Abstract
Background
Robotic procedures are still increasing in abdominal surgery. Yet, little is known about the postoperative Quality of Life (pQoL) after these procedures. The aim of this study was to determine the pQoL of patients who underwent robotic-assisted abdominal surgery.
Methods
As a cross-sectional, retrospective study, several validated questionnaires were used to evaluate the pQoL. After confirmed consent patients who underwent robotic upper gastrointestinal tract (UGI), hepatopancreatobiliary (HPB), and colorectal (CR) procedures between 03/2020 and 03/2023 were enrolled. Subgroup analysis referred to oncologic and non-oncologic indications, postoperative time periods and age >70 years. Scoring was adjusted to a scale of 0 to 100 (as the best QoL) for comparability.
Results
A total of 197 patients were included (n = 111 for oncological indications, n = 86 for functional, non-oncological indications). Organ-related subgroup analyses showed an overall score of >70 for each group (oncologic: UGI: 75.6 ± 16.6; HPB: 85.6 ± 15.7; CR: 81.9 ± 18.5 and non-oncologic: UGI: 76.0 ± 14.8; HPB: 78.9 ± 13.2; CR: 82.4 ± 6.6). A decline in pQoL was observed during the second year after surgery, evident in both oncologic (<1 year: 80.7 ± 16.2 vs 1-2 years: 73.1 ± 19.7 vs 2-3 years: 88.4 ± 11.2, p = .005) and non-oncologic patients (<1 year: 80.7 ± 10.1 vs 1-2 years: 69.7 ± 18.9 vs 2-3 years: 75.6 ± 12.5, p = .033). PQoL was similar for patients under and above 70 years.
Conclusion
The overall pQoL for abdominal surgery was good regardless of the indication or the organ system. A decline in the pQoL was noted during the second year after surgery. Due to the retrospective design and small subgroups, further longitudinal studies are required to determine the long-term QoL and influencing factors.
Introduction
Robotic-assisted surgery has revolutionized the landscape of modern surgical practice, offering enhanced precision, flexibility, and visualization compared with other surgical modalities.1-3 With its increasing adoption across various surgical specialties, including abdominal surgery, 4 there has been growing interest in understanding its impact on patient outcomes and postoperative Quality of life (pQoL) beyond clinical efficacy alone.
Multiple questionnaires assess pQoL from several perspectives and based on specific operations. In oncological patients, questionnaires have been developed and validated by the European Organization for Research and Treatment of Cancer (EORTC).5-13 Criteria modifying EORTC questionnaires, which were defined by Osoba et al. were applied to classify differences in QoL more specifically and to enhance interpretability. 14 Several other questionnaires detect pQoL for non-oncologic surgical indications, including the Short Form 36 (SF36), Gastrointestinal Quality of Life index (GIQLI), Reflux Symptom Questionnaire (RESQ7), and Bariatric Quality of Life index (BQL).15-18 The EORTC QLQ-ELD14 is designed for patients aged 70 years and older due to their specific age-related QoL. 19 All the specific procedural questionnaires contained between 14 and 36 questions. Data on pQoL are available in terms of open and laparoscopic abdominal procedures, which provides a well-established basis of knowledge.20-22 Patients benefit from laparoscopic approach immensely: eg, in colorectal resections with lower blood loss and fewer complications and in hiatal hernia repair with shorter hospital stay and fewer complications.23,24 However, evidence of robotic pQoL outcomes remains limited, especially regarding longitudinal subjective postoperative well-being. Thus, this study aimed to comprehensively assess pQoL following robotic-assisted abdominal surgery to identify critical aspects.
Materials and methods
This is a retrospective, single-center cohort analysis with positive ethical approval (152/20) and patient consent of patients who underwent robotic abdominal surgery.
Inclusion and Exclusion Criteria
All Patients were contacted who underwent abdominal robotic assisted procedures between 03/2020 and 03/2023 at the Department of General-, Visceral-, Vascular- and Transplant Surgery at Magdeburg University Hospital, Magdeburg, Germany. The inclusion criteria were voluntary participation in personal interviews by telephone or in writing and successful completion of the interview. Patients who did not give consent, could not be reached several times, or were deceased were excluded.
Robotic Surgery
Subgroups were distinguished based on oncological and non-oncological indications and related organ systems. Three categories were differentiated: the upper gastrointestinal tract (UGI), hepatopancreatobiliary tract (HPB), and colorectal tract (CR). UGI surgeries included procedures for esophageal and gastric carcinomas, hiatal hernias, and obesity. Within the hepatopancreatobiliary system, operations have been performed for hepatocellular carcinoma, cholangiocellular carcinoma, pancreatic carcinoma, colorectal metastases, cysts, adenomas, and chronic pancreatitis. Records pertaining to the colorectal system include colon and rectal carcinomas, diverticulitis, and chronic inflammatory bowel diseases. All operations that could not be assigned to 1 of these categories were classified as “others”.
