multivariate logistic model. The multivariate logistic regression was performed by Enter method. An odds ratio (OR) with 95% CI was applied for comparison, and p < .05 was considered to be statistically significant.
Demographic Characteristics and Poor Mental Health Status Among the Men in Tehran.

Note. Ref. = reference group; OR = odds ratio; CI = confidence interval.
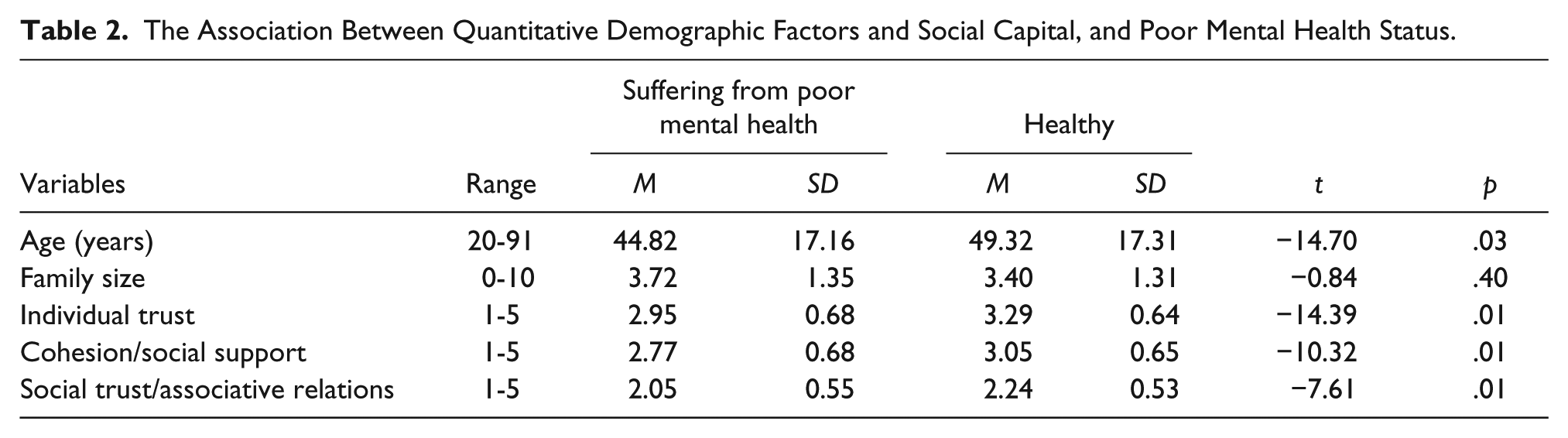
The Association Between Quantitative Demographic Factors and Social Capital, and Poor Mental Health Status.
Results
In a total of 11,064 men, the means of age and family size were 47.14 ± 17.26 years (range = 20-91) and 3.54 ± 1.32 individuals (range = 1-15), respectively. Approximately 5.5% (n = 619) had no education and 9.3% (n = 1,030) had primary education. Considering the 22 districts of Tehran, the majority of the men were living in District 5 (N = 782; 7.08%) and the fewest number of them were living in District 10 (N = 359; 3.25%). Around 16.31% (n = 1,805) of the men were smokers.
The mean score of men’s mental health was 21.98 ± 10.85 (range = 0-84). The mean scores of dimensions of mental health, including somatic symptoms, anxiety and sleep problems, social dysfunction, and depression, were 5.68 ± 3.64, 5.96 ± 4.73, 7.97 ± 3.78, and 2.38 ± 3.82, respectively (range = 0-21). In total, 4,023 men (36.36%, 95% CI [35.46, 37.26]) had a degree of poor mental health (GHQ-28 scores >23).
The mean scores of social capital components, including individual trust, cohesion/social support, and social trust/associative relations, were 3.17 ± 0.66, 2.91 ± 0.67, and 2.15 ± 0.54, respectively (range = 1-5). Accordingly, 5.08% (n = 562), 9.49% (n = 1,050), and 42.71% (n = 4,725) of the men were experiencing low individual trust, cohesion/social support, and social trust/associative relationships, respectively. Other demographic characteristics of the study participants and the association between the demographic characteristics and poor mental health in the men are reported in Table 1.
