Abstract
Keywords
Introduction
The 21-item Wolf Motor Function Test (WMFT) was originally developed to assess the effects of constraint-induced movement therapy on the return of upper extremity (UE) movement ability in stroke survivors. 1 It was subsequently modified and contains 17 tasks, including 2 strength-based tasks and 15 function-based tasks, divided into 2 scales: performance time and functional ability. 2 The reliability and validity of the WMFT have been well established in previous studies. The WMFT had good test-retest reliability 2,3 and criterion validity 3,4 for performance time and functional ability. In addition, interrater reliability of the WMFT was high (range, 0.97-0.99). 5 This test has been widely used as an outcome measure in stroke motor rehabilitation trials. 6-10
Owing to lengthy administration times, the WMFT was further shortened to 6 tasks in a recent study. 11 Although the 6 tasks of the streamlined WMFT had a significant relationship with overall improvement in the Extremity Constraint Induced Therapy Evaluation (EXCITE) trial, 11 no study to date has reported the sensitivity of change of this shortened version. To be of practical use in rehabilitation trials, the short form of an outcome measure should not only show reliability and validity but also be sensitive in measuring change within persons over time. 12 That is, the demonstration of sound clinimetric properties of an outcome measure is a priority before its application in clinical trials or in the evaluation of the effects of rehabilitation therapies. 13,14
Because the streamlined WMFT has not been sufficiently validated, the responsiveness and criterion validity of the short form of the WMFT remain unknown. To address the gap, we evaluated the clinimetric properties of the streamlined WMFT in a stroke cohort other than the sample studied in the EXCITE trial. Responsiveness indicates an instrument’s ability to detect the smallest change in score. 15 Furthermore, responsiveness is neither a constant statistic nor a context-free attribute. 16 In other words, responsiveness of an instrument should be described in relation to a particular group of people under certain conditions. Lin et al 3 studied the responsiveness of the WMFT during the recovery course of the first 6 months after stroke, but no rehabilitation therapy was specified for the change in WMFT. This study evaluated the responsiveness of the streamlined WMFT in patients with subacute stroke, defined as 3 to 9 months poststroke in the Bogard et al study, 11 who had undergone rehabilitation therapies.
As suggested by Bogard et al, 11 this study also examined the criterion validity of the streamlined WMFT. Criterion validity includes concurrent validity and predictive validity, which considers the degree of consistency of an instrument with the criterion measures and the ability of an instrument to predict future events. 17 The examination of the concurrent validity of the streamlined WMFT enables researchers to determine if this streamlined version measures the same construct as is assessed by the 17-item WMFT. The streamlined WMFT may be taken as an important tool for guiding clinical decision making for rehabilitation goal planning if it shows a level of predictive validity similar to that of the 17-item WMFT.
The purpose of the present study was therefore to examine the clinimetric domains of the streamlined WMFT, including the responsiveness and validity (concurrent and predictive validity) in a cohort of subacute stroke patients. Because Bogard et al 11 suggested that the tasks selected for streamlined WMFT depend on the time poststroke (subacute vs chronic), we used the streamlined WMFT with 6 tasks appropriate for subacute patients.
Methods
Participants
The study participants were obtained primarily from those enrolled in one of our previous studies. 18 An additional 10 participants were recruited from the departments of rehabilitation at 3 medical centers. The inclusion criteria were: (1) a first-ever stroke with onset of more than 3 months and less than 10 months; (2) demonstration of Brunnstrom stage III or higher for the proximal part of the affected upper limb 19 ; (3) no serious cognitive deficits, as defined by a score of more than 24 on the Mini Mental-State Exam 20 ; and (4) no excessive spasticity at any joint of the upper limb, as defined by a score of 2 or less on the Modified Ashworth Scale. 21 To eliminate the potential effects of comorbid medical conditions on the study results, we excluded participants with physician-determined major medical problems, such as severe aphasia or a vision problem or those in poor physical condition. Patients were able to understand the meaning of the study and provided written informed consent approved by the ethics committees of the participating sites.
