Abstract
Previous research has reported high prevalence rates of head injury amongst juvenile justice involved youth and relations between head injury and different forms of offending. However, little is currently known about the extent to which head injury is associated with antisocial personality features – characteristics that are strongly correlated with adult antisocial personality disorder symptomatology. The current study aimed to address this void in the existing body of research by analyzing a longitudinal sample of juvenile detainees (N = 881) to examine the relationship between head injury during childhood or early adolescence and a wide range of antisocial personality features in late adolescence. Results from a series of logistic regression models reveal that head injury is associated with impulsivity and aggression more than other features of antisocial personality. The implications of these results for juvenile justice intervention programming and avenues for future research are discussed.
Introduction
A growing body of research suggests that incarcerated individuals and juvenile justice involved youth are more likely to suffer from a head injury than members of the general public (Farrer & Hedges, 2011; Hughes et al., 2015; Mongilio, 2022). While this area of empirical inquiry is currently in its infancy, there are a few reasons to suspect that individuals involved in the justice system may be more likely to have a history of head injury. First, sustaining a head injury early in life has been associated with neuropsychological deficits and the development of symptoms of internalizing and externalizing psychopathology during adolescence (Connolly & McCormick, 2019; Veeh et al., 2018; Katzin et al., 2020; APA, 2020; Schwartz et al., 2017; Fullerton et al., 2019). These outcomes are common amongst juvenile justice involved youth (Veeh et al., 2018). Head injuries have been linked to a host of problematic behavioral and mental health outcomes including aggression, symptoms of anxiety and depression, neurodegenerative disorders, and cognitive problems (Schwartz et al., 2019; see also Mongilio, 2022; McCormick et al., 2021). Second, prior research has documented that head injuries are more strongly tied to aggression and violence, as well as the persistence of violent behavior from adolescence to young adulthood (Schwartz, 2021). Importantly, many of these behaviors are often considered demonstrated features of antisocial personality - a robust correlate of adult antisocial personality disorder (ASPD), which is a clinical personality disorder characterized by showing little regard for right and wrong and the rights and/or feelings of others (APA, 2020). It has been estimated that approximately 35% of adult offenders suffer from ASPD (Black et al., 2010) and 62% of youth offenders suffer from emerging features of this disorder (Livanou et al., 2019).
Although previous research has begun to examine the relationships between head injury and a range of antisocial behaviors such as crime, delinquency, and aggression (Fullerton et al., 2019; Katzin et al., 2020; Schwartz, 2021), much less attention has been focused on unpacking the association between head injury and the development of antisocial personality symptoms during adolescence, when they begin to emerge. A better understanding of how head injury may be uniquely associated with specific facets of this behavioral trait in adolescence amongst juvenile justice involved youth may help to better predict ASPD in adulthood and improve intervention, assessment, and treatment programming (Lilly et al., 2018; Linden et al., 2020). With this in mind, the current study aims to begin to address this void in the current body of research by analyzing longitudinal data from a sample of juvenile detainees to assess the relationship between early life head injury and antisocial personality features during adolescence.
Antisocial Personality Features
Antisocial personality features include affective traits such as aggressive, hostile, and irritable behaviors that may be manifested as intimidating or threatening others and interpersonal traits, such as lack of empathy and intimacy issues that appear as deceitfulness and manipulative and controlling behaviors (Skodol & Oldham, 2021). Antisocial personality features often include rule or law breaking, recklessness, and getting into fights related to impulsivity issues (Skodol & Oldham, 2021). A defining characteristic of antisocial personality is a lack of regard for others and is typically present since age 15. A disregard for others may include reckless behaviors, law breaking, irresponsibility, manipulations, and callousness (Skodol & Oldham, 2021; Fisher & Hany, 2022; American Psychiatric Association, 2013). Although the assessments of adult ASPD and conduct disorder have developed through the editions of the DSM (Pietz & Mattson, 2015), the DSM-V indicates that this disregard for others and the presence of conduct disorder before the age of 15 are criteria for a diagnosis of ASPD (Fisher & Hany, 2022; American Psychiatric Association, 2013).
Research over the past 80 years on ASPD has shown that early symptoms of antisocial personality are usually observed from childhood to late adolescence, and those with earlier symptoms may have more severe outcomes (Black, 2015). Symptoms of conduct disorder are often seen at a younger age in boys, and a higher percentage of boys with conduct disorder are later diagnosed with ASPD (Fisher & Hany, 2022). Antisocial personality is associated with and assessed by aggressive behaviors and violations of societal rules and laws (Pietz & Mattson, 2015). Adolescent aggression has been shown to be a predictor of antisocial personality during this life course stage (Whipp et al., 2019; Schaeffer et al., 2003). In a global study, conduct disorder was prevalent in 8% of youth under age 18 (Mohammadi et al., 2021), while the prevalence of antisocial personality in juvenile youth was estimated to be around 62% (Livanou et al., 2019).
Additionally, the connections between different forms of child maltreatment and behavioral and mental health problems have been studied, with findings suggesting that there is an association between childhood maltreatment and future violent behavior (Fitton et al., 2020). Childhood maltreatment of juveniles, especially those who reported multiple types of physical abuse, is associated with aggression and impulsivity (Papalia et al., 2022), which are predictors of ASPD (Whipp et al., 2019; Schaeffer et al., 2003; Pietz & Mattson, 2015). Focus should therefore be placed on juvenile youth because of their risk for ASPD (Black, 2015) and the prevalence of different forms of physical victimizations such head injury in this population (Perron & Howard, 2008).
