Abstract
Purpose:
The aims of the study were to develop and evaluate a novel residualizing peptide for labeling internalizing antibodies with 124I to support clinical development using immuno-positron emission tomography (PET).
Methods:
The anti-epidermal growth factor receptor antibody ch806 was radiolabeled directly or indirectly with isotopes and various residualizing peptides. Azido-derivatized radiolabeled peptides were conjugated to dibenzylcyclooctyne-derivatized ch806 antibody via click chemistry. The radiochemical purities, antigen-expressing U87MG.de2-7 human glioblastoma cell-binding properties, and targeting of xenografts at 72 hours post injection of all radioconjugates were compared. Biodistribution of 124I-PEG4-tptddYddtpt-ch806 and immuno-PET imaging were evaluated in tumor-bearing mice.
Results:
Biodistribution studies using xenografts at 72 hours post injection showed that 131I-PEG4-tptddYddtpt-ch806 tumor uptake was similar to 111In-CHX-A″-DTPA-ch806. 125I-PEG4-tptddyddtpt-ch806 showed a lower tumor uptake value but higher than directly labeled 125I-ch806. 124I-PEG4-tptddYddtpt-ch806 was produced at 23% labeling efficiency, 98% radiochemical purity, 25.9 MBq/mg specific activity, and 64% cell binding in the presence of antigen excess. Tumor uptake for 124I-PEG4-tptddYddtpt-ch806 was similar to 111In-CHX-A″-DTPA-ch806. High-resolution immuno-PET/magnetic resonance imaging of tumors showed good correlation with biodistribution data.
Conclusions:
The mixed
Introduction
Monoclonal antibodies and antibody drug conjugates are now playing an important role in the management of patients with cancer. 1,2 In order to aid clinical antibody development, the development of immuno-SPECT and immuno-positron emission tomography (PET) reagents can provide a noninvasive technique to aid in patient selection for antibody therapy either by confirming the presence of antibody binding to multiple tumor lesions or by determining the delivered radiation dose in patients planned for radioimmunotherapy. 3 –5
The epidermal growth factor receptor (EGFR) belongs to the ErbB/HER tyrosine kinase receptor family, which consists of 4 receptors (HER1-4). Overexpression of EGFR during tumorigenesis has been associated with many epithelial cancers, correlating with poor disease progression and poor clinical outcome, and makes this receptor an attractive target for therapeutic antibodies. 6,7 One of the EGFR-targeting antibodies that is currently undergoing clinical development, 806, is able to distinguish tumor cells with an amplified/overexpressed EGFR phenotype from normal cells having wild-type levels of EGFR expression and also targets a truncated form of EGFR (EGFRvIII). 8,9 The EGFR is internalized following ligand binding or antibody binding. 9
Immuno-SPECT reagents, 125I- and 111In-CHX-A″-DTPA-labeled chimeric 806 (ch806) 10 , and more recently, 124I-IMP-R4-ch806 for immuno-PET, 11 have been developed and characterized. Both 111In-CHX-A″-DTPA- and 124I-IMP-R4-ch806 showed good tumor uptake and tumor retention in tumor-bearing mice, while 125I-ch806 showed reduced tumor uptake and retention, most likely due to the rapid diffusion of radioiodinated catabolites out of the lysosomes. Excellent tumor uptake of 111In-CHX-A″-DTPA-ch806 was also evident in patients entered into a Phase I clinical trial, and more recently ABT-806i (111In-labeled humanized ABT-806, formerly mAb806) has been successfully explored in a Phase I trial. 12,13 Because of its higher spatial resolution, better signal-to-noise ratio, and straightforward data quantification, the development of a clinically suitable immuno-PET radiopharmaceutical to aid clinical development of 806 is preferable. 5
A large proportion of anticancer monoclonal antibodies are internalized after binding to cell surface antigens and translocated to lysosomes where proteolytic digestion occurs.
