Abstract
The current study aims to explor how men would advise other men about seeking help for lower bowel symptoms and also to determine the factors that may influence help seeking. A purposive sample of Western Australian men aged 18 years and older was recruited for the study. Participants completed 8 of the 28 randomly assigned video vignettes (video clips) displaying men (older or younger) with various combinations of one or more lower bowel symptoms. Participants were asked if the person in the vignette should seek health advice. Subsequently, the participants answered a set of questions based on the Health Belief Model. A total of 408 participants (response rate = 51%) answered 3,264 vignettes. Participants younger than 50 years, participants who were not tertiary educated and those who had lower incomes, or those living in regional or remote areas were less likely to advise help seeking from general practitioner (GP). Participants who visited their general practitioner less frequently were also less likely to advisehelp seeking. There was a trend to consider unintentional weight loss and diarrhea as minor symptoms not necessitating medical attention compared with rectal bleeding. The findings suggest for a need to improve public awareness among men about the need to seek timely medical advice for lower bowel symptoms in primary care. The importance of early presentation of persistent lower bowel symptoms must be specifically targeted at men younger than 50 years, those with lower incomes, or residing in regional or remote areas.
Keywords
Introduction
Colorectal cancer (CRC) is the third most common cancer in men with more than half the cases occurring in developed countries (Ferlay et al., 2013). Australia and New Zealand together account for the highest incidence of CRC in the world with age-standardized incidence rate of 44.8 per 100,000 men (Ferlay et al., 2013). CRC is often symptomatic and has a high potential for curative treatment when detected at an early stage (Lindholm, Brevinge, & Haglind, 2008). In contrast, late stage presentation is associated with a poor 5-year survival (McArdle & Hole, 2004). Although factors related to both patient delay and the health care system delay have been reported to be associated with diagnostic delays in CRC, patient delay accounts for the longest time delay (Langenbach, Johannes Schmidt, Neumann, & Hubert Zirngibl, 2003). The majority of CRC patients experience lower bowel symptoms such as rectal bleeding, change in bowel habit, abdominal pain, and weight loss (D. Smith et al., 2006); however, the rate of seeking medical advice for such symptoms is low (Chaplin, Curless, Thomson, & Barton, 2000; Hamilton & Sharp, 2004; Thompson, Pond, Ellis, Beach, & Thompson, 2000). These symptoms also occur in benign bowel diseases, are also common in the general population and are often self-limiting (Adelstein, Macaskill, Chan, Katelaris, & Irwig, 2011; Courtney et al., 2012b).
In their study on Australian population (n = 1,332), Cockburn, Paul, Tzelepis, McElduff, and Byles (2003) reported that although nearly 70% of adults were aware of rectal bleeding as a sign of CRC, less than half knew about the other potential symptoms of cancer. In the same study nearly 1 in 4 individuals were unaware of at least one symptom of CRC. The authors also identified that the awareness of these symptoms alone did not ensure timely help seeking among the participants. Similar views were echoed by Hashim et al. (2011) who found no association between the knowledge of cancer symptoms and delay in presentation of rectal bleeding and also highlighted the gap between knowledge and help-seeking behavior in Malaysian population. A recent Danish study by Pedersen, Hansen, and Vedsted (2013) reported that CRC patients with rectal bleeding experienced longer delays in seeking medical advice than patients without rectal bleeding when adjusting for other symptoms such as change in bowel habit or abdominal pain. The authors also suggested that the attribution of symptoms to benign causes was not the only reason for patient delay, and emphasized on the need to identify the barriers to help seeking. In another study on Australian adults (n = 1,592), Courtney et al. (2012a) reported that up to 18% of people experiencing rectal bleeding had never consulted a doctor and nearly the same proportion delayed for more than 1 month before seeking medical advice. Up to 20% of people who experienced a change in bowel habit had never sought medical advice and 37% delayed for more than 1 month before seeking advice.
