Abstract
The prevalence of obesity in the United States has increased significantly and is a particular concern for minority men. Studies focused at the community and national levels have reported that geography can play a substantial role in contributing to obesity, but little is known about how regional influences contribute to obesity among men. The objective of this study is to examine the association between geographic region and obesity among men in the United States and to determine if there are racial/ethnic differences in obesity within these geographic regions. Data from men, aged 18 years and older, from the National Health Interview Survey were combined for the years 2000 to 2010. Obesity was defined as body mass index (BMI) ≥30 kg/m2. Logistic regression models were specified to calculate the odds ratio (OR) and 95% confidence interval (CI) for the association between geographic region and obesity and for race and obesity within geographic regions. Compared to men living in the Northeast, men living in the Midwest had significantly greater odds of being obese (OR = 1.09, 95% CI [1.02, 1.17]), and men living in the West had lower odds of being obese (OR = 0.82, 95% CI [0.76, 0.89]). Racial/ethnic differences were also observed within geographic region. Black men have greater odds of obesity than White men in the South, West, and Midwest. In the South and West, Hispanic men also have greater odds of obesity than White men. In all regions, Asian men have lower odds of obesity than White men.
Keywords
Introduction
Over the past few decades, obesity has been identified as a major risk factor for multiple chronic conditions, including hypertension, diabetes mellitus, dyslipidemia, and ischemic heart disease (Griffith, Johnson-Lawrence, Gunter, & Neighbors, 2011; Malnick & Knobler, 2006). Flegal and colleagues reported that the prevalence of obesity among men increased significantly between 1999 and 2010, while the corresponding prevalence among women remained stable during this period (Flegal, Carroll, Ogden, & Curtin, 2010; Kumanyika et al., 2008; Ogden, Carroll, Kit, & Flegal, 2012). This pattern highlights the importance of considering gender in research on obesity. Obesity has also been reported to have an adverse effect on male hormones and prostate health and has been linked to a variety of male-specific comorbidities, including lower testosterone (Du Plessis, Cabler, McAlister, Sabanegh, & Agarwal, 2010), altered sperm (Hammoud et al., 2008), and prostate cancer aggressiveness and mortality, demonstrating the need to examine how obesity affects men (Hsing, Sakoda, & Chua, 2007).
The small but growing body of research examining obesity among men indicates that the prevalence and impact of obesity among men of different races/ethnicities vary considerably. Obesity has been reported to be a particular concern for minority men, as over 40% of Latino men and 37% of African American men are obese (Ogden, Carroll, Kit, & Flegal, 2013). Furthermore, minority men have higher rates of developing and dying from conditions and diseases associated with obesity than other groups of men (Warner & Hayward, 2006). These group differences have been thought to be a function of individual-level risk factors, such as socioeconomic status, genetics, lifestyle, and behavioral characteristics (Bruce, Sims, Miller, Elliott, & Ladipo, 2007; Seo & Torabi, 2006). However, social science and social epidemiologic research has also reported that the social, environmental, and geographic conditions in which people live are associated with health disparities (Bleich, Thorpe, Sharif-Harris, Fesahazion, & Laveist, 2010; Fang, Madhavan, Bosworth, & Alderman, 1998; Gaskin, Price, Brandon, & Laveist, 2009; LaVeist et al., 2008; LaVeist, Thorpe, Galarraga, Bower, & Gary-Webb, 2009; Robert, 1998; Roux et al., 2001; Thorpe, Brandon, & LaVeist, 2008; Thorpe et al., 2013; Thorpe et al., 2014). For example, Thorpe et al. (2014) reported that race differences in obesity between Black and White men were not observed when accounting for the social and environmental conditions in which these men live. Findings from this study underscore the importance of
Understanding regional variation in obesity between men of different races/ethnicities can provide a better understanding of the extent to which population reductions in obesity can be achieved (Singh, Kogan, & van Dyck, 2008). Regional variation in lifestyle factors, environmental/geographical factors, quality of health care, socioeconomic status, infectious processes, and gene prevalence has been reported to influence variation in risk factors and comorbidities associated with obesity (Gillum, 1994; Howard, 1999; Howard et al., 2006; Voeks et al., 2008). Research exploring the degree to which levels of obesity among men can vary by race and region is scarce. The objective of this study is to examine the association between geographic region and racial/ethnic disparities in obesity using data drawn from a nationally representative sample of men in the United States.
