Abstract
Fathers’ mental health help seeking is an understudied area. Using participants (N = 1,989) from the Fragile Families and Child Wellbeing Study, this study hypothesized that few fathers would seek mental health services; and increases in anxiety, depression, and parental stress would predict less mental health help seeking. Only 3.2% of the participants reported seeking mental health counseling. Among the three independent variables, only depression emerged as a significant factor that predicted less mental health help-seeking behaviors in fathers. Future research and clinical efforts need to better understand the low rates of help seeking and to identify pathways that facilitate positive mental health help seeking among fathers.
It is currently understood from the robust literature that men engage in less mental health help-seeking behaviors than women (e.g., Berger, Addis, Green, Mackowiak, & Goldberg, 2013). Prevalence rates of common mental health disorders such as depression and anxiety are typically lower for men compared with women (National Institute of Mental Health, 2012). Yet recent scholarship has indicated that men’s negative emotional experiences are often “invisible” because men actively conceal their vulnerabilities (Addis, 2011). Moreover, research over the past 15 years across health disciplines has reported that adult men in the United States engage in a wide variety of negative health behaviors that increase their risk for disease, injury, and death (e.g., Courtenay, 2000; Garfield, Isacco, & Rogers, 2008; Levant, Wimer, & Williams, 2011). Men’s lack of help seeking is considered to exacerbate the negative health behaviors and result in more physical and emotional concerns (e.g., Hammer, Vogel, & Heimerdinger-Edwards, 2013). Thus, there is growing awareness of men’s health concerns, the various barriers that they experience to their help seeking, and the importance of fostering positive help seeking attitudes and behaviors among men.
There are many groups of adult men in the United States; scholars have highlighted the need to examine help seeking more specifically based on context, developmental stage, and familial roles (Addis & Mahalik, 2003). In the United States, fathers are a group of 70.1 million men with familial roles and thus, may have varied experiences of mental health help seeking (United States Census Bureau, 2014). However, a thorough review of the extant literature indicated that there is a scarcity of research focused on fathers and mental health help seeking. Related research on recruiting fathers to parenting programs has reached similar conclusions as the broader men’s help-seeking literature, that is, fathers do not utilize parenting programs and experience barriers to their service utilization (e.g., Stahlschmidt, Threlfall, Seay, Lewis, & Kohl, 2013). Recent research has highlighted the importance of considering the mental health of men as they transit to fatherhood because fatherhood is associated with both positive and negative changes in psychological well-being (Garfield et al., 2014; Musser, Ahmed, Foli, & Coddington, 2013; Palkovitz, 2002; Pleck, 2012). In terms of potential negative consequences, fatherhood may increase stress and anxiety, relationship conflict, and depressive symptoms (Bronte-Tinkew, Moore, Matthews, & Carrano, 2007; Giallo, Treyvaud, Cooklin, & Wade, 2012). With this increased awareness of father’s mental health needs, more research regarding the mental health help-seeking behaviors of fathers is needed.
Scholarship has been devoted to providing guidance to mental health professionals on how to work with fathers more effectively (Oren & Oren, 2009). That scholarship has assumed that fathers have already sought and accessed mental health services. Two basic gaps in the current literature exist. First, there is limited descriptive data of fathers’ mental health help-seeking behaviors. Second, there are few empirical studies that have investigated the factors that influence mental health help seeking among fathers. The initial steps to developing interventions is to identify basic patterns of behavior and the factors that may affect the mental health help seeking of novel groups of men such as fathers (Hammer et al., 2013). A goal of this study is to specifically investigate fathers and their mental health help-seeking behavior, which may help develop more targeted interventions.
There is a large body of research that has reported that adult men in the United States spend less time with their doctor, schedule fewer doctor visits, and engage in fewer preventative health behaviors than women (Garfield et al., 2008; Levant et al., 2011). There are overlapping barriers between mental health and physical health help seeking for adult men such as masculine gender socialization, stigma, and health practitioners lacking in training to work effectively with men (Courtenay, 2011; Davies, Shen-Miller, & Isacco, 2010; Musser et al., 2013; O’Brien, Hunt, & Hart, 2005). Thus, mental health help seeking is conceptualized as a health behavior on par with getting a checkup from a physician (Courtenay, 2011; Mansfield, Addis, & Courtenay, 2005). As a result, it is hypothesized that a small percentage of fathers will seek mental health services, as research has reported that similar populations of men engage in fewer positive health behaviors (e.g., Courtenay, 2000; Garfield et al., 2008). A baseline investigation of mental health help seeking among fathers would benefit from identifying factors that affect these behaviors. Related research has reported that increased levels of anxiety, depression, and parental stress have been associated with a decrease in positive health behaviors in samples of men (Paulson, Dauber, & Leiferman, 2006). Thus, it is hypothesized that increases in anxiety, depression, and parental stress will be associated with less mental health help seeking.
