Abstract
Background
Our study aimed to compare the effects of repair using polypropylene suture material vs polyglycolic acid-coated (PGA) tube on the development of biliary strictures in rat common bile duct incisions.
Methods
Thirty female rats were randomly divided into three groups. A controlled defect was created in the common bile duct. In Group 1, the defect was repaired with 8/0 polyglycolic acid; in Group 2, with 8/0 polypropylene; and in Group 3, with 8/0 polyglycolide-co-lactide followed by wrapping with an absorbable polyglycolic acid mesh tube. In the second surgical step, at 3 months postoperatively, blood samples were again taken from all subjects, liver biopsies were obtained, and the repaired bile duct area was resected for histopathological evaluation. Liver biopsies obtained before bile duct repair and at 3 months after repair were compared among the groups. Anastomotic sites and proximal bile duct diameters were compared between groups at 3 months post-repair.
Results
Postoperative ALT and GGT levels were significantly higher in Group 1 rats, while ALP levels were statistically significantly lower in Group 2 rats. Epithelial hyperplasia was detected in 20% of rats in Group 3, with fewer proliferative fibroblasts and less collagen scar tissue compared with those in other groups. The Portal edema rate was significantly lower in Group 3 than in Groups 1 and 2.
Conclusions
The use of PGA –coated tubes after PGLA suturing suggests that these tubes may reduce strictures in biliary repair in rats by maintaining a wider anastomotic diameter.
Introduction
Narrowing of the bile duct with subsequent dilation of the proximal segment is defined as a biliary stricture. 1 Approximately 30% of its etiology is attributed to benign conditions, most commonly iatrogenic causes during laparoscopic cholecystectomy. 2
While iatrogenic injuries related to cholecystectomy are the leading cause of bile duct injuries, they can also occur, albeit rarely, during trauma, choledochal exploration, gastric surgeries, duodenal Kocher maneuvers, and hepatectomies. 3 The surgical management of bile duct injuries varies depending on the level, type, classification grade, and timing of the injury. Early detection of injuries during surgery is crucial to prevent stricture formation.
End-to-end ductal anastomosis is a physiological biliary reconstruction used in liver transplantation and in the repair of iatrogenic bile duct injuries. Besides ensuring proper digestive and absorptive function in patients undergoing end-to-end ductal anastomosis, it facilitates postoperative endoscopic diagnostic and therapeutic procedures.
Various techniques and suture materials can be employed during surgical repair. Conduits are tubular materials designed to overcome the adverse properties of autografts.4,5 Conduits are commonly used in nerve repair, promoting tubular formation during nerve regeneration and reducing fibrotic processes.6,7 One such conduit, coated with polyglycolic acid facilitates oxygen transfer from tissues, allows passage of bioactive substances, and promotes fibroblast proliferation.8-10
While there are numerous studies on polyglycolic acid-coated conduits in nerve repair in the literature, there is a lack of research on their application in biliary tract repair. Our study aimed to compare the effects of repair with polypropylene suture material vs a polyglycolic acid-coated tube on the development of biliary stricture in incisions of the rat common bile duct.
Methods
Groups
The study was designed as a two-stage surgical procedure. In the first surgical step, blood samples were collected for biochemical analyses. Subsequently, a controlled defect was created in the common bile duct; the repair was performed using different suture materials during the same session, followed by a liver biopsy. In the second surgical step, blood samples were collected for biochemical analyses. Liver biopsy and resection of the repaired area of the bile duct were performed for histopathological evaluation. The interval between the first and second surgical procedures was planned to be three months.
