Abstract
There is a paucity of research into the strategies occupational therapists use to maintain career longevity professional resilience. The objective of the study was to identify the strategies used by occupational therapists to maintain their professional resilience. Descriptive statistics were used to analyze data from a cross-sectional survey that investigated the professional resilience strategies used by experienced occupational therapists. Valid responses were received from 489 occupational therapists from 29 countries. The most used professional resilience strategies were maintaining a belief in the value of occupational therapy, taking time for reflection on positive outcomes, using personal time management strategies, and engagement in informal and formal professional support networks. A range of professional resilience strategies are used by experienced occupational therapists in health and social care settings. The findings can be used by managers and workplace organizations to support their occupational therapy workforce.
Plain Language Summary
While multiple studies have reported on the challenges in workplaces, there is a lack of research discussing what strategies experienced occupational therapists use to maintain their career longevity. The paper reports on the findings of a survey of 495 occupational therapy respondents, which identified the range of professional resilience strategies experienced practitioners use in practice. The findings can be used by managers and workplace organizations to support the strategies that extend the career longevity of their occupational therapy workforce.
Introduction
Internationally, occupational therapy practitioners face multiple occupational stressors (Abaoğlu et al., 2021; Katsiana et al., 2021; Popova et al., 2022; Porter & Lexén, 2022; Poulsen et al., 2014; Shin et al., 2022). The consequences of these stressors can be burnout, a subsequent poor retention of practitioners with the associated costs of recruitment and retraining for employers (Porter & Lexén, 2022; Scanlon & Hazelton, 2019; Shin et al., 2022). The loss of experienced practitioners and their accumulated clinical skills and practice wisdom can lead to a paucity of experienced supervisors, reduced clinical leadership, and potentially reduces the quality of care provided to the public (Porter & Lexén, 2022).
All health and social care professionals face challenges and experience workplace stressors (Markey et al., 2021; O’Donovan & Mcauliffe, 2020); however, some challenges are unique to occupational therapists. These include professional marginalization in settings where dominant discourses diminish professional identity and where the profession’s core domain of practice is inhibited or marginalized (Walder et al., 2022; Wilding & Whiteford, 2008). These discourses include accepted bodies of knowledge and language that shape service-delivery and priorities in health and social care. They include biomedical (Wilding & Whiteford, 2008), psychological discourses (Ashby et al., 2015), social care, and educational discourses (Lamash & Fogel, 2021). These discourses can influence occupational therapy practice by minimizing the importance of occupation-based practices (Walder et al., 2022) and lead to practitioners experiencing the perception of poor professional status. The pressure to adhere to these dominant practice discourses often creates a dissonance with professional paradigm which for occupational therapists is underpinned by an occupational perspective of health (Walder et al., 2022). An occupational perspective refers to a focus on the necessary and desired occupations of an individual and enabling participation (Fisher, 2014). Pressure to adhere to biomedical and psychological discourses and subsequent tensions in teams contribute to occupational stressors and impact on personal paradigms because although a profession’s broader paradigm shapes practice, an individual practitioner’s personal paradigm may be changed by life experiences and workplace experiences (Björklund, 1999). For occupational therapists, this can be caused by reduced opportunities to use discipline-specific models, concepts, skills, and occupation-based practices (Ashby et al., 2015). In addition, occupational therapists who work in outcome-driven health settings and case management employment (Gupta et al., 2012; Wressle & Samuelsson, 2014) often face pressures to perform genericized roles and to discharge clients within strict timeframes (Lexén et al., 2021). Subsequently, other common factors which contribute to burnout include unmanageable workloads, lack of autonomy, conflict with expectations and requirements of the organization (Porter & Lexén, 2022), and lack of respect from colleagues (Bolding et al., 2021). These factors contribute to stress and job dissatisfaction for occupational therapists through lack of time for client interventions due to large workloads (Porter & Lexén, 2022) and reduced autonomy due to interdisciplinary and managerial pressures. Several authors have explored personal care strategies that can be used by occupational therapists and student-practitioners (Popova et al., 2022; Poulsen et al., 2014). Despite this, there is a paucity of research about the professional resilience strategies that practitioners use to maintain their career longevity.