As indicated in Table 1, age, house ownership, smoking status, and marital, education, and job status were significantly associated with mental health (p < .05). However, no significant association was identified between nationality and poor mental health status in the men (p = .38). The characteristics of the quantitative variables, components of social capital, and their associations with poor mental health have been presented in Table 2.
The mean age of the men with poor mental health (44.82 years) was lower than that of the men without mental health disorders (49.32 years). The study results revealed no significant association between family size and poor mental health status (p = .18). However, the three components of social capital had significant relationships with poor mental health status; their means were higher in the healthy men compared with those with poor mental health status (p = .01).
In multivariate analysis, the significant variables and those close to statistical significance (p < .20) were entered into logistic regression analysis to assess the possible confounding variables. The results are reported in Table 3.
Multivariate Analysis of the Association Between Demographic Factors, Smoking Status, and Social Capital Components and Poor Mental Health Status.

Note. SE = standard error; AOR = adjusted odds ratio; CI = confidence interval. The second category is the reference group in the independent variables.
Unstandardized coefficient.
Based on the findings of the logistic regression model, the individual trust (adjusted odds ratio [AOR] = 0.66, 95% CI [0.51, 0.80]), cohesion/social support (AOR = 0.90, 95% CI [0.81, 0.99]), and social trust/associative relations (AOR = 0.88, 95% CI [0.82, 0.94]) were positively associated with poor mental health status in the men. In addition, family size (AOR = 0.93, 95% CI [0.90, 0.96]), smoking status (AOR = 1.46, 95% CI [1.31, 1.62]), unemployed versus employed (AOR = 1.34; 95% CI [1.16, 1.55]), retired versus employed (AOR = 1.25; 95% CI [1.05, 1.49]), widowed and divorced versus single (AOR = 1.09; 95% CI [1.02, 1.17]), illiterate versus academic (AOR = 1.18; 95% CI [1.09, 1.29]), primary school versus academic (AOR = 1.21; 95% CI [1.01, 1.10]), middle school versus academic (AOR = 1.23; 95% CI [1.02, 1.48]), and high school/diploma versus academic (AOR = 1.55; 95% CI [1.25, 1.88]) had a direct association with poor mental health status. Age (AOR = 1.01, 95% CI [0.99, 1.02]) and house ownership (AOR = 0.97, 95% CI [0.91, 1.06]) indicated no relationships with poor mental health in the logistic regression model.
Discussion
Mental health care in Iran as an undeveloped country is completely deficit-based. There is little known about poor mental health status, especially in men, and associated factors in the Iranian population. Given the SES, sociocultural condition, environmental and work-related stresses (economic and occupational stresses), and restricted social participation in Iranian men (Noorbala & Hafezi, 2012), the present study aimed to explore the association between demographic factors, smoking status, social capital, and poor mental health status in a sample of Iranian men.
According to the study findings, a total of 4,023 men (36.36%, 95% CI [35.46, 37.26]) had a degree of poor mental health (GHQ-28 score >23). In a national study on psychiatric disorders performed using the schizophrenia and affective disorder scale in Iran in 2001, the prevalence of psychiatric disorders was 17.1% in men (Yasamy et al., 2001). In another study on Iranian men (2007), the prevalence of poor mental health was around 29% (Noorbala & Hafezi, 2012). This discrepancy among the findings can be attributed to social, political, economic, and cultural problems in the Iranian population in the recent decade (Yasamy et al., 2001). It is important to note that comparisons of prevalence rates highly depend on sampling methods, instruments, and definitions of psychiatric disorders in different studies (Sharifi et al., 2015).
Based on the results of the univariate analysis in Table 1, age, education level, nationality, job status, and marital status were significantly related to poor mental health status in the men (p < .05). Accordingly, the men with lower education levels had a higher odds of poor mental health status (OR = 1.50, 95% CI [1.26, 1.80]), which was consistent with the previous studies (Alonso et al., 2004). This association can be due to the higher prevalence of social, economic, and cultural limitations among men with lower education levels and their inability to apply more affective coping strategies to stressful situations in life (Noorbala & Hafezi, 2012). The results also indicate that the younger men had a better score of mental health. In the study conducted by Noorbala, aging was related to increased prevalence of mental disorders; the highest rate of mental disorders was reported among individuals older than 65 years. Retirement, loneliness, and biological factors can contribute to the increasing prevalence of poor mental health in older age groups (Noorbala & Hafezi, 2012).
