Abstract
A 54-year-old woman with fibromuscular dysplasia presented with pain and discoloration of multiple fingers in her left upper extremity due to undiagnosed subclavian artery stenosis, which was presumed to be the source of distal embolization to the ulnar artery. After index computed tomographic angiography (CTA) and follow-up outpatient angiogram results were inconclusive, an arterial duplex examination was performed. A focal flow velocity increase and changes in arterial pulse Doppler waveforms identified a more proximal arterial stenosis that was missed on CTA and digital subtraction angiography.
Keywords
Case Presentation
A 54-year-old woman with a past medical history of fibromuscular dysplasia (FMD)-associated ischemic strokes, hypertension, and active tobacco use presented to the emergency department with a 2-week history of pain and discoloration of the left second, third, and fifth fingers. An initial computed tomographic angiography (CTA) of the left upper extremity reported the left subclavian (SCA), axillary, and brachial arteries to be well opacified with distal radial and ulnar artery opacification to the thenar eminence and wrist but without distal visualization secondary to contrast timing and sluggish flow. The patient was ultimately discharged with outpatient hand surgery follow-up and elective angiogram. An angiogram was performed which did not demonstrate focal flow-limiting deficits in the distal axillary or brachial arteries but did show diffusely sluggish distal flow in the ulnar artery with a radial dominant palmar arch and limited visualization of the digital arteries due to patient discomfort (Figures 1 and 2).
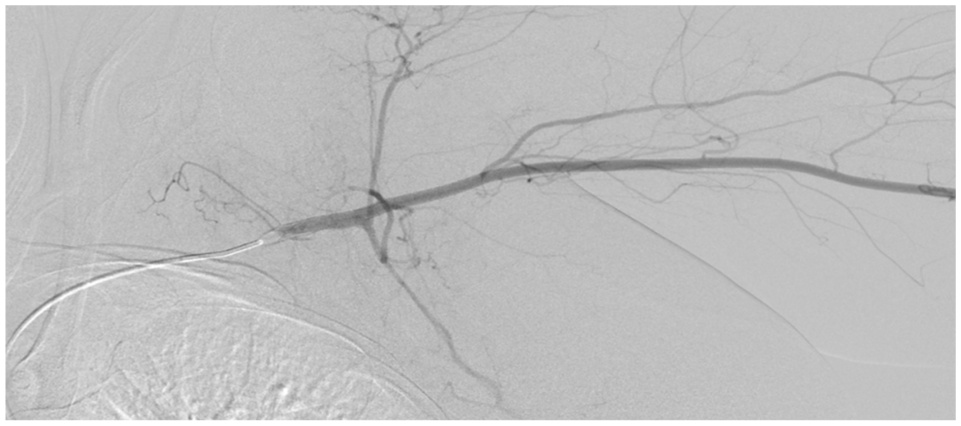
Outpatient angiogram demonstrating patent flow in the axillary and brachial arteries.
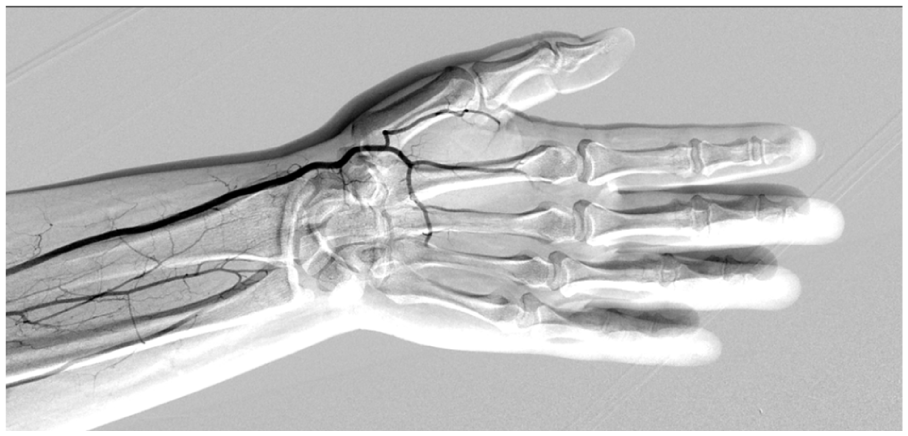
Outpatient angiogram notes that the arteries within the digits were suboptimally visualized due to patient discomfort and patient motion.