Head Injuries and Antisocial Personality Features in Adolescence
Youth involved in the juvenile justice system are more likely to have a history of sustaining a head injury compared to those not involved in the system (Hughes et al., 2015). Head injuries are reported to be associated with neuropsychological deficits and violent behavior amongst adolescents (Veeh et al., 2018; Katzin et al., 2020). Terrie Moffitt’s (1993) developmental taxonomy theory acknowledges the impact of neuropsychological deficits caused by toxins or brain injuries on traits, such as low self-control and impulsivity, which are risk factors for antisocial behavior. A recent study examined head injuries and neuropsychological deficits with offending and found that participants with head injuries demonstrated a higher likelihood of violent offending over time (Schwartz, 2021). Not only have studies assessed the behavioral and development effects of head injuries on children and adolescence, but studies have connected these impairments with head injuries during infancy (Eismann et al., 2020). Antisocial behaviors linked to deficits associated with brain injuries have been studied separately (Katzin et al., 2020) and in conjunction with the study of the development of facets of antisocial personality disorder, such as psychopathy (Koenig et al., 2020).
According to the American Psychological Association, antisocial personality features manifests in “repeated violations of the law, exploitation of others, deceitfulness, impulsivity, aggressiveness, reckless disregard for the safety of self and others, and irresponsibility, accompanied by lack of guilt, remorse, and empathy” (APA, 2020). Head injuries may have adverse effects on the development of self-control, which is related to a range of antisocial behaviors (Mongilio, 2022; Schwartz et al., 2017) and externalizing as well as internalizing problems (Connolly & McCormick, 2019; McCormick et al., 2021). As one study concluded, “head injury may play a significant role in blunting the decline in impulsivity across development, exposing an additional risk factor for antisocial behavior” (Fullerton et al., 2019, p. 1035). An earlier study examining a sample of adjudicated youth assessed the link between head injury, impulse control, and delinquent behavior and reported that impulse control partly mediated the association between head injury and rates of change in aggressive offending from adolescence to adulthood (Schwartz et al., 2018). Fullerton et al. (2019) found that those with early head injuries demonstrated slower decreases in impulsivity and had higher aggression, as opposed to those without head injuries by ages 14 to 15 (Fullerton et al., 2019). Another study examined the association between head injuries, criminal activity, by and changes in moral disengagement and reported that head injuries were associated with decreases in moral disengagement, which could be linked to deficits in the brain associated with decision-making (Schwartz et al., 2020). Although moral disengagement has been assessed in relation to head injuries (Schwartz et al., 2020), and some studies have looked at a lack of concern and disregard for social norms (Duncan et al., 1997), empathy (O’Neil & McMillan, 2012; de Sousa et al., 2011), or cold heartedness (Perron & Howard, 2008), limited research has examined the relationship between head injuries and other facets of antisocial perosonality such as callousness, decietfulness, irresponsibility, reckless disregard for others, and a lack of remorse. The current study focuses on contributing to the existing body of research by examining the connections between head injury and features of antisocial personality in adolescence amongst a sample of previously detained juvenile youth.
The Current Study
There is a growing body of research demonstrating a longitudinal link between head injuries and a range of antisocial and offending behaviors. However, absent from this developing line of research is an empirical evaluation of whether sustaining a head injury is associated with a broader range of symptoms, that are robustly associated with ASPD later in life, during adolescence in a sample of at-risk juvenile justice involved youth. With this in mind, the current study offers a longitudinal evaluation of whether sustaining a head injury is associated with higher odds of meeting symptom thresholds for antisocial personality in general, failure to conform to social norms, deceitfulness, impulsivity, irritability and aggression, reckless disregard for others, irresponsibility, and lack of remorse.
Methods
Data
The data analyzed in the current study come from the Northwestern Juvenile Project Series, which began in 1995 in Cook County, Illinois. Data was collected initially from juvenile detainees for the purpose of assessing their alcohol, drug, and mental health needs and the services received while in custody. The baseline data was collected between 1995 – 1998, which is when the head injury data was collected. Follow-up data was collected through interviews in 1998–2001 (Follow-up Wave 1), 1999 – 2005 (Follow-up Wave 2), 1999 – 2007 (Follow-up Wave 3), 2000 – 2006 (Follow-up Wave 4), 2002 – 2006 (Follow-up Wave 5), and 2004 – 2008 (Follow-up Wave 6) from the baseline sample. Follow-up Wave one data was collected about 3 years after the baseline data was collected and included an assessment of antisocial personality features (Teplin, 2013). Male and female participants from age 10–18 years old were sampled randomly during intake at a Juvenile Temporary Detention Center between 1995 and 1998, and the baseline sample was stratified by age, race/ethnicity, legal status, and gender with a total of 1,829 youth (Teplin, 2018).