Method
Participants and Procedures
The participants (N = 1,989) and data used in this study were obtained from the Fragile Families and Child Wellbeing Study, a national, longitudinal study of children and families born between 1998 and 2000. The Fragile Families and Child Wellbeing Study oversampled for unmarried parents from hospitals in approximately 20 large U.S. cities. Demographics were first gathered at the baseline interview in the hospital or over the telephone and added to as necessary in subsequent waves. The independent and dependent variables were gathered at the 3-year follow-up interview (i.e., when the focal child was approximately 3 years old). Participants’ demographics are reported in Table 1. Complete information about the Fragile Families study (Center for Research on Child Wellbeing, 2014) can be found at http://www.fragilefamilies.princeton.edu/
Participants’ Demographics.

Measures
Parenting Stress
Parenting stress was measured with four questions that assess the extent that the parent is feeling stress due to his role as a father. The questions were adopted from the Child Development Supplement of the Panel Study of Income Dynamics Study and the Parenting Stress Inventory–Short Form (Abidin, 1995). The Parenting Stress Inventory–Short Form is widely utilized to examine parenting stress. The Cronbach’s alpha for the Parenting Stress Inventory–Short Form has ranged between .80 and .87, with a test–retest reliability ranging between .68 and .87 (Abidin, 1995). In samples of mothers and fathers from the Fragile Families study, the Cronbach’s alpha from the four items ranged from .61 to .66 (Cooper, McLanahan, Meadows, Brooks-Gunn, & Johnson, 2009; Nomaguchi & Johnson, 2016). The four questions are the following: (a) Being a parent is harder than I thought it would be; (b) I feel trapped by my responsibilities as a parent; (c) I find that taking care of my child(ren) is much more work than pleasure; and (d) I often feel tired, worn out, or exhausted from raising a family. Responses were strongly disagree (4), disagree (3), agree (2), and strongly agree (1), and reversed scored, with higher scores indicating more parenting stress. Obtained scores ranged from 2 to 16; α = .61; M = 8.22, SD = 2.66.
Depression and Anxiety
Depression and anxiety were measured with the Composite International Diagnostic Interview–Short Form (CIDI-SF; Kessler, Andrews, Mroczek, Ustun, & Wittchen, 1998). The CIDI-SF questions were based on the Diagnostic and Statistical Manual of Mental Disorders–Fourth edition (DSM-IV-TR). The CIDI-SF has been utilized in several epidemiological, cross-cultural, and basic research studies and has been reported to have good psychometric properties (Bronte-Tinkew et al., 2007: Isacco, Garfield, & Rogers, 2010). For example, the test–retest analysis yielded an 86% agreement, kappa of .66, and interrater kappa was .97 on the depression scale and an 89% agreement, .69 kappa, and .96 interrater kappa on the anxiety scale (Wittchen, 1994).
To measure depression, fathers were asked about seven symptoms after endorsing stem questions. The four stem questions were the following: (a) During the past 12 months, has there ever been a time when you felt sad, blue, or depressed for 2 or more weeks in a row? (b) During that time, did the feelings of being sad, blue, or depressed usually last all day long, most of the day, about half of the day, or less than half the day? (c) During those 2 weeks, did you feel this way every day, almost every day, or less often? (d) During those 2 weeks, did you lose interest in most things like hobbies, work, or activities that usually give you pleasure? The seven symptom questions included losing interest, feeling tired, experiencing changes in weight, having trouble with sleep, having trouble concentrating, feeling down, and having thoughts about death. The raw scores are transformed into a probability of caseness for depression, with scores ranging from 0 to 1 (Kessler et al., 1998). In this study, depression scores ranged from 0 to 1; α = .95; M = 0.14, SD = 0.35.
To measure anxiety, fathers were asked about common symptoms of Generalized Anxiety Disorder after endorsing stem questions. The four stem questions were the following: (a) During the past 12 months, did you have a period lasting 1 month or longer when most of the time you felt worried, tense, or anxious? (b) Did you ever have a time in the past 12 months when you worried a lot more than most people would in your situation? (c) Is that period still going on? (d) How many months or years has it been going on? The common symptoms included questions regarding the time period, the strength, and amount of worries. Physical symptoms associated with the manifestation of anxiety were also assessed such as feeling restless, keyed up or on edge, easily tired, difficulty keeping your mind on what you were doing, more irritable than usual, tense, sore or aching muscles, and trouble falling asleep or staying asleep. The raw scores are transformed into a probability of caseness for anxiety, with scores ranging from 0 to 1 (Kessler et al., 1998). In this study, anxiety scores ranged from 0 to 1; α = .95; M = 0.03, SD = 0.18.
