Abstract
High rates of respiratory symptoms (14%) and new-onset asthma in previously healthy soldiers (6.6%) have been reported among military personnel post-deployment to Iraq and Afghanistan. The term Iraq/Afghanistan War-Lung Injury (IAW-LI) is used to describe the constellation of respiratory diseases related to hazards of war, such as exposure to burning trash in burn pits, improvised explosive devices, and sandstorms. Burnpits360.org is a nonprofit civilian website which voluntarily tracks medical symptoms among soldiers post-deployment to the Middle East. Subsequent to initiation of the Burnpits360.org website, the Department of Veterans Affairs started the Airborne Hazards and Open Burn Pit registry. This paper: (a) analyzes the latest 38 patients in the Burnpits360.org registry, validated by DD214 Forms; (b) compares strengths and weaknesses of both registries as outlined at the National Academy of Sciences Institute of Medicine Burn Pits Workshop; (c) further characterizes the spectrum of disease in IAW-LI; (d) describes the risk factors of affected populations; (e) summarizes current practices regarding management of the condition; and (f) defines future research objectives.
Keywords
Adverse environmental exposures in the Middle East region include: 1) burning trash in open air “burn pits” ignited with JP-8 jet fuel; 2) improvised explosive devices (IEDs) with associated “blast overpressure” or shock waves (with the capacity to aerosolize metals); 3) aeroallergens; and 4) massive sandstorms consisting of sharp, respirable, metal-laden, geoparticulate matter (Szema, 2013; Szema et al., 2014).
In 2010, families of affected military personnel started Burnpits360.org, a nonprofit website that functions as a database to voluntarily collect self-reported information on soldiers affected by burn pit exposure. These families raised significant awareness to the issue of open-air burn pits, resulting in the passage of the Open Burn Pits Registry Act by President Obama in 2013 (http://sgtsullivancenter.org/wp-content/uploads/2015/04/IOM-Registry-Final-Letter.pdf).
Subsequently, the Department of Veterans Affairs (VA) established the Airborne Hazards and Open Burn Pit (AH&OBP) registry to monitor health effects due to airborne hazard exposure during deployment. This registry collected data from veterans and active duty service members using a voluntary self-assessment questionnaire from April 25, 2014 to September 30, 2014. Data were acquired from 32,306 participants with 19,082 total completed questionnaires. The first report was released in April 2015 (U.S. Department of Veteran Affairs, 2015).
Multiple authors have noted higher rates of respiratory illness among previously healthy, fit-for-duty, deployable U.S. military personnel during and after deployment to the Middle East (Abraham, DeBakey, Reid, Zhou, & Baird, 2012; Falvo, Osinubi, Sotolongo, & Helmer, 2015; Roop, Niven, Calvin, Bader, & Zacher, 2007; Smith, Wong, Smith, Boyko, & Gackstetter, 2009; Szema, Peters, Weissinger, Gagliano, & Chen, 2010; Szema, Salihi, Savary, & Chen, 2011). During deployment, 13% of U.S. Army Medic visits in Iraq were for new-onset acute respiratory illness (personal communication Michael Kilpartrick, MD, Pentagon). Both asthmatic and nonasthmatic Department of Defense personnel report increased respiratory symptoms of wheezing, cough, sputum production, chest pain/tightness, and allergy symptoms (Roop et al., 2007; Szema et al., 2010). Among patients at the Veterans Affairs Medical Center, Northport, New York, deployment to Iraq and Afghanistan was associated with: (a) higher risk of asthma and (b) higher rates of new-onset respiratory symptoms leading to more frequent ordering of spirometry versus those deployed to other locations, 14.5% versus 1.8% (Szema et al., 2010; Szema et al., 2011). Cumulative length and frequency of deployment are not associated with increased incidence of respiratory disease among U.S. military personnel, suggesting that Middle East respiratory hazards encountered during a single deployment are severe enough to induce acute and chronic lung injury (Abraham et al., 2012).
Among common respiratory hazards are: (a) open-air Burn Pits used to burn trash with JP-8 jet fuel in the absence of incinerators; (b) improvised explosive devices (IEDs), often detonating vehicles roadside; (c) blast overpressure or shock waves causing shear stress on lung tissue; (d) seasonal aeroallergens, as well as indoor dust mite antigens and mold; and (e) naturally-occurring sandstorms (so-called Shamal and Sharq, named for the direction of motion).
