Abstract
Advancing doctoral and postdoctoral international bioethics training in low-and-middle income countries (LMICs) is essential to address the emerging and reemerging healthcare needs of local populations. The COVID-19 pandemic underscored the need for sustenance of global collaboration and rapid adaptability in the future to further prioritize research frameworks to benefit LMICs. Thus, the purpose of the manuscript is to share the successes, challenges, and future considerations of building bioethics research capacity in seven federally funded training programs supported by the Fogarty International Center of the National Institutes of Health D43 mechanism. We advocate for continued investment in training programs recognizing that it requires committed time and effort, specialized funding opportunities, cultural sensitivity, and interdisciplinary faculty support both domestically and internationally. This investment supports cross-disciplinary collaboration, enhances the ethical conduct of research and recognizes the importance of context-sensitive research that generates evidence-based data for global solutions.
Keywords
Introduction
Research ethics training in low- and middle-income countries (LMICs) is essential as it helps ensure that health research is conducted in a manner that is respectful of and responsive to the needs and values of the local population. In reviewing protocols that focus on local and international health issues, LMICs face unique health challenges and ethical issues that may differ from those in high-income countries (Hunt et al., 2019; Milford et al., 2006; Silaigwana & Wassenaar, 2015). Research ethics training is necessary to help established and emerging LMIC researchers navigate these challenges more effectively (Glass, 2013; Millum & Sina, 2014; Ndebele et al., 2014). In particular, disproportionate disease burden and limited resources to support citizens’ health and well-being present numerous ethical challenges, highlighting the need for robust research ethics training. The high disease burden (Coates et al., 2021) necessitates prioritization of research that addresses the most pressing local and international health issues. Research ethicists in LMICs can provide a framework to help guide such decisions to ensure that research agendas are aligned with local needs and that benefits are maximized. Moreover, a sound framework can guide LMIC researchers in planning for sustainable benefits, such as building local research capacity, ensuring long-term access to successful evidence-based interventions, and involving healthcare systems in dissemination.
Since 2000, the National Institutes of Health (NIH), through the Fogarty International Center (FIC), has supported international bioethics research education (R25) programs that entail master's level training and curriculum development (Glass, 2013; Millum et al., 2013; Ndebele et al., 2014; Pratt et al., 2014a, 2014b; Saenz et al., 2014; Silverman et al., 2013; Strosberg et al., 2013). As originally designed, the R25 funding mechanism specifically targeted research ethics educational initiatives for a broad audience. The master's-level research ethics and bioethics training it supported was important in developing professionals with expertise in teaching, research, and ethics review (e.g., Ali et al., 2014; Matar et al., 2014; Millum & Sina, 2014; Ndebele et al., 2014; Pratt et al., 2014a, 2014b; Saenz et al., 2014; Silverman et al., 2013; Strosberg et al., 2013).
In 2017, the FIC adapted the D43 funding mechanism for its bioethics research training program; it was designed to support longer-term, comprehensive bioethics research training at the doctoral (PhD) and/or postdoctoral levels, providing advanced training, supporting research projects and helping participants become national and potentially international leaders in the field. At these levels, the D43 FIC Bioethics Training Program offers more rigorous opportunities for trainees to build sustainable research ethics capacity in their LMIC institutions and solidify their analytic and research expertise through hands-on mentorship, networking activities, and training to develop local expertise and address the shortage of bioethics scholars in host countries. Most countries in which D43 FIC programs exist have fairly well-established master's programs, many previously funded by FIC R25s.
Health research, including complex international clinical trials, is increasing in LMICs (Malekzadeh et al., 2020), driving a need for research ethics expertise beyond the master's level. Individuals with doctoral and postdoctoral training can provide leadership and intellectual support both to develop and serve in research ethics training programs locally and to enhance bioethics programs at LMIC institutions. Leaders in research ethics play a key role in training and mentoring the next generation of researchers and bioethicists. Strong leadership is needed to foster more robust institutions capable of conducting high-quality ethical health research, developing a sustainable research infrastructure and fostering a culture of ethical research. For such institutionalization to occur in LMICs, research ethics capacity must be integrated into the heart of the health research enterprise. Individuals with doctoral degrees in bioethics are needed to enhance national and international credibility of the field. In some institutions, scholars may be limited in what they can teach without a relevant doctoral degree.
The overarching goals of the D43 FIC programs have been to prepare trainees for independent research ethics and bioethics scholarship, including doctoral and/or postdoctoral research projects; to prepare them for teaching research ethics; and to help them develop the capacity to advise biomedical and behavioral social science researchers on complex ethical issues. These programs cover critical scholarship on the foundations, theories and methods of bioethics, and the principles of research ethics; promote leadership skills and networking within the global bioethics community; and heighten knowledge and analytic skills relevant to issues in research ethics, particularly as they emerge in LMIC settings. Empirical studies of locally relevant research ethics questions also inform evidence-based research ethics practice. This paper aims to highlight the doctoral and postdoctoral programs supported by Fogarty's D43 mechanism and the successes and challenges that each faced when implementing training beyond the master's level. We also discuss recommendations that could enhance current efforts to build research ethics capacity in LMICs.
