Abstract
Gay men may not be physically active at recommended levels to achieve health benefits. Thus, a need exists to identify general (i.e., common across populations) and population-specific barriers that hinder or stop gay men from participating in physical activity (PA). Salient barriers may be identified through the extent each barrier limits PA (i.e., barrier limitation) and the level of one’s confidence to overcome barriers and engage in PA (i.e., self-regulatory efficacy). The purposes of this study were to (1) provide a description of general and population-specific barriers to PA among sufficiently and insufficiently active gay men, (2) identify barrier limitation and self-regulatory efficacy for the reported barriers, and (3) examine the associations between meeting the current PA recommendation, barrier limitation, and self-regulatory efficacy. Participants were 108 self-identified gay males aged 21 to 64 years who completed a web-based survey. A total of 35 general barriers and no population-specific barriers were identified by the sufficiently and insufficiently active groups. The sufficiently active group reported higher self-regulatory efficacy and lower barrier limitation for nearly all reported barriers. A binary logistic regression used to examine the associations between PA, barrier limitation, and self-regulatory efficacy was statistically significant, χ2(2, N = 108) = 19.26, p < .0001, R2 = .16. Only barrier limitation significantly contributed to the model. Future research should continue to examine barriers to PA among gay men to determine whether an intervention needs to be designed specifically for gay men or whether a one-size-fits-all intervention would be effective in helping all men overcome common barriers to engaging in PA.
Keywords
Gay men compared to heterosexual men may be at a greater risk for some health issues, including the prevalence of cancer, heart disease, depression, and anxiety disorders (Boehmer, Miao, Linkletter, & Clark, 2014; Boehmer, Miao, & Ozonoff, 2011; Everett & Mollborn, 2013; King et al., 2008). Despite the increased risk of health issues, limited research has examined unique factors associated with participation in health-promoting behaviors among gay men. Of this limited research, one area of emphasis has been accessing health care. Gay men compared to heterosexual men are less likely to (1) have health insurance coverage, (2) see a medical specialist, and (3) obtain necessary prescription medication (Clift & Kirby, 2012; Conron, Mimiaga, & Landers, 2010). In addition, gay men experience additional discriminatory practices within a health care setting based on their sexual orientation, including (1) refusal of care, (2) use of harsh or abusive language by health care providers, (3) physically rough or abusive treatment by health care providers, and (4) health care providers refusing to touch gay men diagnosed with HIV (Lambda Legal, 2010).
While the examination of health care access is important to understanding the unique health concerns of gay men, a need exists to expand this knowledge base and identify whether gay men experience unique factors in relation to other health-promoting behaviors. Once identified, these unique factors can be used to design interventions targeting health-promoting behavior change among gay men. One health-promoting behavior that needs additional research among gay men is physical activity. Participation in moderate to vigorous physical activity (MVPA) has been reported to reduce the onset of many health conditions (e.g., heart disease, some cancers, and anxiety) identified as disproportionately higher among gay men (U.S. Department of Health & Human Services [USDHHS], 2008). Based on the national recommendation, to achieve health benefits, adults should regularly engage in one of the following: (1) a weekly total of 150 minutes of moderate-intensity physical activity, (2) a weekly total of 75 minutes of vigorous-intensity physical activity, or (3) a combination of MVPA totaling a minimum of 150 minutes during a week (USDHHS, 2008).
