Abstract
The mental health needs of aging African American men have been overlooked and few studies have distinguished between more severe clinically diagnosable mental health challenges and less severe emotional states for this population. African American men may not identify with or internalize the terminology of “depression” despite exhibiting the symptom criteria. This exploratory cross-sectional study examined correlates of “downheartedness” as an alternative indicator of emotional health. The authors examined the self-reported responses of 1,666 older African American men on a baseline questionnaire from a larger longitudinal study. Demographic, physical, mental and emotional health, and health system factors were examined as possible correlates of downheartedness. The mean age of participants was 73.6 years and 74.8% of men described themselves as “downhearted and blue” most or all of the time while only 18.5% of them reported feeling moderate to severe anxiety or depression. When other factors were controlled, mobility problems (odds ratio [OR] = 2.36), problems getting health care (OR = 2.69), having a doctor who never listens (OR = 2.18), physical or mental problems that interfere with social activities (OR = 1.34), accomplishing less due to physical health (OR = 1.35), and accomplishing less due to mental/emotional health (OR = 1.57) were all associated with greater odds of being downhearted. The current findings indicate that this sample more closely identified with language accurately describing their emotional health state (i.e., downhearted) and not with clinical mental health terminology (i.e., depression) that may be culturally stigmatized.
The diagnosis and treatment of clinically significant depressive symptoms has been understudied for older African Americans, and the mental health needs of aging African American men have been particularly overlooked (Watkins, Hawkins, & Mitchell, 2015). Studies have reported that more than 7% of all African American men will develop clinically diagnosed depression during their lifetimes (Bryant, Ro, & Rowe, 2003). More recent studies have established that African American men are significantly less likely than men and women of other racial/ethnic groups to be identified for and receive timely diagnosis and treatment for depression and related mental health issues (Conner et al., 2010). Because mental health is a continuum that ranges from less severe emotional states to more severe and clinically diagnosed mental health problems, it is important to understand older African American men’s mental health through the use of emotional health cues. Such cues may include stress and distress (Payne, 2012; Ward & Besson, 2013; Watkins, Hudson, Caldwell, Siefert, & Jackson, 2011; Watkins & Neighbors, 2007) as well as diagnosable mood disorders such as major depressive disorder (MDD; Kendrick et al., 2007; Lincoln, Taylor, Watkins, & Chatters, 2011; Payne, 2012; Ward & Mengesha, 2013; Watkins, 2012; Watkins, Abelson, & Jefferson, 2013). Broader and more inclusive definitions of depression include both clinical depression (i.e., [Diagnostic and Statistical Manual of Mental Disorders] DSM-5-TR major depression, dysthymia, bipolar disorder, or adjustment disorder with depressed mood) and other, non-clinical states of stress and psychological distress, which are important to understand for the purposes of programmatic efforts that target aging African American men with poor mental health.
Of the studies that frame the mental health of African American men broadly, more inclusive symptoms of depression (and less severe social and emotional health states) have been introduced to help redefine ways to understand depression from the perspectives of the men themselves. Some studies suggest that the use of more culturally sensitive and gender-specific definitions of depression will be vital to community-based interventions and strategies to improve mental health outcomes for this underserved group (Watkins et al., 2013). More work needs to be done to distinguish between more clinically diagnosable mental health challenges and less severe emotional states for older African American men. In particular, older African American men are less likely than older African American women and older White men and women to be diagnosed and receive treatment for mental health conditions (Barry et al., 2014). Furthermore, our understanding is limited with regard to how older African American men characterize their own mental and emotional health states, a potentially important indicator of how they communicate their mental health symptoms to clinicians and others. Understanding and recognizing depression among older African American men is of particular importance because the Centers of Disease Control and Prevention reports that in 2013, the highest suicide rate was among adults age 45 to 64 years old, followed by older adults 85 years of age and older (Centers for Disease Control and Prevention, 2015). The current study examines a range of factors that may be associated with the self-reported mental and emotional states of older African American men. We begin with a brief overview of variations in mental health symptomatology.
