Abstract
Background
Although cognitive training has shown potential for treating post-stroke aphasia (PSA), its efficacy varies across studies, and the optimal training approaches remain unclear.
Objective
To evaluate and compare the effects of distinct cognitive training interventions, either combined with or independent of speech and language therapy (SLT), on language function in individuals with PSA.
Methods
A systematic search encompassing PubMed, Embase, Cochrane Library, China National Knowledge Infrastructure, Wanfang, VIP, and Chinese Biomedical Databases was conducted for randomized controlled trials (RCTs). A network meta-analysis evaluated interventions, including computer-assisted cognitive training (CCT), conventional cognitive training (CT), virtual reality (VR)-based cognitive training (vrCT), telerehabilitation computer-assisted cognitive training (tCCT), working memory (WM) training, and attention training (AT).
Results
Eleven RCTs comprising 501 participants were included. Individuals with PSA who underwent combined WM training with SLT led to significantly enhanced Western Aphasia Battery (WAB) Aphasia Quotient (AQ), as well as in spontaneous speech, auditory comprehension, repetition, and naming, compared to those receiving SLT alone. This combination was more effective than both CCT with SLT and tCCT with SLT in improving WAB AQ. Similarly, it outperformed both CCT with SLT and vrCT with SLT in enhancing WAB spontaneous speech. Additionally, both AT and CT combined with SLT were more effective than SLT alone in enhancing WAB spontaneous speech. Specifically, AT combined with SLT proved more effective than vrCT with SLT in this area. Moreover, vrCT combined with SLT significantly improved auditory comprehension compared with SLT alone.
Conclusions
Combining WM training and SLT and integrating vrCT with SLT both significantly enhance language function in individuals with PSA, compared with SLT alone. Our findings advocate for the use of these cognitive training approaches as promising strategies for language rehabilitation in this population. PROSPERO registration number: CRD42023462361.
Introduction
According to the latest 2019 Global Burden of Disease (GBD) report, stroke ranks as the third primary level 3 global cause of both mortality and disability, with ischemic stroke accounting for 62.4% of all new stroke incidents. 1 Aphasic symptoms affect approximately one-third of the more than 10 million new stroke patients.2,3 Post-stroke aphasia (PSA), an acquired language disorder, profoundly affects linguistic functions such as oral expression, auditory comprehension, reading, and writing. 4 This functional impairment consequently leads to compromised social interactions, reduced career competence, and an overall reduced quality of life. 5 These multifaceted challenges impose significant burdens on both affected individuals and society.
The current interventions for PSA encompass a diverse spectrum of approaches, including speech and language therapy (SLT), cognitive neurorehabilitation, melodic intonation therapy, pharmacotherapy, virtual reality, and noninvasive brain stimulation techniques. 6 Of these, SLT is predominantly considered the gold standard in PSA rehabilitation and is widely accepted as such. 7 Although PSA primarily manifests as a linguistic impediment, its frequent co-occurrence with nonlinguistic cognitive impairments, such as deficits in working memory, executive functions, and attention, introduces a substantial obstacle to the language recovery process.8-10 Thus, a transition from language-based rehabilitation to a broader cognitive-focused approach becomes essential, as relying solely on SLT may be insufficient for addressing this complex issue.
Previous studies have established the pivotal role of domain-general cognitive control in facilitating the potential of recovery for individuals with PSA.11,12 The specificity of nonlinguistic cognitive deficits in predicting language function recovery and response to language-oriented treatments among individuals with PSA has been emphasized in more recent studies.13,14 Expanding the therapy spectrum beyond verbal characteristics is becoming increasingly important among researchers, given the important role that nonlinguistic function plays in PSA recovery. This involves the integration of domain-general cognitive components, including but not limited to working memory (WM), attention, and executive functions, into existing language rehabilitation strategies.15,16
In this context, cognitive training has emerged as a promising strategy for addressing PSA, with encouraging outcomes from computerized cognitive training, WM training, and VR-based cognitive training, etc. Specifically, computerized and VR-based training programs offer unique advantages in the realm of telerehabilitation, suggesting a potential avenue for e-health interventions in PSA recovery.
For instance, a recent study demonstrated that combining general cognitive training with SLT significantly improves PSA recovery compared to SLT alone. This general cognitive training includes tasks that target attention, memory, and executive functions. 17 Notably, the combined therapy was administered both in-person and via telerehabilitation, with each modality showing enhanced outcomes compared to SLT alone. Furthermore, WM training has led to significant enhancements in language and memory for PSA compared to the SLT group. 18 A recent systematic review evaluated the efficacy of short-term memory (STM) and WM treatments in PSA. The review reported over 80% improvements in memory functions and spoken language comprehension across various studies. 19 Moreover, VR offers a promising self-administered treatment option, enabling intensive home-based therapy with the potential for extended daily sessions 20 and enhancement of cognitive functions. 21 Recent studies have demonstrated that VR exerts a marginally favorable clinical impact on language impairment severity in PSA when compared with traditional SLT, 22 with evidence supporting the feasibility and safety of VR-based cognitive and language therapy for PSA. 23 Additionally, a previous study showed that incorporating gradual attention training with SLT significantly improved language function in patients with PSA, particularly in listening comprehension and naming abilities. 24 Another study introduced a novel interfered-naming therapy for PSA that integrates linguistic and executive processing. This approach demonstrated improvements in language functions by reducing distractor repetition and improving lexical-semantic processing, highlighting the importance of executive functions in language recovery. 25
Although cognitive training alone can enhance general cognitive functions, its combination with SLT is generally considered to be a more effective strategy for treating language and communication disorders such as PSA. However, more research is needed to elucidate the synergistic benefits of this combined approach and to identify the most effective cognitive training methods for targeting specific language domains in PSA.
Network meta-analysis (NMA), as an essential statistical tool in evidence-based medicine, enables the concurrent comparison and ranking of multiple treatments for a given condition, leveraging both direct and indirect evidence. Unlike conventional pairwise meta-analysis, NMA offers the distinct advantages of evaluating intervention efficacy within a unified framework, enhancing precision, facilitating comparisons between interventions not directly pitted against each other in trials, and establishing a hierarchy of intervention efficacy.26-28
Therefore, NMA was performed to systematically evaluate and compare the effects of various combinations of cognitive training and SLT on PSA. Our findings offer valuable insights for optimizing clinical interventions and tailoring patient care in the context of PSA.
Materials and Methods
This study adheres to the guidelines specified in the extension for NMA of the Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA) statement. 29 Detailed information can be found in Supplemental Material Table S1. The protocol for this study was registered with the International Prospective Register of Systematic Reviews (PROSPERO) under the registration number CRD42023462361.
Search Strategy
A comprehensive search was conducted across multiple databases, including PubMed, Embase, the Cochrane Library, the China National Knowledge Infrastructure, the Wanfang Database, the VIP Database, and Chinese Biomedical Databases, from their inception until 18 June, 2023. We did not apply any language or ethnicity filters for trial participants. Both Medical Subject Heading (MeSH) terms and free-text keywords were utilized. The complete search strategy and terms are available in Supplemental Material Table S2.
Eligibility Criteria
Two investigators, the first and second authors independently screened the records using a predetermined selection pipeline, which included an assessment of titles, abstracts, and full-text articles. In cases of discrepancies, a third reviewer, the third author was consulted for resolution. Studies that met the following criteria were included in the meta-analysis.
Inclusion Criteria
Participants received a confirmed diagnosis of PSA determined by standardized language function scales, including but not limited to the Western Aphasia Battery (WAB), Chinese Rehabilitation Research Center Aphasia Examination (CRRCAE), Aphasia Battery of Chinese (ABC), and neuroimaging techniques such as computed tomography (CT) or magnetic resonance imaging (MRI); (2) The experimental group received cognitive training, encompassing computer-assisted cognitive training (CCT), telerehabilitation computer-assisted cognitive training (tCCT), conventional cognitive training (CT) by language rehabilitation therapists, VR-based cognitive training (vrCT), working memory training (WM), and attention training (AT). The general cognitive training regimen—encompassing CCT, tCCT, CT, and vrCT—targeted a range of cognitive functions such as working memory, attention, executive functions, and information processing. Additionally, separate interventions that each focused on a single specific cognitive function, such as working memory or attention, were also considered. These cognitive training methods can be implemented individually or in combination with SLT; (3) The control group received SLT or any of the cognitive training approaches mentioned above; (4) The primary outcome measures should include the WAB scale, the (AQ) derived from the WAB for assessing the overall severity of aphasia, and the 4 subdomains of speech: spontaneous speech, auditory comprehension, repetition, and naming; (5) Only clinical randomized controlled trials (RCTs) involving human participants were eligible for inclusion.
Exclusion Criteria
(1) Lack of a precise PSA diagnosis; (2) Unavailability of eligible outcome indicators or incalculable data; (3) Interventions that are inconsistent with the inclusion criteria; (4) Types of publications such as systematic reviews, meta-analyses, conference abstracts, case reports, and clinical protocols.
