Abstract
Research ethics is a fundamental part of the entire research. Patients with rheumatoid arthritis are sensitive group of research participants because their long-term health problems cause significant changes in their foot health. In foot health research, data are usually collected through a clinical assessment of the foot or questionnaires. However, there is limited evidence of the reported research ethics of empirical studies on foot health in patients with rheumatoid arthritis. Therefore this review aimed to analyze the reported research ethics of peer-reviewed empirical studies focusing on foot health in patients with rheumatoid arthritis as research participants. This systematic review used the Medline/PubMed, CINAHL, and Embase databases. A total of 1,653 records were identified, and 32 articles were included in the final analysis. Reporting research ethics in studies of patients with rheumatoid arthritis is fragmented, focusing predominantly on ethical approval and informed consent and lacking a broader discussion about research ethics.
Introduction
Research ethics is a prerequisite for robust science in any field and a fundamental part of every step in the research process. Traditionally, ethical principles of scientific research concern respect for individuals, beneficence, justice, and respect for communities (Beauchamp & Childress, 2013). Currently, these principles are strengthened by universally agreed requirements and declarations, such as the Universal Declaration on Bioethics and Human Rights (UNESCO, 2005), and the European Code of Conduct for Research Integrity (Allea, 2017). Moreover, the International Committee of Medical Journal Editors (ICMJE, 2019) has published uniform requirements for scientific publications. Ethical requirements in the field of foot health research are the same as in other fields; however, a systematic description of the reporting of research ethics in foot health research is lacking. In this study, foot health research is a scientific empirical research that focuses on the foot and ankle in patients with rheumatoid arthritis.
The Declaration of Helsinki, drawn up by the World Medical Association (originally 1964, last updated in 2013) is a cornerstone document for research ethics and states the ethical principles for medical research involving human research participants (WMA, 2013). Its fundamental principle is respect for the individual, individuals’ right to self-determination, and their right to make informed decisions. These rights relate not only to participation in research but also to the whole research process, thus giving an individual the right to withdraw from the study without individual consequences. When designing and planning the research, researchers need to clearly state in the research plan how ethical considerations and the principles of the Declaration of Helsinki are addressed in every phase of the study. This plan should be exposed to external evaluation by a research ethics committee before the study begins (WMA, 2013). Privacy has been seen as an increasingly important ethical principle in clinical research (Nurmi et al., 2019). Along with the Declaration of Helsinki, at the European level, the General Data Protection Regulation (GDPR, European Union, 2016) stipulates the privacy of research data and good practice in handling sensitive information. In addition, country-specific ethical principles support the guidance of scientific research.
Institutional review board (IRB) is independent body consisting of qualified members (WMA, 2013). An IRB might be found within a research institution or operate on a regional or national basis (WHO, 2009). The main task of this board is to evaluate compliance with internationally and nationally accepted ethical guidelines and the laws and regulations of the particular countries in which the study will take place (WHO, 2009; WMA, 2013). The main issues under evaluation are with respect to the Declaration of Helsinki and the protection of human participants (WHO, 2009). These points are evaluated based on described participant selection procedures, balance between benefits and harms, and informed consent procedures (WMA, 2013).
Besides ethical approval, permission to conduct the study is required. The application for permission depends on the organization's practices and policies (Emanuel et al., 2008; Taljaard et al., 2014). When applying for permission, the researcher must indicate how ethical guidelines will be followed in the study and what requirements of the study involve the organization in question. In health research, these requirements could involve, for example, naming a contact person (gatekeeper), infrastructure for data collection, or information technology support, for example, when dealing with patient records (Gallo et al., 2012). In some countries, permission to conduct research at a site can be obtained from the IRB at the same time as the ethics of the study are evaluated (Bracken-Roche et al., 2017; O'Mathúna, 2015; Wu et al., 2019).