Intervention and Procedure
Patients were randomized to receive 1 of the following 2-hour therapies every weekday for 3 weeks: distributed constraint-induced therapy (CIT), 22 bilateral arm training (BAT), 23 or conventional rehabilitation. 24 The distributed CIT group focused on restriction of movement of the unaffected limb and intensive training of the affected limb. The BAT group concentrated on moving the affected and the unaffected upper limbs simultaneously with functional symmetric tasks. The conventional rehabilitation group focused on neurodevelopment techniques with an emphasis on functional task practice, when possible. The interventions were provided at the participating hospitals under the supervision of 3 certificated occupational therapists. The patients were evaluated at baseline and immediately after 3 weeks of therapy by 3 raters blinded to the participant group. The raters were trained to administer the WMFT.
Measures
The 15 function-based tasks of the WMFT are divided into the performance time scale and the functional ability scale. 25 Because the streamlined WMFT includes 6 timed tasks, 11 only the performance time scale of the WMFT was used to assess UE movement ability in this study. The 6 tasks included hand to table, hand to box, reach and retrieve, lift can, lift pencil, and fold towel. The UE subscale of the Fugl-Meyer Assessment (FMA) 26 is a valid and reliable index measuring motor impairment in stroke patients. 27,28 The Stroke Impact Scale version 3 (SIS 3.0) 29 consists of 59 items measuring the 8 domains of strength, hand function, activities of daily living (ADL)/instrumental ADL (IADL), mobility, communication, emotion, memory/thinking, and participation, with established reliability and validity. 30-32
Data Analysis
Responsiveness
The responsiveness of the streamlined WMFT compared with the WMFT was examined according to changes from pretreatment to posttreatment. Because of the skewed distribution of the original data, a logarithmic transformation was used.
33
The Wilcoxon signed rank test was performed to determine if statistically significant differences in mean change score (MCS) occurred. The standardized response mean (SRM)
34
was estimated as the ratio of the MCS to the standard deviation of the MCS.
35
To classify the values of SRM as nonresponsive (<0.2), small (0.2-0.5), medium (0.5-0.8), and large (>0.8) using the Cohen criteria for effect size
Validity
Concurrent validity was examined by correlating the average score of the timed tasks of the WMFT with the scores of the FMA and those of the SIS hand function subscale by using Spearman rank correlation coefficients (ρ) at baseline and at follow-up. The FMA and SIS hand function were chosen because they and the WMFT measure similar constructs. Predictive validity between the WMFT scores at baseline and the scores on the criterion measures at follow-up was assessed by examining the association with Spearman ρ correlation coefficients. The strengths of the relationship were classified as excellent (ρ > 0.75), good (ρ = 0.5-0.75), fair (ρ = 0.25-0.5), and low (ρ ≤ 0.25). 15
Results
The demographic and clinical characteristics of the participants (50 men, 14 women; mean age, 53.01 years) are summarized in Table 1. The mean scores of the performance time scale at baseline were 7.45 s for the streamlined WMFT and 9.44 s for the WMFT. Results of the clinimetric study of the streamlined WMFT and the WMFT are presented in Tables 2, 3, and 4 to facilitate the comparison and discussion of the measurement properties between the 2 scales.
