Abstract
Background
The ergonomic design of surgical instruments plays a pivotal role in the efficiency, safety, and comfort of surgeons. Studies confirm that poorly designed instruments can lead to physical discomfort, premature fatigue, and decreased dexterity. This study aims to assess the current usability of surgical instruments to identify problematic designs and highlight areas for ergonomic improvements.
Methods
An anonymized online questionnaire with 18 questions was distributed via email to various surgical societies, professional associations, and the mailing lists of surgical departments at the University Hospital Leipzig. Data on gender, glove size, clinical background, surgical subspecialty, and experience were collected. Participants were asked about physical discomfort, fatigue, precision, and safety issues when using surgical instruments and devices.
Results
A total of 459 surgeons participated, most of whom specialized in orthopedics and trauma surgery (81.48%). Gender differences were noted in glove sizes and frequency of complaints. Women reported significantly more difficulties, such as fatigue and imprecise handling, compared to men. Overall, 88.1% of women and 59.9% of men considered the development of ergonomic instruments important. Only 13% had experience using ergonomic instruments, with nearly half of the participants reporting significant improvements.
Conclusions
The study demonstrates that surgical instruments with inadequate ergonomics, particularly for users with smaller glove sizes, result in physical strain, fatigue, and reduced precision. The findings underscore the necessity for ergonomic modifications to meet the physical requirements of surgeons, ensuring a more efficient and safer surgical workflow.
Existing studies confirm that surgical instruments require ergonomic adaptation, as current models fail to meet modern standards. This study identified inadequately designed instruments that negatively impact surgical performance and safety. The findings could guide the development of new surgical instruments to improve surgeons’ performance during operations.Key Points
What is already known on this topic
What this study adds
How this study might affect research, practice, or policy
Introduction
The ergonomics of surgical instruments significantly affect surgeons’ efficiency, safety, and comfort. 1 Poorly designed tools contribute to early fatigue, reduced precision, and increased risk of musculoskeletal disorders.2-4 These challenges are particularly pronounced given the diverse demographics of surgeons, encompassing a wide range of hand sizes and strengths. Historically, surgical tools have been designed predominantly for the average male hand, neglecting the needs of female and smaller-handed surgeons. Research suggests that ergonomic improvements could enhance surgeons’ comfort and performance, ultimately benefiting patient outcomes. Studies have shown that non-ergonomic instruments can lead to hand fatigue, discomfort, and reduced dexterity, which negatively affect surgical precision and safety, prolonging operation times and increasing complication rates.5-7
This study aims to evaluate the current state of surgical instrument ergonomics through a comprehensive survey of surgeons to identify specific areas needing ergonomic improvements. By examining their experiences and challenges, we aim to raise awareness about the critical importance of tailoring instruments to the diverse needs of the surgical community.
Besides hand anthropometry, factors such as wrist posture, coupling forces, instrument weight, and vibration exposure are acknowledged risk factors for musculoskeletal disorders (MSDs) in surgeons. This study was designed to address self-reported handling difficulty, fatigue, precision, and safety, while acknowledging that these additional determinants should be integrated into future ergonomic research and instrument design.”
Methods
An online questionnaire was created using SurveyMonkey® (https://surveymonkey.com) and distributed between march and June 2024 via email to various professional surgical societies and associations (e.g., German Society of Surgery [DGCH], Society for Arthroscopy and Joint Surgery [AGA], D-A-CH Association for Shoulder and Elbow Surgery [DVSE], Swiss Society for Spine Surgery [SGS]), as well as through LinkedIn and internal mailing lists of surgical departments at the University Hospital Leipzig. No financial or material incentives were offered for participation. The survey was open to surgeons from all specialties; however, recruitment primarily targeted German-speaking countries, which limits external validity.”
The questionnaire in German language (Supplement 1) included 18 questions covering demographic data (gender, glove size, clinical background) and surgical specialization.
Important to note glove size in this study refers to the standard surgical glove size routinely worn by participants in the operating room and was used as a surrogate marker for hand anthropometry. No specialized or instrument-specific gloves were assessed.