The prevalence of psychiatric disorders varies by race, ethnicity, gender, culture, age, and the context in which people live. Depression is complex due to the intersectionality of these factors, the manifestation of behaviors, and the interpretation of symptoms. Findings from the National Institute of Mental Health Collaborative Psychiatric Epidemiology Surveys (2001-2003) indicate that African Americans have a lower lifetime prevalence of MDD compared with U.S.-born non-Hispanic Whites. However, MDD has been reported to be more persistent, severe, and disabling for African Americans in comparison with non-Hispanic Whites (González et al., 2010; Williams et al., 2007). Since depression is expressed differently across various groups, current symptom criteria may not capture all forms and types of symptoms (Jackson et al., 2010). Cultural context influences the expression and reporting of—and hence what is known about—the prevalence of depression, particularly among older adults (Jackson et al., 2010). Variants may exist within specific subcultures, such as the tendency to feel isolated or irritable among depressed African American men (Neighbors, Watkins, Abelson, Martin, & Krenz, 2012), or the experience of neurasthenia symptoms (chronic fatigue and weakness, loss of memory, and generalized aches and pains) among Latino/Latinas (Chun, Moos, & Cronkite, 2006) and feelings of anger, physical pain, or chronic fatigue among Asians (John, de Castro, Martin, Duran, & Takeuchi, 2012; Takeuchi, Chun, Gong, & Shen, 2002). Expanding the list of symptoms, and adding culturally equivalent expressions to the description of the symptoms that currently define MDD, might reveal higher rates of depression among various race/ethnic and gender groups, particularly those who are medically underserved such as older African American men.
Age, race, and gender intersect to uniquely influence the risk profile for depressive symptoms among African American elders. A nationally representative study of mental health in older African Americans reported that nearly 23% of older African Americans have experienced at least one lifetime mental health disorder and those between 55 and 64 years of age were significantly more likely to have a lifetime mood disorder and a lifetime anxiety disorder than African American elders ages 75 and older (Ford et al., 2007). The same study noted that older African American men were significantly more likely than their female counterparts to have any lifetime mental health issues. Similarly, Barry et al. (2014) reported that in a 10-year longitudinal study of mental health in 3,075 older adults, a higher percentage of African American elders were depressed at each interval over the 10 years, and African American elders were significantly more likely than White elders to experience the onset of depression over the study period. In the same study, African American men aged 70 to 79 years were 44% more likely to experience the onset of depression over 10 years than their White male counterparts, even after accounting for sociodemographic background, health history, and body mass index (Barry et al., 2014).
The underdiagnosis of depression and other mental health conditions in older African American men is largely undisputed. Considering evidence that 7% of all African American men will develop clinical levels of depression during their lifetime (Bryant et al., 2003), being African American and male has enormous implications for psychological health and well-being over the life course (Watkins, 2012; Watkins & Neighbors, 2012). Furthermore, this fact is amplified for older African American men who are less likely than their White counterparts to seek mental health treatment or to be appropriately diagnosed (Conner et al., 2010). As African American adults tend to conceal emotional health status (Baker, 2001), researchers have reported positive associations between self-concealment and indications of compromised mental health, such as depression, poor self-esteem, and lower levels of perceived social support (Jackson & Knight, 2006; Masuda, Anderson, & Edmonds, 2012; Wallace & Constantine, 2005). Individuals who do not disclose their symptoms are less likely to have their depression detected. Thereby, studies have reported that primary care physicians are less likely to detect depression among African American and Hispanic patients than among Whites, especially if the doctor and patient are of a different race (Bhugra & Mastrogianni, 2004). In addition, Magai et al. (2003) reported that both American and Caribbean individuals of African descent inhibit emotion more than other ethnic groups and hence tend to report lower rates of all negative effects which indicates the possibility of a common reporting bias among these two groups. It is important for clinicians to understand the context in which “DSM depression” exists for African American men and older African American men in particular. Understanding and empathy by clinicians who work with older African American men can be important for creating a successful therapeutic alliance.
There is a need to understand the mental and emotional health of aging African American men who meet criteria described by the DSM as well as the psychological distress that may coexist with (or be separate from) DSM disorders such as depression. For African American men, the stress or distress may be a response to demoralization following an experience of discrimination, fewer financial and social resources, and lack of environmental safety and stability. This can often complicate the willingness of some older African American men to seek help for depression and the ability of clinicians to treat depressed elder African American male patients. Furthermore, scholars have also examined how many African American men may not identify with or internalize the DSM terminology of “depression” despite exhibiting the symptom criteria (Kendrick, Anderson, & Moore, 2007; Payne, 2012; Watkins & Neighbors, 2007). There is a need to better understand culturally acceptable nomenclature around mental and emotional health for older African American men to reduce missed opportunities for diagnosis, treatment, and community support. Therefore, the purpose of this study is to characterize the self-reported emotional health of older African American men, including the factors that influence self-identification with more informal variations of mental health status such as feeling downhearted. A secondary goal is to understand participant characteristics as they apply to feeling downhearted and blue.