The term professional resilience is defined as the ability of a practitioner to achieve a balance between occupational stressors and life challenges, while fostering professional values and career sustainability (Fink-Samnick, 2009). Within occupational therapy, the term professional resilience was first used by Ashby et al. (2013) in their study of occupational therapists in mental health practice. They proposed that within occupational therapy professional resilience is underpinned and maintained by professional identity and opportunities for occupation-based practice and identified a range of strategies that included the importance of formal and informal support networks including the role of effective supervision. These networks create opportunities for professional socialization and enabled opportunities for shared reflection-on-practice and modeling of effective coping strategies. They include effective supervision and attendance at continuing professional development events. Other studies have identified that effective supervision can also reduce burnout (Porter & Lexén, 2022; Shin et al., 2022).
Thus, the purpose of this study was to identify the professional resilience strategies used by experienced practitioners within the international occupational therapy community.
Method
Design
A cross-sectional study design method was used. Ethical approval was provided by the University of Newcastle Human Research Ethics Committee (H-2017-0041). Participation in the study was voluntary. A respondent information statement attached to the survey informed people that the return to the survey was considered informed consent. The survey was anonymous and therefore respondent anonymity was persevered at all stages of the data collection and analysis: no cookies or tracking software were used.
Participants
The inclusion criteria for the study were as follows: (a) occupational therapists and (b) who had two or more years clinical experience. Convenience sampling methods were used to recruit participants through announcements on occupational therapy social media sites such as occupational therapy sites on Facebook, and the use of occupational therapy users on Twitter (now X) and online newsletters. In addition, emails were sent to 31 World Federation of Occupational Therapists member organizations from predominantly English-speaking countries because the questionnaire was only available in the English language.
Data Collection
Data were collected using the Survey Monkey Inc. platform over a 6-month period from March 2018. An online survey methodology was chosen to increase sample size and enable global distribution. The target sample size for the study was based on the World Federation of Occupational Therapists (2023) estimates that there are 633,000 occupational therapists worldwide. While the experience level of these therapists is unknown for this study, we assumed that all therapists were “experienced” at a 95% confidence level with a 5% margin of error. Thus, the ideal sample size was calculated as 384.
A study-specific survey instrument was developed with questions based on published studies about occupational stressors and causes of burnout (Edwards & Dirette, 2010). The construct of professional resilience had not been explored in standardized surveys, thus the intent of the study-specific design was to elicit descriptive statistics about the professional resilience strategies used by practitioners. The strategies included in the 39 questions were based on findings from Ashby et al.’s (2013) study of experienced practitioners in mental health practice. However, questions were not from pre-existing instruments. The questions included focused on identifying the use of the following strategies: a belief in the value of occupational therapy, an informal professional support network, pursuit of career-building opportunities, opportunity for reflection on positive outcomes, opportunity for reflection on professional values, reflection on financial rewards, maintaining an occupation-based focus, personal time management strategies, regular utilizing breaks and vacations, setting boundaries and structure, and formal support from a supervisor or mentor.
Prior to the study, the survey tool was piloted on 10 experienced practitioners to seek feedback on readability and length. The piloting stage resulted in minor changes to the wording of some questions to improve their readability. This resulted in the survey instrument including 39 closed and open-ended questions about: (a) participant demographics, (b) current position, (c) factors shaping professional resilience, and (d) supervision and mentoring. The survey instrument used a range of response options such as tick boxes, 5-point Likert-type scales, and yes/no and open-ended questions. For the purposes of the current analysis, we report on the quantitative data responses.
Data Analysis
Data were used if respondents completed the demographic information and answered more than 50% of all subsequent questions. Demographic data were summarized using descriptive statistics, and percentages were used to report categorical variables such as country, years of practice, specialty, and nature of role. Quantitative responses were further analyzed using IBM SPSS (version 24; SPSS Inc., Armonk, NY: IBM Corp). Pearson chi-square test of independence determined association between country and the use of professional socialization (supervision and mentoring), years worked, and leaving the profession. For any analysis that violated the assumption of Pearson chi-square test of independence, a likelihood ratio was used. Cramer’s V was then used to determine the strength of association with 0 to 0.1 considered weak, 0.11 to 0.3 moderate, and >0.3 strong (Healey, 2015). It is a measure of association between two nominal variables, giving a value between 0 and +1 (inclusive).