No major improvement in the consultation rates for lower bowel symptoms have been reported over the past two decades (Cockburn et al., 2003; Crosland & Jones, 1995; Thompson et al., 2000). The issue is rather more important in an Australian context where the estimated rates for CRC are reportedly the highest in the world (Ferlay et al., 2013). Adelstein, Macaskill, Turner, and Irwig (2012) observed that patients, who considered their symptoms as less serious, had a threefold higher prevalence of cancer than those who considered their symptoms as serious. Qualitative studies focusing on Australian men have reported that the rationalization of the lower bowel symptoms or self-medication was a common practice among men and prevented them from seeking medical advice. The fear of diagnosis and the cost of consulting a general practitioner (GP) were other barriers to help seeking (Oberoi, Jiwa, McManus, & Hodder, 2015b). Although majority of GPs in Australia (nearly 83%) bulk bill their patients (i.e., the GPs accept Medicare rebate as full fee for their consultation), the patients may have to bear significant out-of-pocket costs (nearly AUD30 for a GP consultation and more than AUD200 for a specialist consultation) if they consult non–bulk billing doctor (Department of Health and Ageing, 2013). Furthermore, it is speculated that the proposed copayment fee to be paid by Australians for each GP visit as well as for diagnostic investigations and the proposed increased copayments for prescription medications in future is further likely to discourage people from seeking timely medical advice (Kirby, 2014). Past studies have also reported that support from female family members played a vital role in encouraging men to seek help (Oberoi, Jiwa, McManus, & Hodder, 2015a, 2015b).
To facilitate timely help seeking among men, it is important to understand the factors that affect their decision to seek help. The current understanding of the medical advice–seeking behavior for lower bowel symptoms is largely based on retrospective studies highlighting retrospective recall of symptoms and time intervals from symptom onset to help seeking (Basaranoglu et al., 2008; Chaplin et al., 2000; Cockburn et al., 2003; Macleod, Mitchell, Burgess, Macdonald, & Ramirez, 2009). In their literature review, Oberoi, Jiwa, McManus, and Hodder (2014) discussed various behavioral factors associated with delay in seeking medical advice for lower bowel symptoms. Such information may be subject to memory-recall bias as it may be difficult to remember the exact timing of vague and nonspecific symptoms and the health actions taken in response to the symptoms (Cockburn et al., 2003; Korsgaard, Pedersen, Sørensen, & Laurberg, 2006).
The current study aimed at exploring the factors that may affect men’s help-seeking decisions with regard to the symptoms of CRC through the use of standardized vignettes. Vignettes (hypothetical patient scenarios) may be useful in eliciting information about the questions that may be personally intimidating, or about the information that may be either underreported or distorted in a socially desirable direction (Barter & Renold, 2000; Brener, Billy, & Grady, 2003; Wallander, 2009). Another advantage is that the vignettes can reflect real-life scenarios, while controlling for external or potentially confounding variables. Vignettes are also reported to control for the contextual variations between the vignette characters (Kinicki, Hom, Trost, & Wade, 1995; Ramanathan, Baratiny, Stocks, Searles, & Redford, 2011), thereby allowing all the participants to respond to similar stimuli. The advantages of using the vignettes in social research have been summarized by Hughes and Huby (2002).
Method
Theoretical Framework
The health belief model (HBM) has been used as the theoretical framework in this study. The HBM purports that people’s decision to commit to a recommended health action (to seek medical advice) is associated with their perception of the severity of symptoms, susceptibility to the disease, the perceived benefits of the action, the absence of barriers to the action and confidence in the GP or family physician (Strecher & Rosenstock, 1997). The model also proposes that demographic variables (i.e., age, sex, or ethnicity), sociopsychological variables (i.e., personality or social class) and structural variables (i.e., knowledge about the disease or personal experience with a condition) may indirectly influence health-related behaviors by affecting an individual’s perception of susceptibility, severity, benefits, and barriers (Pinto, Lively, Siganga, Holiday-Goodman, & Kamm, 2006; Rosenstock, Strecher, & Becker, 1994). As the HBM was originally developed to explain preventive behaviors it is a suitable model for the current research (Shaw, Brittain, Tansey, & Williams, 2008).
Study Population
In this vignette-based study, participants were recruited from the general population in the state of Western Australia through a research recruitment agency and data were collected between August and October 2012. The potential participants were approached by the recruitment agency and those willing to participate were included in the study. Men aged 18 years or older who were able to communicate in English, had access to the Internet, and were willing to complete a self-administered online questionnaire were eligible. Although, the average age at diagnosis of CRC in Australia is around 69.3 years, approximately 6% of patients diagnosed with CRC in Australia are below 50 years of age (Bowel Cancer Australia, 2013; Wu et al., 2012). The sample was selected in a purposive manner so as to closely resemble the Western Australian population with regard to age, income, educational and employment status, relationship status, and country of birth (consistent with Census Western Australia, 2011). The participants were able to give informed consent before participating in the survey.
