Abstract
Bacillus Calmette-Guerin (BCG) therapy for treatment of bladder cancer is a rare cause of Mycobacterium bovis infected aortic aneurysm. Typical presentations have included general malaise, fever, and lower back pain. We present a case with lower back pain and constipation as presenting symptoms, leading to diagnosis of mycotic aneurysm presumed secondary to intravesical BCG therapy. Treatment included open surgical repair with femoral vein grafting and anti-tubercular therapy. This case highlights the importance of a high index of suspicion for less common infectious complications of BCG therapy.
Introduction
Bladder cancer is the fifth most common type of cancer in Canada. 1 Bacillus Calmette-Guerin (BCG) immunotherapy has been a treatment for high-and intermediate-risk non-muscle invasive bladder cancer and has been shown to reduce rates of recurrence and progression of disease. 2 BCG acts by activating the immune system against bladder cancer cells. 3 Adverse effects include lower urinary tract symptoms, flu-like symptoms, inflammation of the genitourinary system, and rarely, BCG infection, with abscess occurring in less than 2% of cases and sepsis occurring in less than 1%. 4 Caution is recommended in patients with known aneurysms or prosthetic devices as they are at higher risk of infection. 4
Mycotic aneurysm is an exceedingly rare complication of BCG therapy, which may lead to delays in diagnosis or in recognizing the causative organism, delaying adequate intervention. We present a case of mycotic abdominal aortic aneurysm secondary to BCG treatment in the absence of prior aortic aneurysm.
Case
We present a 57-year-old male with non-invasive high-grade urothelial carcinoma of the bladder. Treatment consisted of transurethral resection and gemcitabine instillation, BCG immunotherapy and regular surveillance cystoscopies showing no disease recurrence. 6 months prior to presentation a computed tomography (CT) intravenous pyelogram demonstrated no evidence of abdominal aortic aneurysm.
The patient presented to the emergency department 6 months after initiating BCG treatment with 6 weeks of persistent lower back pain and 2 weeks of constipation. Physical examination and laboratory investigations were normal. His diagnosis at discharge was mechanical back pain aggravated by constipation.
