Abstract
Men are less willing to seek health professional advice than women and die more often than women from preventable causes. Therefore, it is important to increase male engagement with health initiatives. This study reports the outcomes of a student-assisted, interprofessional, 12-week health program for overweight adult males. The program included weekly health education and structured, supervised group exercise sessions. Thirteen males (participants) and 18 university students (session facilitators) completed the program. Participants were assessed for a range of health and physical activity measures and health and health profession knowledge. Participants demonstrated significant improvement in activity, knowledge, and perceptions of physical and mental function, and appreciated the guided, group sessions. Students completed an interprofessional readiness questionnaire and reported significant improvement in the understanding of the benefits of interprofessional education and of their role in health care. This program provides evidence of the dual benefit that occurs from the delivery of a student-assisted, interprofessional men’s health program to at-risk community members.
Introduction
Health professionals have identified males as a “hard to reach” population for health promotion and illness prevention initiatives (Bottorff et al., 2014). Males are less willing than females to have an annual checkup, seek health professional advice and attend health education sessions (Bottorff et al., 2014; Harris & McKenzie, 2006), and die more often than females from preventable causes (Bilsker, Goldenberg, & Davison, 2010). It is therefore important to increase male engagement with health-related education and activity by developing male-specific health promotion programs. Approaches that challenge male attitudes to health based on beliefs about traditional masculinity and the socially prescribed roles of the male (Galdas, Cheater, & Marshall, 2005) are recommended. While structured exercise interventions for men are effective at reducing cardiovascular disease risk factors in older adult males (Kerr, Leicht, & Spinks, 2008; Lee, Paffenbarger, & Thompson, 2001), group exercise combined with education has additional psych–social benefits for men, such as improved motivation to exercise, the formation of new friendships, and the feeling of shared identity and normalization of experiences (Barnett, Yau, & Gray, 2014). Combined exercise and education programs have also resulted in improved physical health outcomes such as weight and blood pressure reduction, increased self-reported physical activity, positive alterations in quality of life measures, and confidence with ability to access health care for adult males with diverse health conditions (Barnett et al., 2014; Bazzano et al., 2009; Morgan et al., 2014; Schutgens, Schuring, Voorham, & Burdorf, 2009). Delivering healthy lifestyle programs that combine exercise and health education in collaboration with sporting organizations has been reported to increase health outcomes for both younger (Pringle et al., 2013) and middle-aged to older (Sealey, Twomey, Pringle, Cheffins, & Gupta, 2013) adult males. It has been suggested that the success of these programs is men’s familiarity and comfort with the setting (Bottorff et al., 2014). However, reliance on sporting club settings reinforces some of the male stereotypes that can contribute to poor male engagement with health services and may not engage those males who do not fit the sport stereotype. A health or clinic-based setting may provide an alternative environment without stereotypical gender associations. Contemporary health service delivery promotes an interprofessional practice model of patient care and this is enacted through the development of interprofessional health clinics (Timpone, 2012). The Interprofessional Diabetes Clinic in Washington County is a university-based collaborative teaching and practice model that combined interprofessional practice with interprofessional education (IPE; Timpone, 2012). IPE is defined as “Occasions when two or more professions learn from, with and about each other to improve collaboration and the quality of care,” and there is general agreement that IPE during health training programs is the most effective way to embed interprofessional practice skills in the future health workforce (The Interprofessional Curriculum Renewal Consortium, 2013). The Interprofessional Diabetes Clinic resulted in high patient satisfaction with the provision of care and the flow between services, and high student agreement that the practice enhanced their appreciation of the value of interprofessional care that they benefited from the interaction with other student professionals, and gained better knowledge of the roles of other professionals in patient care (Timpone, 2012). Similarly, students who participated in IPE via case conferencing agreed that it was an effective learning experience, that they learned how other disciplines approach patient care and that the interdisciplinary approach had advantages over single-discipline patient care (Jobst et al., 2013). In light of the health benefits associated with group exercise and education programs, and the benefits of interprofessional models of practice and education, the aim of the current project is to pilot and report on the outcomes of a student-assisted, interprofessional, 12-week education and exercise program for overweight adult males. This article explores the following:
The health outcomes and change in health service knowledge of participants
Participant satisfaction with an interprofessional model of student-assisted health program delivery
Student learning outcomes as they relate to men’s health promotion, discipline-specific, and interprofessional skills and knowledge.