14,15
When such antibodies are labeled directly with radiohalogens such as 124I via endogenous tyrosine residues, resultant radiocatabolites diffuse out of the lysosomes, resulting in reduced overall uptake and retention in tumors. Various residualizing ligands for radioiodination, including nonmetabolizable carbohydrate–tyramine adducts,
16
–21
aromatic acylation agents bearing substituents that will remain charged at lysosomal pH,
22
–24
short
The goal of this study was to design and evaluate novel peptides for residualizing radioiodine labeling based on the observation that flanking a pentapeptide with 3

Schematic diagram indicating conjugation of radiolabeled azide-derivatized residualizing peptide to a DBCO-derivatized antibody via click chemistry. DBCO indicates dibenzylcyclooctyne.
Materials and Methods
All analytical grade reagents, except when stated, were obtained from Merck Pty Ltd (Melbourne, Australia). 125I and 131I in 0.02 N NaOH were purchased from PerkinElmer (Sydney, Australia). 111In in 0.01 N HCl was purchased from Mallinckrodt (Sydney, Australia). 124I in 0.02 N NaOH (>10 mCi/mL) was prepared in house by the Austin Cyclotron (Heidelberg, Australia). Radioactivity was measured either with a dose calibrator (Biodex Atomlab-100; Brookhaven, New York) or Wizard gamma counter (PerkinElmer) with appropriate settings.
Peptide Synthesis
Various peptides, tptddyddtpt (all
Antibodies and Cells
The antibody ch806 targets EGFR that is overexpressed, amplified, or mutated (de2-7 EGFR or EGFRvIII) and was produced in house as described previously. 11 The U87MG.de2-7 glioblastoma cells that overexpress mutated EGFR were obtained and cultured as described previously. 10
Antibody Conjugation and Radiolabeling
Ch806 was iodinated directly using 125I and indirectly with 111In via the bifunctional metal ion chelate CHX-A″-DTPA (Macrocyclics Inc, Dallas, Texas) as described previously. 30 For radioiodination using 125I, reaction was performed using pH-neutralized isotopes, catalyzed by IODO-GEN precoated glass beads ( Thermo Fisher Scientific Pierce, Rockford, Illinois). 11 After a brief 10-minute incubation period, the reaction was purified through a desalting column (Sephadex G50-80; Sigma-Aldrich, Sydney, Australia) equilibrated with phosphate-buffered saline.
For indirect iodination, the ch806 was derivatized with DBCO-PEG4-NHS ester (DBCO-PEG4-NHS, Jena Biosciences, Jena, Germany) at a 5:1 mole ratio according to the manufacturer’s instructions. Azido-derivatized peptides were radiolabeled with one of 125I, 131I, or 124I before attachment to DBCO-PEG4-ch806 (see Supplemental Materials and Methods).
Radiochemical Purity
Radiochemical purity of purified radiolabeled ch806 was analyzed by instant thin-layer chromatography silica gel-impregnated glass fibers (ITLC-SG) using 10% trichloroacetic acid as mobile phase. Radiochemical purity was confirmed by size exclusion chromatography (SEC). A SEC analysis was performed on a Superdex 200 HR10/30 column (Ge Healthcare Australia, Parramatta, Australia) at a flow rate of 0.14 mL/min and fraction size of 3.6 mL. The elution buffer was phosphate-buffered saline at pH 7.4.
Immunoreactivity Assays
The immunoreactivity of radiolabeled ch806 was initially determined using the Lindmo and Scatchard assay as described previously. 11 In these assays, 20 ng of radiolabeled ch806 were mixed with an increasing cell concentration from 0 to 1 × 107 U87MG.de2-7 cells in 1.0 mL of media.
After constant mixing for 45 minutes, the cells were washed by repeated centrifugation and cell pellets counted together with suitable standards. For Scatchard assays, 20 ng of radioconjugates were mixed with an increasing protein concentration from 20 ng to 10 µg in 1.0 mL of media containing 1 × 106 cells. Subsequently, a single point binding assay using a fixed amount of 20 ng of radioconjugates and containing 10 × 106 U87MG.de2-7 cells in 1.0 mL of media, representing conditions for antigen excess, was employed to compare the immunoreactivities of various radiolabeled ch806. The stability of radioconjugate was determined by incubating 15 μg of radioconjugate in a total volume of 75 µL human serum and incubating at 37°C over a period of 7 days. An aliquot of the mixture was diluted for radiochemical purity analysis and single-point immunoreactivity assays (10 × 106 cells) on days 0, 3, and 7.
