Abstract
Background:
Acute compartment syndrome (ACS) is a limb-threatening complication of pediatric tibial tubercle fractures. Despite its severity, the incidence of ACS in pediatric cases has been largely unexplored.
Purpose:
We sought to examine the incidence and risk factors of ACS and associated fasciotomies in pediatric patients with tibial tubercle fractures.
Methods:
We conducted a retrospective cohort study using data from the Pediatric Health Information System, a comprehensive inpatient and outpatient nationwide database. Inclusion criteria specified patients 18 years of age or younger with tibial tubercle fracture (International Classification of Disease, 10th Revision (ICD-10) diagnosis code, S82.151-156) between October 1, 2015, and June 30, 2023. Exclusion criteria were patients with a positive hematologic or immunologic flag and patients with a positive congenital or genetic defect flag. Patients with tibial tubercle fractures were stratified into 3 categories: (1) patients with a diagnosis code for ACS and/or a fasciotomy procedure code; (2) patients with a diagnosis code for ACS and a fasciotomy code; and (3) patients exclusively with a fasciotomy procedure code.
Results:
Of the 6830 included patients with tibial tubercle fractures, 4% had a code for ACS and/or fasciotomy, 1% had a code for ACS and a procedure code for fasciotomy, and 2.9% had a code for fasciotomy only. Univariate analysis revealed that older and male patients had higher rates of ACS and fasciotomies without any corresponding diagnosis of ACS, compared to their counterparts; White patients had higher rates of ACS than patients of other races. Multivariate analysis showed that age was the only significant predictor of ACS across all groups.
Conclusion:
This retrospective database study suggests that ACS is a rare complication of pediatric tibial tubercle fractures and that fasciotomies without any evidence of ACS—interpreted as prophylactic fasciotomies—occur at a higher rate than formally diagnosed ACS.
Level of Evidence:
Level IV: Retrospective Cohort Study.
Introduction
Tibial tubercle fractures are relatively uncommon and, until recently, had only been described in small-volume case reports. The reported incidence of these fractures ranges from 0.4% to 2.7% of all pediatric fractures, although incidence appears to be rising with increased participation in youth athletics.1-5 The primary mechanism of this fracture is either forceful knee flexion against a contracted quadriceps or the contraction of the quadriceps while leg extension is resisted.6,7
The overall complication rate in pediatric tibial tubercle fracture is around 23%; the most common complication is implant removal due to bursitis, occurring in 56% of cases. 8 Other common complications include refracture, ligament, and tendon injuries in the knee, and acute compartment syndrome (ACS).8,9 Considering its limb-threatening severity, we chose to focus on ACS for the purposes of this study.
Reported incidence of ACS in pediatric patients with tibial tubercle fracture ranges from 2% to 21%.2,8,10 Existing data mostly stems from case reports and meta-analyses; incidence and predictors of ACS in pediatric patients with tibial tubercle fracture have largely been unexplored. The etiology of ACS in these cases is theorized to be related to injury of the anterior tibial recurrent artery. 11 An extensive body of research on ACS in adults highlights the importance of early diagnosis as well as emergent fasciotomy to reduce severe pressure in the affected muscle compartment.12-15 Delayed fasciotomy is associated with a higher risk of muscle necrosis, infection, and amputation.6,16 Thus, it is important to thoroughly investigate ACS in the pediatric population as well.
The current study aimed to determine (1) the incidence of ACS and associated fasciotomies in pediatric patients with tubercle fractures in a large-scale dataset and (2) the risk factors for the development of ACS and fasciotomies in these patients through univariate and multivariate analyses.