Method
Data Description
This study used cross-sectional data from the National Health Interview Survey (NHIS). This annual survey was conducted by the National Center for Health Statistics using a nationally representative sample of the U.S. noninstitutionalized population from all 50 states and the District of Columbia. Participants were surveyed regarding their demographic characteristics, health behaviors and conditions, functional limitations, cancer screening, and health care access and utilization. Individuals aged 17 years and older were eligible to participate in the survey, and NHIS oversampled Blacks, Hispanics, and Asians. The use of sampling weights yielded representative population estimates and adjusts for nonresponse. Detailed information regarding NHIS is reported elsewhere (Pleis & Lucas, 2009; Pleis, Schiller, & Benson, 2003).
For this study, data from the 2000-2010 NHIS were combined. Men aged 18 years and older who responded to questions regarding their race/ethnicity, geographic region in which they lived, height, and weight were included in these analyses. This resulted in an analytic sample size of 327,556 male adults.
Measures
The primary outcome in this study was obesity. BMI values were calculated by dividing participants’ self-reported weight in kilograms by their self-reported height in meters squared. A binary variable for obesity was created to identify those men whose BMI was greater than or equal to 30 kg/m2 versus those men whose BMI was less than 30 kg/m2 (1 = yes, 0 = no).
The primary independent variables were race/ethnicity and geographic region. Men reported the state in which they lived, which was then categorized into one of the following regions (Northeast, Midwest, South, and West) as determined by NHIS. Table 1 displays the classification of states into regions. Men also reported their race as White, Black/African American, Asian and their ethnicity as Hispanic or not Hispanic. A variable was created to identify the following different racial/ethnic groups: non-Hispanic White, non-Hispanic Black, Hispanic, and Asian.
Regional Categorization of United States in the National Health Interview Survey 2000-2010.

Demographic variables included age (years), married (1 = yes, 0 = no), income level (<$35,000, $35,000-75,000, ≥$75,000), and education level (0 = less than high school graduate, 1 = high school graduate/general educational development [GED], 2 = more than high school graduate). Health-related characteristics included having health insurance (1 = yes; 0 = no), reporting physical inactivity (1 = yes; 0 = no), reporting fair/poor health (1 = yes; 0 = no), as well as smoking status and drinking status (0 = current, 1 = former, 2 = never).
Statistical Analyses
Mean and proportional differences in demographic and health-related factors between men living in different regions of the United States were calculated using analysis of variance and chi-square tests. To determine the age-adjusted proportions of health-related characteristics, logistic regressions were specified for the total sample and by geographic region. Each health-related characteristic was modeled as a function of geographic region, adjusting for age and survey year. For the multivariate analyses, logistic regression models were used to examine the association among race, region, and obesity, after adjusting for demographic and health characteristics described above and survey year. In the overall model comparing regions, an interaction term between race and region was included and identified as significant (
Results
Table 2 provides the distribution of characteristics of men who participated in the 2000-2010 NHIS by region. Of the 327,556 male adults, 56,092 lived in the Northeast, 69,925 lived in the Midwest, 118,186 lived in the South, and 83,353 lived in the West. Additionally, of the men in the sample, 200,163 were White, 40,211 were Black, 71,416 were Hispanic, and 15,766 were Asian. In the total sample, the mean age was 44.8 years and 72% of men were White, 11% were Black, 13% were Hispanic, and 4% were Asian. Sixty-six percent of men in the overall sample were married, 27% had income below $35,000, and 17% had less than a high school graduate degree. There were differences by region with respect to demographic variables. Mean age varied by region whereby men in the Northeast were older than men living in other regions. There was a difference in the proportions of White, Hispanic, and Asian men across regions. The largest proportion of Whites lived in the Midwest, while the largest proportions of Hispanic and Asian men lived in the West. Socioeconomic differences were apparent by region among men. The largest proportion of men reporting incomes less than $35,000 was in the South, while the largest proportion of men reporting incomes greater than $75,000 was in the Northeast. Differences were also apparent in educational attainment. The largest proportion of men obtaining less than their high school graduate degree/GED was in the South, while the largest proportion of men obtaining their high school graduate degree/GED was in the Midwest. There were similar proportions of men who reported being married, having annual household incomes ranging between $35,000 and $75,000, and obtaining more than a high school graduate degree.
Distribution of Select Demographic Characteristics of Men Aged 18 Years and Older by Geographic Region, National Health Interview Survey 2000-2010.