The following week he presented with abdominal and back pain, loose stools, and 1 day of fever. Loose stools were attributed to laxative use. X-rays of the chest, back, and abdomen were normal. He was advised to seek physiotherapy. 2 weeks later he presented with constipation, abdominal cramps, and back pain. He was discharged with constipation therapy. At these re-presentations physical exam and bloodwork were normal. Following subsequent outpatient follow-up, a non-contrast CT abdomen/pelvis showed new retroperitoneal lymphadenopathy and a suspected soft tissue mass that was partially encasing the aorta. A contrast-enhanced CT scan performed two weeks later to better characterize the mass then identified a 5.8 cm mycotic aneurysm of the abdominal aorta (Figure 1). The patient was clinically stable and promptly admitted. Blood cultures for typical pathogens and Mycobacterium were sent. Coronal (A.), sagittal (B.), and transverse (C.) sections of contrast computed tomography angiogram abdomen/pelvis showing Saccular aneurysm arising from the right anterolateral aspect of the infrarenal abdominal aorta measures 1.3 × 1.3 cm and extensive adjacent soft tissue thickening which encases the aorta and abuts the IVC measuring 7.1 × 4.4 cm.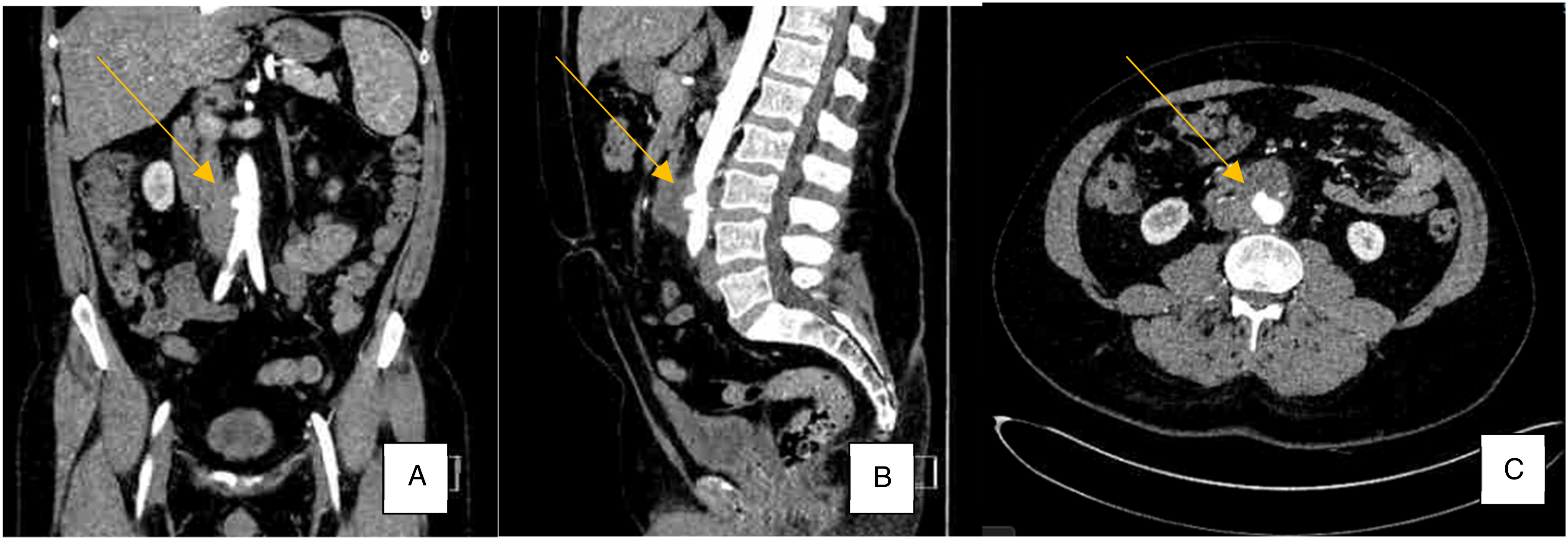
The patient underwent open repair with reversed femoral vein graft harvested from the right limb from above the knee to the juncture with the deep femoral vein performed with a second set of sterile instruments. The aortic bifurcation was not a suitable endpoint and therefore an aortic to right common iliac bypass was performed followed by re-implantation of the left common iliac onto the vein graft. The field was irrigated with bacitracin, vancomycin and rifampin. Aortic and retroperitoneal tissue was debrided of infected and devitalized tissue. The right leg was wrapped with a tensor bandage which was maintained until he was mobilizing. He recovered on the cardiovascular intensive care unit for 24 h and was discharged on post-operative day 7. In hospital the patient was maintained on ASA 81 mg daily and twice daily 5000U subcutaneous heparin for deep vein thrombosis (DVT) prophylaxis.