Method
This project received ethics approval from the James Cook University Human Ethics Committee (H5732). This project was a pilot study.
Participants
Men aged 35 to 65 years, with a self-measured waist girth of greater than 94 cm were eligible to participate. A $99 registration fee was charged to assist with cost recovery. Fourteen participants commenced the program and 13 finished, with 1 participant transferring to an individualized program. Students currently enrolled in the Dentistry, Exercise Physiology (Clinical), Medicine, Nursing Science, Pharmacy, Physiotherapy, Psychology and Speech Pathology courses at James Cook University were invited to participate. Most students were in the final year of their course and the earliest involvement was at the end of the second year of study. Discipline mentors assisted students in preparing for the education session and attended the program evenings when their student group presented. Prior to the program commencement, students met with the program leader (senior lecturer, Exercise Physiology) and the interprofessional coordinator for induction sessions and assistance with education session design. The program leader facilitated the program sessions, supervised the education sessions with the relevant discipline mentor, and collected and analyzed the program outcomes. A recently graduated Accredited Exercise Physiologist was employed to lead the group exercise sessions with assistance from students.
Program Design
The program ran for 12 weeks and consisted of a 10-week (Weeks 2 to 11) combined exercise and education program with a program introduction and baseline data collection (Week 1) and follow-up data collection and program evaluation (Week 12). The session that was scheduled for Week 10 coincided with a public holiday and therefore home-based challenges were set for that week.
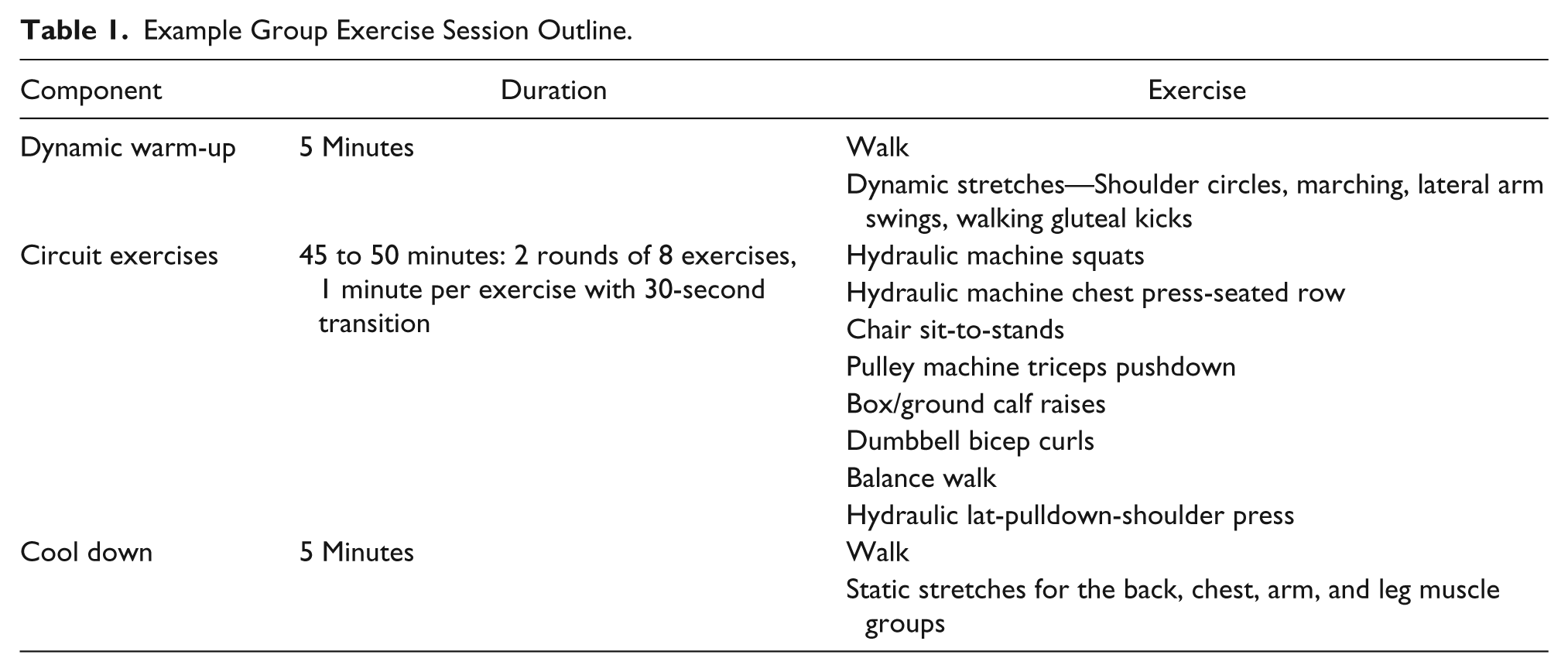
The exercise component of the program involved participation in a 1-hour group exercise class for each of the 10 weeks. The group exercise program was specifically designed to be suitable for the range of fitness and health conditions with inclusion of alternate exercises as needed, and included slight exercise or intensity progressions each week. Each session incorporated a 5-minute dynamic warm-up, a 45- to 50-minute combined low-moderate intensity cardiovascular and resistance circuit session and a 5-minute stretching cool down. Every participant had blood pressure measured before participating in each exercise class. An example exercise session outline is provided in Table 1.