Current Programs and Overall Goals
There are currently seven D43-funded programs. Five involve African countries (including Tanzania, South Africa, Zambia, Botswana, and Uganda), one involves four Central Asia countries (Azerbaijan, Kazakhstan, Kyrgyz Republic and Uzbekistan), and one involves Ukraine. Four of the programs currently support doctoral students only, two support postdoctoral trainees only, and one supports both. Table 1 outlines each of the programs and the number of their trainees. All programs are geared to the development of bioethics and research ethics scholars and leaders who can advance conceptual and empirical research within the host country, some working in collaboration with a US-based institution. Some programs have a goal to establish strong PhD training at LMIC institutions, which will become a platform for scaling up capacity building in research ethics. Moreover, all value diversity of thought; respect for inter-professional, inter-disciplinary dialogue; scholarly mentorship; community engagement; and excellence in science that yields scholars who can develop successful programs of research in their chosen areas of ethics inquiry.
D43 Doctoral and Postdoctoral Funded Programs.
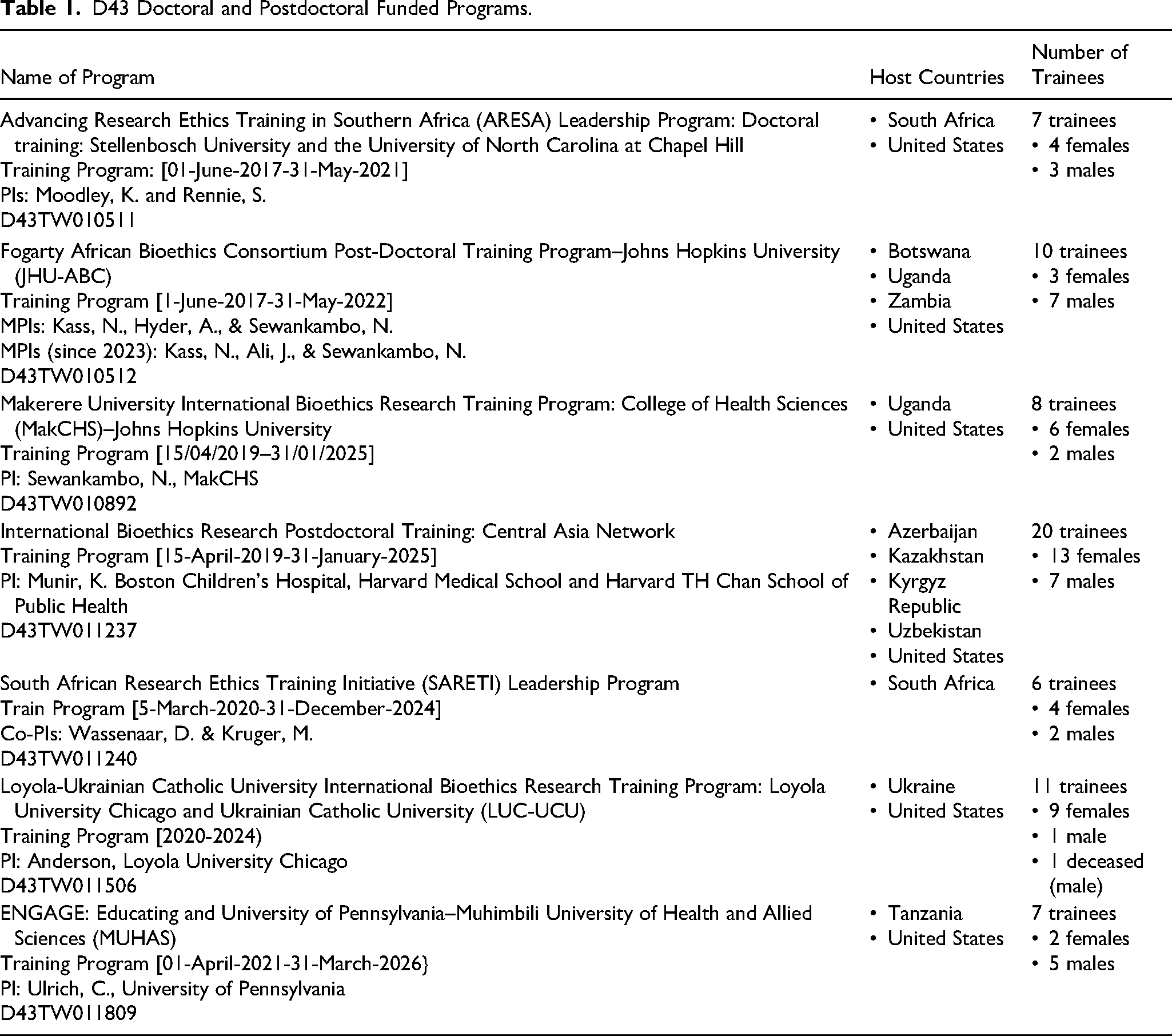
Fogarty-Supported Doctoral and Postdoctoral Bioethics and Research Ethics Trainees
Desired Qualifications
Fogarty doctoral and postdoctoral training programs have sought to attract, through competitive processes, early and mid-career professionals who are able to assume (or resume) leadership roles within their institutions or on their return to their institutions/countries. Depending on existing opportunities for formal bioethics training in their home countries, candidates may already have master's-level degrees in bioethics or research ethics or doctoral degrees in bioethics, research ethics, and/or related disciplines (e.g., MD, PhD in philosophy, law, public health, or social sciences), or they may have graduate training in a scientific, biomedical, or social science discipline. These programs also seek individuals with research ethics–related leadership roles, such as leading or being a member of a research ethics committee or institutional review board (REC/IRB). Additionally, adequate documented support from their home institutions and other evidence of commitment, as well as English language fluency, are critical for candidate inclusion in most of these D43 doctoral training programs.