Data Extraction and Quality Assessment
Data from eligible studies were extracted independently by 2 reviewers (the first and second authors) and assessed by a third experienced investigator (the third author) to ensure accuracy. The extracted data encompassed various key aspects, including demographic information (age, sex, education level, handedness, and first language), stroke conditions (stroke etiology, aphasia type, time post-onset stroke, onset times, and stages of diseases), study characteristics (intervention details, frequency, duration, and total number of sessions), and pre- and post-language outcomes (AQ, spontaneous speech, auditory comprehension, repetition, and naming) using a predefined Excel form.
Using the Cochrane risk-of-bias tool 2.0 (RoB2), 2 independent reviewers (the first and fourth authors) assessed the quality of the included studies. 30 The evaluation covered 5 essential domains: the randomization process, deviations from the intended interventions, missing outcome data, measurement of the outcome, and selection of the reported result. The overall risk-of-bias judgment was classified into “low risk of bias,” “some concerns,” and “high risk of bias.” Any discrepancies between the reviewers’ assessments were resolved through discussion with a senior investigator (the third author) to achieve consensus.
Data Synthesis and Statistical Analysis
NMA was performed using Stata software version 17.0. Language scale values pre- and post-interventions were treated as continuous variables and presented as means with a standard deviation (SD). Given the potential variations across different versions of the WAB, we employed the standardized mean difference (SMD) with an estimated 95% confidence interval (CI) as outcome indicators. To illustrate the direct comparisons among interventions, we used a network evidence plot. Each node in the plot represents a distinct intervention, with connecting lines showing head-to-head comparisons. Node size indicates intervention sample size, while the width of connecting lines reflects the number of studies directly comparing interventions.
To ensure the integrity of our analysis, both local and global inconsistency assessments were conducted. Local inconsistencies were evaluated using the node-splitting method, which compares estimated effects from both direct and indirect comparisons across different interventions. A
To evaluate the relative efficacy of interventions, we employed the Surface Under the Cumulative Ranking Curve (SUCRA) metric. A SUCRA value closer to 100% indicated a higher probability of the intervention being ranked at the top.
32
This information was then synthesized into a league table presenting the relative efficacy of all possible pairwise interventions. Treatments were ranked from most to least effective along the main diagonal of the table. The table showed the SMD (with 95% CI) for each treatment compared to the reference treatment based on the WAB scale. A positive SMD value denoted a favorable effect on improving WAB scores in the corresponding column. Finally, to assess publication bias or other small-study effects, network funnel plots were generated, following the criterion for symmetry
33
along with Egger’s tests (significance level of
Results
Study Selection
A total of 3419 studies were identified through the initial search, of which 634 were excluded due to duplication. Subsequently, 2785 remaining articles were screened based on their titles and abstracts, leading to the exclusion of 2493 articles for reasons of irrelevancy. The full texts of the remaining 292 articles were further evaluated, and 281 articles were excluded (for various reasons, including being reviews or conference abstracts, not being RCTs, lacking standard interventions and controls, not diagnosing with PSA, having no eligible outcomes, or containing incalculable data). Ultimately, 11 studies were included in this NMA. Figure 1 provides a detailed flowchart of the literature search process.
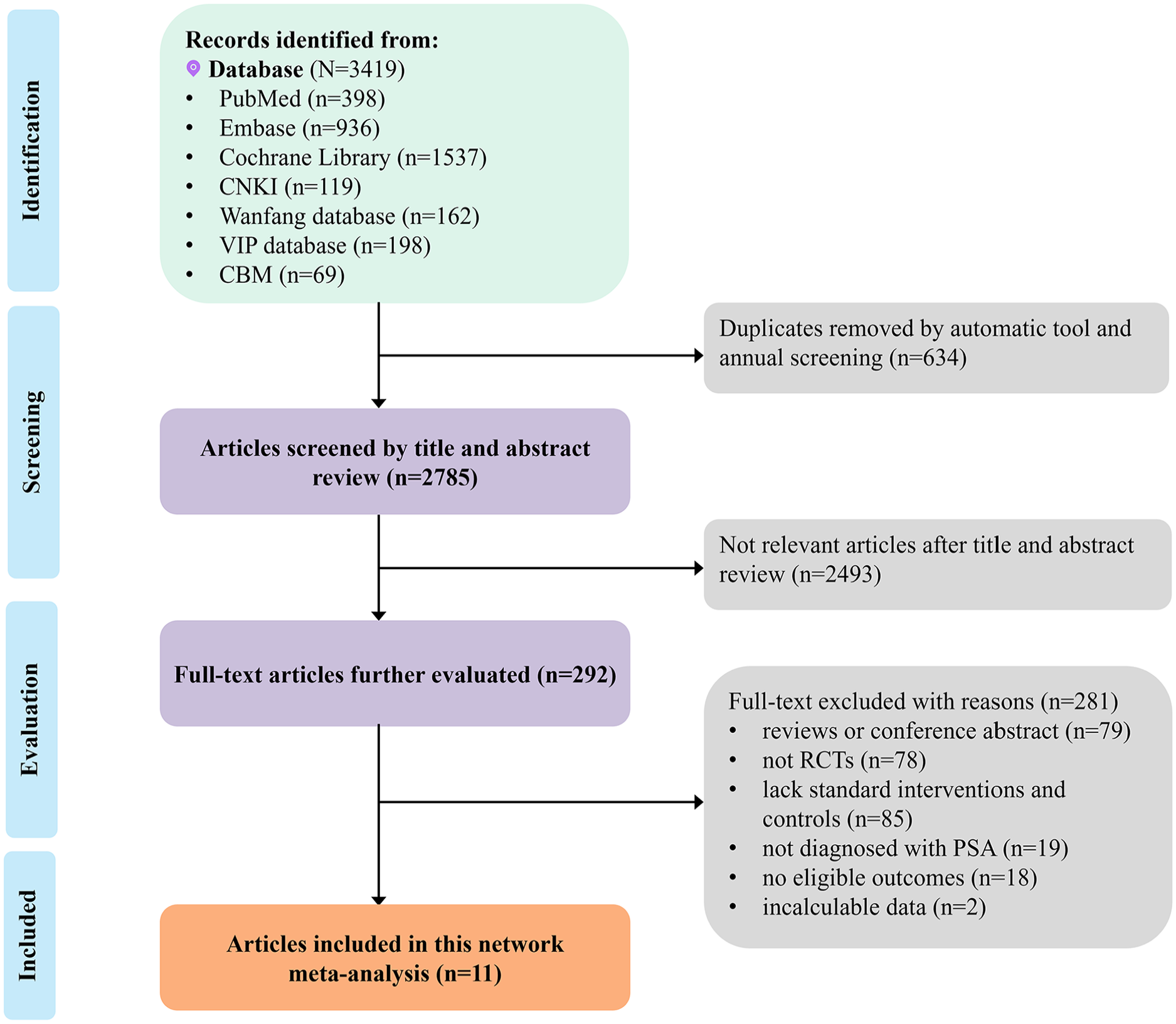
Flow chart of literature search and selection.
Study Characteristics
A total of 501 participants (324 males) with PSA were included in this NMA. Among the 11 selected studies, 5 were published in English and 6 in Chinese. Of these, 2 studies involving participants whose first language was English, while the remaining 9 involved participants whose first language was Chinese. Additionally, the publication dates of these studies ranged from 2017 to 2023.
In terms of interventions, 2 studies utilized CCT and tCCT,17,34 1 employed conventional cognitive training (CT), 35 2 used VR-based cognitive training (vrCT),23,36 4 specifically focused on WM training,37-40 and 2 used attention training (AT).24,41 Notably, both the WM and AT interventions were delivered through computer-assisted methods.
For outcome measurements, all trials reported pre- and post-intervention results from the WAB scale, including AQ, spontaneous speech, auditory comprehension, repetition, and naming. Overall, the data from the studies indicates that various cognitive treatments consistently improve multiple language-related aspects of PSA, as measured by the WAB. These findings suggest the potential efficacy of cognitive training in enhancing language functions in individuals with PSA. Detailed characteristics of the included studies are shown in Table 1 and Supplemental Tables S3/S4/S5.
Characteristics of the Included Studies.