Although limited, research has identified mixed results regarding physical activity levels in gay men. According to Grogan, Conner, and Smithson (2006), gay men (n = 23) participated in physical activity an average of only 1 day each week, which was significantly lower than their heterosexual counterparts (n = 22; i.e., 3 days each week). Additionally, Dilley, Simmons, Boysun, Pizacani, and Stark (2010) conducted a secondary analysis of data from the 2003 and 2006 Washington State Behavioral Risk Factor Surveillance System survey examining health behavior differences (including physical activity) by sexual orientation identity. Based on the results, gay men and heterosexual men had similar rates of insufficient levels of physical activity (i.e., 32.5%, 32.7%). Given the discrepant findings on physical activity levels among gay men and that at least one study (Grogan et al., 2006) only addressed frequency of activity (i.e., vs. duration, too), continued research is warranted to better understand whether gay men meet recommended levels (i.e., a combined duration of 150+ minutes per week of MVPA). To further extend the research, examination of theory-based factors associated with MVPA is ideal (Bandura, 2005; Baranowski, Anderson, & Carmack, 1998; Painter, Borba, Hynes, Mays, & Glanz, 2008).
According to social cognitive theory (Bandura, 1986, 1997), one such factor may be barriers, which are defined as factors that are perceived to hinder or completely prevent participation in physical activity (i.e., perceived barriers; Bandura, 2004; Brawley, Martin, & Gyurcsik, 1998). Individuals may experience a range of barriers to engaging in physical activity that could include both personal (e.g., lack of motivation, too tired, lack of time) and situational (e.g., inclement weather, lack of social support). Barriers identified in previous research examining adult men have included a lack of time, motivation, exercise partner, access to places to be active (e.g., local gyms), neighborhood infrastructure (e.g., running/biking trails), injury, tiredness, and long work hours (Blackford, Jancey, Howat, Ledger, & Lee, 2013; Brownson, Baker, Housemann, Brennan, & Bacak, 2001; Plotnikoff, Mayhew, Birkett, Loucaides, & Fodor, 2004; Sequeira, Cruz, Pinto, Santos, & Marques, 2011).
While a number of studies examining barriers to physical activity have been conducted among the general population of men (Blackford et al., 2013; Brownson et al., 2001; Plotnikoff et al., 2004; Sequeira et al., 2011), no research has been used to identify barriers among men stratified by sexual orientation. The assessment of barriers stratified by sexual orientation has been identified to be critical in understanding factors that are unique in hindering or stopping other sexual orientation minorities (i.e., lesbian women) from being active (Bowen, Balsam, Diergaarde, Russo, & Escamilla, 2006; Brittain, Baillargeon, McElroy, Aaron, & Gyurcsik, 2006; Brittain & Dinger, 2014; Brittain, Gyurcsik, & McElroy, 2008). For example, lesbian women have reported experiencing both general barriers (i.e., common across all populations) and lesbian-specific barriers (i.e., unique to being a lesbian) to participation in physical activity, such as (1) a lack of motivation (i.e., general), (2) being lazy (i.e., general), (3) fear of heterosexual women being uncomfortable sharing the locker room in a fitness facility with a lesbian (i.e., lesbian-specific), and (4) the lack of same-sex partner family memberships at fitness facilities (i.e., lesbian-specific; Brittain et al., 2006; Brittain et al., 2008). Through the identification of general and lesbian-specific barriers, researchers were able to create and implement an intervention designed, in part, to help lesbian women learn effective strategies to overcome their salient barriers and increase their physical activity (Brittain & Dinger, 2014). It may be that gay men also experience population-specific barriers (i.e., unique to being a gay male).
In addition to identifying whether individuals experience general and population-specific barriers, an examination of the extent to which barriers limit physical activity participation (i.e., barrier limitation) and the level of one’s confidence to overcome barriers (i.e., self-regulatory efficacy) is also warranted (Brawley et al., 1998; Brawley, Gierc, & Locke, 2013; Fuller, Gyurcsik, Spink, & Brawley, 2012; Gyurcsik, Brawley, Spink, & Sessford, 2013). In previous research, the frequency with which a barrier occurred (i.e., number of days in a week the barrier was experienced) was not a significant predictor of participation in physical activity; however, barrier limitation had a significant negative association, and self-regulatory efficacy had a significant positive association with physical activity (Brittain et al., 2008; Brittain, Gyurcsik, McElroy, & Hillard, 2011; Fuller et al., 2012; Gyurcsik et al., 2009; Gyurcsik et al., 2013). Furthermore, individuals who were physically active at the recommended levels (i.e., sufficiently active) compared to individuals who were not meeting the recommended levels (i.e., insufficiently active) had significantly lower barrier limitation (Brittain et al., 2008; Brittain et al., 2012) and significantly higher self-regulatory efficacy to overcome barriers (Gyurcsik et al., 2013). Understanding the experiences of individuals who successfully adhere to MVPA (i.e., sufficiently active) and individuals who are unsuccessful at adherence (i.e., insufficiently active) can provide valuable information for the design and implementation of interventions to increase participation in physical activity (Bandura, 2005), particularly among the insufficiently active.