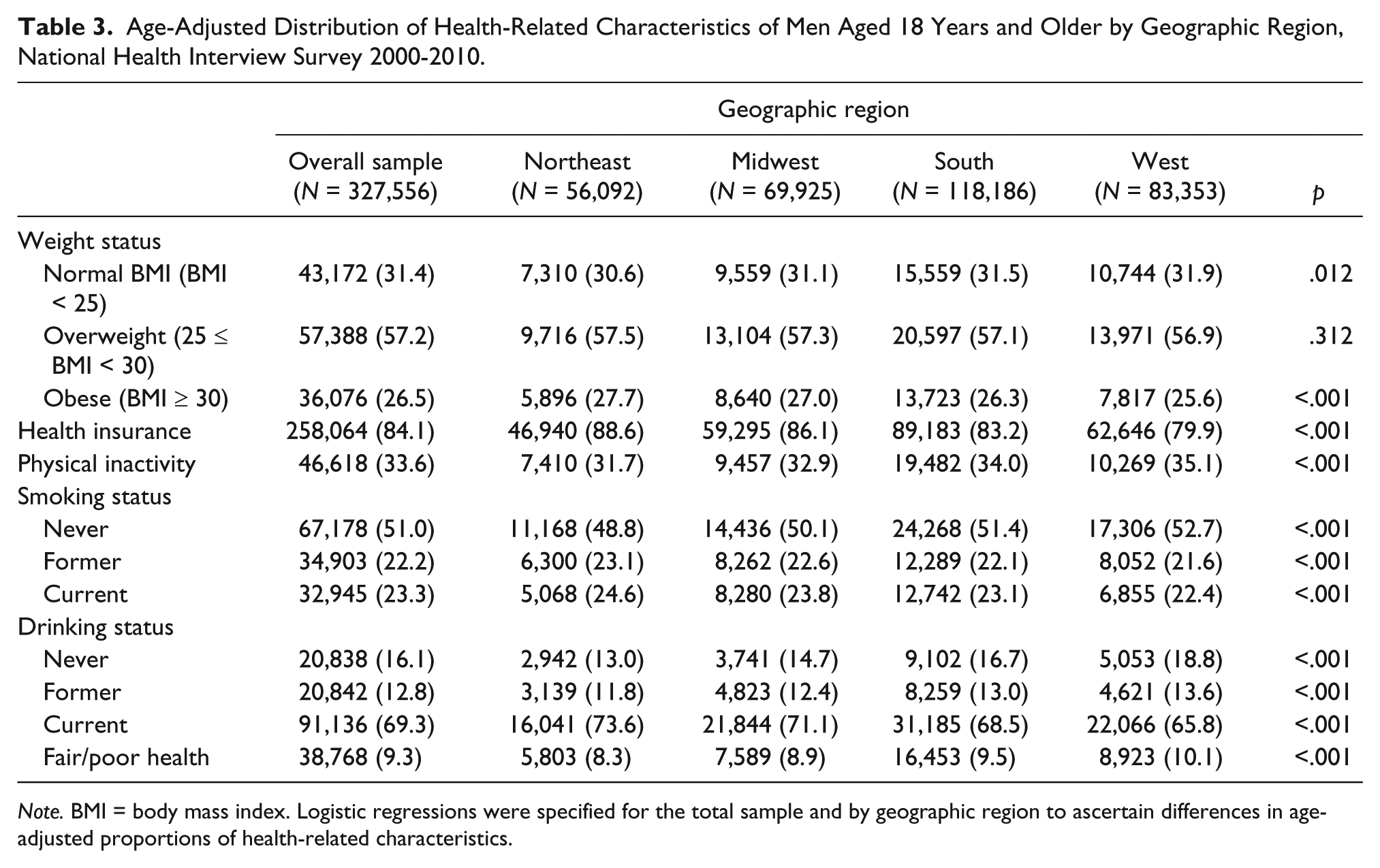
Table 3 provides the distribution of age-adjusted proportions for health-related characteristics and weight status variables for the total sample of men and by the geographic region in which they lived. In the total sample, 27% of men were obese, 84% had health insurance, 51% had never smoked, and 16% had never drunk alcohol. In addition, 9% of men in the overall sample reported that they were in fair or poor health. There were differences by region with respect to health-related characteristics. There was a difference in the proportions of obese men and men of normal weights across regions. The largest proportion of obese men lived in the Northeast, while the proportion of men who reported being of normal weight was largest among men in the West. In addition, the proportion of men who reported having health insurance varied across regions. The largest proportion of men who reported having health insurance was in the Northeast. There was a difference in physical inactivity across regions. The largest proportion of men who were physically inactive was in the West. Smoking status also varied across regions. The proportions of former and never smokers were largest among men in the West, while the proportion of current smokers was largest among men in the Northeast. Drinking status also varied across regions. The proportions of former drinkers and never drinkers were largest in the West, and the proportion of current drinkers was largest among men in the Northeast. In addition, the largest proportion of men who reported being in fair or poor health lived in the West. There were similar proportions of men who reported being overweight.