Informed consent is fundamental to research ethics and is addressed in worldwide ethics guidelines (Belmont Report, 1978; Nuremberg Code, 1947). Informed consent must be obtained before enrolling any study participants in all types of research involving human subjects (Emanuel et al., 2008), and obtaining it involves a process (Kadam, 2017). The process starts by explaining the research procedures, risks, benefits, and rights of the participants (Hammond, 2016). Potential participants usually receive written and oral information about the purpose of the study, data collection, and ethical considerations (Manti & Licari, 2018). Along with this information, the potential participants are provided with an opportunity to ask questions and discuss the study with the researcher to clarify unclear issues or gain more information (Kadam, 2017). Throughout the process, a researcher needs to be aware of the participants’ ability to understand and take in information, thus being competent to provide consent (Beauchamp & Childress, 2013). Finally, the potential participant decides whether to take part or decline participation in the study (Kadam, 2017). Informed consent enables the participants to make rational and voluntary decisions about participation in the study and addresses the understanding of the research process and its risks and benefits (Beauchamp & Childress, 2013). The process of consenting is continuous and is not restricted only to initial consent; the participant has the right to withdraw from the study at any time without providing any explanation or without any effects on their healthcare provision (Emanuel et al., 2008). Informed consent can be provided in written or oral form, and when necessary, may involve parental consent/permission (when investigating children) or assent (child's affirmative agreement to participate when underage, Emanuel et al., 2008), or a surrogate decision-maker responding together with the participant, as is found occasionally in patients with memory disorders (Howe, 2012).
In general, ethics-related research on foot health is scarce. Despite this limited attention, inspecting foot health may pose several ethical issues that need to be addressed. In foot health research, the data are collected from patients, usually through a clinical assessment of the foot (Stolt et al., 2017), where participants need to show their feet to the clinician or nurse. However, revealing one's feet is seldom considered an ethical issue. Some participants who have, for example, severe foot health problems such as those with rheumatoid arthritis, or those who feel the appearance of their feet may not correspond with esthetic expectations, may be reluctant to show their feet or, if they do show their feet, they might feel embarrassed or ashamed. In foot health research, participants’ autonomy, beneficence, and non-maleficence (Helfand, 2006), as well as privacy, integrity, and respect are issues to be considered when facing the patient (Helfand, 1993). An individual approach is fundamental in facing, caring for, and researching people with foot problems because patients’ feet are unique, and their needs are personal (Stolt, 2019). Moreover, professional responsibilities to do good and to avoid harm are key issues in providing ethical high-quality care (Helfand, 1993). International ethical guidelines seem to be lacking in the field of foot health research. However, in rheumatology, along with discussions about ethics in caring for patients with rheumatic diseases (Mckeown, 2015), the European League Against Rheumatism (EULAR) have incorporated research ethics in their recommendations for the reporting of clinical trial extension studies in rheumatology (Buch et al., 2015) and the use of big data in rheumatic and musculoskeletal diseases (Gossec et al., 2020).
Previous reviews have identified inadequate reporting of research ethics, for example, while conducting studies in nursing education (Vierula et al., 2016), with clusters (Taljaard et al., 2011), stepped wedge randomized trials (Taljaard et al., 2017), dental care of older people (Mukherjee et al., 2017), and long-term care settings (Suhonen et al., 2013). The main deficits focus on reporting informed consent (Mukherjee et al., 2017; Suhonen et al., 2013; Taljaard et al., 2011; Taljaard et al., 2017; Trung et al., 2017; Vierula et al., 2016), research ethics review (Taljaard et al., 2017; Trung et al., 2017; Vierula et al., 2016), and access to a research site when studying a vulnerable patient group (Gehlert & Mozersky, 2018). Research on rheumatoid arthritis is expected to grow along with the development of technologies and advanced research methods (Cassotta et al., 2020), thus obligating researchers to commit to ethical standards and good scientific practice. However, a systematic review of ethics in foot health research among patients with rheumatoid arthritis is lacking.
Aim
The aim of this study was to analyze the reported research ethics of peer-reviewed empirical studies focusing on foot health in patients with rheumatoid arthritis as research participants. The ultimate goals were to provide information about the quality of reported research ethics, enhance ethical discussions in the field of foot health research, and promote a high ethical standard in foot health research.
The following questions were set:
What was the justification to conduct the study reported? How were ethical approval and permission for data collection obtained? How was informed consent obtained?
Methods
A systematic review was conducted to synthesize information on research ethics from empirical studies that focus on foot health in patients with rheumatoid arthritis. The present study followed good scientific practices in every phase (Allea, 2017). The Preferred Reporting Items for Systematic Reviews and Meta-Analyses (Page et al., 2021) were used to guide this review.