Measures
Head Injury
Head injury was assessed by asking participants during the baseline wave “Have you ever had a head injury?” Response categories to this question were no (= 0) or yes (= 1). Approximately 45% of participants (n = 797) reported a history of head injury. Participants who reported ‘yes’ were then asked to report how many times they suffered a head injury from several different causes. Figure 1 presents a graphical depiction of the prevalence of head injury by cause based on participants self-reports during the baseline wave. As can be seen, the most commonly reported causes of head injury were hitting one’s head on an object (19.59%), being beaten up (14.57%), falling from a distance (14.07%), and falling down (11.80%). These reasons align with those reported by other empirical studies examining the reasons for pediatric head injury in large population-based samples of youth (Taylor et al., 2017). Self-reported causes of head injury.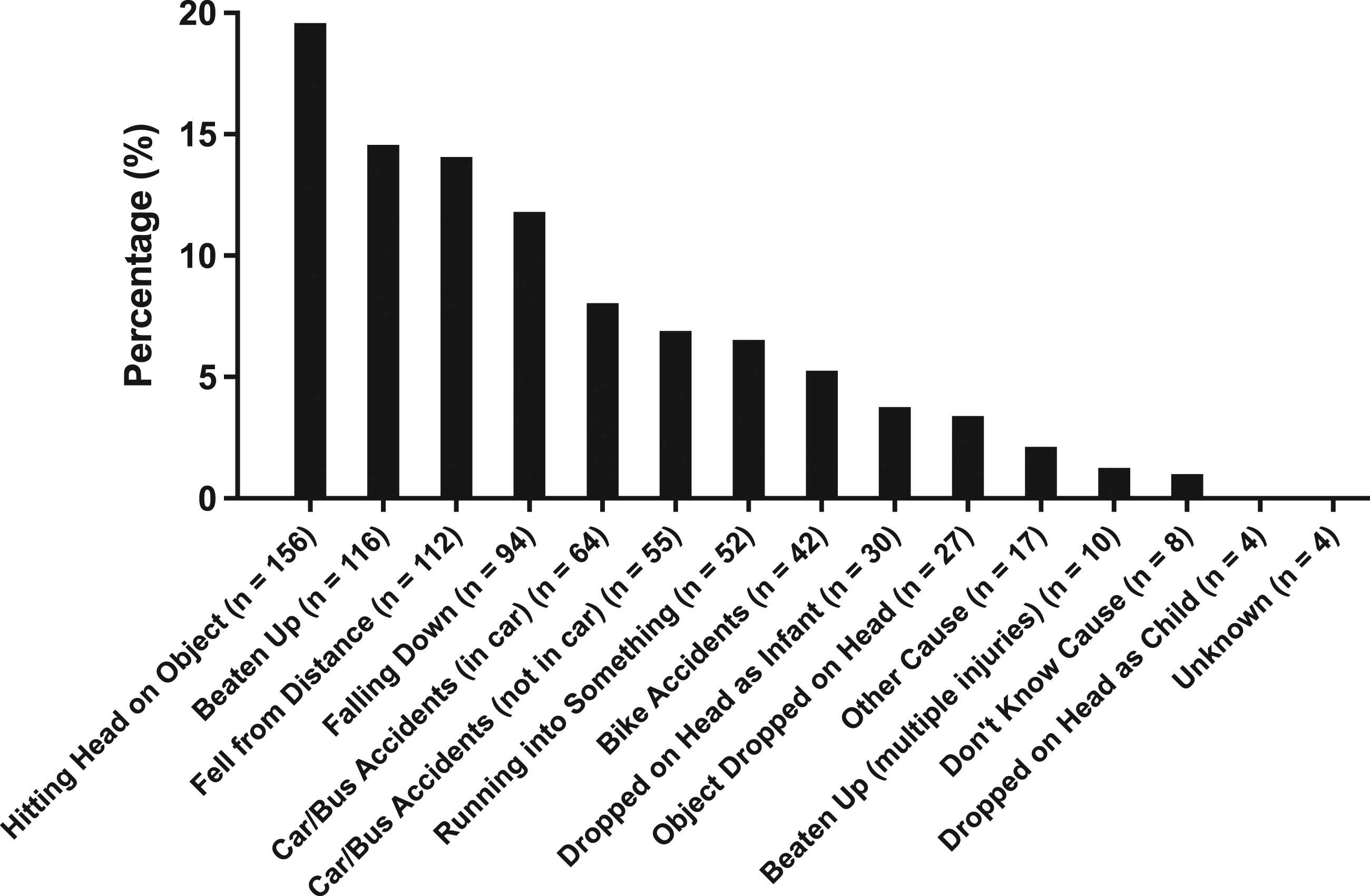
Antisocial Personality Features
Antisocial personality features were assessed by a comprehensive youth assessment instrument based on the DSM-IV, the Diagnostic Interview Schedule for Children (DISC-IV), during Follow-Up Wave 1. The DISC-IV is a structured interview assessment tool, administered by non-clinician interviewers with training, designed to evaluate over 30 disorders in children and adolescents (Shaffer et al., 2000). Depending on the age of the participant, the youth or young adult version of the DISC-IV was administered. The Diagnostic Interview Schedule (DIS-IV) is the young adult version administered to participants 18 and older at Follow-Up Waves 1, which assessed antisocial personality features. The following seven Criteria A symptoms of antisocial personality from the DSM-IV and DSM-V (APA, 2020; APA, 2013) were evaluated and coded as ‘1’ for demonstrating symptoms and ‘0’ for not demonstrating symptoms: 1) failure to conform to social norms with respect to lawful behaviors – stealing, drug sales, vandalism, and harassment; 2) deceitfulness – feigned illness or injury, used an alias, claimed false education/job experience/marital status; 3) impulsivity and failure to plan ahead – no fixed address, walked off jobs, left spouse or partner without warning, never faithful to partner for 1 year, moved frequently; 4) irritability and aggressiveness – started fights, used weapon, threatened with weapon, started hitting spouse/partner, hurt child; 5) reckless disregard for safety of self/others – promiscuity, accident with gun, speeding in city, multiple traffic accident, drove drunk, left child unsupervised; 6) irresponsibility at work or financially – purchases repossessed, periods not working when not ill, quit job, skipped support payments, skipped work, borrowed with no repayment, and; 7) lack of remorse – not sorry to have hurt/upset others, felt victims deserved it, thinks others harmed him/her, no regrets for past behavior, regrets only because adverse outcome.