Questionnaires and Workflow
Data collection was conducted through structured interviews using Vanderbilt University Redcap® 14.0.1. The interviews were conducted between October 2022 and August 2023. The order and selection of questionnaires based on patient characteristics and surgical indications for the procedure. A maximum of 3 attempts was made to reach a patient by phone before a letter was sent, which led to exclusion if unanswered. Figure 1 gives an overview of the included questionnaires and demonstrates the workflow referring to the related organ systems. Patients with oncological surgical indications were assessed with the EORTC QLQ-C30 questionnaire. The EORTC QLQ-C30 consists of 30 questions, including functional and symptom scales. Each subscale ranged from 0-100. Higher scores indicate better preserved function or more severe symptoms. To address specific surgical indications, the following questionnaires were used for UGI: EORTC QLQ-OG25 (25 questions) for all UGI indications, EORTC QLQ-OES18 (18 questions) for esophageal cancer, and EORTC QLQ-STO22 (22 questions) for gastric cancer. For liver procedures, the EORTC QLQ-HCC18 (18 questions) was applied for hepatocellular carcinoma, EORTC QLQ-BIL21 (21 questions) for cholangiocellular carcinoma, and EORTC QLQ-LMC21 (21 questions) for liver metastases due to colorectal carcinoma. Patients with pancreatic cancer were interviewed using the EORTC QLQ-PAN26 (26 questions), and those who underwent colon and rectal surgery completed the EORTC QLQ-CR29 (29 questions). Elderly patients aged 70 years and older received the EORTC QLQ-ELD14 questionnaire (14 questions). The SF36 uses more general elements, eg, physical fitness and mental stress. The GIQLI is based on the structure of the EORTC questionnaires, contains organ- and disease-related elements and is used as a basic questionnaire for each non-oncologic patient (36 questions each). Patients with a hiatal hernia completed the RESQ7 (13 questions). Additionally, patients who underwent bariatric surgery also completed the BQL (14 questions). Applied Questionnaires according to Organ System and Type of Surgery. UGI, Upper Gastrointestinal Tract; HPB, Hepatopancreatobiliary Tract; CR, Colorectal Tract; EORTC, European Organization for Research and Treatment of Cancer; SF36, Short Form 36; GIQLI, Gastrointestinal Quality of Life Index; RESQ7, Reflux Symptom Questionnaire. BQL, Bariatric Quality of Life Index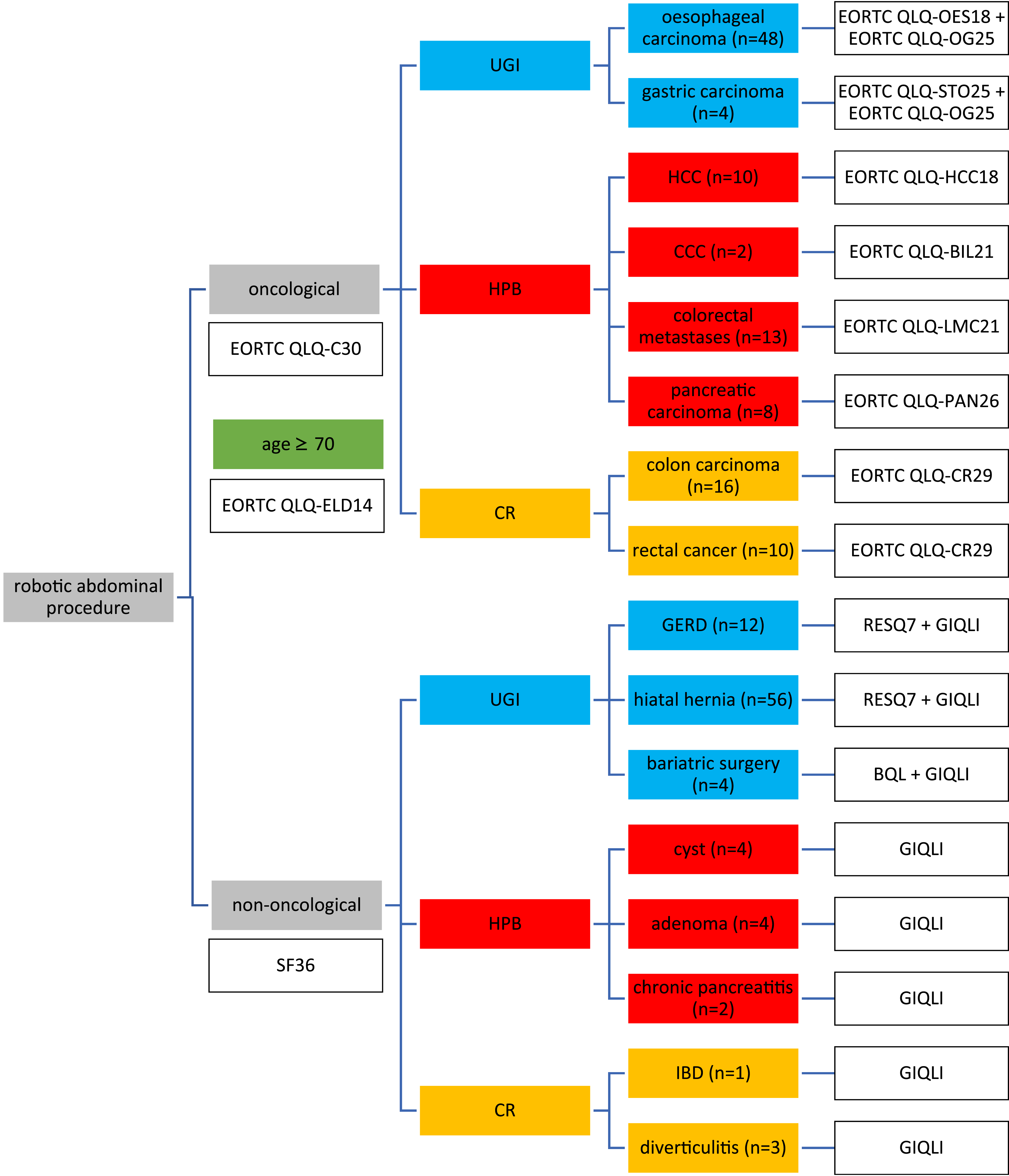
All questionnaires were statistically equalized for the purpose of comparability. As a result, all questionnaires results range between 0 and 100, where higher scores were associated with better pQoL. Therefore, the GIQLI (originally 0-144), the RESQ7 (originally 1-7) and the BQL (originally 14-70) had to be adapted by multiplication with the factor 0.694 (GIQLI) or using the formula (
To evaluate the follow-up period and identify trends, postoperative timing of pQoL assessment was stratified into several time intervals. The more detailed timeline stratification referred to 6 month periods, starting 3 months postoperatively, and resulting in 5 time intervals (3-9 months, 9-15 months, 15-21 months, 21-27 months, 27-33 months postoperatively). Yearly stratification of pQoL referred to the time interval under 1 year (interval 1), between 1 and 2 years postoperatively (interval 2), and between 2 and 3 years after robotic surgery (interval 3).
Statistical Analysis
The demographic and clinical characteristics were summarized using descriptive statistics. Means and SDs were used for continuous variables. The Shapiro-Wilk test was conducted to assess the presence of a parametric distribution. To ensure equal distribution within the variables, a chi-square test for categorical variables, an ANOVA, or the Kruskal-Wallis test was used. Depending on the type of variable, the Kruskal-Wallis test or Mann-Whitney-U test was used for statistical evaluation. IBM® SPSS Statistics 28.0 was used for statistical calculations. P-values of <0.05 were considered statistically significant.
Results
Out of 292 contacted patients, 197 (67.5%) patients were included in the study. In total, 95 (32.5%) patients were excluded due to death (11.0%, 32/292), denial of participation (6.2%, 18/292) and unreachability (15.4%, 45/292).
A total of 111 oncological patients were included with 46.8% (52/111) UGI cases, 29.7% (33/111) HPB cases and 23.4% (26/111) CR cases. In contrast, 86 patients were included with benign indication for surgery with 79.1% (68/86) referring to UGI, 15.1% (13/86) to HPB and 4.7% (4/86) to CR and 1.2% (1/86) was classified as other (incisional hernia). Further subgroup differentiation into UGI, liver, pancreas, colon, and rectum resulted in very small patient groups and therefore, was rejected.