Of note, the proximal axillary artery was not assessed and pressure measurements were unavailable. Given her poor flow on angiography, the patient was subsequently thought to have Raynaud’s disease versus hypothenar hammer syndrome and was scheduled for amputation of the fingertips pending the results of photoplethysmography (PPG) waveforms and wrist/brachial indices. The wrist/brachial index examination protocol at our hospital includes duplex images of the distal brachial, distal radial, and distal ulnar arteries as well as blood pressures to calculate the wrist/brachial index. An outpatient duplex ultrasound examination was performed 1 month after the patient’s initial presentation demonstrating monophasic waveforms at the distal radial, ulnar, and brachial arteries (Figure 3) without any hemodynamically significant stenosis, prompting further investigation at the proximal SCA, where peak systolic velocities were found to be elevated at 656 cm/s with greater than 75% stenosis (Figures 4-6).
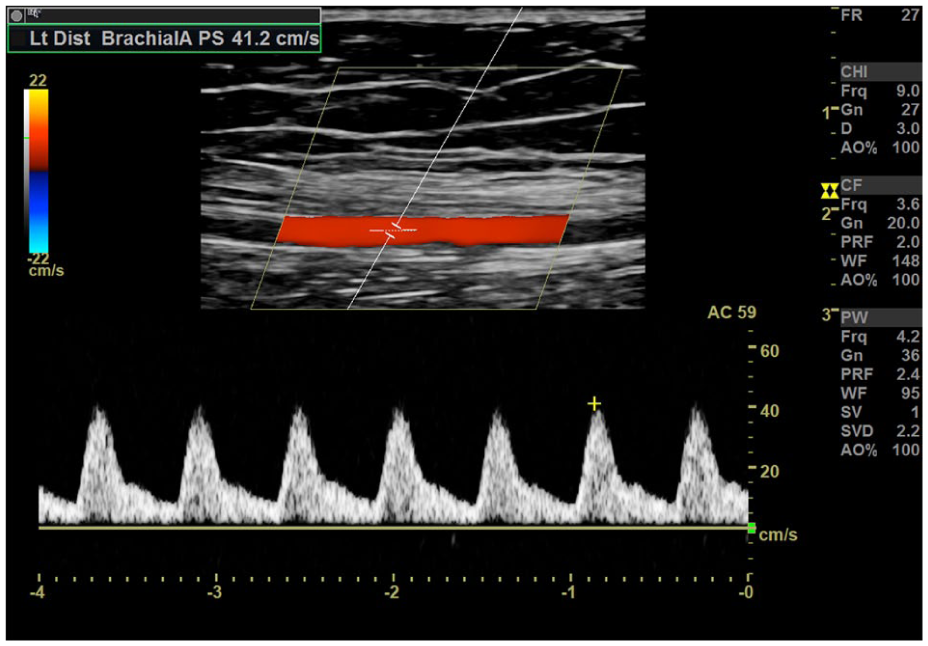
Duplex ultrasound performed 1 month after initial presentation demonstrating monophasic Doppler waveform in the left brachial artery.