Questions addressed handling issues, physical discomfort, fatigue, precision, and safety concerns with specific instruments and devices. Participants could propose solutions for improved ergonomic design.
The questionnaire was sent via email to the mailing lists of the German Society of Surgery (DGCH), the Society for Arthroscopy and Joint Surgery (AGA), the D-A-CH Association for Shoulder and Elbow Surgery (DVSE), the Swiss Society for Spine Surgery (SGS), the association “Die Chirurginnen e.V.”, the association Swiss Female Orthopedic, the German Society of General and Visceral Surgery (DGAV), and the German Society for Thoracic Surgery (DGT). Additionally, a QR code with a link to the survey was shared via the professional network LinkedIn and distributed to the internal mailing lists of the departments of Orthopedics, Trauma Surgery, Plastic Surgery, Neurosurgery, Urology, Pediatric Surgery, Visceral, Transplant, Thoracic, and Vascular Surgery at the University Hospital Leipzig, inviting participation. For the purpose of this study, the term ergonomic/adjustable instruments referred to surgical instruments with design features intended to improve user comfort and reduce physical strain, such as adjustable handle span or grip size, reduced weight, contoured or non-slip handles, or variable activation force. Participants were asked whether they had prior experience with such instruments and, if so, to rate any perceived benefit compared with standard devices.
Statistical Analysis
Data were analyzed using IBM SPSS Statistics, version 29 (IBM Corp., Armonk, NY, USA). Descriptive statistics were generated for all items. Normality of continuous variables was assessed using the Kolmogorov–Smirnov test. Group differences were evaluated with Chi-square tests for categorical data and Kruskal–Wallis tests for ordinal or non-normally distributed continuous data. To account for potential confounders, multivariable ordinal logistic regression models were applied to the main outcomes (handling difficulties, additional hand movements, fatigue, precision, and perceived safety), with glove size, gender, years of experience, and frequency of instrument use entered as predictors. Results are reported as odds ratios (OR) with 95% confidence intervals (CI). Categories with very small numbers were retained but interpreted with caution. Open-ended responses were qualitatively categorized by instrument type and ergonomic risk factor, and their frequency distribution is presented in Supplement Figure 4. A two-tailed significance level of P < 0.05 was applied.
Results
A total of 459 surgeons participated in the survey. Of these, 374 (81.5%) specialized in orthopedics and trauma surgery, 36 (7.8%) in visceral or thoracic surgery, 16 (3.5%) in cardiac or vascular surgery, 15 (3.3%) in neurosurgery, 11 (2.4%) in urology, and 7 (1.5%) in plastic surgery. Orthopedics and trauma surgery are organized as a single combined department; therefore, respondents from these areas were analyzed collectively.
Among the orthopedic and trauma surgeons, the most common subspecialty was arthroscopy (136/331, 41.1%), followed by trauma surgery (116/331, 35.0%), endoprosthetics (39/331, 11.8%), hand/foot surgery (21/331, 6.3%), spinal surgery (13/331, 3.9%), and pediatric orthopedics (6/331, 1.8%). The gender distribution among participants showed a slightly higher proportion of male surgeons, with 56.4% (259/459) male, 43.4% (199/459) female, and one non-binary individual (0.2%). The dominant hand was right for 84.5%, while 6.8% identified as ambidextrous, highlighting the right-hand bias in current instrument design.
The most frequent respondents were male surgeons with extensive experience (more than 20 years: 117/259, 45.2%; 11 to 20 years: 73/259, 28.2%) and women with 5 to 20 years of experience (5 to 10 years: 71/199, 35.7%; 11 to 20 years: 61/199, 30.7%). Surgical instruments and devices were most commonly used 6 to 10 times per week (163/416, 39.2%). A significant proportion of respondents (27.6%, 115/416) reported using instruments more than 20 times per week, while others reported use 11 to 20 times (97/416, 23.3%) or less than 5 times per week (41/416, 9.9%) (Supplement Table 2).