Literature Search
The articles were identified through a systematic literature search of the MEDLINE (PubMed), CINAHL, and Embase databases (Figure 1). The search was conducted on each database from the earliest available to March 31, 2021 and was limited to the English language and title/abstract level. The search terms included the following: rheumatoid arthritis AND (foot OR feet) AND (problem* OR disorder* OR complaint* OR patholog* OR deformit* OR disabilit* OR condition*). The search returned 1,653 records: 631 from Medline/PubMed, 58 from CINAHL, and 964 from Embase.
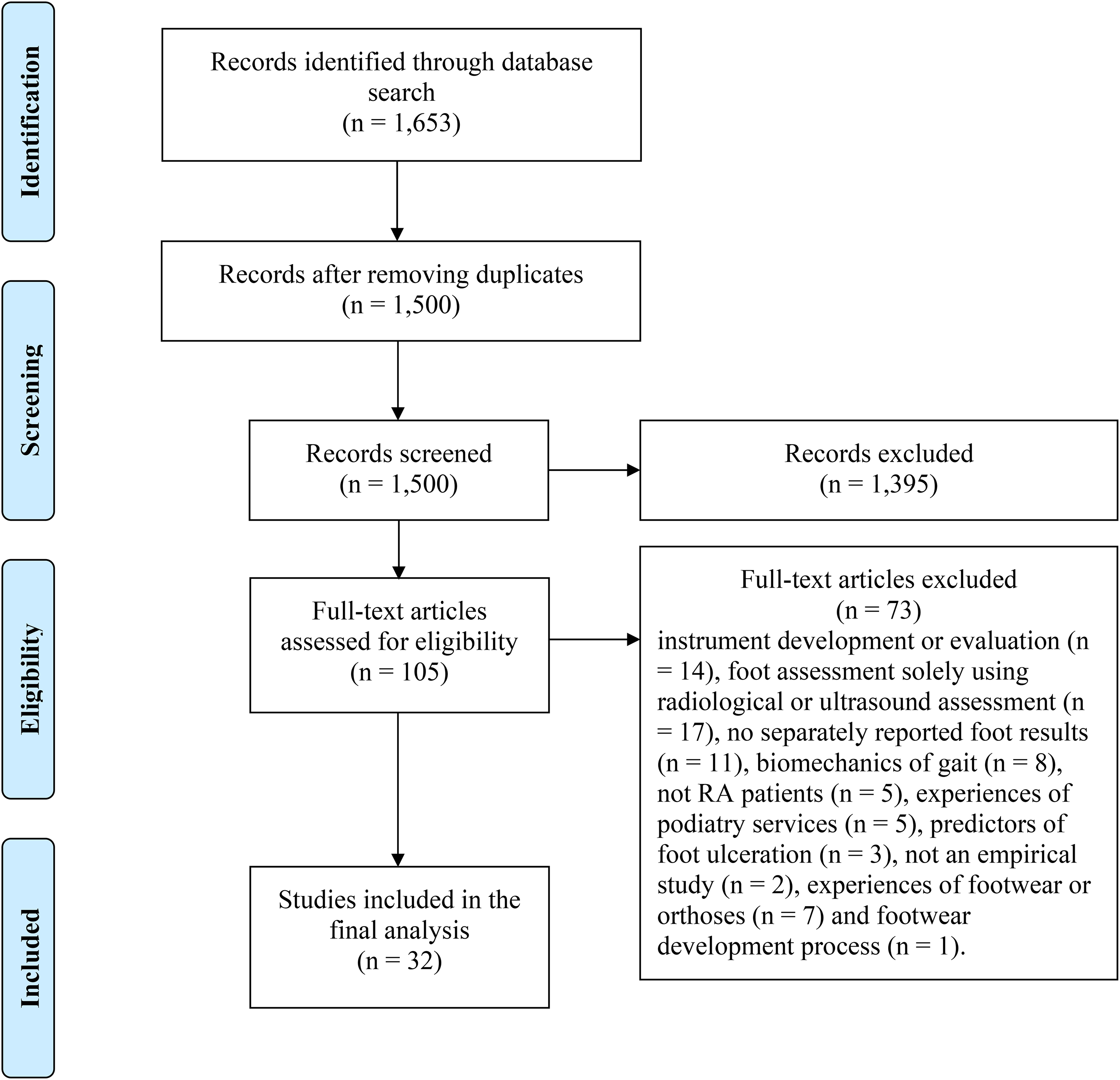
Flow chart of the literature search and retrieval process.