Demographics
Patient Demographics and Clinical Characteristics, Stratified by Oncological and Non-oncological Indications and Compared Across Organ-Related Subgroups (Upper Gastrointestinal [UGI], Hepato-Pancreato-Biliary [HPB], and Colorectal [CR])
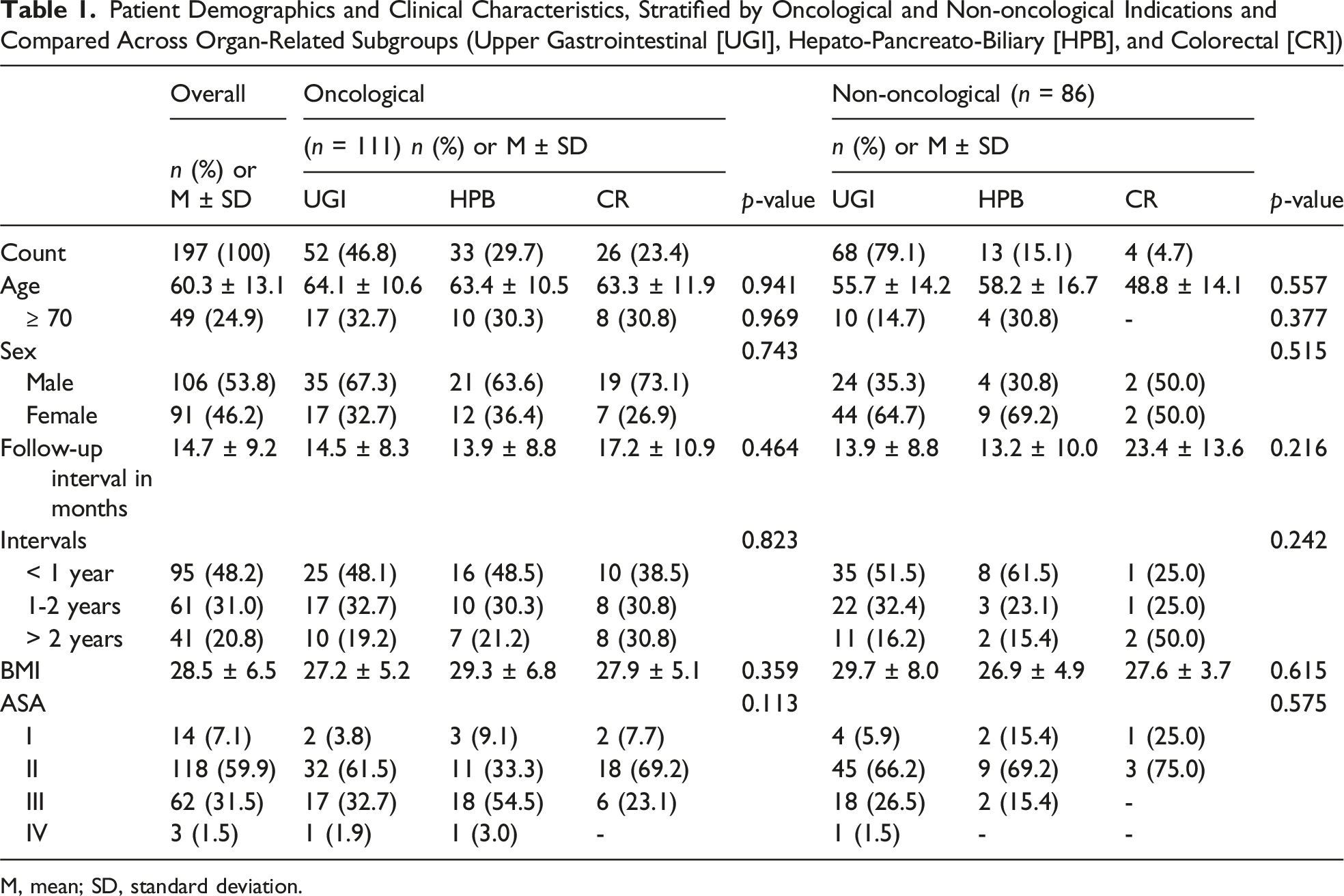
M, mean; SD, standard deviation.
Postoperative Quality of Life
The overall pQoL was 80.0 ± 17.2 in average when considering the EORTC QLQ-C30 for oncological patients and 76.4 ± 14.4 considering the SF36 for non-oncological patients.
EORTC Scores by Organ System in Oncologic Patients: Comparison Across Organ-Related Subgroups (Upper Gastrointestinal [UGI], Hepato-Pancreato-Biliary [HPB], and Colorectal [CR])
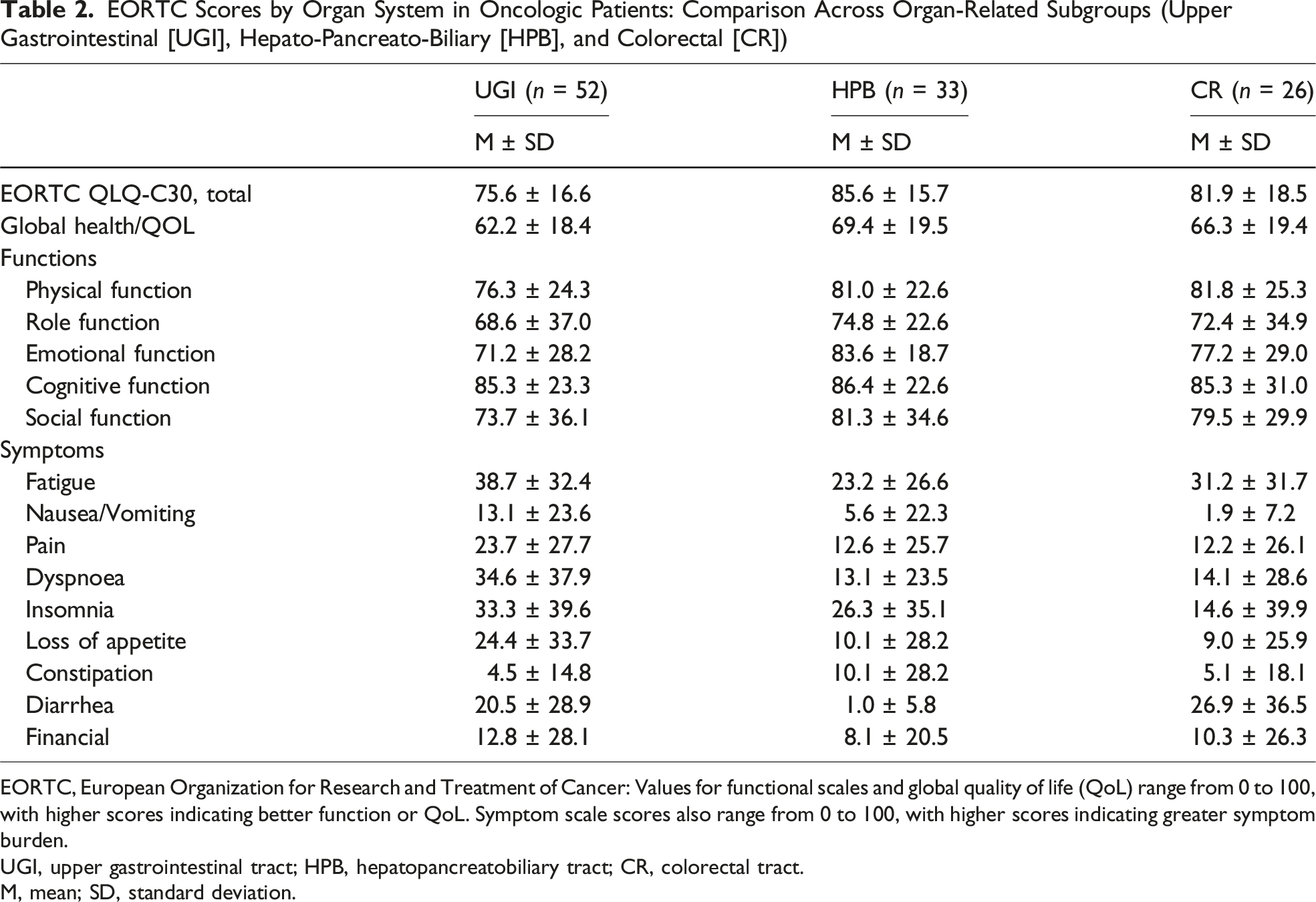
EORTC, European Organization for Research and Treatment of Cancer: Values for functional scales and global quality of life (QoL) range from 0 to 100, with higher scores indicating better function or QoL. Symptom scale scores also range from 0 to 100, with higher scores indicating greater symptom burden.