Burn pits are open-air fields of burning trash ignited by JP-8 jet fuel, utilized for the disposal of water bottles, Styrofoam trays, medical waste, unexploded munitions, and computers (Szema, 2013). Incineration of these products, and use of JP-8 jet fuel containing benzene, releases dangerous toxins, as well as products of incomplete combustion, which accumulate as measurable particulate matter air pollution (Engelbrecht et al., 2009; Szema, 2013). Open air burn pit exposure is analogous to airborne hazard exposures at the World Trade Center disaster post September 11, 2001, in New York City (Prezant et al., 2002). Firefighters and rescue workers were exposed to burning buildings ignited with jet fuel, JP-8, from two airplanes which deliberately crashed into the twin towers. Post 9/11, at 5 years, firefighters and rescue personnel with more than 1,000 hours in the aftermath at Ground Zero had airway hyperresponsiveness on methacholine challenge, as well as accelerated decline in lung function of approximately 500 ml (Banauch et al., 2006). World Trade Center Cough describes a symptom constellation believed to be related to inhalation of dust in lungs, which also was swallowed or nasally inhaled in the midst of massive clouds of airborne particulate matter (Prezant et al., 2002). Children living and attending school in Manhattan’s Chinatown proximal to Ground Zero—and enrolled in an asthma registry in the 12 months preceding September 11, 2001—had reduction in peak expiratory flow rates, compared with those living further away (over 5 miles). These asthmatic children closer to Ground Zero also had more visits to the pediatrician for asthma specifically, and their pediatricians prescribed more asthma medications compared with those living further away (Szema et al., 2004).
The wars in Iraq and Afghanistan (Operation Iraqi Freedom, Operation Enduring Freedom, Operation New Dawn) have seen the prominent use of roadside bombs or IEDs. These are typically detonated with the intent to explode vehicles. For phosphate bombs, this may lead to vaporization of a Humvee within minutes. Some soldiers have been found to have metal in their lungs, with iron bound to titanium in fixed mathematical ratios, supporting the concept that the source is anthropogenic (Szema et al., 2012; Szema, 2013). Specialized techniques and expertise with sophisticated equipment are necessary to determine the spatial resolution of metals in lung; this is often not available, except at quaternary care medical centers associated with national laboratories. Polarizable crystals seen in soldiers’ lungs with constrictive bronchiolitis (King et al., 2011) have been shown to be these metals when particulate matter models are used to duplicate lung injury in mice.
Explosive devices accounted for 36.3% of battle injuries in Operation Iraqi Freedom and Operation Enduring Freedom (Murray et al., 2011). Mortars, roadside IEDs, vehicle IEDs, suicide bombers utilizing C4—all of these culprits cause blast overpressure or shock waves leading to shear stress on delicate lung alveoli. Reported complications related to explosive damage include primary blast lung injury and adult respiratory distress syndrome (Johnston et al., 2013; Mackenzie & Tunnicliffe, 2011; Singleton, Gibb, Bull, Mahoney, & Clasper, 2013; Szema, 2013).
Aeroallergens such as Prosopis and Chenopodia are common in both North America and the Middle East (Mbuthia, Szema, & Li, 2015). Soldiers with sensitivity to weed pollens may experience allergic symptoms during deployment. In certain individuals, chronic dose-dependent exposure to aeroallergens provokes development of allergic diseases depending on the individual’s genotype (Custovic, 2015). Postnasal drip syndrome due to allergic rhinitis may lead to other respiratory diseases like chronic cough and asthma (Mbuthia, Szema, & Li, 2015; Sandhu & Kuchai, 2013). Furthermore, dust mite antigen sensitive asthma is frequent in the Middle East (Farrokhi et al., 2015; Gheybi et al., 2014; Thalib & Al-Taiar, 2012, Hassan, Tayeb, Amir, Wali, & Mohamed, 2013). Cladosporium, Penicillium, Alternaria, and Aspergillus have been detected in Iraq air samples (Muhsin & Adlan, 2012). Aspergillus mold, a putative cause of a severe form of asthma called Allergic Bronchopulmonary Aspergillosis, is also the most common indoor mold in Iraq (Yehia, al-Habib, & Shehab, 1990). Along the banks of the Tigris and Euphrates rivers, the land of ancient Mesopotamia, date palm trees have been cultivated for 5,000 years, so this is the prevalent spring pollen in southern Iraq (Al-Tikriti, Al-Salihi, & Gaillard, 1980).