We focused exclusively on male participants, because men are not only observed to have a higher biological risk and prevalence of CRC compared with women, but are somewhat more likely to delay seeking medical advice for primary symptoms of CRC (Bray, Ren, Masuyer, & Ferlay, 2013; McArdle, McMillan, & Hole, 2003; McCashland, Brand, Lyden, & de Garmo, 2001; Oberoi et al., 2014; Wichmann, Müller, Hornung, Lau-Werner, & Schildberg, 2001).
Based on the number of explanatory variables (n = 20), and to achieve a power of 80% to detect variables exhibiting a moderate effect size, with α = .05, a minimum sample size of 156 participants was required (Green, 1991). The explanatory variables were clinical variables presented in the vignettes (Appendix A), the demographic variables (Appendix C, Section 1a) and the five domains of the HBM (Appendix C, Sections 1b and 2). In consistency with the HBM, which was used as a theoretical framework, demographic variables such as age, income, educational and employment status, relationship status, country of birth and/or duration of stay in Australia, inhabitance (metropolitan or regional/remote areas), and private health insurance were used as covariates.
Materials and Procedure
The Curtin University Human Research Ethics Committee (Approval No.: PH-02-12) approved the study. Informed consent was obtained from the participants.
Survey
Twenty-eight video vignettes (hypothetical scenarios) were developed. The content of the vignettes was informed by the NICE guidelines (National Institute of Health and Care Excellence, 2005) for symptoms indicating high risk for CRC and the clinical and population-based studies (Courtney et al., 2012a; Hashim et al., 2010; Lynch et al., 2008; McMinn, Steel, & Bowman, 2011; Philipp, Wood, Heaton, & Hughes, 1993; Stapley, Peters, Sharp, & Hamilton, 2006). CRC is assumed to be primarily a disease of the elderly and the incidence is higher in individuals aged more than 50 years. The average age at diagnosis of CRC in Australia in 2009 was 69.3 years. However, approximately 6% of patients diagnosed with CRC in Australia are younger than 50 years (Bowel Cancer Australia, 2013; Wu et al., 2012). Therefore, age was used as one of the clinical variables for the vignettes and vignettes were created using both older and younger men. The five binary clinical variables describing each vignette are shown in Appendix A. Each scenario was presented as a short story and styled in the manner shown in the examples in Appendix B. The vignettes were developed using professional actors and the consent to publish the videos was obtained.
The video vignettes were preferred in this study over text-vignettes as video vignettes remove sources of bias not addressed in other survey methods. Various clinical symptoms and psychosocial variables can be presented more realistically in the video vignettes, which may ignite the participant’s own emotions, memories, attitudes, and biases that may influence their responses (Hawley, Adams, & Galbraith, 2010).
Each participant answered a set of demographic questions before proceeding to the vignettes. Based on the scenario played in the vignettes, the participants were asked whether the man in the vignette should seek professional health advice, which health professional should he seek advice from, and how urgently should he seek advice.
As a next step, the participants were asked a set of questions related to clinical scenario presented in the video-vignettes and based on five themes of the HBM: severity of the symptoms (two items), susceptibility to the symptoms (one item), benefits of seeking advice (two items), barriers to seek advice (one item), and confidence (one item). The respondents were asked to assess their level of agreement with each of the statements relating to these themes on a 5-point Likert-type scale (strongly agree to strongly disagree). These questions were informed by literature review of questionnaires previously used in studies with a direct application HBM-based questionnaire on CRC and lower bowel symptoms (Jacobs, 2002; Macrae, Hill, St John, Ambikapathy, & Garner, 1984; Ozsoy, Ardahan, & Özmen, 2007; Rawl et al., 2001). The questionnaire was tested for reliability and validity. The survey was administered to the participants via web-based software (https://www.qualtrics.com/). Eight randomly selected vignettes were presented to each participant. However, considering that some men in the vignettes would need to seek advice for their symptoms from a GP for diagnosis and referral, the survey was also administered to an expert panel comprising five GPs. The expert panel was invited to identify the cases that would need to seek help from GP and the participants’ responses were matched against the recommendations of the expert panel. The complete questionnaire is reported in Appendix C.