Method
Sample
Between 2006 and 2010, a large hospital system in Detroit, Michigan was funded by the Centers for Medicare and Medicaid Services to conduct a demonstration project to examine the efficacy of a longitudinal patient navigation intervention aimed at increasing preventive health screening completion among older African American adults enrolled in Medicare. In an effort to obtain a sample closely representative of the African American elders in Wayne County (where Detroit, Michigan is located) this parent study recruited 5,783 African American adults aged 60 years and older from more than 25 senior residences, nearly 100 senior activity centers, approximately 50 church groups catering to African American elders, and health clinics within the catchment area of the health system. The secondary sample for the current study consisted of the deidentified data for all 1,666 African American men in the parent study and focused on their responses to a structured baseline questionnaire consisting of items adapted from previous instruments to assess the following: mental and physical health history and status, access to and perceptions of health care, health behaviors and beliefs, and demographic items. A trained research assistant or nurse collected the baseline data by phone or in person and the institutional review boards of both the parent hospital and the affiliated university approved the study. Additional details for the parent study have been published elsewhere (Mitchell, Manning, Shires, Chapman, & Burnett, 2014). Using the self-reported responses of older African American men, the authors sought to identify a range of factors (including physical limitations, health care experiences, and others) that may be associated with mental and emotional health status in this population.
Measures
Dependent Variable: Downhearted and Blue
Research demonstrates that cultural variations exist in the subjective experience of depression, the presentation of depressive symptoms, and how individuals identify with and culturally define their emotional health. In particular, studies have documented that African American men often utilize terminology other than “depression” to characterize feelings of despair. To better understand how African American men in this study identify and label distress alternatively to “depression,” an item was utilized that asked, “During the past 4 weeks, how much of the time have you felt downhearted and blue?” Responses included all of the time, most of the time, some of the time, a little of the time, and none of the time. This item was further dichotomized for the analysis so that all of the time and most of the time were combined (coded as 1) and all other responses were combined (coded as 0). This item was developed and validated for the mental health subscale of the Medical Outcomes Study 36-item Short Form Health Survey (SF-36), version 1.0. This is a generic self-reported measure of health-related quality of life used widely in both research and clinical practice. The documented reliability coefficients for the SF-36 range from .65 to .94 across scales and with diverse populations (McHorney, Ware, Lu, & Sherbourne, 1994) and additional psychometric properties have been published elsewhere (McHorney, Ware, Lu, & Sherbourne, 1994; Ware, Kosinski, & Keller, 1996; Ware & Sherbourne, 1992). In addition, Cernin, Cresci, Jankowski, and Lichtenberg (2010) examined the SF-12 with 985 urban African American elders, including 208 older African American men from the Detroit City-wide Needs Assessment of Older Adults. They reported the instrument to be reasonably reliable (Chronbach’s α = .77) and valid for both the physical and mental health component scores with this population. Other studies have also validated the SF-12 and SF-36 in low-income samples of African American community members (Larson, Schlundt, Patel, Hargreaves, & Beard, 2008).
Independent Variables
Each of the independent variables is described below.
Demographic factors
Potential demographic correlates of being downhearted and blue were examined, including age, income, marital status, and living alone. Age was assessed as a continuous item and dichotomized close to the sample’s mean age to reflect participants older than 75 (coded as 1) and those under 75 (coded as 0). Income was constructed during analysis as a binary variable for men with an annual household income at or below $20,000 (coded as 1) and all others to compare men at the lowest self-reported income category with other participants. Marital status reflected those who were married (coded as 1) versus all others (coded as 0) and men who reported living alone (coded as 1) were categorized apart from men who lived with another person (coded as 0).