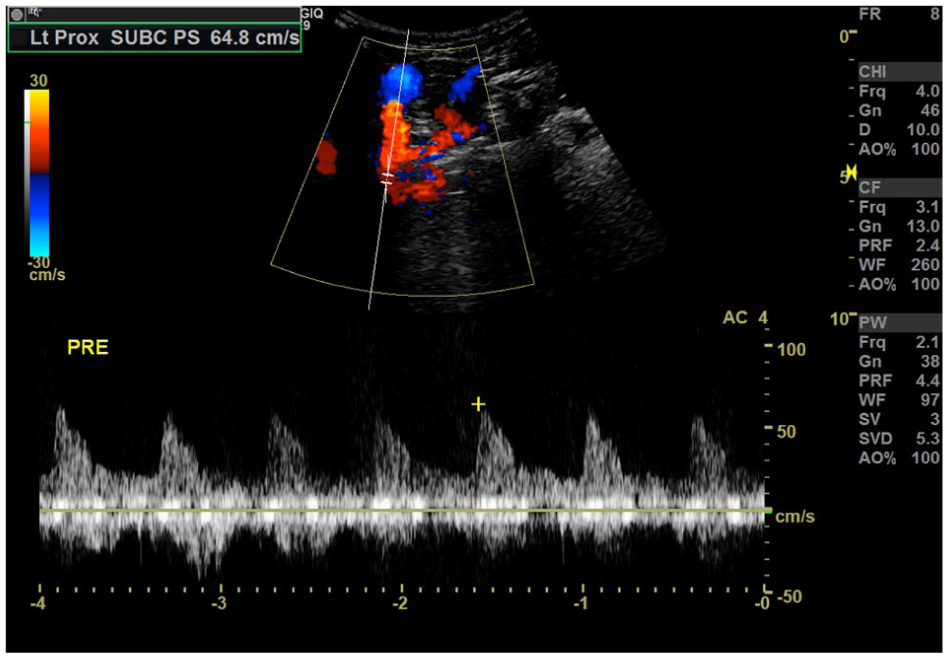
Duplex ultrasound demonstrates a velocity of 65 cm/s prior to the lesion in the left proximal subclavian artery.
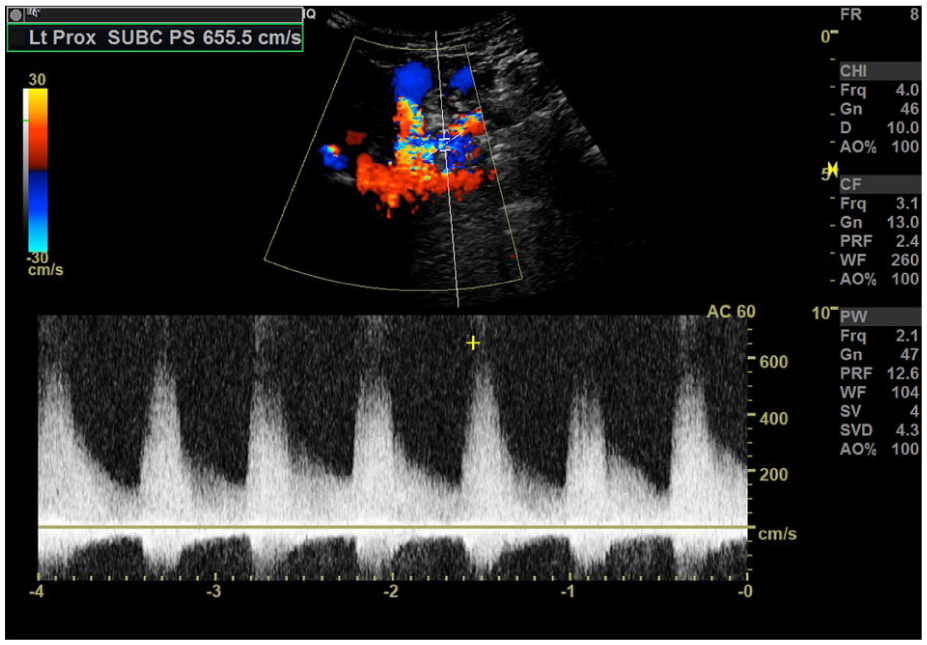
Duplex ultrasound demonstrates elevated velocities of 656 cm/s in the left proximal subclavian artery.