Sandstorms are so frequent in Iraq that the Arabic language has terms Shamal and Sharq for names of sandstorms based on their direction (northerly and easterly, respectively; 2014; El-Baz & Makharita, 1994; Chergui). In Iraq, a 5-year study recorded 569 days with dust storm events where PM10 >200 µg/m3, and 39 days with very severe dust storms PM10 >1000 µg/m3 (Al-Dabbas, Ayad Abbas, & Al-Khafaji, 2012). The U.S. Environmental Protection Agency (2014) PM10 standards allows exposure to 150 µg/m3 within a 24-hour period which is not to be exceeded three times a year. Sandstorms significantly increase exposure to aeroallergens among people in the Middle East. Quantities of airborne bacteria and fungi are, respectively, 100% and 40% higher during a sandstorm (Kwaasi et al., 1998). In collaboration with Richard Reeder and colleagues in the Geosciences Department at Stony Brook University, particle size of grab samples from surface soil have been characterized to (a) contain respirable particles 2.5 microns in size, (b) be sharp and angular in shape, (c) upregulate proinflammatory cytokine IL-2, and (d) promotes fibrosis (Szema et al., 2014). Additionally, Andrea Harrington from New York University has reported at the American Geological Society that dust from Iraq and Afghanistan upregulated hydrogen peroxide in vitro after 24 hours (Harrington, Szema, Tsirka, & Schoonen, 2011a, 2011b, 2012).
Research Aims/Goals
The purpose of this paper is to: (a) analyze the latest 38 patients in the Burnpits360.org registry, validated by DD214 Forms; (b) compare strengths and weaknesses of both VA and Burnpits360.org registries as outlined at the National Academy of Sciences Institute of Medicine Burn Pits Workshop, by highlighting cohort characteristics of each, as well as key survey questions with flaws or omissions; (c) further characterize the spectrum of disease in IAW-LI; (d) describe the risk factors of affected populations; (e) summarize current practices regarding management of the condition; and (f) define future research objectives.
Methods
We received anonymously-coded de-identified data from Burnpits360.org, which was IRB-exempt. Data reported by the VA in their first AH&OBP registry report was compared with data reported by Burnpits360.org. (Data was submitted by the latest 38 veterans to the Burnpits360.org registry who have confirmed status based on the DD214 Form, certificate of release or discharge from active duty, N = 38). The proposed clinical management recommendations for IAW-LI are based on work published by the Denver Working Group on post-deployment health, case reports, scientific literature on recommended procedures, and invited recommendations at the May 1, 2015, National Academy of Sciences’ Institute of Medicine Workshop on burn pits (Rose et al., 2012; King et al., 2011; Morton & Dowling, 1987; Szema, 2013; Szema et al., 2014).