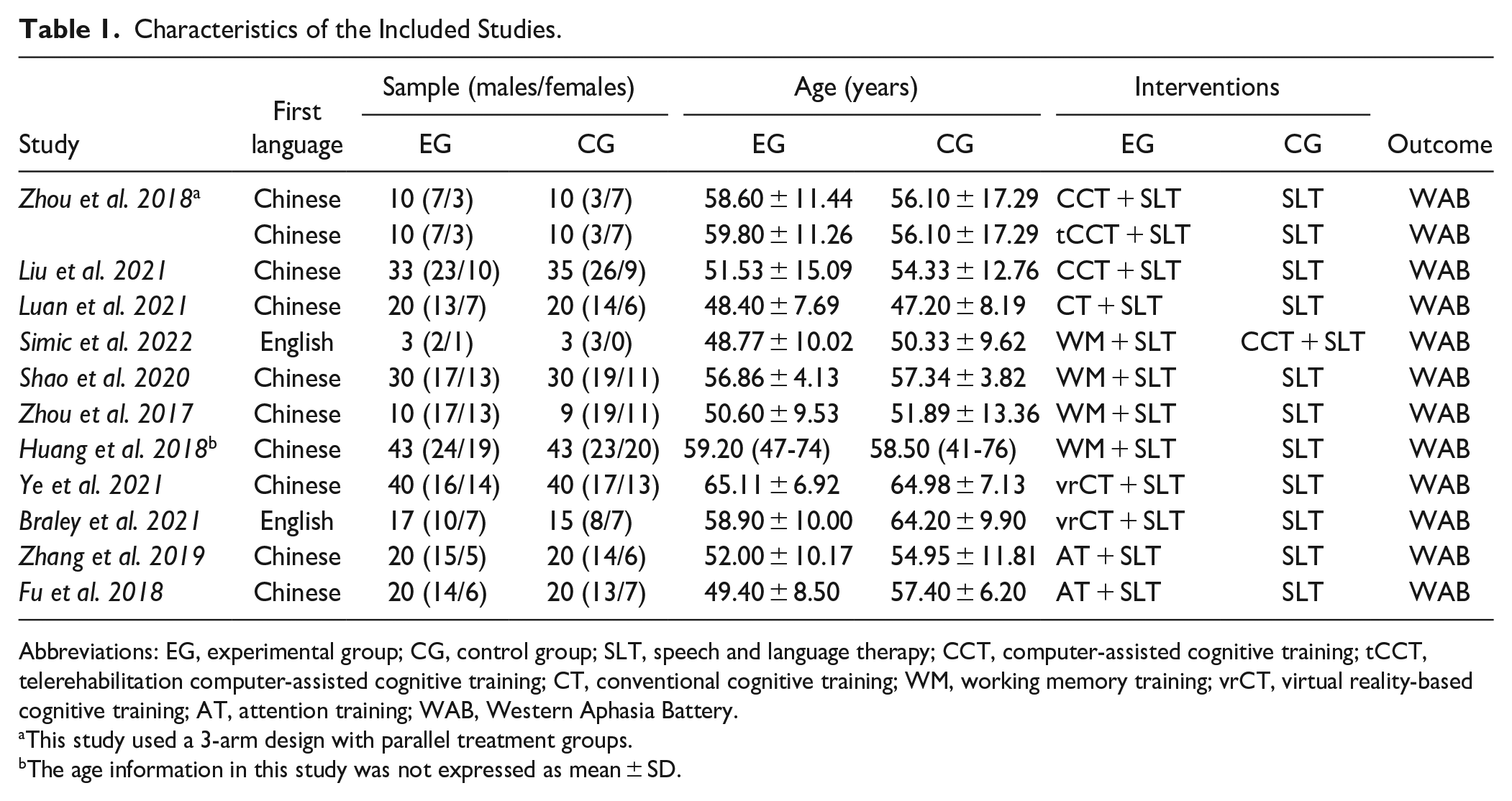
Abbreviations: EG, experimental group; CG, control group; SLT, speech and language therapy; CCT, computer-assisted cognitive training; tCCT, telerehabilitation computer-assisted cognitive training; CT, conventional cognitive training; WM, working memory training; vrCT, virtual reality-based cognitive training; AT, attention training; WAB, Western Aphasia Battery.
This study used a 3-arm design with parallel treatment groups.
The age information in this study was not expressed as mean ± SD.
Risk of Bias
We employed the PRISMA RoB2 tool in the NMA to assess the risk of bias across 5 domains in the included studies. All studies were rated as having some concerns regarding the overall risk of bias. In terms of outcome measurement, only a small proportion of studies presented a high risk of bias. Specifically, issues such as the randomization process, deviations from intended interventions, and selection of reported results were areas of concern in most trials. All trials presented a low risk of bias in terms of missing outcome data. Regarding the outcome measurement, the majority of trials were judged to have low risk or some concerns. However, we identified 1 trial as having a high risk of bias due to potential “diagnostic detection bias” (Supplemental Material Figure S1).
Network Geometry of Interventions
The network geometry of interventions across each language domain assessed through the WAB is presented in Figures 2A, 3A, 4A, 5A, 6A. As shown in Figure 2A, the trials reporting the WAB AQ contained 7 interventions (7 nodes), contributing to 8 pairs (8 edges) of direct comparisons, with the CCT + SLT and WM + SLT showing the highest number of involved participants except for the SLT control. The network geometry of other language subdomains included spontaneous speech (6 nodes, 5 edges), auditory comprehension (7 nodes, 7 edges), repetition (7 nodes, 7 edges), and naming (7 nodes, 7 edges).
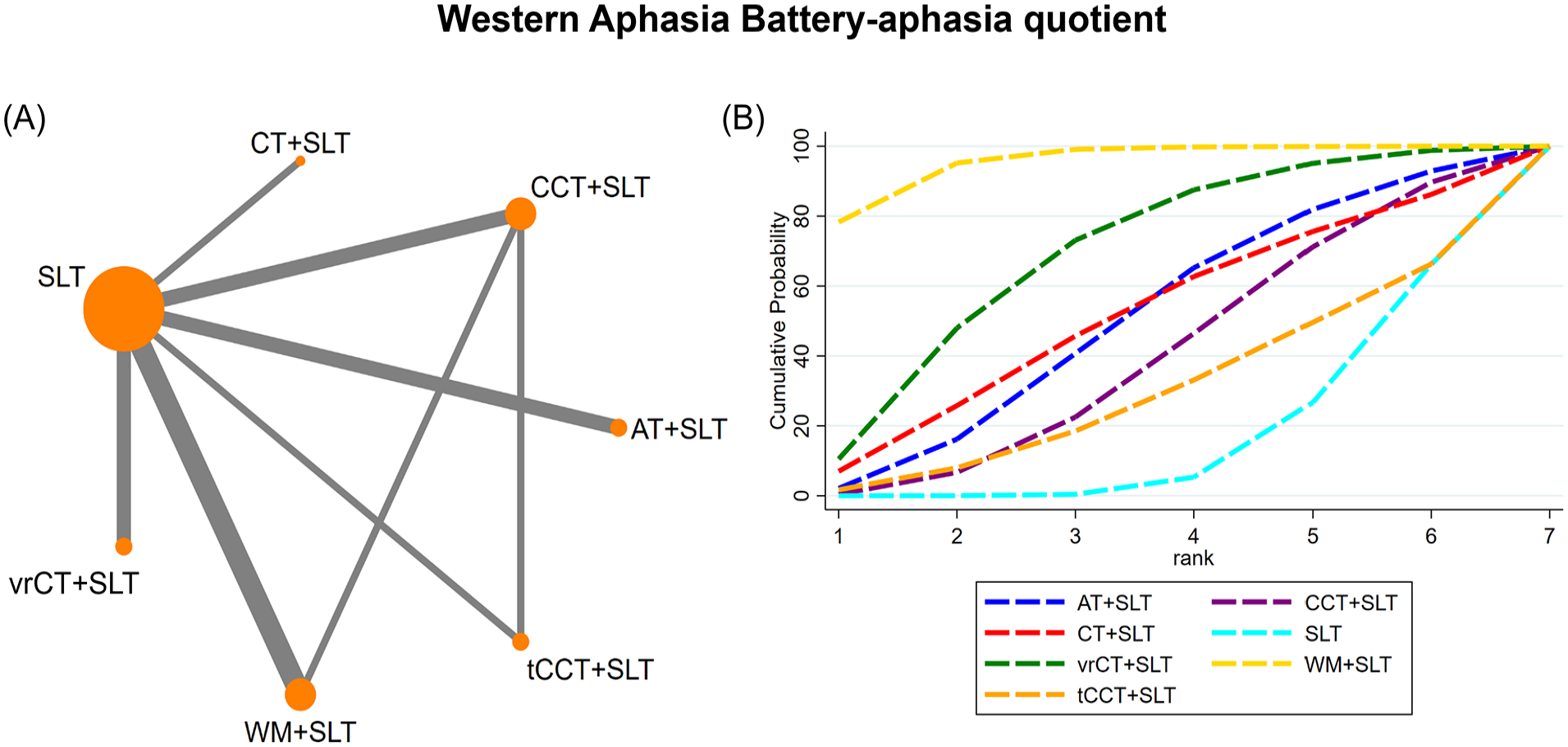
(A) NMA figure for Western Aphasia Battery AQ. (B) SUCRA plot for Western Aphasia Battery AQ.