Animals and Xenografts
The U87MG.de2-7 cells were cultured as described previously. 11 Cells were harvested at the point of confluence using phosphate-buffered saline/0.05% EDTA (w/v) and resuspended in media. For tumor injections, 3.0 × 106 U87MG.de2-7 cells in 0.1 mL of phosphate-buffered saline were injected subcutaneously into the flanks of 4- to 5-week-old female BALB/c nude mice. Tumor sizes were measured using the formula (L × W2) × 0.5, where length (L) was the maximum measurement of the tumor and width (W) was the measurement perpendicular to it. Tumors started to develop 1 week after injection, and mice were used when tumors were greater than 160 mm3. All animal studies were approved by the Austin Health Animal Ethics Committee (Austin Health, Heidelberg, Australia).
Biodistribution Studies
To compare in vivo properties of various ch806 radioconjugates, sterile filtered mixtures of 5.0 µg 125I-ch806 (6 μCi or 222 kBq) and 5.0 µg 131I-PEG4-tptddYddtpt-ch806 (3 μCi or 111 kBq) or 5.0 µg 125I-PEG4-tptddyddtpt (6.5 μCi or 240.5 kBq) and 5.0 µg 111In-CHX-A″-DTPA-ch806 (6 μCi or 222 kBq), in 0.1 mL phosphate-buffered saline/0.05% human serum albumin, were injected in BALB/c nude mice bearing U87MG.de2-7 xenografts (n = 5). Mice were killed at 72 hours after injection by isoflurane (Forane, Baxter Australia, Old Toongabbie, Australia) overinhalation, followed by exsanguination via cardiac puncture to collect blood. Tumors and organs (skin, liver, spleen, intestine, stomach, kidneys, brain, bone [femur], lungs, and heart) were harvested immediately, blot dried, and weighed (Sartorius Basic Balance, Germany). All samples were counted for radioactivity in a gamma scintillation counter (Wizard, PerkinElmer, Sydney, Australia) set with appropriate dual channel windows. Standards of a known radioactive concentration prepared from the injected materials were counted each time with blood and tissue samples enabling calculations to be corrected for the physical decay of the isotopes. Results of labeled antibody distribution over time were expressed as percentage of injected dose per gram (% ID/g) ([counts per minute for tissue sample/counts per minute for standard] × 100 /weight in grams).
In addition, a full biodistribution study was conducted by injecting 5.0 µg of 124I-PEG4-tptddYddtpt-ch806 (3.5 μCi or 129.5 kBq) in U87MG.de2-7 tumor-bearing mice. At 2, 24, 48, 72, 120 and 168 hours after injection, 5 mice were killed and blood and tissues were collected. Blood clearance kinetics were determined using a pharmacokinetic curve-fitting program (WinNonlin phoenix, Pharsight Corp, California).
Positron Emission Tomography/Magnetic Resonance Imaging
A separate group of 5 U87MG.de2-7 tumor-bearing mice were injected intravenously via the tail vein with 74 μg of 124I-PEG4-tptddYddtpt-ch806 (1.92 MBq). PET/magnetic resonance imaging (PET/MRI) was performed on a nanoScan PET/magnetic resonance (MR; Mediso, Budapest, Hungary) on 2 mice at the ACRF Centre for Translational Cancer Therapeutics and Imaging (Melbourne, Australia) at 2, 72, and 168 hours after injection. Mice were anaesthetized with isoflurane via inhalation and maintained in a MINERVE anesthetic assembly (Equipement Vétérinaire MINERVE, Esternay, France). The mouse was then transferred to 1 single-mouse anesthesia/imaging closet chamber for MRI scans in tail-first supine position, followed by a 30-minute PET static scan at 2, 72, and 168 hours after injection. All PET raw data were decay, dead time, random, and attenuation corrected and were reconstructed into volumetric images with a transaxial matrix size of 255 × 255 using the built-in quasi-Monte Carlo simulation algorithm combined with stochastic iteration and filtered sampling. The voxel dimension in the reconstructed images was 0.4 × 0.4 × 0.4 mm. The mice were culled and blood and tissues obtained for radioactive counting together with standards.