Age-Adjusted Distribution of Health-Related Characteristics of Men Aged 18 Years and Older by Geographic Region, National Health Interview Survey 2000-2010.
When examining the relationship between region and obesity, differences in obesity were observed. After adjusting for age, marital status, insurance, income, education, fair/poor health, physical inactivity, smoking and drinking status, race/ethnicity, men living in the Midwest had greater odds of being obese (odds ratio [OR] = 1.09, 95% confidence interval [CI] [1.02, 1.17]), and men living in the West had lower odds of being obese (OR = 0.82, 95% CI [0.76, 0.89]) compared to men living in the Northeast (data not displayed).
Table 4 reports the association between race, region, and obesity. Within the Northeast, Asian men had lower odds than White men of being obese (OR = 0.30, 95% CI [0.22, 0.40]). Within the Midwest, Black men had higher odds of being obese compared to White men (OR = 1.29, 95% CI [1.11, 1.49]), and Asian men had lower odds of being obese compared to White men (OR = 0.29, 95% CI [0.21, 0.42]). Within the South, Black men had significantly greater odds of being obese compared to White men (OR = 1.27, 95% CI [1.18, 1.36]), Hispanic men had greater odds of being obese compared to White men (OR = 1.14, 95% CI [1.05, 1.24]), and Asian men had significantly lower odds of being obese compared to White men (OR = 0.27, 95% CI [0.21, 0.36]). Within the West, Black men had significantly greater odds of being obese compared to White men (OR = 1.50, 95% CI [1.25, 1.80]), Hispanic men had significantly greater odds of being obese compared to White men (OR = 1.43, 95% CI [1.30, 1.58]), and Asian men had significantly lower odds of being obese compared to White men (OR = 0.37, 95% CI [0.32, 0.44]).
Association Between Race/Ethnicity and Obesity (body mass index ≥ 30) Within Geographic Region Among Men Aged 18 Years and Older, National Health Interview Survey 2000-2010.

Discussion
The goal of this study was to determine whether the odds of obesity among men vary between geographic regions and by race/ethnicity. The key findings indicate that the odds of obesity among men differ significantly between geographic regions and within regions by race/ethnicity. Compared to men living in the Northeast, men living in the Midwest have greater odds of obesity, while men living in the West have lower odds of obesity, after controlling for race/ethnicity, age, marital status, insurance, income, education, fair/poor health, physical inactivity, and smoking and drinking status. When looking at differences in odds of obesity within regions between men of different races/ethnicities, Black men have greater odds of obesity than White men in the South, West, and Midwest. In the South and West, Hispanic men also have greater odds of obesity than White men. In all regions, Asian men have lower odds of obesity than White men.
This study describes the association between geographic region and variation in obesity among men, where men in the West experience lower odds of obesity than men in the Northeast. This finding is consistent with prior research on geographic region and obesity, which has identified a lower burden in the West (Wang & Beydoun, 2007). This finding builds on recent work that has highlighted the importance of geographic factors in contributing to obesity among men, particularly at the community level (Gaskin et al., 2009; LaVeist et al., 2008; LaVeist et al., 2009; Thorpe et al., 2008; Thorpe et al., 2013). Beyond the community level, this study implies that there may be regional forces that contribute to varying levels of obesity among men of different races/ethnicities.
Another finding of this study is that men of different races/ethnicities have different odds of obesity when living within the same geographic region, with Black and Hispanic men having higher odds of obesity relative to White men in the Midwest, South, and West regions of the United States. This finding is also consistent with work that has documented disparities in obesity between men of different races/ethnicities, even after adjusting for covariates (Griffith, Johnson-Lawrence, Gunter, & Neighbors, 2011). However, what remains unclear is what drives these interregional disparities in obesity among men. Prior literature is mixed regarding the effects of residential racial composition (K. Li, Wen, & Henry, 2014) and segregation (Boardman, Saint Onge, Rogers, & Denney, 2005; Chang, Hillier, & Mehta, 2009; Grafova, Freedman, Kumar, & Rogowski, 2008; Kershaw, Albrecht, & Carnethon, 2013) on obesity among men. The fact that men of some racial groups are more likely to live in poverty and in closer proximity to polluted environments, be exposed to crime, work in low-paying and dangerous occupations, and experience stress around meeting basic needs underscores the importance of considering how these factors affect the health of minority men (Griffith, Gunter, & Allen, 2011; Thorpe et al., 2013; Treadwell & Braithwaite, 2005; Xanthos, Treadwell, & Holden, 2010; Young, Meryn, & Treadwell, 2008). Investigating the interplay of these factors and how they contribute to obesity and regional variation in obesity would enhance our understanding. For example, what is different about the Northeast compared to other regions where Black and Hispanic men have similar odds of obesity relative to White men? Furthermore, why do Asian men have lower odds of obesity relative to White men in all regions of the United States? This study emphasizes the importance of considering which factors, including race and geographic region, intersect with gender to affect men’s health (Griffith, Metzl, & Gunter, 2011; Griffith, 2012).
