Abstract
Enabling factors that influenced men to seek assistance for mental health concerns—a previous underresearched area—was the primary focus of this research. Past research spanning four decades has focused on men’s barriers to mental health help-seeking with limited research positing social norms within men’s peer groups and reciprocity as potential mental health help-seeking enablers. Using a qualitative design, nine men were interviewed to identify the positive factors they believed assisted their help-seeking decisions. Social norms, reciprocity, a significant other, and helpfulness of their general practitioner were domains identified in the analysis of participant narratives. The study revealed the participants’ mental health and treatment illiteracy. Ignorance and misplaced stereotypes, initially acted as barriers to help-seeking, leading to denial of illness, impeding treatment, and perpetuating stigma. Sportsmen disclosing their mental health issues were identified as a positive influence for other men’s help-seeking and assisted in the development of help-seeking as a social norm. The results of this study contribute to understanding the factors that enable men to seek mental health help.
Men’s mental health help-seeking behavior is described as problematic, failing, and in some countries in a state of crisis (Coyle & Morgan-Sykes, 1998; Karoski, 2011). Men’s reluctance to seek help for mental and physical health concerns was the focus of Fischer and Turner’s (1970) study more than 40 years ago, with men’s help-seeking behaviors remaining stable since this time (e.g., Fischer & Turner, 1970; Vogel, Heimerdinger-Edwards, Hammer, & Hubbard, 2011).
Men’s mental health help-seeking is important for resolving issues that have an impact on an individual’s personal and work-related relationships (Addis & Mahalik, 2003). While men may have lower reported levels of mental health disorders than women, the underdiagnoses in men is due to a reluctance to seek assistance, not the absence of the disorder (McKelley, 2007; Peate, 2010), with denial of illness and “self-management” approaches more likely to lead to poor health outcomes for men (Ogrodniczuk & Oliffe, 2010).
Many possible barriers to help-seeking are posited in men’s mental health research, with most studies investigating gender differences. Men are less likely than women to seek help from mental health professionals due to “masculine beliefs,” identification and conformity to male gender roles, or fear of being stigmatized (Mahalik, Burns, & Syzdek, 2007; Mansfield, Addis, & Courtenay, 2005; Vogel, Wade, & Ascheman, 2009). Boman and Walker (2010) report men who conform to masculine beliefs perceived more barriers to health care than men with lower levels of conformity (Boman & Walker, 2010).
Galdas, Cheater, and Marshall’s (2005) review of the gender comparison literature revealed a need for within-group studies to investigate differences in men and not just between the genders arguing men are not a “homogenous group that can be compared against women” (p. 620). Möller-Leimkühler (2002) identified other factors that may act as barriers to men’s help-seeking including living alone, unemployment, cost, or lack of time. Research however fails to reveal observable change in men’s health help-seeking behaviors in four decades (Möller-Leimkühler, 2002), with limited focus on enablers.
Perceived reciprocity and social norms have been identified as potential enablers. Mansfield, Addis, and Mahalik (2003) reported men are more amenable to help-seeking if they have the opportunity to reciprocate; to repay the debt. Men’s groups exemplify this providing the prospect of reciprocation and adherence to societal expectations of masculinity, thereby “preserving status” and ensuring one is “strong and competent” (Addis & Mahalik, 2003). The Men’s Shed movement is an example of this and provides a sense of belonging, reciprocity, and mateship between men with positive health and social outcomes, including a “vital link to health professionals” and improved social, physical, and mental outcomes (Misan, 2008). The influence of perceived reciprocity on men’s mental health help-seeking behavior, however, requires further investigation.
Past research posits perceived social norms, such as masculinity, stoicism, and gender roles as being negative influences on men’s help-seeking, acting as barriers. Perceptions of social group normativity are of significance to men acting as determinants of mental health help-seeking decisions (Addis & Mahalik, 2003). The role of perceptions of normativity in predicting health behaviors in men revealed men’s own health behaviors were significantly related to their perception of other men’s behaviors (Mahalik et al., 2007).
Vogel et al. (2011) investigated men’s help-seeking attitudes and social norms reporting a significant relationship between norms and attitudes to help-seeking. Attitudes to help-seeking were identified to be less favorable when participants endorsed “dominant masculine norms” (Vogel et al., 2011), and Vogel, Wester, and Larson (2007) identified five factors that inhibit the help-seeking process: social stigma, treatment fears, fear of emotion, anticipated risks, and self-disclosure. The concept of social norms, although salient, is understudied in this help-seeking process. Vogel, Wester, et al. (2007) argue that often those closest to an individual may inhibit the decision to seek assistance due to stigma on the family or in-group and the message that counseling is a negative experience may be a social norm conveyed by family, closest friends, male’s peer groups, or other men in general. Evidence suggests that mental health promotion, health professionals, and the media may play a crucial role in reframing the negative norm of help-seeking for mental health issues (Vogel, Wade, Wester, Larson & Hackler, 2007). Mental health help-seeking, when perceived as a norm behavior, appears to be an enabling factor, when the behavior is presented as positive, and a barrier when the help sought is presented in a negative frame. Thus, the role of perceived norms is important to advancing an understanding of men’s mental health help seeking.