Mental Health Help Seeking
Mental health help seeking was measured with one item, asking, “Yes or No: In the past year, did you receive counseling for personal problems?”
Data Analysis
The data analysis plan used in this study consisted of two components. First, basic descriptive statistics were calculated for the percent of participants that sought mental health services (as measured on the one item), which would be used to test Hypothesis 1 (i.e., a small percentage of fathers will seek mental health services). Second, a logistic regression model was used to test Hypothesis 2 (i.e., increases in anxiety, depression, and parental stress will be associated with less mental health help seeking). A logistic regression model was used to test Hypothesis 2 because it is the appropriate statistical technique for a correlational design with multiple predictors (anxiety, depression, and parental stress) and one categorical/dichotomous, dependent variable (mental health help seeking as measured by a yes or no question; Leech, Barrett, & Morgan, 2015). Logistic regressions require large sample sizes for accuracy (minimum of 60 total cases; 20 per predictor), which fits with the sample size of this study (N = 1,989; Leech et al., 2015). Household income was entered as a control variable because it is a sociodemographic characteristic relevant to this population of fathers in “fragile families” and finances can be a confounding factor in help-seeking behaviors (Chen et al., 2013; Kotila & Kamp Dush, 2012).
Results
Hypothesis 1, positing that a small percentage of fathers will seek mental health services, was supported as 3.2% (64) of participants reported seeking therapy or counseling for personal problems. Hypothesis 2, stating that increases in anxiety, depression, and parental stress will be associated with less mental health help seeking, was partially supported. Given that the dependent variable was dichotomous, a logistic regression model was conducted to assess Hypothesis 2 (Leech et al., 2015). Logistic regressions have very few assumptions; however, similar to multiple regressions, multicollinearity (high correlations between predictors) needs to be tested (Leech et al., 2015). A preliminary analysis of multicollinearity was conducted with bivariate correlations between the predictors. Parenting stress and anxiety were significantly related (r = .05; p < .05); parenting stress and depression were significantly related (r = .13; p < .01); depression and anxiety were significantly related (r = .29; p < .01). The correlations were not elevated to a level that would suggest multicollinearity (.50-.60 or above); thus, the predictor variables were considered to be independent of each other in the logistic regression (Leech et al., 2015).
When all three variables are considered together, and household income is used as a control variable, the model significantly predicted fathers’ mental health help seeking, χ2 = 75.42, df = 4, N = 1,989, p < .000. As seen in Table 2, which presents the odds ratios, depression was the only significant factor, indicating that the odds of fathers seeking mental health services decrease as depression scores increase.
Logistic Regression of Factors Associated With Fathers’ Mental Health Help Seeking.
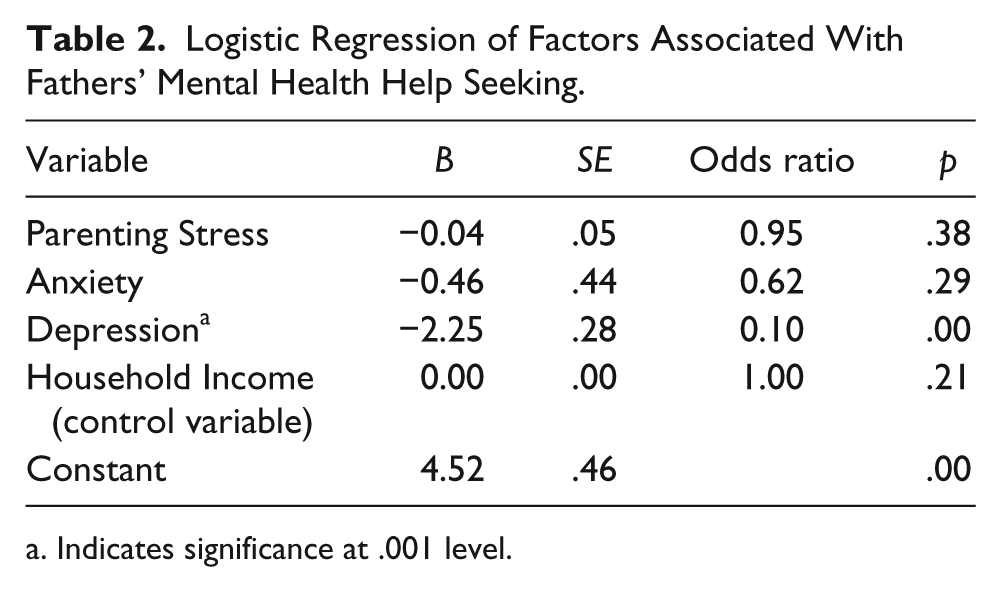
Indicates significance at .001 level.