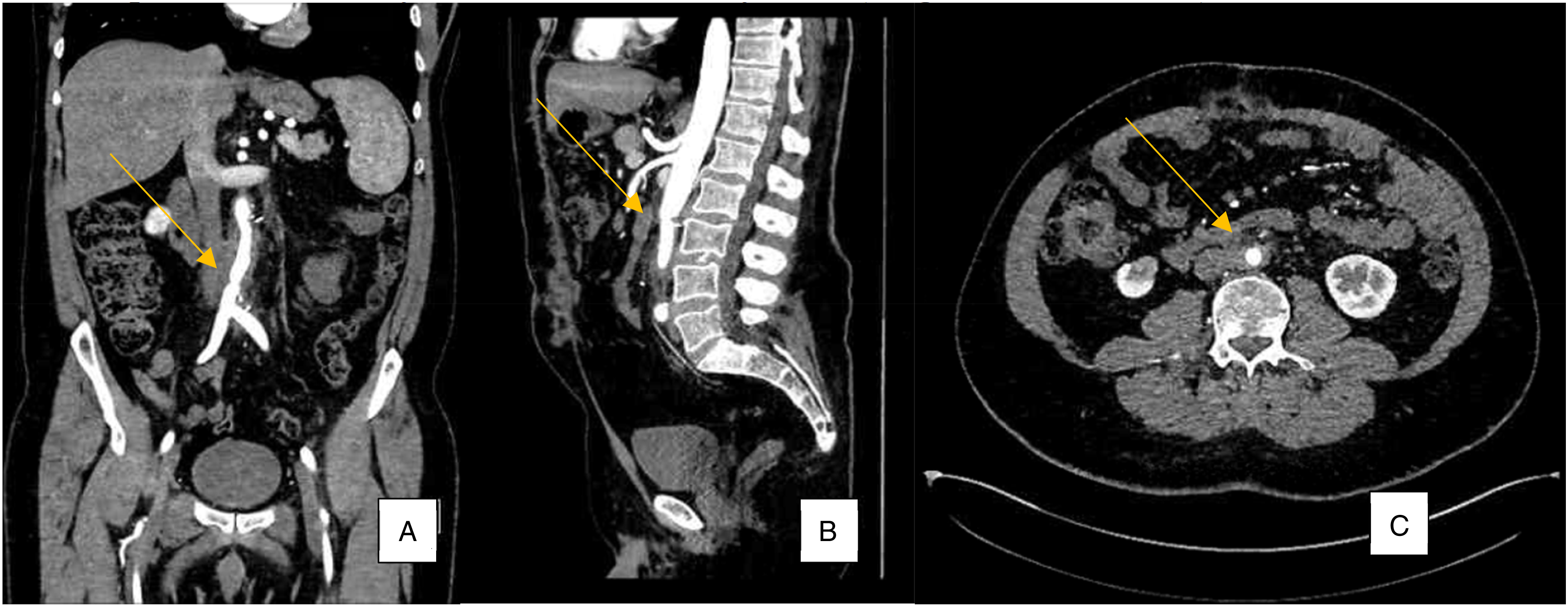
Tissue pathology showed vegetation with fibrin, epithelioid macrophages, giant cells, polymorphs, lymphocytes, and plasma cells (Figure 2). Cultures were sent for Gram and acid-fast bacillus (AFB) stains. Urine mycobacterial cultures were smear positive for AFB. Tissue culture returned positive for M. bovis confirming the mycotic aortic aneurysm was secondary to BCG immunotherapy. He was treated with isoniazid 300 mg daily, rifampin 600 mg daily, and ethambutol 1600 mg daily. At 3 months he was admitted due to peripheral neuropathy and optic neuritis believed secondary to his isoniazid and ethambutol therapy. Antituberculosis therapy was stopped. During this admission an asymptomatic DVT was discovered in the right leg after a small pulmonary embolism was noted incidentally on CT chest. He was started on Apixaban for 3 months followed by lifelong ASA. He never clinically had symptoms of DVT or venous insufficiency