Abstract
Androgens and androgen receptor (AR, NR3C4) clearly play a crucial role in prostate cancer progression. Besides, the link between metabolic disorders and the risk of developing a prostate cancer has been emerging these last years. Interestingly, “lipid” nuclear receptors such as LXRα/NR1H3 and LXRβ/NR1H2 (as well as FXRα/NR1H4 and SHP/NR0B2) have been described to decrease the lipid metabolism, while AR increases it. Moreover, these former orphan nuclear receptors can regulate androgen levels and modulate AR activity. Thus, it is not surprising to find such receptors involved in the physiology of prostate. This review is focused on the roles of liver X receptors (LXRs), farnesoid X receptor (FXR), and small heterodimeric partner (SHP) in prostate physiology and their capabilities to interfere with the androgen-regulated pathways by modulating the levels of active androgen within the prostate. By the use of prostate cancer cell lines, mice deficient for these nuclear receptors and human tissue libraries, several authors have pointed out the putative possibility to pharmacologically target these receptors. These data open a new field of research for the development of new drugs that could overcome the castration resistance in prostate cancer, a usual phenomenon in patients.
Abbreviations
ABCA1, ATP-binding cassette A1; ADT, androgen deprivation therapy; AKT/PKB, protein kinase B; AMACR, α-methylacyl CoA racemase; AP-1, activator protein-1; AR, androgen receptor; CDKN1A/p21CIP1, cyclin-dependent kinase inhibitor 1; CDKN1B/p27KIP1, cyclin-dependent kinase inhibitor 1B; CRPC, castration-resistant prostate cancer; DHT, dihydrotestosterone; ERK1/2, extracellular signal–regulated kinases; FXR, farnesoid X receptor; LXR, liver X receptor; MAPK, mitogen-activated protein kinase; MTOR/mTOR, mammalian target of rapamycin; NFκB1/p105, nuclear factor kappa-light-chain-enhancer of activated B cells; OATP, organic-anion-transporting polypeptide; PCa, prostate cancer; PI3K, phosphatidylinositol-4,5-bisphosphate 3-kinase; PSA, prostate-specific antigen; PTEN, Phosphatase and TENsin homolog; SRC/Src, proto-oncogene tyrosine-protein kinase; SHP, small heterodimeric partner; SLCO1B3/OATP1B3, solute carrier organic anion transporter family member 1B3; SLiMs, selective liver X receptor modulators; SOCS3, suppressor of cytokine signaling 3; SREBF/SREBP, sterol regulatory element–binding protein; UGT2, UDP glucuronosyltransferase 2.
Introduction
Prostate Cancer at a Glance
Even though the Greek physician Herophilos (335-280
Today, PCa, along with colorectal and breast cancer, displays a higher rate of prevalence in the developed countries, with about 6-fold difference in comparison with low-incidence countries. This increment has been linked to different risk factors and diagnostic practices. 2 Indeed, the incidence of PCa is constantly increasing due in part to new diagnostic methods, 3 to the increasing impact of prostate-specific antigen (PSA) testing, to the perceptions of PCa fear, 4 and also to the increase in life expectancy. For example, in high-income countries with a low and gradual increase in the rate of PSA testing, such as Japan or the United Kingdom, the prevalence of PCa continues to slightly increase. 5 However, the role of PSA testing in the reduction of PCa-related mortality rates at the population level is rather controverted.6,7
In contrary to some other cancers, PCa has a relatively slow evolution and about 85% of diagnosed PCa are in patients older than 65 years. 8 It is currently admitted that more men die with PCa rather than from it. Indeed, a study performed by Sakr et al 9 pointed out that 50% of the men of 50 years old have a latent PCa on autopsy analyses and that the initiating events leading to a clinically relevant PCa likely occur decades before. Nonetheless, the development and the etiology of the disease are still poorly understood, and various factors such as genetic/ethnical origin, diet, lifestyle, and environmental factors have been suggested to play a role. 10
As already stated, great differences in the incidence of PCa have been observed depending on the ethnical origin or the country of the patients. 11 A Caucasian American has 30% less risk to develop a PCa compared with an African American,12,13 but at the same time, Asians develop twice less PCa than Americans. 14 Yet the genetic background cannot explain everything because the first generation of immigrants from Asia living in the United States has a more important risk of PCa than those living in Asia. 15 Among various factors putatively identified, higher lipid intake in the United States has been pointed out. 16 A comparable observation had been done years before by Shimizu et al 17 in the Japanese population that moved to America.