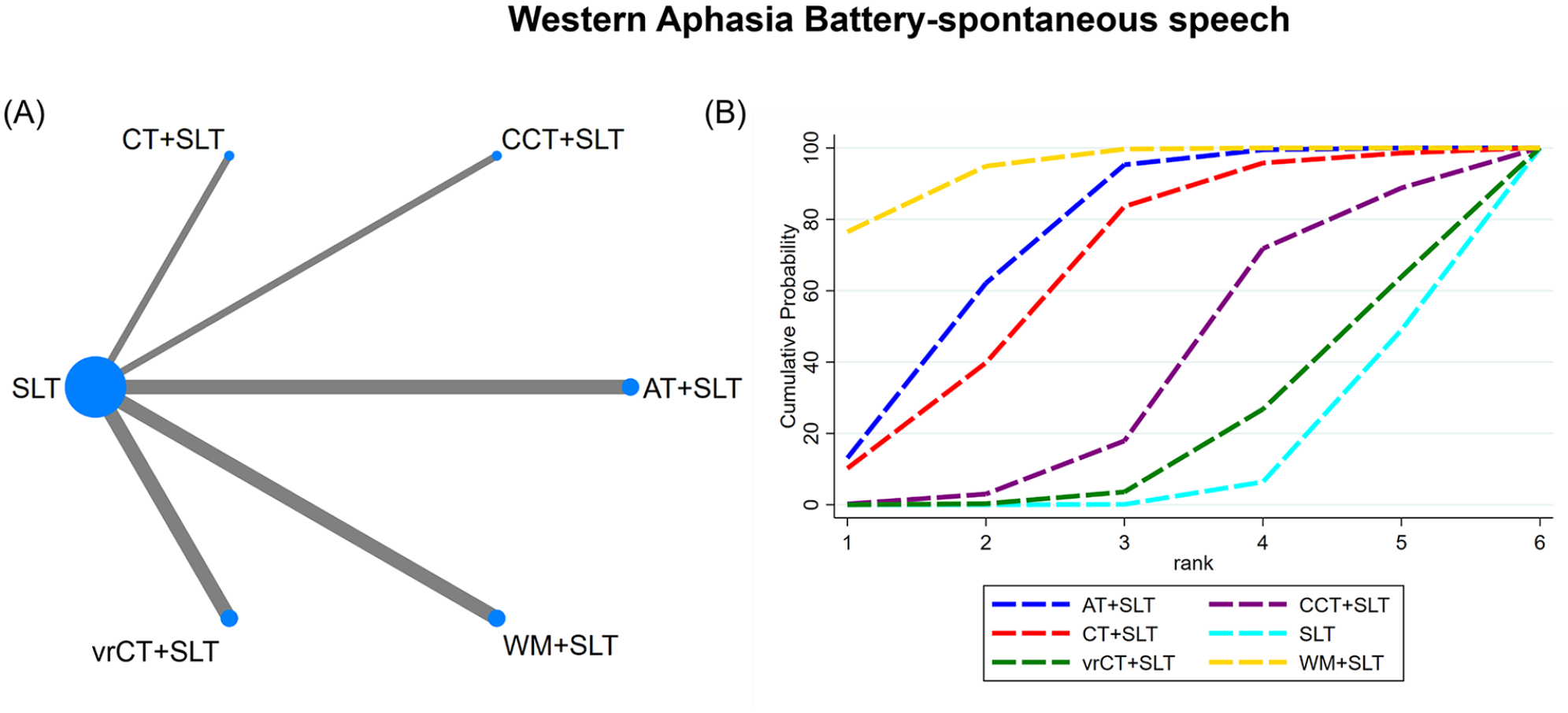
(A) NMA figure for Western Aphasia Battery spontaneous speech score. (B) SUCRA plot for Western Aphasia Battery spontaneous speech score.
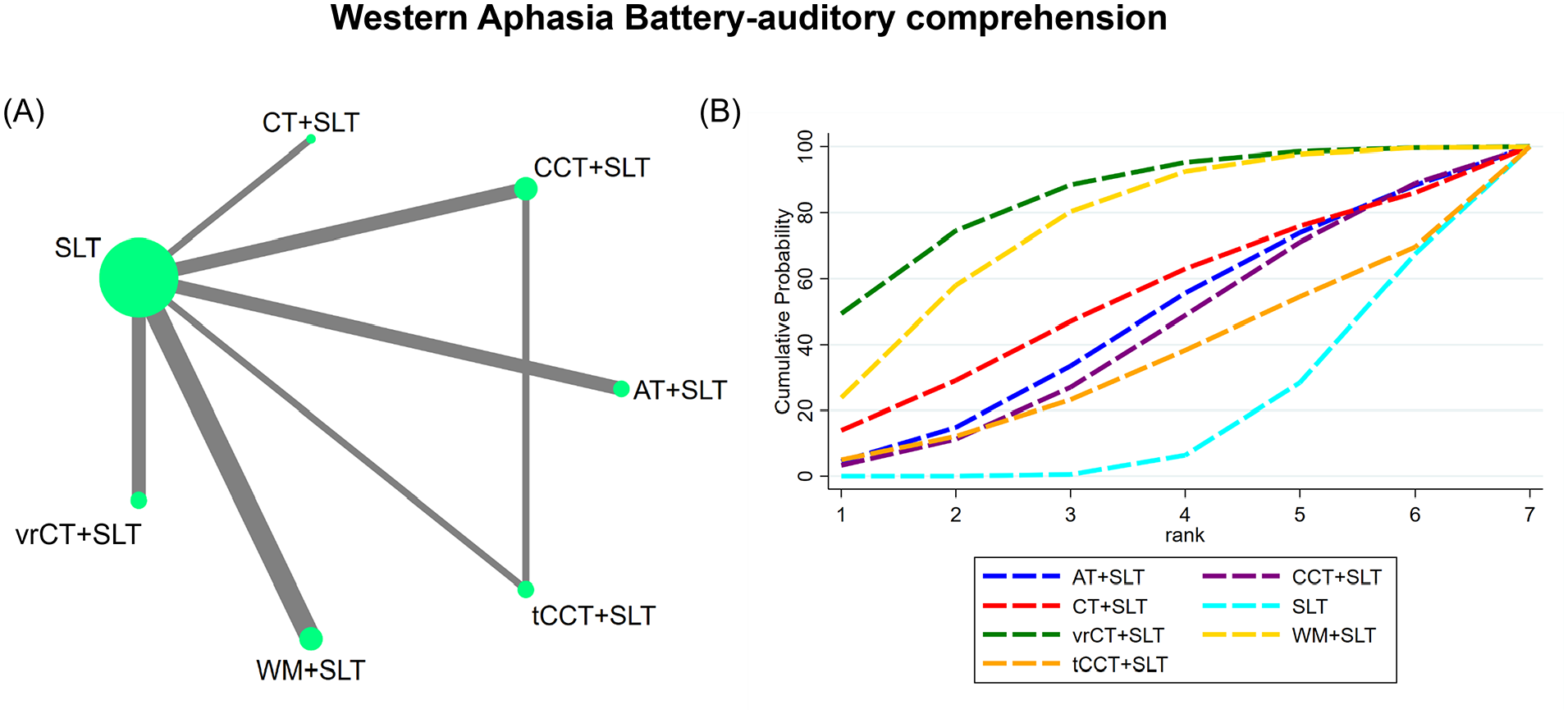
(A) NMA figure for Western Aphasia Battery auditory comprehension score. (B) SUCRA plot for Western Aphasia Battery auditory comprehension score.