There was a significant difference (P < 0.001) in glove sizes between male and female respondents. Men’s glove sizes ranged from 7 to 9, with a median size of 7.5, while women’s glove sizes ranged up to 7.5, with a median of 6.5 (Figure 1). Bivariate analyses (Supplement Table 3) revealed strong gender differences. Women reported handling difficulties far more often than men (≥“sometimes”: 67.4% vs 21.6%, P < 0.001), additional hand movements (74.1% vs 32.1%, P < 0.001), and fatigue (61.2% vs 36.3%, P < 0.001). Perceived safety was also rated lower by women (11.8% vs 2.9% reported ≤“unsafe”, P = 0.002). Similar trends were seen for glove size, with significantly more problems reported in participants with glove sizes ≤7.5 (Items 8 and 9, both P < 0.001, Figures 2 and 3). Glove Size Distribution of Respondents by Gender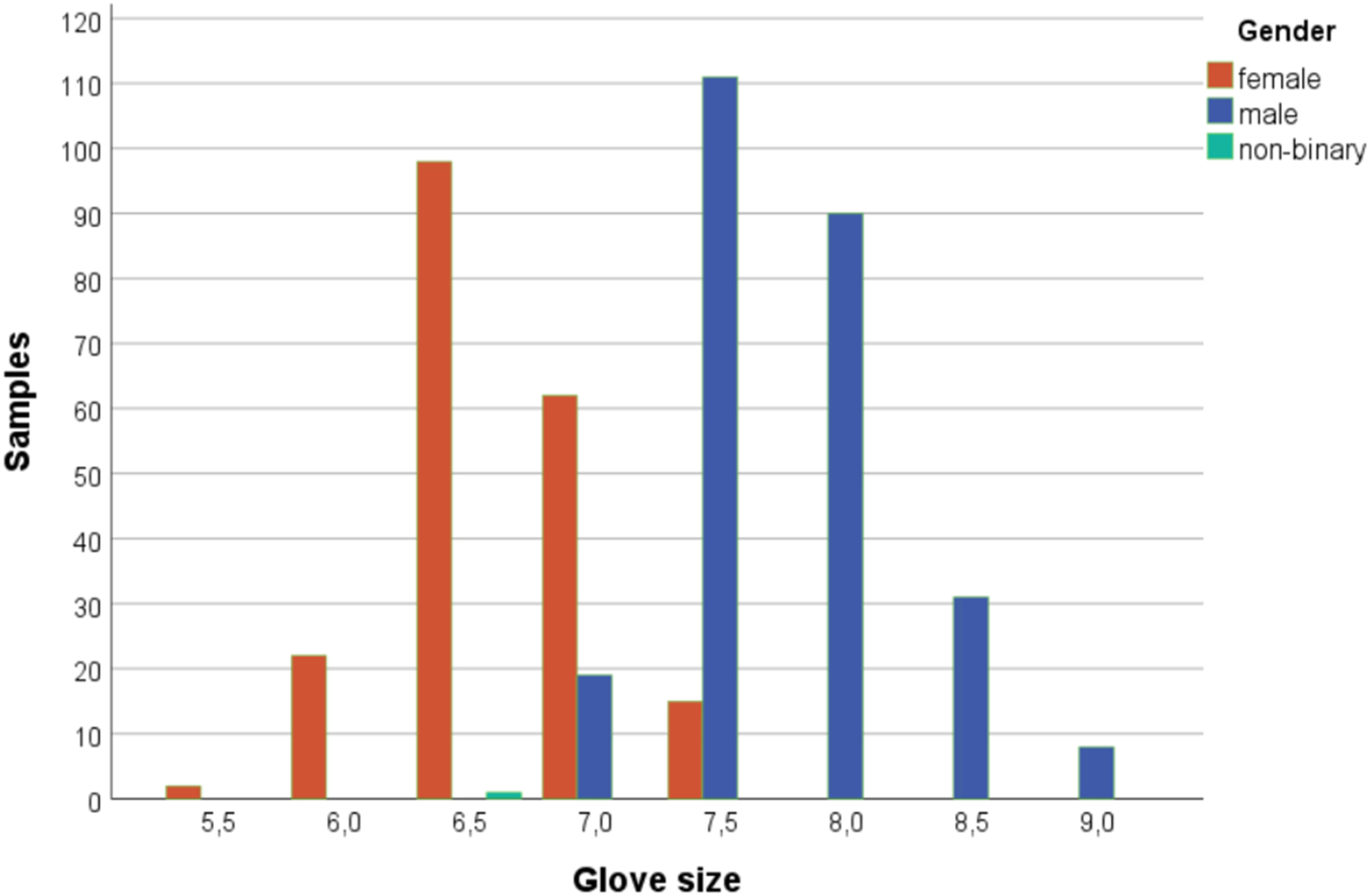
Multivariable regression analyses (Supplement Table 4) confirmed that glove size was a key determinant of ergonomic problems. After adjusting for glove size, years of experience, and weekly use, gender remained a strong independent predictor only for handling difficulties (OR 7.5, 95% CI 5.0-11.3, P < 0.001). For additional hand movements, fatigue, and perceived safety, gender was no longer significant. Instead, very small glove sizes (≤6.0) and higher weekly instrument use were associated with increased risk.