Discussion
First, this study filled a gap in the extant research by providing baseline descriptive data of fathers’ self-reports of mental health help seeking. Only 3.2% of 1,989 participants in this sample sought mental health services, which confirmed our hypothesis. Fathers’ lack of mental health help seeking contributes new information to the extant literature on men’s help seeking by reporting baseline data on an adult group of men with diverse familial roles and contexts. Although there is scarce data on fathers’ mental health help-seeking behaviors, our data are congruent with research that has reported that urban, racial minority, and middle to low SES fathers have low rates of participation in parenting programs (Stahlschmidt et al., 2013). Taken together, the low percentage of fathers seeking mental health and parenting support services continues to be concerning for health practitioners and researchers aiming to improve the health and well-being of fathers and their families.
Since the research continues to report low rates of service utilization among fathers, identification of barriers and facilitating factors has been an important area of exploration. This study hypothesized that increases in depression, anxiety, and parenting stress would be associated with decreases in mental health help seeking. Anxiety and parenting stress were nonsignificant factors in the logistic regression model. Yet as hypothesized, this study identified that as depressive symptoms increased, mental health help seeking decreased. This inverse relationship, which seems counterintuitive, may be explained a few different ways. First, the actual symptoms of depression such as fatigue, loss of energy, a diminished ability to think and concentrate, and indecisiveness may inhibit active mental health help seeking (American Psychiatric Association, 2013). Depressed fathers may withdraw from known supports such as mental health counselors despite the efficacy of many psychotherapies to treat depression among adult men (Cochran, 2005). Given the correlational design of this study, another possible interpretation is to switch the variables and interpret the data: as fathers’ mental health help seeking decreases, depressive symptoms increase. In other words, underutilizing mental health services may exacerbate the depressive symptoms among fathers. Such an interpretation fits with the conceptualization that men’s health-related problems worsen by not accessing the proper services (e.g., Hammer et al., 2013; O’Brien et al., 2005). Finally, we conceptualized mental health help seeking as similar to physical health help seeking. Our finding fits with previous research indicating that depression has an adverse effect on men’s health behaviors, as well as research that has reported that depression and negative health behaviors co-occur in community samples of adults (Paulson et al., 2006; Verger, Lions, & Ventelou, 2009). Thus, it makes sense that depressed fathers in this study are not engaging in the positive health behavior of mental health help seeking.
Limitations and Future Directions of Research
This study examined a large sample of fathers (N = 1,989) in a baseline, primarily exploratory analysis. Thus, the analysis did not include any potential mediators (e.g., stigma) or moderators (e.g., marital status), which future research could explore. The findings from this study are most applicable to African American and White fathers in their late 20s/early 30s, residing in an urban location, and of middle to low socioeconomic status. Generalizing the findings to other groups of fathers is limited and cautioned at this time. This study sought to obtain baseline data about fathers’ mental health help seeking; thus, longitudinal data about fathers’ help-seeking patterns and factors that affect those patterns over time was not obtained. A longitudinal analysis represents an important area of future research. The sample was not separated into various subgroups for group-level analysis of mental health help seeking. Following current research that has examined help seeking among men in various groups based on community, education, and income (Hammer et al., 2013), the next step in this research is to examine the mental health help seeking among different groups of fathers. It is certainly plausible that fathers’ mental health help seeking will vary according to marital status, residential status, race/ethnicity, geographic location, and other salient sociodemographic variables (Doyle, Joe, & Caldwell, 2012; Gordon et al., 2013). In addition to sociodemographic variables, this study did not include a measure of masculinity ideology in the analysis. Masculinity ideology has been reported to be a significant variable in studies of men’s help seeking, including young fathers (Kellom & Hammel, 2013). Thus, future research using correlational designs (e.g., regression models, path analysis) would likely benefit by including masculinity ideology in the analysis of fathers’ mental health help seeking.
In conclusion, the transition to fatherhood can be stressful for men, contributing to depression and other negative health behaviors (Garfield et al., 2014; Garfield, Isacco, & Bartlo, 2010). This brief report highlights that few fathers seek mental health services and the adverse effect that depression plays in paternal mental health help seeking. Future research needs to explore how fathers, families, and practitioners can work together to overcome barriers and to create new pathways that facilitate positive help seeking among fathers.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