and remains symptom free at 6 months. CTA at 1, 3 and 6 months post-op demonstrates intact repair with no evidence of recurrence (Figure 3). Hematoxylin and eosin-stained section of aorta showing intimal vegetation composed of fibrin, epithelioid histiocytes and inflammatory cells (magnification ×400). Coronal (A.), sagittal (B.), and transverse (C.) sections of contrast computed tomography angiogram abdomen/pelvis taken 3 months post-aneurysm repair showing an intact repair.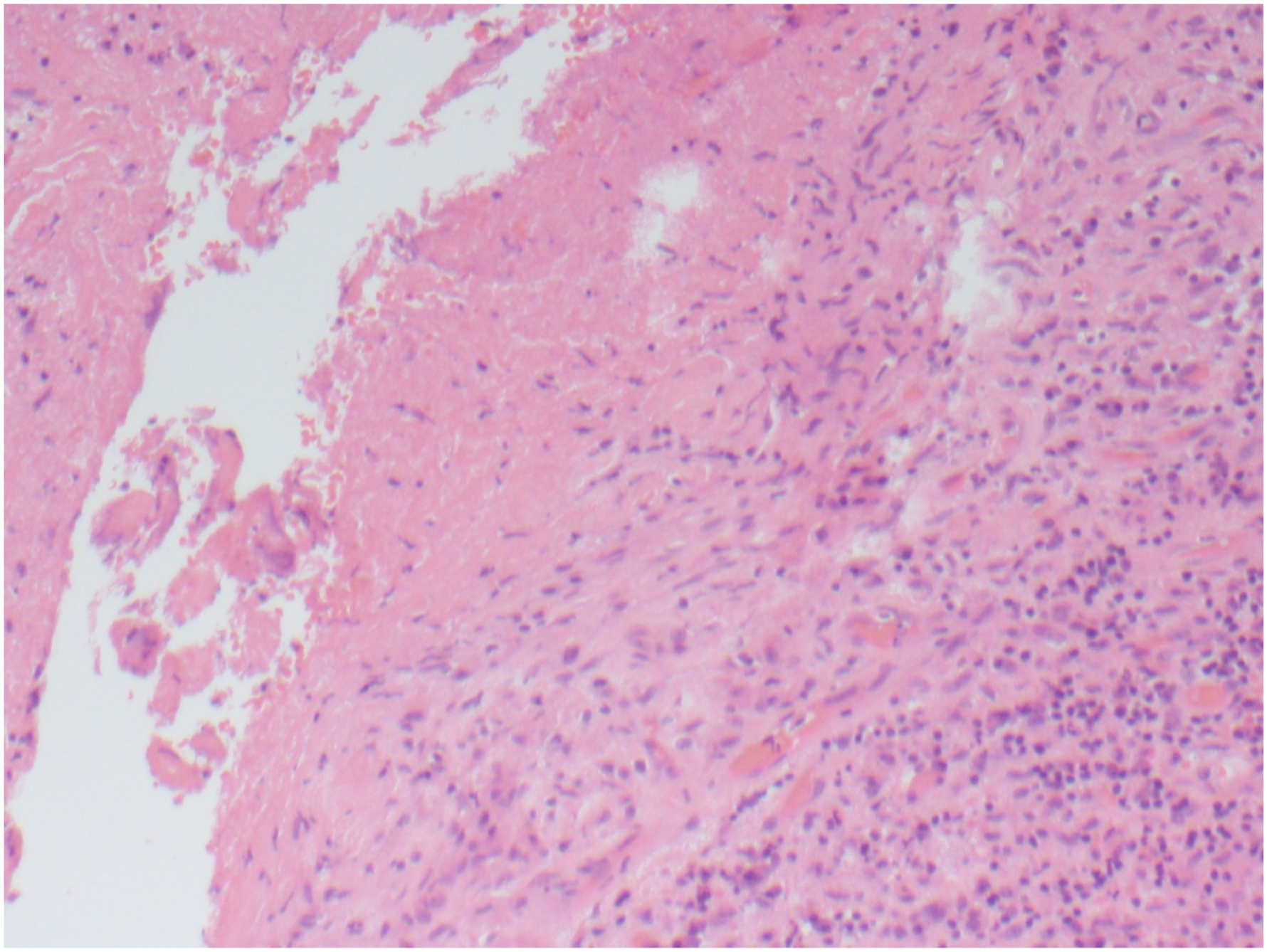
Discussion
BCG is a live attenuated strain of Mycobacterium bovis that is related to Mycobacterium tuberculosis. Complications related to BCG immunotherapy including sepsis, pneumonitis, hepatitis, vasculitis, or infected aneurysm are uncommon and typically present with fever, chills, and malaise following traumatic catheterization, bladder perforation, or premature administration post-transurethral resection. 4
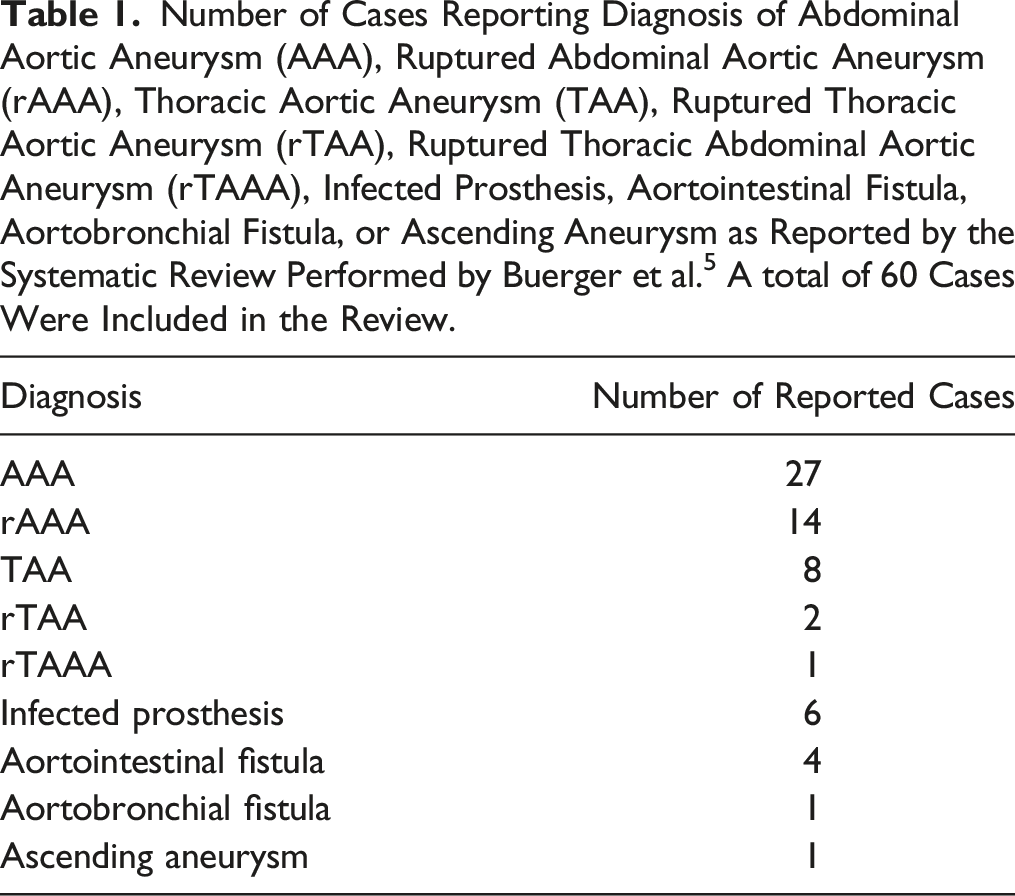
Number of Cases Reporting Diagnosis of Abdominal Aortic Aneurysm (AAA), Ruptured Abdominal Aortic Aneurysm (rAAA), Thoracic Aortic Aneurysm (TAA), Ruptured Thoracic Aortic Aneurysm (rTAA), Ruptured Thoracic Abdominal Aortic Aneurysm (rTAAA), Infected Prosthesis, Aortointestinal Fistula, Aortobronchial Fistula, or Ascending Aneurysm as Reported by the Systematic Review Performed by Buerger et al. 5 A total of 60 Cases Were Included in the Review.
Number of Cases for Each Method of Surgical Management in Treatment of Mycotic Aneurysms Infected with M. bovis Following BCG Treatment as Reported by the Systematic Review Performed by Buerger et al 5 . A Total of 60 Cases Were Included in the Review. Methods Included: Thoracic Endovascular Aortic Repair (TEVAR), Open Aortic Repair (OAR), in-situ Repair (ISR), Ea-Anatomical Repair (EAR), Endovascular Aortic Repair (EVAR), Debridement, Prosthesis Implantation, Aneurysm Resection and Bypass Repairs.