Statistical Analysis
Data are presented as mean ± standard deviation. Statistical analysis was performed using a paired t test (GraphPad Prism, version 6.03, GraphPad Software, La Jolla California USA, http://www.graphpad.com) to compare differences between radioconjugates injected in the same mice and an unpaired t test (GraphPad Prism, version 6.03) to compare differences between radioconjugates injected in separate mice. For multiple comparisons, 1-way analysis of variance (GraphPad Prism, version 6.03) was used. P values are indicated and considered significant when P < .5.
Results
Properties of Radiolabeled ch806 Antibodies
Radiochemical properties of radiolabeled ch806 antibodies are shown in Table 1. Radiolabeling efficiencies of radioiodinated ch806 antibodies ranged from 23% to 70%, radiochemical purities ranged from 98.0% to 99.9%, and specific activities ranged from 22.2% to 48.1 MBq/mg. The binding properties of radioconjugates were initially determined using the Lindmo assay to ascertain conditions for maximal binding in the presence of antigen excess. We observed that maximal binding occurred at a cell concentration of 5 million cells/mL of media (see Figure 2). Subsequently, a single point assay using 10 million cells was deemed suitable to represent conditions for antigen excess (using 20 ng of radioconjugates) for comparing the immunoreactivities of the larger number of radioconjugates, ranging from 64.0% to 79.9% cell binding. Adding meta-bisulfite to the radiolabeled peptide mixture before conjugation to native antibody resulted in <0.1% radiolabeling indicating that it had stopped the iodination reaction. Little direct iodination took place. 111In-CHX-A″-DTPA-ch806 was prepared with 80.4% radiolabeling efficiency, a specific activity of 44.4 MBq/mg, 99.6% radiochemical purity, and 74.6% cell binding in the presence of antigen excess. Results are summarized in Table 1.