Men who experience poor mental health are less likely than women to seek help, deny the presence of a mental illness, and engage in self-management. Research into enablers is sparse with four decades of research focusing on perceived barriers with little known about the men who do engage in help-seeking. The aim of this research was to identify the enablers men engage to facilitate mental health help-seeking with reciprocity and social norms of help-seeking informing this study. The concept of reciprocity and its role within men’s peer groups was explored to determine if the opportunity to reciprocate within the group enabled help-seeking. The influence of men’s perception of counseling as normative and therefore socially accepted within their group was also investigated. The identification of enablers to men’s mental health help-seeking addresses a void in the research into men’s mental health help-seeking behaviors.
The identification of perceived enablers to mental health help-seeking will add to the body of research, which informs strategies and policies to improve men’s help-seeking behaviors, providing a richer understanding to assist in health promotion and engagement with men in practice. Additionally, identification of the factors men perceive enabled their decision to seek help will assist in developing the most effective ways to promote and engage men in therapeutic planning and treatment.
Method
Study Design
Due to a dearth of research on enablers to men’s mental health help-seeking, a qualitative design allowed the use of an inductive approach to develop an understanding (Sarantakos, 1993). An inductive approach allowed for the collection of rich, narrative, and informative data to understand the men’s experiences of mental health help-seeking (Sarantakos, 2005).
Semistructured, in-depth interviews were used to identify and explore the participants’ enabling factors for mental health help-seeking. Interviews allow for an exploration of an individual’s ideas and provide a structured flexibility that facilitates engagement between the researcher and the interviewee (Legard, Keegan, & Ward, 2003). The interview questions covered the following domains: intentions to seek counseling, prompts to seeking counseling, resources used in seeking counseling, family/friends/mates’ experiences of counseling, and other enablers. The study received ethical clearance from the University of Ballarat Research Ethics Committee.
Data Collection
Nine men aged 23 to 65 years were recruited through promotion of the research to psychologist and counselors in Melbourne, Australia. The sampling frame required participants to be receiving counseling or having had received counseling in the past 12 months and for this counseling not be have been mandated or involuntary. At the time of interview all nine participants had completed at least five counseling sessions in the past 12 months. Of these nine men, two identified as gay, with the remaining seven identifying as heterosexual. Four of the participants were in long-term relationships, four were single, and the remaining participant did not disclose his relationship status.
Data Analysis
Data were analyzed using thematic analysis. Thematic analysis is an inductive approach that allows the identification of emergent themes and a deductive approach allowing for the exploration of a priori themes (Ezzy, 2003). After data were transcribed, the transcripts were checked for accuracy and coded. Codes were developed a posteriori, or as emergent ideas evolved, and a priori, or as predetermined concepts such as reciprocity and social norms. These codes were then explored for similarity and themes developed as recommended by Ezzy (2003). An iterative analysis process was used where interviews were analyzed and new data interrogated to ensure coverage of codes. Both researchers coded two interview transcripts and compared codes and coding. Comparisons of coded transcripts were made and a moderation process was used to finalize codes. At the conclusion of the analysis, both researchers checked the codes and coding for confirmability. Theme development was based on both researchers identifying code relationships, comparing of theme development for congruency which informed the final themes.
Rigor in the Research Process
The four elements of qualitative research rigor were applied to the data: credibility, transferability, dependability, and confirmability (Lincoln & Guba, 1985). Credibility refers to the truthfulness of results and whether the research reflects the experiences of the participants. Member checking was available, providing participants with opportunity to check their transcript and verify their interview data—no participant opted for this opportunity. Peer debriefing was undertaken with regular meetings between the researchers to provide an opportunity for reflection and identification of implicitly held ideas; to understand the position taken by the researcher to the data and analysis; to test emergent theories and ideas, and as an opportunity to debrief (Cohen & Crabtree, 2006; Lincoln & Guba, 1985).
Transferability is demonstrating that findings can be applied in other contexts (Liamputtong, 2009). Rich descriptions and detail (Lincoln & Guba, 1985) provides readers with empathy for the participants’ narratives enabling the transfer of themes to new and other similar situations. Dependability refers to the study being consistent and repeatable (Lincoln & Guba, 1985)—that the study can be repeated with similar results. Dependability as a rigorous process is the presentation of the research in a way which enables others to replicate the study. Confirmability is the transparency of the results from the view of the researched not the researchers. Transparency was maintained though the data collection and analysis process through regular meetings between the researchers and the presentation of excerpts from the participants’ interviews as evidence of the codes.
Results
The results are presented below according to the themes identified in the analysis. An overview of the participants is presented in Figure 1 as capsule biographies to outline key information about each participant to enhance understanding of their social world (Dowsett, 1996).

Capsule biographies of participants.