UGI, upper gastrointestinal tract; HPB, hepatopancreatobiliary tract; CR, colorectal tract.
M, mean; SD, standard deviation.
SF36 Scores by Organ System in Non-oncologic Patients: Comparison Across Organ-Related Subgroups (Upper Gastrointestinal [UGI], Hepato-Pancreato-Biliary [HPB], and Colorectal [CR])
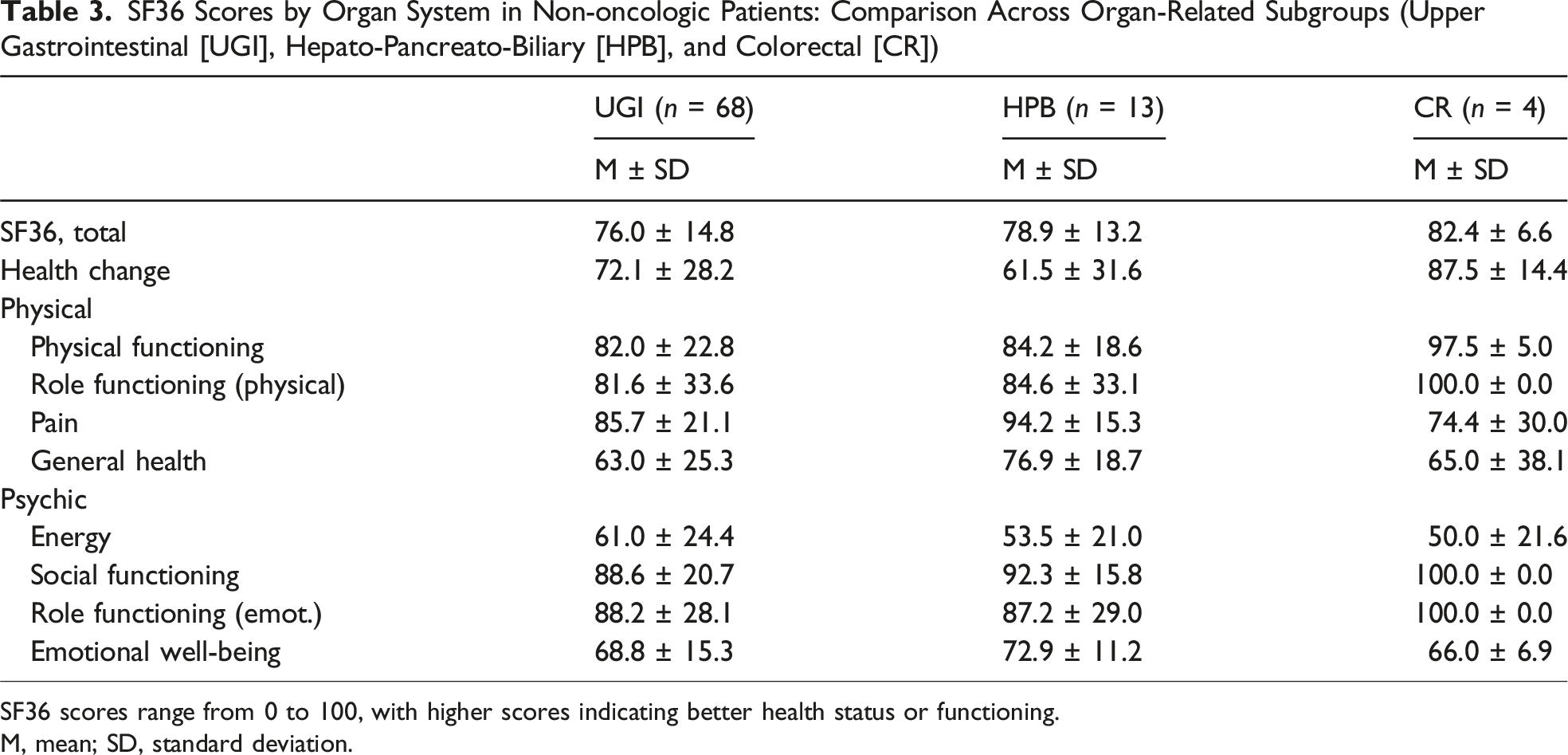
SF36 scores range from 0 to 100, with higher scores indicating better health status or functioning.
M, mean; SD, standard deviation.
Specific organ-related questionnaires, as shown in Figure 1 were completed by all participants. The EORTC QLQ-OG25 was applied to 26.4% (52/197) of the patients and showed an overall pOoL of 77.9 ± 13.6 for patients with carcinoma of UGI, the EORTC QLQ-OES18 used for 24.4% of the patients (48/197) an pQoL of 70.7 ± 13.4 for esophageal cancer and the EORTC QLQ-STO22 was applied to 2.0% (4/197) with results of 80.3 ± 20.1 for gastric cancer. For liver diseases 5.1% (10/197) received the EORTC QLQ-HCC18 showing an overall pQoL of 91.3 ± 6.9 for hepatocellular carcinoma and the EORTC QLQ-BIL21 was applied to 1.0% (2/197) of the patients showing 67.0 ± 37.3 for cholangiocellular carcinoma. Considering colorectal liver metastases the EORTC QLQ-LMC21 used for 6.6% (13/197) showed an average of 81.6 ± 14.4. The pancreatic cancer patients had an overall pQoL of 78.7 ± 11.2 with the EORTC QLQ-PAN26 applying to 4.1% (8/197) and the EORTC QLQ-CR29 showed an overall pQoL of 84.4 ± 10.4 for colon cancer with 8.1% (16/197) of the patients and 77.9 ± 15.2 for those with rectal cancer (5.1%, 10/197). In non-oncologic patients the RESQ7 showed an overall pQoL of 90.8 ± 11.1 applying to 28.4% (56/197) of the patients (original score: 1.46 ± 0.55). The BQL used for 2.0% (4/197) of the patients showed a total score of 73.9 ± 10.7 (original score: 39.3 ± 4.0).
Quality of Life During Follow-Up
No significant differences between the 6-months intervals were discernible for oncological (EORTC QLQ-C30: 3-9 m: 80.5 ± 16.7 vs 9-15 m: 75.2 ± 19.2 vs 15-21 m: 72.2 ± 18.9 vs 21-27 m: 85.5 ± 15.4 vs 27-33 m: 86.0 ± 11.8, p = .085) and non-oncological (SF36: 3-9 m: 80.4 ± 10.1 vs 9-15 m: 79.4 ± 10.2 vs 15-21 m: 73.0 ± 18.1 vs 21-27 m: 68.1 ± 23.0 vs 27-33 m: 71.1 ± 13.1, p = .279) patients.