Physical health factors
Measures to characterize physical health were modified from the pain, general health, and role limitations due to physical health subscales of the SF-36. Due to the older age of this sample and the acknowledged possibility that indicators of physical health could covary with mental health outcomes, items available for secondary analysis were identified that might account for commonly experienced physical health issues such as pain and mobility. A single item to assess self-rated health asked participants to rate their health on a 5-point scale from excellent to poor and responses of fair and poor were combined to create a single category (coded as 1) of suboptimal health to compare with all other responses (coded as 0). Limited mobility was measured by a single item whereby men characterized their mobility as “having no problems walking about,” “having some problems walking about,” or “being confined to a bed.” A negligible frequency of participants reported confinement to a bed, thus, the item was transformed into a binary variable to reflect any problems with mobility so that “having some problems” and “being confined to a bed” were combined. Lastly, participants were asked the degree to which they had trouble performing usual activities such as work, housework, family, and leisure activities. Men who reported having some problems or being unable to perform usual activities were combined (coded as 1) and men reporting no problems performing usual activities were combined (coded as 0) to allow for a comparison of men with and without any functional mobility issues.
Mental and emotional health factors
Items to characterize mental and emotional health were adapted from the role limitations due to emotional problems, energy fatigue, emotional well-being, and social functioning subscales of the SF-36. Participants were asked in two separate questions, “During the past 4 weeks, how much of the time: (a) have you accomplished less than you would like and (b) have you not done work or other activities as carefully as usual—as a result of any emotional problems (such as feeling depressed or anxious)?” Potential responses to both questions included all of the time, most of the time, some of the time, a little of the time, or none of the time (1-5). Respondents were also asked to give an answer that came closest to how they had been feeling during the previous 4 weeks with regard to feeling calm and peaceful and having a lot of energy using the same 5-point scale. Anxiety and depression were characterized by a single self-reported item asking participants to indicate which statement best describes their own mental health state today (with regard to anxiety/depression). Responses were: I am not anxious or depressed, I am moderately anxious or depressed, and I am extremely anxious or depressed. Moderate and extreme self-reported anxiety or depression was collapsed into a single “any anxiety or depression” variable (coded as 1) with all other responses combined (coded as 0) to clearly delineate any issues with anxiety or depression from those having no reported issues. Finally, to assess the extent to which both physical and emotional health problems interfere with social functioning, participants were asked, “During the past 4 weeks, how much of the time has your physical health or emotional problems interfered with your social activities (like visiting friends, relatives, etc.)?” Responses were indexed on a 5-point scale from none of the time to all of the time (1-5).
Health system interactions
The five items available from the baseline questionnaire to measure the extent to which participants encountered problems interacting or communicating with health providers were adapted from the 2003 National Health and Interview Survey (Hesse, Moser, Rutten, & Kreps, 2006). Participants were asked, “During the past 12 months, how much of a problem, if any, has it been to get the care you or your doctor believed was necessary?” Responses included a big problem, a small problem, or not a problem. This variable was dichotomized with those having a “big problem” getting care, as the reference group. In addition, participants were asked four separate questions, “In the past 12 months, how often did your doctors or other health care professionals: (a) listen to you, (b) explain things in a way you could understand, (c) show respect for what you had to say, and (d) spend enough time with you?” Responses for all questions were always, usually, sometimes, or never. Each of these questions was dichotomized to reflect the never response as the reference category (coded as 1) and all others were combined (coded as 0) in order to draw a clear contrast between participants who had never experienced the aforementioned health communication issues and those who had, to any degree.
Analysis
Data for this study were analyzed using SPSS version 19. The frequency of baseline characteristics for the current sample were examined and are detailed in Table 1. A missing value analysis determined that missing values were randomly distributed across all observations and no single variable had more than 20% of missing cases. Item nonresponse was addressed with listwise deletion of cases. The authors decided that binary categories would best capture the more severe emotional health states reported by participants; and that focusing on older African American men who experienced emotional health disruptions most or all of the time would contribute most to an understanding of factors influencing their mental health status. Next, a bivariate analysis was conducted (using chi-square tests of association for categorical predictors and t tests for continuous predictors) to determine the strength and direction of relationship between the outcome variable (i.e., downhearted and blue), and each independent variable. Table 2 presents the categorical factors associated with the downhearted and blue emotional status among older African American male respondents. Table 3 presents the continuous factors. Finally, the authors predicted which older African American men were most likely to report feeling downhearted and blue most or all of the time in the previous 4 weeks in Table 4. Using the automatic stepwise selection procedure of backward elimination, significantly associated covariates were entered into a single model and then removed sequentially until a further deletion resulted in a significantly poorer fit.