There are several limitations of this study that may affect interpretations. First, NHIS is a cross-sectional survey; therefore, causal inferences cannot be made. In addition, because NHIS relies on self-reported data, measures of health statuses may include some bias. While multiple studies have identified that self-reported height and body weight bias do not vary by race/ethnicity (Ezzati, Martin, Skjold, Vander Hoorn, & Murray, 2006; C. Li et al., 2012), bias in self-report data may vary by geographic region (Le et al., 2014). Another limitation of this study is that it did not account for whether men lived in rural versus urban areas, distribution of which may vary by region and would likely affect levels of physical activity and contribute to differing levels of obesity among men (Zhang et al., 2014). Also, NHIS does not account for racial/ethnic or regional differences in work exposures that contribute to disparities in obesity. Men in low-activity occupations have a higher probability of being obese than do men in high-activity occupations (King et al., 2001), and work-related stress has also been reported to be associated with obesity (Kivimäki et al., 2006; Schulte et al., 2007). Some research has identified differences in genetics that may contribute to disparities in obesity between people of different races/ethnicities (Faith & Kral, 2006; Monda et al., 2013). Genetic information was available in the NHIS files that were used for this project.
There are limitations associated with using BMI as a predictor of adverse health outcomes. Body fat, waist circumference, or other measures that take race and gender into account may be better predictors of long-term adverse health effects (Sumner, Ricks, Sen, & Frempong, 2007) but were unavailable for use in this study. For instance, research has identified racial/ethnic differences between BMI and percentage body fat (Deurenberg, Deurenberg-Yap, & Guricci, 2002; Deurenberg, Yap, & van Staveren, 1998; Wagner & Heyward, 2000). More specifically, compared to Whites, Blacks tend to have a higher BMI and Asians tend to have a lower BMI at similar levels of body fat, which suggests that the risk of obesity may be overestimated in Black men and underestimated in Asian men (Deurenberg et al., 1998; Wagner & Heyward, 2000). Research has identified a wide range of BMIs consistent with minimum mortality that vary between people of different races/ethnicities (Durazo-Arvizu, McGee, Cooper, Liao, & Luke, 1998). Furthermore, while a BMI cutoff of ≥30 has good specificity and positive predictive value for identifying obesity, it may misclassify more than half of the general population with excess fat as being normal weight, and for any given BMI, there is substantial intersubject variability in body fat percentage (Romero-Corral et al., 2008). Nonetheless, increasing BMI has been associated with multiple adverse health effects in people of all racial/ethnic groups (Stommel & Schoenborn, 2010).
Despite these limitations, there are several strengths associated with this study. First, this study’s focus on men enabled the authors to examine the relationship of geographic region and obesity in an understudied and important population. Second, this study combined 11 years of NHIS data, which afforded a large sample size with ample statistical power. Additionally, this study was able to account for a wide array of upstream social determinants of obesity, such as income level and educational attainment, and lifestyle determinants of obesity, such as smoking status and drinking status, across men of various races/ethnicities in all regions in the United States. To date, the authors are not aware of another study that has examined the relationship between geographic region and obesity among men of different races/ethnicities.
In documenting the regional and racial/ethnic variations in obesity among men, the findings of the study have implications for a nuanced understanding of the inter- and intraregional forces that contribute to obesity among men. Additional research is needed to better understand how health-related behaviors affect obesity across regions and the particular effects of geographic region in contributing to obesity among men. Future environmentally focused research should aim to provide in-depth explorations of the social, cultural, and historical forces that contribute to disparities in obesity among men at the inter- and intraregional levels. Only then can evidence-based decisions be made regarding resource allocation and intervention development.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Research conducted by the last author was supported by a grant from the National Institute on Minority Health and Health Disparities (P60MD000214) and a grant from Pfizer, Inc.