Example Group Exercise Session Outline.
In addition to the once-weekly supervised group exercise session, participants were each provided with a pedometer (Yamax Digiwalker, Tokyo, Japan) and were encouraged to achieve 10,000 steps each day and to record the daily steps in the diary provided. The Yamax pedometer is a reliable and valid device for measuring step count (Crouter, Schneider, Karabulut, & Bassett, 2003). The 10,000 steps per day recommendation matches the “active” classification for physical activity (Tudor-Locke & Bassett, 2004) and is an acknowledged daily physical activity recommendation (Choi, Pak, Choi, & Choi, 2007). The 10,000 steps program has been successfully implemented as a self-regulated physical activity measure in regional Australian communities (Brown, Eakin, Mummery, & Trost, 2003). While the one group exercise session each week alone does not meet the recommendations for regular physical activity (American College of Sports Medicine, 2014), the combination of the group session and the self-regulated walking program should.
Each week, students from one discipline presented a 1-hour health education session to participants and to students from other disciplines (Table 2). At the start of each education session, students would explain the role of their health discipline in providing health care services. Students were scheduled to attend at least 3 weeks of the program, one when they were presenting and two other sessions where they were able to observe and participate in education activities led by other disciplines and the exercise sessions. Some students voluntarily participated in additional weeks.
Overview of Weekly Student-Delivered Education Sessions.

Note. CVD = cardiovascular disease.
At the end of each evening session, students would participate in a 15- to 20-minute debriefing session facilitated by the program leader. During these sessions, the students discussed what they had learnt about, how the participants responded, and discussed how each health profession could assist with the delivery of health services associated with that evening’s education session.