PCa, Also a Matter of Metabolic Disorder
As enlightened by previous epidemiological studies describing the link between the high lipid intake in Western countries and the risk of developing a PCa, the high prevalence of obesity and metabolic syndrome is associated with worse oncological outcomes in men with PCa 18 ; the tumor is more aggressive and the biochemical recurrence rate is higher. 19 In direction with this link, metformin, an antidiabetic drug that leads to significant improvement of metabolic syndrome parameters, has been shown to induce apoptosis in PCa cells.20,21 However, the use of metformin for the treatment of patients with PCa is still a matter of debate. 22
A high lipogenesis has also been associated to PCa, as it supplies the tumor with key membrane components such as phospholipids and cholesterol. Indeed, cancer cells being characterized by a higher rate of multiplication need to abundantly build membrane for that. 23 Indeed, Swinnen’s group has been among the first to propose pharmacological inhibition of lipogenesis to induce apoptosis in cancer cell lines 24 and to reduce tumor growth in xenograft models, eg, by targeting squalene synthase by zaragozic acid 25 or by blocking acetyl-CoA carboxylases 26 using soraphen A.
Last but not least, cholesterol imbalance has been pointed out in PCa. Cholesterol accumulation in tumors is not a recent observation. White demonstrated in 1909 an “accumulation of crystals of lipid nature in tumors” and suggested that “cholesterol might be associated in some way with the regulation of cell proliferation.” 27 Such cholesterol accumulation was also observed later on in skin cancer. 28 Then Swyer showed for the first time an increase of cholesterol content by 2-fold in a zone of the prostate affected by a hypertrophy compared with the surrounding healthy tissues. 29 Two mechanisms are put forward to explain the intracellular cholesterol accumulation: a higher circulating cholesterol uptake, and an increase in the accumulation of the mevalonate pathway enzymes.30,31
Yue et al identified aberrant accumulation of esterified cholesterol in lipid droplets of high-grade PCa and metastases using imaging data. 32 The authors showed that such cholesteryl ester accumulation was a consequence of loss of the tumor suppressor Phosphatase and TENsin homolog (PTEN), one of the most common genetic events in PCa, and thus subsequent activation of the phosphatidylinositol-4,5-bisphosphate 3-kinase (PI3K)/protein kinase B (PKB/AKT) pathway in PCa cells. In response to the loss of the PTEN, they identified the activation of the mammalian target of rapamycin (MTOR/mTOR) pathway and downstream activation of sterol regulatory element–binding protein (SREBF/SREBP), and the upregulation of LDL receptor (LDL-R 32 ). However, blockade of mTOR by analogs of rapamycin has been shown to be inefficient in castration-resistant prostate cancer (CRPC) so far, 33 but more promising in radioresistant PCa. 34
Hence, despite a higher accumulation of cholesterol within the tumor has been well demonstrated in PCa, no clear link has been however made between circulating cholesterol levels and high Gleason score, positive nodal status, and positive surgical margins. 35 Nevertheless, it has been tempted to test various compounds decreasing the levels of cholesterol in androgen-dependent or -independent cancer cell cultures or in animal models.36-41 Altogether, sufficient data are lacking to support the use of statins for the primary prevention of PCa. Meanwhile, statins have been associated with improved PCa-specific survival, particularly in men undergoing radiotherapy, suggesting usefulness of statins in secondary and tertiary prevention. 42 Yet more epidemiological and mechanistic studies are needed to eventually use statins in PCa. 43
Androgens and Androgen Receptor Control PCa Progression
Androgens and androgen receptor (AR, NR3C4) play a crucial role in PCa. Indeed, since Huggins and Hodges’ princeps article in 1941, 44 it has been admitted that PCa is driven by androgen levels and androgen activity through AR transcriptional regulation.