Trainee Recruitment and Selection Process
Funded programs use social media, professional networks, and listserv outreach for recruitment of scholars. Applicants are required to provide proof of previous academic achievements (e.g., academic transcripts, curriculum vitae, personal statements, prior publications, concept notes and letters of reference). Trainees are competitively selected by committees; most conduct virtual interviews with all candidates, and some use a formal selection process tool developed by the research team. Variety of disciplinary backgrounds and demographics are important, in keeping with institutional goals and guidelines for REC/IRB membership in many countries. In some programs, priority consideration is given, or eligibility based on, affiliation with key partner institutions or to individuals who are citizens of a particular host or partnering country. For example, although Tanzania's program received applications from outside the country, the interdisciplinary applications within country were competitive and would help to build and establish a cadre of doctoral-prepared bioethicists within the home country that was needed. In contrast, as an example, SARETI competitively selected trainees from all Anglophone African countries.
Trainees in all of the programs include physicians; nurses; individuals with clinical, public health, and social science research backgrounds, as well as graduate training in philosophy and theology; individuals in faculty and leadership roles at universities and other research institutions; and REC members and/or administrators. In Ukraine, most doctoral trainees are physicians (MDs) or PhDs (in biomedical sciences) with faculty appointments in medical schools or other university affiliation. The Central Asia postdoctoral program also includes MDs or MD/PhD trainees with varied geographic proximal distribution. Enrollments by gender and other demographics varies by program (Table 1).
Trainee Scholarship
Across all D43 programs, trainees are engaged in conceptual and/or empirical scholarship related to a wide variety of topics primarily related to human research ethics (Table 2). This includes foundational or theoretical ethics concepts; integrity; clinical and public health ethics; ethical issues associated with various research designs, methodologies, and populations; issues related to use of technology, data dissemination, and stakeholder engagement; and the quality of RECs, among other topics. Most programs, ENGAGE and SARETI for example, require empirical research for acquiring a PhD, although conceptual ethical analysis may be approved for some. In the ARESA and Makerere programs, all students have conducted primary data collection for their dissertations. Trainees’ topic selection and methods are largely driven by trainees’ individual background, previous disciplinary training and professional role(s) and are ultimately determined in conversation with mentors and possibly doctoral committees. In the SARETI PhD program, scholars must align their empirical research projects with one of the following key themes: improving health research systems through research ethics leadership; improving effectiveness and efficiency of ethics review systems; or maximizing social value of research. These themes were determined via an interactive process by faculty and graduates at the closing event of the previous three cycles (2003–2017) of SARETI Masters research ethics funding. For trainees in Ukraine, the war has made original data collection challenging, but some trainees continue to work through these difficulties. In Uganda, the COVID-19 pandemic markedly interfered with progress of training and research activities, mainly because of the national lockdown. In the JHU-African Bioethics Consortium Postdoctoral Program, trainees conduct mentored, funded, individual postdoctoral projects that can be either empirical or conceptual in nature, with the expectation of at least one associated publication. The Central Asia Bioethics Research Training Program supported postdoctoral trainee group research projects during the peak of the COVID-19 pandemic, which facilitated more typical mentored empirical research projects involving primary data collection. The range of local and globally relevant research ethics topics supported is shown in Table 2, with the training site in brackets.
Doctoral and Postdoctoral Trainees’ Areas of Interest.

Program Components
All D43 programs aim to advance content knowledge, develop research capacity and leadership skills, and provide networking opportunities for trainees. Some (e.g., SARETI) also train candidates in grant writing skills to facilitate support for further training centers in the future. Content knowledge is advanced mostly through formal coursework and webinars and, for doctoral trainees, completion of the PhD dissertation or other similar program requirements (e.g., multiple scholarly publications for Loyola's DBE program or “PhD by publication” of three or four published articles on a common theme at Stellenbosch and Makerere University). A unique feature of the SARETI program is the intensive participatory selection process. For the final stage of the selection process, candidates participate in on-site workshops and seminars and must also present, defend, and revise their research thesis proposals interactively over several weeks. Successful candidates are funded for the further four years, while unsuccessful candidates leave with a viable PhD proposal, having participated in graduate level research ethics debates and workshops. Another unique feature of the SARETI PhD model is the single cohort approach: a single cohort of six candidates participates for the 4-year duration, instead of taking new candidates annually. This fosters group cohesion and peer mentorship (Loue & Loff, 2013; Munro et al., 2024) and considerable economies with aspects of the program not needing to be repeated annually for new candidates. Rigorous selection is also more likely to correlate with candidate success (Mouton & Cloete, 2015). Those pursuing PhDs by publication at Stellenbosch University (ARESA) engage in tailored coursework on research methodology, data analysis, and academic writing via the African Doctoral Academy in Stellenbosch and the Odum Institute Summer School at UNC. Trainees must have two publication-ready manuscripts before they can graduate. At some institutions/in some countries, requirements are much more specific than those typical of American universities. For example, empirical dissertations at Stellenbosch using qualitative methods have specific requirements for the number of interviews that must be conducted. Some doctoral programs also include requirements for comprehensive examinations or conference presentations. At all programs, compulsory coursework, either for credit or non-credit-bearing, is supplemented by additional seminars and conferences and practical experience, such as by observing or participating in research ethics review or teaching others.