The purposes of this study were to (1) provide a phenomenological description of general and population-specific barriers to participation in MVPA among insufficiently active and sufficiently gay men, (2) identify the related extent of limitation of each barrier and participants’ self-regulatory efficacy to overcome the reported barriers, and (3) examine the associations between meeting the current MVPA recommendation, barrier limitation, and self-regulatory efficacy to overcome barriers. It was hypothesized that gay men would report experiencing both general and population-specific barriers to participation in MVPA. In addition, lower barrier limitation and higher self-regulatory efficacy were expected to be significantly associated with meeting the current MVPA recommendation.
Method
Participants and Procedures
All procedures for this study were approved by the university’s Institutional Review Board. Adult gay men residing within the United States and Canada were recruited to participate in an online survey via (1) study announcements on gay organization listservs, (2) fliers posted at various organization facilities (e.g., university campuses, gay accepting churches), (3) an advertisement on a university research website, and (4) the snowball sampling technique. Snowball sampling is a technique in which individuals who hear about or participate in the study will distribute the study information to other potential participants (Patton, 1990). The link to the online survey was provided on all study announcements and was available for a 4-month period (i.e., mid-February-early June).
Interested individuals accessed the link to the online survey and were first required to provide consent to participate in the study. Then participant inclusion criteria were assessed, which included self-identification as a gay man aged 18 to 64 years, no physical disability that hindered participation in ambulatory physical activity for at least 10 minutes at a time, and the ability to read and write English. Participation in the study included completing a 20-minute online survey via SurveyMonkey to assess (1) physical activity, (2) barriers to physical activity, (3) barrier limitation, (4) self-regulatory efficacy, and (5) demographic information (i.e., education level, height, weight, race, partner/marital status, employment status, annual total household income, general health status, state/province of residence). Participants were also given the option to be entered into a drawing to receive 1 of 12 $10 Starbucks gift cards.
Measures
Physical Activity
The short version of the International Physical Activity Questionnaire (IPAQ, 2001) was used to assess physical activity. The test–retest reliability of the IPAQ short version has shown to be an acceptable level, with 75% of the correlation coefficients observed above .65 and ranging from .88 to .32 (Craig et al., 2003). Concurrent validity has shown reasonable agreement when comparing other short instruments (i.e., .58 [.51-.64]; Craig et al., 2003). Criterion validity of the short version IPAQ data against accelerometers was fair to moderate agreement (N = 781, p = .30, 95% CI [.23- .36]; Craig et al., 2003).
Participants were asked to recall the number of days in the past 7 days they participated in moderate- or vigorous-intensity physical activity for at least 10 minutes at a time. Participants were also asked to indicate the number of minutes spent in each bout of moderate or vigorous physical activity. Vigorous physical activity was defined as “any activity that required hard physical effort and made the participant breathe much harder than normal” (IPAQ, 2001, p. 3). Moderate activity was defined as “any activity that required moderate physical effort and made the participant breathe somewhat harder than normal” (IPAQ, 2001, p. 3).