Covariates
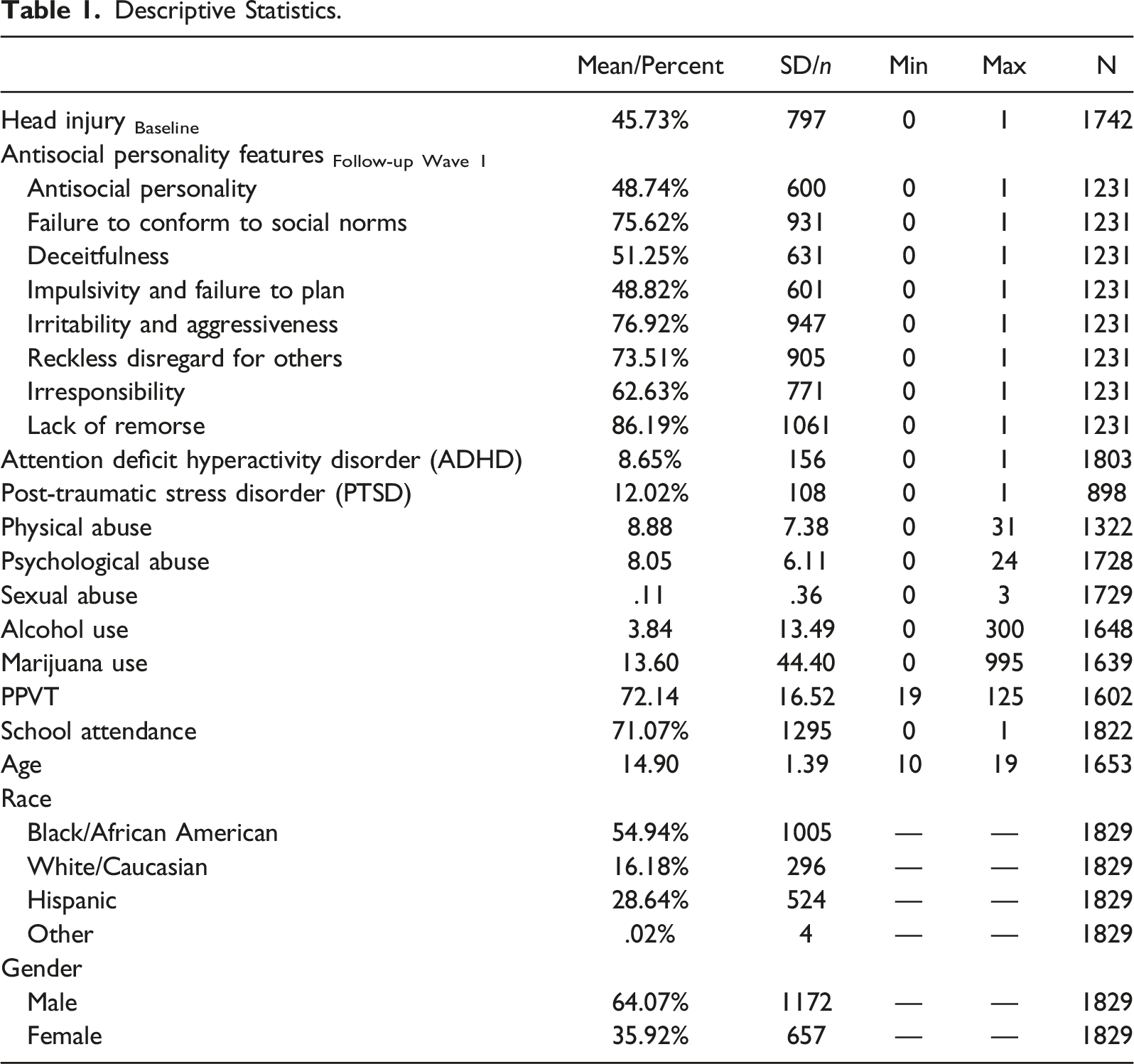
The current study also included several relevant covariates in the analysis. Interviewer evaluations of symptomatology for Attention Deficit Hyperactivity Disorder (ADHD) and Post-Traumatic Stress Disorder by trained and licensed clinicians were used to control for ADHD and PTSD diagnoses (0 = no, 1 = yes). A measure of psychological abuse was also included, which was assessed by combining responses from four items asking respondents about their history with psychological victimization from parents and guardians including being made fun of. Sexual abuse was comprised of responses from five items tapping each respondent’s history of unwanted sexual advances from adults in their lives. Physical abuse was comprised of six items tapping each respondent’s history of physical victimization from parents and guardians including being hit very hard, beaten, and kicked. For each measure of abuse, higher scores indicate more incidents of abuse. School enrollment is a dichotomous measure which indicates if participants were enrolled in school at baseline (0 = no, 1 = yes). The Peabody Picture Vocabulary Test (PPVT) was included as a measure of verbal intelligence and a question asking about current school attendance during Follow-up Wave one was included as a control (0 = no, 1 = yes). The data also included demographic information for age in years, race/ethnicity, and gender during the baseline wave which were controlled for in the analysis. Table 1 presents descriptive statistics for all variables.