Methods
The Pediatric Health Information System is a robust comparative pediatric database from the Children’s Hospital Association (Lenexa, KS, USA) that collects inpatient, observation, ambulatory surgery, and emergency department data from approximately 50 pediatric hospitals nationwide (https://www.childrenshospitals.org/content/analytics/product-program/pediatric-health-information-system). In this study, this dataset was utilized to identify patients and assess rates of ACS via International Classification of Disease, 10th Revision (ICD-10) code, and Current Procedural Terminology (CPT) codes (see Appendix). The dataset included patient age, sex, race, ethnicity, insurance status, admission date, and ICD-10 and CPT codes. IRB approval was not required, as this study used de-identified patient information collected from a publicly available database.
This retrospective cohort study included all patients ≤18 years of age who had an ICD-10 diagnosis code for tibial tubercle fracture (S82.151-156) between October 1, 2015, and June 30, 2023. Exclusion criteria were patients with a positive hematologic or immunologic flag, as defined by patients with an ICD-10 code in the following categories: hereditary anemias, aplastic anemias, hereditary immunodeficiency, coagulation/hemorrhagic, leukopenia, hemophagocytic syndromes, sarcoidosis, acquired immunodeficiency, polyarteritis nodosa and related conditions, diffuse diseases of connective tissue, or other transplantation; and patients with a positive congenital or genetic defect flag, as defined by patients with an ICD-10 code in the following categories: chromosomal anomalies; bone and joint anomalies; diaphragm and abdominal wall, or other congenital anomalies. Duplicate MRNs were then eliminated to retain only the initial patient encounter (Figure 1). ICD-10-Clinical Modification (ICD-10-CM) codes and CPT codes were used to identify individuals with ACS in our inpatient and outpatient cohorts, respectively; in addition, ICD-10-Procedure Coding System (ICD-10-PCS) were used to identify individuals who underwent a fasciotomy. Patients were then stratified into the following 3 groups: group 1, an overall compartment syndrome category, included patients with a diagnosis code for ACS and/or an associated procedure code for fasciotomy; group 2, a true compartment syndrome category, included patients with a diagnosis code for ACS and a procedure code for fasciotomy; and group 3, a fasciotomy-only category, included patients with just a fasciotomy procedure code and no apparent ACS diagnosis. Prior research used comparable categories. 17
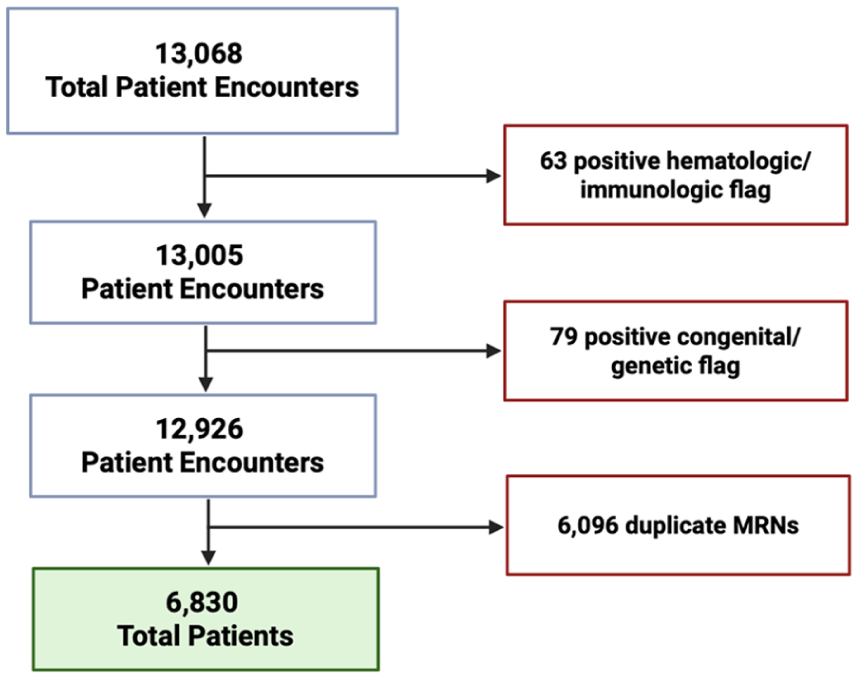
Patient cohort elimination steps.