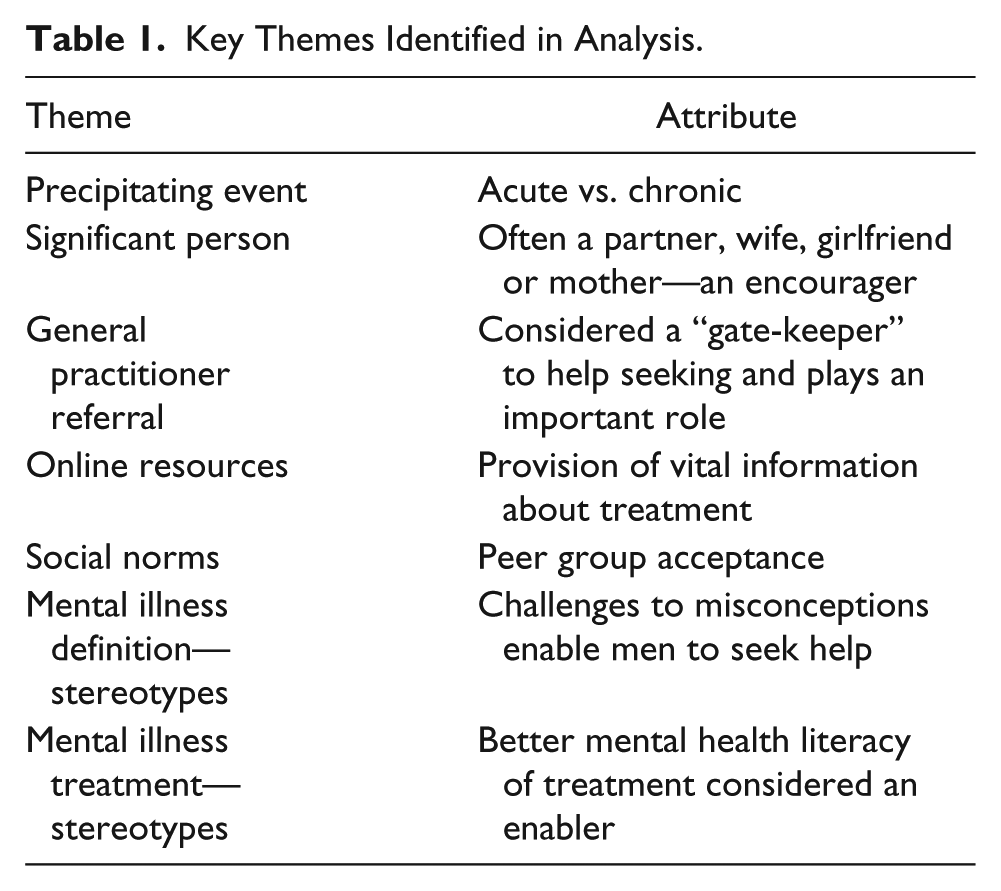
Seven themes were identified through the data analysis with these themes being the amalgam of the codes relating to each theme. The themes contributed to the identification of mental health help-seeking enabling factors and the exploration of the concepts of social norms of help-seeking and the engagement in reciprocity. Participant quotes have been chosen to best illustrate the seven themes presented in Table 1.
Key Themes Identified in Analysis.
Precipitating Event
For some participants the precipitating event that informed the decision to seek counseling was acute, demanding immediate action, and for others it was a chronic condition that had debilitating consequences on everyday living. Cam, Arnold, and Mal describe domestic troubles or a relationship breakdown as the trigger to their decision to seek help; for Max there were difficulties in sexual functioning. For Tommy and Paul, the symptoms of severe anxiety and panic attacks became more frightening and had begun to impact on their day-to-day lives. Paul tolerated the symptoms until they became unbearable, all the time believing them to be physiological:
It was frightening . . . just so frightening. Nine days out of ten I had to pull my car over on a busy freeway then try to get back into traffic. I was shaking. . . . The whole time I thought there had to be something very wrong with me. . . . There had to be a disease, cancer or some heart problem. It was day in day out for such a long time.
Roy, like Paul, reported physiological symptoms, where functioning became difficult with an unrelated hospital admission influencing seeking help for his mental health.
Significant Person
Participants acknowledged the influence of a significant other in the decision to seek mental health assistance. Arnold, Cam, and Max describe their wives or girlfriends as being the main influence on their decision. For these three men, counseling was not something they would have initiated themselves if not for their partners’ encouragement:
If I hadn’t been married or in a close relationship, I wouldn’t have done anything. My wife suggested it for quite a while. . . . I think we might have had a doozy of an argument and then that was maybe when . . . (Max)
Cam was hopeful that couples counseling may have offered some solutions for their marriage difficulties. This period of therapy exposed some personal problems which Cam then sought individual psychotherapy:
Yeah, she definitely initiated it and I thought it was the only way of fixing it or bringing it all out. . . . From there it led to me seeing him [current psychologist].
For Arnold it was the recommendation of his girlfriend and the normalization of seeing a therapist as she had done in the past. Arnold commenced couples counseling with his girlfriend, and saw a psychologist alone for his own benefit:
We were in a relationship, there were challenges, we discussed our problems and she thought it good if I spoke to someone about it.
Roy and Brent each had a female significant other who influenced their decision to commence counseling. For Roy, this was his ex-wife and for Brent this was a close female friend who had undergone counseling in the past. Being able to see how bad she was and the improvement after therapy was sufficient enough motivation to inform Brent’s decision. The decision of Mal’s same-sex partner to consider ending their relationship, believing Mal needed to see someone about the break up was his motivation. It was the role of a significant other who provided an impetus for the participants to seek counseling. For two of the men it was also the normalization posed by the significant other’s past attendance at therapy.
General Practitioner Referral
Irrespective of the impetus to seek assistance, participants consulted a general practitioner (GP)/physician prior to counseling. The experience of a GP consultation varied for these men. For some participants, the GP provided comfort and immediate assistance while others reported the initial consultation as daunting. Cam and his partner consulted their regular GP hoping she knew the best pathways available for alleviating their relationship problems. It was a relief that it “felt as if she [GP] really understood . . . Without her being so proactive. . . . That was really the most important thing.”