As reported in Table 2, the results indicated a significant association between social capital components and poor mental health status (p < .05). This accords with previous research, which demonstrated that promotion of mental health could be facilitated by increasing social support and social capital within communities (Jones, Heim, Hunter, & Ellaway, 2014). A study in Japan (2010) indicated that cognitive social capital, measured by individual and social trust, and structural social capital, measured by associative relations and membership groups, were associated with better mental health status after adjusting for demographic factors (Hamano et al., 2010). This was also in line with the findings of the present study. Similarly, studies performed in the Netherlands as a high-income country (Drukker, Gunther, Feron, & Van Os, 2003) and Chile as a low- and middle-income country (Riumallo-Herl, Kawachi, & Avendano, 2014) reported that social capital had a strong positive relationship with poor mental health status.
In the multivariate analysis, the three components of social capital were related to poor mental health status in the men (p < .05). In addition, family size, smoking status, job status, marital status, and education level had a direct relationship with poor mental health status in the men (p < .05). However, age indicated no association with the men’s mental health in the logistic regression model (OR = 1.01, 95% CI [0.99, 1.02]).
The possible causal association between social capital components and poor mental health is more supported by a twin fixed-effect study that was consistent with the results of logistic regression in the present study. At least two possible reasons may account for the association between social capital and poor mental health in men. First, men who suffer from mental disorders, such as depressive symptoms, may be more likely to have low individual and social trust in their neighborhood and have lower levels of social support and social capital. Second, lower social capital can directly deteriorate mental health by affecting men’s ability to satisfy others, increase loneliness, and cause poorer expectations from the future (Riumallo-Herl et al., 2014).
As indicated in Table 3, the men with poor mental health status were more likely to be smokers compared with those with better mental health (OR = 1.46, 95% CI [1.31, 1.62]), which is consistent with the study conducted by Marc and colleagues in New Jersey (Steinberg, Williams, & Li, 2015). However, another study demonstrated no significant association between reduction of smoking and poor mental health status. It should be noted that the aforementioned study had a small sample size and might, therefore, have had insufficient power to detect the association between smoking status and mental health (Taylor et al., 2015). The results of the multivariate analysis revealed a significant association between marital status and poor mental health status. One possible explanation is that the great majority of single men in Iran live with their parents until getting married and, therefore, may not experience the stressors of independent living. On the other hand, married men, especially divorced ones, are exposed to a number of social and economic stressors commonly associated with poor mental health (Sharifi et al., 2015).
Limitations
An important limitation of the present study was its cross-sectional design through which both exploratory variables and men’s mental health were measured simultaneously. Therefore, temporality was not regarded in determination of the associations. Also, this study was performed using GHQ-28, which is not a structured clinical interview, and was thus unable to determine the real prevalence of poor mental health in the men. The strong points of this study were its population-based design and application of logistic regression model for determining the associations between independent variables and poor mental health.
Conclusion
The results indicated that the prevalence of poor mental health status has increased in Iranian men. Given the high prevalence of psychiatric disorders in men, policy makers should pay greater attention to mental health programs. The results also indicated that family size, smoking status, job status, marital status, education level, and social capital were significantly associated with poor mental health status. The results suggested that changes in social capital could lead to positive effects on mental health status. Paying attention to promotion of education status and provision of recreational facilities for increasing socioeconomic factors and social capital can also have a positive effect on mental health in men. Overall, this population-based study can provide an excellent basis to compare poor mental health between different groups in future studies with limited sample sizes. However, due to the cross-sectional design of the present study, transposition of the relationships between the variables was not exactly specified. Hence, longitudinal studies using clinical measures are recommended to further clarify the relationship between poor mental health status and their associated factors in men.
Footnotes
Acknowledgements
The authors would like to thank Ms. A. Keivanshekouh at the Research Improvement Center of Shiraz University of Medical Sciences for improving the use of English in the article.
Authors’ Note
This article was extracted from the corresponding author’s PhD dissertation titled “The Association Among Some of Social Determinants of Health: In Urban HEART Survey–2” approved by the research vice-chancellor of Shiraz University of Medical Sciences (Proposal No. 94-7470).
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