Results
Table 1 presents the demographics of the 489 occupational therapists from 29 countries who completed the survey. While 100 responses contained missing data, these surveys were included in the overall analysis if more than 50% of questions were completed. Twelve countries had one respondent, and nine had four or fewer respondents these countries are represented in the results as “other.” Occupational therapists from Australia comprised the largest respondent group by country (46.9%, n = 229) followed by the United Kingdom (n = 112) and the United States (n = 63). Respondents were predominantly female (90.2%, n = 441/489), with a mean of 13.6 (SD, 10.2) years’ experience and the majority had an average of 4.9 occupational roles during their career.
Demographic Information of Respondents.
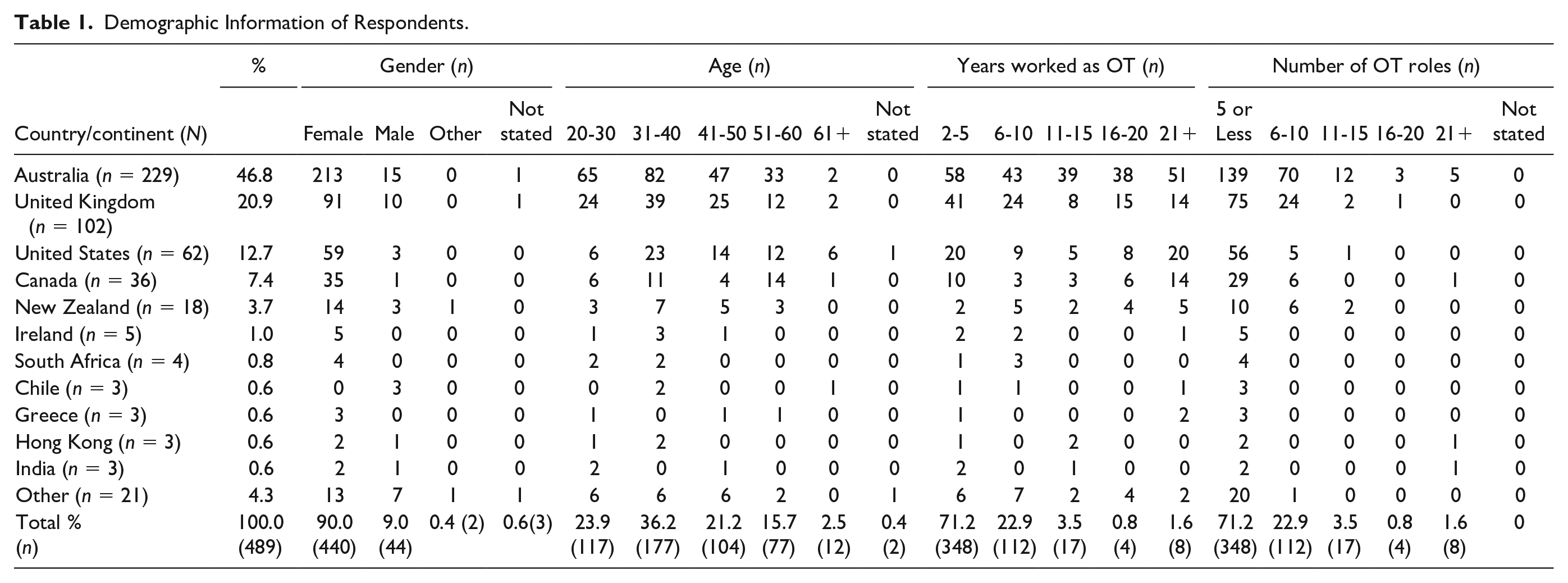
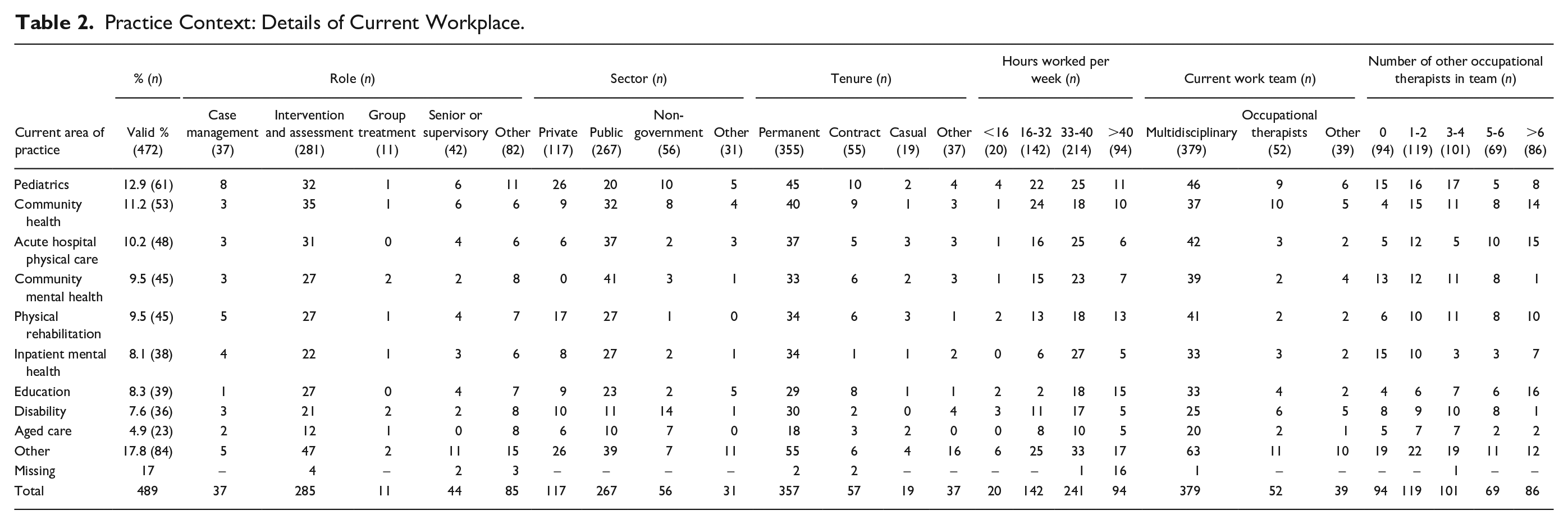
Table 2 presents the respondents’ practice contexts. Due to the scope of current occupational therapy practice, it was not viable to provide categories for all international areas of practice and roles of practitioners, therefore respondents who selected “other” represented the largest group. Pediatrics was the most common current area of practice (n = 61/472, 12.9%), while the smallest sector was aged care (4.9%, n = 23). Most respondents (n = 285/462, 61.7%) identified their current primary role was occupational therapy intervention and assessment. Over half worked in the public sector (n = 267/472, 56.6%). Three quarters (n = 358/471, 76%) of respondents were on permanent tenure. The mean hours worked per week were 35.5 (SD, 10.4), with 19.8% (n = 93/470) working more than 40 hours in an average week. Most worked in a multidisciplinary team (n = 380/471, 80.7%), with at least one other occupational therapist (n = 238/470, 50.6%). In response to the question which asked if respondents had considered leaving the