Results
Data from the VA AH&OBP registry and the Burnpits360.org registry are missing information necessary for proper identification of IAW-LI. Both registries were lacking important questions in their voluntary questionnaires (Table 1).
Missing Questions Within AH&OBP Registry and Burnpits360.org.
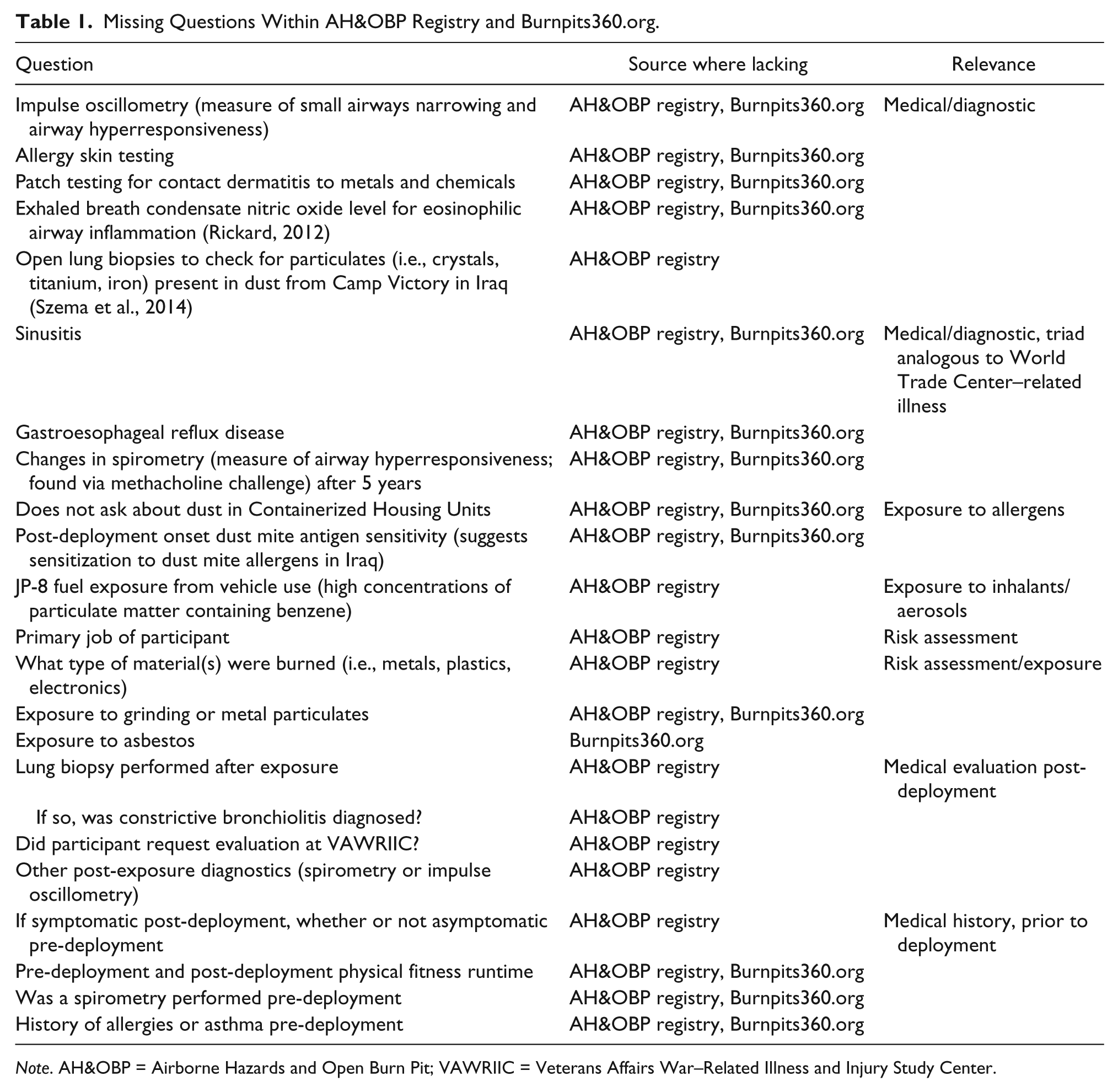
Note. AH&OBP = Airborne Hazards and Open Burn Pit; VAWRIIC = Veterans Affairs War–Related Illness and Injury Study Center.
While the Burnpits360.org registry does ask participants if post-deployment pulmonary function tests (PFTs) and lung biopsies were performed (12.5% reported having PFTs performed and 8.3% reported receiving a lung biopsy), it does not ask about lung biopsy results. Neither registry asks about constrictive bronchiolitis (CB) as a post–lung biopsy diagnosis, further limiting information available to assess lung health. Limitations exist for individual questions asked by the AH&OBP Questionnaire (Table 2).
Limitations in Questions From AH&OBP Questionnaire.

Note. AH&OBP = Airborne Hazards and Open Burn Pit; IED = improvised explosive devices; PTSD = posttraumatic stress disorder.
Categorization of Burnpits360.org Participants.

Note. BP = burn pit.
Participant data from the Burnpit360.org site were analyzed for this study and were associated with DD214 forms. The survey asked specific questions pertaining to symptoms experienced by these veterans, post-deployment (Table 4). Of the 38 participants, 23.7% stated that they worked at the burn pits, 26.3% stated no burn pit duties, while 50% omitted information regarding burn pit duties. From a sample size of 38 (confirmed by DD214 forms), 58% of participants reported general respiratory system–related symptoms. Symptoms reported include, but not limited to shortness of breath (45%) after minimal activity, chronic cough (68%), and asthma-related symptoms (26%). In addition, 11% reported to have been diagnosed with cancer post-deployment. The Burnpit360.org survey also inquired whether veterans received diagnostic testing after deployment. Of the 38 participants, verified by DD214 forms, 8.3% reported to have undergone lung biopsies and 12.5% were evaluated by PFT. The survey also inquired whether or not post-deployment services were made available to participants. The AH&OBP questionnaire omits the 309 cases of CB present in Iraq–Afghanistan War veterans, since it does not inquire specifically about lung biopsies and CB.
Medical Symptoms: Burnpits360.org Participants.
