Abstract
Introduction
Social media is a significant platform for health information. However, the quality and reliability of patient facing surgical content is uncertain. We evaluated the quality and reliability of TikTok and Instagram videos about three common general surgical procedures: laparoscopic appendicectomy; laparoscopic cholecystectomy; and inguinal hernia repair, and compared performance by platform, procedure, and creator type.
Methods
We conducted a cross-sectional study of the top fifty results per procedure per platform. Videos were classified as useful, misleading, personal experience, or irrelevant and quality and reliability assessed with the Global Quality Score (GQS) and modified DISCERN (mDISCERN) score respectively.
Results
300 videos, accruing 592,975 likes and 11,489 comments, were analysed. Videos were low in both quality and reliability across both platforms although higher on Instagram (GQS 1.95; mDISCERN 1.65) than TikTok (GQS 1.27; mDISCERN 0.33; both P < .0001). 53/300 (17.7%) videos were judged to be misleading. Useful content was less frequent on TikTok than Instagram (14/150, 9.3% vs 82/150, 54.7%; P < .0001). Professional content was deemed more useful than that of non professionals (54/117, 46.2% vs 42/183, 23.0%; P < .0001) with higher quality and reliability scores (GQS 1.80 vs 1.49; mDISCERN 1.36 vs 0.76; both P < .0001).
Conclusions
Surgical educational videos across popular social media platforms are low in quality and reliability. Patients should be wary of the risk of possible health misinformation. Clinicians and professional bodies should be aware of the growing popularity of social media and consider the production of evidence-based content on these platforms to disseminate credible information and counter misinformation.
Introduction
Social media has transformed how patients access health information. In 2025, over 5 billion people were estimated to participate actively in social media, with the highest usage among adolescents and young adults, who increasingly prefer short-form, visually driven content. 1 TikTok and Instagram, whose algorithms prioritise brevity and engagement, now compete with or even surpass traditional platforms like YouTube for health-related information.2-4 Within healthcare, social media serves multiple roles ranging from patient education, research dissemination, and public health messaging.5-7 In surgical disciplines, the “SoMe” (social media) movement has been used to disseminate operative tips, support trainee education, and engage patient communities.8,9
However, the speed and visual appeal that make these social media platforms appealing can encourage oversimplification and permit the rapid spread of health misinformation. During the COVID-19 pandemic, TikTok registered more than 93 billion views of coronavirus-related videos in a single month with unverified, unregulated content fuelling health misinformation and disproportionately impacting minoritised communities already facing structural barriers, medical mistrust, and unequal health outcomes.10,11 This volume of misleading content amounted to an “infodemic” where health misinformation can spread faster than evidence ultimately overwhelming the public’s ability to find trustworthy guidance and undermining public health responses. 12
The direct relevance to surgery is significant. Inaccurate or incomplete depictions of indications, risks, benefits, recovery, and alternatives can undermine patient decision-making and informed consent. Expectations of surgery can be distorted leading to heightened anxieties and erosion in clinician trust potentially delaying presentations in time-critical conditions.13-15
Previous assessments of surgical education through online video platforms have focused predominantly on YouTube, where studies have largely demonstrated low to moderate quality and variable reliability through validated tools such as Global Quality Score (GQS) and modified DISCERN (mDISCERN).16-19 Despite the growing popularity of TikTok and Instagram, evaluation of their surgical educational content has not been performed. Whether platforms primarily designed for entertainment purposes can deliver accurate, clinically useful patient education at scale is unknown. This study aims to address this gap through the evaluation of the quality and reliability of TikTok and Instagram videos on three common general surgical procedures – laparoscopic appendicectomy, inguinal hernia repair, and laparoscopic cholecystectomy – and by examining differences across platforms, procedures, and creator types.
Methods
We performed an observational, cross-sectional analysis of publicly accessible short-form social media videos across two popular social media platforms, TikTok and Instagram. As this study required only analysis of public online data without interaction, formal ethics committee approval was not required as per the UK National Health Service Health Research Authority decision tool.