Radiochemical Properties of Various ch806 Radioconjugates.
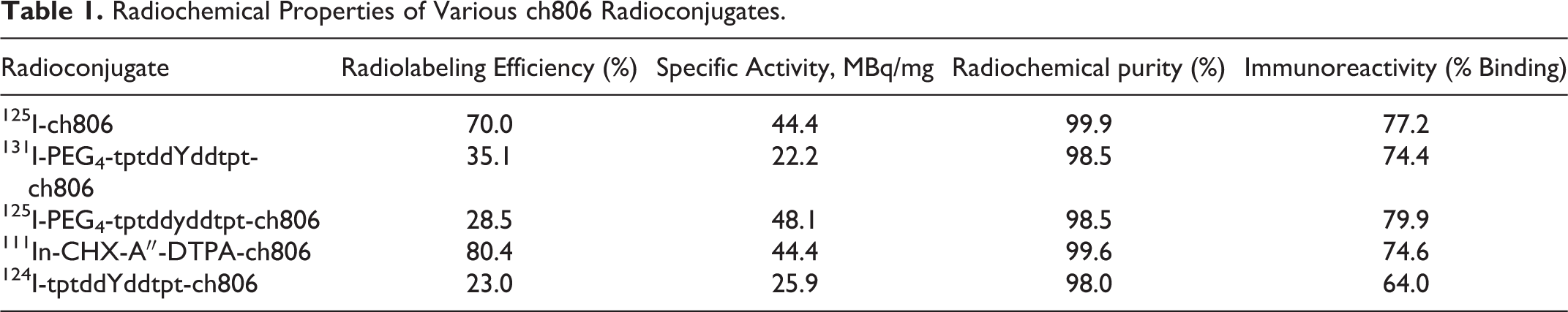
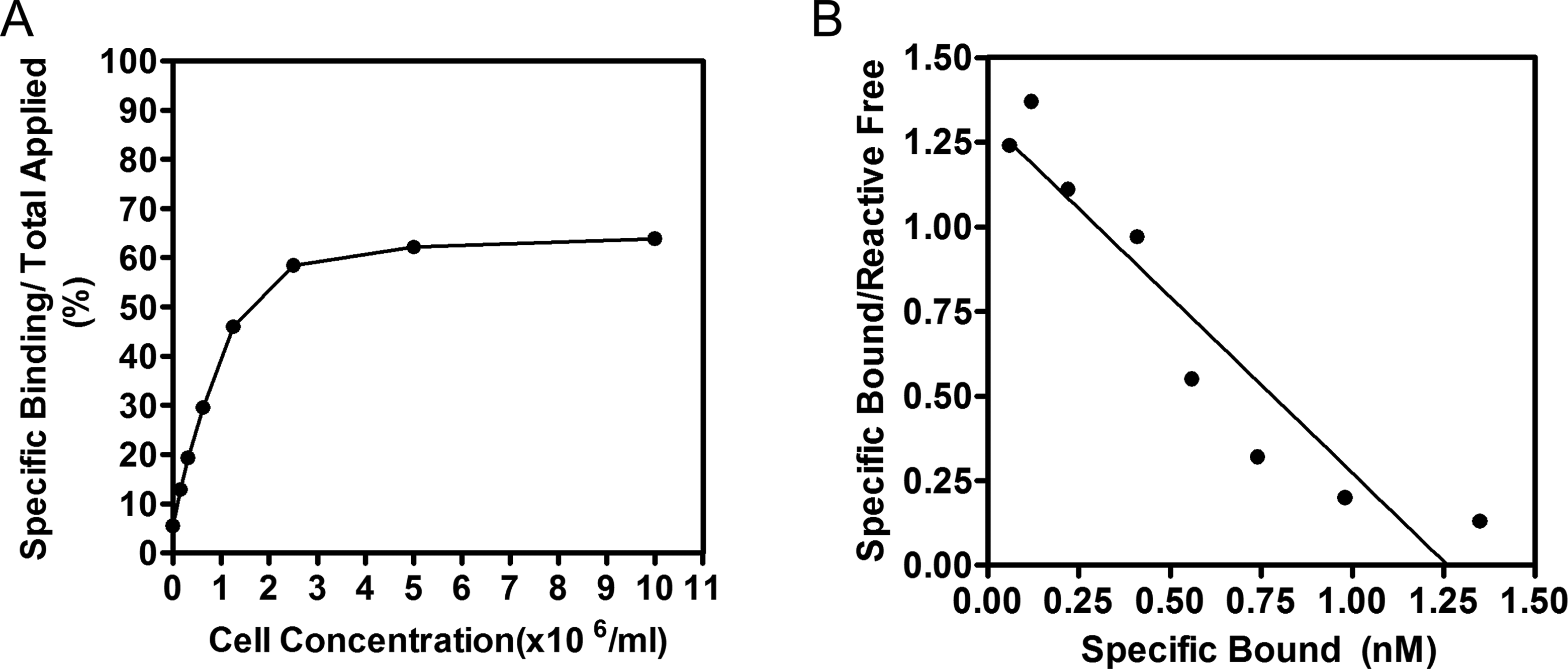
Binding assay for the determination of immunoreactive fraction of an 124I-tptddYddtptch806 antibody binding to U87MG.de2-7 cells. Panel A shows a conventional plot of specific binding over applied radioactivity as a function of increasing cell concentration (Lindmo assay). Panel B shows a Scatchard plot of binding of radioconjugates to the same cells. The abscissa shows the concentration of specifically bound antibody and the ordinate, the ratio of the concentrations of specifically bound over reactive-free antibody.
Lindmo/Scatchard Analysis and Serum Stability of 124I-PEG4-tptddYddtpt-ch806
Radiolabeling efficiency of 124I-PEG4-tptddYddtpt-ch806 was 23.0%, radiochemical purity was 98.0%, specific activity was 25.9 MBq/mg, and immunoreactivity was 64% cell binding in the presence of antigen excess (Figure 2). Scatchard analysis determined that the apparent association constant of 124I-tptddYddtpt-ch806 was 1.04 × 109 M−1, and the number of antibodies bound per cell was approximately 760 000. The stability of the radioconjugate was determined by a single-point immunoreactivity assay after incubation in human serum at 37 C. The immunoreactivity decreased from 64% on day 0, to 44.3% and 39.3% on days 3 and 7, respectively. An ITLC-SG analysis showed a modest decrease in radiochemical purity from 99.6% on day 0 to 93.0% and 87.9% on days 3 and 7, respectively.