Among the various androgens, dihydrotestosterone (DHT) is the most active on AR to induce cell proliferation. DHT is synthesized from testosterone by 5α-reductase 2 (SRD5A2) (Figure 1), which can be targeted in PCa by dutasteride, a 5α-reductase inhibitor, despite some controversies. 45 DHT could also be synthesized from androsterone and 5α-androstane-3α,17β-diol even in small amounts. On the opposite, androsterone, 5α-androstane-3α,17β-diol, and DHT can be transformed in nonactive glucuronides by UDP glucuronosyltransferase 2 (UGT2) B15 and B17. 46 Note that AR downregulates the expression of UGT2B15/17 (Figure 2), thus decreasing the inactivation of androgens. 47
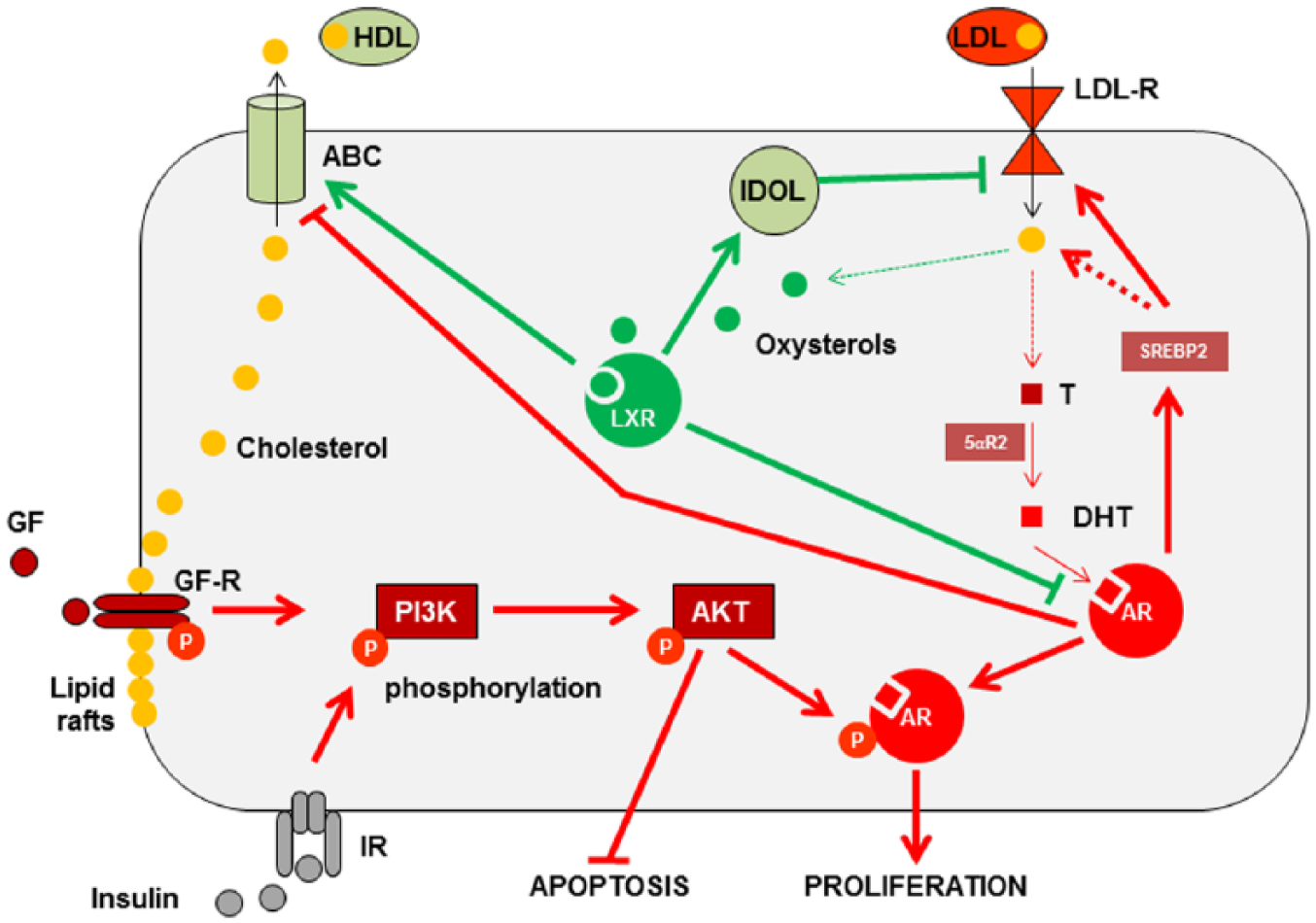
Interconnection between LXRs and AR in prostate cell.