Baseline Characteristics of the Participants (N = 64)
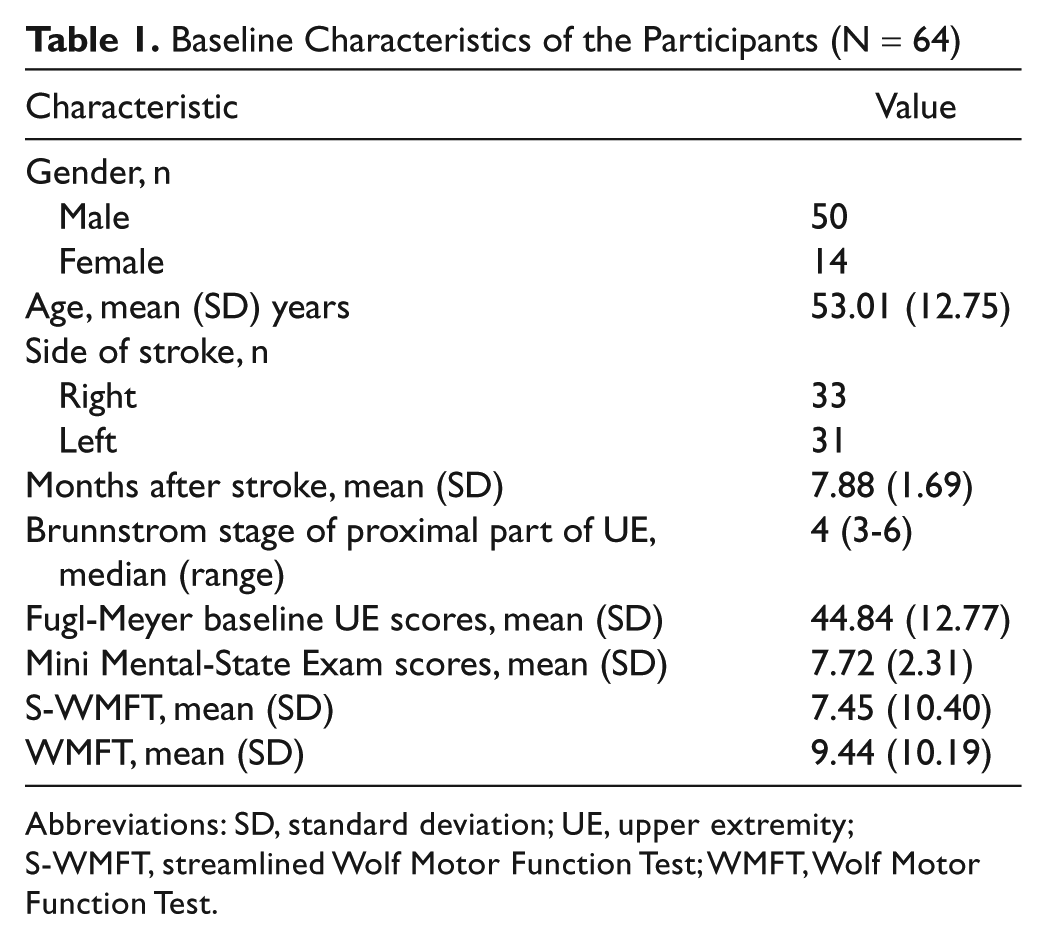
Abbreviations: SD, standard deviation; UE, upper extremity; S-WMFT, streamlined Wolf Motor Function Test; WMFT, Wolf Motor Function Test.
Responsiveness of the S-WMFT and WMFT
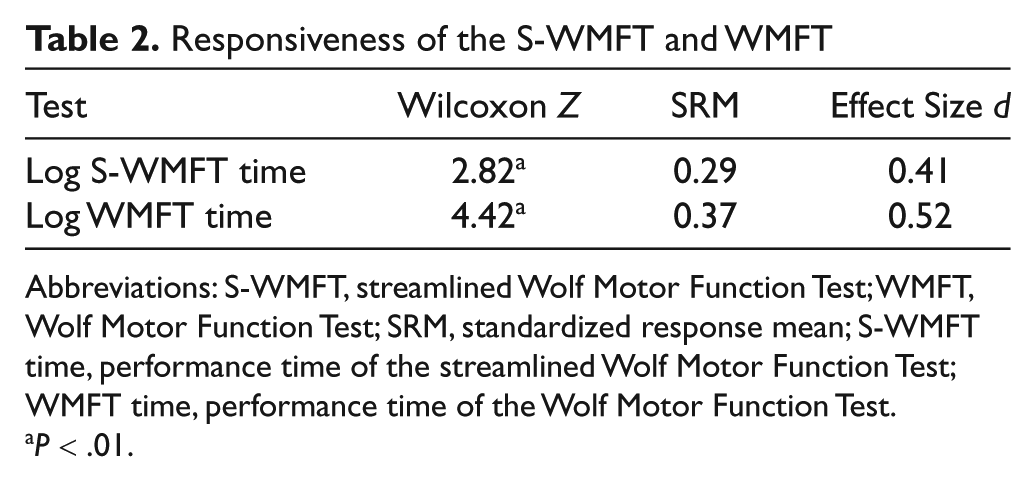

Abbreviations: S-WMFT, streamlined Wolf Motor Function Test; WMFT, Wolf Motor Function Test; SRM, standardized response mean; S-WMFT time, performance time of the streamlined Wolf Motor Function Test; WMFT time, performance time of the Wolf Motor Function Test.