Demographic Characteristics of the Sample (N = 1,666).

Bivariate Associations Between Downheartedness and Categorical Predictors.

Bivariate Associations Between Continuous Predictors and Being Downhearted or Blue.

Logistic Regression Model Predicting Downheartedness.
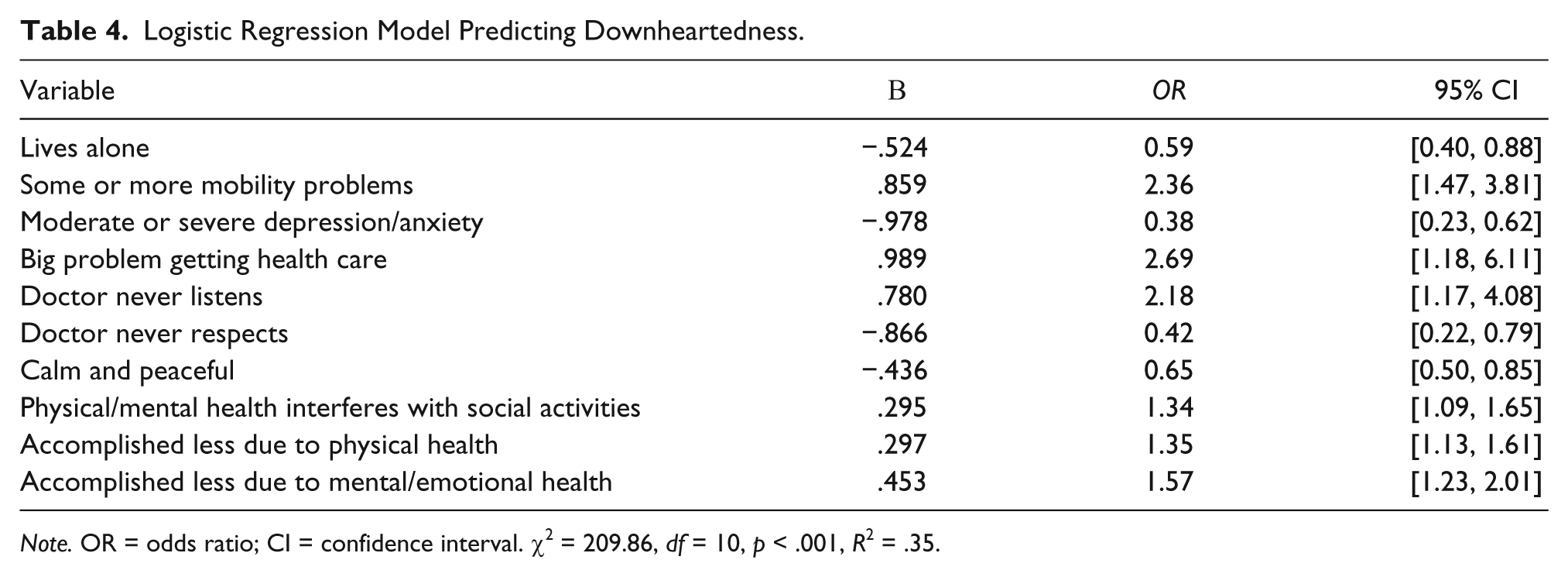
Note. OR = odds ratio; CI = confidence interval. χ2 = 209.86, df = 10, p < .001, R2 = .35.
Results
A total of 1,666 older African American men were included in the final analysis. About half of participants were 75 years of age or older (46.2%) and 38.2% had attended at least some college. Most participants reported an income of less than $50,000 per year (70.9%). The majority of them described themselves as “downhearted and blue” most or all of the time over the previous 4 weeks (74.8%) but only 18.5% of them reported feeling moderate to severe anxiety or depression on the day they completed the questionnaire. Additional demographic characteristics are described in Table 1.