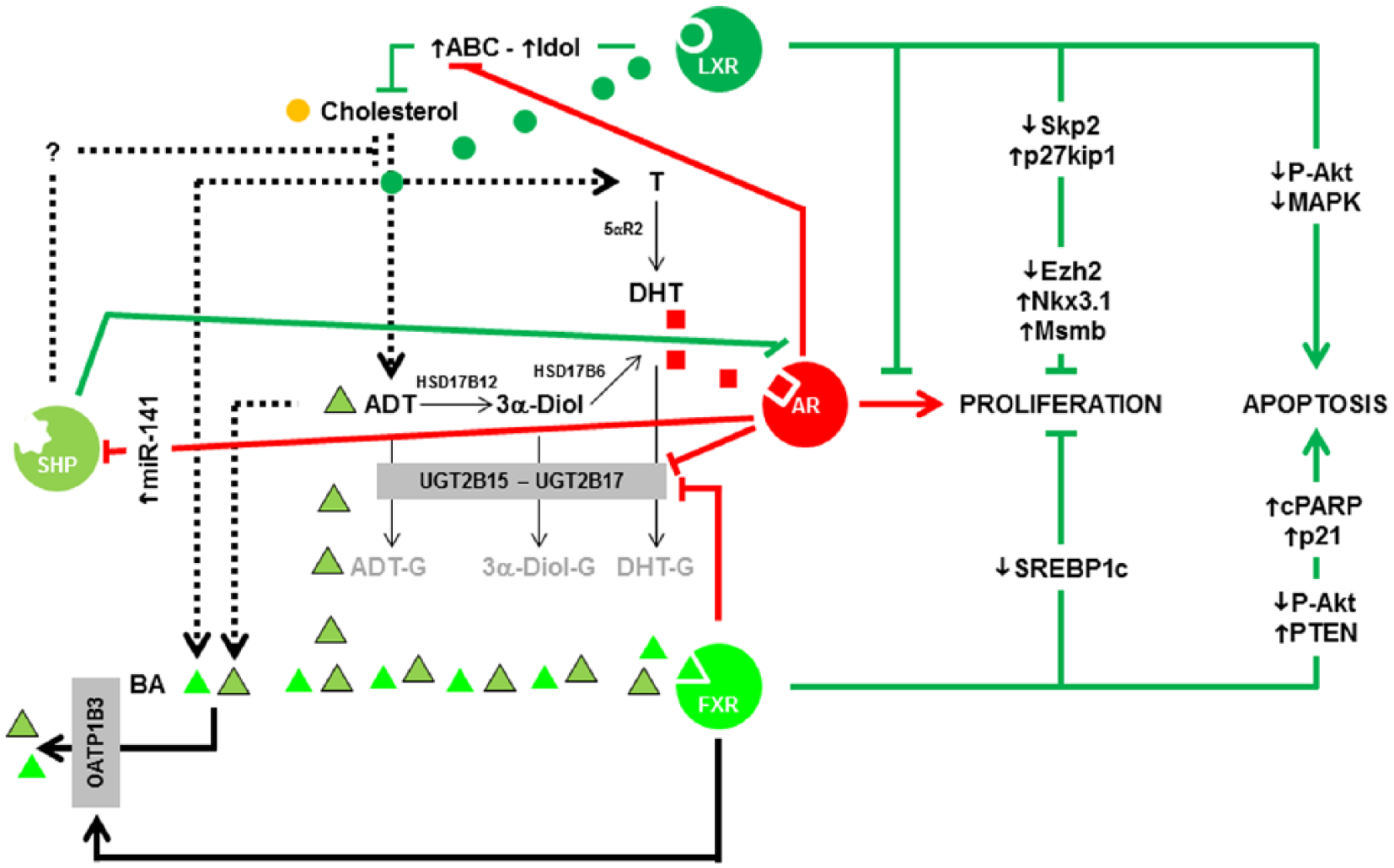
Summary of the interconnections among AR, LXRs, FXR, and SHP in prostate cell.