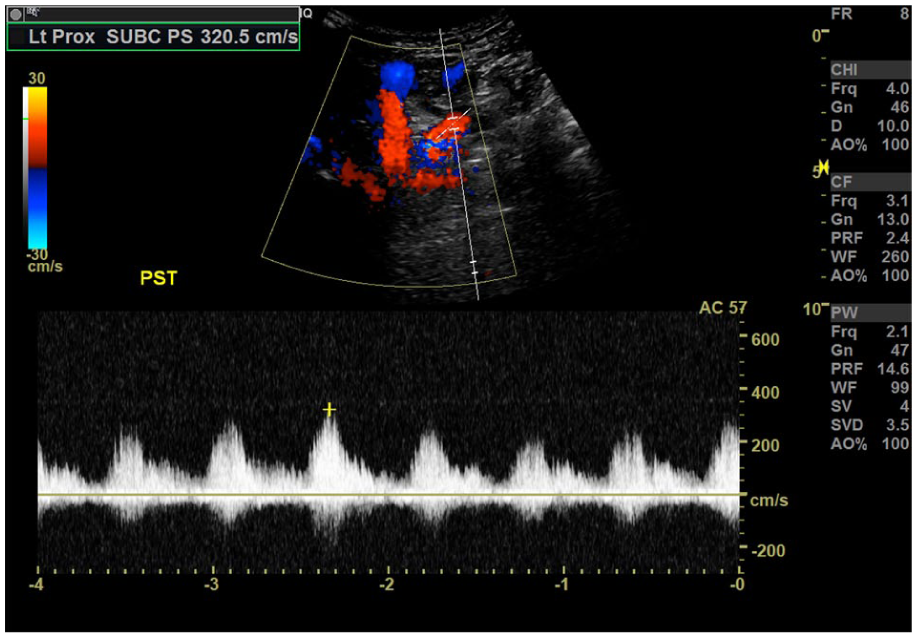
Poststenotic turbulence demonstrated on duplex ultrasound in the left proximal subclavian artery.
The proximal segment of the SCA is often difficult to evaluate optimally with a high-frequency linear transducer; therefore, a curvilinear transducer was used in this case. The left radial and ulnar arteries were patent from origin to wrist. The contralateral distal brachial artery demonstrated a multiphasic Doppler waveform (Figure 7). The left wrist brachial index was mild to moderately reduced at 0.71 with a significant brachial pressure gradient of 36 mm Hg and antegrade flow in the ipsilateral vertebral artery.
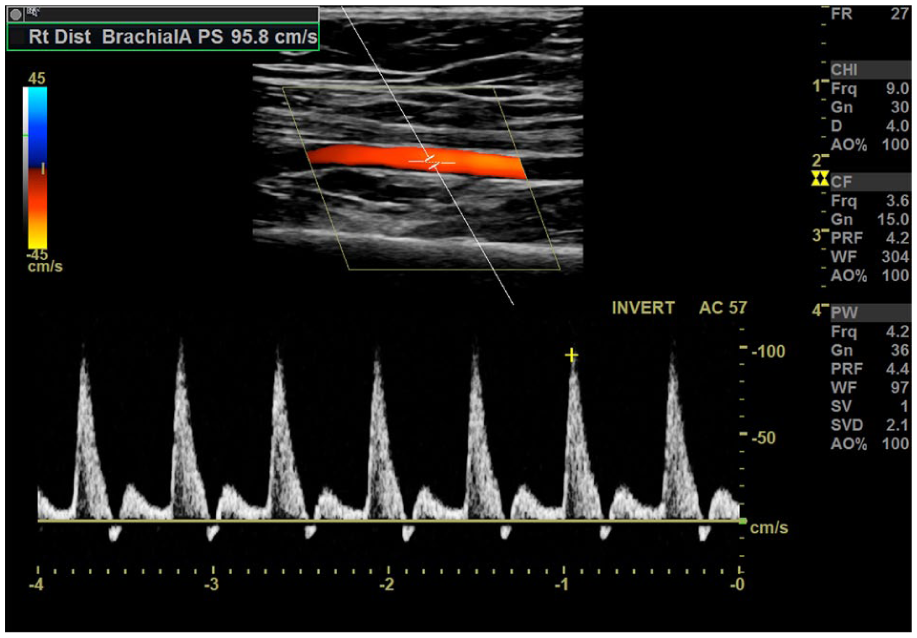
Duplex ultrasound demonstrates a normal multiphasic Doppler waveform in the contralateral distal brachial artery.
Photoplethysmography waveforms demonstrated flatline waveforms in left digits 3 through 5 and decreased pulsatility with delayed upstroke in the first and second digits (Figure 8).