profession, 50.6% (n = 238/470) responded that they had considered leaving the occupational therapy profession. There was a strong association between years worked as an occupational therapist and considering changing profession, C2(3) = 17.0 p < .001. In response to being asked if they had considered leaving the profession, 37.4% who had worked between 2 and 9 years reported that they had considered leaving the profession. This was 37.0% for 10 to 19 years, and there was a reduction to 16.0% in the 20 to 29 years worked group and only 8.8% in the 30+ year group.
Practice Context: Details of Current Workplace.
Workplace Stressors
The experience of common workplace stressors for occupational therapists was measured on Likert-type scales. Overall, the most common stressors respondents agreed with were: “I invest too much energy into my role” (n = 258/451, 57.2%), “there is a lack of occupational therapists in my workplace” (n = 199/451, 44.1%), “I experience pressure to work outside of my domain or role” (n = 191/451, 42.4%). Respondents agreed with the following statements: “I am able to control my workload” (n = 231/452, 51.1%), “I am able to maintain a work/life balance” (n = 276/452, 61.1%), and that “my role is understood by most team members” (n = 332/451, 73.6%).
Professional Resilience Strategies
Table 3 presents the professional resilience strategies used in practice. The most common factors and strategies reported as fostering professional resilience were a supportive home environment (n = 392/452, 86.7%), utilizing breaks and annual leave (n = 340/452, 75.2%), professional socialization (n = 368/452, 81.4%), engaging in professional development (n = 362/452, 80.1%), maintaining professional boundaries (n = 322/452, 71.3%), using time management strategies (n = 373/449, 83.1%), reflecting on positive outcomes (n = 381/452, 84.3%), and financial reward (n = 178/452, 39.4%).