Biodistribution
To screen for suitable residualizing peptides, the tumor uptake of various ch806 radioconjugates was compared using biodistribution studies at 72 hours postinjection only, corresponding to maximal tumor uptake previously observed with 111In-CHX-A″-DTPA-ch806.
10
Figure 3 summarizes the blood and tumor values (% ID/g) of these biodistribution studies. Uptake and retention of radioconjugates in tumors are ranked in following order: mixed
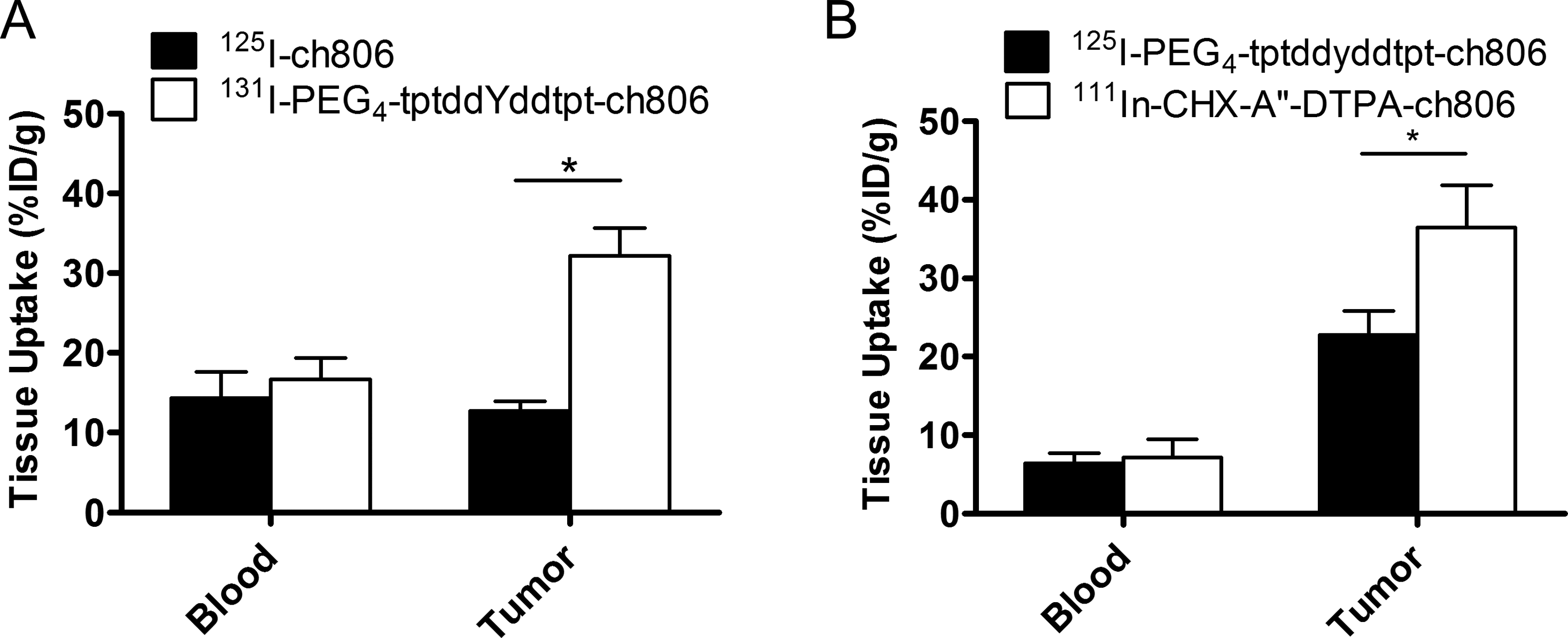
Blood and tumor uptake (% ID/g) of various ch806 radioconjugates in U87MG.de2-7 tumor-bearing mice at 72 hours after injection. Results of biodistribution of 125I-ch806 and 131I-PEG4-tptddYddtpt-ch806 (A) and 125I-PEG4-tptddyddtpt-ch806 and 111In-CHX-A″-DTPA-ch806 (B). Bars, SD; n = 5; *P < .005. SD indicates standard deviation.