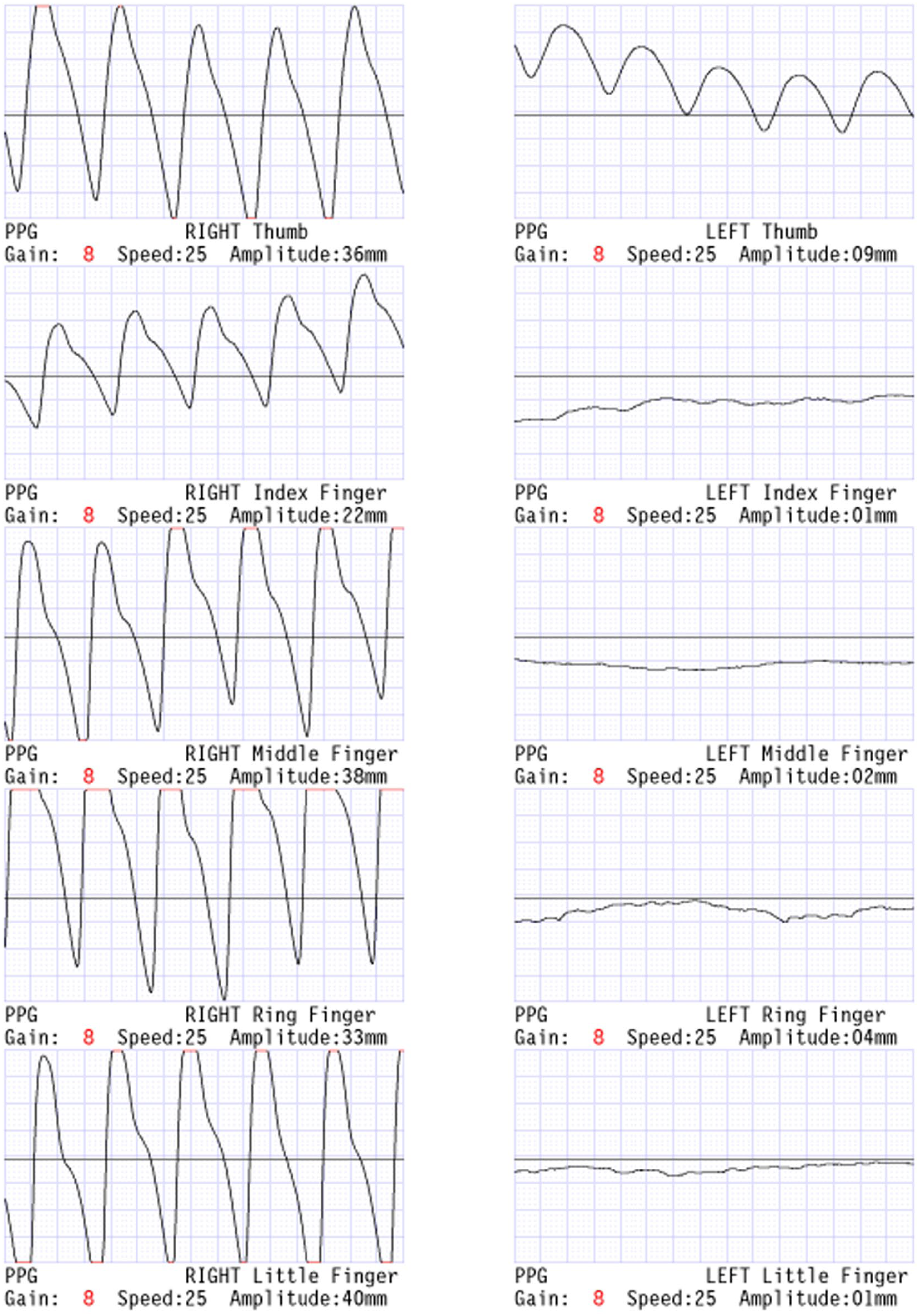
Photoplethysmography (PPG) waveforms performed with duplex ultrasound examination demonstrating flatline waveforms in left digits 3 to 5 and decreased pulsatility with delayed upstroke in the left first and second digits.
