Abstract
To address the understudy of health conditions and infectious diseases that are not strictly related to sexual transmission among men who have sex with men (MSM), this study examined the relative odds of 10 health conditions and two infectious diseases in a sample of MSM compared with a matched general population sample. MSM (N = 653) living mainly in Chicago were sampled through successive administrations of an Internet-based survey (2008-2010) that assessed physical and mental health, substance use, and HIV status. Propensity score matching was used to obtain a demographically comparable sample of men (N = 653) from aggregated administrations (2008-2012) of the National Survey on Drug Use and Health. Multivariate Firth logistic regressions compared the odds of ever having been diagnosed with each condition or disease, controlling for demographics, substance use, psychological distress, and HIV/AIDS status. MSM were more likely (p < .01) to have experienced: ulcers (odds ratio [OR] = 2.3), hypertension (OR = 2.1), liver disease (OR = 5.7), and sexually transmitted infections other than HIV/AIDS (OR = 8.9). Two other conditions, pneumonia and pancreatitis, as well as tuberculosis, were significant at p < .05 but below the statistical threshold used to reduce alpha error. The findings suggest that relative to non-sexual-minority men, MSM are more likely to experience a range of health conditions not specifically attributable to HIV/AIDS, sexual behavior, psychological distress, or substance use. The implications for research on the health status and provision of health care to MSM in light of the study findings are considered.
Keywords
Relative to men who identify as heterosexual and/or who do not have sex with other men, an extensive research literature has documented elevated rates of sexually transmitted infections (STIs) such as HIV/AIDS, gonorrhea, syphilis, chlamydia, and hepatitis A and B among men who self-identify as gay or bisexual as well as men who do not self-identify as such but who nevertheless have sex with other men (Centers for Disease Control and Prevention, 2013; Fenton & Imrie, 2005; Mayer, 2011). Although heterogeneous in many respects (e.g., Lert, Sitta, Bouhnik, Dray-Spira, & Spire, 2010), these groups of men are commonly and collectively referred to as men who have sex with men (MSM); a convention followed for the remainder of this article.
Other studies of MSM have reported that in addition to and closely related “syndemically” to the elevated rates of STIs (Santos et al., 2014), MSM have higher rates of psychosocial and health problems such as substance abuse (e.g., Cochran, Ackerman, Mays, & Ross, 2004; Stall, Paul, Greenwood et al., 2001; Stall & Purcell, 2000), mental illness (e.g., Bolton & Sareen, 2011; Gee, 2006; Safren, Blashill, & O’Cleirigh, 2011), childhood sexual and physical abuse (Stall, Mills, Williamson et al., 2003), homelessness (e.g., Institute of Medicine, 2011), and violent victimization (e.g., Safren, Reisner, Herrick, Mimiaga, & Stall, 2010). Considerations of the reasons underlying the higher rates for these conditions have centered on the chronic experience of stress and stigma associated with sexual minority status, a prevailing culture organized around bars and other venues such as circuit parties as primary meeting places where alcohol and other drugs are readily consumed, ready use of the Internet to connect with multiple casual sex partners, and the lack of accessible, culturally appropriate health care (Fenton & Imrie, 2005; Makadon, Mayer, & Garofalo, 2006; Sandfort, Bakker, Schellevis, & Vanwesenbeeck, 2006; Wim, Nöstlinger, & Laga, 2014). Recent research indicates these risk factors begin early in life, during or even prior to adolescence where they manifest in riskier health behaviors (e.g., smoking, drug use, dietary, and physical activity behaviors), with cumulative effects that can persist over the life course (Coker, Austin, & Schuster, 2010; Institute of Medicine, 2011).
Whereas HIV and other STIs have been the focus of studies on the health and health care needs of MSM, there have been far fewer studies of the relative prevalence of non–sexually transmitted medical health conditions such as heart disease, asthma, or hypertension (Boehmer, 2002; Snyder, 2011). This is a potentially critical barrier to gaining a more complete understanding of and providing for the overall health care needs of MSM. The psychosocial risk factors such as mental illness and substance use—including higher rates of smoking—that contribute to the higher rates of STIs among MSM also potentially increase their risk for a wide range of other medical conditions (Barnett et al., 2012; Saitz et al., 2013; Viron & Stern, 2010).
Several recent studies have attempted to address this knowledge gap by studying the comparative prevalence of non–sexually transmitted health care conditions in the LGBT population. A multiyear (2001-2008) survey using a state-based probability sample of adult Massachusetts residents assessed the relative prevalences of asthma, heart disease, diabetes, and risk for cardiovascular disease among gay, lesbian, bisexual men and women, and heterosexual participants (Conron, Mimiaga, & Landers, 2010). The study provided only limited support for the hypothesis that MSM and other sexual minorities have higher rates of general health conditions compared with nonsexual minorities. After adjusting for sociodemographic characteristics, there were no statistically significant differences by sexual orientation for diabetes and heart disease whereas all three sexual minority groups were more likely to report having had asthma. Additionally, lesbian and bisexual male participants were more likely to report multiple risks such as smoking for cardiovascular disease. Although use of a statewide probability sample meant the study was not subject to the lack of generalizability of studies that use convenience samples, the small numbers of health conditions assessed limit the scope of the findings.