Total weekly minutes for MVPA were calculated separately by multiplying the total days of participation in the specific intensity by the total minutes. Based on the total weekly minutes for each intensity, participants were categorized into two physical activity groups: (1) insufficiently moderately to vigorously physically active (n = 27; i.e., <150 minutes of moderate activity, <75 minutes of vigorous activity, or <a total of 150 minutes of moderate and vigorous activity combined) or (2) sufficiently moderately to vigorously physically active (n = 81; i.e., ≥150 minutes of moderate activity, ≥75 minutes of vigorous activity, or ≥a total of 150 minutes of moderate and vigorous activity combined).
Barriers, Barrier Limitation, and Self-Regulatory Efficacy
Based on previous research, barriers were defined as “anything that made it difficult or stopped you from doing physical activity in the past seven days” (Brittain et al., 2008; Brittain et al., 2012; Gyurcsik et al., 2009). Four open-ended response items were available so that a wide range of salient barriers to physical activity could be captured. By allowing for open-ended responses rather than a “one-size-fits-all” list of barriers (i.e., an investigator-provided list), participants were able to identify and list salient barriers that hindered their participation in physical activity in the past 7 days (Brawley et al., 1998; Gyurcsik et al., 2009).
Furthermore, in accordance with Brawley et al. (1998) and Gyurcsik et al. (2009), barrier limitation and self-regulatory efficacy were assessed for each barrier listed by each participant. Barrier limitation was defined as the extent to which a barrier limited one’s participation in physical activity in the past 7 days and was measured on a 0 (didn’t limit me) to 8 (completely limited/stopped me) response scale (Bandura, 1986, 1997; Brittain et al., 2008; Brittain et al., 2011). An average barrier limitation score was calculated for each participant by dividing the sum of all barrier limitation scores by the total number of barriers reported. 1
Self-regulatory efficacy was defined as one’s confidence in one’s ability to overcome a barrier and do physical activity in the next month (Brittain et al., 2012; Gyurcsik et al., 2009). Self-regulatory efficacy was measured on a 0 (not at all confident) to 10 (completely confident) response scale (Bandura, 1986, 1997; Gyurcsik et al., 2009; Gyurcsik et al., 2013). Participants’ self-regulatory efficacy was assessed for each barrier they reported. An average self-regulatory efficacy score was also calculated for each participant by dividing the sum of all efficacy scores by the total number of barriers reported by the participant. 1
Measures of barriers, limitation, and self-regulatory efficacy followed recommendations by Bandura (1986) and Brawley et al. (1998) with respect to capturing only personally relevant barriers in relation to a specific action (i.e., physical activity in the past 7 days). The measures were also patterned after other published measures (Brittain et al., 2008; Brittain et al., 2011; Brittain et al., 2012; Gyurcsik et al., 2009). Overall, the measures were content valid, which is a key aspect in barrier assessment (Bandura, 1986; Brawley et al., 1998; Haynes, Richard, & Kubany, 1995).
Statistical Analyses
Data-cleaning procedures (e.g., missing data) were conducted according to Tabachnick and Fidell (2013). Descriptive statistics were calculated for the demographic variables for the entire sample. In addition, descriptive statistics for demographics and main study variables (i.e., physical activity, barrier limitation, and self-regulatory efficacy) were calculated for each physical activity group (i.e., insufficiently and sufficiently active) separately. T tests and chi-square analyses were used to examine differences in demographics between the insufficiently and sufficiently active groups.
Data analyses for the first study purpose (i.e., to provide a phenomenological description of barriers to participation in MVPA) included a constant comparative method by two trained researchers. More specifically, a constant comparative method was used to identify barriers listed by the participants, code these barriers into one of 15 main categories (e.g., work-related, outdoor physical environment), and then discuss any discrepancies with barrier identification and categorization until an agreement was determined (Strauss & Corbin, 1990; Tesch, 1990). The initial identification and coding of barriers resulted in 89.6% agreement between the trained researchers.