Inclusion and Exclusion Criteria and Data Retrieval
Predetermined inclusion and exclusion criteria were applied throughout the retrieval process (Table 1). The data retrieval process consisted of three phases, where two researchers (MS, EK-V) worked independently and discussed which records were to be included in the next phase. First, in the screening phase, after removing duplicates (n = 153), all the remaining 1,500 records were screened on the title and abstract levels against the inclusion and exclusion criteria. A total of 1,395 records were excluded, resulting in 105 records for full-text analysis. Next, the full-texts were inspected, leading to the exclusion of 73 records because they reported instrument development or evaluation (n = 14), foot assessment using solely radiological or ultrasound assessment (n = 17), foot health results were not reported separately (n = 11), the focus was on the biomechanics of gait (n = 8), patients with rheumatoid arthritis were not study subjects (n = 5), described experiences of podiatry services (n = 5), predictors of foot ulceration (n = 3), experiences of footwear or orthoses (n = 7), footwear development process (n = 1), or were not empirical studies (n = 2). Finally, 32 records were included in the review and final analysis stages.
Inclusion and Exclusion Criteria.

Data Extraction and Analysis of the Studies
The following descriptive information were gathered from each study in a separate spreadsheet: author, year of publication, country of origin, main topic under investigation, design, data collection method, setting, and number of participants. Related to research ethics a separate table was formed and following aspects were gathered from the studies: how ethical approval was obtained and from which organization or body, the method of requesting informed consent and the form (oral or written), and the person who gave informed consent. Further, the process of informed consent was examined following the procedure in the Belmont report (Belmont Report, 1978), which consists of three phases: (1) providing information about the study, (2) possibility of discussing the study and opportunity to ask questions, and (3) informed consent to participate. Finally, all possible statements or considerations related to research ethics described in any part of the article were examined. The data were analysed with content analysis and quantification.