Mal was referred to a psychologist within the same clinic as his GP. This was reassuring as they were all experienced in same-sex issues. Brent and Paul found their initial consultations were inhibiting. Brent attended his clinics for a general check-up due to feeling really anxious and worked up about a lot of things. Expecting a referral to a mental health professional, he found he initial consultation was discouraging: “I had a check-up done . . . [The GP] went through everything like do I smoke, drink, you know this and that yet I could not engage the GP on what I wanted.” However, a follow up consultation with a female GP facilitated Brent’s referral:
Anyway I went back to the surgery and got a different doctor. . . . With her I could say that things weren’t the way they seemed. I told her all the shit I had going on. She thought I could benefit from seeing someone. I had been thinking about that for a while. She knew a really good one [psychologist] that she referred me to.
Paul’s initial consultation was also disheartening with the GP being dismissive—“Oh, you’re just experiencing panic attacks mate. He gave me a DVD to watch . . . didn’t do much to stop them.”
Tommy presented at different medical clinics as he did not have a regular GP and reported the visits as unhelpful. Like Paul’s experience, the GP was also dismissive: “you’re ok; it’s just a panic attack. You’re not in any physical danger you know.”
Roy had been seeing his same GP for a number of years, presenting with myriad flu-like symptoms and feeling down in the dumps. He was initially given anti-depressants which he had a bit of a reaction to and they didn’t appear to do anything anyway, so he ceased taking them. After his long-term GP retired and was replaced with a young female doctor, at the insistence of his ex-wife, Roy again presented to the surgery:
When my old doctor retired, the lovely Doctor M started. She gave me this sheet about “Automatic Negative Thinking Styles” . . . well at first I thought it was hippy bullshit. . . . She could see my symptoms . . . She got me the Better Access
1
thing and devised my Mental Health Plan, then referred me to [current psychologist]. I think I’ve already gone through two lots of that. . . . I think that I am so lucky that . . . my GP genuinely cares for me. . . . She’s even encouraged gentle stretching classes and even though it’s all been a lot of hard work, it’s been effective.
These experiences highlight the importance the GP can have in enabling men to access mental health help-seeking. These men had little idea about access to therapists, cost, or referral requirements. However, most agreed that a visit to the GP was at least a doorway to the things like therapies that are available and the role of the GP was an important enabler for these men to seek therapy. As noted where the GP was positive and facilitative, the process was smooth and easy and where the GP was not so helpful the process was delayed.
Online Resources
When asked about the use of online resources, the participants reported they had all searched psychologists’ websites postreferral, joined online forums, or used the Internet to search for a counselor. All recalled beyondblue
2
being the major online resource, but admitted to only briefly visiting the site due to the perception that beyondblue was only associated with depression and none of the men believed this was relevant to them. This idea is best summarized by Paul:
People just don’t know where to search. . . . Like beyondblue, it’s just a brand, you don’t just want a brand. . . . They do a lot of stuff and advertising but it’s just depression.
Online resources were utilized further once a referral for counseling had been received. Max and his wife used an internet search before committing to an appointment with a counselor as did Brent prior to making the initial appointment with his psychologist:
Yeah when I first had her name, I googled her and she has this amazing website all about her approach to therapy. I went through it and looked up her suggested reading and things like that. I really sussed her out . . . it was all pretty positive stuff to be honest.
When Peter decided he didn’t want to feel like this anymore he used an Internet search for psychologists and counselors, admitting that he had no clue where to even start. After being dissatisfied with GP advice, Tommy used the internet to help him understand symptoms and found solace in online forums reporting:
After that, I preferred to do my own search. . . . Forums were definitely very helpful. The great thing about them is that it can bring a lot of likeminded people with similar experience together. It’s really good to sort of share knowledge and experiences . . . makes you realize you’re not alone.
The use of online resources was effective in reinforcing the decision to seek counseling once a referral had been sought. Prior to referral the participants were unaware of where to begin an Internet search. The most prominent website mentioned during interviews was beyondblue; however, no participants had used beyondblue’s resources.
Social Norms
The participants were asked during interview to consider their closest male friends’ reactions to them seeing a psychologist or counselor. All participants reported that perceived social norms influenced their decision in discussing their mental health help-seeking with mates. The men tended to divulge more of their personal experiences if it was normalized within their social group. For example, if it were explicit that others in their group had similar counseling experience or mental health issues. There were also definitive boundaries around what was seen as acceptable within their peer group. Max explained:
Like if I lost someone close to me, like not old. Say if my wife passed away. . . . If I went to a psychologist to deal with that, I wouldn’t feel awkward mentioning it. . . . Say what those footballers have all gone through with the death of that Port player in Vegas, there wouldn’t be a problem talking about getting help.
Paul could talk to family about mental health but not close male friends.
It all depends who you’re talking to. Like if I’m talking to mates down at the pub, I don’t talk about depression. I would say “F*cking work, they’ve been stressing me out.” . . . You just can’t open up to a male. It’s just not the same. If you’re just a bit f*cked up from work, then that’s ok. . . . Away from the pub, you could probably try to explain things better. Like to you.
There was a sense of shame associated with going against a peer group’s social norms. This was particularly evident in Cam’s response.