A binary logistic regression was conducted to examine the associations between meeting the current MVPA recommendation, barrier limitation, and self-regulatory efficacy. Crude odds ratios and 95% confidence intervals were used to determine statistical significance. Analyses were conducted using IBM SPSS Statistics (Version 20.0).
Results
A total of 163 individuals accessed the online survey. Of the 163 individuals, 55 were excluded for various reasons, including (1) not providing consent (n = 1), (2) not meeting participant inclusion criteria (n = 15), (3) not completing the physical activity measure (n = 8), and (4) not completing the barriers measure (n = 31). The final study sample included 108 self-identified gay males, aged 21 to 64 years (Mage = 39.5 ± 13.2 years). Participants resided in the United States (n = 101) and Canada (n = 7), and the majority were Caucasian (n = 87, 80.6%). More than half were employed full-time for wages (n = 67, 62.0%) and had a bachelor’s degree (n = 25, 23.1%), master’s degree (n = 37, 34.3%), or doctoral/professional school (medical doctor/dentist) degree (n = 15, 13.9%). The median total household income was $50,000 to $59,999 per year. The mean body mass index of the sample, calculated from self-reported weight and height, was 26.4 ± 5.1 kg/m2. The only demographic variable that significantly differed between the two MVPA groups was “general health status,” χ2(4) = 17.04, p < .01. See Table 1 for participant demographic information by physical activity group.
Demographic Variable Information by Physical Activity Group (N = 108).

Note. SRE = self-regulatory efficacy; MVPA = moderate to vigorous physical activity; BMI = body mass index. There are missing demographic data (i.e., employment status; n = 1) for the insufficiently active group. p<.01.
Purpose 1: Phenomenological Description of General and Population-Specific Barriers
A total of 35 general barriers and no population-specific barriers were reported by participants in the study (see Table 2). Of these 35 barriers, the insufficiently active group (n = 27) reported 24 barriers and the sufficiently active group (n = 81) reported 34 of the 35 barriers. The 10 barriers reported by the sufficiently active group but not the insufficiently active group included (1) work—commute to work, (2) work—stress at work, (3) outdoor physical environment—must drive to get to safe walking trails, (4) other