Results
Description of the Studies
Most of the studies (n = 18, 56%) were conducted in Europe, of which the majority (n = 8) were in the UK, followed by the Netherlands (n = 5), Spain (n = 2), and one in Poland, Portugal, and Sweden. Five studies were conducted in New Zealand, two in the United States, and one in Australia, Brazil, Colombia, Iran, Japan, Korea, and Turkey (Table 2).
Characteristics of the Studies (n = 32).
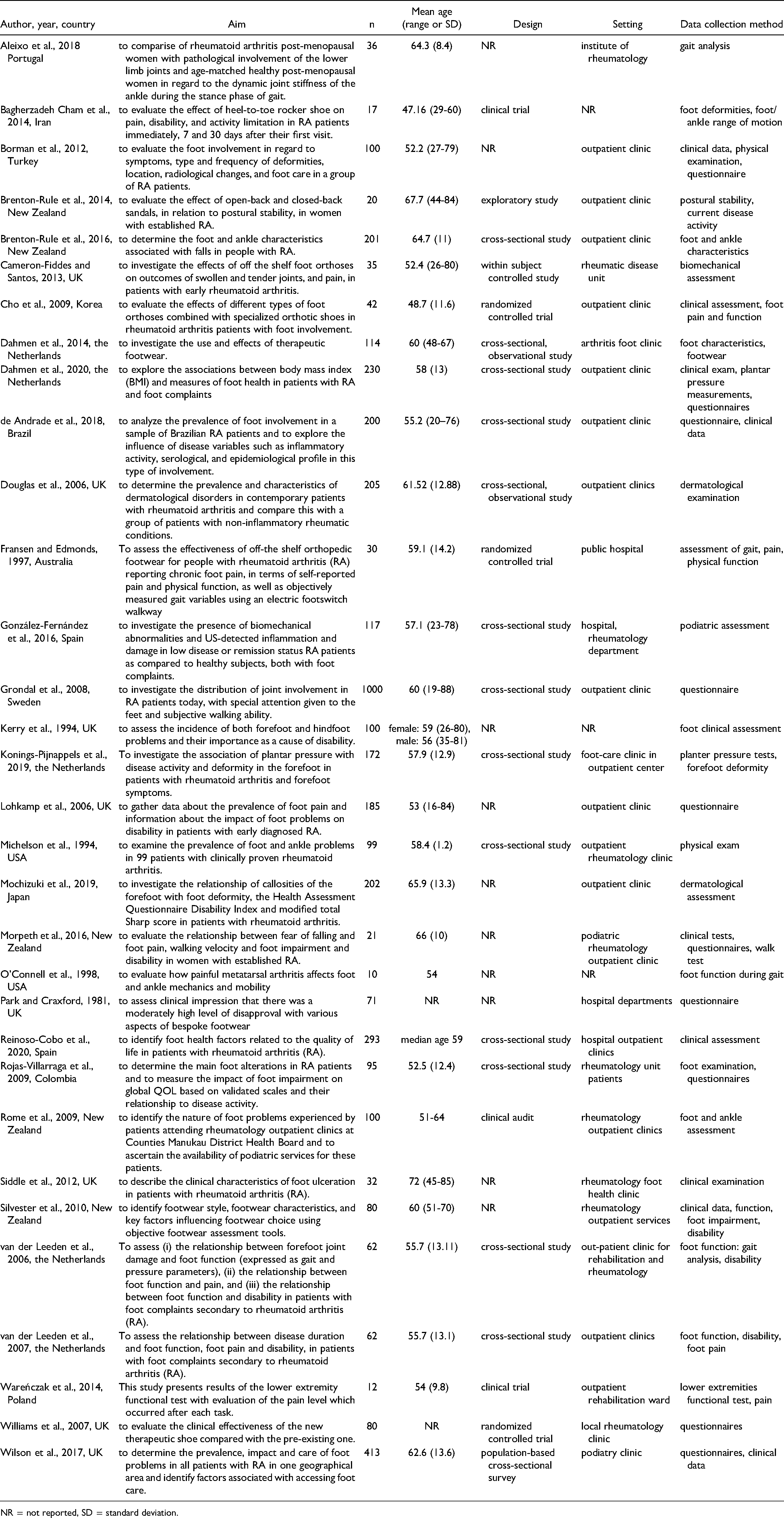
NR = not reported, SD = standard deviation.
The most common focus in the original studies was on foot deformities in patients with rheumatoid arthritis (n = 17, 53%), followed by therapeutic footwear or orthoses (n = 9, 28%) and foot function (n = 6, 19%). The number of participants in the study varied between 10 and 1,000. Participants were adults whose mean age in years varied between 47 and 72 years. The most common design used in the studies was a cross-sectional study design (n = 14, 44%). The studies were predominantly conducted in outpatient clinics for patients with rheumatoid arthritis (n = 22, 69%). In four (13%) studies, the setting was a clinic, a unit, or health care services in general for patients without any information regarding whether the patients were inpatients or outpatients.
Reporting the Justification to Conduct the Study
In all the studies, the justification for conducting a particular study was presented. The reasons for conducting the study were either to identify knowledge gaps in previous studies, to test a new therapeutic method, or to update existing knowledge.
Reporting of Ethical Approval and Permission for Data Collection
Ethical approval and the review body (ethics committee) were reported in most of the studies (n = 26, 81%, Table 3). The types of ethical review boards were independent review boards located in universities (IRBs), or anonymous local ethical committees. A few studies (n = 3, 9%) also reported reference to either international or national ethical standards. However, only one study separately reported permission to conduct the study (Cameron-Fiddes & Santos, 2013).
Reported Ethical Approval and Informed Consent in the Studies (n = 32, in Alphabetical Order).
