Abstract
The Unites States healthcare system is a patchwork, and patients, caregivers, and healthcare providers must craft individual solutions to cope with gaps in the system. Sociological thinking is crucial for forming healthcare systems that provide high-quality care, control cost, and increase access without inheriting the flaws of existing systems. Recent work to develop a “social science of solutions” provides both motivation and a roadmap for progress-oriented work toward redressing social problems and building real utopias. Collaborative Learning Health Systems may be a model for real utopias in healthcare, but they must balance their potential with risks as they grow.
The US healthcare system is a complex social ecology of stakeholders who shape the possibilities of how medical care can be accessed, provided, and funded. By its patchwork nature, our healthcare system produces gaps, and patients, caregivers, and healthcare providers must craft individual solutions to cope with these systemic problems. Creative thinking and skillful political mobilization are crucial for forming healthcare systems that provide high-quality care, control cost, and increase access. While there is no magic fix, the sociological imagination helps us see how we might pursue more just and equitable societies by creatively reimagining healthcare.
A key insight of the sociological imagination is that the status quo could be different—historicizing the present allows us to see that current conditions are not inevitable. In recent years, there have been several calls for a “social science of solutions,” promoting a vision of social science that balances theoretical advancement with progress-oriented work toward redressing social problems. In 2020, calls for a social science of solutions became more urgent as COVID-19 exposed the weaknesses of social institutions. Speaking in the context of educational inequality and the pandemic, Spencer Foundation President Na’ilah Suad Nasir asked, “How do we push systems to experiment with what those new kinds of equitable pathways, institutions, and organizations might look like?”
Erik Olin Wright developed the notion of real Utopias as one way to reimagine familiar social institutions. Wright defined real utopias as “viable, emancipatory alternatives to dominant institutions and social structures.” Wright described Wikipedia as an example of this approach because of its open and collaborative process for compiling encyclopedic knowledge. Wikipedia has already realized a level of community-governed productivity that would not have been imaginable before it was founded. However, Wright points out: “There are no guarantees. That’s precisely why we need serious sociological study of real utopias, rather than fantasy utopias.” Drawing on the real utopias framework might allow us to build a social science of solutions for a wide range of institutions, including healthcare.
A Social Science of Solutions for Healthcare
Real utopias often begin as a departure from the conventional wisdom of how a social institution works, allowing people to begin to imagine different alternatives and try them out in real life. The conventional wisdom of healthcare in the United States has largely been based on a faith in scientific progress to bring ever more effective medical treatments for disease and a positioning of physicians as having the best expertise to address illness. While scientific progress has been astounding, particularly in the last 100 years, this conventional wisdom tends to lead us to medicalization, medical paternalism, and the centering of biomedical ways of knowing. What might a real utopia of healthcare look like?
Over the past 15 years, a multi-stakeholder group of healthcare providers, researchers, patients and families, advocacy groups, and quality improvement specialists has rallied around this question: what if there were a better way to organize healthcare? By tracking health outcomes, including quality of life, as well as organizational processes, these groups have brought the vision of the Learning Health System into practice.
What is a Learning Health System?
A Learning Health System is a continuously “learning” system where members systematically gather data about healthcare provision and the health status of patients and use these data to plan and implement individual- and system-level changes to improve health outcomes. This vision, which the National Academy of Medicine has endorsed since 2007, is being taken up in health systems in the United States and beyond.
The status quo of American healthcare could be different; current conditions are not inevitable.
Pixabay
The conventional wisdom of healthcare in the United States includes a positioning of physicians as having the best expertise to address illness.