priorities—travel/vacation, (5) other priorities—moving, (6) mental health—not wanting other people in the house to hear me exercising, (7) fitness facility issues, and (8) unclassified barriers (see Table 2 for a list of the unclassified barriers). Last, one barrier reported by the insufficiently active group but not the sufficiently active group was “mental health—mental health challenges.”
Reported Barriers, Average Barrier Limitation, and Self-regulatory Efficacy.
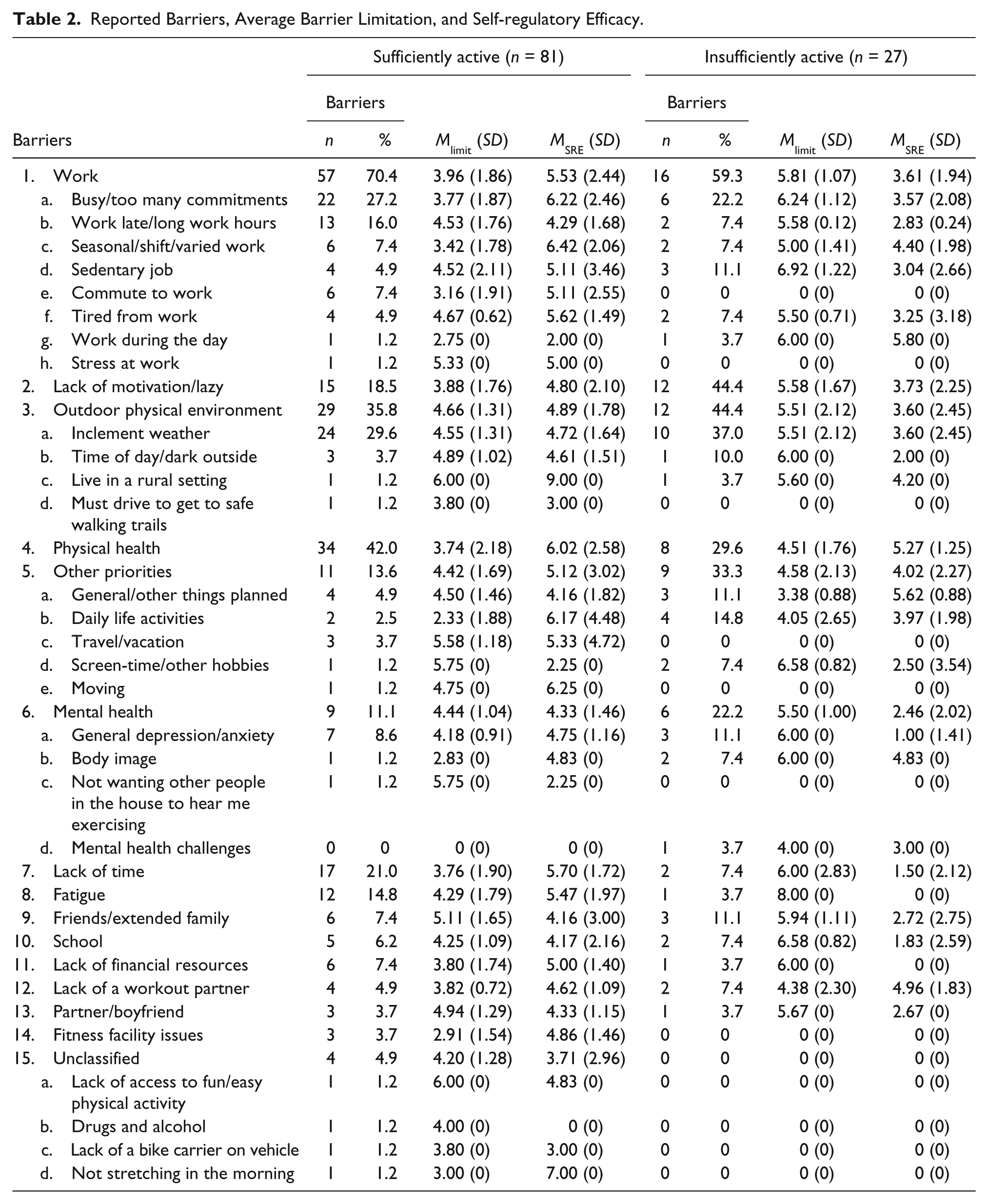
Of the barriers reported by 20% or more of either the insufficiently or sufficiently active groups, the sufficiently active group had a higher percentage of participants, versus the insufficiently active group, who reported the following barriers: (1) the overall category of work (e.g., busy/too many commitments, work late/long work hours), (2) physical health (e.g., asthma), and (3) lack of time. Furthermore, the insufficiently active group reported a higher percentage of the following barriers: (1) lack of motivation/lazy, (2) outdoor physical environment (e.g., inclement weather), (3) other priorities (e.g., general/other things planned, daily life activities), and (4) mental health (e.g., general depression/anxiety). The barriers reported by the highest percentage of participants in both activity groups included (1) the overall category of work and (2) the overall category of outdoor physical environment (see Table 2 for the percentages and ns for the reported barriers by activity group).
Purpose 2: Barrier Limitation and Self-Regulatory Efficacy to Overcome Barriers
Table 1 contains the means for overall barrier limitation and self-regulatory efficacy by group, and Table 2 contains the mean limitation and self-regulatory efficacy of each barrier by activity group. As can be seen, of the barriers identified by both groups, the insufficiently active group reported a higher average barrier limitation for all individual barriers except (1) outdoor physical environment—live in a rural setting and (2) other priorities—general/other things planned. Among individual barriers identified by both activity groups, the sufficiently active group reported higher average self-regulatory efficacy scores with the exception of the following barriers: (1) work—work during the day, (2) other priorities—general/other things planned, (3) other priorities—screen time/other hobbies, and (4) lack of a workout partner.