The patient was subsequently referred to vascular surgery to evaluate for possible embolic etiologies, prompting a CTA of the chest as well as an echocardiogram with bubble study. Although no embolic sources were identified, the CTA more clearly identified the diagnosis of a proximal SCA stenosis with associated thrombus.
Given these findings, the patient underwent angioplasty of the lesion via access from the right common femoral artery with the use of a 5-mm × 40-mm balloon catheter with resolution of the stenosis documented on completion angiogram (Figures 9 and 10). Following angioplasty, she underwent partial amputations of 3 digits due digital necrosis.
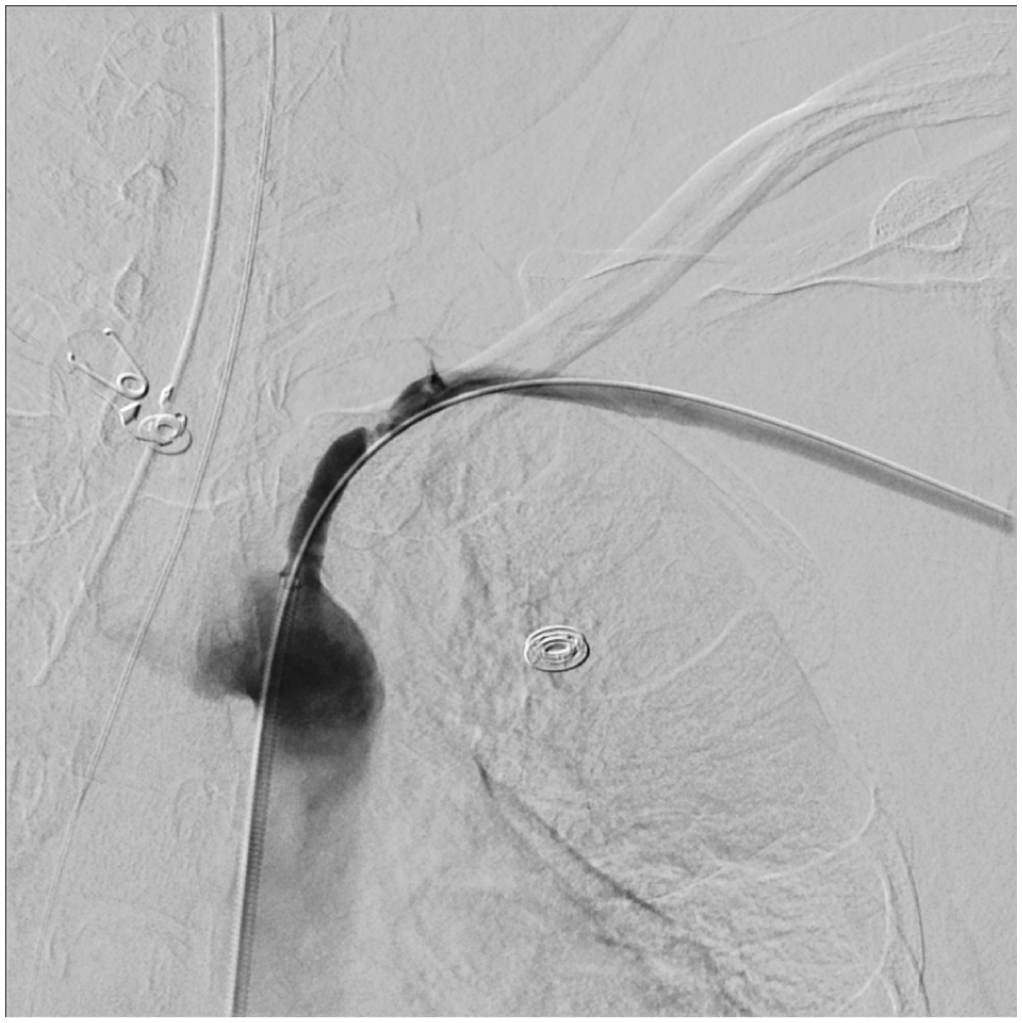
Diagnostic angiogram of the left upper extremity demonstrating focal severe left proximal subclavian artery stenosis.