Analytic Plan
Descriptive Statistics.
Results
Bivariate Correlations.
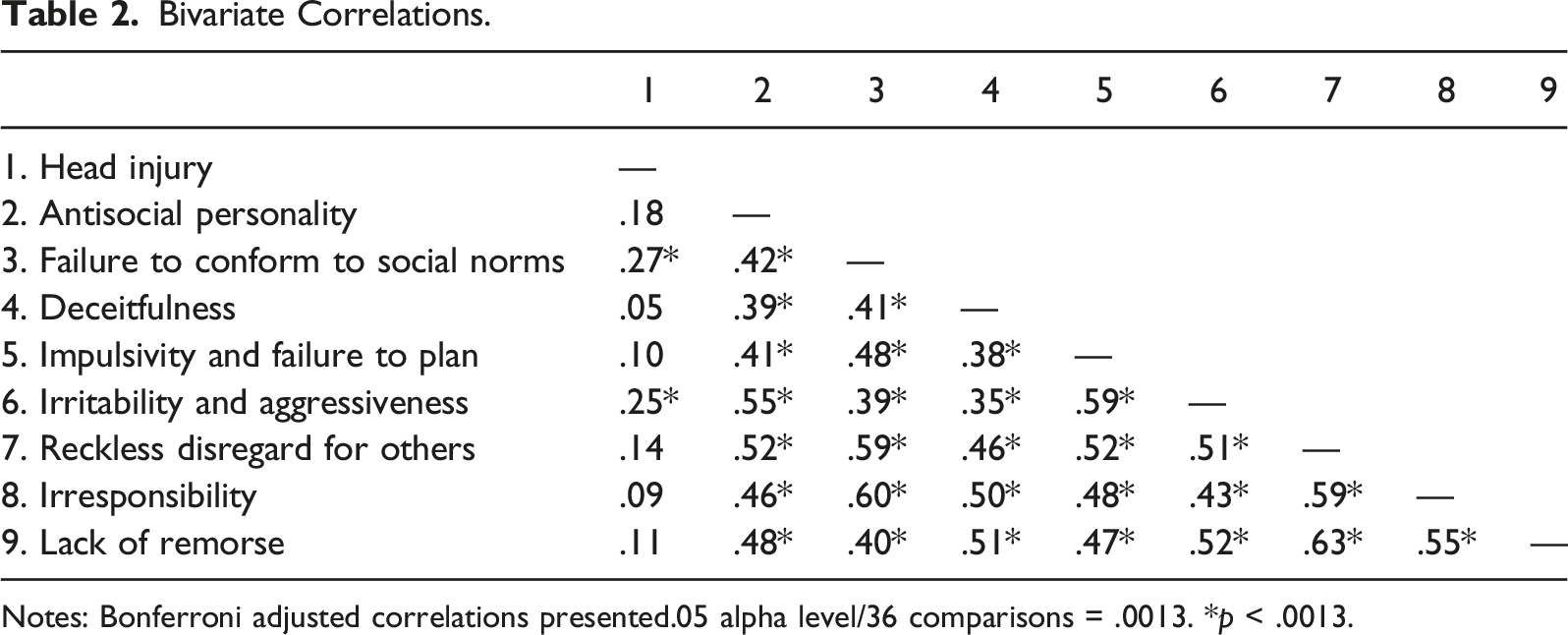
Notes: Bonferroni adjusted correlations presented.05 alpha level/36 comparisons = .0013. *p < .0013.
Logistic Regressions Predicting Antisocial Personality Features.