Another relatively recent study assessed for a more expansive set of health conditions while also drawing from a statewide probability sample of the general population; in this instance, adult California residents (Cochran & Mays, 2007). Based on a follow-up survey of respondents to an initial survey of California households, the follow-up survey oversampled sexual minorities from the initial cohort. In addition to HIV/AIDS, the study assessed for the presence of 13 other health conditions such as asthma, cancer, hypertension, arthritis, and liver disease (see Cochran & Mays, 2007, for the full list). For each health condition, multivariate logistic regression that adjusted for demographic differences was used to compare the odds of currently having that condition for gay, bisexual, and “homosexually experienced heterosexuals” in comparison with heterosexual men. In this study, participants in the sexual minority groups had higher odds of having a number of the assessed health conditions but the results varied by specific sexual minority group and HIV status. Gay men had higher odds of 4 of the 13 health conditions assessed whereas homosexually experienced heterosexuals had higher rates on 7 of the assessed health conditions. There were no significant differences for bisexual men. The statistically significant differences remained when the models were further adjusted to control for the effects of psychological distress. However, all but one of the significant findings for gay men—migraines and headaches—became nonsignificant when the analyses were restricted to HIV-negative participants. The findings for homosexually experienced heterosexuals were more robust and remained significantly higher even when excluding participants who were HIV positive.
One of the main study limitations was the low response rate (38%) of the original sample coupled with the response rate of the follow-up sample (56%). This brings into question the representativeness of the follow-up sample despite the original sample being statewide and probability based. Additionally, despite oversampling sexual minorities, there were still only small numbers in each male sexual minority subgroup surveyed: 29 bisexual, 101 gay, and 23 homosexually experienced heterosexual participants. The small numbers of male sexual minority participants are especially problematic in the context of assessing for health conditions that have low prevalence rates such as stroke in a general population sample.
A study done in the Netherlands that used data collected from a national survey also identified elevated rates of acute physical symptoms (e.g., headache, sore throat, fever, and heartburn) and a higher number of chronic health conditions measured as a count variable based on 19 possible conditions among sexual minority participants (Sandfort et al., 2006). This study too, only had small numbers of sexual minority participants (143 gay/lesbian and 90 bisexual compared with 9,278 heterosexuals) and is likely why chronic health conditions were not assessed individually and why gay men and lesbian women were combined into a single category for the analyses.
These few studies of the health conditions among sexual minorities suggest there are higher prevalence rates for some but not all health conditions with the rates and specific conditions varying by gender—although the study of sexual minority females is outside the scope of the current study, the reviewed studies included both male and female sexual minority participants—as well as by specific sexual orientation. Given the small number of studies, the different conditions studied, and the varied findings, it is not possible as yet to discern if there is a specific constellation of non–sexually transmitted conditions or diseases for which MSM are at clinically meaningful increased risk. Moreover, the small sample sizes of MSM participants have limited the study of health conditions with low general population base rates.
The current study sought to address these limitations and add to the growing knowledge base on general health conditions among MSM by comparing an Internet-survey sample of more than 600 MSM with a statistically matched general population sample to compare the prevalence rates on 10 medical health conditions and 2 infectious diseases, including STIs. This study also employed statistical methods that allow for less biased odds estimation when the probability of a positive outcome (i.e., having a health condition or infectious disease) is very low. The main study hypothesis was that MSM would have higher lifetime rates of many if not most of the health conditions and infectious diseases assessed, even after adjusting for demographics and psychosocial health risk factors such as alcohol and other substance use and psychological distress.
Method
All procedures and materials used for this study were reviewed and approved by the University of Illinois at Chicago, the Chicago Department of Public Health, and the Howard Brown Health Center Institutional Review Boards.
Participants
MSM Sample
The MSM health conditions and infectious disease data analyzed for this study were collected through an Internet-based survey done as part of a 5-year (2007-2011) prevention effort to reduce crystal methamphetamine use and promote healthier lifestyles for Chicago MSM (for details, see Swartz et al., 2008). The target population was MSM living in six contiguous communities on Chicago’s north side, which remain among the Chicago communities with the highest HIV/AIDS incidence and prevalence rates (Chicago Department of Public Health, 2013).
Three surveys were done approximately 1 year apart over the 5 years of the project to monitor epidemiological trends in substance use, HIV risk behaviors, associated mental and physical health conditions, and to assess the project’s effectiveness. However, the first survey did not include questions on physical health conditions. Hence, the data for this study came exclusively from the second (administered October 2008 through June 2009) and third (July 2010 through September 2010) surveys. Aggregating across both surveys, 924 recruits met study eligibility criteria for gender (male), age (>18), and sexual orientation (MSM) and initiated the survey. Excluding a small number of duplicate responders across survey years (<1% per year), 656 unique respondents completed the survey for a total response rate of 71% (656/924).
The 656 respondents who met eligibility criteria were non-transgendered men 18 years of age or older who self-identified as gay (88%), bisexual (11%), or as a heterosexual who had ever had sex with men (1%). The majority of the sample (63%) reported living in Chicago at the time they took the survey. Participants not living in Chicago were divided between those who lived in Chicago’s suburbs (16%) and those who lived downstate or outside Illinois (21%). Seventy-six percent of the sample was non-Hispanic White, 8% non-Hispanic Black or African American, and 10% Hispanic, with the remaining 5% Asian, Native American, or more than one race/ethnicity. The average age was 36.9 years (range = 18-75 years).
General Population Sample
To compare lifetime prevalence rates of medical health conditions and infectious diseases for the MSM sample with those of men in the general population, data from male respondents 18 years of age and older collected for the 2008 through 2012 National Survey on Drug Use and Health (NSDUH) were used. Implemented annually since 1991, the NSDUH collects substance use and other health-related information on the noninstitutionalized U.S. population (United States Department of Human Services [USDHHS], Substance Abuse and Mental Health Services Administration [SAMHSA], Office of Applied Studies [OAS], 2012).