Reliability
The test–retest reliability of the HBM questionnaire ranged between .88 and .98 indicating a highly reliable questionnaire. Cronbach’s alphas for the Severity questions and Benefits questions were .93 and .91, respectively. This shows very high consistency for the pairs of questions used in each of these domains.
Construct Validity
Factor analysis of the HBM responses (after converting the Likert-type scale responses to the numbers 1-5) indicated that a single factor was responsible for 74.1% of the variance in the data. This factor involved all the five domains used in the questionnaire, with four of them (Severity, Susceptible, Confidence, and Benefits) having approximately equal weight, and the weight of the Barrier domain being approximately half (and in a negative direction compared with the others). The factor loadings for the data set were found to be 0.941 (Severity), 0.936 (Susceptible), 0.934 (Confidence), 0.918 (Benefits), and −0.480 (Barriers). This analysis confirms that all domains were relevant and important in explaining the variance in the data set.
Statistical Analysis
A general estimating equation (GEE) was used to identify the relative importance of the HBM, the symptom profile portrayed in the vignette and the demographic profile of the participant in regard to the participants’ decision for vignette referral to seek medical attention. The GEE regression model was used because it took into account the correlation in the data because of the multiple responses made by each participant (eight vignettes per person). Three different GEE models were developed with three dependent variables, respectively: the odds of recommending a help seeking, the odds of recommending help seeking from a GP, and the odds of the participants’ responses agreeing with expert panel comprising five GPs. Observations for the last outcome included those in which the expert panel decided that the men portrayed in the vignettes should seek medical advice for their symptoms. Furthermore, a single HBM score was calculated for each of the participants’ vignette responses based on the factor loadings (a weighted sum of the five responses using the factor loadings as weights). The purpose of the factor analysis was to obtain a single summary score obtained from the linear combination of the HBM questions that could be used in the subsequent regression analyses. To avoid the assumption of a linear relationship between the score and the odds of each outcome, the score for each person was categorized into one of four groups based on the quartiles of the score distribution (scores: 10, 15, 17). The grouped score variable was then introduced into the models as a categorical variable, with the highest quartile group (the most likely to seek advice) used as reference.
Statistical analyses were performed using the SPSS Version 20 and SAS Version 9.2 statistical software programs. A p value < .05 indicates a statistically significant association in all tests.
Results
In the final survey, 408/800 participants recruited to the study met the inclusion criteria and completed the study (response rate = 54.8%). Each participant answered Section 1 of the questionnaire (only once) followed by Section 2 (eight times) based on the eight video vignettes. A total of 3,259 (408 × 8 = 3,264) complete responses to the video vignettes were received (5 responses were incomplete or missing). The demographic profile of the study participants is reported in Table 1. Compared with the Western Australian census data, the survey sample was reasonably representative in terms of age, marital status, country of birth, highest level of education, and occupation.
Demographic Profile of the Study Participants (N = 408).

Results of the GEE Models
The proportion of the participants seeking advice from GP for vignettes featuring older men with symptom duration of 3 weeks ranged between 42% and 78% across all vignettes while for vignettes featuring younger men with similar symptom duration ranges between 26% and 84% across all vignettes with different symptom combinations (Appendix D). Additionally, a disagreement was observed between the participants and the expert panel (comprising five GPs) with respect to referring the vignettes to seek help. Nearly 50% of the participants did not agree with the expert panel with respect to seeking medical advice for rectal bleeding lasting for 3 weeks.