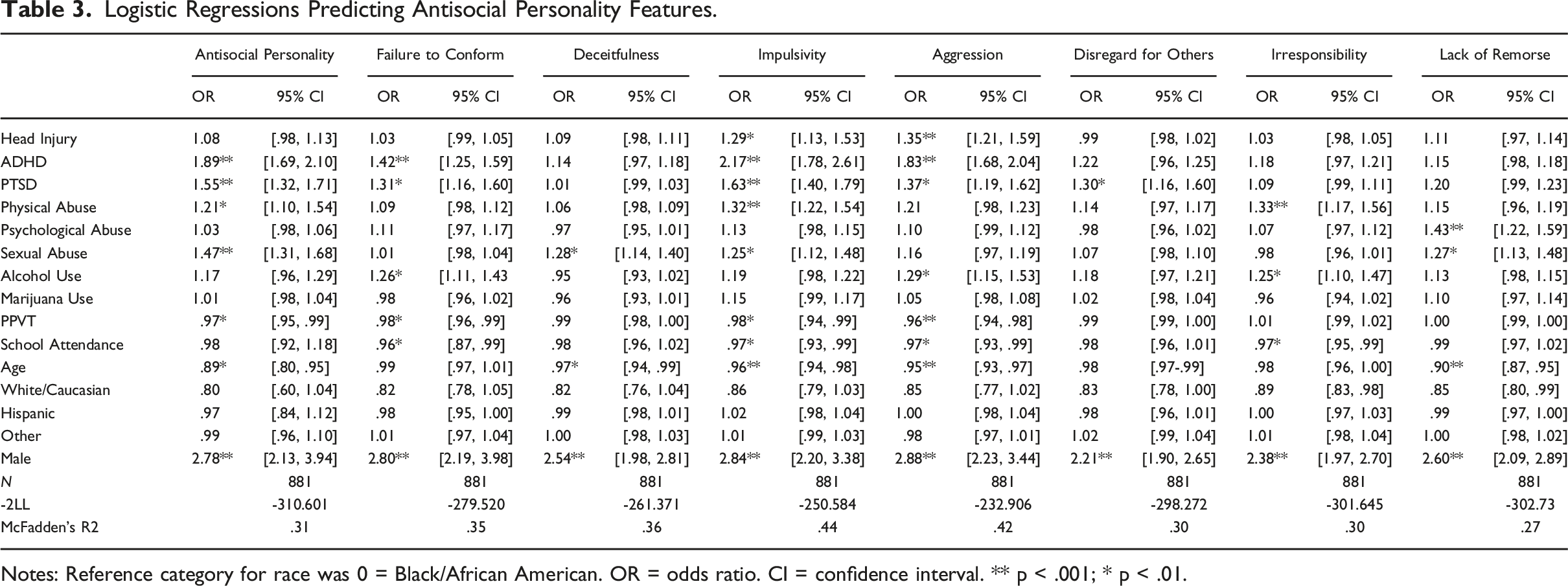
Notes: Reference category for race was 0 = Black/African American. OR = odds ratio. CI = confidence interval. ** p < .001; * p < .01.
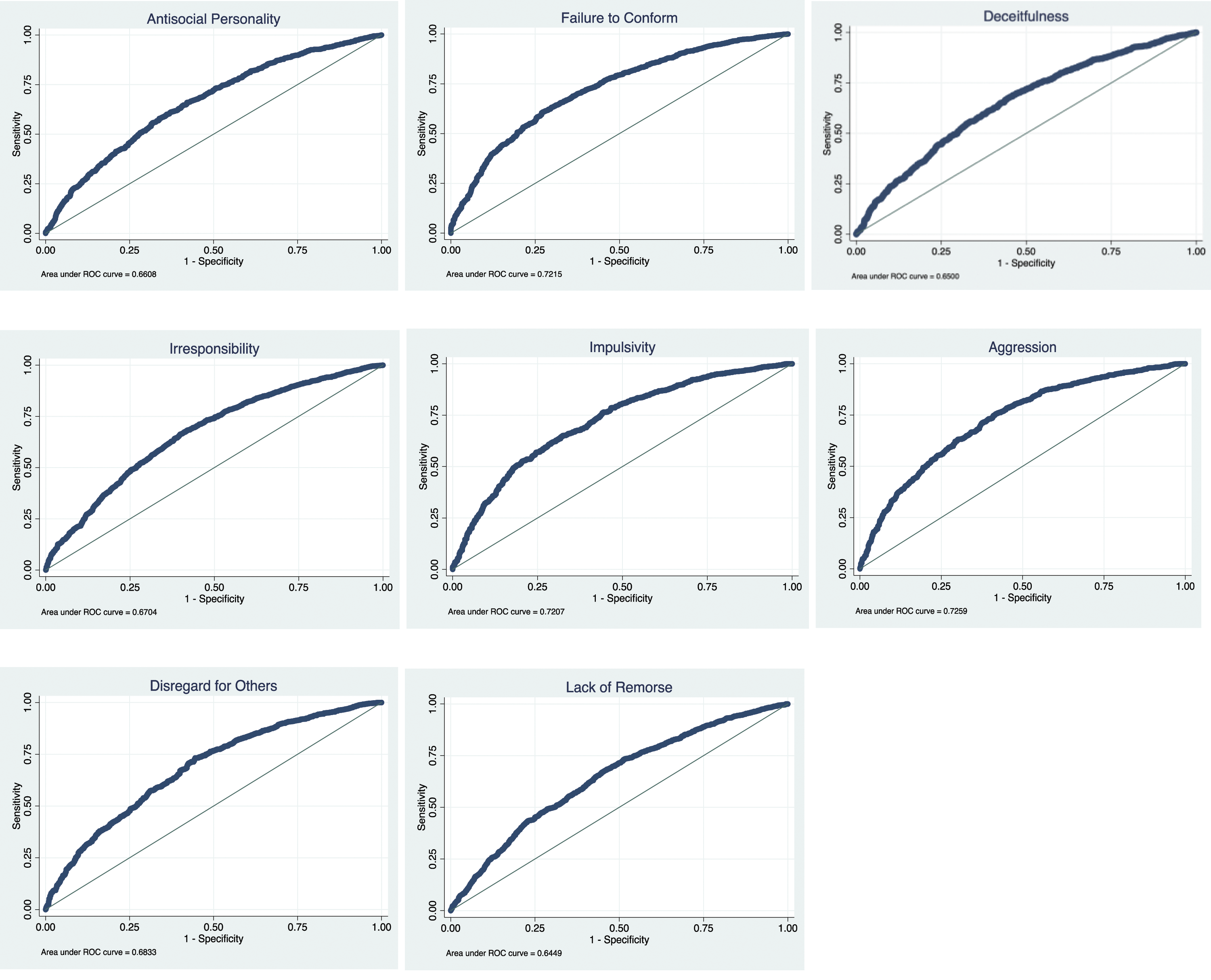
Area under ROC curves for predicting antisocial personality features.