EORTC Scores by Postoperative Intervals (1 year Each) in Oncologic Patients: Comparison Across Organ-Related Subgroups (Upper Gastrointestinal [UGI], Hepato-Pancreato-Biliary [HPB], and Colorectal [CR])
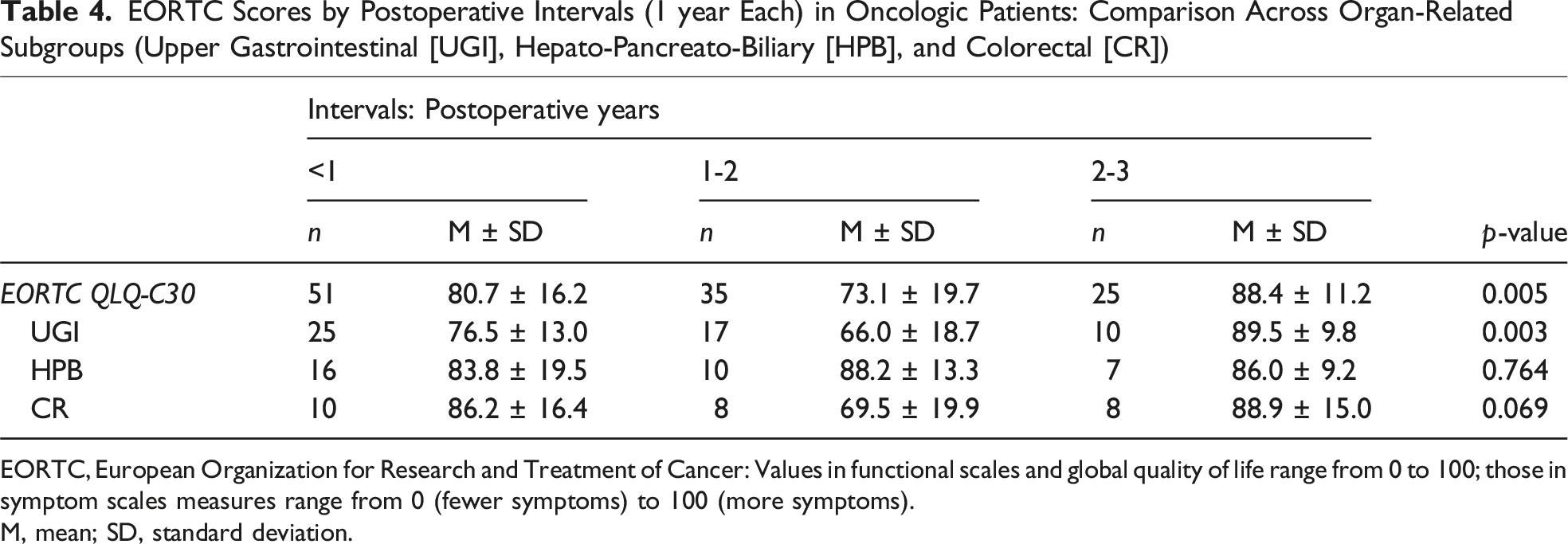
EORTC, European Organization for Research and Treatment of Cancer: Values in functional scales and global quality of life range from 0 to 100; those in symptom scales measures range from 0 (fewer symptoms) to 100 (more symptoms).
M, mean; SD, standard deviation.
SF36 Scores by Postoperative Intervals (1 year Each) in Oncologic Patients: Comparison Across Organ-Related Subgroups (Upper Gastrointestinal [UGI], Hepato-Pancreato-Biliary [HPB], and Colorectal [CR])
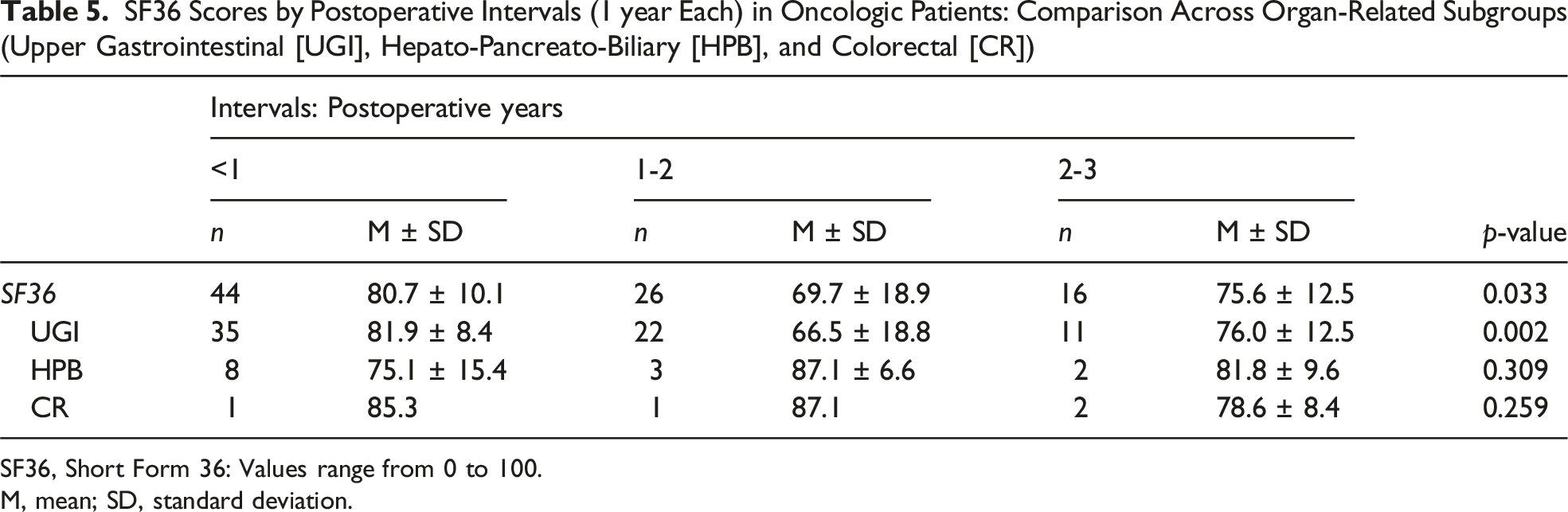
SF36, Short Form 36: Values range from 0 to 100.
M, mean; SD, standard deviation.