I wouldn’t just ring my mates . . . no, they couldn’t know. I couldn’t start crying or stuff like that. . . . You sort of feel embarrassed about it.
Although if the mate or peer group were amenable, the participants were comfortable in discussing their experience.
It would be easier if it came up in conversation that someone else was seeing a psychologist . . . then I could . . . you know, then it’s normal. (Mal)
The role of high-profile sporting identities openly discussing their battles with mental health has influenced the participants’ perception of social norms. Arnold felt that although his peer group is pretty open-minded and not as macho, sporting role models admitting to their struggles has been constructive.
When Nick Riewoldt was the St. Kilda captain and he busted his shoulder, was going to miss three months and started to cry. . . . What he demonstrated was far beyond what he realized. . . . I mean, he was a role model for kids. (Arnold)
The men were able to name many high-profile sportsmen who had talked about personal mental health problems. If elite sportsmen are able to discuss their issues, it assisted men in identifying and normalizing their own issues. As Tommy states,
I’ve noticed that it’s not until they can admit to it . . . for a lot of blokey blokes, it helps them be able to admit to it also.
Participants believed acceptance of mental health help-seeking to be more normal for the younger generation. For Peter, his experience has helped him recognize and mentor young men at a local football club and he believed the use of social networking, particularly Facebook, has played a part in these young men being more open in discussing problems.
Peter believes this group has a greater awareness and can open up due to the older generations doing the hard yards on their behalf. Peter is suggesting that older men are leading the way, enabling the next generation to see help-seeking as positive. For men there are many perceived barriers including whether mental health help-seeking was a normative behavior within their peer group. The men alluded to a sense of relief when mental health issues similar to their own were discussed within their social group.
Mental Illness Definition: Stereotypes
One theme to emerge from all the interviews was the misconception of mental illness definitions and treatment stereotypes. All the men reported self and peer group ignorance of what defines a mental illness. For Cam, Tommy, and Max it was the commencement of counseling that brought clarification. As Max explains,
I would never have thought that something there [sexual] would ever be considered a mental problem. . . . Yeah before that, mental illness was someone walking along the road, talking to themselves. You know, like the ones you see in the city.
For Tommy, receiving a diagnosis gave him an understanding of his illness, enabling him to commence therapy more confident of success:
It really changed my whole outlook since the diagnosis. . . . I never knew why it was happening. . . . I really just kind of imagined I was losing the plot. Once I had a name, I felt like I had a way to go forward. There was light at the end of the tunnel.
For others, diagnoses of mental conditions are contrary to their ideas of gender construction. Depression and anxiety were initially thought to be “female” conditions and it was thought to be more socially acceptable for women to be diagnosed with these illnesses.
Look, I know it’s a bit of a stereotype, but from a woman’s point of view it’s a lot easier, isn’t it? (Peter)
According to Tommy, he and his peer group shared a similar view:
For a lot of us, it feels too feminine, even if they [males] were to admit to just having low moods. . . . Males can’t admit to having a moody or a low day; that’s what women do.
Max was also of the opinion that gender roles played a part in stereotyping, beginning with lessons learnt in childhood; men have to be tough and steer the ship in troubled waters only allowing themselves enough time to be a bit run down or tired. Arnold sees society reinforcing these gender stereotypes by encouraging boys to be strong. Men, according to Arnold, are potentially less in touch with their roles in modern society. He describes his current mental state as a conflict between knowing how much is “me” and should be embraced, celebrated and how much is unhealthy? For Arnold, while strict gender stereotypes may have lessened in some respects in terms of mental health and associated help-seeking, the boundaries are not clear.
The perception that mental illness is only represented as severe or potentially life-threatening in the media was the general consensus among the men. All were able to recount instances of bipolar, schizophrenia, or psychotic outbursts viewed recently on television. On the other hand, they were unable to recall such depictions of more common or less dramatic disorders and in their view, this creates a false belief that mental illness is potentially more extreme. For them, less ignorance would enable more men to seek assistance. The participants’ responses are typified by Max’s words:
For me mental illness was anyone in a white suit and restraints . . . in a loony bin.
Tommy describes his peer group as holding similar views:
Most people I know think mental illness and think people hearing voices in their head, hallucinations, crazy outbursts. . . . People tend to think of cutting their wrists or jumping off bridges. . . . A better understanding would make things so much easier.
The men identified that after attending counseling, they had a better understanding of their presenting condition, removing some of the long-held misconceptions. This was not only from a personal perspective, but reduced the stigma the perceived in others’ problems. The men agreed that health promotion in the media of what constituted mental health would enable more men to seek help.
Mental Illness Treatment: Stereotype
Deciding to seek mental health assistance was met with trepidation due to the stereotypes the participants held surrounding treatment. The men expected their treatment options were Freudian couches and personality changing drugs and after receiving the referral, some men were reluctant to make counseling appointments due to these perceptions. As described by Brent:
I got the referral but didn’t end up going for a few months. . . . I was so surprised when I saw her [psychologist] because it’s not like you see on TV; the whole laying on the couch thing. That would have put me off.
For Mal it was scary due to being so unknown, even though he had completed a degree which included some psychology subjects. Not knowing what a therapy room looked like or how therapy would proceed was still foreign to him. The apprehension was shared by other participants:
He [psychologist] is just so different to that stereotype . . . the whole on the couch thing. It’s like we just get in there and talk . . . that helped with the fear. (Cam)
Asked what he thought his initial therapy session would look like, Paul responded,
Oh good question. I thought it would be, you know, stereotypical, like just some psychiatrist picking at your brain, asking questions.