To minimise algorithmic bias from prior personal search activity, we created new TikTok and Instagram accounts used solely for data collection. For each platform, we retrieved the top 50 results for the terms “laparoscopic appendicectomy/appendectomy,” “laparoscopic cholecystectomy,” and “inguinal hernia repair,” yielding 300 videos (150 per platform). While this approach standardises account status and search terms, both platforms use recommendation algorithms that may present different videos over time or across users. As a result, the exact set of videos identified in this study may not be fully reproducible, even when identical search terms and account settings are applied. These general surgical procedures were selected because they are common, standardised operations frequently searched by patients and trainees, making them ideal cases for assessing the accuracy of publicly available content. Videos were deemed eligible if English-language, publicly accessible, and primarily aimed at informing patients about the nature, process, risks and benefits, or recovery related to these procedures. Non-English, non-public, or non-educational videos were excluded.
The Global Quality Score Taken From 20

The Modified DISCERN Score Ranging From 0-5 With 1 Point Scored for Each Domain. Table Taken From 20
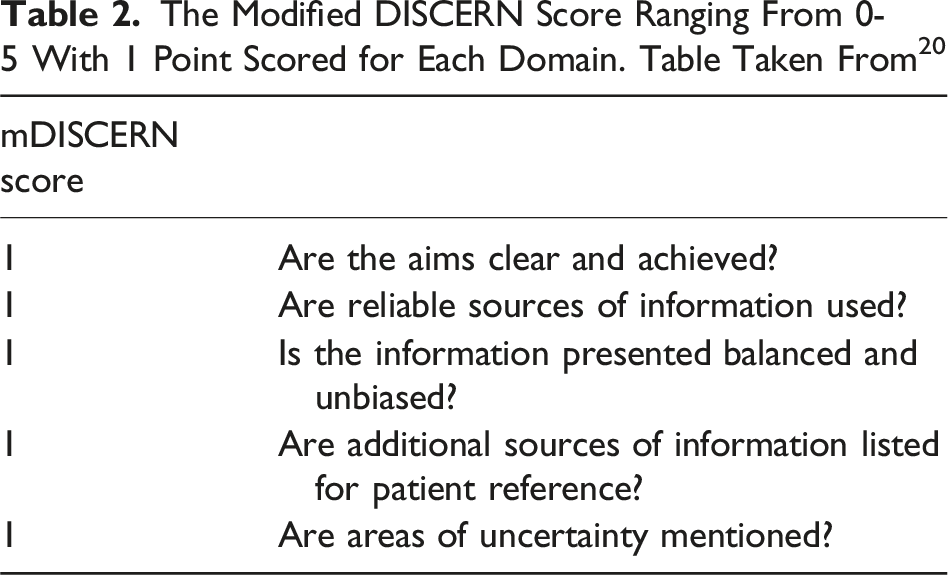

Two independent reviewers (NO and NE) assessed each video with disagreements resolved by a third reviewer (KL). Inter-rater reliability was quantified using quadratic-weighted Cohen’s κ with 95% confidence intervals estimated via non-parametric bootstrap (1000 iterations). Comparisons of proportions were performed using χ2 tests with ordinal and continuous measures compared using t-test for two-group contrasts and one-way ANOVA tests for three-group contrasts. Statistical significance was set at P = .05. All analyses were performed in Python (v3.11) using scikit-learn.
Results
We analysed 300 videos in total, 150 from TikTok and 150 from Instagram, accruing a total of 592,975 likes and 11,489 comments. No videos contained identifiable patient information. The overall agreement between raters was substantial (κ = 0.863, 95% CI 0.824-0.898).