After further subgroup analysis (Figure 2A), this difference in pQoL was observed in patients of the UGI (<1 y: 76.5 ± 13.0 vs 1-2 y: 66.0 ± 18.7 vs 2-3 y: 89.5 ± 9.8, p = .003). A significant higher pQoL between the second and third year postoperatively using EORTC QLQ-C30 was discernible for UGI in the “role function” (<1 y: 73.3 ± 37.0 vs 1-2 y: 47.1 ± 36.0 vs 2-3 y: 93.3 ± 14.1, p = .005), “emotional function” (<1 y: 76.3 ± 25.8 vs 1-2 y: 56.9 ± 29.8 vs 2-3 y: 82.5 ± 23.7, p = .041) and “social function” (<1 y: 79.3 ± 32.0 vs 1-2 y: 52.9 ± 40.9 vs 2-3 y: 95.0 ± 15.8, p = .005), as well as “fatigue” (<1 y: 37.8 ± 30.3 vs 1-2 y: 54.2 ± 33.1 vs 2-3 y: 14.4 ± 21.7, p = .008) and “insomnia” (<1 y: 44.0 ± 42.7 vs 1-2 y: 33.3 ± 39.1 vs 2-3 y: 6.7 ± 14.1, p = .048). The values on the functional scales increased significantly from the second to the third time interval, and the values on the symptom scales decreased significantly. Detailed analysis of the UGI cases in the second period showed postoperative complications, including anastomotic insufficiency with subsequent discontinuous resection and 2 reintubations after postoperative pulmonary instability. (A) EORTC Scores by Postoperative Intervals (1 year Each) in Oncologic Patients. (B) SF36 Scores by Postoperative Intervals (1 year Each) in Oncologic Patients. Comparison Across Organ Related Subgroups (Upper Gastrointestinal [UGI], Hepato Pancreato Biliary [HPB], and Colorectal [CR]. EORTC, European Organization for Research and Treatment of Cancer. Values in Global Quality of Life range from 0 to 100. SF36, Short Form 36. Values range from 0 to 100.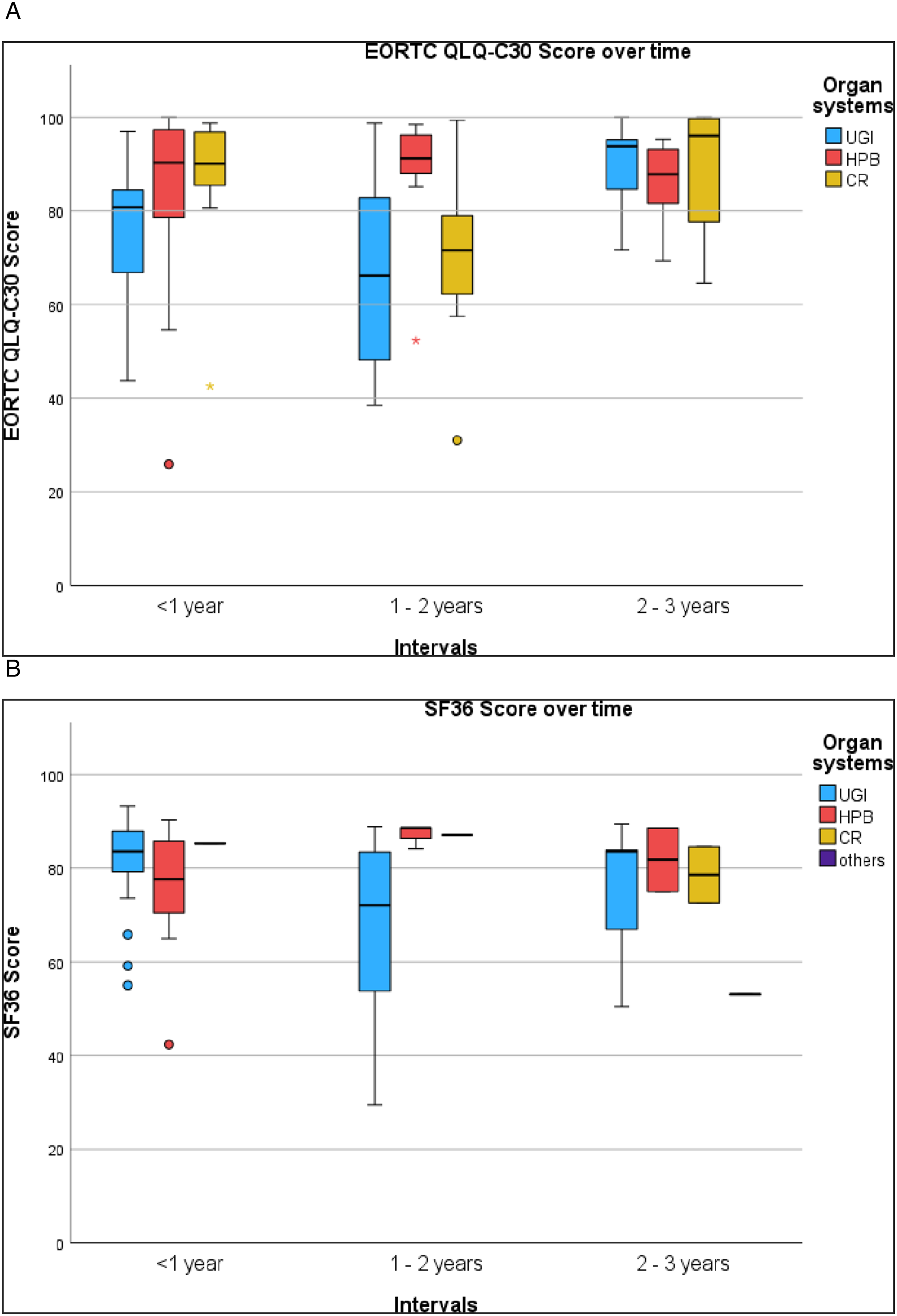
For the organ-related subgroups of HPB (<1 y: 83.8 ± 19.5 vs 1-2 y: 88.2 ± 13.3 vs 2-3 y: 86.0 ± 9.2, p = .764) and CR (<1 y: 86.2 ± 16.4 vs 1-2 y: 69.5 ± 19.9 vs 2-3 y: 88.9 ± 15.0, p = .069) patients, the yearly postoperative time periods did not differ.
The pQoL for patients after rectal procedures was significantly lower within the second year after the operation (<1 y: 88.1 ± 9.2 vs 1-2 y: 65.2 ± 20.2 vs 2-3 y: 98.0 ± 2.9, p = .043). For these patients, a significant difference could be observed for the symptom “insomnia” (<1 y: 11.1 ± 19.2 vs 1-2 y: 53.3 ± 29.8 vs 2-3 y: 0.0 ± 0.0, p = .043). Two of the 5 patients who underwent surgery in the period of 1-2 years showed hepatic metastases.
Regarding non-oncologic patients, the pQoL was significantly higher during the first interval compared to the second interval using the SF36 (<1 y: 80.7 ± 10.1 vs 1-2 y: 69.7 ± 18.9 vs 2-3 y: 75.6 ± 12.5, p = .033). Subgroup analysis (Figure 2B) showed that UGI patients (<1 y: 81.9 ± 8.4 vs 1-2 y: 66.5 ± 18.8 vs 2-3 y: 76.0 ± 12.5, p = .002) had significant lower “physical functioning” (<1 y: 90.1 ± 12.0 vs 1-2 y: 67.3 ± 31.7 vs 2-3 y: 85.5 ± 12.1, p = .014), more “pain” (<1 y: 91.6 ± 16.6 vs 1-2 y: 78.0 ± 25.3 vs 2-3 y: 82.3 ± 20.8, p = .017), lower “general health” (<1 y: 73.7 ± 18.1 vs 1-2 y: 45.9 ± 24.5 vs 2-3 y: 63.2 ± 29.3, p < .001), lower “social functioning” (<1 y: 96.8 ± 9.3 vs 1-2 y: 74.4 ± 26.3 vs 2-3 y: 90.9 ± 21.0, p < .001), lower “emotional role functioning” (<1 y: 95.2 ± 20.0 vs 1-2 y: 77.3 ± 37.6 vs 2-3 y: 87.9 ± 22.5, p = .034) and lower “emotional well-being” (<1 y: 73.4 ± 13.7 vs 1-2 y: 62.2 ± 17.3 vs 2-3 y: 67.6 ± 11.5, p = .029). The subscale “energy” (<1 y: 52.3 ± 23.1 vs 1-2 y: 73.9 ± 21.1 vs 2-3 y: 63.2 ± 24.5, p = .006) showed the opposite, a significant higher pQoL in the second interval compared to the first interval. No significant difference was found in the subscale “physical role functioning”. A significantly higher pQoL in the first postoperative year is shown in the subjective subscale “health change” (<1 y: 82.6 ± 24.8 vs 1-2 y: 63.6 ± 28.6 vs 2-3 y: 54.5 ± 24.5, p = .001).