Participants prescribed antidepressants or antipsychotic medication by their doctor reported concerns that the drugs would change their personality or cause disruption to their normal functioning. A treatment plan including medication and counseling explained to them by their psychologist allayed some of their concerns. All reported relief that the treatment by their respective medical professionals was a more positive experience than they had imaged due to incorrect stereotyping.
Access, Availability, and Cost
The men reported concerns regarding the cost and access to suitable mental health professionals. The cost of psychotherapeutic services was still expensive for some of the men, even after the Better Health Access Medicare rebate. The men reasoned that there were more subsidies and rebates available for physical health concerns and that these should carry over to lessen the costs of mental health services. Out-of-pocket expenses were not the only concern; missing time from work was also disconcerting. For Cam it was all about the time off work. . . . You have to take a half day sickie really. For him there was the added cost of travel from outside of Melbourne due to a lack of immediate access to a psychologist in his area.
One of the hardest things is getting an appointment . . . it’s not that easy to even see a counsellor. We can only get into one every three or four weeks. . . . When it’s urgent, that makes it a bit tricky.
It took Peter more than a week to get an appointment with his psychologist and during that time he felt really agitated and thought about cancelling quite a few times. Peter thought that sourcing his own psychologist and paying the full fee without accessing a rebate would have made his initial appointment available earlier.
Availability of a psychologist within the clinic of the GP eased the burden of appointment making. For Mal, being able to seek help for all health problems in one location was advantageous:
Yeah certainly the clinic that I go to has my GP, psychologist and physio all in the one place. They’re all the people I need and all in the one spot . . . location and convenience.
Seven key themes were identified through analysis and six of these themes can be considered enablers. The exception is the precipitating event. Men who reported a significant other in their lives were enabled to access services, especially if this person (often a woman) had also previously sought mental health help. GPs played a pivotal role in the identification and sourcing of treatment services, and the availability of online resources were identified to better enable men to seek help and normalize the experience of mental health. Positive stereotypes of mental illness definition and treatment enabled the men to challenge preconceived notions of mental illness and how it is treated. Access, availability, and costs of services were vital in maximizing opportunities for these men to seek help. These identified enablers provided opportunity for better mental health literacy and increase in men’s help-seeking.
Discussion
The aim of this study was to identify the factors that influenced and enabled men to mental health help-seek. Past research has focused on the barriers men perceive as impeding help-seeking, with little research on enabling factors. Past studies posit numerous factors for the reluctance in men’s help-seeking attitudes, and according to McKelley (2007) these have remained stable over time and across cultures (e.g., Fischer & Turner, 1970; Good, Dell, & Mintz, 1989; Hausner, Hajak, & Spiessl, 2008; Lohan, 2007; Norcross, Ramirez, & Palinkas, 1996; Peate, 2010). The current study sought to determine the factors men believed enabled their help-seeking decisions with a view to addressing the gap in men’s mental health help-seeking literature.
Peer group social norms about help-seeking and reciprocity were identified as enablers (Addis & Mahalik, 2003; Mahalik et al., 2007; Vogel, Wester, et al. 2007). As expected, these factors were identified by the participants as influences in their help-seeking decisions. However, the men conceded that opportunity to reciprocate and share their experience was only possible if it was normalized within their social groups. An awareness of mental health help-seeking in peers fosters a sense of normativity and acceptance (Addis & Mahalik, 2003). Participants reported their willingness to recommend help-seeking if the subject was broached within their peer group and deemed by them to be a problem common to their peers. This belief is consistent with past studies that reported men more likely to seek help and encourage others, if this did not contravene social norms (Mahalik et al., 2007; Vogel, Wester, et al., 2007). Congruent with past research, participants were influenced by other men’s help-seeking behavior (Vogel, Wade, Wester, Larson, & Hackler, 2007) and informal health promotion by men, for men to foster mental health help-seeking as normal, was identified to be an enabler.
Although deviation from perceived social norms negatively affected the participants, the role of high-profile sportsmen’s admissions of help-seeking has been positive. For the men, sporting elite epitomized masculinity and were admired as role models. All men were able to name elite sportsmen who had disclosed mental health problems, with an admission of depression, anxiety, or dependency by these men assisted in normalizing help-seeking. For example, if high-paid professional footballers sought help for mental health, they were exemplars for other men, and the use of high-profile sportsmen who experience mental health issues will contribute to changing the social norms around help-seeking.
The role of a significant other was reported by all men in this study as an influence on help-seeking and this result is also consistent with past research that reveals the role a significant other plays in encouraging men’s help-seeking decisions (Jarrett, Bellamy, & Adeyemi, 2007; Vogel, Wade, et al., 2007). The significant others in this study were female: wife, partner, close girlfriend, mother as reported in other research (Cusack, Deane, Wilson, & Ciarrochi, 2004; Seymour-Smith, Wetherell, & Phoenix, 2002).