Outcome 1: Vignettes Recommended for Help Seeking
Of the 3,259 completed vignette assessments, 2,076 (63.7%) were recommended to seek advice. The odds of recommending the vignettes for help seeking were lower if the participants resided in regional or remote areas as opposed to metropolitan areas (odds ratio [OR] = 0.44, 95% confidence interval [CI] = 0.23-0.83; p < .002) or if their annual income was ≤AUD50,000 (OR = 0.30, 95% CI = 0.18-0.5; p < .0001). The odds of seeking help were also directly related to the participants’ HBM score and their own frequency of GP visits. Those who never visited the GP themselves were 72% less likely to advise men in the vignettes to seek help compared with those who visited their GPs several times in a year (OR = 0.28, 95% CI = 0.15-0.54; p < .0001). Those with HBM score ≥15 were nearly 1,000 times more likely to advise help seeking than those with HBM scores <10 (OR = 0.001, 95% CI = 0.0003-0.002; p < .0001). With regard to the clinical factors, the odds of help seeking increased with the increasing number and duration of the symptoms. Table 2 reports the results of fitting a GEE model to these data and gives the ORs for seeking advice along with 95% CIs and p values.
Relative Odds of Men From Vignette Being Referred to Seek Help.

Note. OR = odds ratio; CI = confidence interval. The “n/N” column shows the number of vignette responses seeking advice out of the total number of vignette responses in that category of the independent variable. ORs, CIs, and p values were obtained from a general estimating equation model, which takes into account correlations between responses from the same participant. The analysis is based on 3,259 records (all data). Odds ratios greater than 1 indicated a higher likelihood of seeking advice, whereas odds ratios less than 1 indicated a lower likelihood of doing so.
Outcome 2: Vignettes Recommended for Help Seeking From GP
Of the 2,076 vignettes in which the participants recommended seeking health advice, only 1,517 (73%) were recommended to seek advice from a GP as opposed to other health professionals such as a pharmacist or a nurse practitioner. The odds of recommending help seeking from a GP were higher in participants aged ≥ 50 years than those aged < 50 years (OR = 1.65, 95% CI = 1.07-2.54; p = .023). The odds were also lower for participants who studied up to Year 12 compared with those who had received tertiary education (OR = 0.31, 95% CI = 0.20-0.5; p < .0001). Participants who earned between AUD20,000 and AUD50,000 annually were much less likely to recommend than those who earned >AUD50,000 (OR = 0.13, 95% CI = 0.07-0.22; p < .0001).
Men who believed that visiting a GP was time consuming were 61% less likely to recommend help seeking from GP (OR = 0.39; 95% CI = 0.26-0.59; p < .0001). Additionally, those who had HBM scores <10 were half as likely as those with scores ≥15 to recommend help-seeking advice from GP. With regard to the clinical factors presented in the vignettes, the odds of consulting a GP increased with the increase in the number and the duration of the symptoms. For lone symptoms, the odds were higher for rectal bleeding than for weight loss and diarrhea. Table 3 reports the results of the final GEE model for this outcome.