Age and Quality of Life
Elderly patients aged 70 and above did not show significant differences in their pQoL regarding to the EORTC QLQ-C30 (82.2 ± 15.5 vs 75.3 ± 20.0, p = .117) (Figure 3A). Those patients with an oncologic indication (n = 35) had a pOoL of 46.3 ± 15.6 regarding the EORTC QLQ-ELD14 as a specific questionnaire. Considering the individual elements of the EORTC QLQ-C30, “physical function” (<70 y: 82.1 ± 23.2 vs ≥70 y: 72.2 ± 24.5, p = .021) and “cognitive function” (<70 y: 88.6 ± 22.5 vs ≥70 y: 79.0 ± 28.7, p = .037) were significant lower, as well as “fatigue” (<70 y: 26.6 ± 29.2 vs ≥70 y: 44.8 ± 31.8, p = .003) and “dyspnea” (<70 y: 17.5 ± 28.0 vs ≥70 y: 36.2 ± 40.7, p = .022) were significant higher in the elderly group. Differentiating into organ systems, for elderly UGI patients the symptom “dyspnea” (<70 y: 26.7 ± 33.1 vs ≥70 y: 51.0 ± 42.7, p = 0.038) was significant higher. Referring to the organ-related subgroups and the EORTC QLQ-ELD14, no significant difference between organ systems was seen (UGI: 44.1 ± 15.3 vs HPB: 49.7 ± 12.0 vs CR: 46.7 ± 20.9, p = .692). (A) EORTC Scores by Age in Oncologic Patients. (B) SF36 Scores by Age in Oncologic Patients. Comparison Across Organ Related Subgroups (Upper Gastrointestinal [UGI], Hepato Pancreato Biliary [HPB], and Colorectal [CR]. EORTC, European Organization for Research and Treatment of Cancer. Values in Global Quality of Life range from 0 to 100. SF36, Short Form 36. Values range from 0 to 100.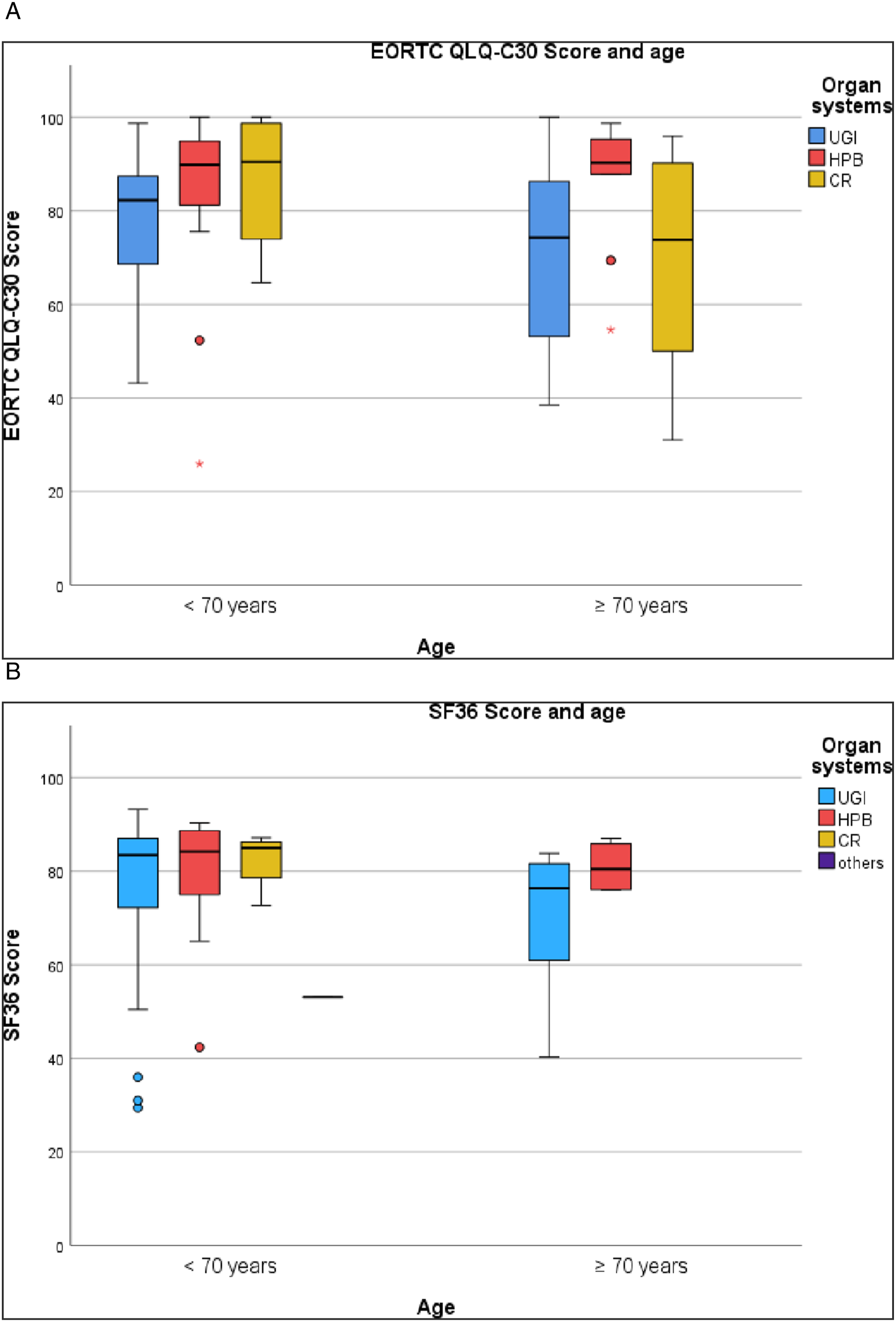
The SF36 questionnaire revealed no significant differences in elderly non-oncologic patients (77.0 ± 14.6 vs 73.4 ± 13.4, p = .111) (Figure 3B). Considering SF36, the “physical functioning” (<70 y: 84.3 ± 22.0 vs ≥70 y: 68.5 ± 23.7, p = .019) was significant lower for elderly UGI patients.