A matched comparison sample was obtained from the aggregated NSDUH data sets by first selecting all male respondents 18 years of age and older, yielding a total of 88,973 NSDUH participants eligible for inclusion in the comparison group. Next, propensity score matching (Rosenbaum & Rubin, 1985) with nearest-neighbor matching on the NSDUH male respondents subsample and the MSM Internet survey sample was implemented using the “psmatch2” add-on for Stata (Leuven & Sianesi, 2003; StataCorp, 2012). The matching covariates included variables common to both data sets that research has identified as influencing the probability of having a health condition or infectious disease: race/ethnicity, education level, age, psychological distress, frequency of alcohol use in the past year, number of other drugs used in the past year, HIV status, and population density based on the core-based statistical area of the respondent’s main residence (Agborsangaya, Lau, Lahtinen, Cooke, & Johnson, 2012; Barnett, Mercer, Norbury, Watt, & Wyke, 2012; Dickey, Normand, Weiss, Drake, & Azeni, 2002).
These procedures matched 653 of the 656 (99%) MSM sample participants with 653 NSDUH participants, yielding an analytic sample of 1,306 cases. Table 1 reports the distributions of the demographic and other variables used for matching by study group and in aggregate and additionally includes past-year substance use for individual drug classes and alcohol. Postmatch likelihood ratio chi-square statistical comparisons of the two groups on the matching variables indicated no significant differences with the exception of HIV status. MSM survey participants were significantly more likely (likelihood ratio χ2(df = 1) = 7.9, p < .01) to report being HIV positive (18.5%) compared with the matched sample of NSDUH participants (12.9%).
Demographics, Nonspecific Psychological Distress, Alcohol and Other Drug Use, and HIV Status by Survey Sample.

Note. NSDUH = National Survey on Drug Use and Health; CBSA = Core Based Statistical Area. All figures reflect unweighted percentages. The NSDUH sample was derived using nearest-neighbor propensity score matching on the following variables: race/ethnicity, age, education, population density, serious mental illness, HIV status, frequency of past-year alcohol use, and number of illicit drugs used in the past year. All tests of statistical significance are based on likelihood-ratio chi-square tests.
Population density is based on CBSAs, which are used by the U.S. Office of Management and Budget to define population centers in the United States.
Nonspecific psychological distress was assessed by the K6 screening scale. Scores greater than or equal to 13 indicate a high level of psychological distress and a likely serious mental illness.
p < .05. **p < .01. ***p < .001; NS = not significant.
Because of missing data on covariates and health conditions, the sample size in the multivariate analyses for 8 of the 10 medical health conditions and the 2 infectious diseases assessed ranged from 1,299 to 1,303. For the remaining two medical health conditions—pancreatitis and pneumonia—a subsample was used for the analyses. These two conditions were assessed at only the last administration of the Internet survey. This reduced the available number of MSM with information on these conditions to 254 participants. Consequently, the multivariate models of pancreatitis and pneumonia were restricted to this subgroup of MSM and their corresponding matched NSDUH participants, yielding a total of 508 cases for these analyses.
Measures
Demographics
Although preliminary analysis identified that the propensity score matching yielded groups statistically comparable on the demographic covariates used for the matching (Table 1), these variables were retained as covariates in the multivariate models as a further control and to directly assess for their effects on having each health condition or infectious disease. The sole exception was that population density was excluded due to the restricted variability on that measure whereby the large majority of participants (96%) lived in a CBSA with a population of greater than 1 million. The demographic covariates included in the multivariate models were race/ethnicity, age in years recoded into four categories, and education level.
Nonspecific Psychological Distress (NPD)
On both surveys, NPD was assessed using the K6 screening scale (Kessler et al., 2002). The K6 was designed to assess symptoms of NPD associated with a broad range of psychiatric conditions. The six questions deal with anxiety and depression experienced in the past year during the month when respondents indicate their symptoms were the worst. Participants report how often they experienced each symptom. Response options range from “none of the time,” scored as 0, to “all of the time,” scored as 4, yielding summed scores that range from 0 to 24. Studies based on national samples indicate scores of 13 and higher indicate severe psychological distress and have a strong association with a serious mental illness (Kessler et al., 2003). The threshold of 13 or higher was used to indicate NPD for both the MSM as well as the NSDUH comparison group. Validation studies of the K6 have indicated it has high validity and internal consistency when compared with longer, clinician-administered diagnostic interviews (Andrews & Slade, 2001; Kessler et al., 2002).
Alcohol and Other Drug Use
Past-year use of alcohol was assessed by classifying participants as being in one of the following three mutually exclusive categories based on self-reported days of alcohol use in the past year: no or less than weekly use; weekly but less than daily use; and daily use. As the use of drugs other than alcohol is much less common there are far fewer daily or weekly users. Therefore, instead of using number of days for drug use, the number of drugs used in the past year was used to assess the level of drug use. The number of drugs self-reported as used during the past year was first summed based on the following list of drugs and drug classes: marijuana, cocaine (any form), hallucinogens, analgesics, heroin, tranquilizers, and methamphetamine. The total number of drugs used was then collapsed into one of three categories: none, one, or two or more.