Relative Odds of Men From Vignette Being Referred to Seek Help From a General Practitioner.
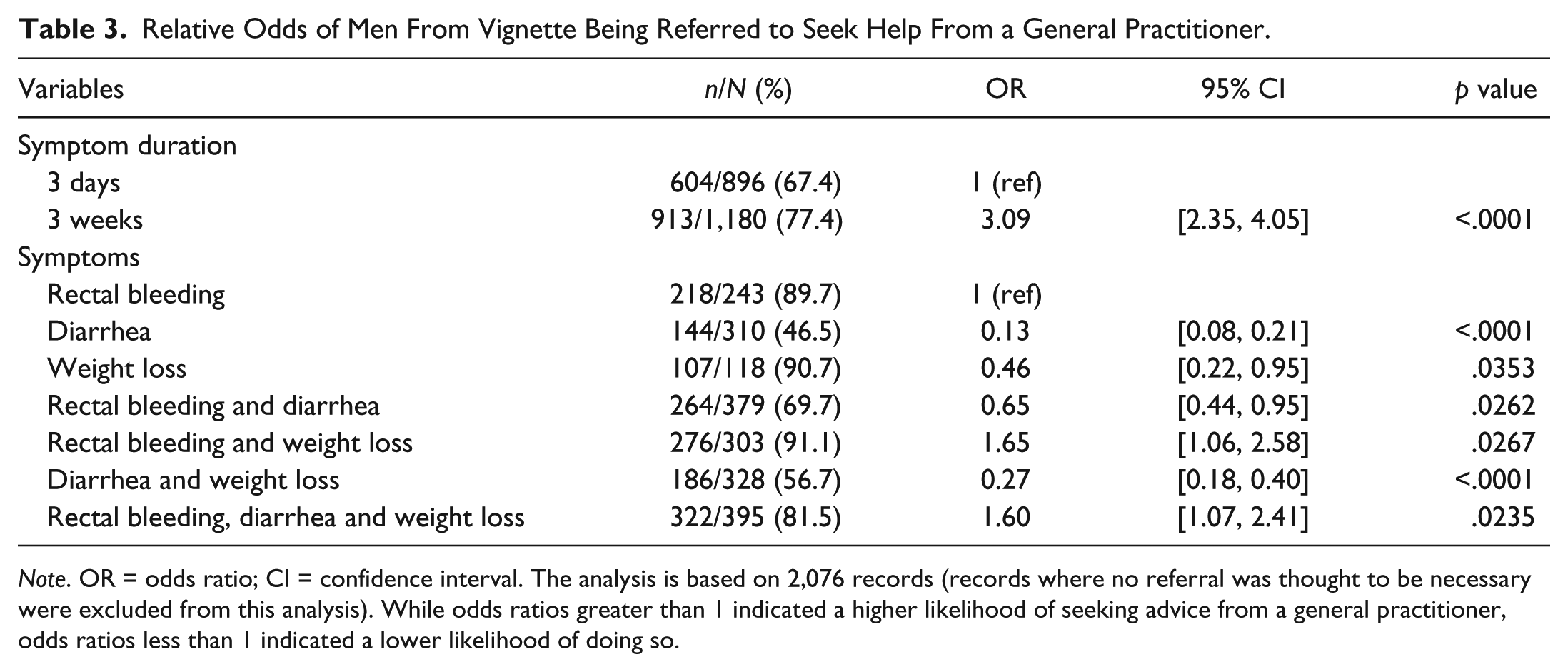
Note. OR = odds ratio; CI = confidence interval. The analysis is based on 2,076 records (records where no referral was thought to be necessary were excluded from this analysis). While odds ratios greater than 1 indicated a higher likelihood of seeking advice from a general practitioner, odds ratios less than 1 indicated a lower likelihood of doing so.
Outcome 3: Vignette Agreement With the Expert Panel
Vignettes appropriately identified as warranting medical attention were defined as participants’ referral of a vignette for seeking advice that matched the opinion of the expert panel in terms of whether a GP should be consulted. Only vignettes that were considered by the expert panel to require referral to a GP were included in this analysis.
Participants aged ≥50 years were more nearly twice as likely to agree with the expert panel in terms of advising the men in the vignettes to seek advice from the GP compared with those aged <50 years (OR = 1.88, 95% CI = 1.23-2.87; p < .003). The participants who lived in regional or remote areas as opposed to metropolitan areas (OR = 0.43, 95% CI = 0.26-0.72; p < .001) and those who were studied up to Year 10 as opposed to those who had received tertiary education (OR = 0.43, 95% CI = 0.25-0.75; p < .002). Participants with higher incomes were also more likely to agree with the expert panel. Participants who visited their GPs at least once a month were nearly 16 times more likely to agree than those who never visited their GP (OR = 15.9, 95% CI = 2.71-93.81; p < .002) and those who believed that visiting a GP was time consuming were 60% less likely to agree (OR = 0.4, 95% CI = 0.26-0.60; p < .0001).
Participants who had lower HBM scores, visited their GPs less frequently, or believed that visiting a GP was time consuming had lower odds of agreeing with the experts. With regard to the clinical symptoms, the odds of agreement were higher for rectal bleeding as opposed to other symptoms and were also higher when all the three symptoms occurred concurrently or lasted for 3 weeks. The results of the final GEE model for this outcome are reported in Table 4.
Relative Odds of the Participants Agreeing With Expert Panel on the Need for Help Seeking From a General Practitioner.

Note. OR = odds ratio; CI = confidence interval. The analysis is based on 1,643 records (videos where the experts considered that referral to a general practitioner were not necessary are excluded from this analysis). Odds ratios greater than 1 indicated a higher likelihood of seeking advice from a general practitioner.