Hence, PCa is initially an androgen-dependent disease; unfortunately, about 30% of patients will relapse after primary therapy. 48 Androgen deprivation therapy (ADT), by surgical or biochemical castration, is the main treatment for relapsed patients and provides temporary relief to tumor burden. 49 This step is performed by downregulating androgen production by using steroid synthesis inhibitors, as well as antiandrogens, that act at the level of AR. 49 However, most of the PCa will dedifferentiate to CRPC and inevitably will develop a more aggressive and metastatic cancer. Despite approved treatment options for this PCa stage (eg, taxane compounds; abiraterone that inhibits 17alpha-hydroxylase involved in androgen synthesis; enzalutamide that blocks AR; sipuleucel-T, a therapeutic vaccine), drug resistance will eventually develop in few months.
The exact mechanism of transition from castration sensitive PCa to castration-resistant disease is still not fully understood, but AR definitely plays a key role as described by Bevan’s group 50 ; several mechanisms could be cited, among them an increased number of the AR encoding gene copies making them more sensitive to lower levels of androgens, development of cellular clones harboring mutations within the ligand-binding domain of AR and hence potentially activated by steroids that usually do not bind AR, and modifications of AR coactivators or corepressors. Hence, despite an extremely low level of circulating androgens, AR remains active and continues to drive PCa progression.
Beside the classical ligand-regulation of the transcriptional activity, AR could also rapidly interact with the nonreceptor tyrosine kinase SRC/Src increasing cell proliferation through activation of the mitogen-activated protein kinase (MAPK)/extracellular signal–regulated kinases (ERK1/2) cascade, 51 or with PI3K/AKT signaling pathway (Figure 1), and controlling cell survival. 52 Based on that, innovative therapies will be necessary to counteract this so-called nongenomic signaling of AR during the establishment of metastatic CRPC. 53
Finally, “androgens meet lipids” (Figure 1) as AR activation increases fatty acid synthesis 23,54-56 and SREBP2, 30 a key-player in de novo synthesis of cholesterol and its cellular uptake, 57 and decreases ATP-binding cassette A1 (ABCA1), a cholesterol export pump. 58 This last point is crucial because cholesterol is an obligatory precursor for testosterone and DHT synthesis, the only two active androgens on AR 59 ; more importantly, tumor cells also have the ability to abnormally synthesize DHT from cholesterol 60 or from adrenal androgens.61,62
Together with AR, other nuclear receptors have been involved in PCa (for a review, see Leach et al 50 ); among them the popular “Ménage-à-trois” LXR-FXR-SHP (liver X receptor–farnesoid X receptor–small heterodimeric partner) has been described to be the major player in the regulation of both cholesterol and bile acid homeostasis. 63 Altogether, targeting this new “Ménage-à-quatre” appears to be of importance to take care of the prostate. Interestingly, the role of these 3 nuclear receptors has been emerging these last years in ex vivo or in vivo experiments, especially with the generation of transgenic animals knock-out for LXRs. Noteworthy, The Cancer Genome Atlas pointed out that these nuclear receptors could present alterations of copy numbers of their respective encoding genes in PCa. 50
LXRα and LXRβ Are Involved in Prostate Physiology
LXRα/NR1H3 and LXRβ/NR1H2 (as well as FXRα/NR1H4 and SHP/NR0B2) are members of the nuclear receptor superfamily. They are composed of several functional domains, among them a central DNA-binding domain and a C-terminal ligand-biding domain. 64 At the end of the 1990s, Janowski et al demonstrated that LXRs are the bona fide receptors for oxysterols,65,66 oxidized derivatives of cholesterol. Hence, it was suggested that LXRs could regulate cholesterol homeostasis in the cell and was demonstrated thanks to the analysis of Lxr-deficient mice. 67 Since this seminal article, others groups have associated LXR roles to numerous physiological functions.64,68