HIV Status
Both surveys assessed self-reported HIV status with a single question included among the questions on other health conditions. For the analysis, responses were collapsed into one of two categories: yes and no/don’t know. This variable was also used for propensity score matching but, as already indicated, was the one variable where the two groups were not statistically equivalent (Table 1). Therefore, HIV status was retained in the multivariate models because of its important potential health consequences, to control for the difference in HIV status between the two study groups, to directly assess for its main effects on each health condition or infectious disease, and to test for interactions with other model covariates including survey group.
Health Conditions and Infectious Diseases
For the MSM Internet survey, questions on lifetime health conditions and infectious diseases were taken from the chronic conditions section of the World Mental Health version of the Composite International Diagnostic Interview Schedule (Kessler & Üstün, 2004). In the 2008-2009 survey, the included questions covered 22 such conditions and infectious diseases. In the 2010 survey, 2 questions were added to assess for pneumonia and pancreatitis. The NSDUH questionnaire includes questions on the lifetime prevalence of 14 medical health conditions and infectious diseases, 13 of which overlapped with those on the MSM survey.
In two instances, responses to several questions were collapsed to provide closer comparability. As the NSDUH survey asks about any STI inclusive of gonorrhea, Chlamydia, herpes, and syphilis, responses to these separate questions on the MSM survey were collapsed into a comparable single variable to reflect infection with any STI other than HIV. Likewise, the responses to separate MSM survey questions on different forms of hepatitis were collapsed with a question on other liver diseases such as cirrhosis and jaundice into a single response indicating any type of liver disease. The NSDUH survey asks separate questions on hepatitis (any form) and cirrhosis. These were combined into a single indicator of liver disease.
In one other instance, the responses for a condition were retained and included in the analyses even though the questions were not strictly comparable across surveys. The NSDUH survey asks about bronchitis whereas the MSM survey asks about chronic obstructive pulmonary disease (COPD), of which bronchitis is one of the main component diseases, emphysema being the other (Barnes, 2000). Because there was considerable albeit not perfect overlap, a variable that reflected either COPD (MSM survey) or bronchitis (NSDUH) to represent chronic lung disease was retained with the caveat that this operationalization difference could affect the outcome.
The 11 medical health conditions included in the bivariate analyses were stroke, heart disease, hypertension, asthma, chronic lung disease, lung cancer, pneumonia, diabetes, ulcers, pancreatitis, and liver problems. The two infectious diseases assessed were tuberculosis and STIs other than HIV. Because no NSDUH participant reported ever having lung cancer (see Table 2), this condition could not be included in the multivariate models because it was perfectly predicted by study group. This reduced the set of health conditions analyzed in the multivariate analyses to 10 conditions.
Bivariate Comparisons of the Lifetime Prevalences of Medical Health Conditions and Infectious Diseases by Survey Sample.
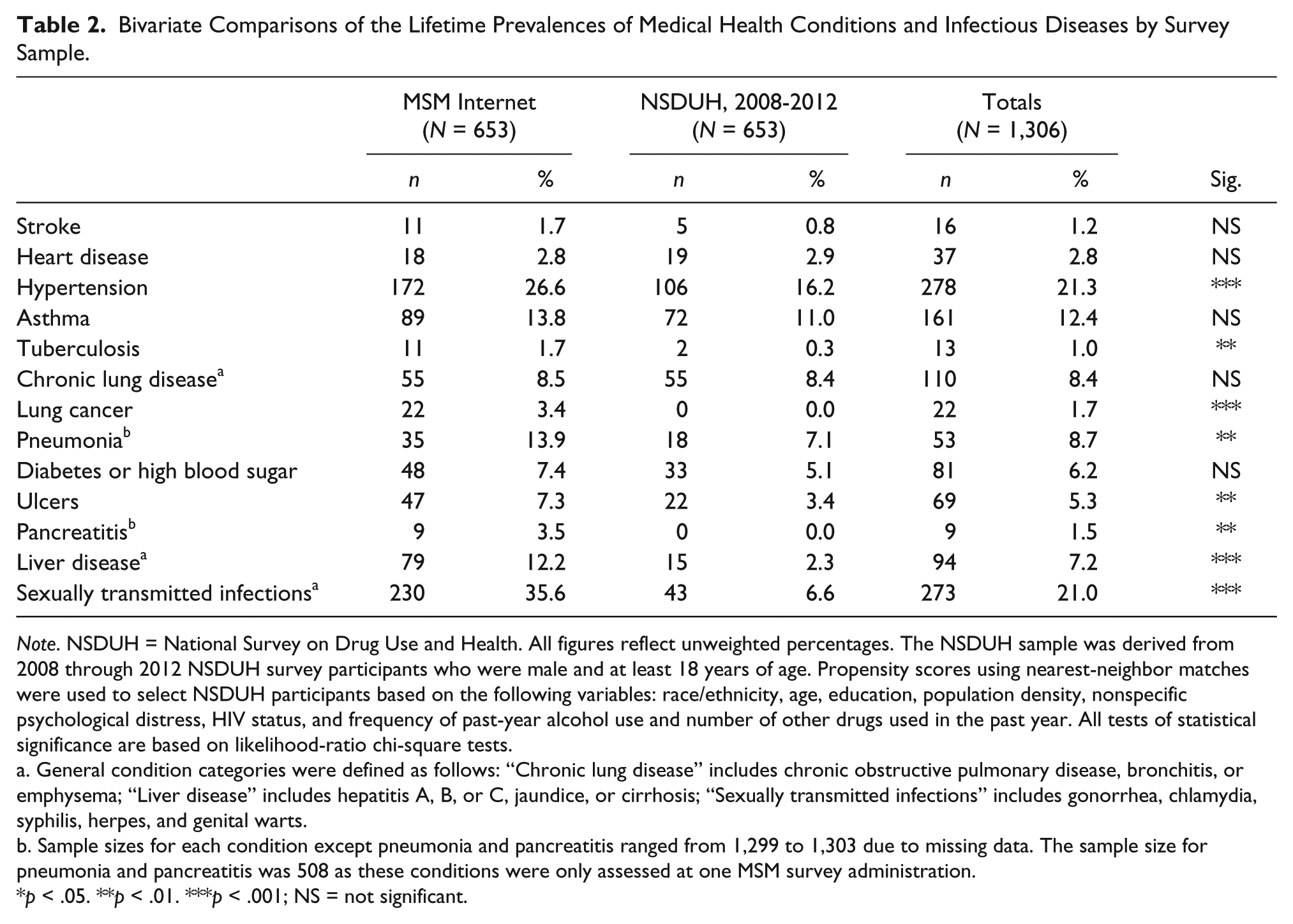
Note. NSDUH = National Survey on Drug Use and Health. All figures reflect unweighted percentages. The NSDUH sample was derived from 2008 through 2012 NSDUH survey participants who were male and at least 18 years of age. Propensity scores using nearest-neighbor matches were used to select NSDUH participants based on the following variables: race/ethnicity, age, education, population density, nonspecific psychological distress, HIV status, and frequency of past-year alcohol use and number of other drugs used in the past year. All tests of statistical significance are based on likelihood-ratio chi-square tests.