Professional Resilience Strategies.
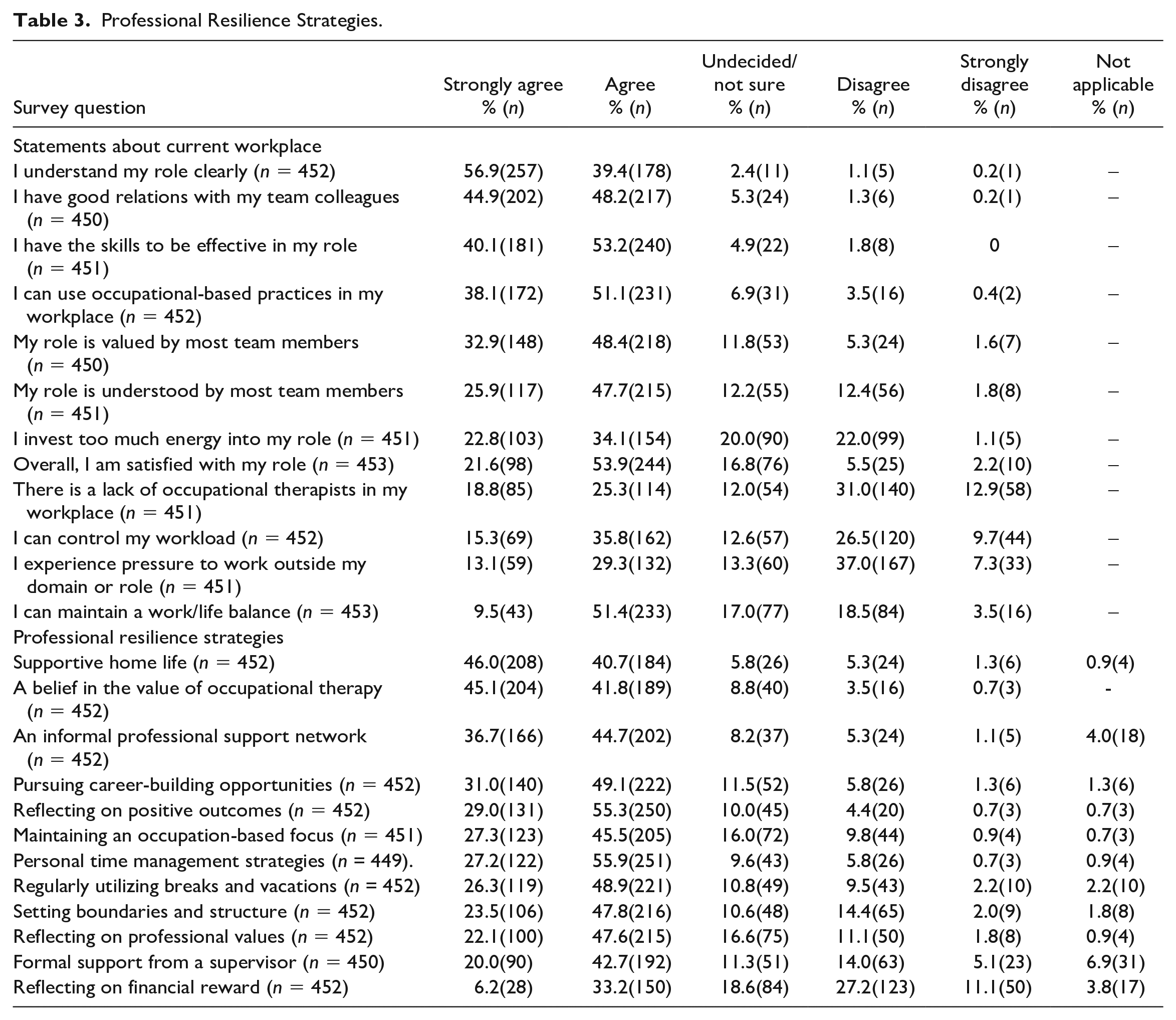
Of the professional resilience strategies used in current workplaces, the largest proportion of respondents (n = 393/452, 86.9%) agreed that “a belief in the value of occupational therapy” mediates work-related stressors, followed by a “supportive home life” (n = 392/452, 86.7%), “reflecting on positive outcomes” (n = 381/452, 84.3%), “personal time management strategies” (n = 373/449, 83.1%), “an informal support network” (n = 368/452, 81.4%), and “pursuing career-building opportunities” (n = 362/452, 80.1%) (see Table 3 for all strategies). In addition, 30% (n = 135) of respondents reported resigning from jobs to avoid burnout.