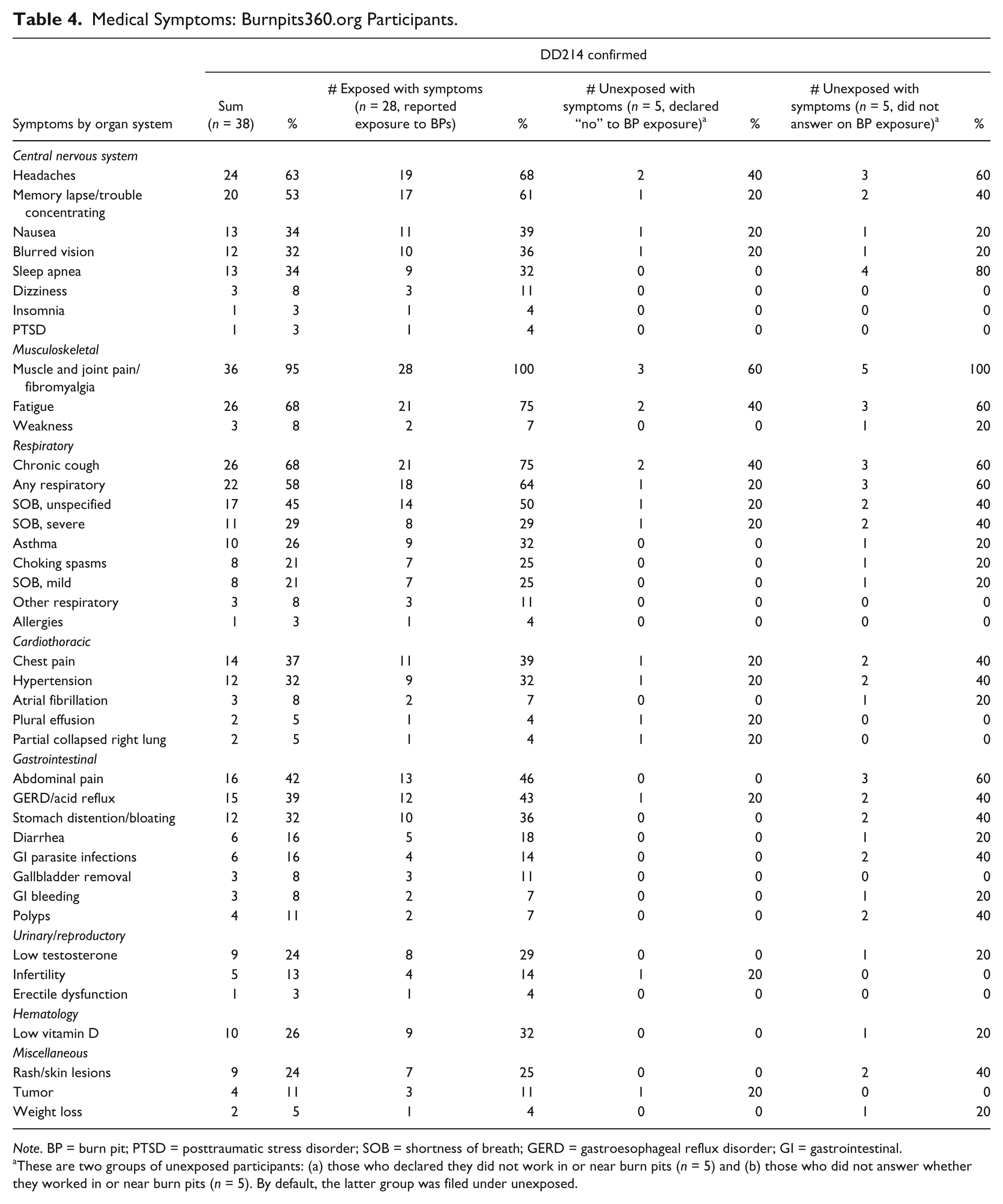
Note. BP = burn pit; PTSD = posttraumatic stress disorder; SOB = shortness of breath; GERD = gastroesophageal reflux disorder; GI = gastrointestinal.
These are two groups of unexposed participants: (a) those who declared they did not work in or near burn pits (n = 5) and (b) those who did not answer whether they worked in or near burn pits (n = 5). By default, the latter group was filed under unexposed.