Under an operating microscope at 6× magnification, the abdominal cavity was entered through a 3-cm median incision below the xiphoid process. The common bile duct was explored, dissected from surrounding tissues, including the portal vein, and mobilized. A controlled 180° defect was created on the anterior surface of the distal bile duct with a scalpel. Following these standard procedures, the rats were divided into three groups: 1. Group 1 (n = 10): A defect in the bile duct was repaired primarily under an operating microscope at 6× magnification using 8/0 polyglycolic acid (%90) and lactide (%10) (PGLA) (Glycolak®) (Figure 1). 2. Group 2 (n = 10): The bile duct defect was repaired primarily under an operating microscope at 6x magnification using 8/0 polypropylene (Prolene®). 3. Group 3 (n = 10): After primary repair with 8/0 PGLA under an operating microscope at 6× magnification, the repair area was surrounded by a Polyglycolic Acid Mesh Tube (PAMT; Neurotube®) (Figure 2). Primary repair of the defect with 8/0 PGLA Steps of placement of the polyglycolic acid mesh tube after repair
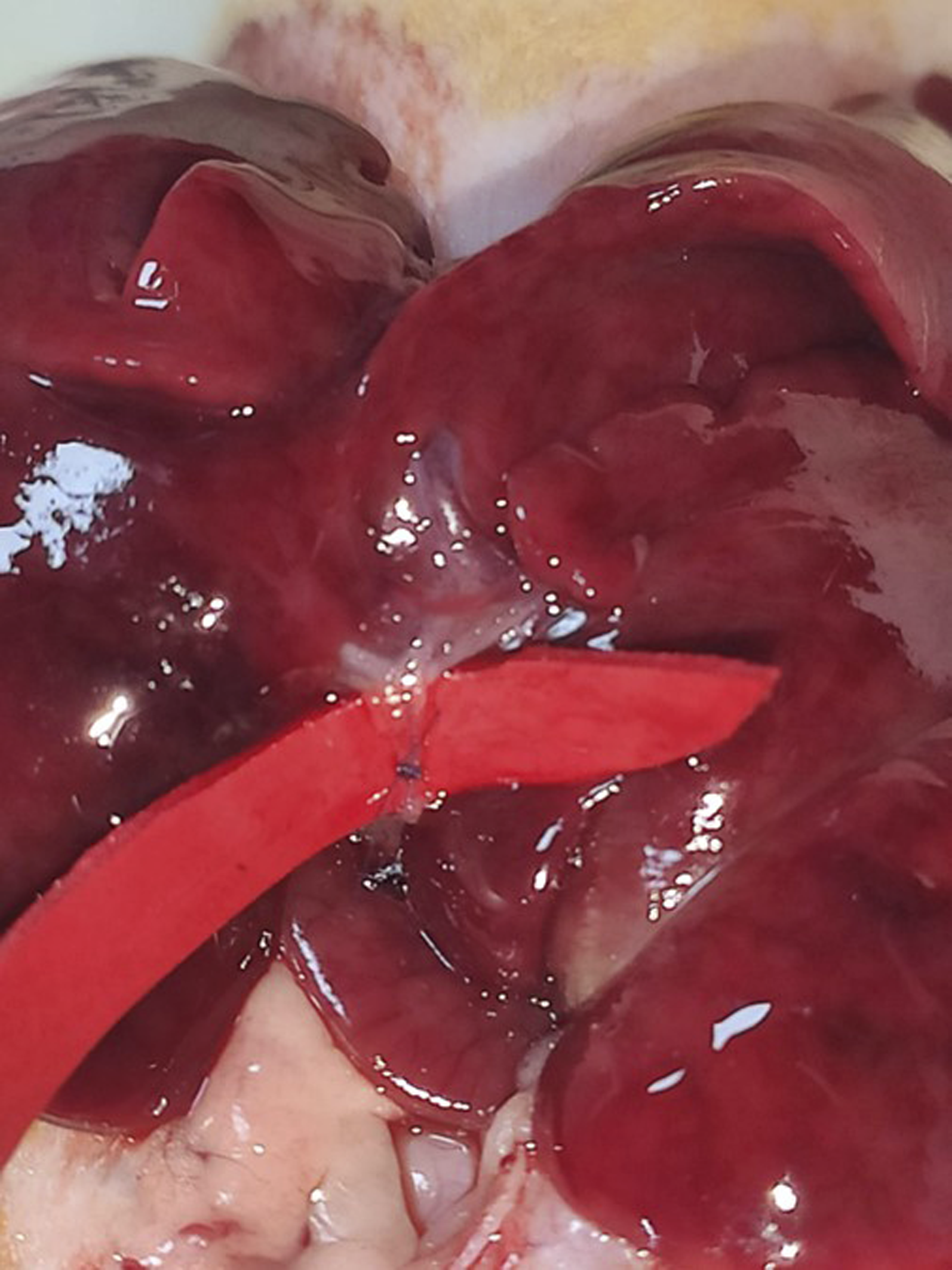
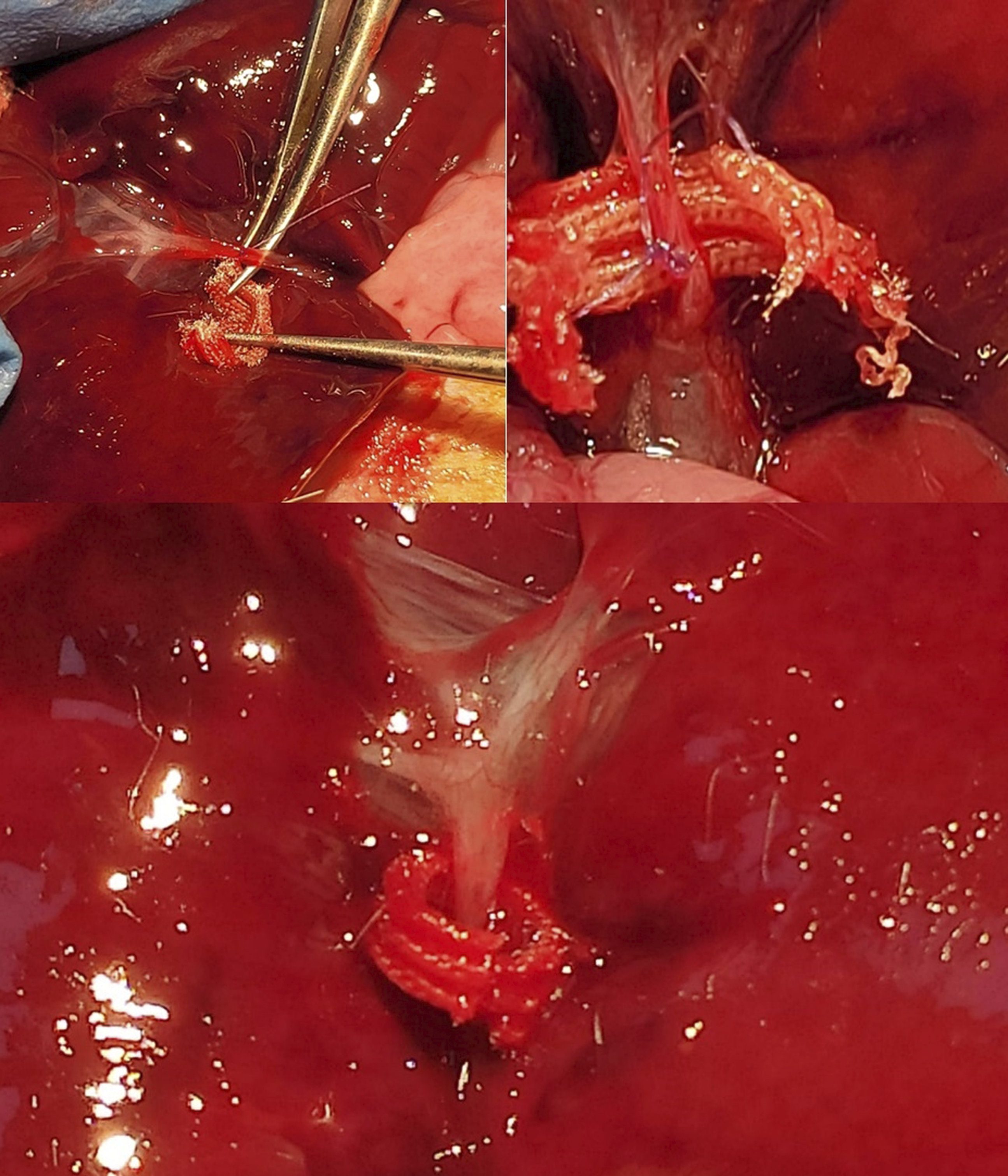
After each of the three surgical repairs, 5-mm liver biopsies were obtained from the left lateral lobe using a micromachete and stored in formaldehyde for histopathological examination.
Following the first surgical procedure, the rats were monitored under standard conditions for 3 months. No complications or losses were observed among the subjects during the follow-up period. Subsequently, the second surgical procedure was initiated.
Preoperatively, 1.5 cc of blood was collected from the tail vein of each rat into standard biochemical tubes. The abdominal cavity was entered under an operating microscope at 6× magnification. The common bile duct was explored, dissected free from surrounding tissues and adhesions, and freed from the underlying portal vein. After identifying the repair site in the bile duct, the area was resected with intact proximal and distal surgical margins. The long and short diameters of the anastomotic site and proximal bile ducts were measured in micrometers (µm) using CellSens Standard software.