Purpose 3: Associations Between Meeting the Current MVPA Recommendation, Barrier Limitation, and Self-Regulatory Efficacy
A binary logistic regression model was used to examine the associations between meeting the current MVPA recommendation, barrier limitation, and self-regulatory efficacy to overcome barriers. The logistic regression model with barrier limitation and self-regulatory efficacy was statistically significant, χ2(2, N = 108) = 19.26, p < .0001, Cox–Snell R2 = .16. Barrier limitation was the only variable that significantly contributed to the model (see Table 3). The odds of not meeting the MVPA recommendation increased by 36% for every interval increase on the barrier limitation scale. For example, a rise in barrier limitation from 3 to 4 increased the odds of being insufficiently active by 36%. The nonsignificant Hosmer and Lemeshow, χ2 = 12.36, degrees of freedom = 8, p = .14, suggested the model adequately fit the data when all variables were included.
Summary of Binary Logistic Regression Analysis for Factors Associated With Meeting (n = 81) Versus Not Meeting (n = 27) the Moderate to Vigorous Physical Activity Recommendation.

Statistically significant.
Discussion
This study was the first to examine barriers to MVPA among gay men. A total of 35 barriers were identified among the insufficiently and sufficiently active groups. While gay men have previously identified unique barriers to engaging in health-promoting behaviors (i.e., accessing health care services; Clift & Kirby, 2012; Conron et al., 2010; Lambda Legal, 2010), participants in the current study did not identify any population-specific barriers to participation in physical activity. This lack of population-specific barrier identification is contrary to a plethora of studies examining barriers to physical activity among various populations—for example, adult men and women with chronic conditions (Gyurcsik et al., 2013; Stroud, Minahan, & Sabapathy, 2009), overweight children (Zabinski, Saelens, Stein, Hayden-Wade, & Wilfley, 2003), and women of varying races and sexual orientations (Brittain et al., 2006; Eyler et al., 2002).
Barriers identified in this study and previously reported in literature examining the general population of adult men included (1) lack of time, (2) lack of motivation, (3) lack of financial resources, (4) lack of an exercise partner, (5) busy/too many commitments at work, and (6) work late/long hours (e.g., Blackford et al., 2013; Brownson et al., 2001; Plotnikoff et al., 2004; Sequeira et al., 2011). In particular, Blackford et al. (2013) reported that the most commonly reported barriers were related to work, which is consistent with the results of the present study. In the present study, 70.4% of the sufficiently active group and 59.3% of the insufficiently active group reported work-related barriers, which was the most frequently reported category of barriers by both physical activity groups.
Barrier Limitation and Self-Regulatory Efficacy to Overcome Barriers
As hypothesized, barrier limitation was significantly associated with meeting the current MVPA recommendation. More specifically, a rise in every barrier limitation unit increased the odds of being insufficiently active by 36%. This result is consistent with previous studies that examined barrier limitation among sufficiently and insufficiently active groups (e.g., Brittain et al., 2008; Brittain et al., 2012; Gyurcsik et al., 2009). Taken together, research findings identifying the consistent association between limitation and activity suggest that assessment is warranted in future research. In line with contentions from Brawley et al. (1998), the extent to which barriers are perceived to be limiting may be more important in predicting activity levels than the mere experience of the barriers.