The biodistribution properties of 124I-PEG4-tptddYddtpt-ch806 in xenografted mice over 7 days are shown in Table 2. The mean uptake of 124I-PEG4-tptddYddtpt-ch806 by U87MG.de2-7 tumors reached a maximum of 36.03% ± 5.08% ID/g at 72 hours after injection, when tumor sizes were 528.20 ± 75.58 mg. The tumor uptake decreased to 7.44 ± 1.84% ID/g by day 7 after injection. The tumor-to-blood ratios increased from 0.32 ± 0.02 (at 2 hours after injection) to 8.18 ± 1.82 at 72 hours after injection and continued to increase to a high of 35.84 ± 19.47 at 168 hours postinjection. Uptake in normal tissues (eg, kidney and liver) was low, with a time-dependent decrease paralleling that in the blood (Table 2). There was some transient activity in the stomach, which cleared rapidly. The serum half-life of the initial phase of disposition (t½α) was 1.95 ± 0.63 hours, the terminal half-life (t½β) was 25.96 ± 5.29 hours, the area under the curve (AUC) was 46.23 ± 4.56 h.μg/mL, and the total serum clearance was 0.11 ± 0.01 mL/h. The AUC for tumor was 186.13 ± 18.31 h × μg/mL, providing a tumor-to-blood ratio for AUC of 4.03. On day 7, the biodistribution properties of the imaging dose (74 µg/1.92 MBq) in 5 mice were similar to the lower dose (5µg/0.13 MBq; Table 2). The % ID/g values were as follows: blood (0.54 ± 0.21), brain (0.05 ± 0.03), heart (0.46 ± 0.09), lung (0.79± 0.20), stomach (0.35 ± 0.07), spleen (2.25 ± 0.42), liver (2.71 ± 0.31), kidney (6.97 ± 1.58), small intestine (0.19 ± 0.03), colon (0.28 ± 0.14), muscle (0.20 ± 0.04), bone (0.90 ± 1.07), skin (0.87 ± 0.19), and tumor (12.79 ± 3.2). The exceptions were values for blood and tumor. Blood: 0.54 ± 0.21 vs 0.22 ± 0.09 vs 0.54 ± 0.21 % ID/g (P = .0141) and tumor: 12.79 ± 0.88 vs 7.44 ± 2.05 % ID/g (P = .0007). The significantly higher values of the imaging doses in blood and tumor were likely to be related to the higher protein dose used.
Biodistribution of 124I-PEG4-tptddYddtpt-ch806 in BALB/c Nude Mice-Bearing U87MG.de2-7 Xenografts.a

aData presented are % ID/g tissue values (mean ± standard deviation [SD]; n = 5).
Positron Emission Tomography/Magnetic Resonance Imaging
Tumor uptake of 124I-PEG4-tptddYddtpt-ch806 was evident at 72 hours as shown by the fused PET and MR surface-rendered image, together with coronal and transaxial images (Figure 4). Clearance of blood pool activity with time, and some thyroid and abdominal uptake, is consistent with the pharmacokinetics and catabolic pathways of radioiodinated intact antibodies. The average thyroid uptake values of 2 of 5 mice one of which is shown in Figure 4 were day 0 (0.09 g/mLl, day 2 (0.14 g/mL), and day 7 (0.05 g/mL). The corresponding tumor values were day 0 (0.27 g/mL), day 2 (1.27 g/mL), and day 7 (0.63 g/mL). No other normal tissue uptake was observed at the later time points, consistent with the biodistribution study on tissues obtained by radioactive counting of blood and tissues. Coronal and transaxial plane views of PET/MRI image data sets confirmed high uptake of 124I-PEG4-tptddYddtpt-ch806 by the tumor (Figure 4).

Example of fused PET (maximum intensity projection)/MRI (T1-weighted surface rendered) images of U87MG.de2-7 tumor-bearing mice taken at 2 (A), 72 (B) and 168 hours (C) after injection of 124I-PEG4-tptddYddtpt-ch806 showing uptake of radioconjugates in U87MG.de2-7 tumor in the left flank at 72 and 168 hours after injection. Corresponding coronal and transaxial images are also shown (top-bottom). PET indicates positron emission tomography; MRI, magnetic resonance imaging.