In the prostate, Liao’s group was the first to evoke a putative positive role of LXRs in PCa. 58 The authors showed that ABCA1, a bona fide LXR-target gene which increases cholesterol export, was downregulated by androgens (Figure 2) in LNCaP cells. 58 The same group identified that activation of LXRs by the synthetic agonist T0901317 decreased the percentage of S-phase LNCaP cells in a dose-dependent manner and increased the expression of cyclin-dependent kinase inhibitor CDKN1B/p27KIP158, by decreasing the S-phase kinase associated protein 2 (SKP2) involved in the degradation of cell cycle inhibitors. 69 At last, Chuu et al demonstrated that LXRs and some of their target genes were decreased during the progression of androgen-dependent tumor to androgen-independent relapsed tumors in a xenograft model. 70 These data thus made a clear link between LXRs and the proliferative capacities of PCa cells (Figure 2). Likewise, we identified that Lxrα;β-deficient mice fed a high cholesterol diet presented prostatic intraepithelial neoplasia characterized by an accumulation of the oncogene and histone methyl transferase Enhancer of Zeste Homolog 2 (EZH2) which results in the downregulation of the tumor suppressors microseminoprotein beta (MSMB) and NK3 homeobox 1 (NKX3.1). 71 It is noteworthy that overexpression of EZH2 has been described in patients with an aggressive PCa. 72 EZH2 controls prostate cell proliferation through the epigenetic silencing of NKX3.1 73 and MSMB. 74 In wild-type mice fed a high cholesterol diet, LXRs induce the transcription of Inducible Degrader of the LDL receptor MYLIP/IDOL (Figures 1 and 2), a ubiquitin ligase that targets LDL-R, and of ABC transporters, altogether maintaining a controlled level of cholesterol and a low amount of EZH2. 71 So far, it has not been possible to dissociate the exact role of each LXR isoform as they both compensate each other.
In addition to the role of LXRs in the control of cellular cholesterol content and prostate cell proliferation, we showed that the activation of LXRs by various natural or synthetic ligands increases the level of apoptosis in LNCaP cells. 75 This phenomenon is linked to the presence of smaller and thinner lipid rafts after LXR stimulation and the downregulation of AKT phosphorylation in these lipid rafts. After having derived new models of epithelial cells from the dorsal prostate (MPECs) of wild-type or Lxr-deficient mice, Dufour et al enlightened that LXRs modulate AKT and MAPK phosphorylation accumulation, making them potential mediators of LXRs in cell cycle control 76 (Figure 2). Altogether, these results confirm that LXRs are becoming exquisite pharmacological targets for PCa, unless specific modulators, we called SLiMs (selective LXR modulators77,78), could be developed.
On the other side, LXRs also control AR activity. Indeed, Lxr-deficient mice also develop benign prostatic hyperplasia (BPH). 79 In man, BPH is clearly due to an excessive activity of AR and the production of DHT. 80 Using transgenic animals, we were able to demonstrate that LXRα acts as a key modulator of the cross talk between the stromal and epithelial compartments, which is essential for the integration of androgen signaling in the prostate and its effect on the epithelium. 81 Interestingly, Tsui et al 82 pointed out that LXR expression was higher in androgen-sensitive LNCaP cells than in other PCa cell lines. Moreover, T0901317-activated LXRs decrease AR accumulation and PSA production in LNCaP. Overall, AR and LXRs are definitively interconnected (Figure 1). These data open numerous opportunities to develop new therapeutic concepts especially in CRPC situations where AR activity could become independent of androgen levels. If LXRs negatively modulate AR accumulation, a SLiM could increase PCa cell apoptosis, as well as decrease AR activity, hence, bypassing the castration-resistant stage.