Supplemental Analysis
Based on the results generated from the primary multivariate analyses, a series of supplemental models were estimated to assess the potential role of the frequency of head injury on the association between sustaining a head injury, impulsivity, and aggressiveness at Follow-up Wave 1. Descriptive statistics for head injury frequency at the baseline wave revealed that of the 797 respondents from the sample who reported a head injury (45%), 470 (27%) reported one head injury, 166 (9%) reported two head injuries, and 158 (8%) reported three or more head injuries. The results from the analyses revealed that head injury frequency conditioned the association between head injury reported during baseline and aggressiveness assessed during Wave 1 (OR = 1.13, 95% CI = 1.06, 1.92, p = .011). An illustration of the differences in ORs predicting aggressiveness across head injury frequency are shown in Figure 3. Head injury predicting aggressiveness across number of head injuries.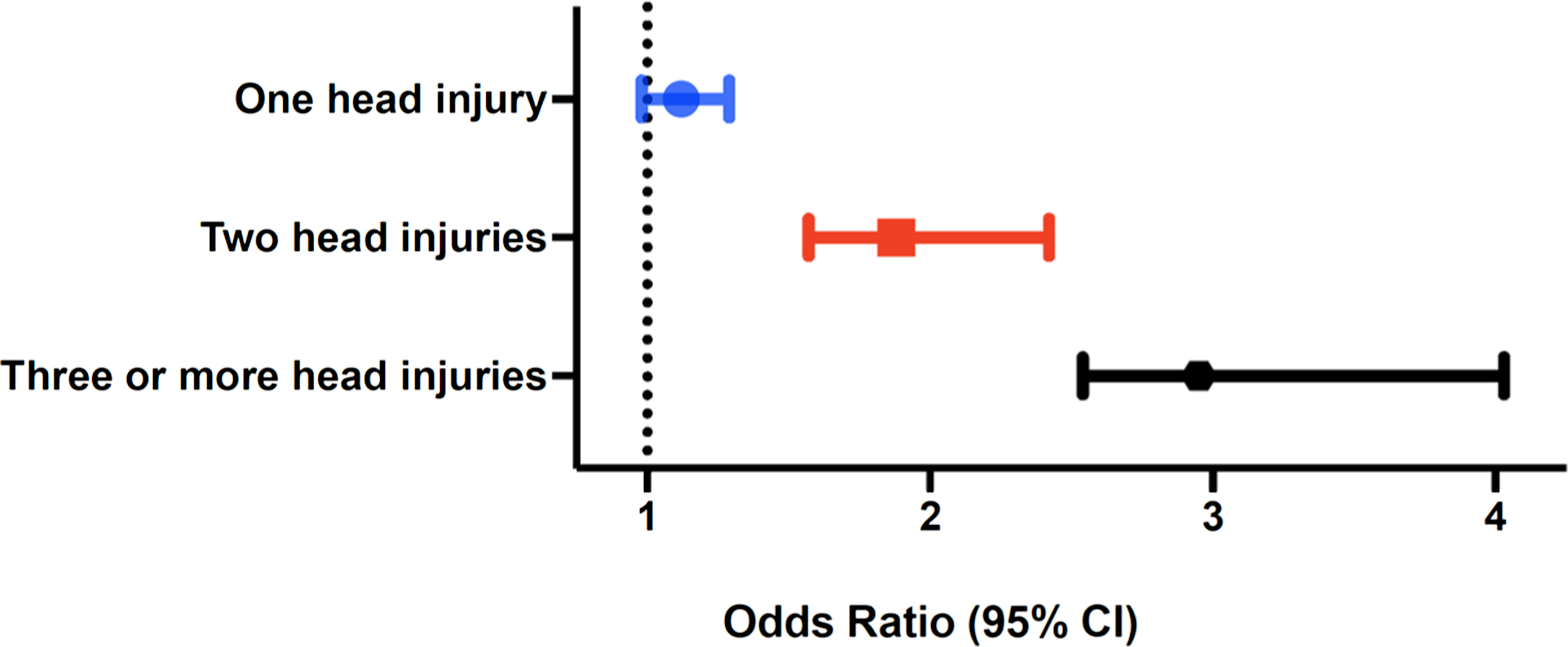
Discussion
The current study aimed to examine the common and unique associations between head injury and antisocial personality features in adolescence among a sample of juvenile justice involved youth. While existing evidence suggests that head injury is associated with general delinquency (Connolly & McCormick, 2019; Mongilio, 2022) and aggressive offending (Schwartz, 2021), less is known about whether head injury is related to other symptoms robustly correlated with future ASPD, such as failure to conform to social norms, deceitfulness, failure to plan, a reckless disregard for others, irresponsibility, and lack of remorse. As assessment of these characteristics are commonly used in many juvenile justice youth assessment instruments and argued to be predictive of future problematic behavior and offending (Skodol & Oldham, 2021; Livanou et al., 2019), thus a better understanding of the underlying factors associated with these problems could help create more targeted prevention and intervention programming. In an effort to begin to address this gap in the existing body of research, data from a longitudinal sample of juvenile detainees were analyzed to assess whether and to what extent head injury is related to antisocial personality in general and features of this trait during adolescence. Two key findings emerged from the analysis that warrant further discussion.