At Makerere University College of Health Sciences, PhD trainees are required to undertake four mandatory courses (philosophy of methods, advanced gender research methods, qualitative and quantitative research methods and scholarly writing), and are required to have two published bioethics papers in peer-reviewed journals and proof of submission of two other manuscripts to peer-reviewed journals before they can graduate. At Muhimbili University of Health and Allied Sciences, trainees must have three papers accepted for publication, or published, prior to graduation, with a fourth paper submitted to a journal for review. Other requirements include thirty credits in coursework, presentation at four conferences (two international and two local), a pre-defense presentation, and final defense and submission of their dissertation. Stellenbosch University requires 2 published papers and 2 “publication ready” papers for the hybrid format of the PhD dissertation to be examined. The 2 published papers are inserted into the dissertation as papers with an introduction and conclusion on that chapter and the 2 publication ready papers are included as chapters of the dissertation.
Once the examiner passes the candidate, and the required changes/edits have been implemented to the satisfaction of the supervisors/examiners, the student may graduate. However, the student is expected to publish the remaining 2 papers that were deemed “publication ready” as soon as possible.
Research capacity is also developed through formal coursework, and many programs provide additional research training through intensive seminars and workshops in specific methods (e.g., qualitative research) and individually mentored research projects. Although requirements for scholarly work products vary, all programs aim to expose trainees to the full range of methods used in multidisciplinary bioethics scholarship, including philosophical and legal analysis and empirical qualitative and quantitative approaches. At Makerere University, the program designed and developed a curriculum that focuses on philosophical foundations and methods that help fellows gain and demonstrate an understanding of the nature of philosophy and specifically moral philosophy and its methods, and how this influences inquiry into the practice of bioethics. This course grounds PhD trainees in bioethical moral reasoning. Likewise, the Central Asia trainees have an opportunity to participate in research ethics coursework and in IRB meetings at Boston Children's Hospital and at Harvard TH Chan School of Public Health. This is integrated with the clinical compliance and regulatory affairs programs implementing policies and procedures in areas of human research, lab safety, biosafety, and research integrity. In addition, trainees receive specific mini-course modules to promote methodological excellence in research proposal design, implementation, and analysis, augmented by the available Boston Children's Biostatistics and Research Design Center. In the JHU-ABC postdoctoral program, coursework in research ethics and foundational/theoretical bioethics is required unless trainees have previously received this training; postdocs can supplement this with other coursework as desired. A targeted seminar is held with postdocs, and most training for the postdoctoral program is at the individual level, with intensive mentoring for individualized postdoctoral scholarly projects.
Leadership and Networking Opportunities
Development of leadership skills is supported in a variety of ways. Most significantly, in some programs, trainees are mentored to design and implement leadership projects at their home institutions. They are also engaged in assisting with organizing seminars and newsletters; for example, trainees from the ARESA program help to organize an annual seminar in Cape Town and contribute to the content and dissemination of an annual newsletter; the SARETI program will end with fellows organizing and hosting a pan-African research ethics conference (AHRES IV), for which they will also have to apply for funding – as a training exercise. Some programs offer formal leadership skills seminars or courses, as well as exposure to individuals in leadership positions for informal engagement and discussion.
Networking opportunities include occasional or regular participation in national and global bioethics conferences; membership in relevant professional bioethics associations, such as the African Doctoral Academy, the Research for Ethical Data Science in Southern Africa African Consortium of Bioethicists, or the Global Infectious Disease Ethics Collaborative, the Global Forum for Bioethics in Research (Littler et al., 2014); research residencies at US/UK collaborating institutions, which allow for networking not only with global experts but also with postdoctoral trainees from other countries; and virtual seminars with invited guest experts. In some cases, trainees are involved in month-long scholarly exchanges to other regional institutions across a bioethics network, such as the African Bioethics Consortium, which was established through the JHU Fogarty African Bioethics Post-Doctoral Training Program. Makerere University students visit the Johns Hopkins University Berman Bioethics Institute twice during their training for 2 to 3 months each trip. During this visit, they take courses, receive intensive mentoring on their dissertation research projects, visit US national institutions involved in research oversight, and network with other doctoral and postdoctoral students and different faculty who are experts in the students’ areas of research interest. The Central Asia Bioethics Research Training postdoctoral fellows are also able to visit the Boston Children's and TH Chan School of Public Health as visiting scholars. Although interrupted by the COVID-19 pandemic in the initial two years, it was possible to bring different trainee groups in fall or spring semesters to provide formative exposures. In addition, networking sessions are organized at LMIC sites. Sustained online support is provided on statistical methods and data analysis, with scheduled consultations troubleshooting issues in real time or on flexible schedules.
Mentorship
Mentorship is an integral part of advanced bioethics training. And there are extremely few bioethicists, research ethicists, and philosophers trained at the doctoral level who can provide the required mentorship. The Makerere bioethics alumni network provides a forum for interaction and peer mentorship of both past and current Makerere University trainees who participate in activities (which they manage themselves) with support by mentors. In addition, these trainees receive mentorship from resident ethicists and long-stay expatriate faculty engaged in research projects in the country. These efforts are supplemented by interactions with highly experienced researchers who have had shorter training in bioethics but have rich knowledge and skills acquired through wide health research experience.