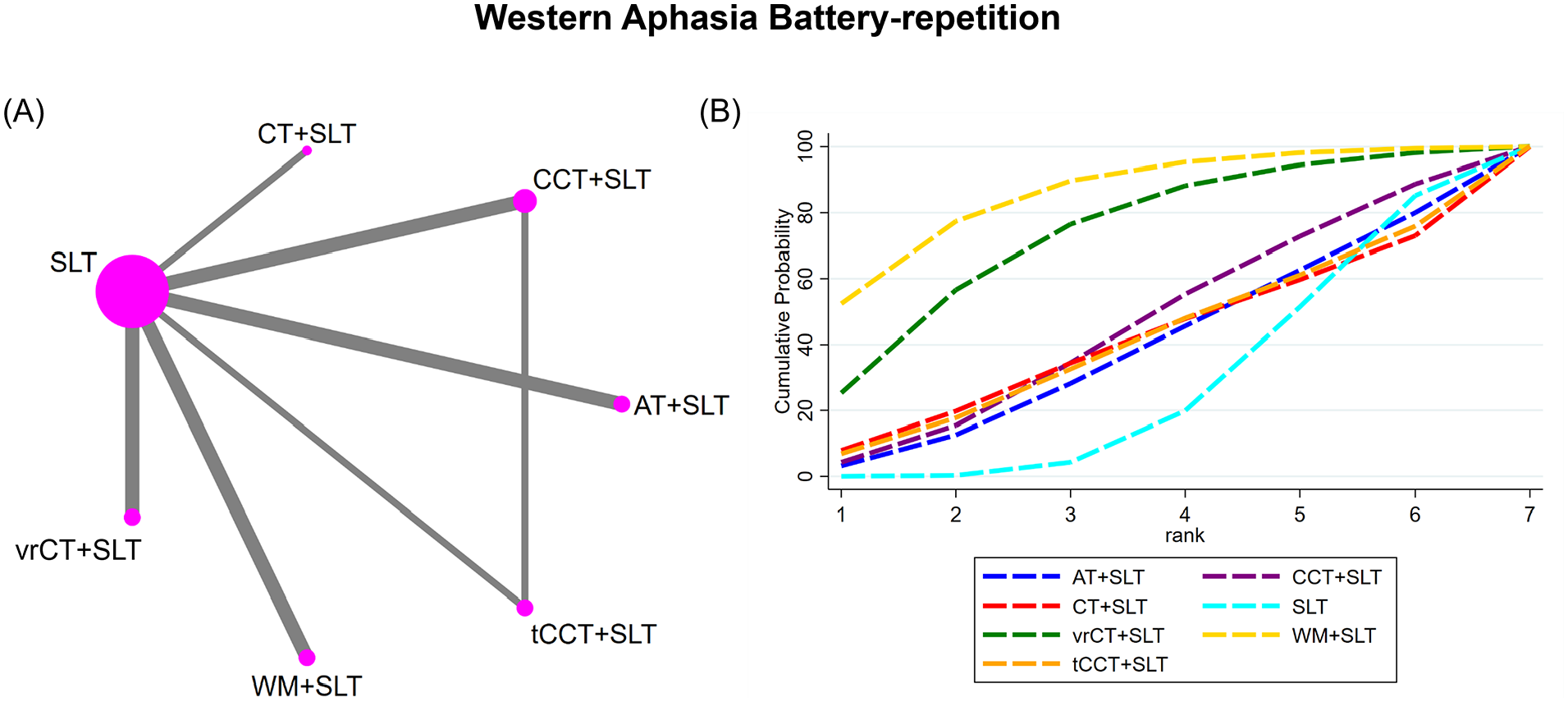
(A) NMA figure for Western Aphasia Battery repetition score. (B) SUCRA plot for Western Aphasia Battery repetition score.
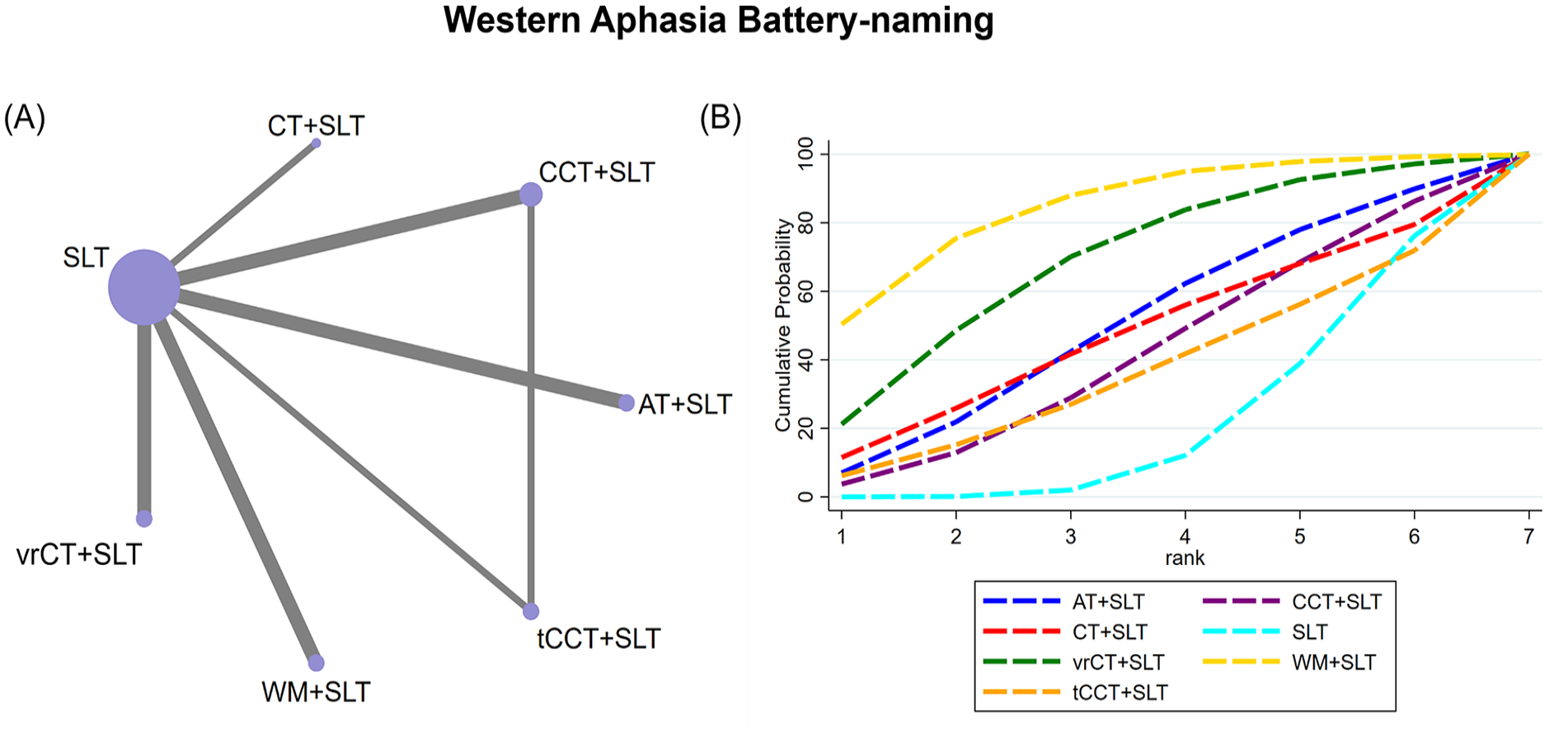
(A) NMA figure for Western Aphasia Battery naming score. (B) SUCRA plot for Western Aphasia Battery naming score.
Effect of Different Interventions on the WAB AQ
A total of 11 RCTs reported the efficacy of cognitive training on the WAB AQ in individuals with PSA, including 7 treatment regimens. By employing both the global inconsistency test and node splitting assessment (Supplemental Material Figure S2), we found no significant inconsistency between direct and indirect comparisons (
Our NMA results demonstrated that, compared to CCT + SLT, the WM + SLT intervention was more effective in improving the AQ (SMD = 1.55, 95% CI = 0.29-2.80). Similarly, in comparison to tCCT + SLT, WM + SLT yielded better results in improving the AQ (SMD = 1.79, 95% CI = 0.07-3.52). Furthermore, when compared to the SLT control group, the WM + SLT intervention showed significantly greater improvement in the AQ than the other treatment approaches (SMD = 1.94, 95% CI = 1.06-2.82), as provided in Table 2.
Network Meta-analysis Results of the WAB AQ.
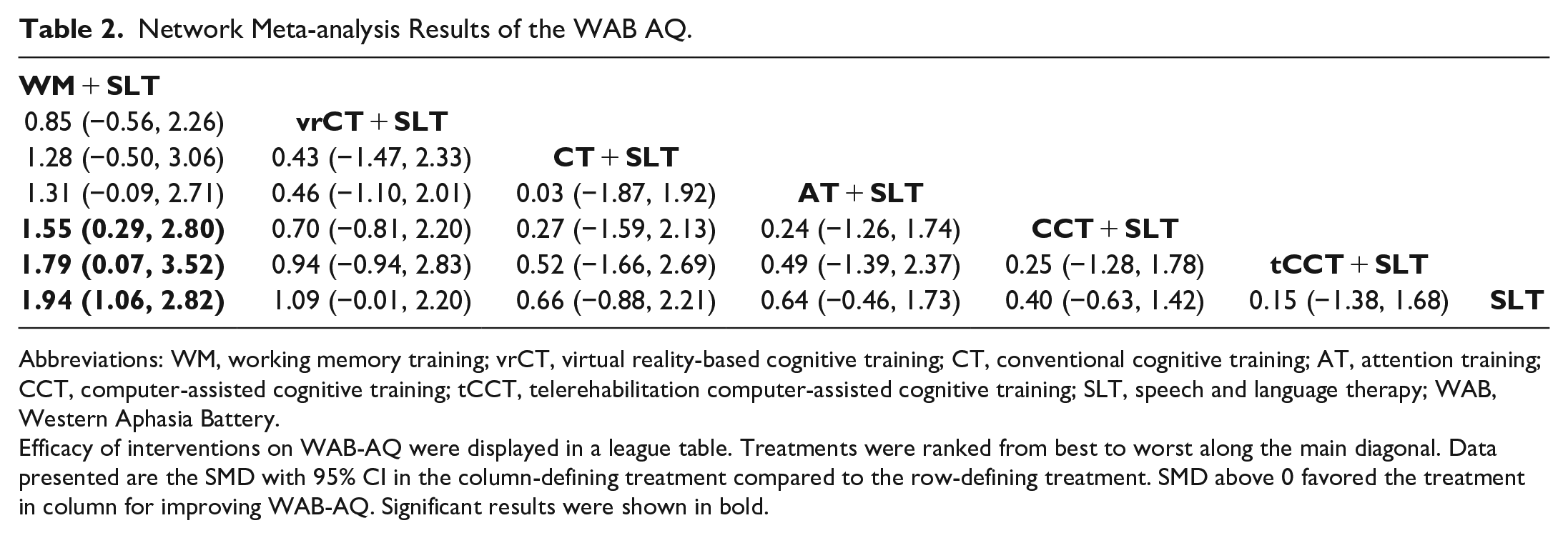
Abbreviations: WM, working memory training; vrCT, virtual reality-based cognitive training; CT, conventional cognitive training; AT, attention training; CCT, computer-assisted cognitive training; tCCT, telerehabilitation computer-assisted cognitive training; SLT, speech and language therapy; WAB, Western Aphasia Battery.