Platform-Level Findings
Quality, Reliability, and Engagement Metrics by Social Media Platform
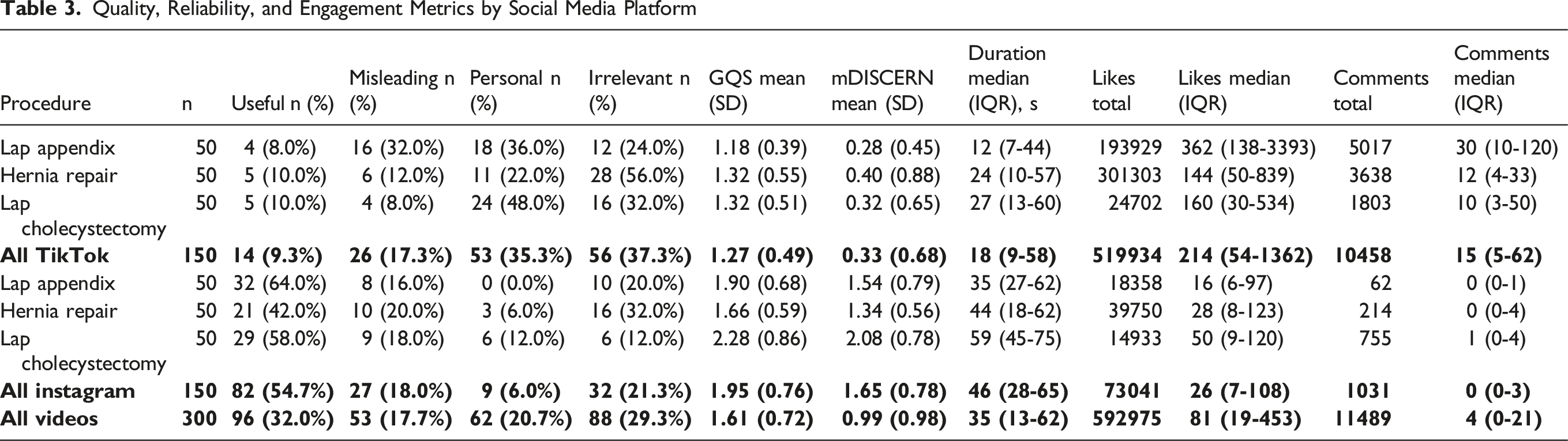
Procedure-level Comparisons
Across procedures, the proportion of videos rated useful did not differ significantly (P = .276). GQS and mDISCERN scores varied by procedure (P = .005 and 0.034 respectively), with the highest mean scores for both observed for laparoscopic cholecystectomy.
Creator-type Comparisons
Quality, reliability, and Engagement Metrics by Creator
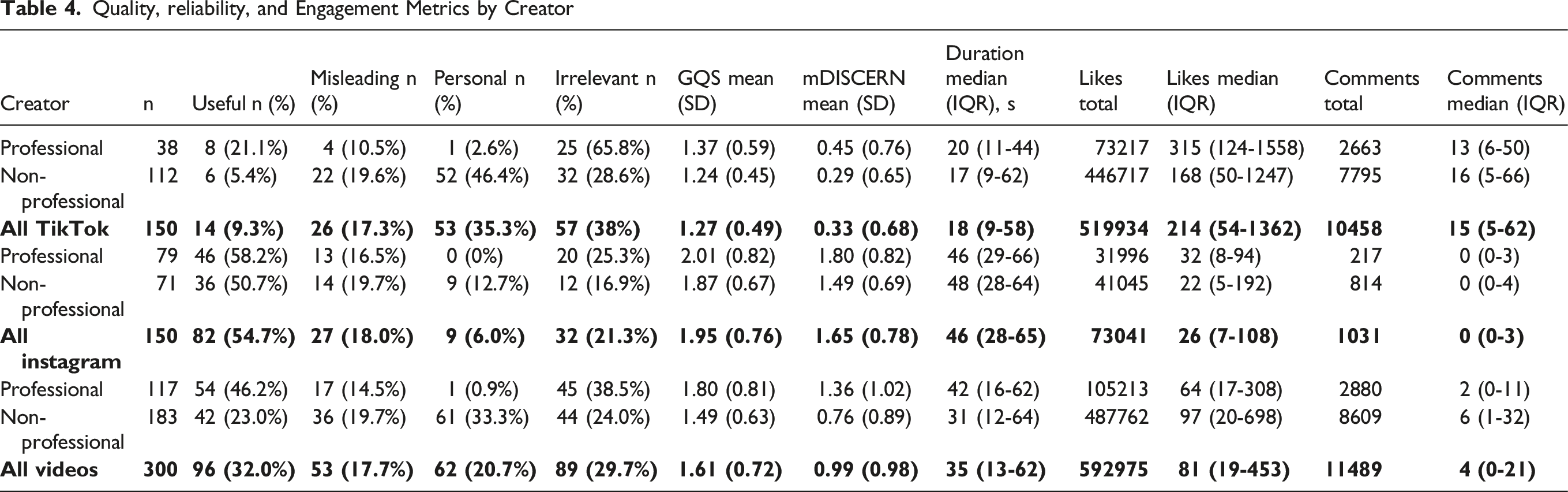
Non-professional TikTok videos were more often personal (52/112, 46.4%) than professional TikTok videos (1/38, 2.6%), while professional TikTok uploads more frequently fell into the irrelevant category (25/38, 65.8%) than non-professional TikTok uploads (32/112, 28.6%). No personal content was identified among professionals on Instagram (0/79, 0%) but this was present among non-professionals (9/71, 12.7%).