Concurrent Validity of the S-WMFT and WMFT
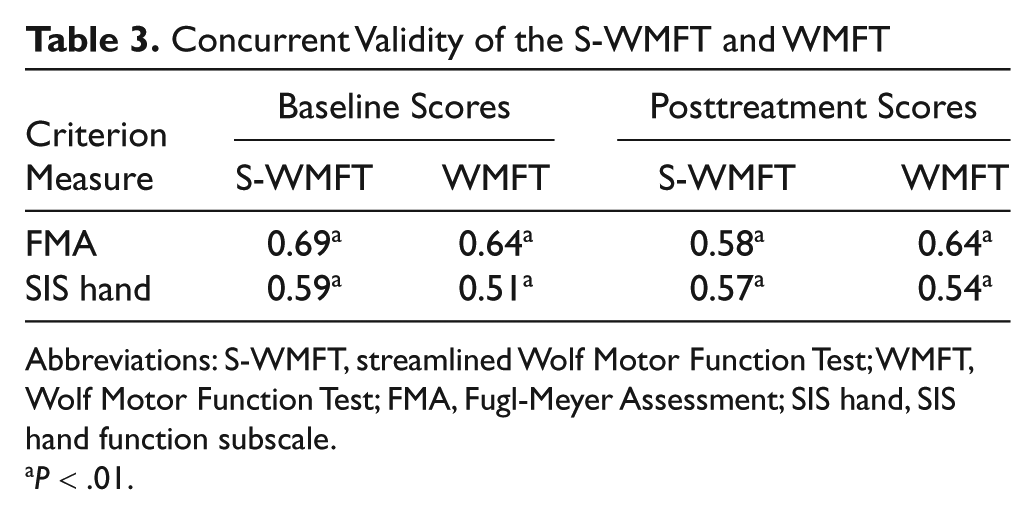
Abbreviations: S-WMFT, streamlined Wolf Motor Function Test; WMFT, Wolf Motor Function Test; FMA, Fugl-Meyer Assessment; SIS hand, SIS hand function subscale.
Predictive Validity of the S-WMFT and WMFT
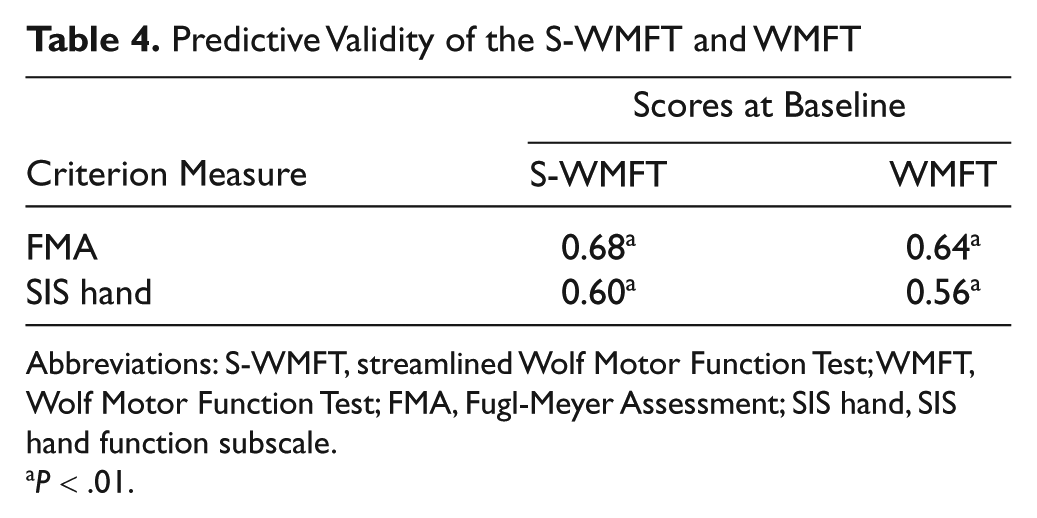
Abbreviations: S-WMFT, streamlined Wolf Motor Function Test; WMFT, Wolf Motor Function Test; FMA, Fugl-Meyer Assessment; SIS hand, SIS hand function subscale.