General condition categories were defined as follows: “Chronic lung disease” includes chronic obstructive pulmonary disease, bronchitis, or emphysema; “Liver disease” includes hepatitis A, B, or C, jaundice, or cirrhosis; “Sexually transmitted infections” includes gonorrhea, chlamydia, syphilis, herpes, and genital warts.
Sample sizes for each condition except pneumonia and pancreatitis ranged from 1,299 to 1,303 due to missing data. The sample size for pneumonia and pancreatitis was 508 as these conditions were only assessed at one MSM survey administration.
p < .05. **p < .01. ***p < .001; NS = not significant.
Procedures
NSDUH Survey Data
Detailed information on the sampling design, survey protocol, response rate, questionnaire, public use data set, and codebook for the 2008 through 2012 NSDUH is available at the Inter-University Consortium for Political and Social Research (ICPSR) at the University of Michigan website (United States Department of Health and Human Services, 2008, 2009, 2010, 2011, 2012). The public use survey data set was downloaded in Stata format (StataCorp, 2012) for each annual administration of the NSDUH from the ICPSR website, concatenated the data sets, and then extracted the subset of variables needed for the analyses.
MSM Survey Data
Each administration of the MSM Internet survey was advertised through banner ads on the websites of the community-based provider agencies that collaborated on the prevention study, through email announcements to those who signed up to receive them on the project website, and through print advertisements placed in magazines and newspapers that target the Chicago LGBT community. The surveys were administered using the facilities of the Survey Monkey website.
Before beginning the survey, participants electronically signed an informed consent after which they were directed to the survey questions. Data collection lasted approximately 6 months each cycle with the survey remaining available until the target sample size had been reached. On conclusion of data collection, an electronic file containing the survey data in Excel format was downloaded and converted to Stata for analysis. Data for each survey administration were screened for out-of-range responses, missing values, and completeness. Because of the data checking routines available with electronically administered surveys to enforce skip patterns and preclude invalid responses, few such errors were detected during preliminary screening.
Prior to analyses, the data sets for each administration of the MSM survey were concatenated into a single data set, and the variables to be used in the analyses renamed and recoded to be consistent with the naming and coding conventions used in the NSDUH survey. The MSM and NSDUH data sets were then combined, propensity scores obtained, and the matched cases selected into the final analytic data set.
Analyses
All analyses were conducted using Stata version 12.0 (StataCorp, 2012). Prior to running the multivariate logistic models, simple bivariate analyses were run and likelihood ratios were used to compare the unadjusted prevalence rates of each health condition and infectious disease by comparison group. For the multivariate analyses Firth penalized likelihood logistic regression models were used to determine the odds of having each health condition or infectious disease (Firth, 1993). Compared with the maximum likelihood estimation algorithm used in ordinary logistic regression, Firth’s penalized likelihood algorithm more accurately estimates the odds of binary outcomes when the outcome of interest is rare as is the case with a number of the health conditions assessed in this study such as stroke, heart disease, and lung cancer. Moreover, Firth penalized likelihood logistic regression models provide estimates for the effects of model predictors when there is “complete or quasi-separation” as when one category of a predictor perfectly or nearly perfectly predicts the dependent variable (Allison, 2012; King & Zeng, 2001).
The multivariate models were first run using only main effects for each covariate. If study group (MSM compared with a general population sample) was a significant predictor in the model, interaction terms were added for it and any other significant predictors and the model rerun to test for interaction effects. As no significant interaction effects were obtained, only the main effects models are presented. Postestimation, models were assessed for misspecification error using the Stata “linktest” procedure (StataCorp, 2012). Model effect sizes (i.e., pseudo-R2) were estimated using Tjur’s (2009) recommendation for a “coefficient of determination.” This effect size statistic is also assessed postestimation and is calculated as the difference between the mean predicted probabilities of having a given condition for observed cases and noncases and tested for significance using the t-statistic. To reduce the experiment-wide alpha error rate (i.e., inflated Type I error attributable to running multiple statistical tests), a conservative alpha level of p < .01 was adopted and only those results that were statistically significant at this level or higher are emphasized. However, given the exploratory nature of the study, the included tables indicate those findings that were significant at the p < .05 level. These findings are briefly discussed with the caveat that they are statistically provisional only.