One of the most challenging issues in PCa is to slow down the metastatic potential of the tumor. 83 Fu et al described an interesting effect of GW3965, another LXR synthetic ligand, on LNCaP cells. Activation of LXR increases the suppressor of cytokine signaling 3 (SOCS3) accumulation, followed by a decrease of phosphorylated AKT, activator protein-1 (AP-1), and nuclear factor kappa-light-chain-enhancer of activated B cells (NFκB1/p105). 84 GW3965 also inhibited PCa invasion in xenografted mice, suggesting that LXRs could be targetable to prevent metastases.
However, these potential effects of LXRs in PCa treatment should be modulated. Indeed, it should be kept in mind that, in prostate, tumor cells are surrounded by immune cells such as dendritic cells that initiate immune responses, including antitumor activity after their CC chemokine receptor-7 (CCR7)-dependent migration to lymphoid organs. Activation of LXRα inhibits CCR7 expression dampening the antitumor immune responses. 85 Likewise, drugs inhibiting cholesterol synthesis (and thus LXR ligands), such as zaragozic acid, increase the efficacy of the treatments in xenografted mice with tumors. 86 Once again, these contradictory results enlighten the necessity to develop tissue- and cell-specific LXR ligands to decipher the exact roles of each LXR in each cell type. It should also be noticed that no variation of LXRα and/or LXRβ expression has been linked to cancer grades. This would imply to stratify patients’ cohorts, which has not been performed so far.
Putative Role of FXR in PCa
FXR/NR1H4 is the nuclear receptor for bile acids. 87 However, the inactive androgen androsterone has also been described as a potent activator of FXR. 88 This point is important because androsterone is present in prostate. Conversely, to LXR and the historical story of cholesterol accumulation in prostate tumors, the link between FXR, bile acids, and prostate physiology is less evident.
The first “historical” link came with Wang and Schaffner 89 who observed that BIO 87-20 hamsters, developing spontaneous cystic prostate hypertrophy, had a lower prostate size and weight with much less distended prostatic acini when were treated with colestipol, a bile-acid-sequestering anion-exchange resin. More recently, it has been shown that bile acid content is increased in patients with a PCa treated with an ADT 90 ; in parallel, ADT has been associated with an increased risk of diverse biliary diseases. 91 Alpha-methylacyl CoA racemase (AMACR) is overexpressed in PCa 92 and is a better diagnostic marker than PSA. AMACR plays a key role in the β oxidation of branched chain fatty acids and the bile acid intermediates dihydroxycholestanoic acid and trihydroxycholestanoic acid. Furthermore, AMACR is highly expressed in androgen-sensitive PCa cell lines and is required for the proliferation of these cells. 93
Even though lithocholic acid selectively induces apoptosis in androgen-sensitive and -insensitive prostate cell lines,94,95 few studies have focused on the molecular effects of FXR activation in androgen-sensitive or androgen-insensitive prostate cell lines. Indeed, FXR inhibits cell proliferation by decreasing lipid metabolism via targeting SREBP1c (Figure 2). 96 Likewise, chenodeoxycholic acid (CDCA, a natural FXR ligand) and GW4065 (a synthetic FXR agonist) decrease LNCaP cell proliferation by the induction of PTEN accumulation, which in turn decreases the phosphorylation of AKT and the survival pathway. 97 Interestingly, new derivatives of ursodeoxycholic acid and CDCA induce the apoptosis of human prostate androgen-insensitive carcinoma PC-3 cells by increasing cyclin-dependent kinase inhibitor 1 CDKN1A/p21CIP1 and the cleaved form of poly [ADP-ribose] polymerase 1 PARP1. 98 However, it has not been proved yet that FXR mediates the effect of these molecules. Finally, the most important point is that FXR accumulation was found to be significantly lower, at both mRNA and protein levels, in human PCa tissues compared with the pair-matched adjacent normal tissues. 97 Again, no correlation was made with grades/stages of the tumors by the authors. Based on these results, one can suggest that FXR ligands could have some benefit in the treatment of PCa.