Discussion
This study represents the first systematic evaluation of TikTok and Instagram as vehicles for delivering surgical education to patients. While prior research has largely focused on YouTube as the dominant platform for medical information, the rapid growth of short-form, algorithm-driven media has shifted public information-seeking behaviour toward newer, highly engaging formats. TikTok and Instagram, with their billions of active users and personalised content feeds, have become central sources of health-related information particularly among younger, digitally native audiences who may be less inclined to consult traditional sources, representing a shift to image and video-based platforms, illustrating a preference for visual content endorsed by influencers with mass followings, over professionally disseminated information. 21 However, there is a clear conflict between this usage and the design of these platforms, which fundamentally prioritises entertainment and engagement over education.
Consistent with prior YouTube-centric evaluations, videos on these social media platforms underperformed on quality and reliability when assessed with validated instruments.16-19 Although Instagram outperformed TikTok across all primary endpoints, absolute scores on both platforms were low, demonstrating the distance between what patients currently encounter and what is desirable for informed decision-making.
Despite these clear deficiencies in accuracy, depth, and educational value, however, the content analysed achieved high levels of reach and engagement. It is of concern that almost 20% of videos were judged to be misleading. The most widely circulated posts accrued thousands of likes, shares, and comments, suggesting that such material is routinely exposed to large audiences. This level of dissemination underscores the disproportionate influence that even a small proportion of inadequately produced or misleading content can have on public perceptions of surgical practice. Surgeons should be wary of the dangerous combination of high reach and low quality or even false information as such content risks widening disparities by amplifying fear of surgery, delaying presentation for urgent conditions such as appendicitis, and eroding trust during consent encounters.
It is noteworthy to highlight the differences found between TikTok and Instagram. TikTok’s emphasis on brevity and engagement favoured visually striking videos with simplified narratives resulting in sacrifices to balanced patient information, such as alternatives, complications, and realistic recovery timelines.
Comparative analysis by creator type indicates that professional accounts outperformed non-professional accounts on all metrics: a higher proportion of videos were rated useful; and mean GQS and mDISCERN scores were higher for professional creators across both platforms. It is notable that professional posts had lower reach, with lower median likes and comments than non-professionals. This is however unsurprising when considering the fact that non-professional content is often created specifically to generate engagement rather than to educate.
It is of concern also that within these platforms, recommendation systems are likely to privilege engagement over provenance.
Importantly, these results raise broader questions about the evolving landscape of patient education. Beyond individual clinicians, formal educational accounts led by professional societies, academic departments, and established surgical practices could play a central role in raising the baseline quality of surgical information on short-form platforms. These organisations are well positioned to develop evidence-based videos aligned with guideline-recommended care, to implement internal peer-review processes for footage prior to publication, and to maintain ongoing moderation, including timely correction or removal of outdated material. Partnerships between societies, universities, and patient advocacy groups could also support multilingual adaptations, co-creation of content with patients, and dissemination through verified institutional accounts, therefore increasing both the visibility and perceived trustworthiness of high-quality surgical content.
The speed, accessibility, and emotional appeal of short-form video make it a powerful tool for shaping understanding, yet these same features create vulnerabilities: algorithmic promotion rewards attention-grabbing content over accuracy, and users are often ill-equipped to discern credible information from misinformation. 22 By systematically characterising how surgical topics are presented and received on TikTok and Instagram, this study not only fills a gap in the current literature but also emphasizes the urgent need for clinicians, professional bodies, and educators to engage proactively with these platforms. Surgical teams and professional societies should adapt evidence-based materials to short-form conventions, for example, producing succinct risk-benefit summaries with clear on-screen captions while maintaining fidelity to best evidence. Professional partnerships with social media platforms could allow quality signalling, for example through trusted health source labels or labelling of non-verified content and explore up-ranking of verified educational content around surgical keywords. These partnerships will aim not only to make high-quality, evidence-based information available but also ensure it is competitive in visibility and appeal when compared with less reliable sources.