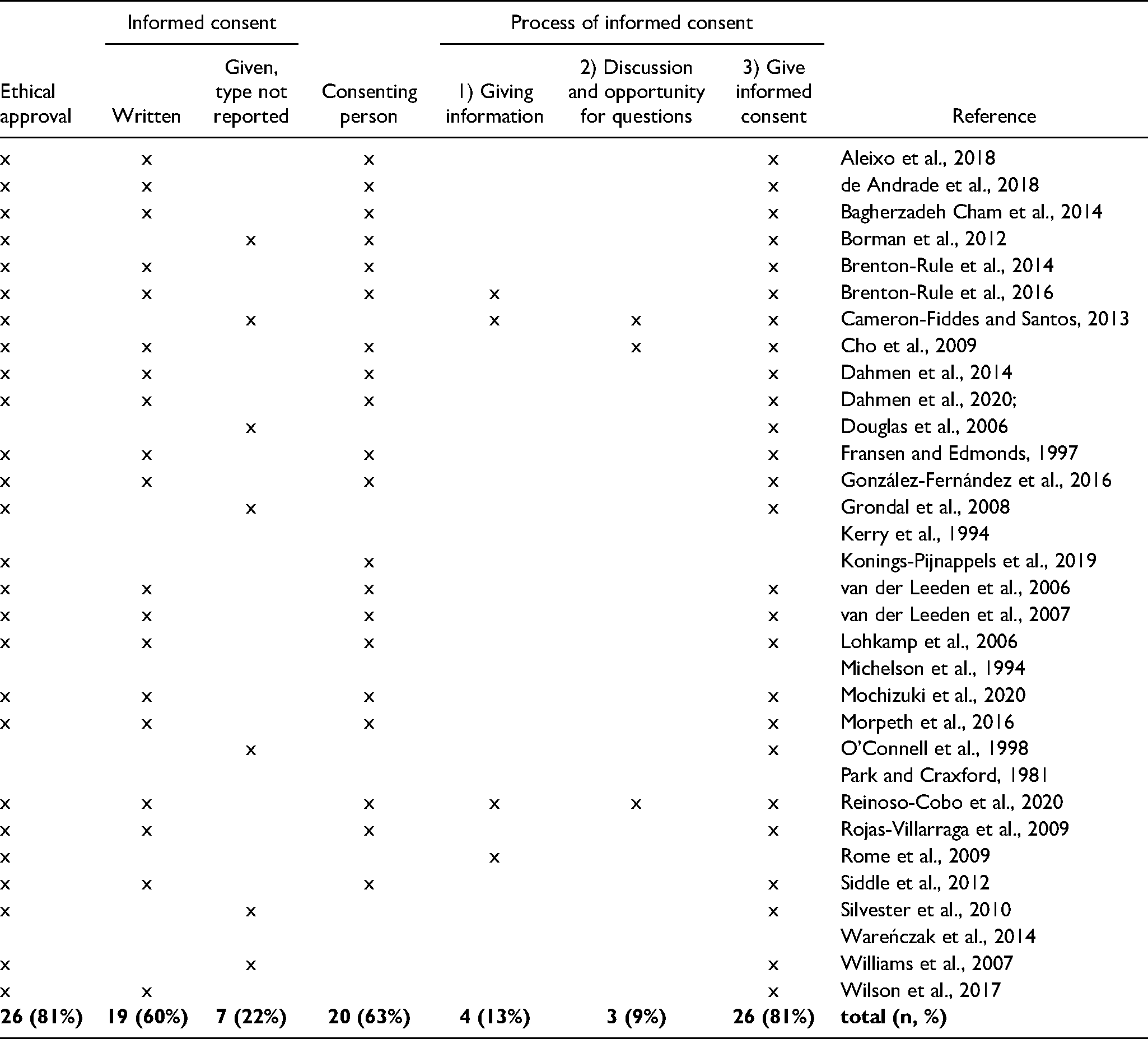
Obtaining Informed Consent
Most studies (n = 26, 81%) obtained informed consent (phase 3 according to the Belmont report, 1978), majority (n = 19) of which obtained a written informed consent. However, in only a small number of studies (n = 2, 6%) the informed consent process was reported, including providing information (phase 1 according to the Belmont report). In addition, only a few studies (n = 3, 9%) reported a discussion about the study and the opportunity to ask questions (phase 2 according to the Belmont report) (Table 3). The persons who gave informed consent were the participants themselves, and this was reported in most (n = 20, 63%) of the studies.
Discussion
This review demonstrated that research ethics of empirical studies focusing on foot health in patients with rheumatoid arthritis as research participants are insufficiently discussed and described. This finding supports previous studies in other areas (Suhonen et al., 2013; Wu et al., 2019) and confirms the need to improved transparency and standards of ethical reporting (Wu et al., 2019).
Ethical approval and the body reviewing the study were reported in most of the studies. Obtaining informed consent was also reported in most of the studies, but permission from organization or hospital to conduct the study was reported only in one study; thus, it is unclear whether permission to conduct the study was granted by the organization or institution from which the data were collected. This may indicate that informed consent is more important when reporting study ethics. The discrepancy in reporting permission to conduct the study could be related to the varying approving bodies. The studies in this review were conducted in different countries, which may have different procedures for ethical approval and organizational permission to conduct a study. In some countries, ethical approval is first considered by an IRB within a hospital and, if approved, in line with internal delegation, permission to conduct the study is decided by the responsible body of the unit or sector in which it is planned to be conducted. In some countries, the same body, such as an IRB in a hospital, can provide both ethical approval and permission to conduct the study, whereas in other countries, for example, ethical approval is sought from a university ethical review board, while permission to conduct the study is obtained from a particular organization. However, the reporting of these permissions should be clear and unambiguous (Dunn & Jeste, 2001; Taljaard et al., 2014).