Discussion and Conclusion
Discussion
In the current study, the HBM score (a score based on five domains of the HBM, i.e., severity of the symptoms, susceptibility to major bowel pathology, benefits of and barriers to seeking medical advice, and the participants’ confidence in their GP to help with their symptoms)—was strongly associated with the odds of the participants recommending help seeking. In general, a high overall HBM score was associated with higher odds to seek advice thus highlighting the role of health beliefs in regard to seeking advice for lower bowel symptoms. These findings were consistent with previous studies that used the HBM as a theoretical framework (Jacobs, 2002; Ozsoy et al., 2007; Ueland, Hornung, & Greenwald, 2006). The role of health belief factors such as the severity of symptoms and confidence in the recommended health action in response to the symptoms have also been recently supported by the findings of Esteva et al. (2013).
The odds of vignette referral were also strongly associated with participants’ own pattern of GP visits and were much lower for participants who visited their GPs less frequently. Finding time to visit a GP and the monetary costs associated with consultation were other barriers to refer the vignettes for seeking help. Furthermore, the odds of referral of vignettes to GP were lower for participants who believed that visiting a GP was time consuming or expensive. The participants with lower household incomes and those with lower educational qualifications (educated up to or less than high school vs. tertiary educated) had lower odds of seeking medical advice. These variables have been independently shown to play a favorable role in men’s help-seeking behavior in previous studies, which suggests that health care cost could be an important factor in determining the use of health care services in patients requiring medical attention (McCaffery, Wardle, & Waller, 2003).
Among other demographic factors, the participants who resided in regional or remote areas were less likely to refer compared with those in metro areas. Factors such as availability and access to health services and the service cost are important in determining health care utilization (Corboy, McDonald, & McLaren, 2011). These factors are relevant particularly for Australian men living in regional and remote areas characterized by limited access to health services due to geographic isolation, poor transport links, and shortage of health care providers (Australian Institute of Health and Welfare, 2005). Previous studies report that increased awareness of symptoms and the risk of disease through mass media or through lay support networks is known to trigger help seeking, whereas lack of awareness of symptoms or of treatment act as barriers to help seeking (Smith, Pope, & Botha, 2005).
In this study, a disagreement was observed between the participants and the expert panel (comprising five GPs) with respect to referring the vignettes to seek help. Nearly 50% of the participants did not agree with the expert panel with respect to seeking medical advice for rectal bleeding lasting for 3 weeks. This finding is consistent with previous studies reporting low rate of help seeking for rectal bleeding (Chaplin et al., 2000; Cockburn et al., 2003; Courtney et al., 2012a; Esteva et al., 2013; Kocher & Saunders, 1999). Nearly one third of the participants disagreed with the expert panel on seeking medical advice for symptoms of unintentional weight loss or change in bowel habit occurring concurrently with rectal bleeding and lasting for 3 weeks. This may be a cause for concern as persistent rectal bleeding (particularly in the absence of peri-anal symptoms) may be indicative of significant bowel pathology and warrants medical attention (Ellis & Thompson, 2005). Nearly a quarter of the participants disagreed with the expert panel for vignettes comprising all the three symptoms—rectal bleeding, diarrhea, and weight loss—lasting for 3 weeks. The age of the men in the vignettes had no impact on the level of agreement as the respondents had similar advice for both younger and older men. This is again a cause for concern as these symptoms are known to increase the risk of bowel cancer particularly in the elderly (Adelstein et al., 2011; Bekkink et al., 2009; Bhargava, Aldameh, Stewart, & Hill, 2007). A number of participants sought health advice for symptoms and symptom combinations presented in the vignettes (rectal bleeding, diarrhea, and unintentional weight loss) from health professionals other than a GP such as pharmacists and nurse practitioners. This suggests that other health professionals especially community pharmacists could play a vital role in educating men about the risks of CRC based on their symptoms and subsequently advise them to seek medical advice from their GP (Sriram, McManus, Emmerton, Parsons, & Jiwa, 2014).