Efficacy of interventions on WAB-AQ were displayed in a league table. Treatments were ranked from best to worst along the main diagonal. Data presented are the SMD with 95% CI in the column-defining treatment compared to the row-defining treatment. SMD above 0 favored the treatment in column for improving WAB-AQ. Significant results were shown in bold.
Moreover, our SUCRA analysis indicated that the WM + SLT intervention presented the highest probability of being the most effective strategy in improving the AQ (SUCRA: 95.4%), followed by vrCT + SLT, CT + SLT, AT + SLT, CCT + SLT, tCCT + SLT, and finally the SLT (Figure 2B).
Effect of Different Interventions on the WAB Spontaneous Speech Score
A total of 8 RCTs evaluated the efficacy of cognitive training on the spontaneous speech score of the WAB in individuals with PSA, encompassing 6 treatment regimens. Assessments for both global and local inconsistency were not performed due to a lack of sources for inconsistency; all data were derived from direct comparisons.
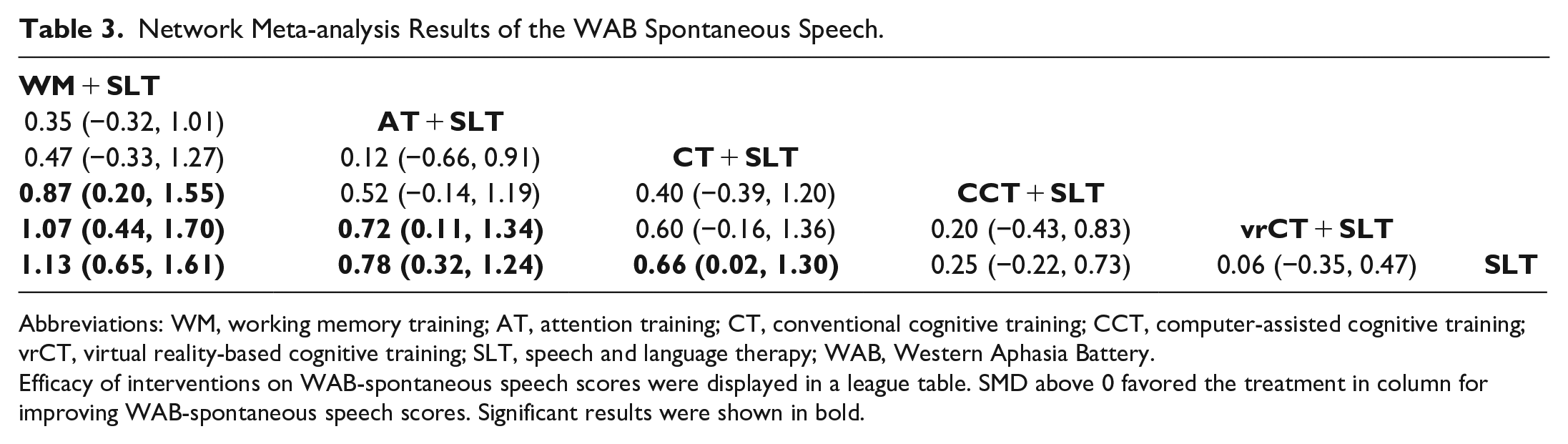
According to our NMA results, the WM + SLT intervention resulted in better spontaneous speech score compared to CCT + SLT (SMD = 0.87, 95% CI = 0.20-1.55) and vrCT + SLT (SMD = 1.07, 95% CI = 0.44-1.70). Similarly, AT + SLT showed superior efficacy in improving the spontaneous speech score compared to vrCT + SLT (SMD = 0.72, 95% CI = 0.11-1.34). Furthermore, compared to the SLT control group, WM + SLT intervention led to a significantly greater improvement in spontaneous speech scores (SMD = 1.13, 95% CI = 0.65-1.61), as did AT + SLT (SMD = 0.78, 95% CI = 0.32-1.24) and CT + SLT (SMD = 0.66, 95% CI = 0.02-1.30; Table 3). Moreover, our SUCRA analysis indicated that the WM + SLT intervention presented the highest probability of being the most effective strategy in improving the spontaneous speech score (SUCRA: 94.2%), followed closely by AT + SLT, CT + SLT, CCT + SLT, vrCT + SLT, and SLT (Figure 3B).
Network Meta-analysis Results of the WAB Spontaneous Speech.
Abbreviations: WM, working memory training; AT, attention training; CT, conventional cognitive training; CCT, computer-assisted cognitive training; vrCT, virtual reality-based cognitive training; SLT, speech and language therapy; WAB, Western Aphasia Battery.
Efficacy of interventions on WAB-spontaneous speech scores were displayed in a league table. SMD above 0 favored the treatment in column for improving WAB-spontaneous speech scores. Significant results were shown in bold.
Effect of Different Interventions on the WAB Auditory Comprehension Score
A total of 10 RCTs evaluated the efficacy of cognitive training on the auditory comprehension score of the WAB in individuals with PSA, including seven treatment approaches. Both the global inconsistency test and node splitting assessment (see Supplemental Material Figure S3) demonstrated no significant inconsistency between direct and indirect comparisons (
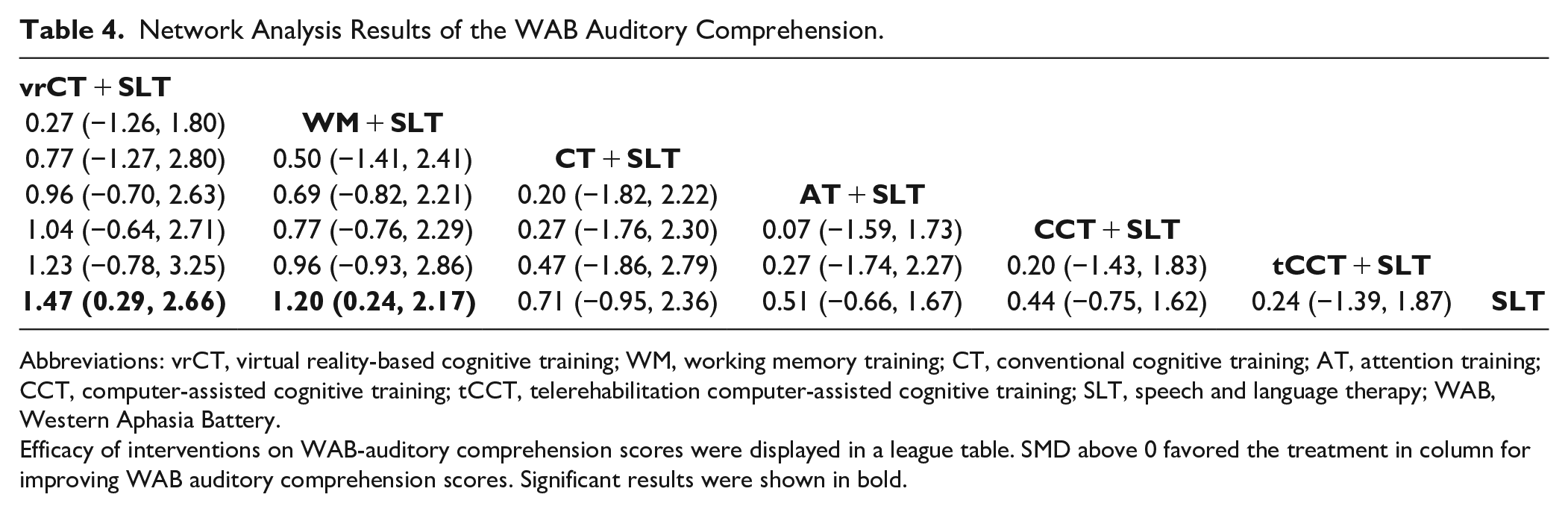
Our NMA results demonstrated that compared to the SLT control group, vrCT + SLT intervention demonstrated a significantly greater improvement in the auditory comprehension score (SMD = 1.47, 95% CI = 0.29-2.66), as did WM + SLT (SMD = 1.20, 95% CI = 0.24-2.17; Table 4). Moreover, our SUCRA analysis indicated that the vrCT + SLT intervention presented the highest probability of being the most effective strategy in improving the auditory comprehension score (SUCRA: 84.3%), followed marginally by WM + SLT, CT + SLT, AL + SLT, CCT + SLT, tCCT + SLT, and SLT (Figure 4B).