Reporting of the informed consent process was fragmented. Only a few studies have described the entire informed consent process, following the Belmont report (1978). Notably, there were some studies where the informed consent process was not reported at any level, although this does not automatically mean that informed consent was not obtained. However, scientific journals and publishers are increasingly asking for a statement on the ethics of the study during the submission process. In future studies, thorough reporting of research ethics is needed, particularly on issues related to informing participants of their rights. The articles identified in this review seldom reported on anonymity, confidentiality, and voluntariness, which are basic ethical requirements in data collection. This indicates that it is necessary to include a detailed description of data collection in the articles’ methodology section to increase critical thinking and ethical reasoning, particularly in studies with invasive research methods. According to the literature, organized, shorter, and more readable consent forms, simplified text, and illustrated formats may improve participants’ understanding (Kadam, 2017; Misra & Agarwal, 2020). As the foot health research is commonly conducted in clinical settings, it is important to highlight to participants what components belong to professional foot care and which to scientific foot-related research. Written informed consent was used in those studies that reported on informed consent, but no additional detailed structure or content of the informed consent was reported in the studies.
There are some limitations to be discussed before interpreting the results. This review focused on articles dealing with foot health in patients with rheumatoid arthritis. Articles related to surgical procedures, radiography, foot kinematics evaluation, and pharmacological studies were excluded because the focus was on non-invasive foot health studies. This might have limited the generalizability of the results to a wider patient population with rheumatoid arthritis or other long-term foot health conditions. However, ethical issues and requirements are similar in all patients and should be considered in every study. Finally, this review reports and synthesizes these ethical issues and the considerations that the original researchers have reported.
In summary, the reporting of research ethics in studies focusing on foot health in patients with rheumatoid arthritis is fragmented. It is predominantly focused on ethical approval and informed consent, and a wider discussion about research ethics is lacking. It is necessary to improve the level of reporting on research ethics by taking a more comprehensive perspective to include aspects of participants’ rights and research integrity. In foot health research, a high ethical standard is required across the entire research process. Research ethics should not only be seen as a prospective mechanical review of ethical issues while preparing documents for ethical approval (Dawson et al., 2019). Instead, the entire research process should be carried out in the most ethical way possible.
Best Practices
This review provides information based on descriptions in research publications; therefore, it is not possible to analyze actions that have been taken in conducting these studies in different countries. The information produced in this review can be utilized to improve the quality of reporting, procedures in empirical research, and ethics education.
Patients with rheumatoid arthritis are a sensitive group of research participants because they have long-term health problems that restrict their autonomy and daily activities. Moreover, rheumatoid arthritis causes significant changes in the shape and appearance of the feet; thus, many patients generally consider their feet to be unaesthetic and do not feel comfortable revealing their feet to others. These are ethical issues that need to be considered during the entire research process.
Research Agenda
Our findings highlight the need for further research on research ethics. The present study focused on analyzing the reported research ethics in scientific publications. However, in the future, it would be beneficial to explore researchers’ perceptions of issues related to reporting research ethics. This study focused only on a narrow group of patients; thus, in the future, it would be interesting to analyze how reporting of research ethics has been conducted among other patient groups.
Educational Implications
Careful consideration of the ethical aspects of reporting is mandatory for every publication. However, the reporting of research ethics from a researcher's perspective is a balancing act between tighter word limits and cohesive reporting of results. Due to limited publication space, authors tend to trim their reporting of ethics to the most central aspects, such as ethical approval and informed consent, leaving out other important ethical perspectives. As ethical guidelines and data protection regulations have become more stringent, more detailed reporting of research ethics is needed. Scientific publishers could consider extending word limits and requiring a comprehensive description of research ethics. Open access publishing could provide a forum for this type of reporting. The Ethical Review Boards could provide education for researchers about research ethics and remind that reporting research ethics is as important as ethical approval.
Source of Support:
This study was supported by the Turku University Hospital (funding reference 2018/13240).
Footnotes
Author Contributions
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Turun Yliopistollinen Keskussairaala (grant number 13240).