Online group mentorship from partners at JHU is offered through regular conference calls. Trainees also need research mentorship to develop their research proposals and to narrow the subject matter to design a significant and feasible project. Additionally, this includes mentorship regarding science publications (e.g., choosing journals, formatting proposals to meet journal guidelines, appropriate referencing of material, and screening for plagiarism). Trainees also may need a mentor's help to focus on the best path for professional career growth. Critically, LMIC trainees also need to be mentored on what it means to be a good mentee, for example, being proactive in reaching out to mentors when they are having problems. For example, for Ukrainian trainees, having mentors who were accessible and responsive to their questions was a new experience, and it initially took some time for them to trust that reaching out for help was a positive step.
Publishing bioethics scholarship of an international standard can be mentorship intensive. For example, MUHAS requires doctoral students to publish three papers, and a fourth paper must be submitted. This is difficult and creates pressure to publish in a timely fashion before students can graduate. Providing mentorship for publication purposes and shaping manuscripts based on their dissertations when ready for publication is time and labor intensive. High publication fees for open access publishing in some journals can present another obstacle, and is budgeted for by some programs. Along with bioethics and research ethics mentorship, interdisciplinary mentorship is needed in qualitative, quantitative, and mixed-method methodologies.
Key D43 Program Challenges
The COVID-19 pandemic affected all Fogarty D43 programs, albeit in different ways. In-person activities and travel were curtailed during 2020–2022, which affected some programs more significantly than others. In-person data collection was also disrupted for many students. During the COVID-19 pandemic, many programs developed alternatives to in-person training components and continued these after in-person restrictions loosened. For example, in the Fogarty JHU-ABC program, COVID precipitated a one-year pause in matriculation of new trainees and for those already under training. This created delays in implementation of research, and an accommodation was made to allow trainees to complete month-long in-country scholarly exchanges with local research institutions, rather than international exchanges with other consortium institutions as borders were closed. Likewise, at its inception phase (2020–2022), the US training components of the Central Asia program were delayed and replaced by a comprehensive online schedule that extended across different years of trainee cohorts, enabling greater interaction with and learning from each other. Such interactions can sustain and foster a rich learning community, promoting knowledge exchange, and can enhance the overall training experience through aggregation of trainee cohorts.
For the LUC-UCU program, originally planned to be almost completely online, the full-scale invasion by Russia in February 2022 posed challenges in terms of safety, electricity, and internet access, as well as other family and professional commitments. To counter this national crisis, the PI and research team tried to minimize the burden of additional requirements for students (e.g., having several seminars on topics related to professional/career development) so they could focus on successful completion of coursework. This team also integrated the war into their learning and research (e.g., receiving a Fogarty supplemental grant to focus on the ethics of research during war). In Uganda, the complex and slow ethics review processes at the university's REC/IRB, along with research proposal clearance at the Uganda National Council for Science and Technology (UNCST), followed by approval by the university's higher-degree committees continue to remain a challenge, even though a change to online submissions of applications helped somewhat. Similarly, implementation of the SARETI leadership program was delayed, initially by COVID-19 and then by unforeseen institutional obstacles, for over three years, including candidate selection, which was only completed in 2024.
Communication and Commitment Challenges
For trainees in some LMICs, communications can be challenging because channels are fragile (e.g., intermittent internet access) or the trainees are overwhelmed by their employment duties. Unlike most traditional American and European PhD students, most Fogarty bioethics trainees are unable to work anywhere near full-time on their dissertations. For all programs, finding time for trainees to devote to their coursework, research, and writing is a challenge, considering their extenuating circumstances. In all programs, whether an 18-month postdoctoral or doctoral program planned for 4 years, most (although not all) trainees have had trouble completing requirements during the allotted time. While, in theory, trainees can seek release from duties at their home institutions, the reality is that most of these individuals have unique, sought-after skills in under-resourced institutional environments and often cannot be easily replaced, even for short periods. This means that students will often exceed the planned period to complete coursework, dissertation, or other scholarly activities, and funds to support their work may run out. Completing required activities is most challenging when trainees are in their home countries conducting independent research and writing. Trainees who complete coursework in the US and then return home are pulled in multiple directions and back into their previous responsibilities. Many excellent candidates are unable to leave their home institutions and families for extended periods. Given the general challenge of working professionals in LMICs and being away from home/work for a period of time, the JHU-ABC program altered the timing of the Johns Hopkins training component to permit an (optional) return home half-way through to enable trainees to reconnect with their families and address their other obligations.
Knowledge, Skills, and Training Gaps
Another challenge is that while most trainees already have graduate degrees, there are still gaps in their knowledge and skill base that manifest when conducting bioethics research and scholarship. For example, many trainees exhibit weak argumentation and critical thinking skills when evaluating the relevant literature and their own research results; particularly when providing ethical analysis of cases or of empirical results. In addition, most of their required graduate research requires advanced social science methodology and analytic skills, which the background training of many candidates (e.g., lawyers, philosophers, physicians) excludes. Case-based discussions, pushing and challenging on argumentation, can be a centrally important training approach. For empirical research, repeating intensive training and mentoring as well as quality control is needed to prepare REC submissions, guide trainees through the submission and review process, and analyze results. SARETI prescribes a (digital) social science methodology text to support candidates with this process (Terre Blanche et al., 2006). For some trainees, writing for publication also requires intensive mentoring as academic writing in English is challenging because many trainees may not have been exposed to in-depth writing prior to their Fogarty training. Not surprisingly, even some students with excellent fluency in English need intensive support for academic writing. Moreover, there is limited availability of high-quality training and mentoring for writing at the undergraduate and master's level in many LMIC institutions.