Unfortunately, other data showed a negative role of bile acids and FXR in the development of PCa. First of all, androgen metabolite androsterone, which is also an activator of FXR, reduces the glucuronidation of androgens catalyzed by UGT2B15/B17 in an FXR-dependent manner in LNCaP cells. 99 Such an action would increase the levels of androsterone, 5α-androstane-3α,17β-diol, and finally DHT, and thus activate AR and induce cell proliferation. On the contrary, the increase of androsterone could also neutralize the AR-induced proliferation by blocking the proliferation via FXR (Figure 2). This dual paradoxical effect of FXR is also seen in the regulation of the solute carrier organic anion transporter family member 1B3 SLCO1B3/OATP1B3, which is an export pump for steroids and bile acids 100 and seems to be upregulated by FXR in the prostate, 101 but not in the liver. 102 If this regulation is efficient in the prostate, FXR would deplete the cells in steroids (including bile acids) by increasing OATP1B3; bile acid depletion will act as a safety valve and will reduce FXR activity. More investigations are thus needed using adequate in vivo models to understand how FXR targeting could be interesting in PCa management.
SHP, a Noncanonical Nuclear Receptor With Significant Potential in PCa
Short heterodimer partner (SHP/NR0B2) is an atypical orphan nuclear receptor: It lacks the classical DNA- and possesses a ligand-binding domain. Despite its strong repressive activity on other nuclear receptors such as AR, no known ligand for SHP has been identified so far. 103
Initially described as downregulating bile acid synthesis in liver by decreasing 7α-cholesterol hydroxylase CYP7A1 in an LXR-dependent manner, 104 SHP became a member of the Triad with LXR and FXR when it appeared that FXR was the nuclear receptor for bile acids 105 and SHP was one of its bona fide target genes.
Indeed, it was the discovery of synthetic SHP ligands that gave the opportunity to link SHP to PCa. 106 Some of these ligands had a strong inhibitory effect on proliferation and inducing effect on apoptosis in the PCa androgen-insensitive DU-145 cells (50% efficacy less than 1µM).
In spite of SHP role in the regulation of androgen synthesis directly in the testis 107 or indirectly via gonadotropin hormones, 108 such role has never been described so far in prostate, but cannot be excluded. Besides, SHP seems to play an antitumor role in many types of cancers 109 ; unfortunately, SHP mRNA and/or protein accumulation has never been studied in prostate tumors. The centerpiece pointing out SHP as interesting in PCa comes from the fact that AR negatively regulates the amount of SHP (Figure 2). 110 Indeed, miR-141 which targets SHP is induced by AR in LNCaP cells. One could thus hypothesize that increasing concentration of active androgens would block SHP, which antagonizes AR activity and neutralizes the proliferative role of androgens.
Conclusion and Perspectives
PCa incidence is drastically increasing in Westernized countries. Today, the main challenge is to have good diagnostic and prognostic markers that could help in the management of the patients. As androgens have been playing a central role in the progression of the tumors, most of these markers were previously obtained focusing on the screening of AR target genes. The involvement of other transcription factors, members or not of the nuclear receptor superfamily, has made possible to identify new signaling pathways regulating progression of the tumor until metastasis. LXR, FXR, and SHP have been associated for many years to the regulation of metabolism. It is finally not surprising to find them as putative pharmacological targets to treat PCa, especially knowing that they can regulate androgen levels and AR activity (Figure 1). Altogether, developing new specific molecules regulating these nuclear receptors will give the opportunity to offer different therapeutic arsenals. This is probably the most challenging issue, especially in CRPC, which is the fate of almost all PCa.
Footnotes
Author Contributions
M.C., S.D., S.M., S.B., A.M., and J.-M.A.L. collected the information, wrote the manuscript, and drew the figures; all authors read and approved the manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Part of this work was financed by grants from Université Blaise Pascal, Region Auvergne Rhône Alpes, Fond Européen de Developpement Régional (FEDER), AAP Plan Cancer Environnement 2016.