Samples were obtained and stored in 10% formaldehyde for histopathological examination, and preoperative and postoperative evaluations included total bilirubin, alanine aminotransferase (ALT), aspartate aminotransferase (AST), alkaline phosphatase (ALP), and gamma-glutamyl transferase (GGT). Liver tissue from the left lateral lobe and tissue resected from the bile duct anastomotic site and the proximal bile duct were sectioned into 4-5 μm slices for H&E staining. These sections were examined by a pathologist under a light microscope to evaluate portal edema, fibrosis, inflammation, bile duct proliferation, and cellular and tissue parameters such as polymorphs, mononuclear cells, proliferative fibroblasts, collagen scar tissue, and epithelial hyperplasia at the bile duct anastomotic site (Figure 3). (A) Polymorphous and mononuclear common bile duct, (B) Liver inflammation, (C) Anastomotic fibrosis, (D)Preoperative liver fibrosis, (E) Short-diameter anastomotic common bile duct, (F) Long-diameter anastomotic common bile duct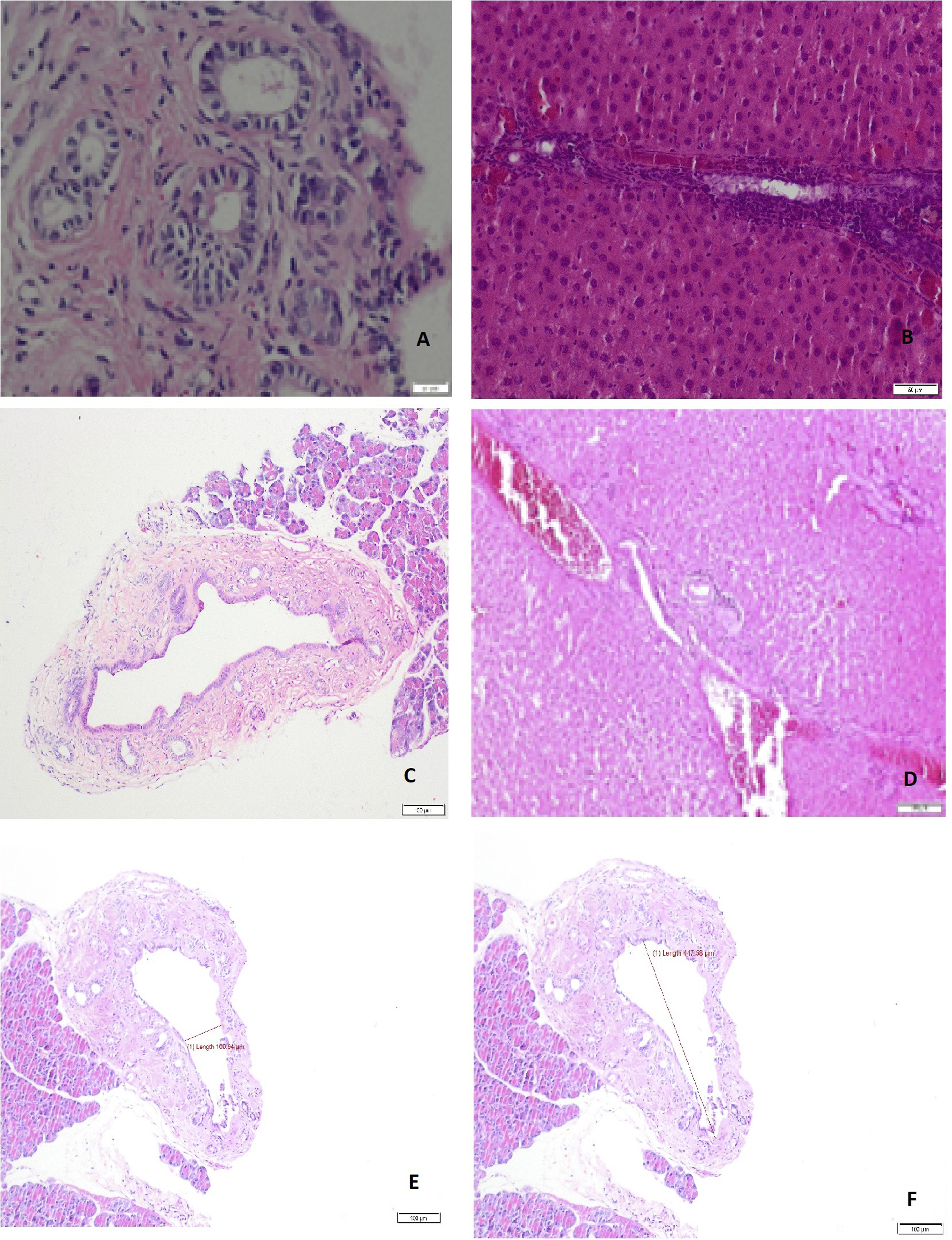
Statistical Analysis
Data obtained from all studies were analyzed using SPSS (Statistical Package for Social Sciences) version 18.0. Numerical data were presented as mean ± standard deviation (SD); frequency data were presented as number (n) and percentage (%). Chi-square (χ2) test was used to compare data across different categories. The Kolmogorov-Smirnov test evaluated whether the data were normally distributed. One-way ANOVA tests for differences in the means of numerical data among three or more groups. A post hoc analysis using Tamhane’s test was performed for parameters identified as statistically significant. Distributions of non-normally distributed data across three or more groups were compared using the Kruskal-Wallis test. The Mann-Whitney U test was used for pairwise comparisons. The McNemar test was used to compare preoperative and postoperative liver histopathological findings. Statistical significance was set at P < 0.05, and results were evaluated with 95% confidence intervals.