Professional Supervision and Mentoring
As presented in Table 3, 62.7% (n = 282/450) agreed that formal supervision was a professional resilience strategy that mediated work-related stressors with 86.0% (n = 277/322) agreeing that it was beneficial. Of the 332 respondents who used professional supervision during their career, 72.9% (n = 242) had received supervision within the last 6 months. The reasons provided by the 21.2% (n = 93/450) of respondents who had never accessed professional supervision were primarily that it was not available, or not necessary. There was a significant, strong association between the country of practice and whether professional supervision was received, C2 (5) = 63.9, p < .001. Those who had never used professional supervision were predominantly from Canada (59.4%) and the United States (46.2%).
Of the respondents who reported never utilizing supervision, 40.9% (n = 36/88) stated they had access to mentoring. In contrast, there was no significant association between country and having access to mentoring, C2 (5) = 3.8, p < .58, with 58% (n = 236/407). Of those who accessed mentoring, 70.1% (n = 155/221) reported they utilized it as needed. The majority of respondents (n = 200/218, 91.7%) who reported utilizing mentoring agreed that it was worthwhile.
Discussion
The development of a greater understanding of professional resilience strategies is important for the profession, managers, and those who employ occupational therapists. This study identified experienced occupational therapists draw upon a range of professional strategies in their practice. For those concerned with retention of occupational therapists in the workforce, the study identified that 50.6% of respondents had considered leaving the profession.
The stressors reported by practitioners were similar to those identified in previous studies (Abaoğlu et al., 2021; Katsiana et al., 2021; Porter & Lexén, 2022; Poulsen et al., 2014; Shin et al., 2022; Wressle & Samuelsson, 2014). These stressors included the inability to maintain a work–life balance, a need for excessive investment of effort and energy in work, insufficient numbers of occupational therapists in workplaces, pressures to work outside domain or role, and difficulty managing workloads. While these difficulties remain in workplaces, it is important for the profession to promote the strategies used by practitioners to combat the cumulative impact of these stressors to reduce job dissatisfaction and burnt out (Bolding et al., 2021; Lexén et al., 2021).
The protective professional resilience strategies used by experienced occupational therapists included trying to maintain boundaries, negotiating workload, and taking available breaks and leave. Practitioners also indicated that time management skills were a professional resilience strategy. These findings support Holland et al. (2019) who suggest that human resource management strategies can assist practitioners who work with high clinical caseloads. Teaching strategies such as time management skills in entry-level curricula may enable a more effective transition into professional practice. In addition, it may be useful for employers and professional organizations to provide postgraduate opportunities to develop time management skills.
The study indicates that at practitioner-level strategies which sustain professional resilience are the ability to use occupation-based practice and to reflect on positive client outcomes. Other key strategies were the maintenance of an occupation-focus through ongoing education, intentional use of discipline-specific skills and theory, and skills in advocating for occupation-based practices. This is of particular importance in practice areas such as mental health, where there is often pressure to perform a generic health worker role which inhibits practitioners from engaging in occupation-based practices (Ashby et al., 2015).
Occupational therapists value supportive teamwork. Indeed, previous studies report that practitioners often select positions which have supportive workplace environments, supportive management policies, and responsive, respectful colleagues (Mason & Hennigan, 2019). In turn, the promotion of staff cohesion and positive relationships, which reinforces being a valued team member, are integral to retention of all health care workers (Markey et al., 2021; O’Donovan & Mcauliffe, 2020). For retention rates to improve, it may be necessary for health and social care organizations to adopt recommendations to ensure workplaces provide effective management strategies to create a supportive workplace culture (Opoku et al., 2020). The importance of informal and formal professional socialization with other occupational therapists was also a key professional resilience strategy. This supports other studies which have indicated that the development of strong professional networks within an organization or workplace can improve retention (Ashby et al., 2013; Opoku et al., 2020).