The present study exhibits several methodological strengths that enhance the validity and reliability of its findings. By employing an observational, cross-sectional design, the study provides a representative snapshot of current surgical education content on TikTok and Instagram. The use of newly created accounts minimised algorithmic bias, ensuring that video selection reflected publicly available content rather than personalised search histories. A comprehensive sampling strategy which collected the top 50 videos per procedure per platform ensured broad coverage of relevant content, while clear inclusion and exclusion criteria restricted the analysis to English-language, publicly accessible, patient-focused educational material, thereby enhancing comparability across platforms. Methodological rigor was further strengthened by the adoption of a structured analytical framework based on previously published categorisation methods, and the utilisation of validated assessment tools, including the GQS and mDISCERN instrument, to evaluate video quality and reliability. Each video was independently reviewed by two assessors, with inter-rater reliability calculated to ensure objectivity, and additional metadata, including engagement metrics, video length, and the presence of patient-identifiable information, was systematically recorded. Collectively, these design features provide a robust approach to evaluating the quality and reliability of social media content for patient education and offer a reproducible framework for future research in this emerging area.
However, this study is subject to several important limitations. First, the dataset comprised only 300 videos, representing a relatively small sample given the vast quantity of content available on these platforms. Second, despite the use of newly created accounts, personalised recommendation algorithms can present different content to different users or at different time points, therefore limiting the strict reproducibility of our video sample even when the same search terms are applied. Third, the analysis was restricted to English-language material, excluding potentially relevant content in other languages. Moreover, while established tools such as the GQS and mDISCERN instrument were employed, no universally accepted framework currently exists for evaluating the quality of health information within social media contexts, limiting the comparability of results across studies. Engagement metrics, while practical, may not be perfect proxies for reach and they fail to capture impressions or watch time. Finally, despite efforts to standardise the review process, subjective judgement and inter-rater variability remain potential sources of bias.
Practical Implications for Clinicians and Professional Bodies
Based on our findings, clinicians and professional organisations seeking to use short-form social media for surgical education should consider several practical principles. Firstly, content should prioritise accuracy and completeness over entertainment and engagement, explicitly addressing key information, for example, indications, alternatives, and red-flag symptoms within the constraints of short-form formats and linking to reputable longer-form resources where needed. Secondly, creators should adopt transparent practices, including clear disclosure of professional status, institutional affiliation, and the date of content creation or last review, as well as avoiding promotional language that could be perceived as advertising. Thirdly, internal peer-review processes within departments, hospitals, or societies could help ensure that content reflects current guideline-concordant practice. Finally, professional bodies, universities, and formal surgical practices could create template series which can be adapted locally while maintaining core evidence-based messages.
Clinicians should anticipate that an increasingly digitally literate population will encounter surgical information first on short-form social media platforms. To remain ahead of the curve, development and evaluation of targeted interventions to improve the quality and accessibility of surgical education on social media should be prioritised. This could include collaborations between platforms and professional surgical societies, patient advocacy groups, and platform developers to create verified, evidence-based content, as well as the use of algorithmic strategies to prioritise high-quality educational material. Technological advances, for example through Generative AI, may also allow rapid content production, but human expert review will remain essential for accuracy and safety for now.23,24 Digital literacy campaigns aimed at helping patients critically appraise online surgical information should also be championed and could help to mitigate the influence of misleading or oversimplified content. 25 Evaluating the impact of such interventions on patient knowledge, decision-making, and postoperative outcomes would provide critical insights into strategies for integrating social media into safe and effective patient education.
Future research should analyse larger and more representative samples of content while accounting for variability introduced by personalised recommendation algorithms. Multilingual evaluations will be essential to fully characterise the global reach and influence of platforms such as TikTok and Instagram, especially when considering the health misinformation effects on minority population groups. In addition to content appraisal, patient and public involvement will be crucial to assess downstream effects of surgical misinformation on knowledge, anxiety, and help-seeking.
Conclusion
Short-form videos on social media platform have an increasingly growing reach and are emerging as an important medium for surgical information distribution. In this study of three common general surgical procedures, the majority of TikTok and Instagram videos offered limited educational quality and reliability. Surgeons should be aware of this potentially hazardous combination of high reach and low quality for informed consent and expectations of surgical care. However, the popularity of social media also represents an opportunity for surgeons and professional organisations to collaborate proactively with these platforms and produce high quality, engaging short-form content to elevate credible information for patients.
Footnotes
Author Contributions
NO: Data collection, Data analysis, Manuscript drafting.
NE: Data collection, Manuscript revision.
KL: Conceptualisation, Methodology, Data analysis, Manuscript drafting, Manuscript revision, Supervision.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was not funded however KL receives support from a NIHR Clinical Lectureship.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