Discussion
Postoperative quality of life represents a key outcome in the surgical treatment of patients with both oncological and non-oncological conditions. In the present study, overall good pQoL following robotic abdominal procedures was favorable, with scores exceeding 70/100. Among oncological patients, “fatigue” and “insomnia” consistently constituted the most significant symptoms, whereas non-oncologic most frequently reported reduced “energy”. A significant decline in pQoL was observed during the second postoperative year in both UGI and CR cohorts. In elderly patients, pQoL did not differ significantly; however, variates were noted in specific subscales. In non-oncological patients, considerable discrepancies between questionnaires were identified: while the SF36 yielded a mean score of 76.4, the GIQLI indicated a substantially higher mean score of 86.1.
The present study provides a comprehensive assessment of pQoL across the entire spectrum of robotic-assisted abdominal surgical procedures for oncological and non-oncological cases over a period of 3 years as a cross-sectional study.
The SF36 uses more general elements 15 and the GIQLI is based on the structure of the EORTC questionnaires and contains organ- and disease-related elements. 16 The detection of comorbidities is an advantage of the SF36 in contrast to the GIQLI, which has the advantage of better clinical interpretability with its disease-specific instruments. 25 Therefore, with our SF36 data (76.4) and GIQLI results (86.1), comorbidities may have a greater influence than organ-specific problems in general.
Regarding UGI patients, Aiolfi et al published an average of 72.5 with SF36 for hiatal hernia patients after laparoscopic surgery, 26 and Amprayil et al. described an average of 70.8 for a 1-year follow-up with SF36 for laparoscopic hiatal hernia repairs. 27 Likewise, Sunde et al. investigated QoL 1 year after diagnosis in oncological cases, such as carcinomas of the upper gastrointestinal tract. 28 In their investigation, Sunde et al delineated a mean quality of life of 73 for esophageal cancer patients utilizing the EORTC QLQ-C30 instrument, with a reference value of 89 for the general population. By Neuschütz et al. reported the pQoL for esophageal cancer patients as 77.2 for open surgery cases and 77.7 for patients that underwent robotic-assisted surgery. 29 Wang et al. published pQoL for patients who underwent esophagectomy and described values for video-assisted thoracoscopy of 77.9 and values of 75.0 for open surgery. 30 The pQoL of our study showing 76 for patients after robotic hiatal hernia repair and 75.6 for patients who underwent robotic oncologic esophagectomies is comparable to the pQoL after laparoscopic or open surgery. Therefore, the robotic approach does not seem to have a negative impact. However, considerable variation was observed in pQoL among oncologic UGI patients during the second time interval.
Regarding rectal surgery, a comparison was drawn between robotic-assisted and laparoscopic rectal surgery with regard to QoL in a meta-analysis conducted by Martins et al, revealing no significant disparities between the 2 surgical approaches. 31 For robotic-assisted surgery, the pQoL ranged between 61.4 and 74.9. However, the average in our study was higher with 78.6 and contributed to the potential advantage of the robotic approach. An advantage was found in the dimensions of physical functioning and perception of body image in the robot-assisted patient group, which can be explained by the physical advantages of the surgical technique. 32 The observed low role function scores in rectal cancer patients (55.0) may suggest various factors contributing to this outcome, including potential implications on sexual function. However, similar findings have been reported in studies investigating both open and laparoscopic approaches in rectal surgery.33-35 In conclusion, the data are inconsistent regarding the effect of the robotic approach on the role and sexual function. Especially long-term investigations are needed to investigate this further.
Our study showed that relevant fluctuations in QoL appeared within a period of 1 year with the lowest quality of life within 1-2 years postoperatively due to well-known influencing factors of QoL such as disease progression, recurrence, metastases, and long-term complications.36-38 Among non-oncological patients, a large proportion of our patient group had undergone surgery for hiatal hernias (65.1%). Based on the study of Nguyen et al. there is a very high risk of recurrence within the first 2 years postoperatively. 39 This can lead to more complex reoperation procedures which was the case in our study. 40 Therefore, our study results are in alignment with these findings. As a positive outcome, the QoL increases again afterwards.
Elderly patients, aged 70 and above, exhibited differences in certain aspects of pQoL, like “fatigue”, “social functioning” and “burden of illness”. They often suffer from comorbidities, which are addressed in the EORTC QLQ-ELD14 questionnaire. 19 Currently, there are no data on elderly patients after surgical interventions. Yet, Schmidt et al. emphasize that “elderly” patients define life satisfaction as a factor that is more insignificant than maintaining routines.. 41 Therefore, we believe that lower functional outcomes and higher fatigue in our study population are not related to comorbidities that are more prevalent in elderly patients.
Limitations
The cross-sectional and retrospective nature of this single-center study introduces a potential for selection bias. Associations between perioperative variables and pQoL are therefore restricted in causality. Additionally, some patients were lost to follow-up because of death or unreachability, which resulted in a skewed cohort. These patients may have experienced systematically different outcomes compared with those included in the analysis. However, it provides a comprehensive overview of the validated questionnaires for oncologic, non-oncologic, and elderly patients.
The small subgroup sizes and heterogeneity of the study caused limitations in statistical power and reduce the generalizability of the findings. However, to optimize the interpretability of the pQoL scores, the total scores of 3 questionnaires were adjusted to a scale of 0 to 100, facilitating immediate classification. However, the original scores were included for transparency.
Beyond age, organ system, indication for surgery, and follow-up period, partially unevaluated factors such as patients pre-existing comorbidities or those emerging after surgery, postoperative complications (classified via Clavien-Dindo), everyday life restrictions (via ECOG), and tumor staging (using UICC stages) merit consideration, potentially offering a more comprehensive understanding of their influence on postoperative quality of life outcomes.
Conclusion
Patients undergoing robotic-assisted abdominal surgery generally maintain high postoperative quality of life (pQoL), with fatigue most relevant in oncological patients and low energy in non-oncological patients. Cognitive function remained high across all groups. Elderly patients showed reduced pQoL, potentially related to comorbidities, without implying a causal effect of surgery. Non-oncological liver patients showed particularly favourable outcomes. A decline in pQoL was observed in the second postoperative year, followed by improvement in the next year. Overall, robotic-assisted surgery does not appear to negatively affect pQoL, and further studies are needed to identify patients who may benefit most.
Footnotes
Author Contributions
J. Stockheim, MD, and F.-L. Fiedler contributed equally to the study. Prof. Perrakis, J. Stockheim, MD, and F.-L. Fiedler contributed to the study conception and design. Prof. R. S. Croner, MD, Prof. A. Perrakis, MD, J. Stockheim, MD, and F.-L. Fiedler provided the resources, contributed to the implementation of the research and to the analysis of the results. F.-L. Fiedler designed the figures. All authors contributed to the writing of the manuscript including review and editing. Prof. Roland Croner, MD, Prof. Aristotelis Perrakis, MD, Mihailo Andric, MD, Sara Al-Madhi, MD, Maximilian Dölling, MD, Jessica Stockheim, MD, and Felix-Lukas Fiedler have no conflicts of interest to disclose or financial ties to disclosure.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