Outcome Measures
At the baseline and final data collection sessions, participants completed a series of physical health measures, surveys, and questionnaires. The physical health measures included height, mass, body mass index (BMI, calculated from height and mass), waist girth, and resting blood pressure. BMI, waist girth and blood pressure are known risk factors for cardiovascular disease (American College of Sports Medicine, 2014). Participants completed the International Physical Activity Questionnaire Short Form (IPAQ; Ekelund et al., 2006) and the Short Form 12 Health Survey® (SF12; Maruish, 2012). The IPAQ is a valid and reliable self-report questionnaire (Craig et al., 2003) that provides a 7-day recall of time spent being physically active and has been used previously to assess physical activity programs that included the 10,000 steps goal (De Cocker, De Bourdeaudhuij, Brown, & Cardon, 2011). The IPAQ includes four questions that ask the participant to quantify the duration of vigorous-intensity physical activity, moderate-intensity physical activity, walking, and sitting that occurred in the previous week. The SF12 is a 12-item self-report questionnaire that provides a quantitative measure of physical and mental components of health. The survey includes a 5-point overall health rating, questions relating to the frequency and extent of daily activity limitations associated with general health, physical and emotional health problems and pain, and a 1-week recall of emotional state. Participants completed a questionnaire that asked them to describe the role that each of the eight participating health professions have in providing health care services to community members, with the responses scored according to correctness and comprehensiveness of the answer. One mark was assigned for each answer that was both correct and comprehensive, while a half mark was assigned if the response was correct but brief in detail. Participants also completed a nine-item health knowledge questionnaire designed by the students and that was based on the content of the education sessions. The health-knowledge questionnaire was scored in the same way as the health professions questionnaire.
Students completed the same health professions knowledge questionnaire as the participants, and completed the Readiness for Interprofessional Learning Scale (RIPLS) questionnaire, which is used to explore student perceptions and attitudes toward interprofessional learning (Parsell & Bligh, 1999). Items 10 to 12 and 17 to 19 of the RIPLS were recoded for analysis due to the negative nature of the wording, to allow for an overall RIPLS sum to be reported.
At the final session, the participants and students completed paper-based evaluations and attended separate focus groups facilitated by the program leader and the interprofessional coordinator.
Statistical Analysis
Data from the participant health measures and questionnaires are reported as means and standard deviations, while evaluation information collected from surveys and focus groups were reported as common themes and example responses. Preprogram and postprogram comparisons were carried out using repeated measures analyses of variance with an alpha significance level of p < .05. Cohen’s d effect sizes were calculated as the difference between the premean and postmean, divided by the combined standard deviation. Data included in the repeated measures analyses of variance were normally distributed with no violation of standard statistical assumptions.
Results
Participant Health Outcomes
The average age of participants was 50 ± 8 years (range: 35-64 years). Participants self-reported the presence of health conditions such as cardiovascular disease, diabetes, acute and chronic musculoskeletal complaints, inflammatory bowel syndrome, and gout. Participant attendance averaged 11 out of 12 sessions (range: 9-12). Participants indicated being overweight, having current health conditions, and the opportunity to participate in a group program as the motivators for participation. Postprogram changes in blood pressure, waist girth, mass, and BMI were not statistically significant (p = .05-.65, Table 2). Participants reported a range of lifestyle changes adopted throughout the program, such as modifications to exercise, nutrition, dental hygiene, and medications, that resulted in a positive shift in physical and mental function (SF12) and physical activity (IPAQ; Table 3), as further evidenced by the following participant comments: Feel more energetic, not as breathless when I do things like climbing on truck etc. (Survey Response) Better sleep, more relaxed compared to time prior to the program. (Survey Response)
Prehealth and Posthealth Measures and Questionnaire Responses.