Network Analysis Results of the WAB Auditory Comprehension.
Abbreviations: vrCT, virtual reality-based cognitive training; WM, working memory training; CT, conventional cognitive training; AT, attention training; CCT, computer-assisted cognitive training; tCCT, telerehabilitation computer-assisted cognitive training; SLT, speech and language therapy; WAB, Western Aphasia Battery.
Efficacy of interventions on WAB-auditory comprehension scores were displayed in a league table. SMD above 0 favored the treatment in column for improving WAB auditory comprehension scores. Significant results were shown in bold.
Effect of Different Interventions on the WAB Repetition Score
A total of 9 RCTs reported the efficacy of cognitive training on the repetition score of the WAB in individuals with PSA, including 6 treatment approaches. Both the global inconsistency test and node splitting assessment (Supplemental Material Figure S4) revealed no significant inconsistency between direct and indirect comparisons (
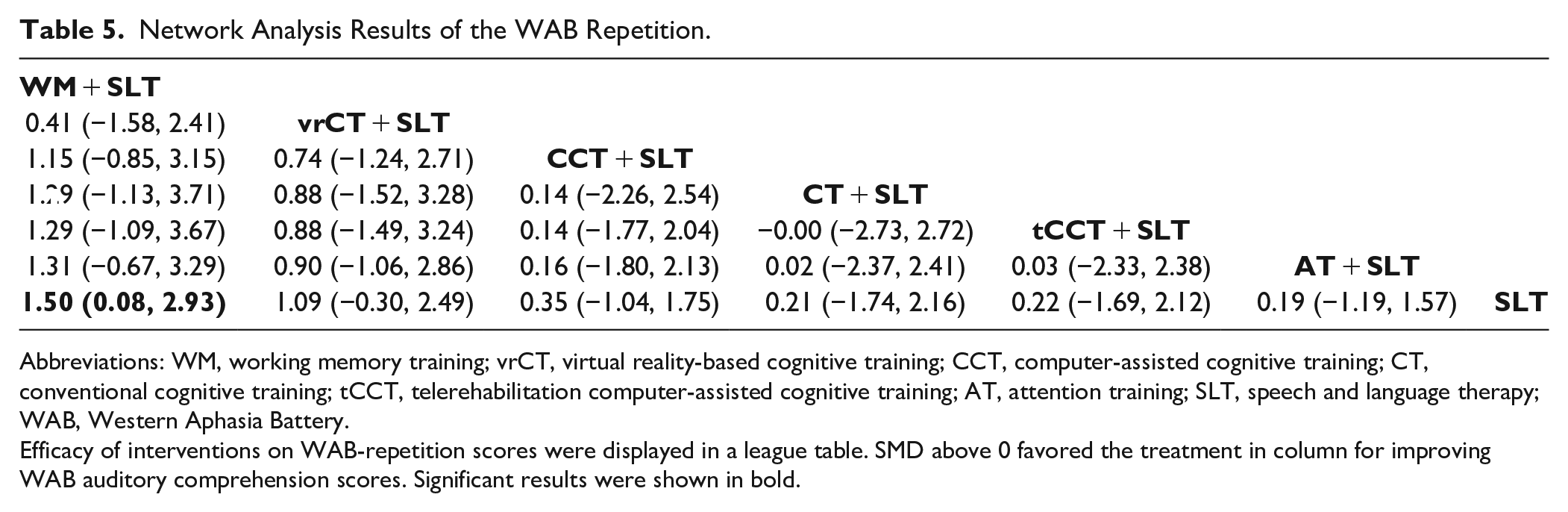
In our NMA results, the WM + SLT intervention led to superior improvements in repetition scores compared to SLT (SMD = 1.50, 95% CI = 0.08-2.93). No significant differences were observed among the other treatment approaches (Table 5). Moreover, our SUCRA analysis indicated that the WM + SLT intervention presented the highest probability of being the most effective strategy in improving the repetition score (SUCRA: 85.5%), followed by vrCT + SLT, CCT + SLT, CT + SLT, AT + SLT, and SLT (Figure 5B).
Network Analysis Results of the WAB Repetition.
Abbreviations: WM, working memory training; vrCT, virtual reality-based cognitive training; CCT, computer-assisted cognitive training; CT, conventional cognitive training; tCCT, telerehabilitation computer-assisted cognitive training; AT, attention training; SLT, speech and language therapy; WAB, Western Aphasia Battery.
Efficacy of interventions on WAB-repetition scores were displayed in a league table. SMD above 0 favored the treatment in column for improving WAB auditory comprehension scores. Significant results were shown in bold.
Effect of Different Interventions on the WAB Naming Score
A total of 9 RCTs evaluated the efficacy of cognitive training on the naming score of the WAB in individuals with PSA, including 7 treatment approaches. The global inconsistency test and node splitting assessment (Supplemental Material Figure S5) provided evidence of no significant inconsistency between direct and indirect comparisons (
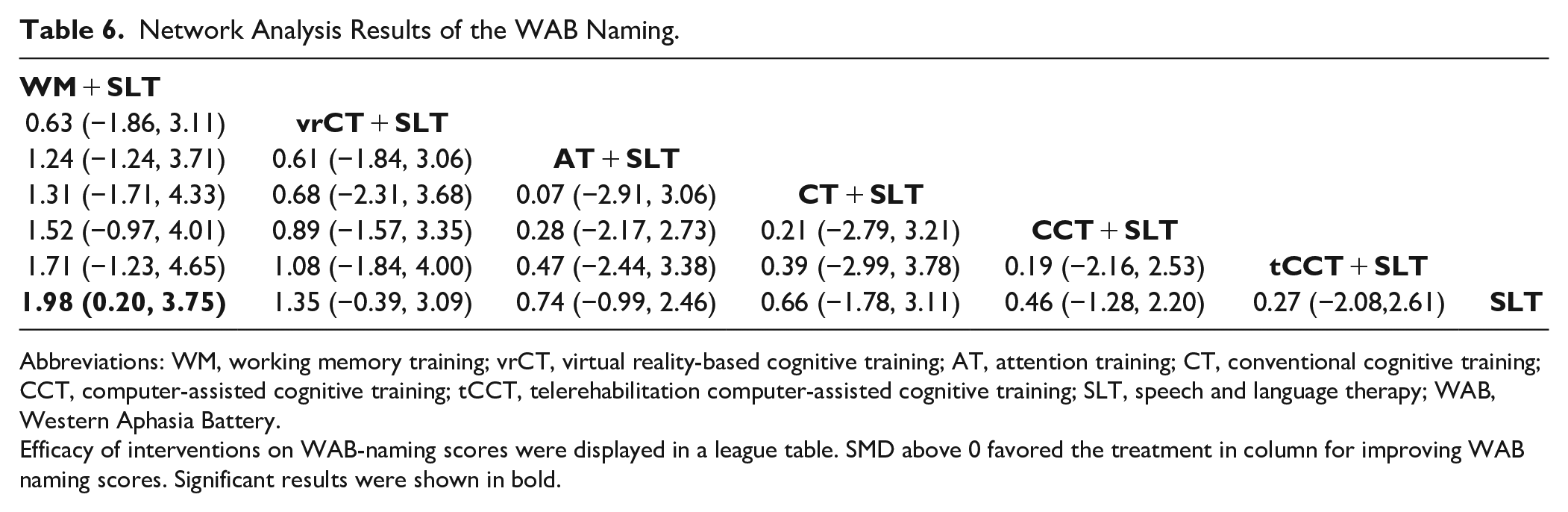
Based on our NMA results, the WM + SLT intervention was found to be more effective in improving the naming score compared to SLT alone (SMD = 1.98, 95% CI = 0.20-3.75). No significant differences were observed among the other treatment approaches (Table 6). Moreover, our SUCRA analysis indicated that the WM + SLT intervention presented the highest probability of being the most effective strategy in improving the naming score (SUCRA: 84.4%), followed closely by vrCT + SLT, AT + SLT, CT + SLT, CCT + SLT, tCCT, and SLT (Figure 6B).
Network Analysis Results of the WAB Naming.
Abbreviations: WM, working memory training; vrCT, virtual reality-based cognitive training; AT, attention training; CT, conventional cognitive training; CCT, computer-assisted cognitive training; tCCT, telerehabilitation computer-assisted cognitive training; SLT, speech and language therapy; WAB, Western Aphasia Battery.
Efficacy of interventions on WAB-naming scores were displayed in a league table. SMD above 0 favored the treatment in column for improving WAB naming scores. Significant results were shown in bold.