The only demographic data available from Burnpits360.org are the ages of some of the participants. No information was provided regarding date of birth, race, or gender. Of the 11 participants (27.5%) who reported their ages, they ranged between less than 30 and 54 years of age. Among the 19,082 participants of the AH&OBP database, most were between 35 and 44 years of age; however, the range was greater from younger than 30 to older than 55 years. The AH&OBP registry does not stratify the percentage of personnel who reported burn pit duties within a given branch of service. What is actually reported is the fraction of the total number of soldiers among all branches of service who reported exposure to burn pits and reported to have burn pit–related duties. Since the majority of deployed troops in Iraq and Afghanistan were in the Army, it is critically important to know what percentage of Army forces was exposed to burn pits.
Not every participant of the Burnpits360.org website reported his/her number of Middle East deployments or total lengths of service. However, among those who reported their number of deployments and/or lengths of deployments, length of deployment ranged from 12 to 35 months. Of those with specified deployment lengths, 2.7% reported serving for less than 6 months, 13.5% reported 6 to 11 months of service, 62.2% reported serving 12 to 13 months, and 5.4% reported serving 24 to 35 months. Of those reporting burn pits duties, the majority (77.8%) served 36 to 47 months, while 11.1% served 12 to 23 months. The majority of those who did not report having burn pit duties (57.1%) served 12 to 23 months, while 14.3% served fewer than 6 months. Only 3.6% served more than 48 months.
The Burnpits360.org website does ask specifically whether personnel were exposed to other air contaminants while deployed. However, among these participants, 5% reported exposure to fuels. Of the Burnpits360.org participants, 13.5% reported working in vehicle operations. The number of participants with burn pit duties in this group is unknown; however, of those with unknown burn pit duties status, 27.8% also reported working in vehicle operations.
Refueling maintenance affected only a limited number of deployed troops (8.1%), with 22.2% of those with burn pit duties. The other deployment-related environmental exposures, reported in the Burnpits360.org registry, included agriculture duties, with 2.7% of the total participants exposed to pesticides. The Burnpits360.org website did not ask questions about exposure to inhalants outside from military duty.
Based on responses provided by the Burnpits360.org participants, we found that 13.2% of total participants were exposed to vehicle pollutants from the flight line or air base, 5.3% were exposed to fuels (likely fumes), and 10.5% were exposed to a combination of pollutants. Only 2.6% had agricultural exposure (possibly due to pesticides). The type of non-occupational exposures for the remaining 71.1% is not specified.
Of the 38 Burnpits360.org participants, 45.5% claimed to be former smokers and 54.5% claimed to be non-smokers. Twenty percent of all participants reported smoking between 0 and 5 years, 20% reported smoking between 11 and 16 years, 50% reported smoking 17 and 25 years, and 10% reported smoking for more than 25 years. None smoked between 6 and 10 years. Of former smokers surveyed by Burnpits360.org, all of whom reported burn pits exposure, 100% reported to have smoked between 1 and 2 packs of cigarettes per day. Of the total number of Burnpits360.org participants, 45.5% reported being former smokers, while 54.5% were nonsmokers. There was an even split of former smokers and nonsmokers among both those who reported burn pit duties in the Burnpits360.org survey and those who did not report burn pit duties. Among participants whose burn pit duties remain unknown, 40% reported previous smoking histories, while 60% reported no smoking history. Ages and amount of cigarettes smoked among current smokers, as well as whether or not the participants started smoking during deployment cannot be determined as this was unreported by Burnpits360.org participants; however, total years smoking and amount of cigarettes smoked among former smokers was recorded and is as follows: Of participants reporting burn pits duties, an even number reported smoking between 0 and 5 years, 11 and 16 years, and 17 and 25 years (33.3% each), while 0% reporting smoking for either 6 and 10 years or >25 years. Among those who did not report burn pit duties, 66.7% reported smoking 17 to 25 years and 33.3% reported smoking >25 years, with 0% smoking for anything less than 17 years. Only 20% of those with unknown burn pits duties status reported smoking 17 to 25 years, while 10% each reported smoking 0 to 5 years and 11 to 16 years. All former smokers, regardless of their burn pit duties statuses, reported smoking between 1 and 2 packs of cigarettes per day. Information provided by Burnpits360.org participants was insufficient to suggest what type of smoking products each participant used prior to deployment, or whether an individual started smoking during deployment. Similarly, there is no information provided about participants’ alcohol consumption prior, during, or after deployment.