Responsiveness
The responsiveness indices of the streamlined WMFT and WMFT are listed in Table 2. The pretreatment to posttreatment changes assessed by both tests were significant (
Concurrent Validity
Table 3 shows that the interrelationships of data obtained with the streamlined WMFT, WMFT, FMA, and SIS hand function were ρ ≥ 0.51 (
Predictive Validity
The scores of the streamlined WMFT and WMFT significantly correlated with the scores of FMA and SIS hand function (ρ ≥ 0.56,
Discussion
The present study is the first to systematically assess the clinimetric properties of the streamlined WMFT in participants with subacute stroke. This research extended what Bogard et al 11 reported by showing that the sensitivity to change after rehabilitation therapies for the streamlined WMFT was not significantly different from that for the original version. Furthermore, the criterion validity of the streamlined WMFT was essentially identical to that of the original performance time scale of the WMFT.
Responsiveness is an important quality for any instrument used to evaluate change over time.
15
Responsiveness involves at least 2 aspects: the improvement over time and the magnitude of the change in scores.
39
The time score of the streamlined WMFT improved after rehabilitation (Wilcoxon
The findings on responsiveness of WMFT and streamlined WMFT extend the results of the Bogard et al 11 study on the streamlined WMFT and the Lin et al 3 study on the WMFT in rehabilitation therapy and sample characteristics. Specifically, the participants in the present study received a 3-week therapy of distributed CIT, BAT, or the conventional rehabilitation, whereas those in the EXCITE trial 11 attended a 2-week therapy of standard CIT and those in the Lin et al 3 study might not have attended specific intervention programs. The WMFT and streamlined WMFT tasks that change in response to CIT may also respond to other types of UE training approaches, such as distributed CIT and BAT in our present study. In addition, the participants in this study were different from those in the EXCITE study by Bogard et al, 11 which may increase the applicability and value of the streamlined WMFT.
The validity of an instrument informs researchers about whether the tool evaluates what it is intended to measure. 15 In the present study, the associations between the streamlined WMFT and the FMA as well as the SIS hand function subscale (ρ = 0.57-0.69) were similar to those of the original scale (ρ = 0.51-0.64). These findings lent strong support for the concurrent validity of the streamlined WMFT for assessing UE movement ability in stroke survivors. For predictive validity, our results showed that the correlations between the streamlined WMFT and the criterion measures (ρ = 0.60-0.68) were slightly higher than those of the original scale (ρ = 0.56-0.64), which provides strong evidence to suggest that the streamlined WMFT score is a good predictor of return of UE function after stroke rehabilitation. Taken together, the findings of our study confirm the criterion validity of the streamlined WMFT as an outcome measure for patients with subacute stroke.
The results of the present study need to be considered in light of some limitations. First, only patients with subacute stroke were included, and the results may not be generalizable to other patient populations. Future research needs to address the issue of applicability of the streamlined WMFT in patients with characteristics different from those enrolled in this study and those studied by Bogard et al 11 in order to promote the clinical utility of this assessment tool. Second, because the current findings were derived from a small sample size, more research with larger sample sizes will be required to further examine the clinimetric properties of the streamlined WMFT. Such research may help improve outcome evaluations in stroke patients. Third, because the scores on the streamlined WMFT were extracted from the original scale, further study needs to validate the current clinimetric findings by directly administering the 6-item version of the WMFT to the participants.
Conclusion
The streamlined WMFT demonstrated good criterion validity in patients with subacute stroke. Although the streamlined WMFT was slightly less sensitive than the original performance time scale of the WMFT, no significant difference in sensitivity between the 2 versions was found. Taken together, because the values of the responsiveness of the 2 scales are modest, and the streamlined WMFT has similar concurrent validity and slightly better predictive validity when compared with the original scale, we consider that this 6-item version of the WMFT showed improved clinical utility.
Footnotes
The author(s) declared the following potential conflicts of interest with respect to the authorship and/or publication of this article.
The author(s) received no financial support for the research and/or authorship of this article.
This project was supported in part by the National Science Council (NSC-97-2314-B-182-004-MY3, NSC-97-2811-B-002-101, and NSC-98-2811-B-002-073) and the National Health Research Institutes (NHRI-EX99-9742PI and NHRI-EX99-9920PI) in Taiwan.