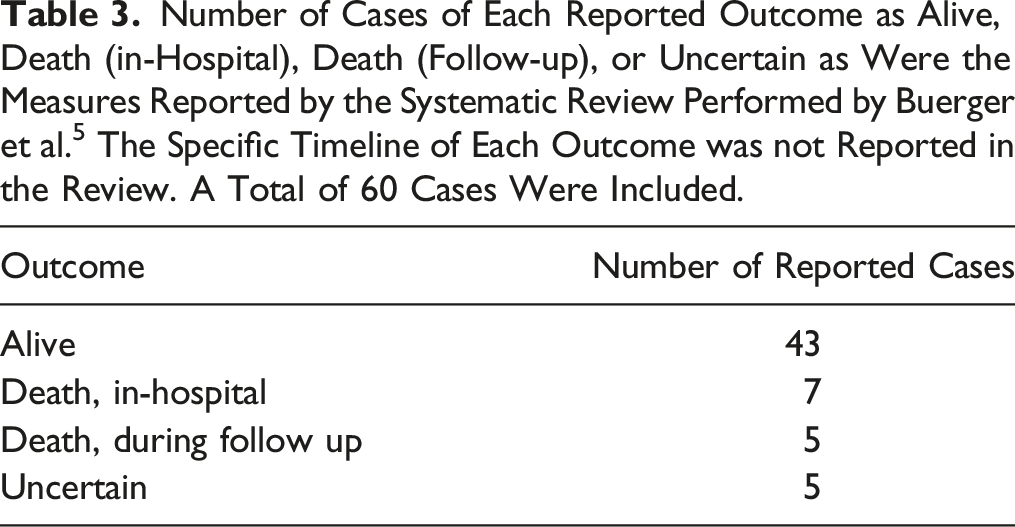
Number of Cases of Each Reported Outcome as Alive, Death (in-Hospital), Death (Follow-up), or Uncertain as Were the Measures Reported by the Systematic Review Performed by Buerger et al. 5 The Specific Timeline of Each Outcome was not Reported in the Review. A Total of 60 Cases Were Included.

Definitive treatment of mycotic aneurysm generally involves open surgical repair with extra-anatomic reconstruction or in-situ repair, using a rifampin soaked prosthetic or biologic graft followed by anti-tubercular therapy. 5 Endovascular repair has been reported but is associated with a high recurrence rate (61%) and is usually reserved for those unfit for open reconstruction. 7 Due to our patients young age, good health and clinical stability we performed an in-situ reconstruction with a femoral vein graft. We believe this is the most durable approach in physiologically suitable patients. Prosthetic grafts have a risk of reinfection and extra-anatomic bypass has a risk of long-term failure in a young patient. Recurrent infection is possible following alloplastic repair (25%) though femoral vein may be less prone to infection than other biologics. 6 Despite an incidental DVT secondary to hospitalization, at 6 months postoperatively this patient had no symptoms associated with the vein harvest. Subsequent surveillance CTA in our patient demonstrated no sign of recurrent infection at 6 months. Imaging will be repeated at 1 year post-op.
Mycotic aortic aneurysm is a rare but serious complication of BCG immunotherapy. This report adds to the literature of reported M. bovis infection following BCG therapy and highlights the importance of further investigation of atypical presentations in those who have undergone BCG therapy.
Conclusion
Mycotic aneurysm infected with M. bovis is a rare complication of BCG therapy for bladder cancer. In this case, diagnosis required multiple presentations before receiving appropriate investigations and interventions, as symptoms were initially attributed to constipation. Treatment consisted of an open femoral vein autograft and anti-tubercular therapy.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
Island Health’s policy about case studies does not require formal human research ethics review when the cases are two or less. Therefore, this project was exempt from REB review. Appropriate consultation with the Research Ethics and Compliance office and attention to privacy and confidentiality requirements were upheld.
Informed Consent
Verbal consent from the patient was obtained and documented in the clinic note from by Dr Linda Lee.