Two-sample t-tests and χ2 tests were implemented to perform inferential univariate statistics comparing demographic differences within each of the 3 patient categories; multivariate analysis using multiple logistic regression models were used to assess predictors of ACS and fasciotomies. Statistical significance was set at P < .05. All means were reported as mean ± standard deviation. All statistical analyses were performed on RStudio (Version 2024.04.1+748; Posit Software, PBC). The STROBE checklist was used in the reporting of this study.
Results
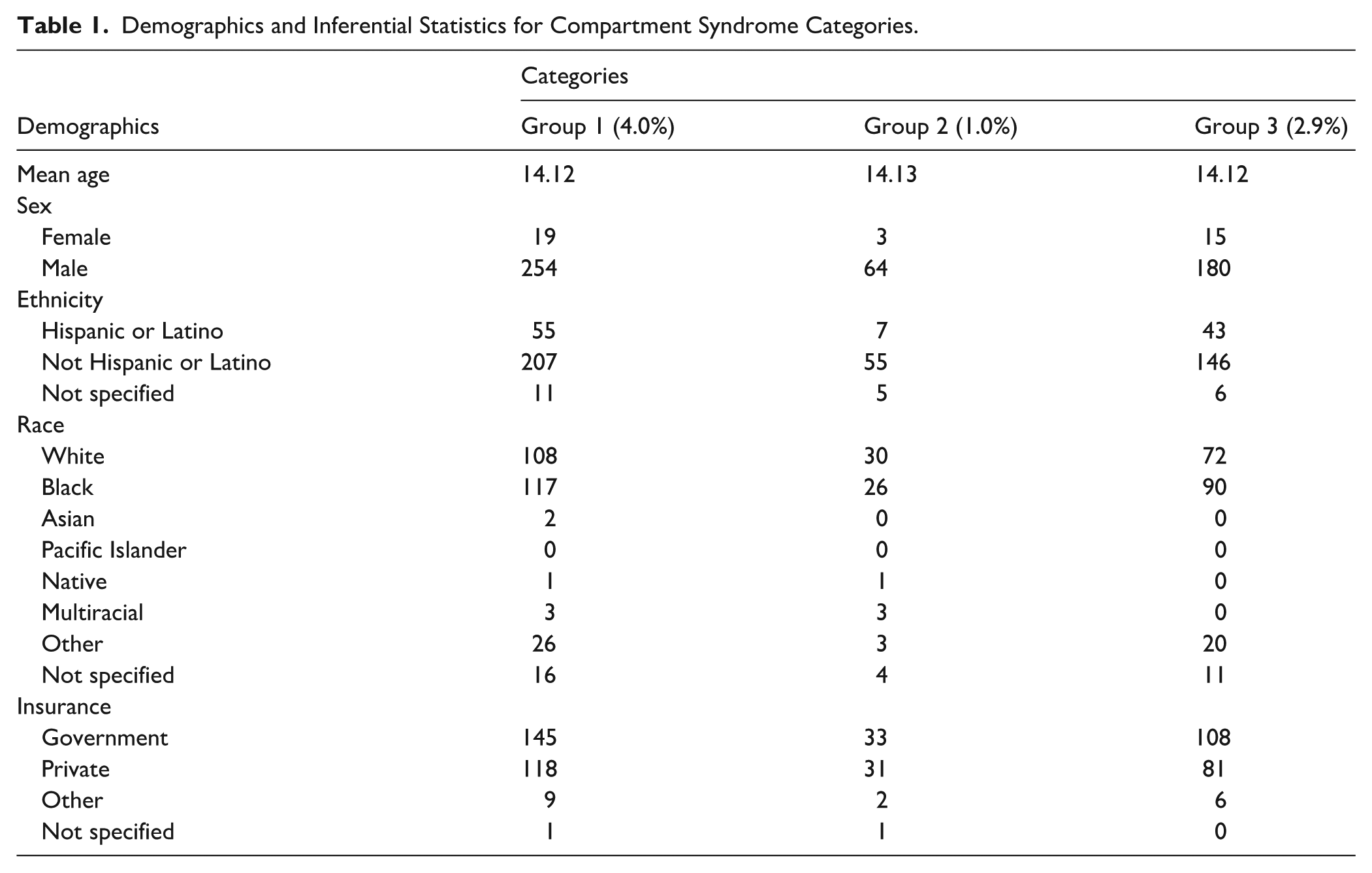
This study included 6830 total patients. The average age was 13.27 years, 14.8% were female, and 38.8% were White (Table 1). Group 1 included 4.0% of patients; group 2 included 1.0% of patients; and group 3 included 2.9% of patients.