Results
Results for the bivariate comparisons of the unadjusted lifetime prevalence rates for the 11 assessed health conditions and two infectious diseases (including the disease class of STIs) are reported in Table 2. Compared with men in the matched general population sample, men in the MSM sample had significantly higher (p < .01 or lower) lifetime prevalences on 7 of the 13 conditions and diseases assessed: hypertension, tuberculosis, pneumonia, ulcers, pancreatitis, liver disease, and STIs. The largest differences were for STIs (35.6% MSM vs. 6.6% for men in the matched NSDUH sample), hypertension (26.6% vs. 16.2%), pneumonia (14.2% vs. 6.6%), liver disease (12.2% vs. 2.3%), and lung cancer (3.4% vs. 0%). In contrast, there were no statistically significant findings in the direction of men in the matched general population sample having a higher lifetime prevalence rate for any condition.
Table 3 presents the adjusted odds ratios of having these same conditions for each survey sample controlling for demographics, alcohol and other drug use, HIV status, and severe psychological distress. In comparison to the bivariate models there were fewer statistically significant differences between the MSM and comparison samples after adjusting for these covariates. Nevertheless, significant differences remained and were again all in the direction of MSM having increased odds of having the condition or infectious disease. Of the health conditions and infectious diseases assessed in the multivariate models—excluding lung cancer, which was unreported in the MSM sample—four met the more stringent p < .01 significance threshold: hypertension (odds ratio [OR] = 2.1, confidence interval [CI] = 1.5-2.7); ulcers (OR = 2.3, CI = 1.4-3.9); liver disease (OR = 5.7, CI = 3.2-10.2); and STIs (OR = 8.9, CI = 6.9-12.9). Additionally, the odds of having tuberculosis (OR = 4.4, CI = 1.1-17.4), pneumonia (OR = 2.1, CI = 1.1-3.7), and pancreatitis (OR = 16.6, CI = 1.1-271.6) were significant at the more liberal p < .05 threshold, suggesting the possibility the odds of having these conditions could also be elevated among MSM although the lower bounds of the confidence intervals (OR = 1.1) indicated potentially very small effects owing to group membership. In no instance were the odds of having a condition or infectious disease significantly elevated among men in the general population sample.
Odds Ratios for Medical Health Conditions and Infectious Diseases.
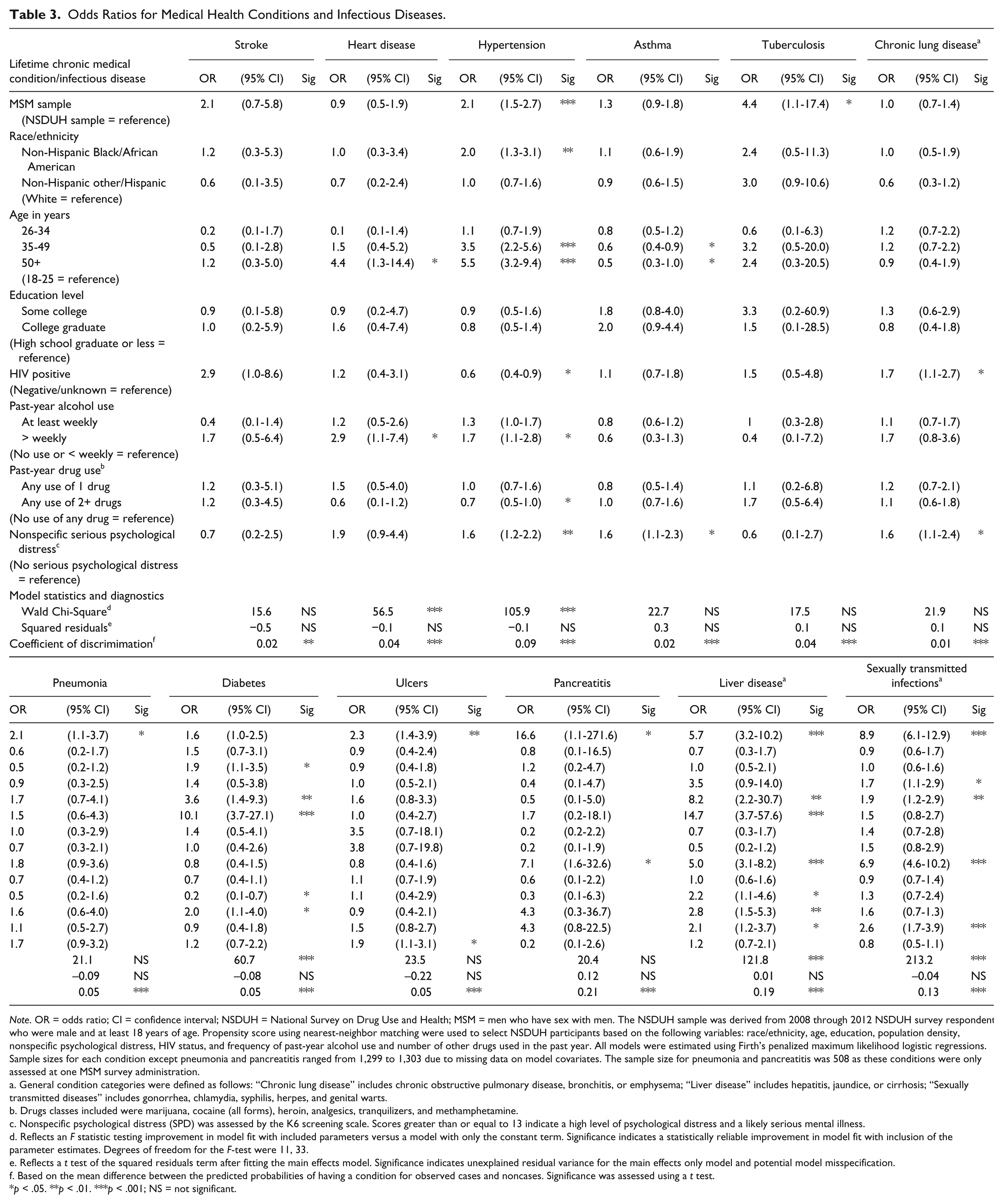
Note. OR = odds ratio; CI = confidence interval; NSDUH = National Survey on Drug Use and Health; MSM = men who have sex with men. The NSDUH sample was derived from 2008 through 2012 NSDUH survey respondents who were male and at least 18 years of age. Propensity score using nearest-neighbor matching were used to select NSDUH participants based on the following variables: race/ethnicity, age, education, population density, nonspecific psychological distress, HIV status, and frequency of past-year alcohol use and number of other drugs used in the past year. All models were estimated using Firth’s penalized maximum likelihood logistic regressions. Sample sizes for each condition except pneumonia and pancreatitis ranged from 1,299 to 1,303 due to missing data on model covariates. The sample size for pneumonia and pancreatitis was 508 as these conditions were only assessed at one MSM survey administration.
General condition categories were defined as follows: “Chronic lung disease” includes chronic obstructive pulmonary disease, bronchitis, or emphysema; “Liver disease” includes hepatitis, jaundice, or cirrhosis; “Sexually transmitted diseases” includes gonorrhea, chlamydia, syphilis, herpes, and genital warts.