Strengths and Limitations
The use of video vignettes, instead of typical opinion surveys is a major strength of this study. The behaviors that have a social stigma attached to them or are personally threatening, may be either underreported or distorted in a socially desirable direction (Brener et al., 2003). The vignettes are thus, appropriate for studying the actual determinants of human judgments with more valid and reliable measures of the participants’ responses compared with typical opinion surveys (Wallander, 2009) as the questions may be personally less intimidating and therefore less susceptible to social desirability bias (Alexander & Becker, 1978; Finch, 1987). The use of video vignettes as a method of data collection is well established (Hawley et al., 2010). The various clinical symptoms and other variables, such as patients’ emotions, their body language and appearance cues, and social and psychological information, embedded in the vignettes can be presented more effectively in the video format than in the text vignettes, which may ignite the respondent’s own emotions, memories, attitudes, and biases that may influence their responses (Hawley et al., 2010).
Past studies (Chaplin et al., 2000; Cockburn et al., 2003; Crosland & Jones, 1995; Langenbach et al., 2003; Talley & Jones, 1998) have explored the help-seeking behavior in people who had experienced lower bowel symptoms, such as rectal bleeding and change in bowel habit, in the past. In one of the recent studies, Courtney et al. (2012b) highlighted the factors associated with early medical advice seeking behavior for potential symptoms of CRC. However, the time interval since exposure to the symptoms is known to affect the recall of exposures (Cockburn et al., 2003). The current study is designed to understand the help-seeking behavior of people in the general population regardless of symptoms, thereby minimizing the risk of recall bias and gaining better understanding of their help-seeking behavior.
As the sample was nonrandom, the findings may have limited generalizability. A nonrandom sample and the survey’s application in other settings will further validate the survey and will also increase confidence in the generalizability of the results.
Furthermore, the HSB questionnaire used in the survey did not include a subscale to measure “cues to action,” another domain of the HBM. The development and testing of the items for “cues to action” and additional items for each construct of the HBM scale may further increase the amount of common variance and further explain men’s help-seeking behavior as would a revision to the wording and scoring of the existing items. It may also help in future studies to include additional symptoms such as constipation or abdominal pain in the vignettes that were excluded in this study.
In this study, participants’ knowledge of the symptoms relating to CRC was not measured directly. Hence, it would be difficult to suggest if men’s underestimation of the symptoms severity that warranted medical attention was related to their suboptimal help-seeking behavior and if the programs leading to increase in men’s knowledge about the symptoms would lead to help seeking. It may be helpful in future research to study men’s knowledge about the potential causes for the symptoms presented in the vignettes and its correlation with their help-seeking behavior. It would also be interesting to conduct a similar survey among women in order to explore gender differences.
Another limitation is that the current study did not control for men’s recent receipt of a CRC investigation or diagnosis. Another limitation of the study is that only men who had access to Internet and a computer (desktop, laptop, or tablet) were able to answer the survey. It remains to be seen if the population of men with no Internet access would respond to the vignettes in a similar or different manner. Lastly, in regards to CRC risk stratification the authors in this study did not develop individual models for different age groups. Future studies may undertake models for individuals in lower risk (age groups ≤ 50 and > 50 years).
Conclusion
This study provides insight into the influence of the demographic and clinical characteristics and the personal health beliefs on the intention to seek timely advice from a health professional about lower bowel symptoms. The findings report that a considerable proportion of men would not advise other men even with significant lower bowel symptoms to seek help from GP. The HBM was an applicable model to study men’s help-seeking behavior and the HBM score, a measurement of men’s health beliefs regarding the symptoms, was directly related with the odds of seeking help.
Practical Implications
The study explores the factors affecting men’s decision to seek timely medical advice for symptoms that may mimic CRC orcolorectal pathology. The knowledge of these factors may be considered in developing interventions aimed at encouraging timely medical advice seeking for lower bowel symptoms and facilitating early diagnosis among men. It may be possible to encourage men to seek timely medical advice if public health messages on the importance of early presentation of persistent lower bowel symptoms are targeted at men with lower incomes or residing in regional or remote areas. As men younger than 50 years were less likely to seek health advice, such men should be targeted more specifically in public health campaigns.
Footnotes
Appendix A
Appendix B
Appendix C
Appendix D
Acknowledgements
We would like to thank Prof. Jeff Hughes, Curtin University for his suggestions in the design of the study and for proof reading the article.
Authors’ Note
This article was presented at the Cancer and Primary Care Research international Network Conference, 2014, Winnipeg, Canada and the abstract from the conference was published in the supplementary issue of the European Journal of Cancer Care. The funding body had no role in the data collection or report writing.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded through an internal grant from Curtin University.