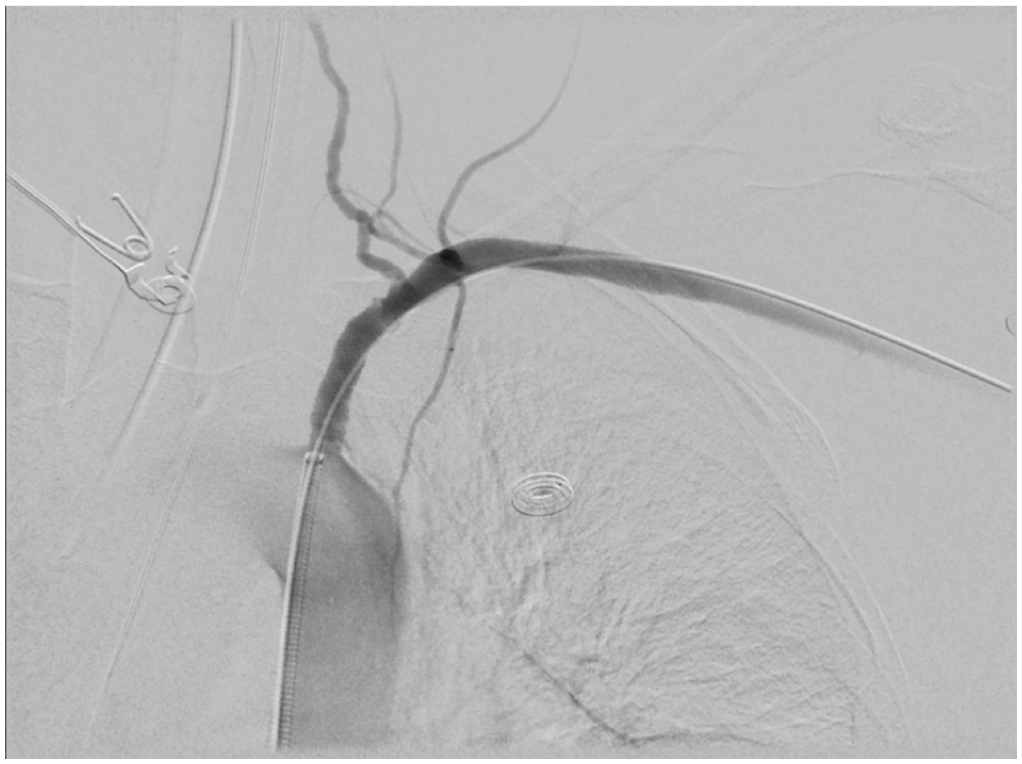
Completion angiogram following angioplasty with 5-mm × 40-mm balloon.
On her 1-month follow-up, the patient reported resolution of her symptoms and repeat duplex ultrasound demonstrated left brachial pressures had increased from 92 to 112 mm Hg with improved velocities and waveforms.
Discussion
The patient’s history of FMD is the likely etiology of her focal left SCA lesion, ultimately manifesting as digital ischemia, reducing her left wrist/brachial index, causing pressure gradient discrepancies on duplex. Fibromuscular dysplasia is a proliferative medium-to-small vessel disease that often manifests as non-atheromatous focal or multifocal “beads on a string” lesions that typically affect lower extremities, although upper extremity FMD does occur in a smaller subset (15.9%) of cases, and when symptomatic, is treated with balloon angioplasty. 1
This case highlights the diagnostic utility of ultrasound when other imaging modalities such as CTA and digital subtraction angiography fail to provide conclusive evidence of focal, flow-limiting lesions such as in carotid artery webs, FMD of internal carotid and renal arteries, and stenotic venous valves. While the initial CTA results were equivocal, independent review did demonstrate a focal stenosis versus possible thrombus near the origin of the left vertebral artery (Figure 11) and follow-up CTA of the chest confirmed that the stenosis was unchanged from the index CTA. This diagnosis was missed on the index scan, potentially due to its small focal area and with patent nondiseased opacification of the mid and distal SCA. The index angiography missed the critical area of disease by advancing beyond the lesion and beginning at the axillary artery. As a result, analyzing the peak systolic velocities and duplex waveforms played a crucial role in identifying the high-grade stenosis of the proximal SCA. This scenario also illustrates the significance of obtaining diagnostic imaging of both inflow and outflow vessels, including evaluation of the aortic arch and supra-aortic trunks, during angiography. Furthermore, the utility of duplex ultrasound and waveform analysis cannot be underestimated, especially when clinical suspicion is high for poor perfusion, and may help prevent delayed diagnosis and limb salvage efforts.