Discussion
In recent years, with the availability of 89Zr and suitable bifunctional metal ion chelates, immuno-PET has more and more been used in early-phase cancer clinical trials.
4,5,31
The PET isotope 124I, which has a comparable decay half-life and is suitable for long half-life antibodies, has also been used but has been restricted to antibodies that are not extensively internalized and catabolized which avoids dehalogenation from intracellular enzymes.
32
In an attempt to trap radioiodinated catabolites in lysosomes, various strategies have been developed.
16
–28
A DTPA-appended
In this study, a
The present study showed that 124I-PEG4-tptddYddtpt-ch806 could be radiolabeled efficiently and maintained radiochemical purity for up to 7 days. Although the immunoreactivity of 124I-PEG4-tptddYddtpt-ch806 declined with time, the results are consistent with other immunoconjugates successfully applied in the clinic. 34,35 124I-PEG4-tptddYddtpt-ch806 showed biodistribution properties and tumor retention in U87MG.de2-7 xenografts similar to that of 111In-CHX-A″-DTPA-ch80610 and 124I-IMP-R4-ch806. 11 In terms of clinical applications, this peptide should be useful for immuno-PET. Doses of up to 185 to 370 MBq of directly radiolabeled 124I-antibodies such as cG250 have been successfully used for immuno-PET in the clinic, 36,37 with preclinical tumor uptake of radioiodinated cG250 similar to as observed with 124I-PEG4-tptddYddtpt-ch806. These doses can be obtained with the current labeling efficiency observed (23.0%-35.1%). This peptide is a first-generation reagent, and modifications can be made to improve radiolabeling yields. In one instance, the more recent click chemistry pair of transcyclooctene and tetrazine linkage is reported to be more efficient compared to the present DBCO and azido linkage. We have also introduced the use of soluble tyrosine peptides (ddYdd or DDYDD) to quench the iodination reaction before adding derivatized antibody. These measures will likely improve the overall radiolabeling efficiency of radioiodination.
124I-PEG4-tptddYddtpt-ch806 showed a 3-fold increase in tumor uptake compared to directly radioiodinated 125I-ch806, and tumor-to-blood ratios increased from 0.32:1 at 2 hours after injection to 35.84:1 at 168 hours after injection. These values are similar to values found with other improved
The potential effect of peptide modifications of ch806 antibody on changes in physical, chemical, and subsequent biodistribution properties should be minimal. In our previous studies, 10,11 we have shown that using low conjugation ratio between ligand and antibody did not alter properties in a measurable way. Derivatizing ch806 with the bifunctional metal ion chelate CHX-A″-DTPA (approx molecular weight 1200), containing 5 negative charges, did not alter the biodistribution properties of the 111In-CHX-A″-DTPA ch806 compared to the reference standard 125I-ch806 in terms of pharmacokinectics and tissue distribution (except for tumor uptake).10 Subsequently, we performed a similar study using a residualizing peptide IMP-R4, containing 10 negative charges, to modify the same antibody ch806. Biodistribution studies again showed similar uptake of 124I-IMP-ch806 in tumors and normal tissues, 11 comparable to the well-documented 111In-CHX-A″-DTPA ch806. 10
Our present study used DBCO-PEG4-NHS (molecular weight 649.68) to derivatize the antibody. The PEG4 would have reduced the lipophilicity of DBCO. As the conjugation ratio is again kept low as before, no more than 2 or 3 molecules are expected to be attached to the antibody (molecular weight 150 000). The radioiodinated residualizing peptide-containing 4
The exact mechanism by which 124I-PEG4-tptddYddtpt-ch806 accumulates in tumor cells is as yet unknown.
Conclusions
The present study shows that a mixed
Footnotes
Acknowledgments
The authors wish to thank Ms Rose Bogdal and Mrs Malarmarthy Ramachandran for technical assistance in binding assays and biodistribution studies.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported in part by NHMRC Project grant 1003085 and NHMRC Program grant 487922. Operational Infrastructure Support Program funding was provided by the Victorian Government and funds to purchase the imaging equipment was provided by the Australian Cancer Research Foundation.