Regarding experience, surgeons with 5-10 years reported more frequent handling problems compared to those with <5 years (OR 1.99, 95% CI 1.07-3.73, P = 0.030). By contrast, those with >10 years of practice did not show higher risk, suggesting a possible adaptation effect or survivor bias.
Despite these differences, 39.7% of men (94/237) and 71.9% of women (128/178) reported specific issues with certain instruments. Furthermore, 88.1% of women (very important: 40.1%, 71/177; important: 48%, 85/177; neutral: 10.2%, 18/177; unimportant: 1.1%, 2/177; very unimportant: 0.6%, 1/177) and 59.9% of men (very important: 19%, 45/237; important: 40.5%, 96/237; neutral: 31.6%, 75/237; unimportant: 5.9%, 14/237; very unimportant: 3%, 7/237) expressed the importance of prioritizing the development of ergonomic instruments for all users. Fatigue Caused by the Use of Surgical Instruments/Devices Based on Glove Size Additional Hand Movements Required During the Use of Surgical Instruments/Devices Based on Glove Size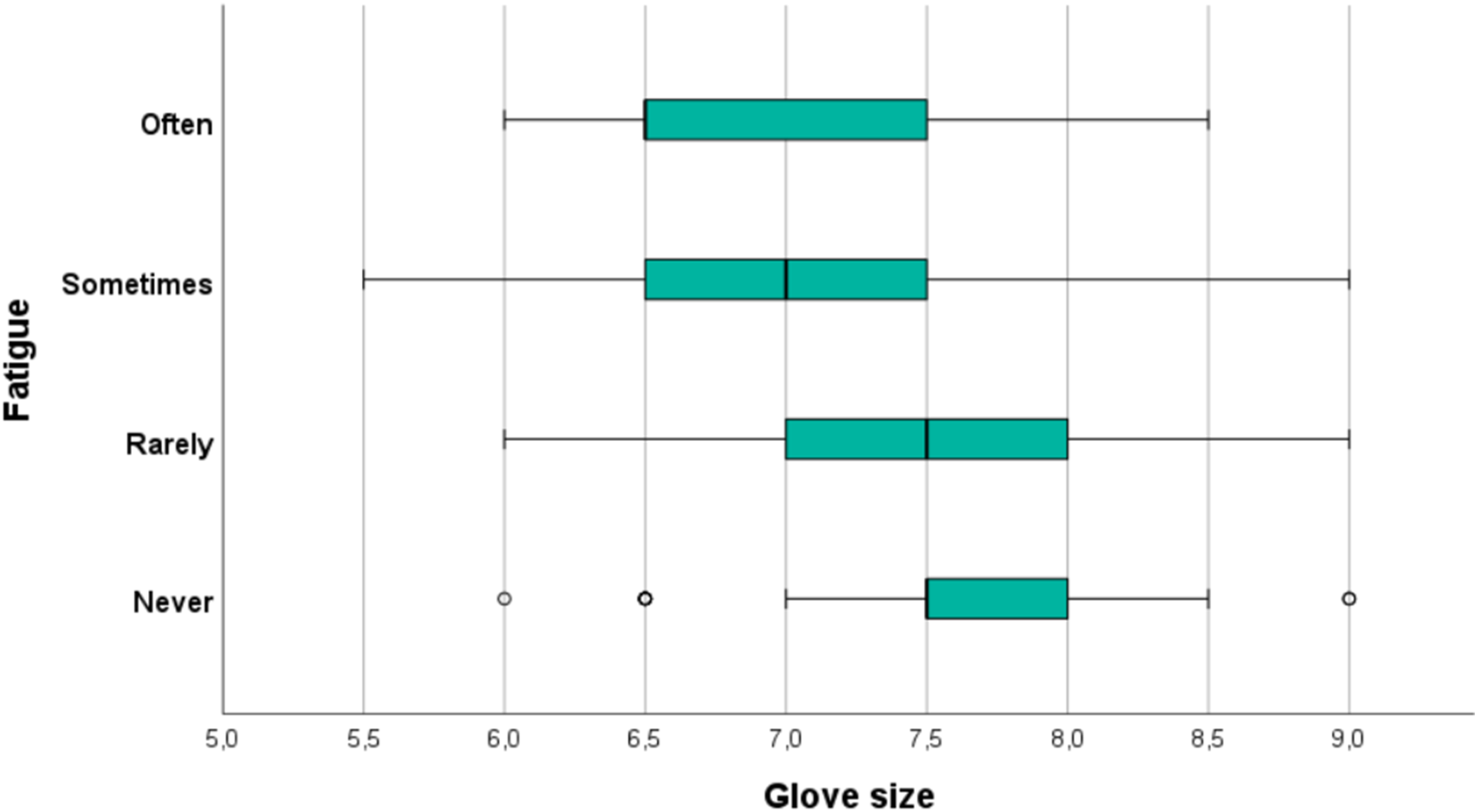
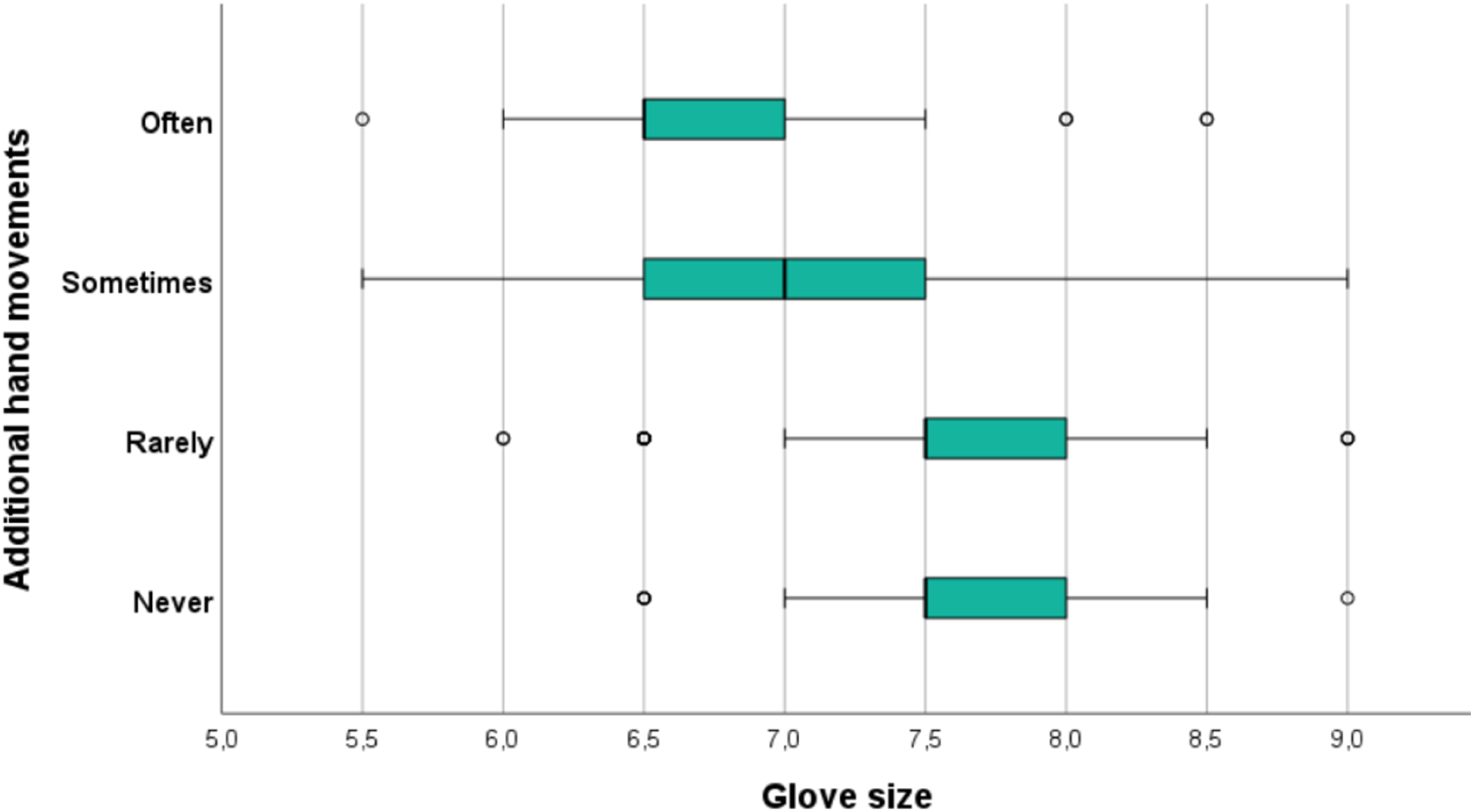
Free-text responses (Items 12, 13, 17, 18, 20) identified recurrent categories of problematic instruments, including rongeurs, retractors, laparoscopic hand instruments, powered drills, and staplers. Reported issues involved excessive weight, large span width, poor balance, and awkward button positioning (Supplement Figure 4).