Drugs classes included were marijuana, cocaine (all forms), heroin, analgesics, tranquilizers, and methamphetamine.
Nonspecific psychological distress (SPD) was assessed by the K6 screening scale. Scores greater than or equal to 13 indicate a high level of psychological distress and a likely serious mental illness.
Reflects an F statistic testing improvement in model fit with included parameters versus a model with only the constant term. Significance indicates a statistically reliable improvement in model fit with inclusion of the parameter estimates. Degrees of freedom for the F-test were 11, 33.
Reflects a t test of the squared residuals term after fitting the main effects model. Significance indicates unexplained residual variance for the main effects only model and potential model misspecification.
Based on the mean difference between the predicted probabilities of having a condition for observed cases and noncases. Significance was assessed using a t test.
p < .05. **p < .01. ***p < .001; NS = not significant.
Apart from these findings, there did not appear to be any striking pattern for other model covariates. Therefore, these results are only briefly considered given they were not a focus of the study. Race/ethnicity was significant only for hypertension with African American/Blacks having higher odds relative to Whites (OR = 2.0, CI = 1.3-3.1). Perhaps more surprising is that HIV status was significantly associated with higher odds for a single health condition (liver disease; OR = 5.0, CI = 3.1-8.2) and for STIs (OR = 6.9, CI = 4.6-10.2). Increasing age was associated with hypertension (OR = 3.5, CI = 2.2-5.6 for 35- to 49-year-olds; OR = 5.5, CI = 3.2-9.4 for 50 years of age and older), diabetes (OR = 3.6, CI = 1.4-9.3 for 35- to 49-year-olds; OR = 10.1, CI = 3.7-27.1 for 50 years of age and older), and liver disease (OR = 8.2, CI = 2.2-30.7 for 35- to 49-year-olds; OR = 14.7, CI = 3.7-57.6 for 50 years of age and older). Being between the ages of 35 and 49 was associated with a higher rate of STIs (OR = 1.9, CI = 1.2-2.9). However, age was not, as had been expected, associated with stroke, heart disease, or chronic lung disease. Education level and past-year alcohol use were not significant in any model at p < .01 and psychological distress was only significantly associated with an increased risk for hypertension (OR = 1.6, CI = 1.2-2.2). Use of any two drugs other than alcohol was significantly associated with an increased risk for STIs (OR = 2.6, CI = 1.7-3.9) and use of a single drug was significantly associated with an increased risk for liver disease (OR = 2.8, CI = 1.5-5.3).
Discussion
The present study provides some support for the main hypothesis that MSM are at increased risk for health conditions and infectious diseases beyond those that are related to sexual behavior. After statistically controlling for demographics, substance use, HIV status, and psychological distress, there were elevated rates for three health conditions: hypertension, ulcers, and liver disease. In addition, consistent with a large body of past research, MSM were at elevated risk for STIs. Using a more liberal alpha level that is subject to a greater likelihood of a Type I error, the sample of MSM also had elevated rates of tuberculosis, pneumonia, and pancreatitis. Moreover, in both the bivariate and multivariate models there were no significantly higher rates for any assessed health condition or infectious disease for the comparison group of men in the general population sample.