Reports of living quarters distance by all Burnpits360.org participants revealed that 2.6% lived less than 100 meters from the burn pits, 7.9% lived at a distance of 100 to 200 meters from the burn pits, 7.9% lived between 300 and 500 meters away, 5.3% lived at a distance between 500 meters and 1 kilometer away, and 5.3% lived at a distance greater than 1 kilometer. Seventy-one percent of the registry either did not specify by distance or omitted a response. Among participants who specified burn pits duties, 11.1% lived less than 100 meters from a burn pit, while 22.2% lived between 100 and 200 meters; 66.6% of participants either did not specify by distance or omitted a response. Those who reported no burn pits duties also either did not specify by distance or left their responses blank. Of those whose burn pits duties status is unknown, 5.3% lived between 100 and 200 meters from a burn pit, 10.5% lived between 300 and 500 meters away, 10.5% lived between 500 meters and 1 kilometer away, and another 10.5% lived at a distance greater than 1 kilometer away. The remaining participants of unknown status either did not specify by distance or omitted a response. With regard to working quarters distance from burn pits, 26.3% of all participants reported living less than 100 meters from a burn pit, 7.9% worked between 100 and 500 meters away, 2.6% worked between 500 meters and 1 kilometer away, and another 7.9% worked at a distance greater than 1 kilometer away; 55.3% either did not specify by distance or omitted a response.
Among those reporting burn pits duties, 44.4% worked at a distance less than 100 meters from a burn pit, 11.11% reported working 100 to 500 meters away, and the remaining 44.4% did not specify by distance or omitted a response. Ten percent of those reporting no burn pits duties worked less than 100 meters from a burn pit, 10% worked between 500 meters and 1 kilometer from a burn pit, and 15.8% worked at a distance greater than 1 kilometer from a burn pit; 47.3% either did not report a specific distance or did not respond. Of the 50% of all participants had duties, which required them to be less than 100 meters from the burn pits while stationed at their base; 14.3% worked between 100 and 500 meters from the burn pits, 7.1% worked 500 meters to 1 kilometer from the burn pits, and 28.6% worked more than 1 kilometer away. Of those who reported burn pit duties, all worked within 500 meters, with the vast majority (66.7%) working less than 100 meters away; and all of those who did not report burn pit duties worked 500 meters to 1 kilometer away from the burn pits. Sixty percent of those whose burn pits duties status remains unknown worked within 500 meters of the burn pits, with 50% working less than 100 meters away. The remaining 40% worked more than 1 kilometer away.
Discussion
Both registries provide a basic understanding of the exposure, such as identifying burn pits duties among deployed military personnel, but do not elaborate on the extent of these duties. Similarly, the absence of several key questions makes analysis of either data set incomplete. However, strengths and weaknesses of both registries become evident when looking at the information obtained. Examples of the AH&OBP registry’s strengths include a broader base of volunteers from which to interpret data; it asks participants of non-military occupational exposures to dust, gas or fumes, and asbestos; and it also asks detailed questions on alcohol intake and smoking history.
The Burnpits360.org registry does ask whether or not its participants are smokers, nonsmokers, or former smokers, as well as the number of packs per day (similar to the AH&OBP questionnaire), but it does not give their alcohol history. However, the Burnpits360.org registry asks specific questions regarding their exposure to burn pits, such as whether or not they were provided masks and the proximity of their living and working quarters from the burn pits. The AH&OBP registry fails to provide this information; additionally, though the AH&OBP report states that nearly all participants were exposed to burn pits, it considers those who did not specify a deployment segment to be “unexposed” (U.S. Department of Veteran Affairs, 2015). Because of this narrow definition of exposure, a potentially large number of military personnel who were exposed may be underreported.
A problematic area in the AH&OBP questionnaire is its approach to dust exposure. It asks participants whether they were exposed to dust storms during deployment, even though soldiers may not be aware when they are exposed to dust storms. Soldiers firing weapons from a supine position are constantly exposed to contaminated dirt and dust, even in the absence of dust storms. Being present in a desert environment, as all deployed participants were, exposes them to metal-laden dust, regardless of proximity to burn pits or status of burn pit duties. Additional instances of dust exposure include being in the presence of Humvees, which stir up surface dust, even in the absence of dust storms.
The Burnpits360.org reported symptoms, illnesses, cancer diagnoses, and cancer statuses, as well as whether or not post-deployment services were at all offered. These details provide deeper insight into the illnesses developed in returning military personnel. Despite the inclusion of post-deployment symptoms and illnesses, the Burnpits360.org registry lacks information on the triad of cough, reflux, and sinusitus (Table 1), analogous to World Trade Center–related illness, which would also be relevant to this analysis. The AH&OBP registry also omitted any information pertaining to this triad. Without further elaboration, one cannot determine with full confidence whether troops developed these symptoms (sinusitis, gastroesophageal reflux disorder, or airway obstruction) prior to or after their deployments.