Administrative Hurdles in Funding Transfers and Granting Degrees
In terms of grant and program administration, transfer of funds between institutions is often mired in bureaucracy and can take up to 6 months in the African context. For US partner institutions, securing visas for trainees can be a prolonged and complex process. Moreover, PhD programs at LMIC partner universities can have significant administrative requirements that can complicate program timelines. For example, at Stellenbosch University and Makerere University, students must first register as “Pre-Docs” and are allowed up to 6 months (1 year at Makerere) to develop their proposal and have it approved by a PhD Protocol Review Committee. Subsequently, the doctoral student registration process requires approval via multiple postgraduate research committees at departmental and institutional levels, as well as RECs and Faculty Board and Senate approval. Formatting errors can trigger a long bureaucratic process of correction. REC approval may be lengthy, further delaying the full registration of the student. Submission deadlines are tight along this approval process, which may easily take up to a year. At some partner institutions (Muhimbili University of Health and Allied Sciences, for example) students must initially write their concept of interest (e.g., literature review, gaps in knowledge, proposed methods) before they take formal course work. This takes intense mentoring and revisions to get the proposal university- and REC/IRB-approved. If publications (especially of empirical research findings) are a requirement of granting the degree, this can extend timelines even further.
Key D43 Program Successes
While there have been challenges within the various D43 programs, there have also been important successes. Indeed, ARESA's first graduate was, to program leaders’ knowledge, the first African to obtain a Fogarty-funded bioethics PhD from an African institution. ARESA has two further trainees who graduated in December 2024, bringing the total of D43-funded graduates from this doctoral program to five. There have also been graduates from the other D43-funded programs, including the Loyola-Ukrainian Catholic University International Bioethics Research Training Program (two doctorates in bioethics [DBEs]).
As intended, the JHU-ABC program successfully accepted ten postdoctoral fellows to the program from Makerere University College of Health Sciences (MakCHS), the University of Botswana, and the University of Zambia. Most completed program requirements. Trainees continue to make progress. Several ENGAGE scholars have had their research proposals approved through the local academic system and the national Tanzanian REC and are collecting data. In addition to two recent DBE graduates and a third about to complete capstone requirements, there are eight more LUC-UCU doctoral trainees at different stages of coursework on schedule to complete their DBE degrees in the next two years, and there has been no attrition in this program (sadly, there has been one death). Some of Makerere's eight trainees will be completing this academic year 2024/2025, and others by the end of 2025. Additionally, seeking research ethics approval at two levels, i.e., at the university REC and at the UNCST, and the COVID pandemic caused major delays in trainees’ progress. The UKZN SARETI program implementation has only just begun (2024) and will depend on FIC no-cost extensions to complete all program deliverables.
Publications
To date, ARESA graduates have produced 15 peer-reviewed publications (Burgess et al., 2023; Burgess et al., 2024; Masiye et al., 2023a, 2023b; Mtande et al., 2019; Mtande et al., 2022; Mtande et al., 2024; Ochieng et al., 2021; Ochieng et al., 2022a, 2022b; Ochieng et al., 2024; Singh & Moodley, 2021; Singh et al., 2022a; Singh et al., 2022b; Singh et al., 2023), and JHU-ABC postdoctoral trainees have published over two dozen papers (examples include Barugahare & Kass, 2022; Chongwe et al., 2023; Jacobs et al., 2023; Koloi-Keaikitse et al., 2021; Zulu et al., 2023). Four LUC-UCU doctoral trainees have published in peer-reviewed bioethics journals, and three trainees have publications currently under review (Basarab & Anderson, 2022; Kachkovska, 2024; Novick & Kachkovska, 2023; Paryzhak & Vari, 2024; Sulaieva et al., 2022; Sulaieva et al., 2023; Sulaieva et al., 2024). Seven Central Asia postdoctoral trainees have published individual or group papers in peer-reviewed journals, including a paper in this journal (Salayev et al., 2024), and three have publications under review. Several others have published blogs and narrative pieces. Makerere PhD trainees have so far nine publications in peer-reviewed journals and five under journal review (examples include Kituuka et al., 2023; Kituuka et al., 2024; Nabukenya et al., 2024).
Trainees in Leadership Positions
ARESA's first graduate now serves as Chair of the Biomedical Research Ethics Committee at the University of KwaZulu-Natal and Vice Chair of the National Health Research Ethics Council of South Africa. A LUC-UCU doctoral student led the efforts to establish an REC at UCU and now serves as chair. Another will serve as director of clinical ethics at UCU's newly established medical clinic. A recent graduate and faculty member at Sumy State University in Ukraine, has been asked by the Dean to reconstitute and retrain both REC and IACUC members and develop bioethics curricula for medical students, PhD students in biomedical sciences, and faculty scientists. Four Makerere PhD trainees are already in leadership positions, even before they graduate. One is serving as head of research compliance and regulatory assurance at the UNCST, a second is the Regulatory and Monitoring Officer at the Infectious Diseases Institute at Makerere University, a third is the Chair of the REC of the Makerere University School of Health Sciences, and a fourth is a committee member of the National Formulary of the National Drug Authority (NDA) in Uganda.