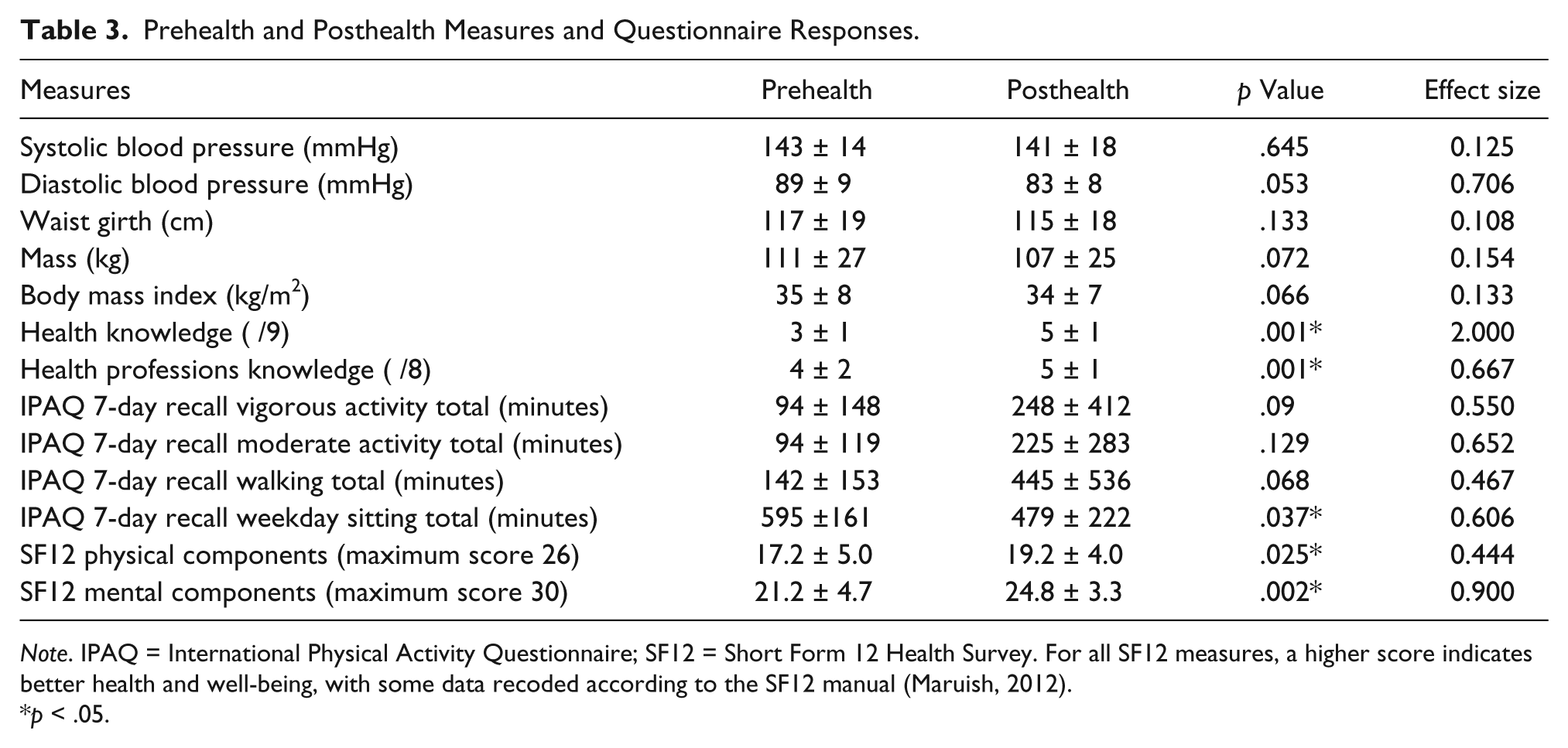
Note. IPAQ = International Physical Activity Questionnaire; SF12 = Short Form 12 Health Survey. For all SF12 measures, a higher score indicates better health and well-being, with some data recoded according to the SF12 manual (Maruish, 2012).
p < .05.
The group average daily step count was approximately 6,600 steps (range: 1,500-8,700 steps). While steps did not increase across weeks, the pedometers were useful as an educational tool: One of the biggest incentives for me of the whole program was the pedometer diary . . . I was determined to try to increase that thing, I think the best I ever did in a day was 9,850 or something, I never got to the 10,000 but it was there remind me to try to go that extra bit of distance. (Focus Group Response)
Participant Satisfaction With the Student-Assisted Program
All participants rated the exercise sessions as useful (54% extremely useful and 46% very useful) and the majority rated each education session as either extremely or very useful (67%-91%). Participants appreciated the group setup, and the organized, tailored, and supervised routine of the exercise sessions.