Vidal Balielo Jr. via Pexels
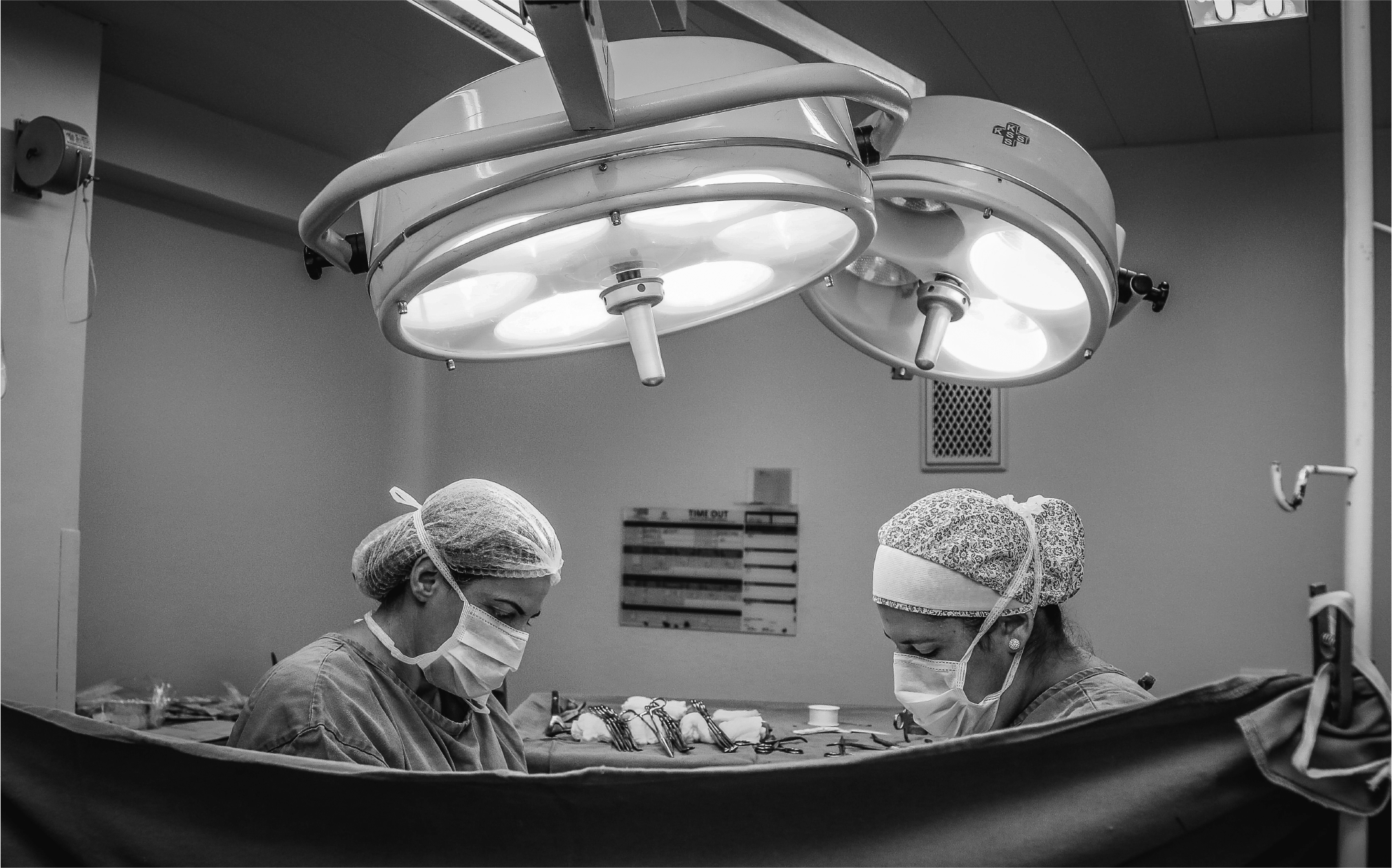
The underlying notion of the Learning Health System is that the everyday activity of healthcare delivery and research produces an unfathomable amount of data that are not effectively used to understand and improve the health outcomes of patients or the performance of healthcare systems. While many clinical research findings are shared in scholarly outlets, the results take a very long time to be implemented in the actual delivery of care. In fact, consensus among researchers in the field is that it takes 17 years for research findings to be implemented as changes in the standard of care. To remedy this, the vision of the Learning Health System is to create a closed-loop system. At an abstract level, this means that the findings from clinical research can be fed back into the healthcare system as actionable information for healthcare providers. As the feedback loop is closed, participants in the system can make the healthcare system “learn” by, for example, changing treatment recommendations based on research insights. The participants in the system can also learn directly—providers and patients can monitor the patient’s health status over time using data that are available in a registry or integrated into the electronic health record. Providers and institutions can receive feedback on their performance, like whether treatment changes impact patient outcomes. They can also receive feedback on process improvements, such as reducing time to treatment and error rates.
Some Learning Health Systems focus primarily on improving the use of data to help providers optimize treatments. But another vision of the Learning Health System is to have improvement initiatives follow the priorities of multi-stakeholder communities that self-organize around “shared problems of interest,” such as improving health outcomes for people living with a particular health condition. In these groups, collaboration is foregrounded, and so they are called Collaborative Learning Health Systems. The members of Collaborative Learning Health Systems are patients, families, healthcare providers, researchers, and community and advocacy organizations. Group members work in a concerted way to identify relevant data that are collected during the routine course of care. They also collect new data to understand and improve health and healthcare processes impacting their desired outcomes. As these groups form and grow, members benefit from skilled coaching by quality improvement specialists, program managers, and data scientists. The community “owns” the system and decides what data to collect and what initiatives to pursue. This requires a reimagining of governance and an alignment of priorities that can shake up some of the established relations between stakeholders. As a local intervention, the Collaborative Learning Health System is not a fix-all for the problems of the US healthcare system. Still, this model does offer an alternative to the status quo that could be cultivated and spread.
Can We Create a Real Utopia with Collaborative Learning Health Systems?