Although the impetus was provided, help-seeking was not immediate for the participants. The men acknowledged their reluctance until a chronic or acute precipitating event forced a decision. For some it took a relationship breakdown, for others a demand for improvement in functioning. Seymour-Smith et al. (2002) reported women (significant other/partners) played a pivotal role in facilitating men’s access to help-seeking. This theme was consistent in the current study with participants trusting their problem would “just sort itself out” (Max) or “if I could have found another way to cope, I would have just kept going along, going along” (Paul). The men in the current study all conceded that while it may not have been their choice at first, all had benefited from couples or individual therapy and were grateful for the encouragement. Arnold summarized the men’s admission—“in retrospect, I should have gone years ago.”
General practitioners play a pivotal role as “gate-keepers” to mental health support and are therefore a key enabler. The men had differing experiences with their GPs and for some, the referral appointment delivered relief and a way forward. In contrast, for other participants the GP was less understanding and did not facilitate an opportunity for further assistance. The role a GP plays in the initial help-seeking decision is crucial given that men are reluctant to present at surgeries for any health concerns (Jarrett et al., 2007). Men visit doctors infrequently, consult for short periods, and generally delay help-seeking until late-illness (Andrology Australia, 2010); and therefore, it is critical for the initial contact with the GP to be positive and as necessary provide a potential pathway to a mental health professional. Nevertheless, some participants claimed the GP dismissed or downplayed their concerns, offering medication to alleviate physical symptoms rather than also taking into account their psychological needs.
The men in the current study reported feeling awkward or embarrassed to disclose their concerns. Men are reluctant to discuss sensitive problems, particularly mental health and sexual dysfunction (Andrology Australia, 2010). Wrigley, Jackson, Judd, and Komiti (2005) reported some men experienced discomfort in consulting a GP for mental health either due to embarrassment or the belief that their GP was an inappropriate source of help. This was evident in the narratives of this study’s participants.
The GPs’ attitudes and values informed their practice and impacted on the participants decisions. For one participant, a clinic that specialized in same-sex issues enabled him to seek assistance for all his health concerns and this played an important enabler for him to recognize and seek treatment without fear of stigma or embarrassment. The GPs and other practitioners in the clinic understood his same-sex issues, whereas Brent’s experience of his GPs assumption he was heterosexual delayed his help-seeking. Ogrodniczuk and Oliffe (2010) caution that GPs’ explicit values and biases may also influence potential or successive help-seeking in men.
Men in the current study were unfamiliar with the role a GP played in mental health help-seeking or if alternative pathways to counseling were available. This was consistent with past research, finding men’s primary care source as GPs and unfamiliarity of alternatives. Greater collaboration between multiple disciplines is needed to improve men’s knowledge of and subsequent engagement with mental health help-seeking options (Smith, Braunack-Mayer, & Wittert, 2006). Doctors and health professionals working collaboratively is essential for improving outcomes for patients, particularly as GPs are the “gatekeepers” to specialist referral (Fredheim, Danbolt, Haavet, Kjonsberg, & Lien, 2011).
Other men reported the consultation with their GP as a positive experience, enabling a recommendation and/or referral to a suitable counselor. There was relief for these men with the positive experience revealing pathways to assistance. This supports Cusack et al.’s (2004) finding that GPs frequently influenced the men’s help-seeking decisions. The results support the GP consultation as either an enabling or inhibiting factor for the participants. With men’s reluctance to seek help well documented, a positive initial GP consultation was crucial to positive mental health management.
The men were asked to describe the help-seeking pathway and whether it included the use of online resources. Most reported they had made use of websites postreferral more than prior to visiting either their GP or counselor. The most notable website for the men in the current study was beyondblue; however, the men believed the content not relevant to their particular circumstances. All men were of the opinion that beyondblue promoted depression awareness yet believed their problem to be an alternative diagnosis. The men were not aware of the other resources available online. Although self-help is readily available, men are not guaranteed to use it (Hausner et al., 2008). Past research suggests the use of the internet for help-seeking in mental health is low in Australia (Burns, Davenport, Durkin, Luscombe, & Hickie, 2010).
Online information was used to reinforce participants’ treatment decisions once an appointment was made. Online searches were employed by the participants to consider their counselors’ credentials and treatment expertise. Other men reported online forums helpful once they had received a diagnosis. One participant remarked that chatting online with men with similar conditions had a normalizing effect for him. Being able to share experiences and impart knowledge from his treatment with other men reduced his sense of isolation. For this participant the role of normalization and Internet access brought a positive outcome. Oh, Jorm, and Wright (2009) investigated perceived helpfulness of online mental health information. When presented with vignettes and treatment options, the participants preferred counseling as a method of mental health assistance before Internet and books. Consistent with the men in this study, websites were considered less helpful by the respondents for someone with depression than other mental illnesses (Oh et al., 2009). The study’s recommendations included marketing the “anonymity and easy access” of websites for people experiencing mental health distress (Oh et al., 2009).
Misconceptions of mental health definitions and treatment were a salient theme to emerge a posteriori. All participants agreed that their diagnosis and subsequent treatment were more positive experiences than anticipated, and had the men not held negative stereotypes, assistance would have been sought earlier with the disorder having less impact on day-to-day living. The preconceived ideas of counseling included laying on chaise lounges and having a psychiatrist ask countless questions. McKelley’s (2007) examination of men’s resistance to seeking help offers a similar representation of counseling practices. While in reality this may not describe the rooms, this stereotype is ubiquitous in men’s perceptions, acting as a barrier to help-seeking.