Bivariate analyses resulted in a number of statistically significant associations between demographic, physical and mental health, and health system-related variables, and being downhearted or blue (Tables 2 and 3); those factors included increasing age, greater income, being married, and not living alone. Three of the four indicators of poor physical health (pain, limited mobility, and trouble with usual activities) were all inversely associated with being downhearted. Participants who indicated that they had a big problem getting care, a doctor who never listened, a doctor who never explained, a doctor who was never respectful, and a doctor who never spent enough time with them were all significantly more likely to report being downhearted compared with other participants. Those who reported that they were not downhearted or blue were more likely to report that they were calm and peaceful and had better self-rated health. Participants who indicated that they were downhearted and blue reported accomplishing less due to their emotional/mental health, accomplishing less due to their physical health, and that their physical or emotional health interfered with their social activities more often compared with participants who were not downhearted or blue.
Table 4 summarizes the binary logistic regression coefficients and the estimated change in odds for feeling downhearted and blue most or all of the time in the previous 4 weeks when all significant predictors are controlled. A test of the full model compared with the null model was statistically significant, χ2(10, N = 793) = 209.86, p < .001, R2 = .35. Reporting some or more mobility problems (odds ratio [OR] = 2.36), big problems getting health care (OR = 2.69), having a doctor who never listens (OR = 2.18), physical or mental that interferes with social activities (OR = 1.34), accomplishing less due to physical health (OR = 1.35) and accomplishing less due to mental/emotional health (OR = 1.57) were all associated with greater odds of being downhearted when other factors were controlled. Living alone (OR = 0.59), reporting moderate or severe depression/anxiety (OR = 0.38), having a doctor who was never respectful (OR = 0.42), and being calm and peaceful (OR = 0.65) were all associated with lower odds of downheartedness in the logistic regression model.
Discussion
The purpose of this study was to understand the factors associated with self-reported mental and emotional health among older African American men, namely, feeling depressed or anxious compared with feeling downhearted and blue. The present study demonstrated that self-reported depression or anxiety was negatively associated with feeling downhearted and blue among the African American men from the sample, which may suggest a disconnect between the way older African American men express (and link) their mental health in relation to their emotional health. Depression expression has been examined in previous studies, with a particular focus on the challenges of measuring depression among African American men (Kendrick et al., 2007; Payne, 2012; Watkins & Neighbors, 2007; Watkins, 2012) as well as the importance of language in community and clinical representations of depression among older men (Jarrold et al., 2011) generally and African American men specifically (Ward & Mengesha, 2013; Watkins & Neighbors, 2007). From a measurement perspective, research has underscored the value of richer, more in-depth examinations of the depressive experience for African American men; especially since reports have suggested that standard measures may not capture these experiences very well (Payne, 2012; Watkins & Neighbors, 2012). For example, measures for depressive symptoms, such as the Center for Epidemiologic Studies–Depression scale, was thought to be a less suitable measure for some samples of African American men (Love & Love, 2006) due to its more emotion-focused symptomology, which may be more characteristic of women (Branney & White, 2008; Perkins, 2013). Though there are mixed findings with regard to using the Center for Epidemiologic Studies–Depression with African American men, studies supporting the use of the CES-D with African Americans and other ethnic racial groups have been conducted (Roberts, Chen, & Solovitz, 1995; Watkins, Green, Rivers, & Rowell, 2006).
From a gendered perspective, there is a discrepancy between men’s outward and more physical displays of depression and predominately used emotion-focused assessment strategies (Perkins, 2013). This limitation impedes the accurate detection of depression in men and may contribute to the low incidence of depression in epidemiological reports (Branney & White, 2008). These challenges are exacerbated by the additional experiences of not only being male, but being an African American man. These confounding factors (i.e., being male and being African American) may result in difficulties in assessing the depressive experiences using instruments that were not originally developed with and for individuals matching these sociocultural and economic identities. Additional challenges in measurement are the result of such intersectionality and due to the widespread acceptance of depression as a part of the “Black experience” and the inevitability of African American life (Kendrick et al., 2007; Watkins & Neighbors, 2007).
Findings from the current study also underscore the importance of language in community and clinical representations for depression for African American men. The language of depression becomes essential in how African American men perceive their own mental health experiences and how they communicate symptomatology to clinicians. When discussing perceptions of depression with older African American focus group participants, Conner et al. (2010) reported that while participants could often identify clinical symptoms of depression such as “sadness,” they recognized those symptoms as normal experiences and did not connect depressive symptoms to having a MDD (Conner et al., 2010). The current findings that 74.8% of older African American men in the study reported being downhearted while only 18.5% described themselves as depressed or anxious may indicate that this sample more closely identified with language accurately describing their emotional health state, (i.e., downhearted); while eschewing clinical mental health terminology such as (i.e., depression) that may be more culturally stigmatized.