First, approximately 45% of juvenile detainees in the sample reported suffering from at least one head injury during the baseline wave. This estimate aligns with previous studies examining samples of at-risk youth (Hughes et al., 2015) and further highlights the high prevalence rate of this type of injury and likely subsequent trauma faced by vulnerable youth. Recent research suggests that children from disadvantaged backgrounds who suffer from this type of injury are likely to experience other adversities in their household and community such as emotional, physical, and sexual abuse (Papalia et al., 2022), substance use (Vaughn et al., 2019), social and emotional impairments (Bernstein & Davies, 2018), depression, anxiety, and delinquency (Connolly & McCormick, 2019). In line with these arguments, self-reported information from participants on the causes of their head injury revealed that being hit in the head with an object, beaten up, and falling were the most common causes of head injury. To the best of our knowledge, this is the first type of information analyzed and reported in contemporary research on head injury from a sample of previously detained male and female juveniles in the United States. These findings shed new and much needed light on the reasons behind high rates of head trauma early in life. Future research should begin to unpack these reasons and evaluate factors associated with these causes of head injury to better identify targets for prevention.
Second, head injury was associated with 29% higher odds of meeting the criteria for impulsive tendencies and failure to plan. Previous research suggests that head injuries may play a role in slowing the improvement of impulsiveness as an adolescent gets older (Fullerton et al., 2019) and in decision-making (Schwartz et al., 2020). It is possible that damage to the brain during this sensitive period of develop may stunt growth in immature regions of the brain responsible for regulating impulsive propensities, such as the prefrontal cortex. With this in mind, sustaining a head injury was also associated with 35% increased odds of meeting the criteria for irritability and aggression. This is consistent with prior research that reports a stronger association between head injuries and violence and aggression (Schwartz, 2021). These findings are also consistent with research indicating that breaking rules or laws and getting into fights is related to impulsivity issues related to ASPD (Skodol & Oldham, 2021). Adolescents often engage in pleasure-seeking and risky activities related to the imbalance of development in the prefrontal cortex and limbic system (Konrad et al., 2013); however, individual neural differences may play a role in the level of risky behaviors they engage in (Casey et al., 2008). As an adolescent’s brain changes with the prefrontal cortex developing later than the limbic system, making adolescents more susceptible to negative environmental factors (Konrad et al., 2013), head injuries could cause neural deficits that affect developmental differences that result in more impulsive or aggressive behaviors. Head injuries could “cause disruption of neurofunctional circuits” leading to lasting cognitive and emotional problems (Konrad et al., 2011, p. 1207). Further investigating how head injuries affect specific neural functions during adolescence, when the brain is still developing, and the impact these developmental deficits have on antisocial behaviors would provide a better understanding of the role head injuries play and what interventions are needed.
Despite the contributions this study makes to understanding the relationship between early life head injury and antisocial personality features, the data is not without limitations. First, the data used for the analyses are drawn from a sample of juvenile justice involved youth in one region of the United States, the Midwest. Replicating this study on samples from other parts of the country, as well as with samples from the general population, would help to strengthen external validity. Second, head injury data during the baseline wave did not include other pertinent details surrounding a respondent’s head injury such as the age at which they experienced their first head injury. Future research should aim to replicate the reported findings with head injury data across participants’ life course to better establish temporal order. Third, the sample did not have a strong measure of socioeconomic status, which may have been an important covariate to include in the analyses and could affect the pattern of results. Although the data analyzed in this study has some limitations that may want to be considered with future research, the results contribute to the literature on head injuries and antisocial personality features in a sample of at-risk youth. These results have implications for future research and policy involving at-risk and juvenile justice involved youth. Continuing to assess the neuropsychological deficits associated with head injuries, as well as this relationship with mental health disorders that are associated with criminal offending, such as ASPD, is important for juvenile justice. Adding to this body of knowledge may assist in the identification of youth most at-risk to demonstrate antisocial personality features that are related to violating social norms and engaging in criminal behaviors. These risks and behaviors may begin early in adolescence before contact is made with the juvenile justice system. Better understanding the increased risk head injuries may have on at-risk youth in school could help improve early interventions and possibly reduce the development of ASPD and the school-to-prison pipeline risk. Adolescents are still developing and may be more responsive to treatment at an early age, making this a critical time in the life course to intervene and reduce future involvement in the justice system.
Conclusion
Through an empirical examination of the relationship between early life head injury and antisocial personality features using longitudinal data from a sample of juvenile justice involved youth, this study provided evidence of an association between head injury and antisocial personality features. Specifically, this study found that head injury was associated with higher odds of meeting the criteria for impulsive tendencies and irritability as well as aggressiveness. In addition, descriptive statistics from self-reports of the causes of head injury from participants provided new insight into some of the reasons at-risk youth experience head injuries. Collectively, the results stress the need to consider head injury as a risk factor for the development of specific antisocial behavior features in adolescence. The impact head injuries may have on cognitive functioning, impulse control, and aggression suggests a need for more research on the causes and consequences of head injuries in at-risk and juvenile justice involved samples of youth.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