Demographics and Inferential Statistics for Compartment Syndrome Categories.
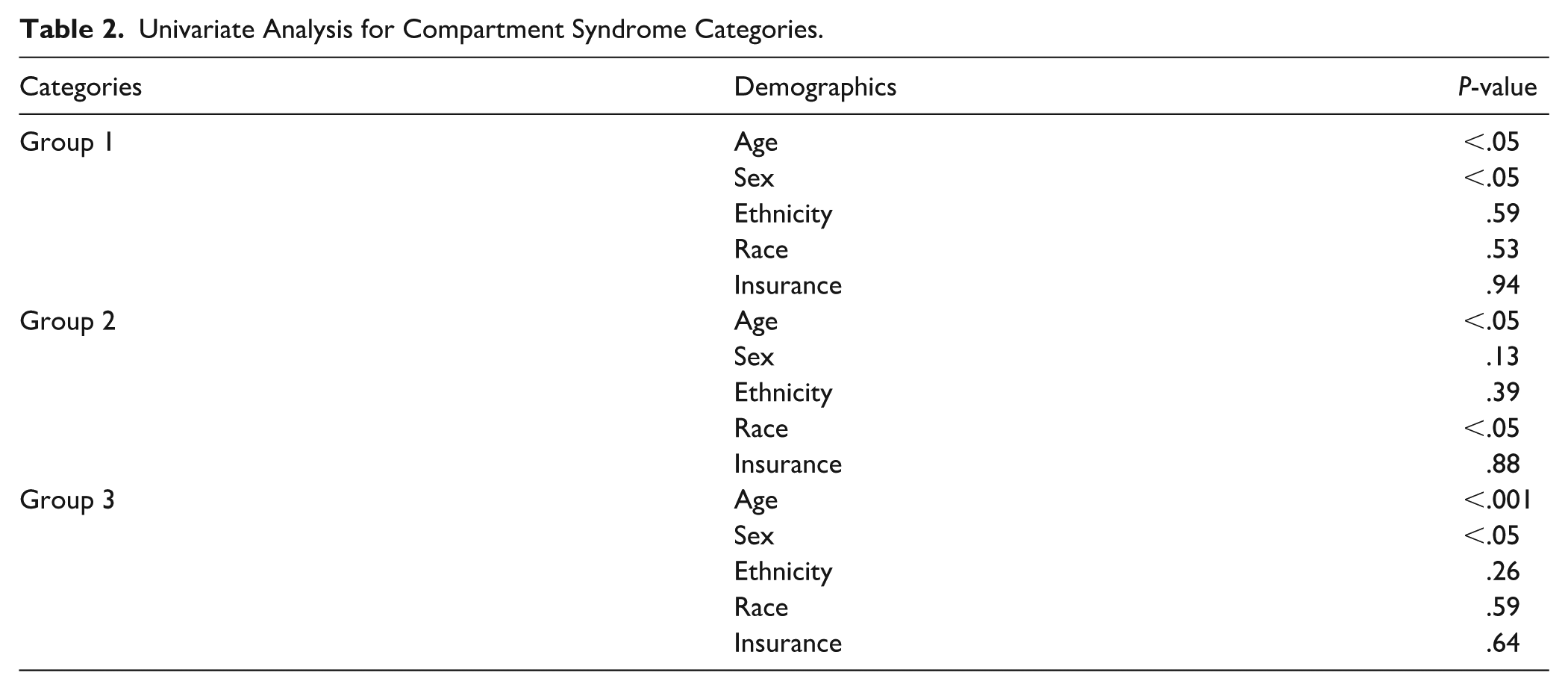
In our univariate analysis, age was a significant predictor in all 3 groups, with older patients having higher rates of compartment syndrome and fasciotomies without an associated ACS diagnosis, compared to younger patients, P < .05 (Table 2). Overall, the mean age of patients with ACS and/or an associated fasciotomy code was significantly higher than the mean age of those without, 14.12 ± 1.38 versus 13.23 ± 2.43, t(345.83) = −9.96, P < .001. Additionally, sex was a significant predictor in groups 1 and 3 (P < .05), with males more often associated with compartment syndrome and fasciotomies without an associated ACS diagnosis, compared to females, respectively. Lastly, race was a significant predictor in group 2, with White patients being more associated with compartment syndrome than non-White patients, P < .05.
Univariate Analysis for Compartment Syndrome Categories.
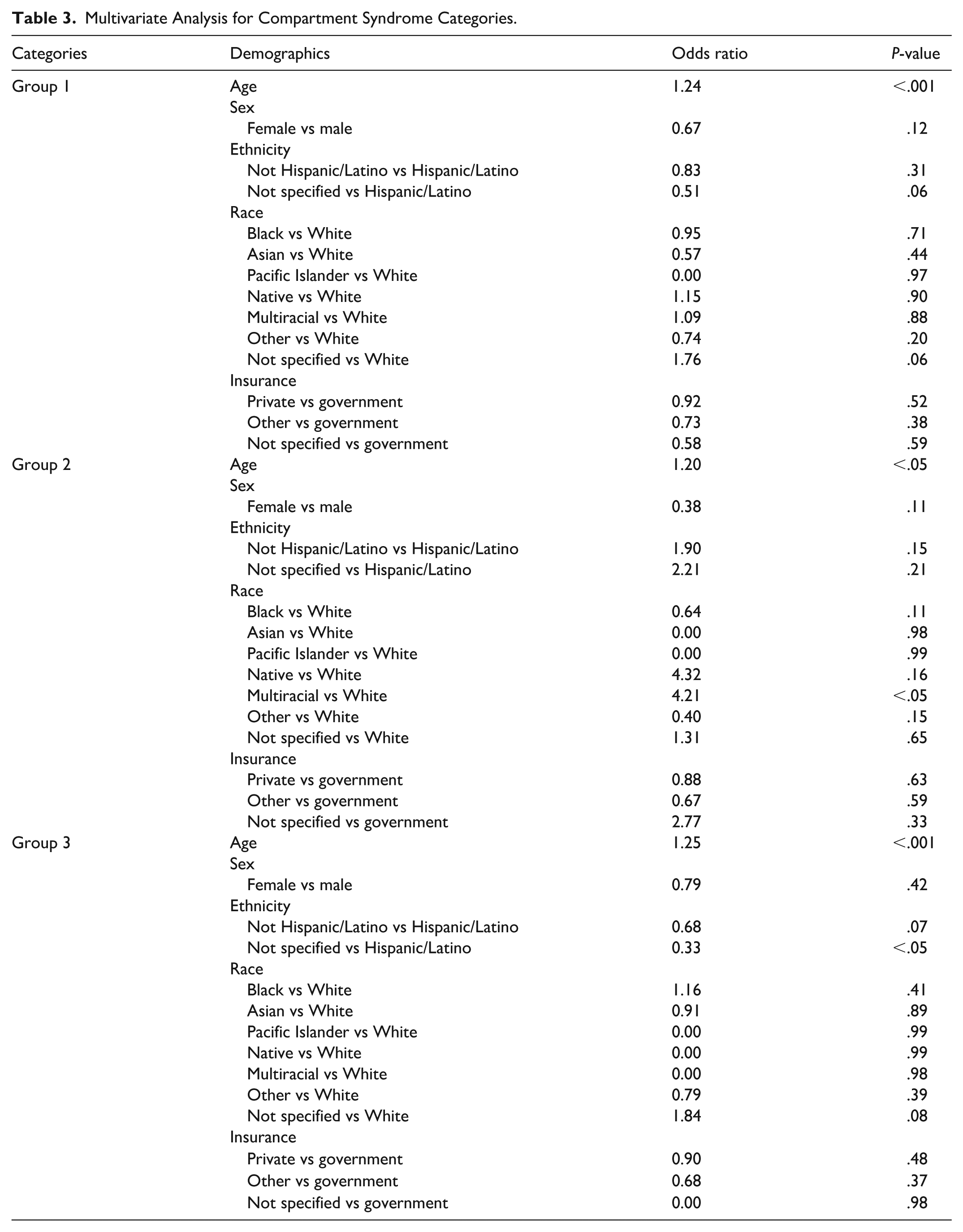
In our multivariate analysis, age was the only significant predictor in all 3 ACS groups, P ≤ .05 (Table 3). Most other multivariate associations were nonsignificant. The exceptions were in group 2: multiracial patients were more likely to have ACS than White patients (P < .05) and in group 3, patients with an unspecified ethnicity were less likely to have a fasciotomy with no associated ACS diagnosis than Hispanic/Latino patients (P < .05).