Results
Comparison of Preoperative and Postoperative Laboratory Values Among Groups
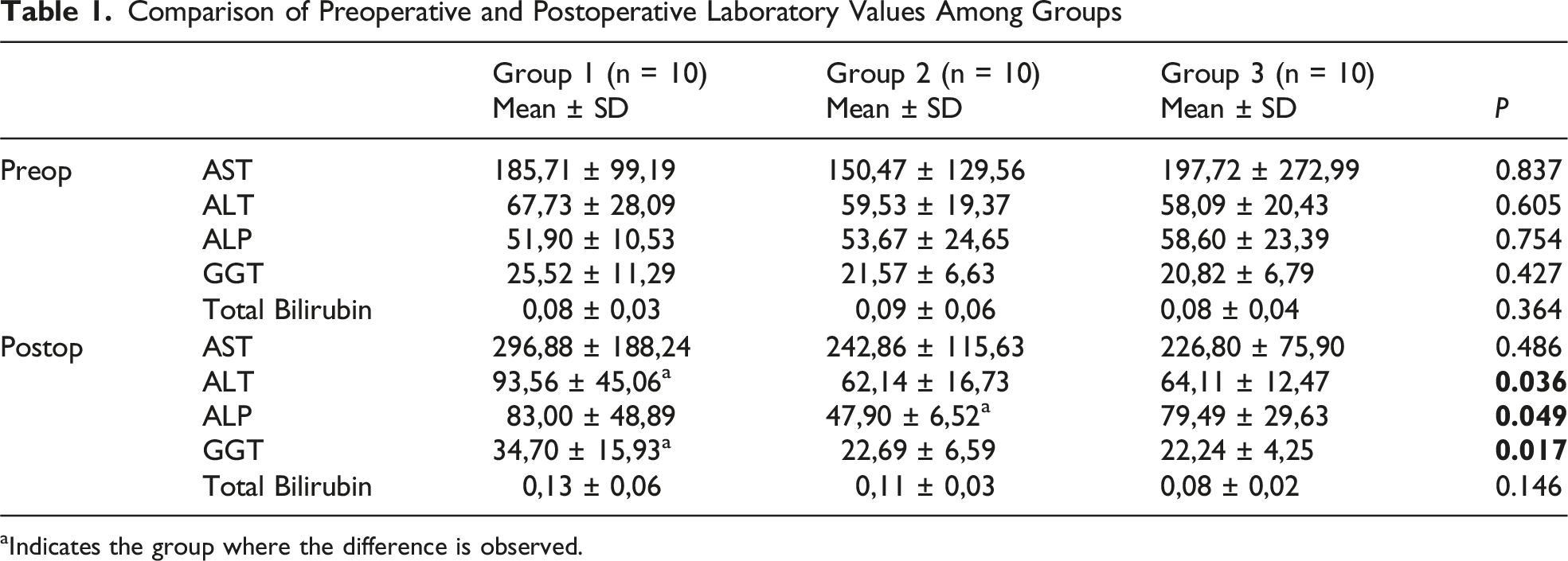
aIndicates the group where the difference is observed.
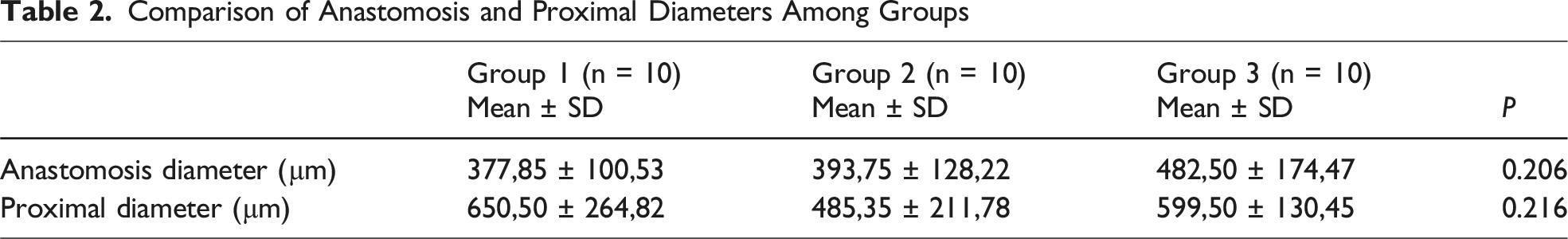
When comparing the diameters of the bile duct anastomosis and proximal segments among groups, no statistically significant differences were found (P = 0.206 and P = 0.216, respectively).