For experienced occupational therapists, leaving a job was identified as a professional resilience strategy. The use of resignation to sustain career longevity is similar to findings from Ashby et al. (2013), where practitioners reported that leaving a job is used as a last resort by practitioners when they perceive they have no agency to change the workplace or have no support from managers to make changes. While practitioners can implement professional strategies, an organizational, managerial approach to rectifying these problems could maintain workforce retention and reduce recruitment costs. Indeed, Opoku et al. (2020) argued that in health and social care improved leadership and validation of discipline roles can reduce the impact of occupational stressors. Furthermore, implementation of training for managers should be a key strategy for those concerned with workforce stability in health and social care. In addition, the findings of the current study indicate that employers seeking to support professional resilience of occupational therapists consider the implementation of strategies that enable, support, and validate evidence-based, occupation-based practices, and reduce the pressure to work outside of professional domains and expertise.
Supervision was utilized by the majority of the practitioners in the current study. However, it is important to note that more than 30% of practitioners did not consider it to be a professional resilience strategy. Of concern was that more than 20% of practitioners in the study reported never receiving supervision. This may reflect that while effective supervision should include time for reflection-on-practice, some workplaces have shifted away from supportive and educational supervision due to increased service pressures, which reduces the restorative aspect of supervision that involves supporting personal well-being (Ashby, 2020). The number of practitioners not utilizing supervision may be problematic as professional socialization and professional supervision support the maintenance of professional identity, assist practitioners to learn and reflect, and build cohesive teams (Ashby, 2020).
Mentoring was accessed by 59.3% of respondents. Doyle et al. (2019) argue that the advantage of mentoring is that it provides practitioners with a perspective from outside of their organization and is a source of advice on long-term career planning. It is a form of professional socialization as it provides validation and support for those not receiving effective supervision, or who work as sole therapists. Indeed, some professional organizations have promoted mentoring for their membership as a means of supporting practitioners in the workforce (Schoen et al., 2021; Wilding et al., 2003). The study indicates that rather than using mentoring and supervision as ongoing restorative strategies, some experienced practitioners may access them when it is perceived as a need, rather than as a regular means of maintaining their professional resilience. This is problematic as Shin et al. (2022) identified that regular supervision can reduce burnout. More research is required into what factors contribute to effective mentoring and supervision as a professional resilience strategy.
Limitations
Professional resilience is an under-investigated area in occupational therapy, which led to the use of a self-developed, study-specific survey. This limited its psychometric properties, including face and construct validity. In addition, it is acknowledged that this is an exploratory international study as the sample size was 489 and that participant responses were shaped by health and social care policies within their country. While online surveys allow recruitment of the greatest number of international participants, it is acknowledged that convenience sampling using social media may have resulted in sampling bias. While the authors accessed members of national professional associations which did not require the authors’ formal membership, or payments this limited recruitment from countries where professional associations required membership or payments. It is also acknowledged that although practitioners from 29 countries responded, participation was limited because the survey tool was only available in English. This limits the representation of non-English-speaking practitioners. These limitations mean that the findings are skewed to reflect practice issues in English-speaking countries.
Conclusion
The study provides a greater understanding of the professional strategies used by experienced occupational therapists to foster and maintain their professional resilience. While health and social care workplaces inherently include occupational stressors, implementation of professional resilience strategies at service level, practitioner level, and education level may assist in mitigating stressors. For employers, losing experienced occupational therapists creates instability in the work force, creates costs in recruitment for organizations, and leads to a lack of experienced practitioners to supervise graduates. The promotion of effective workplace professional resilience strategies may assist in sustaining workforce retention.
The study indicates that employer-level strategies can include responsive management, promotion of occupational therapy, provision of breaks and vacations, access to education and professional development, and prioritization of professional supervision. Practitioner-level strategies include setting clear workload boundaries, fostering professional identity through socialization, extending knowledge of how to assertively argue for occupation-based practices, improving time management strategies, maintaining occupation-based personal paradigms seeking effective supervisors who support reflective practice, and by accessing mentors who can provide support and advice on occupation-based practice development. At an educational level, entry-level and postgraduate curricula can provide practitioners with foundational skills for the development of professional identity and curation of professional resilience strategies. National professional associations for occupational therapists can also foster training and educational options, which nourish professional resilience by expanding knowledge on how to sustain professional identify through occupation-based practices.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
Ethical approval was provided by the University of Newcastle Human Research Ethics Committee (H-2017-0041).
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