This study was motivated by a concern that older African American men in particular are at an increased risk for undiagnosed depression. Prior research reports that advanced age is negatively associated with depressive symptoms, psychiatric disorders, and psychological distress in older African American men (Lincoln et al., 2011). Scholars have termed this phenomenon the “healthy survivor effect,” whereby cohorts of older African American men without significant mental health issues are likely to live into advanced age or outsurvive their peers who experience more severe or persistent mental health problems (Ford et al., 2007; Lincoln et al., 2011). While older age was not a significant predictor of downheartedness in the final logistic regression model for this sample, accomplishing less than desired due to emotional issues and experiencing an interruption to social activities due to physical health or emotional problems both significantly predicted feeling downhearted. These findings are consistent with previous research that identified associations between functional limitations due to health problems, a lack of social support, and clinically significant depressive symptoms in older adults (Greenglass, Fiksenbaum, & Eaton, 2006).
Demographic and Health System Factors
This study revealed that older African American men who reported that their doctor “never listens” to them were over twice as likely as their counterparts to experience downheartedness most or all of the time. In line with this finding, consistent data indicate that patients who perceive that their doctor listens more and is more empathetic, report higher satisfaction with health care experiences, and feel more supported (Pollak et al., 2011). Furthermore, studies have reported that older African American men’s perceptions of physician attentiveness and communication are strong predictors of their satisfaction with and ratings of care, trust in physicians, and participation in informed decision making (Cooper et al., 2012; Moore et al., 2012). The body of knowledge relating physician who listen and communicate well to patient’s mental and emotional health outcomes is more limited; however, it is reported that patients who experience weak interpersonal relations with their physicians often feel that those physicians are ill-equipped to meet their mental health needs; patients report feeling deterred from disclosing psychosocial distress, or discussing possible depressive symptoms as a result (Kravitz et al., 2011). Very little is known about how older African American men’s experiences communicating with their physician influences their mental and emotional health outcomes, though the current study offers an important first step in this direction.
Limitations and Conclusions
The baseline questionnaire analyzed for this secondary study was cross-sectional and lacked random sampling, thus limiting the ability to establish causality and the capacity for making predictions about factors contributing to the emotional health status of this sample of older African American men beyond a limited scope of time. Furthermore, due to the secondary nature of the data, the authors were confined to the available items that were previously collected; thus, were unable to further analyze why some findings, such as marriage positively predicting downheartedness, were discordant with extant literature. Also, the original study did not utilize a validated measure of depression to inform a clinical diagnosis, thus the self-reported mental health measures represent a limitation to how the results are interpreted. Selection bias is a potential threat to external validity due to the lack of random sampling employed in the parent study. Lastly, the majority of participants were drawn from one geographical area, which further limits the ability to generalize findings to older African American men more broadly, and findings could be attributed to a number of factors beyond the scope of the current investigation, such as health literacy specific to mental health. These limitations notwithstanding, the authors believe that findings from this study support efforts to educate practitioners who work with older African American men about variations in the expression of DSM depression and about the role of sociodemographic, health communication, and other factors that accompany and complicate traditional depression care, and entry into care by some older African American men. Future studies seeking to overcome certain limitations noted in the current study might utilize a longitudinal nationally representative sample of African American men.
Although this study highlights a potential discrepancy in how some older African American men identify with clinical terminology to identify mental and emotional health status, which is an important clue to reducing missed opportunities for disclosure about psychological distress in this population, future studies should also assess the link between reported mild depression and terms such as “downhearted” and “blue” in this population. Furthermore, while important associations such as the relationship between anger and depression were not available for analysis in this study, future research might consider whether the expressed emotion of anger masks depressed mood among African American men in particular. More needs to be done to engage older African American men in more conversations about their feelings, in general, and depression more specifically.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received financial support for the research, authorship, and publication of this article in part from the Southeast Michigan Partners Against Cancer and the Centers for Medicare and Medicade Services (CMS; Award 1 AO CMS 3000068).