Contrary to one of the study hypotheses, self-regulatory efficacy was not significantly associated with meeting the current MVPA recommendation. In previous research, only one study has examined self-regulatory efficacy and physical activity, and it was among adults with arthritis. The current study results are consistent with this research from Gyurcsik et al. (2013), in which sufficiently active adults with arthritis reported higher average self-regulatory efficacy scores to overcome barriers when compared to insufficiently active adults with arthritis. Furthermore, it is important to note that the average self-regulatory efficacy score for the sufficiently active group (i.e., 5.35) in the present study was just below the midpoint of the scale (i.e., 0 = not at all confident to 10 = completely confident). This average self-regulatory efficacy score for the sufficiently active group was lower than the scores identified among both the sufficiently active (i.e., 7.33) and insufficiently active groups (i.e., 5.74) in the Gyurcsik et al. (2013) study. One important distinction between the two studies is that the self-regulatory efficacy scores reported by Gyurcsik et al. were in relation to arthritis-specific barriers, whereas the self-regulatory efficacy scores in the present study were regarding general barriers. Perhaps the breadth of barriers reported by men in the present study contributed to their lower self-regulatory efficacy scores. That is, when individuals are faced with similar barriers and succeed in overcoming them, their self-regulatory efficacy subsequently increases (Bandura, 1986). It could be that men in the present study simply did not have sufficient experiences in mastering their barriers to have higher levels of self-regulatory efficacy.
Moderate to Vigorous Physical Activity
Seventy-five percent of the current study sample was meeting the national MVPA recommendation, which was much higher than the overall national rate for the general population of men in the United States (52.1%; Centers for Disease Control and Prevention, 2014). The high percentage of gay men meeting the national recommendation for MVPA in the current study was similar to findings from Dilley et al. (2010) in which 67.5% of gay men were sufficiently active. However, Grogan et al. (2006) reported that gay men in England participated in physical activity an average of only 1 day each week. The discrepancies in physical activity levels among the current study and the study by Grogan et al. may be due to differences in the operationalization of physical activity. The current study operationalized physical activity according to national recommendation for MVPA, whereas the study by Grogan et al. used a one-item response scale measure of activity, “How frequently do you exercise/play sport?” (never, less than once a week, once a week, twice a week, three times a week, more than four times per week).
Strengths and Limitations
Several study limitations existed. Participants were mostly Caucasian, educated volunteers who needed Internet access and a computer to complete the survey. There were also a disproportionate number of participants who resided in Canada versus those who resided in the United States. Thus, the generalizability of the results is limited. All study information was self-reported by participants, which could have resulted in biased reporting. Furthermore, the current study was a cross-sectional design, which did not allow for cause and effect conclusions to be postulated. Finally, understanding that this was a preliminary study examining barriers to physical activity among gay men, the odds ratios were not adjusted.
In addition to the novelty of the present study findings within the physical activity literature, there were several strengths. First, the current study was theory-based in which social cognitive theory (Bandura, 1986, 1997) was used in the design and evaluation of this study. Second, based on previous recommendations (e.g., Brawley et al., 1998), barriers were assessed through an open-ended procedure rather than a “one-size-fits-all” measure that would have included a list of barriers. This open-ended procedure was used to maximize the identification of participants’ most relevant barriers. Finally, MVPA was measured according to the current, national MVPA recommendations to improve health (USDHHS, 2008).
Conclusions and Future Directions
Future research should continue to examine barriers to MVPA among gay men. Continued research would result in a better understanding of whether gay men experience population-specific barriers or not. Surprisingly, men in the present study did not report any population-specific barriers. It may be that the study participants were somehow unique in not reporting these types of barriers. Alternatively, not reporting population-specific barriers may be related to a more complex explanation involving factors about sexual orientation (e.g., the embodiment of heterosexual gender norms, level of comfort regarding sexual orientation disclosure, level of connection with the gay male community). Only the conduct of future research can illuminate a reason for this unique study finding. Ultimately, through additional research on barriers to physical activity among gay men, a determination can be made regarding whether an intervention needs to be designed specifically for gay men (i.e., to help them overcome population-specific barriers) or whether a one-size-fits-all intervention would be effective in helping all men overcome common barriers to engaging in physical activity.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