Multivariate Analysis for Compartment Syndrome Categories.
Discussion
Tibial tubercle fractures in pediatric patients have been associated with ACS, but the incidence rate and risk factors of this limb-threatening complication have generally been unexplored. Therefore, this retrospective database study examined the incidence of ACS and sought to identify risk factors for both ACS and fasciotomies in pediatric patients with tibial tubercle fractures. We found that 4.0% of pediatric patients with a tibial tubercle fracture were diagnosed with ACS and/or underwent a fasciotomy; however, only 1.0% of patients had a diagnosis code for ACS and a procedure code for fasciotomy. We interpret this group as representing patients with true ACS. Furthermore, 2.9% of patients had a procedure code for fasciotomy without a diagnosis of ACS, which we interpret as patients who underwent a prophylactic fasciotomy. When controlling for other demographic variables, older age was significantly associated with ACS.
Limitations of this study include challenges introduced by the coding of the data. For instance, group 3 consisted of patients who had an ICD-10-CM code for a fasciotomy and no CPT or ICD-10-CM code for ACS. It is possible that these patients were charted incorrectly or incompletely (e.g., coding omissions, separate-coding encounters), and their diagnosis of ACS was not visible in the available data. Furthermore, we could not classify tibial tubercle fractures or assess the mechanism of injury that may be correlated with ACS. These limitations highlight the difficulty of performing a database study in which further investigation into individual patients cannot be readily performed. Additional research is needed to confirm these findings in other populations, and additional study is needed to understand surgeon decision-making and identify patients at risk for ACS in the setting of a tibial tubercle fracture.
Only a few studies have used large-scale datasets to explore the incidence and complications of ACS in pediatric tibial tubercle fractures. For instance, in a retrospective study of over 25 000 patients, Milner et al similarly found that older age, in addition to male sex, were significant risk factors in the development of ACS in pediatric tibial tubercle fractures. 18 Among an inpatient pediatric population with tibial tubercle fractures, Martinez et al found that only 1.35% of cases developed ACS. Notably, 3.72% of cases included a fasciotomy without an ACS diagnosis, which they characterized as prophylactic fasciotomies. However, no associations were found between ACS and demographic factors (such as age, race, and insurance status). 17 Our findings are consistent with these studies since the true rate of ACS is ~1% and older age is associated with developing ACS. Older age may be an important factor since it may be correlated with severity of injury or additional bony injury relative to physical injury.