Omissions of other questions (Table 1) and limitations of questions provided within the AH&OBP questionnaire (Table 2) prohibit extensive analysis of the onset of the myriad of diseases developed by veteran participants. Other AH&OBP questions ignore details, which would also explain lung injuries. Question 1.3.B (Table 2) asks the length of time participants were exposed to heavy smoke from various sources, but does not reflect the fact that many soldiers had multiple deployments, or that the number of times per week participants were exposed varied, depending on the dates and location of deployment. Although one exposure alone is sufficient to cause symptoms, prolonged and repeated exposure to burn pits may exacerbate these conditions. Furthermore, the frequency of burn pit activities varied dependent on the specific deployment segment a soldier served. Additionally, when responding to the AH&OBP registry questionnaire, soldiers were unable to specify burn pit frequencies for specific deployment segments. Furthermore, when soldiers are out in the field, outside of military bases, personnel are required to burn their own trash. The AH&OBP registry does not inquire about nor mention these exposures to burning trash and human waste, which are not associated with burn pit exposure.
The length of the questionnaires may also play a role in the responses provided by participants; in conjunction with the lack of rewards from taking the questionnaires, participants may have been less incentivized to thoroughly answer the questions, and other veterans suffering from related illnesses may have not felt it necessary to participate. These issues also limit the capacity to further additional analyses of IAW-LI in Iraq and Afghanistan War veterans.
Answers to these questions, as well as elaboration on questions that were limited in scope or omitted, would allow a superior comparison of the soldiers’ overall health pre-deployment and post-deployment and increase comprehension of the effects of burn pits and various lung-related injuries present in Iraq–Afghanistan War veterans. Additional questions to be considered in more detail, particularly to improve understanding of nonburn pits–related illnesses, would be those on sandstorms and IED exposure. (Questions asked on IED exposure are currently too limited, ignoring traumatic brain injury and posttraumatic stress leading to IAW-LI as well as asthma.)
Based on the information obtained from both the AH&OBP and Burnpits360.org registries, a list of clinical guidelines for the treatment of returning IAW-LI soldiers has been compiled. This article has highlighted the gap in evidence and the need for a consistent evidence-based approach to managing IAW-LI. Our proposed recommendations (based on our team’s clinical experience) for testing soldiers entail:
Tracking military personnel’s 2-mile run times, as well as performing spirometry examinations pre-deployment and post-deployment (Rose et al., 2012; Vonfeldt, Robinson, & Rose, 2012);
Excluding allergic asthma from the list of possible symptoms/illnesses;
Performing fractional exhaled nitric oxide examinations via NIOX (Rickard, 2012);
Skin testing military personnel for allergies;
Performing impulse oscillometry examinations on military personnel pre-deployment and post-deployment (Manoharan, Anderson, Lipworth, & Lipworth, 2015; Short, Anderson, Manoharan, & Lipworth, 2015);
Having military personnel exercise while using a right heart catheter, as well as undergo a stationary echo to compare results of pulmonary circulation during exercise (Keusch et al., 2014). Alternatively, in our experience, some soldiers can avoid right heart catheterization when their pre- and post-exercise transthoracic echocardiogram show pulmonary artery hypertension on the basis of estimation from the tricuspid regurgitation jet;
In patients healthy enough to tolerate biopsies, performing biopsy when symptoms are out of proportion to test results (Findikcioǧlu, Kiliç, Karadayi, Canpolat, & Hatipoǧlu, 2014; Han et al., 2015);
Sending biopsy samples to a laboratory for iron stains, polarizable crystals, and electron microscopy for metal analysis, and follow-up with submission of these samples to a center for Synchrotron Studies to determine if metals are bound in fixed mathematical ratios (Szema et al., 2012) and whether they are found in certain geographic locations in the lung(s) with a quantification of the metal amount;
Providing reassurance to veterans that their illness is not psychological;
Accurately characterizing veterans’ diseases so appropriate future therapies can be tested;
Potentially administering RuX (Patent Number 86013581), a novel medication which has been shown to attenuate lung injury from Iraq dust in mice. Another possible future therapy with success in lung injury models is Vasoactive Intestinal Peptide (VIP), which has an IND from the FDA.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