Creating real utopias depends on imagining different futures and testing good ideas in a spirit of experimentalism. This work happens best in community, so I want to focus especially on Collaborative Learning Health Systems. In these networks, members work together to identify ideas that might “move the needle” on health outcomes and then try them to see if they work. Their learning is gradual, inductive, and organized around a consensually chosen “shared problem of interest.” These groups can use targeted data collection and iterative plan-do-study-act (PDSA) cycles to understand if changes in practice produce actual improvements.
The Collaborative Learning Health System model is gathering evidence to support this approach. Gradually, groups are finding that employing an approach focused on achieving stakeholder alignment, using purposive data collection to establish the baseline state of the system, and using quality improvement methodology to implement interventions can make a meaningful difference in patient outcomes. For example, ImproveCareNow, a multi-stakeholder network focused on improving outcomes for children and young adults with Crohn’s disease and ulcerative colitis, had achieved 82% remission rates as of 2020, with 57% of enrolled patients at participating centers having achieved remission for more than one year. Members of the Epilepsy Learning Healthcare System demonstrated that their newly implemented seizure documentation practices were able to be sustained despite the transition to telemedicine care at the beginning of the COVID-19 pandemic. And as part of a broader initiative to reduce preterm births, the Ohio Perinatal Quality Collaborative was able to use quality improvement approaches to reduce the number of scheduled births before 39 weeks without a documented medical reason.
The wonderful thing about real utopias is that even the mere act of imagining a different future can call conventional wisdom into question and prepare groups for social and structural change. In the case of the Collaborative Learning Health System model, its growth and development hinge on balancing its revolutionary potential against the risks that become salient as this new model takes shape in the world.
Collaborative Learning Health Systems Elevate Patients as Agenda-Setters
Because Collaborative Learning Health Systems are designed to invite diverse stakeholders to the table and give them robust agenda-setting power, they have tremendous potential to shift entrenched power relations in healthcare. For example, if a group takes up the issue of improving quality of life for people with a health condition, then people with that health condition are centered in figuring out where to begin this work. Because those with lived experience participate in setting the agenda for what problems the group will focus on, this fundamentally shifts whose expertise is considered most relevant and can be a revolutionary experience for group members. These transformations may also pave the way for the recognition of expertise of a wider range of healthcare providers, especially pertinent as advanced practice providers like nurse practitioners and physician assistants become increasingly integral to healthcare delivery.
However, it is one thing to have representatives from all stakeholder groups at the table and quite another to have the representatives actually reflect the needs and experiences of the group they are representing. Removing barriers to participation is a key challenge for Collaborative Learning Health Systems as they develop. In addition, it is not always evident how to align stakeholder priorities and adopt a new culture that can support reimagined social relations. Here, sociologists, who have a wealth of expertise in describing the broader context of organizational processes and culture, can contribute to helping Collaborative Learning Health Systems build social structures that help them achieve their goals.
Over the past 15 years, a multi-stakeholder group of healthcare providers, researchers, patients and families, advocacy groups, and quality improvement specialists has rallied around this question: what if there were a better way to organize healthcare?
Collaborative Learning Health Systems Use Data and Strategy to Identify Effective Interventions
Collaborative Learning Health Systems aim to reduce unintended variation in healthcare so that less is left up to chance when patients seek care. This can be accomplished by analyzing data collected from the electronic health record and returning the results to providers in easily digestible forms, such as graphs of patient and population health outcomes over time. The data and graphs are discussed frequently at stakeholder gatherings and can help stakeholders understand which healthcare interventions are effective and which are not. Thus, unlike other ways of using clinical data, such as for rankings, accreditation, or legal reasons, in Collaborative Learning Health Systems, data are used for learning together to achieve a shared goal.
Aggregating data into purpose-built registries often grants insight into patient and population health status. These registries can receive data collected during the routine course of care, as well as data collected purposively by the Collaborative Learning Health System’s stakeholders. These data can inform the care of individual patients, track the health status of patient populations, and can also help stakeholders understand the quality of the data in their registry. Using the framework developed by scholars Rob Kitchin and Tracey Lauriault, this type of data aggregation is best understood as “small data” rather than “big data” because they are collected with the purpose of answering specific questions. However, even small data aggregation brings new challenges to Learning Health Systems. For example, one challenge is that stakeholders must develop novel practices of data sharing and establish new norms that accompany these practices. Another is that as Collaborative Learning Health Systems grow, they become large data repositories that may contain not only clinical data but also patient-reported outcomes, quality of life data, and data passively collected from wearable devices or smartphones. Patient data may be an attractive commodity for a funder, and the patients themselves may become desirable as a population of potential clinical trial participants. These new understandings of patients and their data may require Collaborative Learning Health Systems to make difficult choices about granting access to their databases or patient populations.