Comparison of Anastomosis and Proximal Diameters Among Groups
Preoperative histopathological examination of liver tissues showed no fibrosis or bile duct proliferation in any of the rats in Group 3. There were no statistically significant differences in the presence of portal edema and inflammation among the three groups. In Group 2, Fibrosis was present in 20% (n = 2) of rats, and bile duct proliferation was observed in 40% (n = 4) of rats. The prevalence of bile duct proliferation in Group 2 rats was significantly higher than in the other groups (P = 0.031).
Distribution of Postoperative Liver Histopathological Findings Among Groups
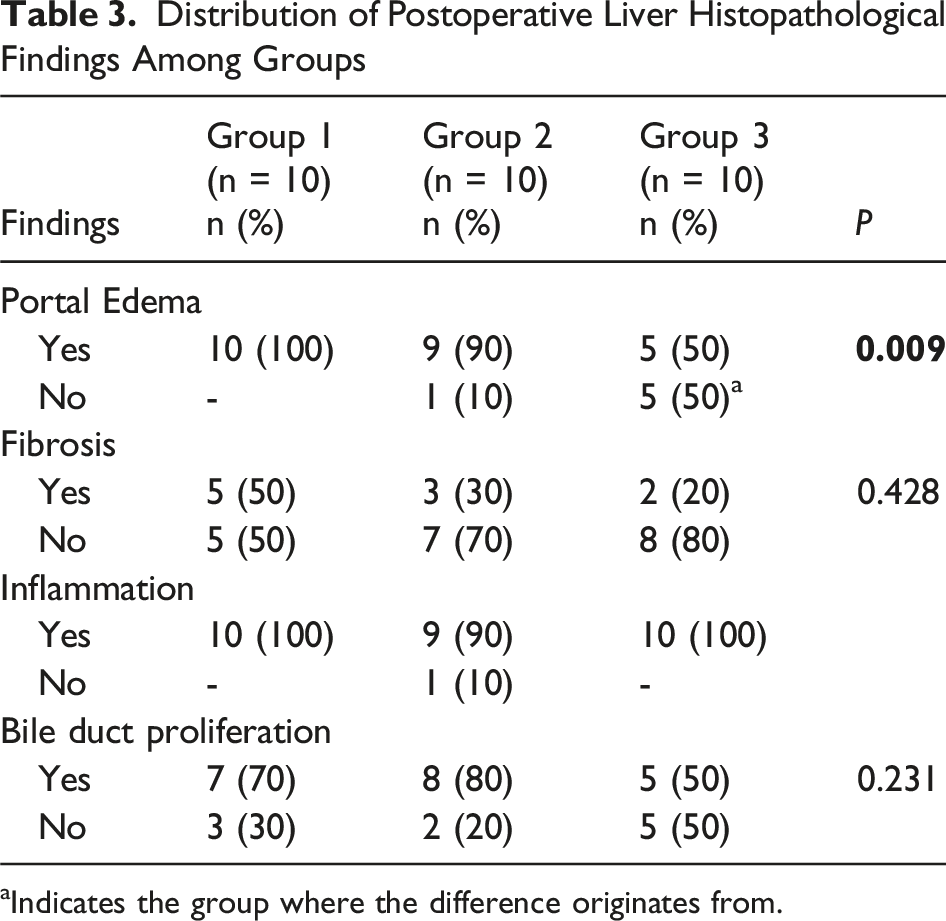
aIndicates the group where the difference originates from.