Because there are very few studies of non–sexually transmitted health conditions and infectious diseases in MSM, there is little relevant research context against which these findings can be compared. All the studies reviewed in the introduction that have studied this issue have had results identifying elevated rates for some health conditions or the summed number of health conditions reported. However, differences in the populations sampled, the specific conditions studied, and the differentiation among gay, bisexual, and homosexually experienced heterosexual men makes direct comparison this study’s findings with those of prior findings difficult. At present, this study and the reviewed studies suggest MSM are at a modestly increased risk for some medical conditions but that there is no single health condition or infectious disease for which MSM are at especially high risk beyond those that are sexually transmitted including hepatitis. This study therefore supports that STIs including HIV are the biggest health concerns among MSM above and beyond the normal health concerns experienced by all men regardless of sexual orientation.
It is also important to note that by statistically controlling for substance use, HIV status, and psychological distress, the analyses effectively removed differences between MSM and non-MSM directly associated with these conditions/issues. However, all of these conditions/issues are associated with higher risk for having a chronic medical problem. To the extent that rates of these conditions/issues are more prevalent among MSM, which numerous studies suggest is the case (Safren et al., 2010; Stall & Purcell, 2000), adjusting for these covariates could have, in effect, resulted in underestimating the differences in population prevalence and degree of risk for the assessed chronic medical conditions.
One possible explanation for these findings is that at least some of the psychosocial health issues that place men at more immediate risk for HIV/AIDS and other STIs (e.g., alcohol and other substance use, psychological distress and mental illness) might not have immediate effects on health conditions such as heart or liver disease. In these instances, the consequences of the psychosocial issues would be better understood as cumulative, only becoming manifest later in life. If this is true, it could be that it is chiefly older MSM that have the highest relative risk for many of the health conditions assessed in this (and other) studies in comparison to older nonsexual minority men and that there are few such differences among younger MSM. This suggests that studies that can evaluate the longitudinal effects of substance use and mental health problems might reveal more substantial health differences.
Owing to important study limitations, however, these findings are not definitive and further research in this understudied area is clearly necessary. This sample of MSM used for this study is a convenience sample and not representative of all MSM. The main problem with using a general population sample to study health issues among MSM, however, is that there are few nationally representative studies that include questions on sexual orientation although this appears to be changing. Even in general population samples that do include questions on sexual orientation and practices, unless there is oversampling of sexual minorities, the small numbers obtained make it difficult to model health conditions with low base rates. Hence, although lacking broad generalizability, convenience samples such as the one used here remain one of the few ways to obtain adequate numbers of sexual minority men to statistically model these sometimes rarely occurring conditions.
Another study limitation was the general population sample used as the comparison group. It is very likely that some percentage of the comparison sample were MSM although if population rates hold, this would include only about 3% to 4% of the participants in the comparison sample (Gates & Newport, 2012). However, given some of the matching criteria used to obtain the sample (living in a metropolitan statistical area where there are greater than 1 million people, relatively high HIV rate, relatively high rate of psychological distress, etc.) it is likely that the comparison group had a higher proportion of MSM than would be expected with simple random sampling. This would mean that the comparison group was not as distinct from the MSM sample in terms of sexual identity and behavior as implied, which would in turn reduce the likelihood of finding statistically significant differences. This would make the study estimates of the increased odds of having a given health condition or infectious disease very conservative.
To explore the potential effects that comparison sample selection criteria had on the findings, the propensity score matching was rerun to select a matched sample from among NSDUH male participants 18 years of age and older who were married or had ever been married. Given that marriage among gay and bisexual men was still very rare during the period over which the NSDUH surveys were administered, sampling this way would reduce but not eliminate the proportion of the comparison group that was MSM but unknown as such. The multivariate regressions were then rerun against this second matched general population sample of men to see if more health conditions or infectious diseases reached statistical significance. These models reproduced the same significant conditions as those presented with the exception that MSM now had significantly higher odds of diabetes and pneumonia using the more stringent alpha level of p < .01. This reanalysis provides some evidence the findings are conservative in terms of the number of conditions that were statistically significant. Until general population health studies routinely include questions on sexual orientation and behavior and oversample sexual minorities, there will be a limited ability to explore these issues with improved methodological rigor and generalizability.
Another limitation is that men who identified as gay were combined with men who identified as bisexual and with those who identified as heterosexual but reported having sex with men. Research suggests that these groups might have different health risks (Cochran & Mays, 2007). The data on health conditions including HIV status were self-reported for both samples. This could mean that the actual prevalence rates were either over- or underreported; some participants might not have been aware they had a given condition while others could be aware but chose to not fully disclose their complete health status. It would be ideal to have study participants have full medical exams and histories conducted by a health professional but samples drawn from health clinics and private practices where such data would be available are also unrepresentative of the general population of MSM and likely have higher rates of health conditions (i.e., Berkson’s fallacy). And last, the list of health conditions and infectious diseases was not comprehensive; some related but distinct conditions such as different forms of hepatitis and STIs were aggregated. This was mainly out of necessity to be consistent with the categories in the national health survey but reflects a loss of information about health conditions that are different in terms of pathology and epidemiology.
These limitations notwithstanding, this area of research deserves further study with larger, representative, population-based samples polled on a larger number of conditions (see also Mayer, Bradford, Makadon et al., 2008). In particular, studies of older MSM who might be most at risk for higher relative rates of health conditions owing to the cumulative effects of psychosocial risk factors over the life course are needed. At the very least, considerations and study of the health care needs of MSM should be broadened beyond illnesses related mainly to sexual activity, as prevalent and as important as these are.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research and/or authorship of this article: Funding for the Crystal Prevent Project and Internet survey of MSM was provided through a grant from the Chicago Department of Public Health (Grant #14357).