With the relatively low risk of developing ACS in pediatric tibial tubercle fractures, the appropriate management of these patients should continue to be investigated. Our study suggests that prophylactic fasciotomies may occur at a higher rate (2.9%) than patients with true ACS (1.0%), suggesting that some patients might be exposed to unnecessary surgical risk. However, it is possible that some patients who underwent a prophylactic fasciotomy may have developed ACS if they had not been managed prophylactically. In a retrospective review examining 47 cases of pediatric tibial tubercle avulsion fractures, Bergen et al found that no patients developed ACS in their postinjury or postoperative course. Based on this experience the researchers suggest that risk of ACS may be so low as to allow for same-day discharge after fracture repair. 19
In conclusion, our retrospective cohort study suggests that ACS is a relatively rare complication of pediatric tibial tubercle fractures, although the rate of ACS is not insignificant. Older children require closer attention and evaluation since they may have a higher incidence of ACS in the setting of tibial tubercle fractures. Prophylactic fasciotomies—those performed without an associated diagnosis of ACS—are done in practice, and additional study is needed to identify indications for this procedure.
Supplemental Material
sj-docx-1-hss-10.1177_15563316251404023 – Supplemental material for Assessing the Rate and Risk Factors of Compartment Syndrome in Pediatric Tibial Tubercle Fractures
Supplemental material, sj-docx-1-hss-10.1177_15563316251404023 for Assessing the Rate and Risk Factors of Compartment Syndrome in Pediatric Tibial Tubercle Fractures by Alex Youn, Abbott Gifford and Ishaan Swarup in HSS Journal®
Supplemental Material
sj-docx-2-hss-10.1177_15563316251404023 – Supplemental material for Assessing the Rate and Risk Factors of Compartment Syndrome in Pediatric Tibial Tubercle Fractures
Supplemental material, sj-docx-2-hss-10.1177_15563316251404023 for Assessing the Rate and Risk Factors of Compartment Syndrome in Pediatric Tibial Tubercle Fractures by Alex Youn, Abbott Gifford and Ishaan Swarup in HSS Journal®
Supplemental Material
sj-docx-3-hss-10.1177_15563316251404023 – Supplemental material for Assessing the Rate and Risk Factors of Compartment Syndrome in Pediatric Tibial Tubercle Fractures
Supplemental material, sj-docx-3-hss-10.1177_15563316251404023 for Assessing the Rate and Risk Factors of Compartment Syndrome in Pediatric Tibial Tubercle Fractures by Alex Youn, Abbott Gifford and Ishaan Swarup in HSS Journal®
Footnotes
Appendix
International Classification of Disease, 10th Revision Coding System (ICD-10-CS) codes:
M79A21, M79A22, M79A29, T79A0XA, T79A0XD, T79A0XS, T79A21A, T79A21D, T79A21S, T79A22A, T79A22D, T79A22S, T79A29A, T79A29D, T79A29S, T79A9XA, T79A9XD, T79A9XS.
Current Procedural Terminology (CPT) codes:
27600, 27602.
ICD-10-Procedure Coding System (ICD-10-PCS) codes:
0J8N0ZZ, 0JDN3ZZ, 0JNP0ZZ, 0JQN0ZZ, 0JBP0ZZ, 0J9P0ZZ, 0JDN0ZZ, 0JQP0ZZ, 0JNN0ZZ, 0JDN0ZZ, 0JBP0ZZ, 0KNS0ZZ, 0KNT0ZZ, 0KBS0ZZ, 0JCP0ZZ.
Ethical Considerations
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration.
Consent to Participate
Informed consent was waived for all patients included in this retrospective cohort study.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Required Author Forms
Disclosure forms provided by the authors are available with the online version of this article as Supplemental Material.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