Highlights of the education sessions included the students’ knowledge and professionalism, easily understood format, and informative and relaxed nature of the sessions. Sessions that included specific practical applications such as how to brush teeth and how to screen for prostate cancer featured highly in the positive participant comments. The participants were highly appreciative of the role students played in the program and were impressed by their dedication and professionalism, as indicated by the following response: The students did a great job. The fact they volunteered shows commitment to their career choice. (Survey Response)
All participants agreed that they would recommend the program to others, with reasons including the following: Great starting point for those who want to change lifestyle for the better. (Survey Response) It is good to have a safe place to talk about your health because men typically don’t do this in the workplace or other places . . . it is good where everyone has made the commitment to come into something and already you are opening yourselves up to new ideas and to talk. (Focus Group Response)
All participants also indicated that they were planning further lifestyle changes including increasing activity, diversifying activity, and improving time management. Overall, a key outcome of the program was the enhanced understanding of health: It has woke [sic] me up and think that actually each one of these things is part of my health and I need to update it all the time, I need to stay on top of my exercise, I need to stay on top of my healthy eating, I need to go to the dentist, I need to get my prostate checked, I need to do all of these to keep rolling forward. (Focus Group Response)
Student Learning Outcomes
In total, 18 students across eight disciplines participated, with 17 students completing the RIPLS questionnaires and survey, and 16 students participating in focus groups. Fourteen students participated in at least two sessions presented by other disciplines in addition to their own presentation; with the other four students participating in at least one other-discipline evening. There were three occasions where a student did not attend a scheduled session, and this was due to other assessments being due (two students) and car trouble (one student). Students from the Exercise Physiology and Psychology disciplines were able to include the program participation as clinical placement hours and the Speech Pathology students were able to include the education flyer that they designed for the participants in their professional portfolio. Students from all other disciplines indicated that their participation would not contribute to their course. Five students had prior experience in interprofessional activities, and this was linked to participation in group assessment or learning activities with other disciplines in previous subjects (four responses) and participation in another community-based program (one response).
There was a statistically significant positive change in the students’ responses to the RIPLS questions “I don’t want to waste my time learning with other health care students” (recoded numbers 4.4 ± 0.6 up to 4.7 ± 0.5, p = .04) and “I am not sure what my professional role will be” (recoded numbers 4.0 ± 1.2 up to 4.8 ± 0.4, p = .01), indicating an improved understanding of the benefits of IPE and of their role in health care. No other RIPLS changes were significant, despite a positive shift in the overall score (80.3 ± 12.7 up to 83.6 ± 7.6). When student responses were compared between those undertaking the final year of the degree (n = 12) and those in the earlier years of study (n = 3), the biggest RIPLS overall score change was seen in nonfinal year students (12 ± 10, median increase in overall score of 9; compared with 2 ± 4 median increase in overall score of 0). A student comment on the RIPLS questionnaire that illustrates the benefit of the program states Firstly, I had more autonomy during this IP clinic to develop skills in our own preferred way, where as our normal placements are followed closely by an educator. More independence allowed me to go to my own space and strengthen areas of practice that I feel is important. The most valuable aspects were working with people from different disciplines, of whom you had no prior connections, working in a new environment, learning to be a better communicator, getting real time feedback on how my area of practice affects peoples’ lives/health. (Survey Response)
Despite being able to provide basic information about each profession at program commencement, students significantly improved their knowledge of the role of the health professions from 5.2 ± 1.0 up to 6.3 ± 1.0 (maximum score out of 8; p < .001). The increased scores were mostly reflected in the additional level of detail provided to the answers.