Among respondents, 13% (54/415) had experience with adjustable or ergonomically improved instruments. Of these, 48.1% (26/54) reported significant improvement, 25.9% (14/54) observed slight improvement, and 25.9% (14/54) noted no change.
In the open-text responses regarding problematic instruments, the Luer rongeur instrument was mentioned most frequently. Specific issues highlighted included its oversized dimensions and span, difficulty with one-handed operation, and the material properties affecting grip. Following this, arthroscopic and laparoscopic cameras were frequently criticized. Respondents noted that these devices were often oversized, making one-handed operation difficult, and that the functional buttons were positioned too far apart. Particularly problematic were instruments used in minimally invasive surgery, such as shavers, laparoscopic and arthroscopic forceps, and arthroscopic tools like trocar sleeves. Issues with the size, weight, and distance of functional buttons on battery-powered devices were also noted. Staplers, commonly used in visceral surgery, were repeatedly mentioned as problematic. Respondents described them as too heavy, with a release span that was too wide, requiring significant force or even two-handed operation. Some participants also criticized the fact that most instruments are designed for right-handed users, which can be a limitation. Additionally, the responses highlighted issues with instruments that were too small, such as the small handles of screwdrivers used in hand surgery. In summary, the open-text responses emphasized that the size, weight, span, and grip of various instruments were frequently problematic. These issues often led to early fatigue or made one-handed operation impossible, necessitating additional hand movements or assistance.
Discussion
The aim of this study was to evaluate the current state of the ergonomics of surgical instruments and devices through a comprehensive survey of surgeons in order to identify specific areas where ergonomic improve Besides hand anthropometry, factors such as wrist posture, coupling forces, instrument weight, and vibration exposure are acknowledged risk factors for musculoskeletal disorders (MSDs) in surgeons. ments are required.
A key finding was the minimal overlap in glove sizes between male and female surgeons. Smaller glove sizes were associated with a significantly higher frequency of fatigue, compensatory movements, reduced subjective surgical precision, and lower safety ratings for existing instruments and devices.