Recommendations for Future Consideration
The rapid advancement of new technologies, such as artificial intelligence (AI), genomics, biomedical applications, research during public health emergencies, and digital health, is transforming the global landscape of scientific research. These developments introduce complex ethical challenges internationally, including data privacy concerns, potential for data manipulation, and inherent biases in AI algorithms. Addressing these challenges will require rigorous and continuous ethical scrutiny to ensure that such innovations are employed responsibly and equitably across diverse global populations. The development of advanced research ethics scholars will be paramount. They stand to play a critical role in establishing and upholding ethical research standards, fostering trust in research, and safeguarding the dignity, rights, and welfare of individuals globally while seeking ethical evidence-based solutions to health-related challenges. Their expertise will be indispensable in addressing emerging ethical dilemmas, guiding ethical decision-making processes, and promoting ethical practice in research and healthcare. Therefore, as scientific research becomes more intricate and interconnected globally, the demand for competent bioethics scholars is likely to grow. Over the next decade, investment in bioethics training will ensure that the ethical dimensions of future technological developments are understood and managed, leading to more ethical and socially responsible scientific progress. Therefore, our recommendations for future consideration are in three broad areas: extramural funding, training and support for scholars, and a multifaceted strategy to publicize the programs and increase outside and within-country support.
The foresight that Fogarty had in 2000 to begin funding the training of LMIC scholars in research ethics and bioethics has been nothing short of transformational. Hundreds of scholars now exist across the global south with expertise in bioethics (see e.g., Glass, 2013; Millum et al., 2013; Ndebele et al., 2014; Pratt et al., 2014a, 2014b; Saenz et al., 2014; Silverman et al., 2013; Strosberg et al., 2013), and since 2017, there are trainees with doctoral- and postdoctoral-level training in research ethics and bioethics, providing both more sophisticated expertise and the opportunity for bioethics leadership in research institutions. Trainees have published, have obtained important positions teaching bioethics, and have been recognized internationally. Our experience running several programs allows us to suggest how this opportunity could be expanded and refined to improve impact.
We provide suggestions below for funders interested in supporting bioethics and research ethics training and scholarship in LMICs. Substantive investment in institutional capacity development in research ethics and bioethics is needed, not just investment in individuals. Ongoing NIH/sponsor investment in institutional capacity (e.g., short-term faculty development programs) will help provide trainees with adequate support in their home countries. This will be important to support postdoctoral trainees in their longer-term faculty roles serving as mentors and enabling sustained growth. National investment is also important. Many programs are based in public universities where programming and priorities are heavily influenced by national actors. Well-informed and engaged national entities (ministries of health, science, education, technology, etc.) can contribute significantly to advancing bioethics opportunities, including establishment of bioethics faculty positions. The UNCST, for example, relies extensively on trained bioethicists to support policy development, organize annual national research ethics conferences, conduct clinical trial site monitoring etc. Similarly, national bioethics committees can be strengthened through closer working relationships with bioethics PhD and postdoctoral programs. Achieving these goals will require budgetary support. In the 24 years that Fogarty has funded bioethics, the overall annual budget for D43 programs has not changed, whereas costs of tuition, travel, visas, faculty salaries, health insurance, and other supports have all greatly increased.
We also recommend broader funding for research ethics and bioethics training, as well as continual support for LMIC research ethics scholars beyond doctoral and postdoctoral training. This includes not only prolonged support from NIH/Fogarty but also other potential bioethics or capacity development funders who can provide additional support for research training needs in LMICs (e.g., conferences, networking activities, infrastructure support, research activities). Indeed, we encourage other bioethics and healthcare funders, such as the Greenwall Foundation, the Commonwealth Fund, Wellcome Trust, the European Union's European and Developing Countries Clinical Trials Partnership, the Robert Wood Johnson Foundation, the Josiah Macy Jr. and John Templeton Foundations and others, to consider this type of support in LMICs. Relatively few funding opportunities for advanced research ethics researchers exist in LMICs, particularly in Africa. The Fogarty Emerging Global Leader Award (K43) allows junior faculty in LMICs to have protected time (3 to 5 years) to advance their research scholarship. To our knowledge, however, no bioethics scholars have applied for and received this grant.
Like the K43 mechanism, the K99/R00 Pathway to Independence Award for LMIC research ethics and bioethics postdoctoral scholars could provide needed career development mentorship for transition to an academic position. Private-public partnerships should also be explored to support global health research and capacity building in LMICs and coursework that would benefit doctoral and postdoctoral students. Funders should also support the development of employment opportunities for doctoral candidates at academic and research institutions in low-resource settings. We also would like to see institutions in LMICs consider creating research ethics posts and career tracks for graduates funded by the D43 doctoral and postdoctoral training awards. Unfortunately, faculty career-development tracks in bioethics are rare in LMICs. Thus, we encourage Fogarty and other funders to consider supporting research in LMICs as part of their future portfolios.