Student participation in the exercise and the education sessions delivered by other disciplines’ resulted in a range of interprofessional learning outcomes: I learned about the role of other health professionals and how we all must work together to better a patients’ health. (Survey Response) I need to talk more to other professions as my understanding of their roles was obviously very limited. Pharmacy has a larger role to play. . . . Many of the professions overlap. By working together and giving similar advice we can improve health significantly, e.g., diet and teeth, overall health, etc. (Survey Response)
Students indicated the development of self-confidence, discipline and context knowledge, group speaking skills, leadership and communication skills, teamwork skills, organizational skills, professionalism skills and advocacy and engagement skills as a direct result of preparing and facilitating their discipline-specific education session, as highlighted in the following responses: Talking to men about sexual health is always challenging, so I suppose I honed the skill of getting people to engage, which will be important as a Doctor. (Survey Response) Furthering my knowledge base in the topic area, team bonding/working, confidence in myself, and advocating for our profession. (Survey Response) Cementing my knowledge of nutrition, teamwork skills, leadership, and communication. (Survey Response)
Students faced the challenges of time management, study commitments, nervousness with public speaking, and understanding the client’s circumstances. Despite these challenges, the students were overwhelmingly positive about their experience and reported that meeting and working with other students, seeing the health changes and enjoyment of the participants, achieving specific learning outcomes, and the overall program organization were the best aspects of the program.
Ability to work with other health professions, develop my knowledge, skills and educate others, make a difference and have fun learning. (Survey Response) Seeing the men after 10 weeks and noticing health changes. Knowing I provided them with valuable info to help them change their health is something really special and what I am proud of. (Survey Response)
All students indicated that they would recommend the program to other students with example responses including the following: For sure! There is a wealth of experience that you get from an opportunity like this that you wouldn’t normally get as an undergraduate student, definitely worth it. (Survey Response) Yes, again I feel that improving relationships with other health professionals will allow better communication in the workplace, and ultimately better the care towards the patients. (Survey Response)
Discussion
Overall, participants were highly satisfied with a student-assisted, interprofessional men’s health program that resulted in improved health outcomes. Students were highly satisfied with the professional and interprofessional learning opportunities afforded by the program.
This study resulted in significant improvement in both the health and health professions knowledge of the participants. Participants in an Ireland-based lifestyle intervention program for adult males also reported increased knowledge and awareness of health and health-related issues and the opportunity to talk to health professionals (McMahon, Hodgins, & Kelleher, 2002). The findings from both studies may indicate an increased likelihood for participants to undertake self-help measures to improve lifestyle and to seek assistance from the relevant health professionals when health concerns arise.
A significant improvement in both the physical and mental components of health and well-being was evidenced in the current program. The physical improvements related to reduced limitations associated with moderate activities and with climbing several flights of stairs and reduced incidence of problems with performing daily activities. The improved mental components were vitality and mental health, which were represented as the frequency of having a lot of energy in the past week, and the frequency of feeling calm and peaceful and not feeling downhearted and depressed in the past week, respectively. The improvement in the mental components of health was also evident in the survey and focus group comments with feelings of happiness, being relaxed, being energetic, and being in control reported. This relatively acute mental health improvement has been previously documented for healthy lifestyle and for exercise-only interventions in older adult males. (Sealey, 2010; Sealey et al., 2013). It appears important therefore to include exercise or physical activity in healthy lifestyle intervention programs for men due to the direct influence of exercise on well-being.
The participants (as a group) did not significantly improve their blood pressure, waist, or BMI measures across the program. However the 2/6 mmHg reduction in blood pressure, the 2 cm reduction in waist girth, and the 1-point reduction in BMI is similar to the proportional reduction in blood pressure noted as a significant outcome of a combined exercise and education program for unemployed adults (Schutgens et al., 2009), and may be a clinically relevant overall group improvement that requires statistical interrogation with a larger sample size. There was also a significant reduction in self-report weekday sitting time by approximately 2 hours, coinciding with a threefold increase in overall self-report weekly activity duration (330 minutes vs. 918 minutes) despite not achieving the 10,000 step per day target. Despite the daily steps being below the national average (Australian Bureau of Statistics, 2013), the pedometers were a useful awareness tool, allowing participants to recognize how much walking they typically undertake each day, and how much walking time is needed to achieve the recommended 10,000 steps.