Publication Bias and Data Consistency
Separate funnel plots were constructed for all outcome indicators to assess potential publication bias. As shown in Supplemental Figure S6, the points within the funnel plot are symmetrically distributed between the funnel borders, suggesting minimal publication bias. Results from Egger’s tests further support this, revealing insignificant publication bias in the WAB AQ as well as in all language domains, including spontaneous speech, auditory comprehension, repetition, and naming (
Discussion
In this study, we conducted an NMA to assess and compare the efficacy of various cognitive training modalities—specifically WM, AT, CT, CCT, tCCT, vrCT—when combined with SLT for individuals with PSA. Our results demonstrated the superiority of these specific modalities combined with SLT over SLT alone in treating PSA. Notably, WM training combined with SLT led to significant improvements in WAB AQ, WAB spontaneous speech, WAB repetition, and WAB naming scores, compared to SLT alone. This combination was more effective than both CCT with SLT and tCCT with SLT in improving WAB AQ. Furthermore, it was more effective than both CCT with SLT and vrCT with SLT in enhancing WAB spontaneous speech. Additionally, both vrCT and WM training combined with SLT proved to be the most effective approach for improving WAB auditory comprehension, as compared to SLT alone.
WM Training for PSA
WM has been conceptualized as a system designed for short-term information maintenance, processing, and manipulation. 42 Numerous studies have demonstrated that PSA is frequently accompanied by WM impairment, which further compromises the PSA recovery process. 43 The WM impairments in PSA include interference control within the linguistic system, phonological and semantic control, serial order information storage, and attentional and executive control. 44 Furthermore, PSA-associated WM deficits typically involve selective WM components, suggesting a component- and process-oriented WM strategy for PSA treatment.
Recent studies have demonstrated the potential of WM training for improving both WM (near transfer effect) and language function, such as spoken sentence comprehension and functional communication (far transfer effect), in individuals with PSA.18,44 Consistent with this, our findings indicated that WM training combined with SLT contributes to ameliorating overall aphasia severity and improving spontaneous speech, repetition, and naming function in PSA. The methodologies employed for WM training in the studies included primarily used N-back tasks to target the storage and processing components of WM and the Corsi Block-Tapping Task (CBTT) to focus on the visuospatial components of WM.38,39
WM training for PSA typically utilizes the N-back task, a well-established paradigm in which participants determine if a given stimulus matches the 1 presented in N trials earlier. 45 While often regarded as a measure of WM updating, the N-back task also assesses active maintenance, WM capacity, and interference control when lure stimuli are introduced into the sequence.46,47 Another widely used approach for visuospatial WM training is the CBTT, in which participants are tasked with memorizing a sequence of spatially presented blocks in ascending order of complexity.48,49 Although our findings indicate that WM training holds promise for enhancing the language functions in PSA, the existing research in this area remains limited. To evaluate the overall effects of WM training for PSA, our study included different types of WM strategies, primarily N-back and CBTT. However, further investigation is required to determine the optimal WM strategy selection tailored to individuals with specific types of PSA.
Previous studies have shown the effects of WM training on behavioral performance and neural systems.50,51 Changes in neural plasticity, involving intrinsic brain activity, as well as alterations in gray and white matter structures and dopamine D1 receptor density in prefrontal and posterior parietal regions, have been demonstrated following training.50,52-54 However, the neural mechanisms underlying the effectiveness of WM training in PSA remain unclear, necessitating further investigation, especially in terms of the transfer effects. 55
VR-Based Cognitive Training for PSA
In recent years, VR technology has emerged as a promising tool in the rehabilitation of PSA, offering a computer-generated, semi-immersive environment for language practice in real communication contexts. 56 Despite the fact that VR interventions have demonstrated substantial benefits in stroke rehabilitation, 57 their application in PSA remains relatively elusive. Recent literature highlights the innovative potential of VR for language rehabilitation,20,22,56 particularly within an embodied cognition framework. 58 These studies demonstrate VR’s ability to create immersive and engaging environments, increase treatment intensity, enhance sensorimotor stimulation, reduce social stigma, and improve the ecological validity of PSA therapy.
A recent meta-analysis 59 suggested that variations in treatment outcomes correlate with the frequency, intensity, and dosage of SLT. Specifically, this study suggests that the most significant improvements in overall language and auditory comprehension were observed with higher dosages, exceeding 20 to 50 hours of SLT or more. However, achieving these higher dosage levels within existing resources can be challenging, necessitating innovative delivery models. Thus, VR training emerges as a potential solution, as it not only enables home-based practice but also addresses accessibility issues for patients who live far from rehabilitation centers or have motor impairments.
In line with prior research, our study demonstrates that the combination of vrCT and SLT enhances auditory comprehension function in PSA. Notably, 1 study in our analysis employed an advanced VR setup, comprising a mobile trolley, playback devices, three-dimensional (3D) playback software, 3D glasses, and earplugs, 36 while training material was based on the embodied cognitive rehabilitation system (E-core). 60 Another investigation utilized a tablet equipped with the constant therapy-research (CT-R) software, featuring an extensive library of over 100,000 stimuli across more than 350 difficulty levels in 9 distinct cognitive, speech, and language domains.61,62
To date, a limited number of studies have investigated the mechanisms underlying the efficacy of vrCT for PSA. Previous investigations of healthy individuals found that virtual actions can elicit motor simulation and influence language processing. This suggests the possibility of a simulation-driven mechanism induced by VR training, which could influence language performance. 63 Therefore, we speculate that vrCT may follow a similar mechanism. However, further research is needed to establish a concrete link between the cognitive representations triggered by virtual experiences and their roles in language recovery. Recent reviews have also highlighted the importance of exploring the roles of immersion and presence as promising avenues for understanding the underlying mechanisms of VR therapy in PSA rehabilitation. 20
Limitations and Future Directions
Our study has several limitations that warrant discussion. First, cognitive treatment includes a wide range of interventions, leading to variability in the interpretation of treatment effects across studies. This variability stems from the lack of uniform categorization, with different studies targeting various cognitive constructs such as attention, working memory, or executive function, which makes generalization challenging. Second, some of the included studies lacked specific information on random sequence generation and allocation concealment methods, introducing the possibility of bias. Moreover, given the inherent nature of cognitive training and SLT, participants and intervention providers were often aware of the assigned interventions, potentially leading to deviations from the intended interventions. Third, the clinical heterogeneity observed may be attributed to variations in treatment duration, intensity, frequency, and the diversity of cognitive training programs used among the included studies. Due to the limited number of available studies, we could not conduct subgroup analyses to account for these variables. Future research with access to larger datasets may find it useful to employ meta-regression analysis to better account for these potential moderators and refine rehabilitation strategies. Another limitation lies in the assessment tools used in the included studies; they primarily utilized the WAB scale, focusing specifically on the AQ and 4 language subdomain functions, thus limiting the scope of our analysis.
Future research would benefit from conducting more standardized RCTs with larger sample sizes and multicenter involvement. This would strengthen the evidence base for integrating cognitive training into traditional SLT for PSA. Furthermore, it is important to differentiate between the cognitive constructs addressed by the treatment—such as attention, working memory, executive function—and their delivery methods, including in-person, computer-assisted, and virtual reality approaches. Additionally, exploring personalized cognitive training protocols that target specific cognitive components and sub-components of functions such as working memory (eg, central executive, phonological, and visuospatial) in the context of PSA, is warranted. While our findings underscore the effectiveness of WM training and vrCT combined with SLT in improving language abilities, alternative cognitive training approaches tailored to individual needs should be considered for incorporation into existing PSA language rehabilitation strategies.
Conclusions
In summary, our NMA underscores the substantial potential of cognitive training, specifically WM combined with SLT and vrCT combined with SLT interventions, for significantly improving language function in individuals with PSA. These findings indicate a promising avenue for enhancing PSA management and offer crucial guidance for clinicians and researchers working to optimize therapeutic options for this population.
Supplemental Material
sj-docx-1-nnr-10.1177_15459683241274755 – Supplemental material for Comparative Efficacy of Cognitive Training for Post-Stroke Aphasia: A Systematic Review and Network Meta-Analysis
Supplemental material, sj-docx-1-nnr-10.1177_15459683241274755 for Comparative Efficacy of Cognitive Training for Post-Stroke Aphasia: A Systematic Review and Network Meta-Analysis by Qiao Kong, Jiaqi Wang, Xing Huang, Junyi He and Jingling Chang in Neurorehabilitation and Neural Repair
Footnotes
Author Contributions
Qiao Kong: Conceptualization; Data curation; Formal analysis; Investigation; Methodology; Software; Writing—original draft. Jiaqi Wang: Investigation; Methodology; Writing—review & editing. Xing Huang: Investigation; Writing—review & editing. Junyi He: Investigation; Writing—review & editing. Jingling Chang: Conceptualization; Supervision; Writing—review & editing.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the National Natural Science Foundation of China (grant number 81973790), National Administration of Traditional Chinese Medicine, International Cooperation Department for Traditional Chinese Medicine, Base-Type Project of the Special Project of International Cooperation in Traditional Chinese Medicine (0610-2240NF021548), and Beijing University of Chinese Medicine Dongzhimen Hospital Clinical Research and Achievement Transformation Capacity Enhancement Pilot Project (DZMG-XZYY-23008).
Supplementary material for this article is available on the
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