Our findings suggest that the ergonomic challenges reported by surgeons with smaller glove sizes are not caused by the gloves themselves but by the insufficient adaptation of instrument size, span, weight, and grip to smaller hand dimensions.
Oversized handles and wide activation spans force surgeons with smaller hands to use compensatory movements, such as increased thumb abduction or wrist ulnar/radial deviation, which can lead to early fatigue and contribute to musculoskeletal disorders (MSDs).
Moreover, most surgical instruments are primarily designed for right-handed use, which may disadvantage left-handed or ambidextrous surgeons by increasing the need for compensatory hand movements and potentially contributing to fatigue and reduced precision.”
By explicitly linking hand anthropometry to these mechanical demands, we highlight the need for surgical instruments that accommodate a broader range of hand sizes to minimize physical strain and support precision.
The association between smaller glove sizes and increased fatigue or compensatory hand movements should not be interpreted as a problem of glove fit itself. In our study, glove size was used as a practical proxy for hand dimensions. The findings likely reflect a mismatch between the size and span of currently available surgical instruments and the smaller hands of many users rather than issues with surgical glove sizing. Multivariable analyses further confirmed that glove size, rather than gender alone, accounted for most ergonomic disadvantages. Only handling difficulties remained independently associated with gender, suggesting that additional ergonomic factors—such as grip strength, coupling forces, or wrist posture—may also contribute.
Depending on the subspecialty, differing needs were observed in the prioritization of specific features for instruments and devices, reflecting the diverse range of surgical procedures across various disciplines. Free-text responses further identified problematic instruments including rongeurs, retractors, laparoscopic hand instruments, powered drills, and staplers, highlighting specific device categories where ergonomic redesign is most urgently required.
The association between smaller glove sizes and increased fatigue or compensatory hand movements should not be interpreted as a problem of glove fit itself. In our study, glove size was used as a practical proxy for hand dimensions. The findings likely reflect a mismatch between the size and span of currently available surgical instruments and the smaller hands of many users rather than issues with surgical glove sizing. Surgeons with smaller hands may be forced to apply greater force or use additional movements to operate oversized instruments, which can lead to premature fatigue and reduced precision.
The existing literature supports the observation that physical discomfort and fatigue can arise from the use of non-ergonomic surgical instruments and devices. Fram et al. reinforce the relevance of these issues, reporting that 69.8% of surveyed surgeons regularly experience physical discomfort related to the use of surgical instruments, with 47.7% requiring therapy, including over-the-counter medications in 39% of cases. 8
The literature also confirms that the hand sizes of practicing surgeons overlap minimally at a glove size of 7.5. 8 Glove size distribution ranges between 5.5 and 9.6.6,8
A glove size of 6.5 or smaller is significantly associated with greater difficulty in using standard surgical, endoscopic, and laparoscopic instruments, which aligns with the findings of this survey.9,10 Experimental testing comparing ergonomic and standard screwdrivers demonstrated a significant reduction in thumb-tip force for glove sizes 6 and 7, potentially reducing fatigue, compensatory movements, and musculoskeletal discomfort. 11
According to a previous survey, 60.3% of surgeons believe their glove size affects their ability to use surgical instruments. 9 Additionally, 41.5% with glove sizes of 6.5 or smaller report that their hand size negatively impacted their ability to learn surgical procedures. Female surgeons are 3 times more likely to encounter problems when using surgical instruments and devices. 9 The present results are consistent with these reports but add nuance: gender differences observed in unadjusted analyses largely disappeared once glove size was included, further supporting hand anthropometry as the key ergonomic determinant.