Understanding of therapy and the therapeutic process was identified as an enabler. White (2009) reports men have poor knowledge of counseling and held counselors in low regard. When asked about the initial therapy appointment, participants admitted to uneasiness due to not knowing what to expect with this fear leading to men delaying assistance seeking. For these participants, less ignorance would have been an enabler earlier in their condition. This notion was advanced by the men that more could be done to promote “typical” counseling experiences in the media. Most men suggested the media play an important role in the stereotypes and misconceptions.
Clear definition rather than ignorance on what constituted a mental illness was identified as an enabler to mental health help-seeking. Once a diagnosis had been made or clarity received from the therapist, the men were able to redefine their schemas. The men believed those with mental health issues were dangerous and a potential threat to self or others. This ideal was believed to also be media driven. Pervasive in the men’s interviews were illustrations of people with mental illness as “people hearing voices . . . jumping off bridges” (Tommy) or “walking along, talking to themselves” (Max). For the men, more common symptoms of depression, anxiety, or sexual dysfunction were far removed from these people. Although stigma and discrimination is widespread for those with a mental illness, this is thought to be due to the public being unfamiliar with the conditions. People with a mental illness are often portrayed to be dangerous and aggressive and should be avoided—a stereotype perpetrated and reinforced by the media (Zartaloudi & Madianos, 2010).
Another consequence of these misconceptions was the men’s beliefs around antidepressants and other medication to treat mental health problems. Participants were of the opinion that medication had the capacity to alter their personality. Most were resistant to a course of medication until compelled due to severity of symptoms. The men report medication being prescribed without adequate information provided and not seeing immediate benefits of medication caused some of the participants to cease taking the medication.
Factors that enable other men to seek assistance for mental health included the influence of a significant other and the effectiveness of their GP to empathize and refer. These findings have regularly been reported in past research (e.g., Norcross et al., 1996; Richards, Ryan, McCabe, Groom, & Hickie, 2004; Smith, Robertson, & Houghton, 2006). The recognition of the men’s mistaken beliefs surrounding treatment and illness definition was of particular importance. While initially these misconceptions acted as a potential barrier to help-seeking, they retrospectively became an enabler. Access to accurate information would have resulted in earlier detection and treatment of illness for the participants of the present study. With media involvement, an accurate representation of mental health may alleviate some of the perceived barriers for other men’s help-seeking. Sportsmen who embody traditional masculinity, yet reveal mental health struggles, also improve mental health stigma for men (Boman & Walker, 2010). Effective campaigns targeted at reducing stigma and changing perceptions of social norms is suggested by Mahalik et al. (2007). Evident in the current study was the importance men placed on their own social group norms. Many authors suggest a new approach to marketing or “reframing” mental health information and services to better enable men to seek mental health assistance (Jarrett et al., 2007; Vogel, Wester, et al., 2007).
Conclusion
A qualitative approach to investigate men’s help-seeking influences was adopted for this study. Men’s help-seeking behaviors appear to have not changed discernibly in 40 years with many perceived barriers are still encountered by men (Möller-Leimkühler, 2002). Little new knowledge has been uncovered in past studies, particularly with regard to enabling factors. It is anticipated the factors advanced here will provide a better understanding of enabling factors for men’s mental health-seeking.
The men in the current study were supported in their help-seeking by a significant other; in all cases except one, a woman. Most of the men’s partners or female friends had sought psychotherapeutic assistance themselves at some point. However, it was not apparent in the analysis if the female’s experience was an enabler for the men. Once the decision had been made to seek assistance, the perceived support of the GP was important for the men to progress with counseling. The men reported feelings of relief when counseling commenced as they were able to understand their illness and subsequent treatment plans. There was a functional approach adopted by the men once they had a strategy. For them a diagnosis became a way to alleviate some of the confusion surrounding their symptoms. Prior to diagnosis, there was little understanding of even common mental disorders; most men believing their problems to be physiological. The men’s misconceptions of mental illness had a significant impact on their help-seeking. These misconceptions were attributed to negative portrayals in the media. It could be posited that these ill-informed beliefs maintain and reinforce the stigma associated with mental illness, acting as a barrier to help-seeking.
All men observed the effectiveness of therapy, which had allowed them to see the trees instead of the forest. For the men this was significant, their illness having had devastating effects on their daily lives including their relationships. Many admitted to being in a “dark” or “confusing” place prior to treatment, and although the experience had been positive, the men admitted that opportunity to recommend to others was conditional. This centered on the men’s views of what constituted normativity within their peer group. While the participants could see opportunity to reciprocate and impart knowledge, there had to be sufficient evidence of unquestionable acceptance by other males. Denial of illness and attributing symptoms to stress and tiredness was the alternative disguise. Accurate media messages and the removal of stigma are postulated by the men to enable future help-seeking in men. The disclosure of sportsmen’s struggles with mental health issues is seen as a positive advancement and addresses these issues through creating a social norm of the action.
The importance of identifying and acting on the positive or enabling factors in men’s help-seeking cannot be underestimated. The National Male Health Policy (Department of Health and Ageing, 2010), the first in Australia, provides numerous opportunities to inform future policy. While many barriers to help-seeking are identified, it is timely to take a strengths-based approach and acknowledge enablers and positive influences. Assisting men to assist themselves in leading more meaningful and constructive lives is a priority, potentially creating role models for other’s help-seeking intentions. Improvement to men’s mental health benefits men, women, society in general, and the health of future generations.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