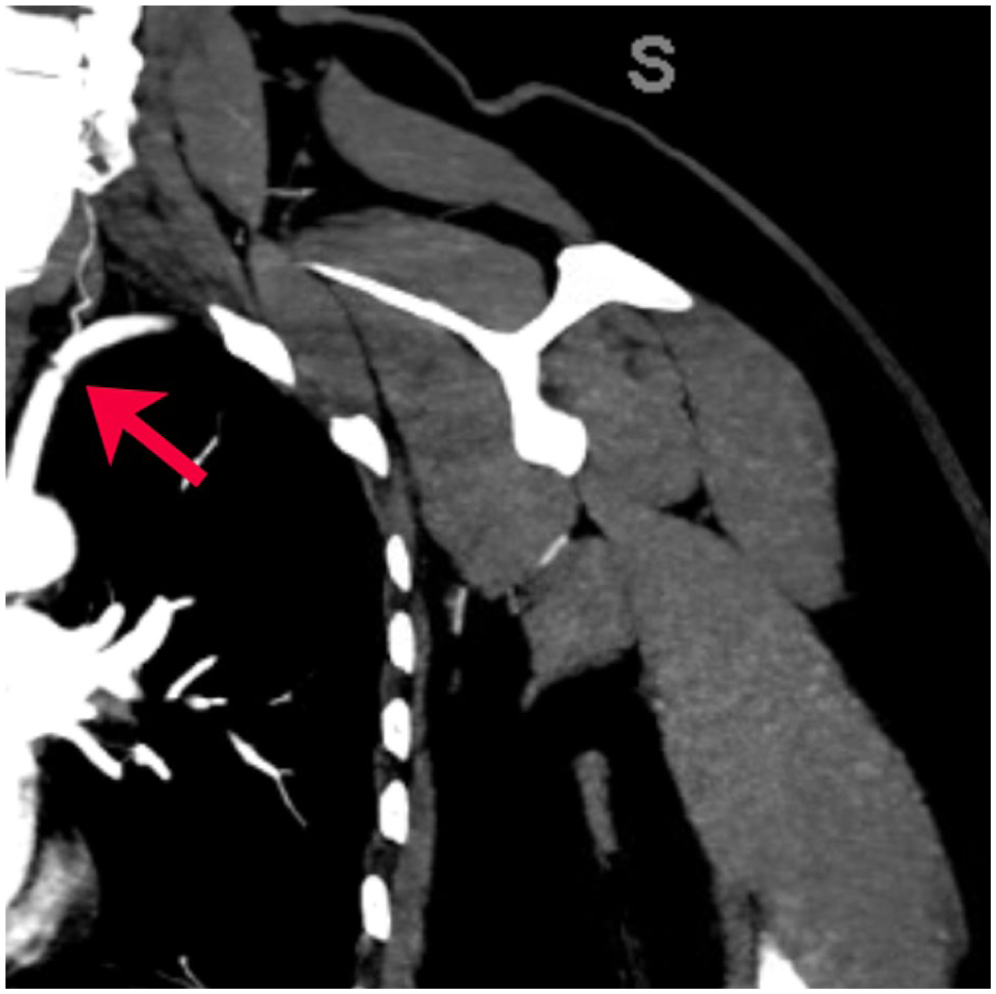
Index CT angiogram of the left upper extremity.
Conclusion
Although diagnostic angiography remains an important modality even in the setting of more invasive and more sensitive cases, inadequate visualization of inflow and outflow vessels limited its diagnostic utility in this case. As a result, duplex ultrasound, with velocity measurement and waveform analysis, can serve a crucial role in providing objective data in identifying clinically significant lesions when alternative imaging is inconclusive.
Footnotes
Acknowledgements
None
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