Comparison of Liver Histopathological Findings before and after Surgery in the Group of Rats
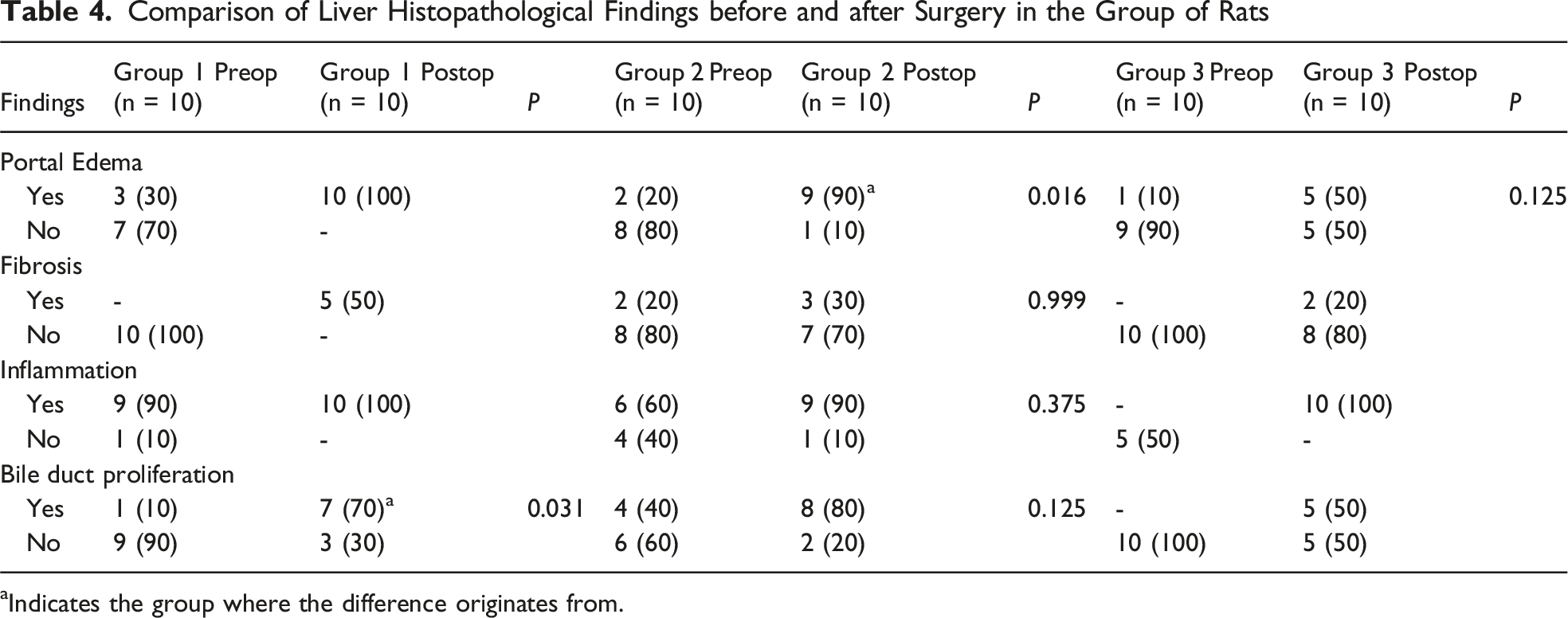
aIndicates the group where the difference originates from.
Among Group 2 rats, the rates of fibrosis, inflammation, and bile duct proliferation were similar in the preoperative and postoperative periods. The presence of portal edema on postoperative examination was significantly higher than the preoperative examination (P = 0.016) (Table 4).
The presence rates of portal edema in Group 3 rats during the preoperative and postoperative periods were similar (P > 0.05). While no fibrosis was detected in any of the rats (n = 10) in Group 3 during the preoperative period, 20% (n = 2) had fibrosis in the postoperative period. All rats in Group 3 (n = 10) exhibited inflammation in the postoperative period; 50% (n = 5) exhibited bile duct proliferation (Table 4).
Discussion
In recent years, with the widespread adoption of laparoscopic cholecystectomy and live donor liver transplantation, complications involving the bile ducts, especially strictures, have increased.11,12 Advanced inflammatory responses at biliary anastomoses increase the risk of strictures. Therefore, the technique of anastomosis and the materials used are crucial.13,14
Kenneth W. Sharp and colleagues conducted a study comparing PGLA, chromic catgut, and poliglecaprone suture materials for biliary tract anastomosis in 76 dogs. They found that postoperatively, serum alkaline phosphatase (ALP) and bilirubin levels initially increased (>80 U/L) and then decreased over time. 15 Young Sik Woo and colleagues investigated changes in liver enzymes and the development of complications in 203 cases of liver transplantation. They observed that cases developing bile duct strictures tended to show higher serum ALP levels and slower decreases in serum gamma-glutamyl transferase (GGT) levels. 16 Sances-Morales and colleagues concluded, based on a study of 329 patients, that elevated ALP levels (>323 mg/dL) after the fourth postoperative week could indicate long-term anastomotic dysfunction. 17 In our study, we found significantly higher ALT and GGT levels in Group 1 during the postoperative examination, and significantly lower ALP levels in Group 2 compared to other groups. laboratory examinations indicated that rats repaired using polypropylene (Prolene) sutures may exhibit less alteration in liver function tests and markers of cholestasis compared with rats repaired using other suture materials. This suggests that in the group where Prolene is used for repair, there may be less stenosis at the anastomosis.