However, male surgeons also did not report an ideal state for the usability of instruments and devices in the operating room. Fram et al. identified problematic instruments for both men and women, including designs like the rongeur and repositioning forceps, which appeared unsuitable for either gender. Women additionally reported significant issues with battery-powered drills, arthroscopes, and arthroscopic shavers. 8 Lurie et al. 5 noted problems with the arthroscope (over 66% of respondents) and periarticular repositioning forceps (55%). Surgeons with glove sizes of 7 or smaller reported significantly greater difficulties with wire cutters, Jacob chucks, and motor-driven systems with quick couplings for K-wires, findings consistent with this survey. Ergonomic shortcomings may thus extend beyond user comfort to affect surgical precision and potentially patient safety. Glove size is not the sole factor in evaluating the usability of instruments. Other aspects, such as the distance between functional buttons, the span required for operation, the force needed to activate functions, and the overall hand length—impacted by elastic gloves—should also be considered in instrument design.4,7,12,13 Surgical instruments and devices must be tailored to the physical requirements of surgeons’ hands, the external force demands of procedures, instrument-specific force needs, practicality, and overall ergonomics to ensure efficient and harmonious surgical workflows.
Multiple recent studies confirm the need to adapt current commercially available surgical instruments and devices, as existing prototypes no longer meet modern requirements.7,11,12,14
This study has several limitations. First, selection bias cannot be excluded, as surgeons experiencing ergonomic challenges may have been more motivated to participate. The survey distribution through German and Swiss professional societies and one university hospital mailing list resulted in an overrepresentation of orthopedics and trauma surgeons (81.5%), which limits generalizability to other surgical specialties and international populations. Because the exact number of invitations was not available, a precise response rate could not be calculated.
Second, all data were self-reported, which may introduce recall and perception bias. Objective ergonomic or performance measures (e.g., force analysis, motion tracking, operative time) were not collected to validate subjective outcomes. In addition, while the questionnaire was developed by a multidisciplinary team and piloted internally for clarity, no formal reliability testing (e.g., Cronbach’s α) was performed.
Third, the analysis used glove size as a practical proxy for hand anthropometry. While this approach is supported by prior literature, it does not capture other relevant dimensions such as grip strength, thumb span, or hand length.
Finally, outcomes were not stratified by handedness. Since most surgical instruments are designed for right-handed use, left-handed or ambidextrous surgeons may be at a disadvantage, potentially requiring compensatory movements that contribute to fatigue and reduced precision.
Despite these limitations, the large sample size and wide professional diversity strengthen the validity of the findings and highlight the need for ergonomic adaptations in surgical instrument design.
Conclusion
This study shows that many surgeons — particularly those with smaller glove sizes — report physical discomfort, fatigue, and reduced perceived precision when using instruments with inadequate ergonomics. These findings highlight the need for ergonomic adaptations of surgical instruments to better meet the physical requirements of surgeons and may help reduce physical strain and support surgical precision. However, our data are self-reported and do not allow conclusions about objective operative performance or patient safety.
Glove size emerged as the strongest predictor of ergonomic strain, while gender-related differences were largely explained by hand anthropometry. In addition, specific instruments were identified as particularly problematic, providing concrete starting points for ergonomic redesign. Tailoring surgical instruments to the physical diversity of users may help reduce musculoskeletal strain and improve both surgeon well-being and operative precision.
Supplemental Material
Supplemental Material - Evaluation of the Ergonomics of Surgical Instruments Across Surgical Specialties: Responses From 459 Surgeons
Supplemental Material for Evaluation of the Ergonomics of Surgical Instruments Across Surgical Specialties: Responses From 459 Surgeons by Maria Elze, Georg Osterhoff, Alice Wermke in Surgical Innovation
Footnotes
Acknowledgments
The authors would like to thank the following societies for distributing the questionnaire through their networks: the German Society of Surgery (DGCH), the Society for Arthroscopy and Joint Surgery (AGA), the D-A-CH Association for Shoulder and Elbow Surgery (DVSE), the Swiss Society for Spine Surgery (SGS), the association “Die Chirurginnen e.V.,” Swiss Female Orthopedic, the German Society for General and Visceral Surgery (DGAV), and the German Society for Thoracic Surgery (DGT).
Ethical Consideration
The local ethics committee granted an exemption for anonymized surveys. Consent Statement: By completing the questionnaire, participants provided their consent for further use of the analyzed data.
Author Contributions
AW, ME, and GO had the idea for and designed the study, collected and analyzed the data and wrote the first draft of the manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
Anonymized data can be requested from the corresponding author.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