Although continued investment in research ethics education and training in LMICs is critical, we recommend that NIH and other research funders extend training support to other areas of bioethics (e.g., clinical and public health ethics) where needs in LMICs are also significant (National Academies of Sciences, Engineering and Medicine, 2024; Rennie & Hunter, 2020). Such needs are particularly evident in terms of challenges of conducting locally and globally relevant research in LMICs with diverse populations with differential risks, benefits and social value. The COVID-19 pandemic also revealed many clinical, organizational, societal, and research-related ethical issues (Rossouw et al., 2021; Salamanca-Buentello et al., 2024). A broad, formal international needs assessment could identify priority foci.
Given the gaps in knowledge, skills, and training identified above, funding for short-term, formal, predoctoral programs of 12 months of intensive training in research methodology, writing skills, and data analysis could help identify and prepare the best candidates. For example, a bidirectional T32 US and D43 LMIC could support short-term predoctoral training through an international university, perhaps virtually, while individuals stay in their home institutions, to develop critical thinking skills and conceptual analysis that are not always sufficiently taught in master's programs. Diversifying and leveraging funding mechanisms to support the transition from masters to doctoral training in LMICs would help to attract and retain the best candidates. Funding for graduate and postdoctoral training in research ethics and bioethics should not be restricted to those who can undertake full-time study, or who can spend long periods away from home, or commit to long-term training. Part-time, virtual, and short-term options (or some combination) seem critical to attracting individuals with potential to be national and global leaders in research ethics scholarship, oversight, and policy, as these must be individuals with relevant expertise and maturity who are already in positions of influence. This is especially true in those LMICs affected by violent conflict and other humanitarian disasters and in LMICs with shortages of healthcare providers, and if we want to attract a spectrum of mature mid-career trainees.
Engaging national policymakers is vital to showcasing the tangible benefits of advanced bioethics training internationally. By elucidating the role of bioethics in ensuring ethical research practices, such programs can be integrated into national legislative frameworks, thereby securing dedicated funding within national budgets. Such engagement involves demonstrating how research ethics scholarship and training can improve the global integrity and credibility of research, protect participants, and enhance local and international public health outcomes (Abdool Karim et al., 2017). Enhancing regional networks and alliances among LMICs to share resources, expertise, and best practices can greatly amplify the impact of training programs. Creating a robust collective voice for research ethics training at both national and regional levels should be a strategic priority. These networks foster collaboration, knowledge exchange, and mutual support, which are essential for sustaining and expanding bioethics initiatives.
Supporting existing collaborations among various D43 programs, each with distinct training approaches, could promote the development of regional alliances, knowledge hubs, best practices and partnerships. Collaborative efforts enhance the effectiveness and reach of bioethics training initiatives, allowing for a more comprehensive and cohesive approach to addressing ethical challenges in research. Adopting a flexible approach to advanced training, like the flexibility afforded by R25 research educational activities, is also crucial. Recognizing that there is no one-size-fits-all model in postdoctoral and doctoral degree training, D43 programs should be tailored to be relevant and responsive to the specific challenges and opportunities within different LMICs.
Ensuring local relevance and engaging communities in discussions about research ethics remain critical components of these initiatives. By emphasizing how research ethics safeguards participants’ rights and welfare, we can foster community buy-in, leading to broader support and acceptance of more sophisticated bioethics initiatives within LMICs. This engagement builds trust and encourages active participation in research, which is essential for the international success and impact of bioethics programs.
Conclusion
Training the next generation of research ethics and bioethics scholars will require committed time and effort, specialized funding opportunities, cultural sensitivity, and interdisciplinary faculty support both domestically and internationally. Our hope is that developing global leaders in bioethics will build a sustainable group of scholars who can address the most pressing health-related ethical concerns locally and globally in the future. The COVID-19 pandemic has provided us with valuable insights into critical ethical issues and the necessity for global leaders with ethics backgrounds to tackle international research and public health ethics questions, ensuring the ethical conduct of globally-relevant research and equitable global access to the products of such research, such as treatments and vaccines. The pandemic also underscored the need for sustenance of global collaboration and rapid adaptability in the future to further prioritize research frameworks to benefit LMICs. This can be achieved through rigorous application of sound principles and well-designed empirical research addressing pressing local challenges. Investing in the training and development of an advanced, and diverse group of bioethics scholars in LMICs is essential to building resilient, context-sensitive research infrastructures that can drive impactful and equitable health solutions. The evidence from the programs described above provides promising support for expansion of this initiative and its potential global impact.
Footnotes
Acknowledgments
Emily E. Anderson is supported in part by Fogarty International Center, NIH D43TW011506; Kerim Munir is supported in part by Fogarty International Center, NIH D43TW011237; Joseph Ali, Nancy Kass and Nelson Sewankambo are supported in part by Fogarty International Center, NIH D43TW010512; Nelson Sewankambo is supported in part by Fogarty International Center, NIH D43TW010892; Douglas Wassenaar and Mariana Kruger are supported in part by Fogarty International Center, NIH D43TW010131; Stuart Rennie and Keymanthri Moodley are supported in part by Fogarty International Center, NIH D43TW010511; and Connie M. Ulrich, David Urassa and Bruno Sunguya are supported in part by Fogarty International Center, NIH D43TW011809.
Declaration of Conflicting Interests
The authors declare no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Fogarty International Center, (grant number D43TW010131, D43TW010511, D43TW010512, D43TW010892, D43TW011237, D43TW011506, D43TW011809).