In the context of the COVID-19 pandemic, calls for a social science of solutions became ever more urgent.
Anna Shvets via Pexels

Here sociologists can contribute uniquely to helping Collaborative Learning Health Systems think through their data collection and use. Thus far, Collaborative Learning Health Systems have tended to avoid pitfalls of data use highlighted by scholars such as Virginia Eubanks, since they typically use small data to describe the baseline state of a system and pursue quality improvement interventions, rather than aggregating data to produce predictive analytics such as risk scores. However, sociologists such as Safiya Noble have described the subtle ways in which technologies can incorporate the biases of their architects and users, effectively re-inscribing bias through a seemingly neutral technological interface. Currently, discussions of data quality in Learning Health Systems tend to focus on completeness and standardization. Still, bias should also be considered as a factor shaping what data are collected and how. Discussions must also anticipate the consequences of data aggregation, as potential biases from contributing data sources are inevitably aggregated along with the data themselves.
Building a Learning Health System Can Be a Source of Professional & Personal Purpose
Collaborative Learning Health Systems promote an emotional connection to healthcare improvement work, and many participants see this work as purposeful and meaningful. However, this emotional connection can lead participants to overwork and take on uncompensated work. Especially when healthcare work conditions have been creating burnout even before the onset of the COVID-19 pandemic, it is important that new healthcare models do not reproduce these conditions. A better way forward is to build a Learning Health System that is structurally resistant to burnout—by attending to the amount of work each person is asked to accomplish, whether that work is fairly paid, and whether that work has enough novelty, enjoyment, and purpose.
Learning Health Systems Grow Out of Existing Healthcare Systems
A related challenge is that a Learning Health System grows out of, or alongside, an established health system or medical center. The established organizational processes of the health system can constrain the growth of Learning Health Systems. Effortful engagement is thus required to reshape organizational processes to accommodate new ways of providing healthcare. However, the Learning Health System may have positive potential for reducing our sense of individual medical centers as walled gardens by creating, for example, extra-organizational data repositories that link stakeholders in a Learning Health System that spans organizational boundaries.
As these examples highlight, the Learning Health System is designed to construct an alternative cultural and information technology infrastructure to conventional healthcare organizations in order to systematically improve health outcomes. However, built without care, the Learning Health System can inherit and reproduce the limitations of current healthcare systems.
Looking Forward
In highlighting these aspects of Learning Health Systems, and particularly Collaborative Learning Health Systems, I hope to convey the potential of this new way of organizing healthcare delivery and continuous improvement. These systems are important sites for real structural change. As Learning Health Systems grow and evolve, we will see the continued expansion of this model into new patient populations. Moreover, the Learning Health System approach may also be used to understand the role of social determinants of health, moving beyond understandings of individual medical factors in patient outcomes. This may, in turn, help researchers understand how to build “learning” infrastructures in non-medical settings to help address other social problems.
Learning Health Systems systematically gather data about healthcare provision and the health status of patients and use these data to plan and implement changes to improve health outcomes.
cottonbro via Pexels

Beyond the Learning Health System lie more fundamental questions about the future of US healthcare: should we pursue national reform, reviving discussions about a single-payer option or a single-payer system? How will the increasing numbers of advanced practice providers like nurse practitioners and physician assistants change access to healthcare and the composition of the healthcare workforce? How will the ongoing pandemic change healthcare delivery, the healthcare workforce’s well-being, and patients’ access to treatment? These questions about the healthcare system unfold against an even broader backdrop of social change: the COVID-19 pandemic, serious questions about the future of American democracy, and struggles for racial, gender, and reproductive justice.
Momentum is building around social science work that blends the intellectual projects of theory-building and promoting change through partnership with communities. A current of emancipatory thought animates a “social science of solutions,” where sociological insights help us construct alternative forms for familiar social institutions. A social science of solutions approach reminds us that a fundamental orientation of sociology is toward uncovering how current social structures and relations got to be how they are. This insight reminds us that the status quo is not an inevitability. With creative thought and action we can pursue more just and equitable societies. Some might dismiss this as an unachievable aim, but sociologist Erik Olin Wright’s work reminds us that there have always been groups of people working together for positive change—what Wright has described as a real utopia. Real utopias are spaces that have been carved out through will and creativity in the service of creating a more just world. A social science of solutions promotes the identification and support of new organizational, institutional, and relational forms that aim to fulfill the promises of social change.
Footnotes
Acknowledgements
This research was supported by a Patient-Centered Outcomes Research Institute (PCORI) Award (RI- LHS-2018-001). The statements in this publication are solely the responsibility of the author and do not necessarily represent the views of the Patient-Centered Outcomes Research Institute (PCORI), its Board of Governors, or Methodology Committee.
Data Accessibility
Due to agreements with research participants, the data associated with this research are not available for third-party access.