Eighteen students from eight health disciplines assisted with the delivery of the men’s health program. The students experienced an interprofessional learning environment where they were able to teach and learn in a collaborative interprofessional environment. Students self-reported the development of a range of professional skills, knowledge, and attributes and significantly improved knowledge of the role of health professions in health service delivery. For those students who were in the early stages of their degree, a 12-point median change between the pre- and post-RIPLS was noted, and while no statistical comparisons were calculated due to the small sample size of this cohort, the early IPE experience may have contributed to positive student perception of and readiness to engage in interprofessional activities. Similar IPE learning outcomes of enhanced knowledge and respect and understanding of other professions have been previously reported for students who are positioned in the early stages of the degree; however, students reported concern about being forced to learn irrelevant skills (Tunstall-Pedoe, Rink, & Hilton, 2003). It has been acknowledged that students entering health degrees have already established stereotypical views of health professions, some of which are negatively oriented toward the “other” professions (Reeves, 2000). Incorporating IPE experiences early and frequently throughout the degree is expected to elicit positive changes in these views (Carpenter, 1995a). Parsell, Spalding, and Bligh (1998) described how IPE experiences in final year students across a range of health professions elicited a positive change in perception of professions, particularly with respect to knowledge of the role of other professions and enhanced respect. Similar attitudinal shifts were reported for final year students by Carpenter (1995b); however, the positive change was not consistent across all professions. In the current study, while the final year students did not report a positive change in their perceptions of IPE, it should be noted that their prior perceptions were already positive in nature and therefore the IPE experience may have consolidated the positive perceptions. Therefore, early IPE may reshape negative perceptions and provide the opportunity for early professional advocacy, while later IPE should aim to consolidate, enhance, and broaden professional skills and knowledge.
The self-reported achievement of learning outcomes in the current study included an appreciation of the roles of difference professions and the importance of interprofessional practice in the health services, enhanced communication skills particularly when discussing challenging or sensitive topics, improved discipline-specific content knowledge, enhanced teamwork skills, and improved ability to and recognition of the importance of advocating the profession in an interprofessional context. Previous projects have similarly reported student perceptions of enhanced learning with a focus on enhanced knowledge, working in teams, communication, ethical considerations, and problem-solving processes (Parsell et al., 1998; Ponzer et al., 2004; Tunstall-Pedoe et al., 2003). These findings provide evidence that IPE plays an important role in the development of professional skills, and future research should focus on processes to assess and assure the development of professional skills, knowledge, and attributes in authentic learning environments.
The strengths of the current program include the voluntary commitment by staff mentors and the students, institutional support, regular positive and constructive feedback to students (by way of weekly debriefing sessions), and the willingness of the participants to engage in a student-assisted program. These strengths align with the contact hypothesis model presented by Hewstone and Brown (1986), where positive attitudinal changes occur through a combination of positive expectations, cooperative environment, perception of typicality, institutional support successful joint work, status equality, positive feedback, and understanding of differences and similarities in roles.
The main limitations of the study design were the small sample size (pilot research), the absence of a control group, the absence of long-term follow-up data collection, and the inclusion of only one exercise session each week with encouragement to participate in self-directed walking on other days. An increase of supervised and structured exercise sessions to two or three sessions each week is likely to have resulted in further improvements in health outcomes in adult males, as evidenced previously (Kerr et al., 2008; Sealey & Tope, 2011). The main limitation of the student-assisted interprofessional component of the program was the limited number of sessions attended by students due to the pilot nature of this program and the inability for most students to count their participation as formal placement at the time of program establishment.
Future iterations of this program should consider broadening the scope of the education sessions, an increase in the number of exercise sessions each week, and involvement of more participants and students.
Conclusion
Overall, this program has provided evidence of the dual benefit that occurs from the delivery of a student-assisted, interprofessional men’s health program to at-risk community members. Participants enjoyed the program, improved in some aspects of self-reported health and well-being, and demonstrated increased knowledge of health care and health professional service provision. Students reported high satisfaction with program participation and reported improvements in and development of a range of professional knowledge, skills, and attributes as a result of assisting in the facilitation of a translational and authentic community-based program.
Footnotes
Acknowledgements
The authors gratefully acknowledge the contribution of the students and discipline mentors who assisted with program facilitation.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