Lykins and colleagues compared 6/0 Prolene and 6/0 poliglecaprone sutures in vasovasostomy in an experiment with 3-month measurements of vasoconstriction, resulting in 58% luminal clarity with Prolene and 85% with poliglecaprone. Poliglecaprone sutures were associated with reduced vascular and perivascular fibrosis on both macroscopic and microscopic examination. 18 Chiu and colleagues compared Prolene with poliglecaprone (Maxon) sutures for aortic anastomosis in 20 pigs. In the Prolene group, sutures protruded into the lumen and were associated with thrombus formation. Stenosis was significantly greater in the Prolene suture group than the poliglecaprone suture group. 19 In our study, microscopic measurements of the bile ducts at 3 months showed a 42% narrowing in Group 1, while Groups 2 and 3 showed a 20% narrowing. Although there was no statistically significant difference in anastomotic diameters between the Prolene and conduit repair groups, we found that the anastomotic diameter was relatively larger in the conduit repair group. Since we could not perform preoperative cholangiographic measurements, we believe that histological measurements do not optimally reflect luminal clarity because the lumen was empty and folded. Consequently, we could not detect significant differences in anastomotic diameters.
Jeans and colleagues compared polypropylene, PGLA, and poliglecaprone sutures for bile duct anastomosis in 30 pigs; liver biopsies from all animals did not show any features suggestive of extrahepatic biliary obstruction, particularly portal tract edema, fibrosis, inflammation, or bile duct proliferation. 20 In our study, when liver biopsies were compared, no statistically significant differences in fibrosis and inflammation parameters were observed within each group. While portal edema was statistically significantly higher in the prolen repair group (P = 0.016), bile duct proliferation was significantly more common in the polypropylene suture repair group (P = 0.03). Although we could not detect statistically significant differences in postoperative fibrosis, inflammation, and bile duct proliferation parameters among the groups, we found that the rate of portal edema was significantly lower in Group 3 compared with the other groups. We believe that this finding supports the hypothesis that PGA conduit repair reduces the rate of strictures.
Galletti and colleagues found that the inflammatory tissue response was lower in the poliglecaprone group than in the non-absorbable nylon suture group in pig bile duct anastomoses. 21 In our study, although there were no statistically significant differences in parameters including polymorph numbers, mononuclear cells, proliferative fibroblasts, and collagen scar tissue among the PGLA, Prolen, and conduit repair groups, the conduit repair group showed proportionally fewer proliferative fibroblasts and less collagen scar tissue compared with the other groups. Although we did not find statistically significant differences in inflammatory responses at the anastomosis site between the PGLA and conduit repair groups, conduit repair may have resulted in a reduced inflammatory response by creating a barrier around the anastomosis.
Kanemeru and colleagues compared poliglecaprone conduits with autologous nerve grafts for recurrent laryngeal nerve repair in dogs and found functional nerve regeneration in the poliglecaprone conduit group, whereas no regeneration was observed in the autologous graft group. They concluded that the PGA conduit served as a scaffold for axonal growth. 22 In our study, we did not find significant histological differences between the conduit group and the other groups. However, on histological examination epithelial hyperplasia was not detected in the other groups, whereas it was detected in 20% of the conduit group. We believe this finding supports the notion from the literature that the conduit serves as a scaffold for epithelialization.
Conclusion
We found that a PGA-coated conduit reduces the inflammatory response and may lead to epithelial hyperplasia. The larger anastomotic diameter observed in rats implanted with polylactic acid-coated tubes suggests that these tubes may reduce strictures in bile duct repair. In contrast to previous studies, the non-absorbable monofilament suture material Prolene produced significantly smaller elevations in transaminases and cholestatic enzymes than those observed in other groups, suggesting potential superiority in preventing strictures. However, larger-scale studies are needed to establish more reliable findings.
Footnotes
Ethical Considerations
Our study obtained ethical approval from the Necmettin Erbakan University Animal Experiments Local Ethics Committee (HAYDEK) with approval number 2023-005, dated April 6, 2023. We used 30 Wistar-Albino rats and adhered to the principles outlined in the Guide for the Care and Use of Laboratory Animals, ensuring the protection of animal rights.
Author Contributions
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study is supported by Necmettin Erbakan University.
Declaration of Conflicting Interests
The authors have no conflicts of interest regarding the research, authorship, and/or publication of this article.
